Anorexia nervosa is among the most worrying conditions presented to adolescent mental health services. A consequence of the patient's ill health, family and professional concern and often the patient's resistance to intervention is that a number of teenagers are hospitalised in the course of their illness. Admission to hospital, whether to a paediatric or a psychiatric service, enables a number of short-term benefits. These include physical evaluation and monitoring, providing relief to the patients' family and of professional anxiety, and re-establishment of adequate calorie intake, either by firm encouragement or by nasogastric or other interventions.
The impact of hospital admission on long-term outcome, however, is uncertain. The present study utilises data from two naturalistic studies to compare the outcome of those who had received in-patient treatment during their illness with those who had not. Each subject had received a comprehensive baseline assessment enabling evaluation of the impact of treatment received as against other presenting variables in determining clinical outcome.
METHOD
Subjects
Seventy-five consecutive cases of adolescent-onset anorexia nervosa were drawn from a series attending a regional adolescent service. The service specialises in the treatment of eating disorders and attempts to treat these where possible on an out-patient basis. Where admission is required, it is generally within the general purpose adolescent unit, though on occasions, young people are admitted to either general paediatric services or to specialist eating disorder units, generally within the independent sector. The decision will in an individual case reflect the wishes of the family, community services and local funding policy.
Thirty-five of the cases (four male) were taken from a prospective study into the impact of family variables in anorexia nervosa, which has been reported elsewhere (Reference North, Gowers and ByramNorth et al, 1995; Reference Gowers, North and ByramGowers et al, 1996). These cases were evaluated comprehensively at presentation, at which time the Schedule for Affective Disorders and Schizophrenia-Child Version (K-SADS) diagnostic interview (Reference Ambrosini, Metz and PrabuckiAmbrosini et al, 1989) was administered to confirm the diagnosis, and an assessment of severity, the Global Assessment Score based on the Morgan-Russell Outcome Assessment Schedule (Reference Morgan and HaywardMorgan & Hayward, 1988) was calculated. This comprises five sub-scales covering physical status, menstruation, mental state, sexual adjustment and socio-economic status. Details of length of illness and eating disorder subtype were also recorded, in a detailed record which included weight, height, body mass index and menstrual history.
Subsequently, an additional 40 cases (all female) were obtained from the 40 immediately preceding cases presenting to the department. All had had a detailed clinical assessment with records of heights, weights, clinical subtype and menstrual history, etc. Many of the cases were subsequently treated within the adolescent service and the clinical notes were comprehensive. Details of a range of presenting variables were coded from the case notes retrospectively to match those obtained prospectively in the other study. The items coded included age at onset, age at presentation, length of illness, clinical subtype, weight and height at presentation and weight as percentage of expected weight. Finally, all available clinical data were used to calculate a presenting Global Assessment Score (Reference Morgan and HaywardMorgan & Hayward, 1988) at presentation. This method of calculating a severity score on detailed clinical case notes has been employed elsewhere (Reference Gowers, Crisp and JoughinGowers et al, 1991) and the interrater reliability found to be acceptable.
Follow-up
The 35 cases in the (prospective) family functioning study were contacted after two years. All cases were traced and 33 face-to-face interviews arranged. In two cases, although traced, follow-up assessment was declined and adequate information was not available to provide adequate outcome information. The additional 40 cases were contacted at between three- and seven-year follow-up from initial assessment. All 40 cases were traced. Face-to-face interviews were arranged with 23, of whom 17 also permitted an interview with an informant. Six further subjects were interviewed by telephone, of whom four agreed to an interview with a relative and one contact with their general practitioner. Of the remaining 11 subjects for whom no interview was obtained with the subject, substantial information was provided through an interview with a relative in five cases and contact with the general practitioner in three cases, on one occasion being supplemented by an information sheet, completed by the patient. There was insufficient information available for one of the subjects and two subjects were deceased. Information about these cases was provided by a psychiatrist and a social worker, respectively. Thus, 56 out of 73 surviving cases received all clinical assessments with recorded weight and height information. For these and a further 10 cases with detailed information from informants, the Morgan-Russell Outcome Assessment Schedule was completed. The approved cut-off points for this scale enable classification into good, intermediate and poor outcomes. Although the full Morgan-Russell Global Assessment Score (MRGAS) could not be computed for the remainder, a broad outcome category could be assigned for 72 cases.
Data analysis
Six key variables were identified as likely outcome predictors: age, length of illness, weight as a percentage of mean matched population weight, presenting MRGAS, presence or absence of purging, and setting of treatment received. The data were examined for differences between the two series on key presentation variables. Associations between these variables and outcome group was explored by ANOVA for continuous variables and χ2 for categorical variables. Stepwise multiple regression analysis (enter) was employed to determine the relationship between covarying predictor variables with MRGAS at follow-up as the dependent variable. F was set between 0.05 and 0.1.
RESULTS
Presentation variables
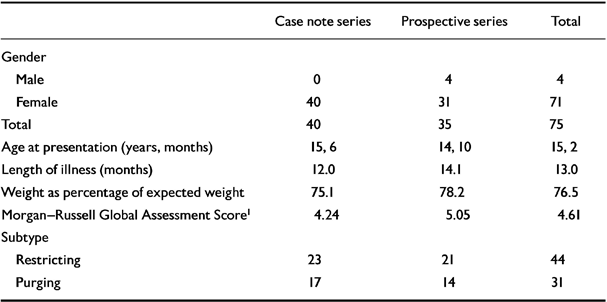
The clinical variables are shown in Table 1. A comparison of clinical variables between the two samples to explore for differences in coding of the MRGAS between prospective and case note methods showed a slightly greater severity (lower MRGAS) for the case note series in comparison to the prospective series. However, it is note-worthy that the case note series was slightly thinner and had a larger proportion of ‘binge-purgers’ in the series, suggesting that the lower MRGAS may reflect a true difference in severity rather than a difference in the method of coding.
Table 1 Clinical variables at presentation
| Case note series | Prospective series | Total | |
|---|---|---|---|
| Gender | |||
| Male | 0 | 4 | 4 |
| Female | 40 | 31 | 71 |
| Total | 40 | 35 | 75 |
| Age at presentation (years, months) | 15, 6 | 14, 10 | 15, 2 |
| Length of illness (months) | 12.0 | 14.1 | 13.0 |
| Weight as percentage of expected weight | 75.1 | 78.2 | 76.5 |
| Morgan—Russell Global Assessment Score1 | 4.24 | 5.05 | 4.61 |
| Subtype | |||
| Restricting | 23 | 21 | 44 |
| Purging | 17 | 14 | 31 |
General outcome
Outcome was defined as good if weight was maintained above 85%, menstruation had resumed and social functioning was satisfactory. In practice, this equated to an MRGAS score of ≥9. Intermediate outcome was recorded if a substantial improvement in eating disorder had been obtained with weight maintained above 85% of expected weight, but where either menstruation had not resumed or there was significant concern about eating and weight or there was another psychosocial difficulty. This equated to a MRGAS score of 6-9. A poor outcome (MRGAS <6) was assigned if the subject was still suffering from an eating disorder and in all cases where weight was maintained below 85%. Table 2 shows the general outcome at two- to seven-year follow-up.
Table 2 General outcome at 2-7 years

| Outcome | n (%) |
|---|---|
| Good | 34 (45.3) |
| Intermediate | 23 (30.7) |
| Poor (including deceased) | 15 (20.0) |
| Inadequate information | 3 (4.0) |
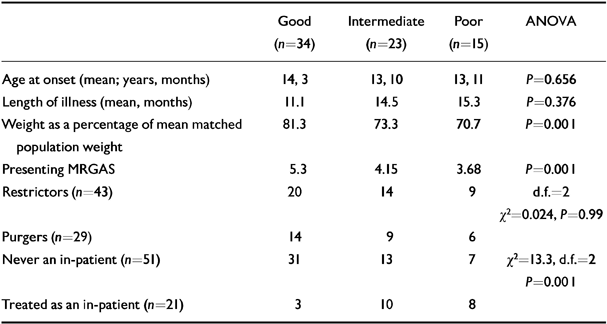
Of the five presentation variables selected as possible predictors, weight at presentation as a percentage of expected weight and presenting MRGAS were both strongly predictive of outcome (see Table 3), age at onset of disorder, length of illness and presence of the purging subtype were not predictive. In addition, treatment received between assessment and follow-up was highly predictive of outcome. If the subject had never been treated as an in-patient, they had a 62% chance of having a good outcome, whereas of those treated as in-patients, only three out of 21 (14.3%) had a good outcome (see Table 3).
Table 3 Outcome of key predictor variables
| Good (n=34) | Intermediate (n=23) | Poor (n=15) | ANOVA | |
|---|---|---|---|---|
| Age at onset (mean; years, months) | 14, 3 | 13, 10 | 13, 11 | P=0.656 |
| Length of illness (mean, months) | 11.1 | 14.5 | 15.3 | P=0.376 |
| Weight as a percentage of mean matched population weight | 81.3 | 73.3 | 70.7 | P=0.001 |
| Presenting MRGAS | 5.3 | 4.15 | 3.68 | P=0.001 |
| Restrictors (n=43) | 20 | 14 | 9 | d.f.=2 |
| χ2=0.024, P=0.99 | ||||
| Purgers (n=29) | 14 | 9 | 6 | |
| Never an in-patient (n=51) | 31 | 13 | 7 | χ2=13.3, d.f.=2 |
| P=0.001 | ||||
| Treated as an in-patient (n=21) | 3 | 10 | 8 |
To explore the relationship between admission to hospital and other predictor variables the six predictor variables were entered into a multiple regression analysis as described in the method. The multiple regression analysis is shown in Table 4.
Table 4 Multiple regression analysis

| Variable entered | Multiple R | R 2 | F | Significance of F | |
|---|---|---|---|---|---|
| Step 1 | In-patient admission | 0.41 | 0.16 | 13.02 | 0.0006 |
| Step 2 | Presenting MRGAS | 0.50 | 0.25 | 10.54 | 0.001 |
The best fit model selected presence of in-patient admission first, followed by presenting MRGAS second. No other variables were selected as significant predictors of outcome once these two variables had been selected.
DISCUSSION
General outcome
The mortality of anorexia nervosa is said to exceed that of any other adolescent psychiatric disorder including depression, with a lethal outcome in up to 15% of cases (Reference Herzog, Rathner and VandereyckenHerzog et al, 1992). In the long term the outcome, though variable, is often chronic (Reference Ratnasuriya, Eisler and SzmuklerRatnasuriya et al, 1991). Only about 50% of younger subjects can be expected to recover fully (Reference Bryant-Waugh, Knibbs and FossonBryant-Waugh et al, 1988).
The outcome of in-patient treatment is very variable. One well-conducted study comparing two forms of follow-up therapy after discharge from hospital gave poor overall outcomes (Reference Russell, Szmukler and DareRussell et al, 1987), though patients may have been selected for this service on the basis of illness severity. There are no randomised controlled trials of in-patient v. out-patient treatment in adolescent anorexia nervosa. An attempt at such a study with patients spanning adolescence and adulthood (Reference Crisp, Norton and GowersCrisp et al, 1991) suffered a number of practical and ethical difficulties in which adherence with treatment was a significant one. This study showed no advantage for in-patient treatment over out-patient approaches, while the latter showed some advantages in terms of social adjustment at one-year follow-up. Further progress towards recovery occurred for the out-patients in the ensuing year (Reference Gowers, Norton and HalekGowers et al, 1994).
The outcome of the present series of 75 cases with adolescent anorexia nervosa is comparable to the outcome reported in the literature, with just under half having a good outcome at 2-7 years. The mortality rate of two cases out of 75 provides confirmation of the danger of this condition.
Predictors of outcome
There is a clear association between the severity of the condition at presentation and its medium- to long-term outcome. Thus, the more underweight the patient, particularly if below 70% of expected weight, and the lower the score on the MRGAS, which equates to global severity, the worse the outcome. Age, length of illness and presence of the purging subtype, however, were not significantly associated with out-come, though there was a non-significant trend towards an association between longer illness before assessment and poor outcome.
Treatment received was strongly associated with outcome, those treated as in-patients having a notably poor outcome. Although in-patient treatment is likely to be reserved for those with the most severe form of disorder, the results do not lend compelling support to the effectiveness of this intervention. Those admitted are likely to have attained normal weight during the course of admission, further pointing to the poor association between weight restoration alone and good outcome. The multiple regression analysis suggests that when treatment is considered alongside other predictors of outcome, receipt of in-patient treatment is the most important predictor of poor outcome. This important finding requires further examination.
Patient's views
Admission to hospital is not always perceived negatively by the patient. Particularly in settings where attention is given to psychological aspects of the disorder, the patient may well see these as supportive. Sometimes the understanding and care of professional staff exceeds that experienced outside the hospital setting, while the peer group and educational setting within the adolescent unit is perceived as a safer environment, divorced from the stresses of life in the outside world. In such a situation, discharge from hospital requires an enormous adjustment in terms of resumption of responsibilities and obligations relating to eating and otherwise, while it can also be experienced as involving a significant loss of support. Not infrequently, life outside hospital is seen as tough and when this results in return of anorexic behaviours, the possibility of return to hospital is perceived by the patient, not negatively, but as an opportunity for further escape.
There are a number of reviews asking patients about their experiences of hospital treatment. These are variable and some are very positive about their experiences. In general, however, in-patient treatments do not appear to be well received nor identified as the main element in recovery where this has occurred. Although not necessarily representative, the accounts collated by the Eating Disorders Association published elsewhere are often extremely critical (Reference ShelleyShelley, 1997). Bruch (Reference Bruch1974) has also drawn attention to a mismatch in perception between professionals' and patients' views; that is to say, the treating professionals often saw admission as having been helpful to the patient while the patient did not.
Clinical implications
In deciding to admit an adolescent to hospital for treatment of anorexia nervosa, the likely positive impact on outcome of the condition should be considered carefully, as well as the possible costs. In practical terms, the cost of hospitalisation is high, with the cost of a typical three-month stay in an adolescent unit amounting to £15 000-20 000 (1999 figures: Mersey Regional Young People's Centre; further details available from the first author upon request). There are, of course, other costs such as disruption of education and family life, some of which may be merely inconveniences, others having relatively long-term repercussions. Other consequences might possibly impact negatively on the disorder itself. Poor self-esteem and lack of social confidence are usually integral features of the disorder. Admission to hospital, particularly with coercive treatments, is unlikely to improve these (Reference Tiller, Schmidt and TreasureTiller et al, 1993), while a sense of personal ineffectiveness, particularly where this might be rooted in a history of abuse, may be reinforced by enforced treatment. Where patients manage to recover from anorexia nervosa, as in recovery from an addiction or a phobia, it is usually necessary for them to take an active part in treatment especially with regard to making a positive decision to overcome difficulties. The importance of addressing motivation in therapeutic work has recently been explored (Reference Ward, Troop and ToddWard et al, 1996). The decision to hospitalise may give an unrealistic message to the patient and family that this is a condition which can be overcome by professionals ‘doing something to’ the patient rather than supporting him or her in the decision to change. It is possible that the decision to admit selects out a poorly motivated subgroup, where early response to treatment has been poor.
All effective treatments are likely to have the potential to cause negative (side-) effects as well as positive benefits. The possible negative consequences of in-patient treatment are under-researched. They may be particularly important for younger subjects. The implication for adult treatment is unclear. Although admission to hospital can clearly provide short-term benefits in terms of restoration of physical health and on occasions might be life-saving, the possibility that lengthy admissions might undermine the potential for longer-term recovery, requires urgent further consideration. In the absence of randomised-controlled trials, less powerful research methods such as those employed here can contribute usefully to the treatment debate.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The extra value of in-patient treatment over out-patient management needs further investigation.
-
▪ Admission may cause harm as well as benefit in anorexia nervosa.
-
▪ Gains achieved in hospital are frequently reversed by longer-term follow-up.
LIMITATIONS
-
▪ A randomised-controlled trial is necessary to clarify the relative merits of in- and out-patient approaches.
-
▪ Some of this series was rated partly using retrospective methods.
-
▪ Comprehensive face-to-face interviews were not obtained for a quarter of the sample.









eLetters
No eLetters have been published for this article.