Comorbidity between panic and depression is the single strongest type of anxiety-mood comorbidity in both treatment (Reference ClaytonClayton, 1990) and general population (Reference Merikangas, Angst and EatonMerikangas et al, 1996) samples. Largely based on clinical studies, this specific comorbidity is also thought to be a more severe condition associated with greater symptom severity (Reference Clancy, Noyes and HoenkClancy et al, 1978; Reference Van Valkenberg, Akiskal and PuzantianVan Valkenberg et al, 1984; Reference Vollrath and AngstVollrath & Angst, 1989; Reference Noyes, Reich and ChristansenNoyes et al, 1990; Reference Roy-Byrne, Vitaliano and CowleyRoy-Byrne et al, 1992), poorer outcome (Reference Clancy, Noyes and HoenkClancy et al, 1978; Reference Noyes, Reich and ChristansenNoyes et al, 1990) and treatment response (Reference Keller, Lavori and GoldenbergKeller et al, 1993), more suicide attempts (Reference Johnson, Weissman and KlermanJohnson et al, 1990) and more functional impairment (Reference Clancy, Noyes and HoenkClancy et al, 1978; Reference Van Valkenberg, Akiskal and PuzantianVan Valkenberg et al, 1984) than either pure panic or pure depression. However, these studies have numerous limitations that include: failure to compare the comorbid syndrome to both disorders; focusing on symptom severity rather than outcome and disability; not controlling for the effects of additional comorbid diagnoses (Reference Stein, Tancer and UhdeStein et al, 1990); focusing only on current comorbidity; not considering effects of the primary v. secondary distinction (i.e. which disorder appeared first); and using treatment samples where treatment-seeking and severity of illness are confounded, thus compromising the ability to elucidate more fundamental processes and relationships. To address these shortcomings, the current report presents epidemiological data on lifetime panic-depression comorbidity from the National Comorbidity Survey (NCS; Reference Kessler, McGonagle and ZhaoKessler et al, 1994), which is a large nationally representative survey of the US household population.
METHOD
Sample
The NCS is a nationally representative household survey of persons aged 15-54 years in the non-institutionalised civilian population of the 48 co-terminous states, along with a representative supplemental sample of students living in campus group housing. The NCS was administered to 8098 respondents between 14 September 1990 and 6 February 1992 in face-to-face in-home interviews. The response rate was 82.4%. The data reported here have been weighted to adjust for differential probabilities of selection and non-response. More details on the NCS design, field procedures and sample weights are reported elsewhere (Reference KesslerKessler, 1995).
Diagnostic assessment
The NCS diagnoses are based on a modified version of the Composite International Diagnostic Interview (CIDI; World Health Organization, 1990), which is a fully structured interview designed to be administered by interviewers who are not clinicians and to generate diagnoses according to the definitions and criteria of both DSM-III-R (American Psychiatric Association, 1987) and ICD-10 (World Health Organization, 1991). The WHO CIDI field trials found good short-term test-retest reliability (for major depression, κ=0.62; for panic disorder, κ=0.84) and procedural validity (for major depression, κ =0.53; for panic disorder, κ=0.43) of the CIDI compared with clinical assessments made by psychiatrists using a DSM-III-R check-list (Reference WittchenWittchen, 1994). Good reliability and validity compared with clinician assessments were also found for retrospective age of onset reports (Reference Wittchen, Burke and SemlerWittchen et al, 1989).
The DSM-III-R diagnoses of special interest in this report are panic attack, panic disorder with or without agoraphobia and major depressive episode. Regarding panic, it is important to note that the NCS obtained separate information on age of onset of first panic attack and age of onset of panic disorder (four or more attacks in a four-week period or a month of persistent worry of having another attack). Regarding major depression, it is important to emphasise that we focus on major depressive episode (i.e. without diagnostic hierarchy exclusions) rather than major depressive disorder. This means that we include conditions known to have high rates of comorbid panic, such as bipolar disorder and psychotic depression, in the definition of depression. We also examine comorbidities with the other DSM-III-R disorders assessed in the NCS. These include other anxiety disorders (phobias, generalised anxiety disorder, post-traumatic stress disorder), mania, addictive disorders (alcohol and drug abuse and dependence), conduct disorder, adult antisocial behaviour and non-affective psychosis.
Analysis procedures
The Kaplan-Meier method (Reference Kaplan and MeierKaplan & Meier, 1958) was used to examine the cumulative lifetime prevalences of panic and depression. Conditional probabilities and odds ratios were used to study comorbidity. Retrospective age of onset reports were used to study temporal priorities between first onset of panic and depression. Logistic regression analysis (Reference Hosmer and LemeshowHosmer & Lemeshow, 1989) was used to study the consequences of comorbidity for impairment and course. Significance tests were computed using the method of jack-knife repeated replications (Reference Kish and FrankelKish & Frankel, 1974) to adjust for design effects introduced by clustering and weighting of observations.
RESULTS
Lifetime prevalences and comorbidities between panic and depression
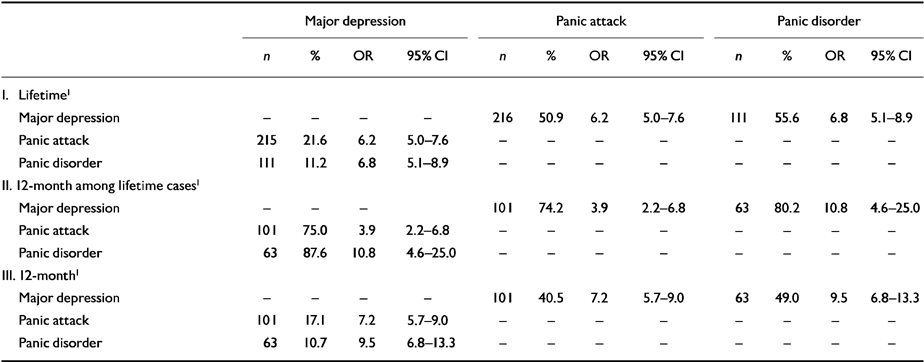
The lifetime and 12-month prevalences of DSM-III-R panic and depression in the NCS have been reported previously (Reference Blazer, Kessler and McGonagleBlazer et al, 1994; Reference Eaton, Kessler and WittchenEaton et al, 1994) and include 7.2% (n=423) and 4.2% (n=250) for panic attack, 3.4% (n=200) and 2.2% (n=129) for panic disorder and 16.9% (n=995) and 10% (n=589) for major depressive episode. As shown in Part I of Table 1, substantially more respondents with lifetime panic attack and panic disorder meet the lifetime criteria for major depression than people with lifetime major depression meet lifetime criteria for panic attack or panic disorder. The odds ratios (ORs) between panic and depression, also reported previously (Reference Kessler, Stang and WittchenKessler et al, 1998), are substantial in magnitude. The slightly higher OR for panic disorder than panic attack means that major depression is modestly related to panic disorder in the subsample of respondents with panic attacks. The results in Part II of Table 1 show that there is also significant episode comorbidity between panic and depression among those with a lifetime history of both disorders. This means that the persistence of one disorder is associated with that of the other. The results in Part III show the joint effects of lifetime comorbidity and episode comorbidity among lifetime cases, the combined effects of which lead to stronger total-sample ORs between 12-month than between lifetime disorders.
Table 1 Lifetime and 12-month comorbidities of major depression, panic attack and panic disorder
| Major depression | Panic attack | Panic disorder | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | OR | 95% Cl | n | % | OR | 95% Cl | n | % | OR | 95% Cl | |
| I. Lifetime1 | ||||||||||||
| Major depression | - | - | - | - | 216 | 50.9 | 6.2 | 5.0-7.6 | 111 | 55.6 | 6.8 | 5.1-8.9 |
| Panic attack | 215 | 21.6 | 6.2 | 5.0-7.6 | - | - | - | - | - | - | - | - |
| Panic disorder | 111 | 11.2 | 6.8 | 5.1-8.9 | - | - | - | - | - | - | - | - |
| II. 12-month among lifetime cases1 | ||||||||||||
| Major depression | - | - | - | 101 | 74.2 | 3.9 | 2.2-6.8 | 63 | 80.2 | 10.8 | 4.6-25.0 | |
| Panic attack | 101 | 75.0 | 3.9 | 2.2-6.8 | - | - | - | - | - | - | - | - |
| Panic disorder | 63 | 87.6 | 10.8 | 4.6-25.0 | - | - | - | - | - | - | - | - |
| III. 12-month1 | ||||||||||||
| Major depression | - | - | - | - | 101 | 40.5 | 7.2 | 5.7-9.0 | 63 | 49.0 | 9.5 | 6.8-13.3 |
| Panic attack | 101 | 17.1 | 7.2 | 5.7-9.0 | - | - | - | - | - | - | - | - |
| Panic disorder | 63 | 10.7 | 9.5 | 6.8-13.3 | - | - | - | - | - | - | - | - |
Association of comorbidity with symptoms
Respondents suffering from panic attack with comorbid lifetime major depression reported a significantly larger number of physiological symptoms during their attacks (9.1) than those without lifetime major depression (7.9, z=5.7, P<0.001). This was even more significant when other diagnoses were controlled for (7.5 v. 6.7, z=3.6, P=0.0003). Respondents with 12-month major depression did not report more panic attack symptoms than those with lifetime major depression alone (z=0.1) and order of onset of major depression and panic attack had no effect on these results. Respondents suffering from major depression with comorbid lifetime panic attack reported a significantly larger number of DSM-III-R Criterion A depressive symptoms during their episodes of major depression (7.1) than those without lifetime panic attack (6.5, z=6.6, P<0.001). This was also more significant when other diagnoses were controlled for (6.6 v. 6.3, z=3.6, P=0.0003). Respondents with 12-month panic attack did not report more major depressive symptoms than cases with lifetime panic attack alone (z=0.8) and order of onset of major depression and panic attack again had no effect on these results. Furthermore, a significant linear association was found between number of physiological symptoms during panic attacks and number of depressive symptoms during depressive episodes in the subsample of respondents with a lifetime history of both panic attack and major depression (r=0.32, z=3.1, P=0.002), as well as in those with just 12-month major depression and panic attack (r=0.48, z=3.1, P=0.002). However, these results disappeared when other diagnosis were controlled for. Finally, there was no relationship between comorbidity and symptom profiles. In particular, respondents suffering from major depression with comorbid panic did not differ from those without panic in whether they had typical or atypical (reverse vegetative) symptoms of depression.
Association of comorbidity with impairment, course and help-seeking
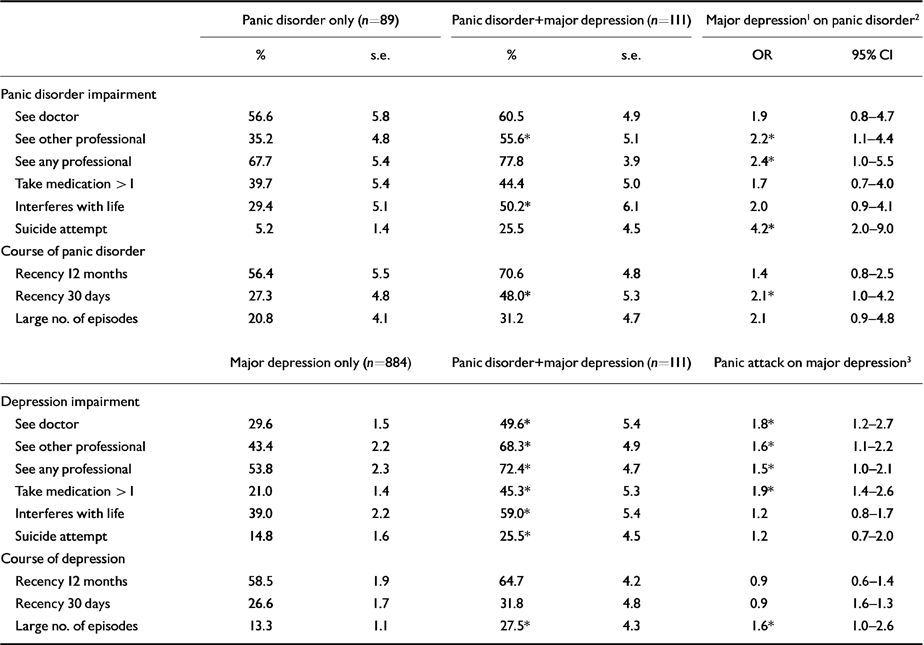
Table 2 focuses on the association of lifetime panic disorder and major depression comorbidity with several different measures of lifetime impairment (help-seeking, perceived role impairment, suicide attempts) and course of illness (recency of active disorders, frequency of lifetime depressive episodes or panic attacks). The top half of Table 2 looks at the association of comorbid major depression with the impairment and course of panic disorder in the subsample of respondents with a history of panic disorder. Without controlling for potential demographic and clinical-diagnostic confounding factors (i.e. the presence of other prior psychiatric disorders), patients with lifetime comorbidity were significantly more impaired and showed a more severe course than those with panic disorder alone. Striking findings are the greater professional help-seeking, perceived role impairment and prevalence of attempted suicide compared with panic disorder alone, and more recent panic attacks in these patients with lifetime depression. A logistic regression analysis of the same variables, controlling for demographics and other prior psychiatric diagnoses, did not change the findings. The bottom half of Table 2 looks at the association of comorbid panic disorder with the impairment and course of major depression in the sub-sample of respondents with a history of major depression. The association of comorbidity with greater impairment and more severe course is again evident in the initial analyses, which do not control for confounding factors, with greater professional help-seeking, perceived role impairment, prevalence of attempted suicide and more depressive episodes in depressed patients with lifetime panic. When logistic regression was used to control for demographics and other prior psychiatric diagnoses, only the association of panic with additional depressive suicide risk disappeared. Temporal priority of panic disorder and major depression had little impact on the outcome measures in Table 2 (see table footnote).
Table 2 Association of lifetime panic disorder-major depression comorbidity with lifetime impairment and course of illness
| Panic disorder only (n=89) | Panic disorder+major depression (n=111) | Major depression1 on panic disorder2 | ||||
|---|---|---|---|---|---|---|
| % | s.e. | % | s.e. | OR | 95% Cl | |
| Panic disorder impairment | ||||||
| See doctor | 56.6 | 5.8 | 60.5 | 4.9 | 1.9 | 0.8-4.7 |
| See other professional | 35.2 | 4.8 | 55.6* | 5.1 | 2.2* | 1.1-4.4 |
| See any professional | 67.7 | 5.4 | 77.8 | 3.9 | 2.4* | 1.0-5.5 |
| Take medication > 1 | 39.7 | 5.4 | 44.4 | 5.0 | 1.7 | 0.7-4.0 |
| Interferes with life | 29.4 | 5.1 | 50.2* | 6.1 | 2.0 | 0.9-4.1 |
| Suicide attempt | 5.2 | 1.4 | 25.5 | 4.5 | 4.2* | 2.0-9.0 |
| Course of panic disorder | ||||||
| Recency 12 months | 56.4 | 5.5 | 70.6 | 4.8 | 1.4 | 0.8-2.5 |
| Recency 30 days | 27.3 | 4.8 | 48.0* | 5.3 | 2.1* | 1.0-4.2 |
| Large no. of episodes | 20.8 | 4.1 | 31.2 | 4.7 | 2.1 | 0.9-4.8 |
| Major depression only (n=884) | Panic disorder+major depression (n=111) | Panic attack on major depression3 | ||||
| Depression impairment | ||||||
| See doctor | 29.6 | 1.5 | 49.6* | 5.4 | 1.8* | 1.2-2.7 |
| See other professional | 43.4 | 2.2 | 68.3* | 4.9 | 1.6* | 1.1-2.2 |
| See any professional | 53.8 | 2.3 | 72.4* | 4.7 | 1.5* | 1.0-2.1 |
| Take medication > 1 | 21.0 | 1.4 | 45.3* | 5.3 | 1.9* | 1.4-2.6 |
| Interferes with life | 39.0 | 2.2 | 59.0* | 5.4 | 1.2 | 0.8-1.7 |
| Suicide attempt | 14.8 | 1.6 | 25.5* | 4.5 | 1.2 | 0.7-2.0 |
| Course of depression | ||||||
| Recency 12 months | 58.5 | 1.9 | 64.7 | 4.2 | 0.9 | 0.6-1.4 |
| Recency 30 days | 26.6 | 1.7 | 31.8 | 4.8 | 0.9 | 1.6-1.3 |
| Large no. of episodes | 13.3 | 1.1 | 27.5* | 4.3 | 1.6* | 1.0-2.6 |
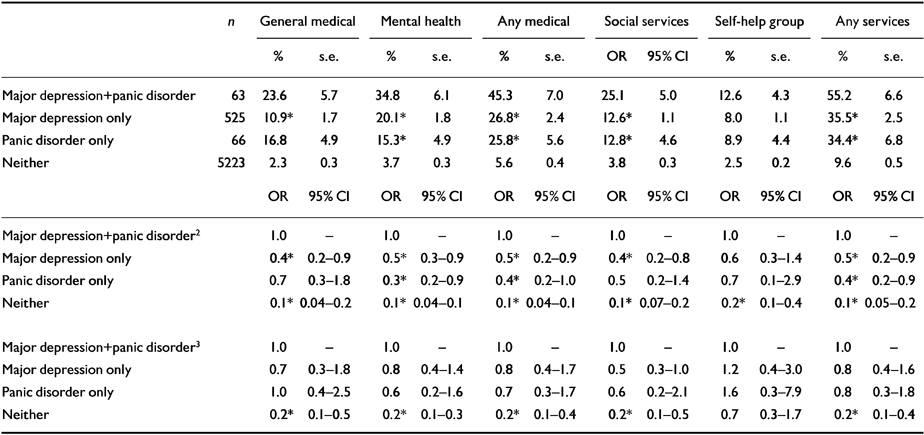
Table 3 focuses on recent (past 12 months) use of services for psychiatric problems among respondents with 12-month panic disorder and/or major depression compared with those without either 12-month disorder. The top part of Table 3 shows that prevalences of any service use are significantly higher among those with comorbid panic disorder and major depression than those with only one of the two disorders in each of the major treatment sectors other than the self-help sector. There is also a fairly consistent trend across service sectors for treatment intensity to be greater for those with comorbidity than pure disorders, as indicated by average number of visits among those in treatment. However, only two of these contrasts are statistically significant owing to the small number of observations in the treatment subsamples. The middle and bottom parts of Table 3 fit logistic regression models to the descriptive service use data in the top part and show that the comorbid group is at increased risk for 12-month service use when only demographics are controlled for (middle part) but that when other comorbid psychiatric disorders are controlled for (bottom part) this increased service use risk disappears.
Table 3 Association of 12-month comorbidity with service use (% in treatment) for psychiatric problems1
| n | General medical | Mental health | Any medical | Social services | Self-help group | Any services | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| % | s.e. | % | s.e. | % | s.e. | OR | 95% CI | % | s.e. | % | s.e. | ||
| Major depression+panic disorder | 63 | 23.6 | 5.7 | 34.8 | 6.1 | 45.3 | 7.0 | 25.1 | 5.0 | 12.6 | 4.3 | 55.2 | 6.6 |
| Major depression only | 525 | 10.9* | 1.7 | 20.1* | 1.8 | 26.8* | 2.4 | 12.6* | 1.1 | 8.0 | 1.1 | 35.5* | 2.5 |
| Panic disorder only | 66 | 16.8 | 4.9 | 15.3* | 4.9 | 25.8* | 5.6 | 12.8* | 4.6 | 8.9 | 4.4 | 34.4* | 6.8 |
| Neither | 5223 | 2.3 | 0.3 | 3.7 | 0.3 | 5.6 | 0.4 | 3.8 | 0.3 | 2.5 | 0.2 | 9.6 | 0.5 |
| OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | ||
| Major depression+panic disorder2 | 1.0 | - | 1.0 | - | 1.0 | - | 1.0 | - | 1.0 | - | 1.0 | - | |
| Major depression only | 0.4* | 0.2-0.9 | 0.5* | 0.3-0.9 | 0.5* | 0.2-0.9 | 0.4* | 0.2-0.8 | 0.6 | 0.3-1.4 | 0.5* | 0.2-0.9 | |
| Panic disorder only | 0.7 | 0.3-1.8 | 0.3* | 0.2-0.9 | 0.4* | 0.2-1.0 | 0.5 | 0.2-1.4 | 0.7 | 0.1-2.9 | 0.4* | 0.2-0.9 | |
| Neither | 0.1* | 0.04-0.2 | 0.1* | 0.04-0.1 | 0.1* | 0.04-0.1 | 0.1* | 0.07-0.2 | 0.2* | 0.1-0.4 | 0.1* | 0.05-0.2 | |
| Major depression+panic disorder3 | 1.0 | - | 1.0 | - | 1.0 | - | 1.0 | - | 1.0 | - | 1.0 | - | |
| Major depression only | 0.7 | 0.3-1.8 | 0.8 | 0.4-1.4 | 0.8 | 0.4-1.7 | 0.5 | 0.3-1.0 | 1.2 | 0.4-3.0 | 0.8 | 0.4-1.6 | |
| Panic disorder only | 1.0 | 0.4-2.5 | 0.6 | 0.2-1.6 | 0.7 | 0.3-1.7 | 0.6 | 0.2-2.1 | 1.6 | 0.3-7.9 | 0.8 | 0.3-1.8 | |
| Neither | 0.2* | 0.1-0.5 | 0.2* | 0.1-0.3 | 0.2* | 0.1-0.4 | 0.2* | 0.1-0.5 | 0.7 | 0.3-1.7 | 0.2* | 0.1-0.4 | |
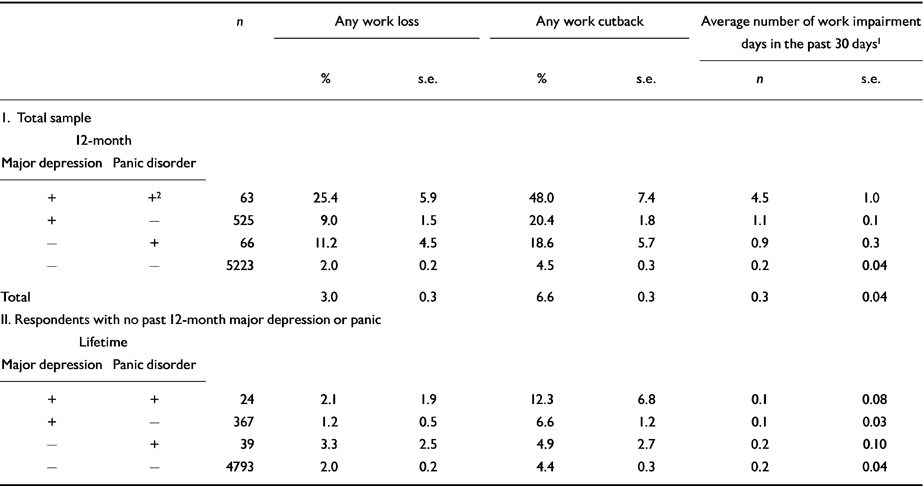
Table 4 focuses on recent (past 30 days) role impairment. The results in Part I of the table show that a quarter of respondents with 12-month comorbid panic disorder and major depression reported missing at least one day of work in the past month because of emotional problems, whereas close to half reported having to cut back on how much they got done at work in the past month because of emotional problems. These proportions are more than twice as high as among respondents with only one of these two 12-month disorders and over 10 times as high as among those with neither disorder. The average number of overall past-month work impairment days (a weighted combination of work loss and work cutback days, where a work cutback day is 40% of a day of lost work) among respondents with past-year comorbidity averages 4.5 days and is over four times as high as among those with only one of the two disorders and over 20 times as high as among those with neither of the disorders. The results in Part II of the table show that there is no significant elevation of these role impairments among respondents with lifetime panic disorder or major depression, or both, whose illnesses are not active, suggesting that these role impairments remit with symptom remission. A logistic regression fit to the descriptive data in Table 4 (see Table 5) confirms that it is indeed 12-month rather than lifetime comorbidity that predicts work impairment.
Table 4 Prevalence of 30-day work loss and work cutback associated with pure and comorbid major depression and panic disorder
| n | Any work loss | Any work cutback | Average number of work impairment days in the past 30 days1 | |||||
|---|---|---|---|---|---|---|---|---|
| % | s.e. | % | s.e. | n | s.e. | |||
| I. Total sample | ||||||||
| 12-month | ||||||||
| Major depression | Panic disorder | |||||||
| + | +2 | 63 | 25.4 | 5.9 | 48.0 | 7.4 | 4.5 | 1.0 |
| + | - | 525 | 9.0 | 1.5 | 20.4 | 1.8 | 1.1 | 0.1 |
| - | + | 66 | 11.2 | 4.5 | 18.6 | 5.7 | 0.9 | 0.3 |
| - | - | 5223 | 2.0 | 0.2 | 4.5 | 0.3 | 0.2 | 0.04 |
| Total | 3.0 | 0.3 | 6.6 | 0.3 | 0.3 | 0.04 | ||
| II. Respondents with no past 12-month major depression or panic | ||||||||
| Lifetime | ||||||||
| Major depression | Panic disorder | |||||||
| + | + | 24 | 2.1 | 1.9 | 12.3 | 6.8 | 0.1 | 0.08 |
| + | - | 367 | 1.2 | 0.5 | 6.6 | 1.2 | 0.1 | 0.03 |
| - | + | 39 | 3.3 | 2.5 | 4.9 | 2.7 | 0.2 | 0.10 |
| - | - | 4793 | 2.0 | 0.2 | 4.4 | 0.3 | 0.2 | 0.04 |
Table 5 Comorbidity predictors of role impairment
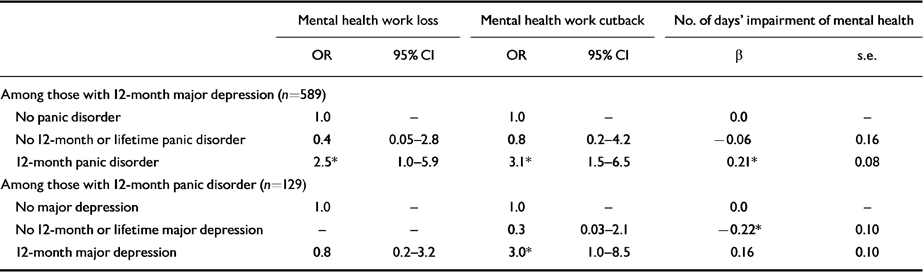
| Mental health work loss | Mental health work cutback | No. of days' impairment of mental health | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | β | s.e. | |
| Among those with 12-month major depression (n=589) | ||||||
| No panic disorder | 1.0 | - | 1.0 | - | 0.0 | - |
| No 12-month or lifetime panic disorder | 0.4 | 0.05-2.8 | 0.8 | 0.2-4.2 | -0.06 | 0.16 |
| 12-month panic disorder | 2.5* | 1.0-5.9 | 3.1* | 1.5-6.5 | 0.21* | 0.08 |
| Among those with 12-month panic disorder (n=129) | ||||||
| No major depression | 1.0 | - | 1.0 | - | 0.0 | - |
| No 12-month or lifetime major depression | - | - | 0.3 | 0.03-2.1 | -0.22* | 0.10 |
| 12-month major depression | 0.8 | 0.2-3.2 | 3.0* | 1.0-8.5 | 0.16 | 0.10 |
DISCUSSION
The patterns of comorbidity reported here are similar to those found not only in previous epidemiological samples but also in treatment samples, showing strong odds ratios, the presence of depression in the majority of people with panic and the occurrence of panic in a substantial minority of those with depression. In addition, our finding that episode comorbidity is stronger than lifetime comorbidity means that panic and depression covary over time, a result that has been documented previously in treatment samples (Reference Uhde, Boulenger and Roy-ByrneUhde et al, 1985). This finding is part of a larger pattern of NCS results, again consistent with previous research, that comorbid panic-depression is more severe and persistent than either pure panic or pure depression. Severity of symptoms (number of symptoms during both panic attacks and depressive episodes) was also greater in lifetime comorbid cases, showing a more distant association of comorbidity with episode severity than just the expected current comorbidity association. Similarly, patients with lifetime comorbidity were more impaired on various measures (professional help-seeking, perceived role impairment) than people with only one of the two disorders.
Comorbidity and suicide
The substantially higher prevalence of suicide attempts in comorbid cases of panic and depression compared with pure cases (25% in both v. 16% in depression v. 5.2% in panic) is noteworthy, and consistent with prior epidemiological analyses. As presented in Table 2, when additional diagnostic comorbidity was considered as a covariate, comorbidity was only associated with increased suicide attempt rates compared with panic alone (OR=4.2) and not major depression alone (OR=1.2). Furthermore, in additional analyses not reported in Table 2, we find that after adjusting for other comorbid disorders, respondents with panic alone but not major depression had no elevated risk of suicide attempts compared with people with neither panic nor depression (OR=1.7; 95% CI=0.8-3.6). Taken together, these results are consistent with the suggestion in previous research that the higher rates of suicide attempts among patients suffering from panic might be due to co-occurring diagnoses rather than to panic itself (Reference Friedman, Jones and ChernenFriedman et al, 1993; Reference Lepine, Chignon and leheraniLepine et al, 1993).
Comorbidity and service use
The association of comorbidity with increased service use is also consistent with previous clinical studies documenting greater treatment intensity in this group. Greater service use was evident throughout the medical, mental health and social service sectors when measured as the proportion of patients with use, but not when measured as the number of visits, owing to the large variance of the latter measure. This is consistent, however, with studies documenting a high use of medical services by patients with both mood and anxiety disorders. The disappearance of this finding when control for other diagnoses was introduced is at variance with our earlier finding (Table 2) that lifetime comorbidity was associated with increased professional help-seeking. However, these two measures of service use differed along two dimensions: time of use (just in the past year v. over the lifespan) and reason for use (any mental health treatment v. treatment of focal disorder). Nevertheless, the association between comorbidity and lifetime service use related to the focal disorder is important and noteworthy.
Comorbidity and role impairment
Finally, comorbidly ill patients had more work impairment, measured as reduced days per 100 workers, documenting the significant disability that is quite consistent with previous reports in both clinical and epidemiological samples. This association was, not surprisingly, confined to 12-month comorbidity and was not present when lifetime comorbidity alone was considered. This suggests that lifetime comorbidity is not simply a marker of some underlying propensity to be impaired when anxious or depressed. Instead, it is only important in predicting impairment when the comorbidity is active. If treatment can help an anxious (or depressed) person recover from their depression (or panic) and not have it come back, then the impairment associated with the panic (depression) will be no worse than that of a person who never had depression (panic).
Clinical Implications and Limitations
CLINICAL LIMITATIONS
-
▪ Panic disorder occurs together with major depression more often than any other anxiety disorder and clinicians should suspect panic in their depressed patients.
-
▪ Patients with co-occurring panic and depression have a more severe illness, with greater symptom severity, more persistent course and more impairment. Hence, treatment may be more difficult and clinicians must be creative and persistent in their interventions.
-
▪ The increased risk of suicide in depressed patients with panic attacks seen in previous clinical studies may be due to additional comorbidities such as personality disorder and substance abuse.
LIMITATIONS
-
▪ Lay-interviewer-obtained diagnoses may not be as accurate as clinician diagnoses, although previous studies show that the two are consistently related.
-
▪ The Composite International Diagnostic Interview is less valid in identifying bipolar depression, so the depressed group may be more heterogeneous.
-
▪ The cross-sectional nature of the interview compromises the accuracy of temporal ordering of appearance of disorders (primary/secondary distinction).
ACKNOWLEDGEMENTS
The National Comorbidity Survey (NCS) is a collaborative epidemiological investigation of the prevalences, causes and consequences of psychiatric morbidity and comorbidity in the USA, supported by the National Institute of Mental Health (R01 MH46376, R01 MH49098 and R01 MH52861) with supplemental support from the National Institute of Drug Abuse (through a supplement to MH46376) and the W. T. Grant Foundation (90135190), R.C.K., Principal Investigator. Peparation for this report was also supported by a Research Scientist Award to R.C.K. (K05 MH00507) and an unrestricted educational grant from SmithKline Beecham Pharmaceuticals. Collaborating NCS sites and investigators are: The Addiction Research Foundation (Robin Room), Duke University Medical Center (Dan Blazer, Marvin Swartz), Harvard Medical School (Richard Frank, Ronald Kessler), Johns Hopkins University (James Anthony, William Eaton, Philip Leaf), the Max Planck Institute of Psychiatry Clinical Institute (Hans-Ulrich Wittchen), the Medical College of Virginia (Kenneth Kendler), the University of Miami (R. Jay Turner), the University of Michigan (Lloyd Johnston, Roderick Little), New York University (Patrick Shrout), SUNY Stony Brook (Evelyn Bromet) and Washington University School of Medicine (Linda Cottler, Andrew Heath). A complete list of all NCS publications, along with abstracts, study documentation, interview schedules and the raw NCS public-use data files, can be obtained directly from the NCS Homepage by using the URL: http://www.umich.edu/~ncsum/










eLetters
No eLetters have been published for this article.