Older people with mental illness often have complex needs because of the frequent co-existence of disability, physical illness and social problems. Effective evaluation of long-term and multiple problems may be particularly difficult without standardised methods aimed at comprehensive and systematic assessment of needs. Although certain needs are postulated to be ‘universal’ in humans generally (Reference MaslowMaslow, 1954), different sections of the population will have additional, more specific types of need. For example, older people with dementia may have specific and unique needs related to their disabilities but their range of general needs is the same as everyone else's (Reference MurphyMurphy, 1992).
The Medical Research Council's topic review of health of the UK's elderly people (Medical Research Council, 1994) recommended that in future, “research in community care should be focused on areas of particular relevance to the changes in care within the community notably, needs based approaches”. Comprehensive needs assessment helps to highlight specific areas where health and social services can concentrate their energies in providing individually tailored, high-quality care. Until now there has been a lack of adequate measures for defining needs in older people with mental health problems. This paper describes the development of a new instrument intended to fill that gap comprehensively.
METHOD
Development
The Camberwell Assessment of Need for the Elderly (CANE) is based on the structural model of the Camberwell Assessment of Need (CAN) and had similar criteria set out for it before development was started (Reference Phelan, Slade and ThornicroftPhelan et al, 1995). These criteria were that it should have adequate psychometric properties, be valid and reliable, be completable within 30 minutes, be usable by a wide range of professionals, be easily learned and used without extensive training, be suitable for routine clinical practice and for research, and be applicable to a wide range of populations and settings. It should also measure both met and unmet needs, incorporate staff, patients' and carers' views of needs and have a section on the needs of carers. Lastly, it should measure levels of help received from informal carers as well as from statutory services.
The initial adaptation of the CAN was carried out by one of the authors (M.A.) and colleagues, and resulted in a draft version called the Camberwell Assessment of Need for Older Adults (CANOA), which covered 27 different areas - 25 regarding the service user and two specific to the carer (the original CAN has 22 topics, all related to the service user). The overall format of the CAN was preserved and a number of the topics covered were identical, although the format of questions was of necessity adapted to be more suitable for the target population. The process of adaptation took place in the context of focus groups consisting of service users (the target population) and professionals working in mental health services for the elderly. The CANOA was piloted on an inner-city sample of 70 elderly African-Caribbean people with various mental health problems. Following this, further adjustments were made to the draft.
Further development of draft version - the Delphi process
A modified Delphi process was the consensus method used in refining the instrument (Reference PillPill, 1971; Reference Rowe, Wright and BolgerRowe et al, 1991). After piloting, a questionnaire was sent to service users, carers and professionals, involved in all aspects of care of the elderly (psychiatrists, psychologists, geriatricians, nurses, social workers, representatives of voluntary groups and occupational therapists), asking them to rate the various topics on a five-point scale of importance and asking for suggestions on any other areas that they might consider important. Following the feedback from these questionnaires and subsequent focus groups (again with service users, carers and various professionals), a second draft version was prepared. This draft was the subject of a consensus conference aimed at further refinement of the CANE.
Consensus conference - continuing the Delphi process
Thirty-eight delegates attended the consensus conference representing most of the relevant professional and voluntary groups involved in care of the elderly (including representatives from the charities Age Concern and the Alzheimer's Disease Society, mental health service managers, psychiatrists, psychologists, general practitioners (GPs), social workers, nurses and occupational therapists). The delegates were allocated to different workshop groups (each group concentrating on specific topics in the draft version) and scrutinised the layout and wording in detail to make sure that all the most important areas were covered as far as possible. Each workshop group had a core of specialists in the topics that they covered (psychiatrists covering the aspects of psychiatric morbidity, GPs covering physical health issues, etc.) and each group fed back to the whole conference after each session. The results of these sessions were collated in order to prepare a penultimate draft version of the CANE, which was later circulated to the conference delegates for final opinions.
Pilot study
The penultimate draft was used to interview ten patients in an old age psychiatry day hospital, their key staff and carers. The final draft (CANE version 2) was prepared following these interviews; it involved only some minor changes in wording and item order in order to clarify some areas and to make it more user-friendly.
Table 1 compares the CAN and CANE. Overall, seven new items were created for the CANE (five relating to the service user and two relating to the carer). Two items from the CAN (‘education’ and ‘telephone’) were not used, while two (‘drugs’ and ‘transport’) were expanded (‘drugs’ to encompass problems with medication as well as possible drug misuse, while ‘transport’ became ‘mobility’ in the CANE so as to cover getting about inside and outside the home). The item ‘sexual expression’ from the CAN was subsumed under ‘intimate relationships’ in the CANE.
Table 1 A comparison of contents of the CAN and CANE. Items in bold are exclusive to either the CAN or the CANE. Items in italics have been expanded in the CANE compared with their counterparts in the CAN

| CAN | CANE |
|---|---|
| 1. Accommodation | 1. Accommodation |
| 2. Food | 2. Food |
| 3. Household skills | 3. Household skills |
| 4. Self-care | 4. Self-care |
| 5. Occupation | 5. Daytime activities |
| 6. Physical health | 6. Physical health |
| 7. Psychotic symptoms | 7. Psychotic symptoms |
| 8. Information about condition and treatment | 8. Information |
| 9. Psychological distress | 9. Psychological distress |
| 10. Safety to self | 10. Safety (deliberate self-harm) |
| 11. Safety (accidental self-harm) | |
| 12. Safety (abuse/neglect) | |
| 11. Safety to others | 13. Behaviour |
| 12. Alcohol | 14. Alcohol |
| 13. Drugs | 15. Drugs |
| 14. Company of others | 16. Company |
| 15. Intimate relationships | 17. Intimate relationships |
| 16. Sexual expression | |
| 17. Child care | 18. Caring for someone else |
| 18. Transport | 19. Mobility/transport |
| 19. Money | 20. Money |
| 20. Welfare benefits | 21. Benefits |
| 21. Basic education | |
| 22. Telephone | |
| 22. Memory | |
| 23. Eyesight/hearing | |
| 24. Continence | |
| Two items for carers | |
| (a) Carer's need for information | |
| (b) Carer's psychological distress |
Data collection
Copies of the final draft and of some other rating scales (see below) and pro formas used for gathering demographic details were sent to three centres in the UK (North Wales, Liverpool and Southport), one in Sweden (Jönköping) and one in the USA (Lebanon, PA). The other scales, aimed at helping further in the validation process, were the 12-item General Health Questionnaire (GHQ-12; Reference GoldbergGolberg, 1978) (used as a measure of carer stress); the Barthel Activities of Daily Living Index (Reference Wade and CollinWade & Collin, 1988) (used as a measure of functional ability); the Medical Outcomes Study (MOS) 36-item Short-Form Health Survey (SF-36; Reference Ware and SherbourneWare & Sherbourne, 1992; Reference McHorney, Ware and RaczekMcHorney et al, 1993) (used as a quality-of-life instrument); and the behaviour rating scale from the Clifton Assessment Procedures for the Elderly (CAPE-BRS; Reference Gilleard and PattieGilleard & Pattie, 1979) (used as a measure of dependency). All of these scales were used as comparative measures in order to help establish criterion and concurrent validity.
Reliability data
Data were collected on 55 cases for the interrater and test-retest reliability analysis. These data were collected by one of the authors (T.R.) and four co-workers (two nurses and two psychiatrists) in a variety of settings in a psychiatry of the elderly service covering urban and rural settings in Hertfordshire and Essex (out-patients departments, day hospitals, acute psychiatric wards, continuing care and dementia assessment wards). Initially, 41 service users, 53 staff members and 22 carers were interviewed in the presence of one of the four co-raters; one week later (on average), 40 service users, 53 staff and 18 carers were re-interviewed by T.R. Prior power analysis had indicated that with power set at 0.9 and significance level set at 0.05 we would need a sample size of about 46 to demonstrate that a reliability (κ) of 0.4 or above was different from zero.
Table 2 shows details of the study sample. Service users, staff and carers were interviewed separately, with the interviewer and observer both rating responses. The interviewer and observer switched roles with alternate cases in order to minimise interviewer bias. Fourteen (25%) of the service users could not be interviewed - 12 had moderate to severe dementia, one had chronic schizophrenia with clinical symptoms that precluded interview (severe negative syndrome) and one had depression.
Table 2 Demographic details of subjects in the reliability study

| Variable | |
|---|---|
| Mean age (years) | 75.4 (s.d.=8.15, range 59-97)1 |
| Gender (n(%)) | |
| Female | 29 (53%) |
| Male | 26 (47%) |
| Marital status (n(%)) | |
| Single | 4 (7%) |
| Married | 21 (38%) |
| Divorce/separated | 5 (9%) |
| Widowed | 25 (46%) |
| Living situation (n(%)) | |
| Alone | 25 (45%) |
| With partner | 21 (38%) |
| With others | 9 (17%) |
| Geographical area (n(%)) | |
| Urban | 52 (95%) |
| Rural | 3 (5%) |
| Service contact (n(%)) | |
| 0-5 years' duration | 35 (64%) |
| 6-20 years' duration | 7 (14%) |
| > 20 years' duration | 13 (22%) |
| Mean number of previous admissions | 2.5 (s.d.=4.76, range 0-25) |
| Mean length of service contact (years) | 11.5 (s.d.=14.5, range 1-50) |
| Status at interview (n(%)) | |
| Day patient | 31 (56%) |
| In-patient | 24 (44%) |
| Diagnosis (n(%)) | |
| Dementia | 19 (34%) |
| Depression | 18 (33%) |
| Bipolar affective disorder | 7 (13%) |
| Schizophrenia | 4 (7%) |
| Anxiety disorder | 3 (5%) |
| Other | 4 (7%) |
| Has a carer? (n(%)) | 37 (67%) |
| Is a carer? (n(%)) | 2 (4%) |
Staff came from a variety of professional backgrounds - occupational therapy, social work, psychiatry and (mainly) psychiatric nursing. Two-thirds (n=37) of service users had an informal carer, of whom 60% (n=22) were interviewed. Carers in all cases were spouses, partners or family members.
Validity data
The validity data included those from the reliability sample plus records collected in the other five centres (14 from Southport, 12 from Liverpool, 10 from North Wales, 6 from Sweden and 4 from the USA), making a total of 101 cases. Much of the validity was assessed concurrently with the development process.
Analysis
Data for the validity and reliability studies were analysed using the Statistical Package for the Social Sciences, version 6.0 for Windows (SPSS, 1993). Cohen's κ coefficient (Reference CohenCohen, 1960) and percentage complete agreement were calculated in order to assess the degree of agreement between binary variables, and intraclass correlations, based on analysis of components of variance, were used to compute interrater and test-retest reliability of summary scores. Confidence intervals (95%) were calculated for mean values and for the main reliability coefficients.
Each item in the research version of the CANE has four sections (a structure similar to the research version of the CAN). Section 1 asks whether a need exists, sections 2 and 3 rate the level of help received from family/friends and statutory services, respectively, and section 4 rates whether the right amount and type of help are given. If no need exists, sections 2-4 are not completed. The measurements of agreement in this study are based on section 1.
RESULTS
The mean total numbers of needs identified by staff, patients and carers, calculated from all 101 cases, were respectively, 8.65 (95% CI 7.85-9.45), 6.55 (95% CI 5.75-7.35) and 8.77 (95% CI 7.53-10.00). While carers and staff rated approximately the same number of needs, patients rated 25% fewer needs than carers. It is important to note that similar numbers of needs identified do not mean that the same needs were identified.
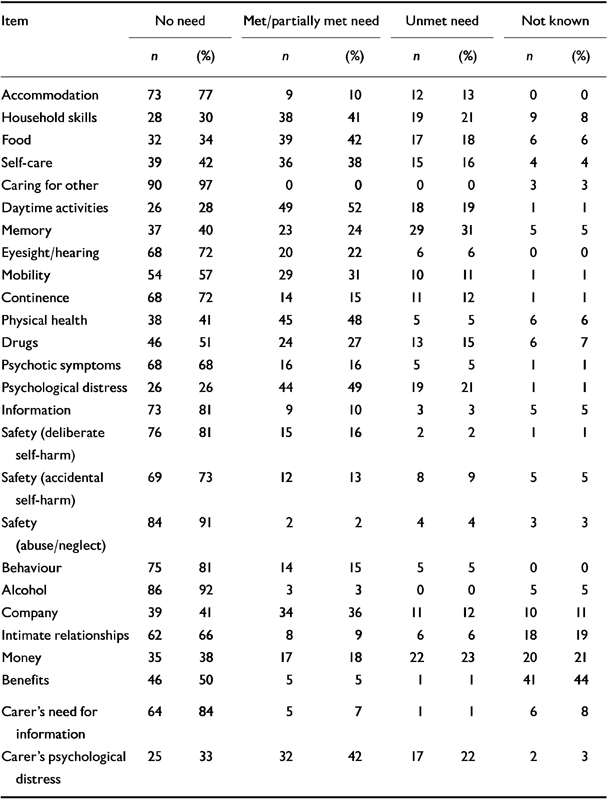
The number of needs rated by staff for each item of the CANE in the total sample is shown in Table 3, which shows that staff felt that approximately a fifth of patients had serious unmet needs relating to household skills, food, daytime activities and psychological distress; almost a third had serious unmet needs concerning memory (reflecting the numbers with dementia); almost a quarter had serious unmet needs with money; and over a fifth of carers were also rated as suffering from significant psychological distress. Staff were able to rate needs for most items, but approximately a fifth did not know whether there were any needs with money and intimate relationships, and over two-fifths did not know whether their clients were receiving the appropriate state benefits. Half of the sample was receiving some help with daytime activities, physical health and psychological distress, and two-fifths with food. Over two-fifths of carers were receiving help with psychological distress. The serious unmet needs least often identified in the patient sample were in the areas of benefits (1%, but skewed by the number of unknowns), deliberate self-harm (2%), information (3%), abuse/neglect (4%) and behaviour (5%). None of the sample was regarded as having a serious unmet need with alcohol, but 3% were receiving some help for alcohol misuse. Only one of the sample of carers (n=65) was rated as having a serious unmet need for information.
Table 3 Levels of need as rated by staff
| Item | No need | Met/partially met need | Unmet need | Not known | ||||
|---|---|---|---|---|---|---|---|---|
| n | (%) | n | (%) | n | (%) | n | (%) | |
| Accommodation | 73 | 77 | 9 | 10 | 12 | 13 | 0 | 0 |
| Household skills | 28 | 30 | 38 | 41 | 19 | 21 | 9 | 8 |
| Food | 32 | 34 | 39 | 42 | 17 | 18 | 6 | 6 |
| Self-care | 39 | 42 | 36 | 38 | 15 | 16 | 4 | 4 |
| Caring for other | 90 | 97 | 0 | 0 | 0 | 0 | 3 | 3 |
| Daytime activities | 26 | 28 | 49 | 52 | 18 | 19 | 1 | 1 |
| Memory | 37 | 40 | 23 | 24 | 29 | 31 | 5 | 5 |
| Eyesight/hearing | 68 | 72 | 20 | 22 | 6 | 6 | 0 | 0 |
| Mobility | 54 | 57 | 29 | 31 | 10 | 11 | 1 | 1 |
| Continence | 68 | 72 | 14 | 15 | 11 | 12 | 1 | 1 |
| Physical health | 38 | 41 | 45 | 48 | 5 | 5 | 6 | 6 |
| Drugs | 46 | 51 | 24 | 27 | 13 | 15 | 6 | 7 |
| Psychotic symptoms | 68 | 68 | 16 | 16 | 5 | 5 | 1 | 1 |
| Psychological distress | 26 | 26 | 44 | 49 | 19 | 21 | 1 | 1 |
| Information | 73 | 81 | 9 | 10 | 3 | 3 | 5 | 5 |
| Safety (deliberate self-harm) | 76 | 81 | 15 | 16 | 2 | 2 | 1 | 1 |
| Safety (accidental self-harm) | 69 | 73 | 12 | 13 | 8 | 9 | 5 | 5 |
| Safety (abuse/neglect) | 84 | 91 | 2 | 2 | 4 | 4 | 3 | 3 |
| Behaviour | 75 | 81 | 14 | 15 | 5 | 5 | 0 | 0 |
| Alcohol | 86 | 92 | 3 | 3 | 0 | 0 | 5 | 5 |
| Company | 39 | 41 | 34 | 36 | 11 | 12 | 10 | 11 |
| Intimate relationships | 62 | 66 | 8 | 9 | 6 | 6 | 18 | 19 |
| Money | 35 | 38 | 17 | 18 | 22 | 23 | 20 | 21 |
| Benefits | 46 | 50 | 5 | 5 | 1 | 1 | 41 | 44 |
| Carer's need for information | 64 | 84 | 5 | 7 | 1 | 1 | 6 | 8 |
| Carer's psychological distress | 25 | 33 | 32 | 42 | 17 | 22 | 2 | 3 |
All reliability interviews were timed; mean times for patient, staff and carer interviews were 23.5 minutes (range 9-60), 12.5 minutes (range 3-28) and 23.5 minutes (range 5-45), respectively.
Validity
Face validity
The extensive development process entailed rigorous scrutiny by a large number of experts, clinicians, carers and service users in the UK and other countries. The overall consensus was that the CANE covers the main areas of need for the target population. The choice of words and word length are suitable for most readers. The Flesch reading ease score (71.8) and average word length (4.4 characters) indicate that most readers could comprehend the vocabulary. We therefore conclude that the CANE has good face validity.
Content validity
The 26 items of the CANE were drawn from a survey of currently available assessment tools and the expert discussions held during the validation process. Using the questionnaire mentioned above, a survey of patients (n=35), carers (n=30), professionals and representatives of voluntary organisations (n=55) was carried out. The average scoring showed that all items were rated as at least moderately important (a rating of three on a five-point scale), precluding item bias. No additional areas of need were suggested by more than two respondents. Content (or sampling) validity is therefore shown to be good.
Consensual validity
The overall consensus from the surveys, focus groups and conference was that there was a definite requirement for a needs-assessment instrument for elderly people with mental illness and that the CANE would certainly help to fulfil that requirement comprehensively. Although some of the original CAN items such as ‘telephone’, ‘basic education’ and ‘sexual expression’ were felt to be potentially important areas to assess in the elderly age group, the consensus was that their inclusion was not essential in the CANE (on the grounds that we were trying to cover the most important areas of need rather than all possible areas), but space could be included in the final documents for research and clinical use so that raters could add these or other topics in order to ‘customise’ their own data-gathering.
Construct validity
Both convergent and divergent construct validity were assessed by creating a correlation matrix for the first section of all 26 items as rated by patients, staff and carers and examining whether there were positive or negative correlations between items where one would intuitively expect to find such correlations (‘convergent’) or whether there was a lack of any correlation where it is obvious that no relationship should exist (‘divergent’). Evidence of convergent construct validity is particularly shown in correlation measures between memory and those functions that one would expect to be impaired with cognitive impairment (Table 4) - in the staff domain the correlation between memory and self-care is 0.43 (P < 0.001), that for memory and accidental self-harm is 0.39 (P < 0.001), that for memory and money is 0.41 (P < 0.001), and that for self-care and household skills is 0.7 (P < 0.001). Similarly, there are good correlations for these items in the carer domain. However, there are poor correlations between these items in the patient domain, presumably because of poor recognition of functional disability among the cognitively impaired group in the sample. Divergent validity is shown by the lack of any significant correlations between items such as carer's and patient's need for information and all other items. Overall, the correlation coefficients indicate reasonable construct validity.
Table 4 Correlation coefficients illustrating aspects of construct validity

| Item pairs | r | ||
|---|---|---|---|
| Carer | Staff | Patient | |
| Memory/self-care | 0.54 | 0.43 | 0.05 |
| Memory/money | 0.50 | 0.41 | 0.07 |
| Memory/accidental self-harm | 0.44 | 0.40 | 0.22 |
| Memory/carer's psychological distress | 0.22 | 0.40 | 0.15 |
| Memory/household skills | 0.43 | 0.24 | 0.05 |
| Self-care/household skills | 0.60 | 0.70 | 0.50* |
Criterion validity
As there was no contemporary scale specific to needs of elderly people with mental illness, there is some difficulty in establishing concurrent validity. However, as mentioned above, we used four other scales to act as comparisons: the CAPE-BRS to rate dependency and behavioural function; SF-36 as a quality-of-life measurement, the Barthel Index as a measure of physical functional status; and the GHQ-12 for measuring carer stress. Analysis yielded the correlation coefficients shown in Table 5. There is strong correlation between specific CANE items and corresponding items of the CAPE-BRS. Similarly, the CANE total score (the sum of met and unmet needs) correlates strongly with the total CAPE-BRS score (r=0.66) and has a strong negative correlation with the Barthel score (r=-0.53). There is also a strong correlation between the carer-item ‘carer's psychological distress’ and the GHQ-12 score (r=0.6). When comparing with the SF-36, negative correlations would be expected. Interestingly, there are weak negative correlations generally between staff-rated CANE scores and the (patient-rated) SF-36 scores, except between the CANE item ‘distress’ and the SF-36 general health perception sub-scale (r=-0.46). On the other hand, there are significant negative correlations between patient-rated CANE items and sub-scales and corresponding SF-36 scores (Table 5). These results suggest reasonable criterion validity.
Table 5 Criterion validity — correlations between CANE items and established scales

| CANE item | Item from other scale | Correlation (r) |
|---|---|---|
| Self-care | CAPE 1 (bathing/dressing) | 0.72 |
| Self-care | CAPE 6 (appearance) | 0.66 |
| Memory | CAPE 5 (confused) | 0.81 |
| Mobility | CAPE 2 (walking) | 0.75 |
| Continence | CAPE 3 (incontinence) | 0.85 |
| Eyesight/hearing | CAPE items (eyesight/hearing) | 0.53-0.63 |
| Total (met+unmet needs) | CAPE total | 0.66 |
| Total | Total Barthel score | -0.53 |
| Total | SF-36 total score | -0.24* |
| Total unmet needs1 | SF-36 total score | -0.38 |
| Distress1 | SF-36 mental health sub-score | -0.6 |
| Distress | SF-36 general health perception sub-score | -0.46 |
| Carer's psychological distress2 | GHQ-12 | 0.6 |
Reliability
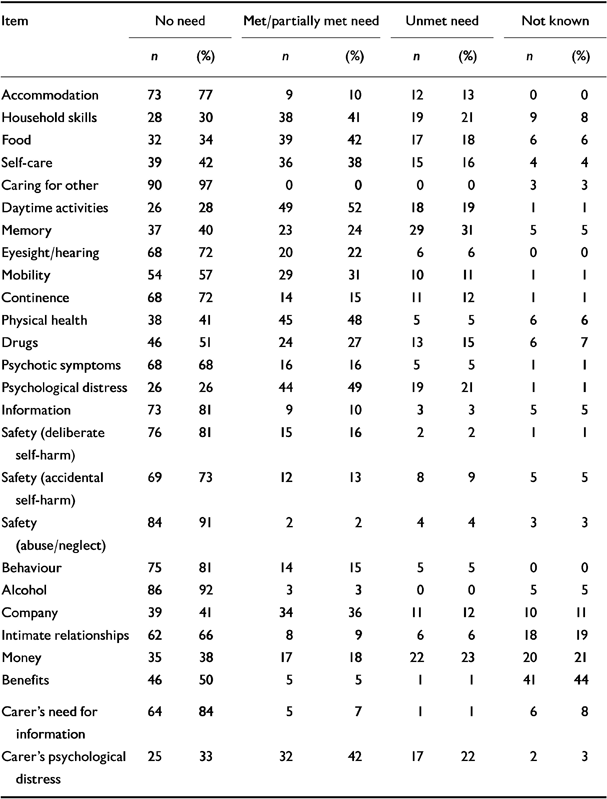
Interrater and test-retest reliability were assessed by calculating percentage complete agreement and κ coefficients for the first section of the CANE (level of need present) for each item in patient, staff and carer ratings. According to Fleiss (Reference Fleiss and Fleiss1981), a κ value of less than 0.40 indicates poor agreement, values of 0.40-0.59 show fair agreement, values of 0.60-0.74 show good agreement and values of 0.75-1.00 show excellent agreement. The values of κ for interrater reliability in patient, staff and carer domains are therefore generally excellent with all but one reaching 0.75 or above (Table 6). In the interrater staff interviews the mean value of κ is 0.97 (range 0.87-1.00). Overall, ratings of κ for test-retest reliability (Table 7) are lower than for interrater reliability, but in general they appear adequate, with a mean of 0.77 (range 0.35-1.00) in the staff domain. Agreement on retesting for 58% of items in this domain was excellent (κ < 0.75), while for 31% of items it was good (0.60-0.74). In the patient domain, on retesting, agreement for 27% of items was excellent, 35% good, 8% fair and 15% poor; agreement for the remaining 15% was impossible to calculate because of very low base rates in the binary characteristics. In the carer domain, κ showed excellent agreement on retesting in 58% of items, good agreement in 12% and fair agreement in 12%; it could not be calculated for the remaining five items. Intraclass correlations between summary scores, based on analysis of components of variance, showed a correlation coefficient of 0.99 (95% CI 0.99-1.00) for interrater reliability for patient, staff and carer ratings. Calculations for test-retest reliability yielded correlations of 0.87 (95% CI 0.78-0.92), 0.93 (95% CI 0.90-0.96) and 0.97 (95% CI 0.93-0.98) for patient, staff and carer ratings, respectively.
Table 6 Interrater reliability: percentage agreement and κ scores

| Item | Patients (n=41) | Staff (n=53) | Carers (n=23) | |||
|---|---|---|---|---|---|---|
| % complete agreement | κ | % complete agreement | κ | % complete agreement | κ | |
| Accommodation | 100 | 1 | 100 | 1 | 100 | 1 |
| Household skills | 97.6 | 0.95 | 97.7 | 0.97 | 100 | 1 |
| Food | 97.5 | 0.95 | 95.7 | 0.93 | 100 | 1 |
| Self-care | 100 | 1 | 98 | 0.97 | 95.7 | 0.93 |
| Caring for someone else | 100 | 1 | 100 | 1 | 100 | 1 |
| Daytime activities | 95.1 | 0.91 | 100 | 1 | 95.5 | 0.93 |
| Memory | 92.7 | 0.87 | 93.9 | 0.91 | 100 | 1 |
| Eyesight/hearing | 100 | 1 | 100 | 1 | 100 | 1 |
| Mobility | 97.6 | 0.96 | 98.1 | 0.97 | 90.9 | 0.85 |
| Continence | 100 | 1 | 100 | 1 | 95.2 | 0.85 |
| Physical health | 97.9 | 0.95 | 97.9 | 0.95 | 100 | 1 |
| Drugs | 100 | 1 | 91.7 | 0.87 | 95.5 | 0.91 |
| Psychotic symptoms | 100 | 1 | 100 | 1 | 100 | 1 |
| Psychological distress | 97.6 | 0.96 | 98.1 | 0.97 | 100 | 1 |
| Information | 91.7 | 0.79 | 100 | 1 | 100 | 1 |
| Safety (deliberate self-harm) | 97.5 | 0.91 | 100 | 1 | 100 | 1 |
| Safety (accidental self-harm) | 100 | 1 | 100 | 1 | 100 | 1 |
| Safety (abuse/neglect) | 100 | 1 | 98 | 0.87 | 100 | 1 |
| Behaviour | 100 | 1 | 100 | 1 | 100 | 1 |
| Alcohol | 100 | 1 | 100 | 1 | — | — |
| Company | 95 | 0.90 | 100 | 1 | 85 | 0.75 |
| Intimate relationships | 100 | 1 | 97.3 | 0.92 | — | — |
| Money | 95 | 0.91 | 91.7 | 0.87 | 76.2 | 0.60 |
| Benefits | 100 | 1 | — | — | — | — |
| Carer's need for information | — | — | 100 | 1 | 100 | 1 |
| Carer's psychological distress | 95.7 | 0.84 | 100 | 1 | 90.9 | 0.86 |
Table 7 Test—retest reliability: percentage agreement and κ scores

| Item | Patients (n=40) | Staff (n=52) | Carers (n=17) | |||
|---|---|---|---|---|---|---|
| % complete agreement | κ | % complete agreement | κ | % complete agreement | κ | |
| Accommodation | 92.5 | 0.54 | 96.2 | 0.91 | 88.9 | 0.71 |
| Household skills | 87.5 | 0.75 | 93 | 0.89 | 94.1 | 0.86 |
| Food | 87.2 | 0.73 | 91.5 | 0.86 | 100 | 1 |
| Self-care | 85 | 0.68 | 89.8 | 0.84 | 88.9 | 0.79 |
| Caring for someone else | — | — | 100 | 1 | 100 | 1 |
| Daytime activities | 67.5 | 0.38 | 79.2 | 0.64 | 78.2 | 0.53 |
| Memory | 87.5 | 0.76 | 83.7 | 0.75 | 77.8 | 0.65 |
| Eyesight/hearing | 87.5 | 0.68 | 94.3 | 0.86 | 94.1 | 0.88 |
| Mobility | 82.5 | 0.68 | 84.6 | 0.70 | 66.7 | 0.44 |
| Continence | 89.7 | 0.62 | 96.2 | 0.91 | 94.1 | 0.81 |
| Physical health | 92.3 | 0.84 | 88.9 | 0.75 | 94.4 | 0.87 |
| Drugs | 76.3 | 0.58 | 87.2 | 0.8 | 100 | 1 |
| Psychotic symptoms | — | — | 94.1 | 0.80 | 100 | 1 |
| Psychological distress | 85 | 0.76 | 69.2 | 0.51 | 77.8 | 0.60 |
| Information | 74.3 | 0.29 | 95.3 | 0.72 | 100 | 1 |
| Safety (deliberate self-harm) | 92.3 | 0.64 | 84.3 | 0.35 | 94.4 | 0.77 |
| Safety (accidental self-harm) | 95 | 0.03 | 90 | 0.65 | — | — |
| Safety (abuse/neglect) | 100 | 1 | 98 | 0.85 | 100 | 1 |
| Behaviour | — | — | 90.6 | 0.68 | — | — |
| Alcohol | 100 | 1 | 100 | 1 | — | — |
| Company | 78.9 | 0.61 | 78 | 0.62 | 81.3 | 0.59 |
| Intimate relationships | 97.4 | 0.89 | 97.3 | 0.9 | — | — |
| Money | 78.9 | 0.63 | 93.3 | 0.90 | 88.2 | 0.80 |
| Benefits | 87.6 | 0.07 | — | — | — | — |
| Carer's need for information | — | — | — | — | 100 | 1 |
| Carer's psychological distress | 80 | 0.41 | 73.7 | 0.57 | 88.9 | 0.82 |
DISCUSSION
The complex issue of mental health needs and their assessment has been the subject of a broad spectrum of opinion and varied research approaches in the UK, particularly since the introduction of legislation (National Health Service and Community Care Act 1990) aimed at generating more coordinated and comprehensive service provision by social services and the National Health Service. Mental ill-health is commonly associated with social adversity - both as a contributory factor and as a consequence - and this underpins the inclusion of items covering social care in assessment instruments designed to measure needs in those with mental illness.
The MRC Needs for Care Assessment (Reference Brewin, Wing and MangenBrewin et al, 1987) was designed to measure the needs of people with long-term mental illness, where need was deemed to be present if a patient's level of functioning fell below, or threatened to fall below, some minimum specified level and if a potentially effective remedy existed. Although a number of studies suggest that the scale has good reliability if used by trained investigators (Reference Brewin and WingBrewin & Wing, 1993), some problems were highlighted when it was used in hostels for the homeless (Reference Hogg and MarshallHogg & Marshall, 1992) and when used for long-term in-patients (Reference Pryce, Griffiths and GentryPryce et al, 1993). Hogg & Marshall (Reference Hogg and Marshall1992) concluded that their data were difficult to interpret because of a failure to take account of patients' and carers' views “in sufficient detail”; they therefore went on to develop a suitably modified version (Reference Marshall, Hogg and GathMarshall et al, 1995).
The CAN (Reference Phelan, Slade and ThornicroftPhelan et al, 1995) was developed to measure the needs of people in the general adult population with severe mental illness, and has been shown to have good reliability and validity. Studies comparing the assessments made by staff and patients showed that the two groups tended to rate similar numbers of needs (but different ones), agreeing moderately on met needs but less often on unmet needs (Slade et al, Reference Slade, Phelan and Thornicroft1996, Reference Slade, Phelan and Thornicroft1998).
Elderly patients may also have perceptions of their needs that differ from those of clinicians (Reference McEwanMcEwan, 1992), but standardised needs assessment in elderly people with mental illness has been largely neglected until now (Hamid et al, Reference Hamid, Howard and Silverman1995, Reference Hamid, Holloway and Silverman1998). There has been some literature looking at population needs (Reference VictorVictor, 1991; Reference Cooper, Jacoby and OppenheimerCooper, 1993), but specific attempts to address assessment of need have concentrated on people with dementia (Reference Aronson, Cox and GuastadisegniAronson et al, 1992; Reference Wattis, Hobson and BarkerWattis et al, 1992; Reference Gordon, Spicker and BallingerGordon et al, 1997; Reference McWalter, Toner and McWalterMcWalter et al, 1998), just as the CAN is aimed at those with severe mental illness.
Gordon et al (Reference Gordon, Spicker and Ballinger1997) designed the Tayside Profile for Dementia Planning, an instrument aimed at gathering data for population needs assessment and service planning for people with dementia. They found that it had satisfactory validity and reliability but noted that informal carers and professionals perceived needs differently. As it was not clear which group had the more valid opinion, a mix of informal carers and professionals as informants is postulated to offer the best approach when using the profile.
The Care Needs Assessment Pack for Dementia (Reference McWalter, Toner and McWalterMcWalter et al, 1998) was designed to allow multi-disciplinary teams to rate the met and unmet needs of people with dementia and their carers in the community and related settings (e.g. day hospitals). It does not differentiate between information sources (such as interviews with the person with dementia, the carer or others involved, and information from case notes) but allows discrepancies or differences of opinion to be recorded at the rater's discretion for each of the seven sub-scales of need (health and mobility, self-care and toileting, social interaction, thinking and memory, behaviour and mental state, house-care, community living). The section specific to the carer allows assessment of need over six domains - health, daily difficulties, support, breaks from caring, feelings and information. Preliminary research suggests that the instrument has a degree of validity and resonable reliability.
By contrast, the CANE is designed for the whole elderly population with mental illness (not just those with dementia or severe mental illness). As it allows patients, their carers and staff to rate their own opinions on need, it automatically records differences in perceptions of need at the key interface. This sort of data not only will help at the ‘micro’ level in the formulation of highly specific individual care planning but can also be used on the ‘macro’ level to plan health service provision based on the identified needs.
Psychometric properties
According to the criteria outlined at the beginning of the study, the CANE performs well. The initial development and piloting involved working with a sample of innercity Black Caribbean elderly people, whereas subsequent development and the main reliability study involved a sample population from rural and urban areas in Essex. This broad sample was further enhanced in the main validity work by collaboration with other centres in England, Wales, Sweden and the USA. It was therefore a varied group in terms of both sample and opinion. We also used a variety of consensus methods in the initial development and, as there is no agreement about which consensus methods are most appropriate (Reference Jones, Hunter, Mays and PopeJones & Hunter, 1996), it is hoped that the multiple methods lead to greater validity of the instrument. Raters came from backgrounds in nursing, social work, psychology and psychiatry, demonstrating the CANE's usability by a wide range of professionals. All raters were able to use the instrument after consulting the brief instruction document, occasionally supplemented by short discussions via telephone and the internet. Staff who were interviewed commented consistently on the usefulness of the CANE in honing their own assessment skills. The inclusion of a section specifically looking at the needs of carers was a universally popular idea during development. Providing carers with the opportunity to give their opinions on the patients' needs was also universally appreciated, particularly by carers of people with dementia, for whom the process often proved cathartic. The good correlation between the CANE item ‘carer's psychological distress’ and the GHQ-12 should further enhance the instrument's usefulness.
The staff ratings in the CANE were easily completed in under 30 minutes (mean 12.5 minutes), meeting the time criterion. However, as it is a slightly longer instrument than the CAN and also has an additional section for carers, the process of completing staff, patient and carer ratings in full would clearly take considerably longer. The version of the CANE proposed for clinical practice is a much shorter instrument. A follow-up paper to this one (details available from the first author upon request) will detail the relationship between staff, patient and carer views of needs.
Test-retest κ coefficients for the item ‘psychological distress’ were modest in all domains, despite relatively good percentage agreements. This may be due to a skew in the distributions of the ratings, low numbers of actual needs or changing needs over time between the two ratings. In particular, the test-retest value of κ was low for the item ‘deliberate self-harm’, an area where one would clinically expect to see change in a short time frame. Further work needs to be done to assess whether this means that the CANE has a degree of sensitivity that makes measurements of change in needs possible over a short interval of time.
Other items
There were various arguments for and against the inclusion of certain items from the CAN that were not, in the end, included in the CANE. Of these items, ‘telephone’ is worth further consideration, as deterioration in ability to use the telephone is one of four domains of instrumental activities of daily living significantly associated with cognitive impairment, and is therefore a potentially useful screening item (Reference Eccles, Clarke and LivingstoneEccles et al, 1998). The other three domains (managing medication, using transportation and managing a budget) are covered in the CANE. A possible option would be to include ‘telephone’ as an additional prompt in the item ‘household skills’ when the CANE is being used to assess the needs of those with suspected cognitive impairment. This may lead to a greater correlation between ‘memory’ and ‘household skills’ as a construct validity measurement (Table 4).
Limitations
Interrater reliability as measured by intraclass correlations between summary scores is almost perfect. This means that raters were rating almost exactly the same numbers of needs - usually, although not always, the same ones. In fact, the κ scores for individual interrater items are also generally very high. This finding is likely to reflect a natural bias in the method of data collection for this part of the study. Raters were not blind, and the layout structure of the instrument means that the interviewer does not ask any subsequent questions if he or she decides to rate at zero (‘no need exists’) each item in Section 1. This provides a cue to the co-rater, which potentially biases the ratings. A study using only the first section would help to prevent this occurrence, although there would still be some lack of independence as only one rater asks the questions.
Although the carer data for test-retest reliability are limited by the small sample size (n=18), the intraclass correlation, as measured by components of variance analysis, takes account of the whole carer sample (n=65) in the estimation of between-patient variance. Although not making up for the limited size of this part of the sample, this does add some credibility to the test-retest results for the carers. It should also be noted that although the confidence intervals reflect the influence of small sample size on precision, they do not reflect the upward bias in interrater reliability estimates caused by lack of independence. However, further testing in this area would be warranted before making any definitive statements.
Reliability, validity and use of the CANE
The results of this study indicate that the CANE is popular and easy to use, and overall has good validity. Intraclass correlations also demonstrate very good reliability. Although these correlations apparently demonstrate almost perfect interrater reliability, the interpretation of this part of the study has to be guarded in light of the limitations discussed. However, test-retest reliability as measured by intraclass correlations of summary scores is generally excellent, and this part of the reliability study did not have the same potential limitations.
Interest in the CANE has resulted in its translation into five other European languages (Swedish, Spanish, German, French and Portuguese), and it is currently being used in several centres in the UK and Europe for research studies or clinical work. With experience, completion of the CANE took much less time. The time taken to complete the assessment would be further improved in clinical settings where the patient is well known or where the CANE is used as part of the standard assessment procedure. As mentioned above, it is envisaged that the clinical version will be a much shorter instrument, incorporating only the first section for each item. The final versions for general use will be published in a single pack that includes an instruction manual containing case vignettes and scoring examples.
Further work needs to be done to supplement this study and assess the qualities of the instrument in more detail, but it can be said at this stage that the CANE is able to assess the needs of elderly people with mental illness effectively and comprehensively over a wide range of diagnoses and settings. Our hope is that it will contribute positively to delivering better-quality mental health services to the elderly.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The Camberwell Assessment of Need for the Elderly (CANE) comprehensively measures met and unmet needs across the full spectrum of mental illness in the elderly population.
-
▪ Assessments can easily be carried out by any member of a multi-disciplinary team without formal training.
-
▪ The CANE provides individual clinical needs assessment and the possibility of identifying gaps or shortcomings in service provision.
LIMITATIONS
-
▪ The page layout for each item in the research version of the CANE results in an inherent bias during interrater reliability assessments.
-
▪ The sample size was small for the carer group in the reliability study.
-
▪ By comparison with the validity sample, the reliability sample was not ethnically diverse.
ACKNOWLEDGEMENTS
We thank all participants, patients, staff and carers in this study in the UK and abroad. We are particularly grateful for the enthusiasm, helpful comments and data collection of the raters in the various centres. Howard Cattell and Jan Srinivasen in North Wales; Bo Ericson in Sweden; Scott Shreve and Ron Jones in the USA; Iris Guilman, Helen Mangan and colleagues in Liverpool; Marie Mayson, Chris Aspinall and colleagues in Southport; Okunle Ashaye, Marianne Collarbone and Barbara Richardson in Essex. We are also much indebted to the health professionals and representatives of Age Concern and the Alzheimer's Disease Society who helped us with their comments and participation in the consensus conference. Dr Graham Dunn kindly gave initial advice on the power analysis. This study was funded by a grant from the North Thames National Health Service Executive.










eLetters
No eLetters have been published for this article.