Over 30 case-control comparisons of the incidence of obstetric complications in people with schizophrenia and normal controls have been published in the past 20 years, and these have convinced many investigators not only that the incidence of obstetric complications is raised in schizophrenia, but also that they contribute to the aetiology of the syndrome. So far as we are aware, however, there has been no comparison of a substantial population of affective psychoses with normal controls based on obstetric information recorded at the time of birth. Lewis & Murray (Reference Lewis and Murray1987) studied large groups of patients with bipolar disorders and unipolar depression, but their obstetric information was derived from the routine case notes of adult psychiatric patients. Verdoux & Bourgeois (Reference Verdoux and Bourgeois1993) studied 23 patients with bipolar disorder and 23 normal controls, but their obstetric information was obtained retrospectively (by a non-blind interviewer) from the subjects' mothers. Rifkin et al (Reference Rifkin, Lewis and Jones1994) compared 100 patients with schizophrenia and 67 with affective psychoses, but their information was also obtained retrospectively from the mothers and they had no normal controls. Done et al (Reference Done, Johnstone and Frith1991) and Buka et al (Reference Buka, Tsuang and Lipsitt1993) both studied large birth cohorts for whom extensive obstetric information had been recorded at the time and both identified which members of these birth cohorts had developed affective as well as schizophrenic illnesses in early adult life. However, their numbers of subjects with psychoses were small and neither obtained convincing evidence that the incidence of obstetric complications was raised in either schizophrenia or affective disorders, although Done et al (Reference Done, Johnstone and Frith1991) did find a significantly reduced duration of pregnancy in their 32 subjects with affective psychoses. Our study was planned against this background. We also assumed that it was established that the incidence of obstetric complications was raised in schizophrenia, and likely that some of these complications contributed to the aetiology of schizophrenia. We wanted, therefore, to find out whether the aetiological role of intrauterine or perinatal trauma was specific to schizophrenia or whether it contributed to the genesis of affective psychoses as well.
METHOD
Basic design
The study was carried out alongside the study of obstetric complications and schizophrenia described by Kendell et al (Reference Kendell, McInneny and Juszczak2000, this issue) and the overall design of the two studies was almost identical. Briefly, it consisted of a case-control comparison based on subjects born in Scotland between 1 January 1971 and 31 December 1978. The obstetric data were derived from a cumulative register of all hospital births in Scotland (Scottish Morbidity Record 2, SMR2) containing fairly detailed demographic and obstetric information in a set numerical format, and members of the birth cohort who developed affective psychoses in adolescence or early adult life were identified from a register (Scottish Morbidity Record 4, SMR4) of all admissions to psychiatric hospitals or units in Scotland. Subjects with affective psychoses were individually matched with controls from the same birth cohort who had never been admitted to a psychiatric hospital with a discharge diagnosis of either schizophrenia or an affective psychosis on six different variables — the obstetric unit of birth, gender, date of birth (±2 months), maternal age (±2 years), maternal parity (first baby v. second or subsequent baby) and father's occupation (manual v. non-manual). Salient items in the SMR2 (obstetric) records of the probands and their controls were then compared. Further information is given in the previous paper describing the schizophrenia study (Reference Kendell, McInneny and JuszczakKendell et al, 2000, this issue). As in Kendell et al's study, the 1971-74 and 1975-78 birth cohorts were analysed separately, mainly because the content and layout of the form used to record obstetric (SMR2) information was changed on 1 January 1975.
Diagnostic criteria
For most of the relevant time period the National Health Service (NHS) in Scotland recorded all hospital diagnoses by their ICD-9 code numbers (World Health Organization, 1978). For the purpose of this study it was therefore straightforward to define ‘affective psychosis’ as ICD-9 code numbers 296.0-296.9. It is important to note, though, that category 296 in ICD-9 corresponded to the Kraepelinian concept of manic-depressive psychosis, which embraced severe depressive illnesses whether or not they were accompanied by hallucinations or delusions as well as manic and bipolar illnesses. However, ICD-9 was replaced by ICD-10 (World Health Organization, 1992) on 1 April 1996 and this classification does not contain either a category of affective psychosis or a category corresponding to Kraepelin's manic-depressive psychosis. Nor is there any official translation from ICD-9 to ICD-10. For this reason affective psychosis had to be defined after 1 April 1996 by an arbitrary grouping of ICD-10 codes (F30, F31, F32.2 and 32.3 and F33.2 and 33.3) chosen to correspond as closely as possible to the previous 296 code. Discharge rather than admission diagnoses were used throughout and in subjects with more than one psychiatric admission the most recent discharge diagnosis was used.
Matching with controls
SMR2 (obstetric) records were found for 343 (51%) of the 668 subjects with affective psychoses born in 1971-78 originally identified from the SMR4 (psychiatric) file. The main reasons for failure to identify a matching SMR2 record were birth outside Scotland and domiciliary delivery. Vital demographic information (mainly the father's occupation) was missing from 26 obstetric records, which reduced the total available for matching from 343 to 317. It proved possible to match all but 16 of these on all of the six variables described above. We therefore obtained 301 matched pairs — 217 born in 1971-74 and 84 born in 1975-78. There are far fewer in the 1975-78 cohort because its members are, on average, 4 years younger and only just entering the risk period for the development of an affective psychosis.
At the time the SMR4 (psychiatric) data were extracted from the master file (October 1997) the age of the 1971-74 affective probands ranged from 22-26 years. Fifty per cent were male and 102 (47%) had manic or bipolar illnesses. The age of the 1975-78 probands ranged from 18-22 years. Fifty per cent were male and 45 (54%) had manic or bipolar illnesses. Probands and controls were compared using the same standard case-control analysis of matched case-control sets as the parallel study of obstetric complications and schizophrenia (Reference Kendell, McInneny and JuszczakKendell et al, 2000, this issue).
RESULTS
1971-74 births
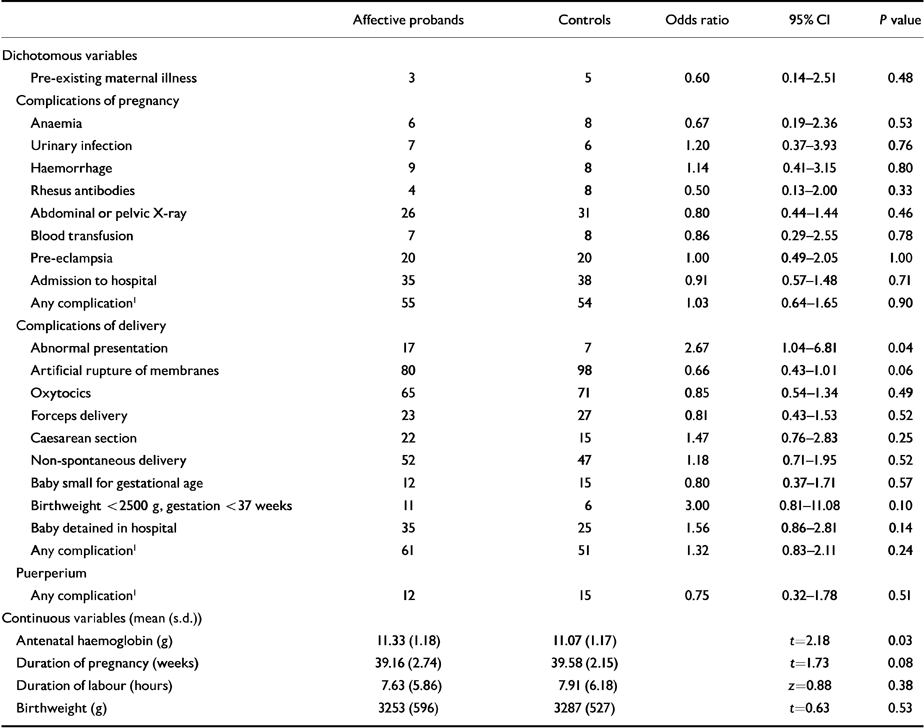
The results of the proband-control comparisons are shown in Table 1. The incidence of complications of both pregnancy and delivery is very similar in the affective probands and their controls. Indeed, there is only a significant difference between them for two of the 24 items studied. Abnormal presentation of the foetus is more common in the probands (17 v. 7; P=0.04) and a maternal haemoglobin level below 10 g is more common in the controls (16 v. 7; P=0.05). The mean maternal haemoglobin level is also 0.26 g lower in the controls (P=0.03). As in the schizophrenia study, all the complications recorded on the SMR2 form by their ICD-8 (World Health Organization, 1967) code numbers were compared individually, but there was only one significant difference. Delivery complicated by malpresentation of the foetus was more common in the affectives (9 v. 1; P<0.02), but this is really the same item as before.
Table 1 1971-74 births. Complications of pregnancy, delivery and the puerperium. Comparison of probands with affective psychoses and their controls (217 matched pairs)
| Affective probands | Controls | Odds ratio | 95% CI | P value | |
|---|---|---|---|---|---|
| Dichotomous variables | |||||
| Pre-existing maternal illness | 3 | 5 | 0.60 | 0.14-2.51 | 0.48 |
| Complications of pregnancy | |||||
| Anaemia | 6 | 8 | 0.67 | 0.19-2.36 | 0.53 |
| Urinary infection | 7 | 6 | 1.20 | 0.37-3.93 | 0.76 |
| Haemorrhage | 9 | 8 | 1.14 | 0.41-3.15 | 0.80 |
| Rhesus antibodies | 4 | 8 | 0.50 | 0.13-2.00 | 0.33 |
| Abdominal or pelvic X-ray | 26 | 31 | 0.80 | 0.44-1.44 | 0.46 |
| Blood transfusion | 7 | 8 | 0.86 | 0.29-2.55 | 0.78 |
| Pre-eclampsia | 20 | 20 | 1.00 | 0.49-2.05 | 1.00 |
| Admission to hospital | 35 | 38 | 0.91 | 0.57-1.48 | 0.71 |
| Any complication1 | 55 | 54 | 1.03 | 0.64-1.65 | 0.90 |
| Complications of delivery | |||||
| Abnormal presentation | 17 | 7 | 2.67 | 1.04-6.81 | 0.04 |
| Artificial rupture of membranes | 80 | 98 | 0.66 | 0.43-1.01 | 0.06 |
| Oxytocics | 65 | 71 | 0.85 | 0.54-1.34 | 0.49 |
| Forceps delivery | 23 | 27 | 0.81 | 0.43-1.53 | 0.52 |
| Caesarean section | 22 | 15 | 1.47 | 0.76-2.83 | 0.25 |
| Non-spontaneous delivery | 52 | 47 | 1.18 | 0.71-1.95 | 0.52 |
| Baby small for gestational age | 12 | 15 | 0.80 | 0.37-1.71 | 0.57 |
| Birthweight <2500 g, gestation <37 weeks | 11 | 6 | 3.00 | 0.81-11.08 | 0.10 |
| Baby detained in hospital | 35 | 25 | 1.56 | 0.86-2.81 | 0.14 |
| Any complication1 | 61 | 51 | 1.32 | 0.83-2.11 | 0.24 |
| Puerperium | |||||
| Any complication1 | 12 | 15 | 0.75 | 0.32-1.78 | 0.51 |
| Continuous variables (mean (s.d.)) | |||||
| Antenatal haemoglobin (g) | 11.33 (1.18) | 11.07 (1.17) | t=2.18 | 0.03 | |
| Duration of pregnancy (weeks) | 39.16 (2.74) | 39.58 (2.15) | t=1.73 | 0.08 | |
| Duration of labour (hours) | 7.63 (5.86) | 7.91 (6.18) | z=0.88 | 0.38 | |
| Birthweight (g) | 3253 (596) | 3287 (527) | t=0.63 | 0.53 | |
1975-78 births
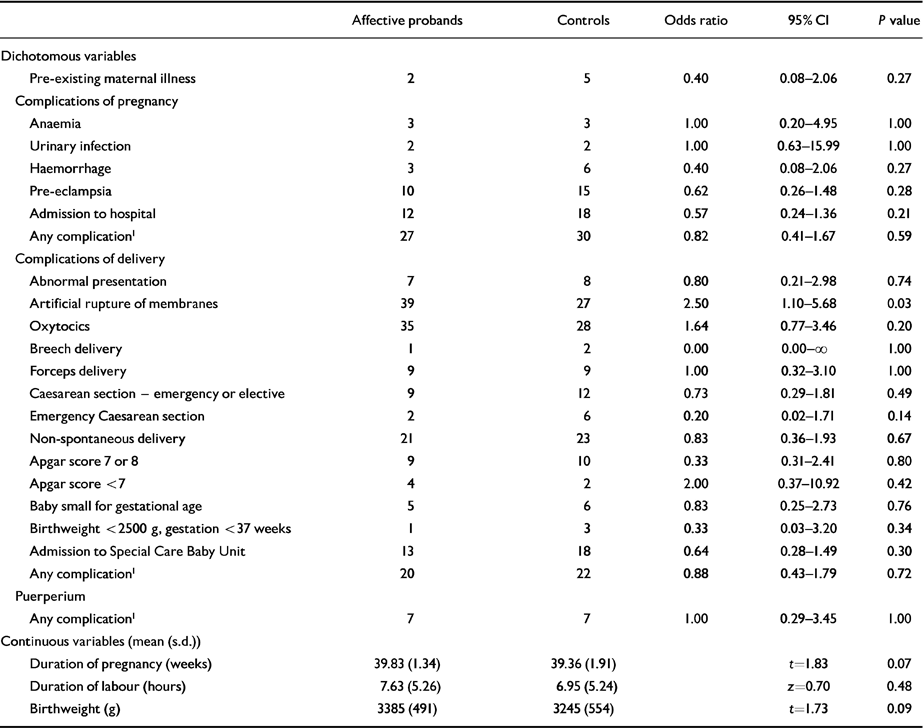
The results of the proband-control comparisons are shown in Table 2. Again, the incidence of complications of both pregnancy and delivery is very similar in the affective probands and their controls — there is a significant difference between the two for only one of the (slightly different) set of 24 items studied. Artificial rupture of the membranes is more common in the probands (39 v. 27; P=0.03). It is important to note, though, that in the 1971-74 cohort artificial rupture of the membranes was more common in the controls (98 v. 80; P=0.06), suggesting that this is a chance finding. Similarly, abnormal presentation of the foetus is marginally more common in the control group (8 v. 7) suggesting that the higher frequency in the probands in the 1971-74 birth cohort may also have been a chance finding.
Table 2 1975-78 births. Complications of pregnancy, delivery and the puerperium. Comparison of probands with affective psychoses and their controls (84 matched pairs)
| Affective probands | Controls | Odds ratio | 95% CI | P value | |
|---|---|---|---|---|---|
| Dichotomous variables | |||||
| Pre-existing maternal illness | 2 | 5 | 0.40 | 0.08-2.06 | 0.27 |
| Complications of pregnancy | |||||
| Anaemia | 3 | 3 | 1.00 | 0.20-4.95 | 1.00 |
| Urinary infection | 2 | 2 | 1.00 | 0.63-15.99 | 1.00 |
| Haemorrhage | 3 | 6 | 0.40 | 0.08-2.06 | 0.27 |
| Pre-eclampsia | 10 | 15 | 0.62 | 0.26-1.48 | 0.28 |
| Admission to hospital | 12 | 18 | 0.57 | 0.24-1.36 | 0.21 |
| Any complication1 | 27 | 30 | 0.82 | 0.41-1.67 | 0.59 |
| Complications of delivery | |||||
| Abnormal presentation | 7 | 8 | 0.80 | 0.21-2.98 | 0.74 |
| Artificial rupture of membranes | 39 | 27 | 2.50 | 1.10-5.68 | 0.03 |
| Oxytocics | 35 | 28 | 1.64 | 0.77-3.46 | 0.20 |
| Breech delivery | 1 | 2 | 0.00 | 0.00-∞ | 1.00 |
| Forceps delivery | 9 | 9 | 1.00 | 0.32-3.10 | 1.00 |
| Caesarean section - emergency or elective | 9 | 12 | 0.73 | 0.29-1.81 | 0.49 |
| Emergency Caesarean section | 2 | 6 | 0.20 | 0.02-1.71 | 0.14 |
| Non-spontaneous delivery | 21 | 23 | 0.83 | 0.36-1.93 | 0.67 |
| Apgar score 7 or 8 | 9 | 10 | 0.33 | 0.31-2.41 | 0.80 |
| Apgar score <7 | 4 | 2 | 2.00 | 0.37-10.92 | 0.42 |
| Baby small for gestational age | 5 | 6 | 0.83 | 0.25-2.73 | 0.76 |
| Birthweight <2500 g, gestation <37 weeks | 1 | 3 | 0.33 | 0.03-3.20 | 0.34 |
| Admission to Special Care Baby Unit | 13 | 18 | 0.64 | 0.28-1.49 | 0.30 |
| Any complication1 | 20 | 22 | 0.88 | 0.43-1.79 | 0.72 |
| Puerperium | |||||
| Any complication1 | 7 | 7 | 1.00 | 0.29-3.45 | 1.00 |
| Continuous variables (mean (s.d.)) | |||||
| Duration of pregnancy (weeks) | 39.83 (1.34) | 39.36 (1.91) | t=1.83 | 0.07 | |
| Duration of labour (hours) | 7.63 (5.26) | 6.95 (5.24) | z=0.70 | 0.48 | |
| Birthweight (g) | 3385 (491) | 3245 (554) | t=1.73 | 0.09 | |
As before, all the complications recorded on the SMR2 forms by their ICD-8 code numbers were compared individually, but no significant differences emerged.
DISCUSSION
The most plausible explanation of these findings is that the incidence of obstetric complications is not raised in affective psychoses and that they are not a risk factor for the development of an affective psychosis. In both the 1971-74 and 1975-78 birth cohorts the incidence of complications of both pregnancy and delivery was very similar in the affective probands and their controls. The one complication that was significantly more common in the affective group in the 1971-74 cohort — abnormal presentation of the foetus — was marginally more common in the controls in the 1975-78 cohort and the only complication that was more common in the affective group in the 1975-78 cohort — artificial rupture of the membranes — was considerably more common in the controls in the larger 1971-74 cohort. Both complications are also different from those (emergency Caesarean section and a labour lasting over 12 hours) which were significantly more common in our probands with schizophrenia than in their controls (Reference Kendell, McInneny and JuszczakKendell et al, 2000, this issue) and the reduced duration of pregnancy previously reported in their affective patients by Done et al (Reference Done, Johnstone and Frith1991).
This conclusion is subject to two qualifications. First, none of the subjects even in the 1971-74 birth cohort was over the age of 26 years, so none had passed through the main risk period for the development of an affective psychosis. It is possible, therefore, that the incidence of obstetric complications is raised in the mainly unipolar or depressive psychoses presenting later in life. Second, the obstetric (SMR2) and psychiatric (SMR4) data on which this study was based were recorded, albeit in a set numerical format, in the course of ordinary clinical practice and little is known about their reliability (see Reference Kendell, McInneny and JuszczakKendell et al, 2000, this issue). If their reliability was very low genuine proband-control differences could have failed to emerge. With a total sample size of over 300 matched pairs, however, it is unlikely that major differences could have been completely obscured, particularly as there was not even a trend for complications to be commoner in the affectives than in their closely matched controls.
APPENDIX
After this study was completed a very similar Swedish investigation was published by Hultman et al (Reference Hultman, Sparén and Takei1999). As here, this case-control study was based on a national birth cohort from the 1970s and obstetric information recorded shortly after birth. Affective psychosis was defined in the same way (ICD-9 category 296); the number of affective probands was smaller but still substantial (n=198). Apart from a relationship with birth in January to April (the ‘season of birth effect’) the only obstetric variable that was significantly commoner in the affective psychoses than their controls was uterine atony (odds ratio 2.2, 95% Cl 1.2-4.1), and when males and females were examined separately the difference was only significant in the former. This study therefore strengthens our conclusion that obstetric complications are unlikely to be a risk factor for the development of an early onset affective psychosis.
Clinical Implications and Limitations
CLINICAL IMPLICATION
-
▪ It is unlikely that obstetric complications contribute to the aetiology of early onset affective psychoses.
LIMITATIONS
-
▪ Little information is available about the reliability of the routinely recorded obstetric data on which the study was based.
-
▪ People with affective psychoses were identified by clinical diagnoses at the time of discharge from in-patient care.
-
▪ Subjects were all under the age of 27 years, and so had not passed through the main risk period for affective psychosis.







eLetters
No eLetters have been published for this article.