The management of psychotic symptoms using cognitive-behavioural therapy (CBT) as an adjunct to traditional psychiatric care is looking increasingly promising (Reference Bouchard, Vallierres and RoyBouchard et al, 1996). This conclusion is supported by the results of controlled trials of CBT for acute positive symptoms (Reference Drury, Birchwood and CochraneDrury et al, 1996a ) and drug-resistant positive symptoms (Reference Kuipers, Garety and FowlerKuipers et al, 1997; Reference Tarrier, Yusupoff and KinneyTarrier et al, 1998). However, although the effectiveness of CBT programmes appears to be maintained at the 9-month follow-up (Reference Drury, Birchwood and CochraneDrury et al, 1996a ) and may even improve (Reference Kuipers, Fowler and GaretyKuipers et al, 1998; Reference Sensky, Turkington and KingdonSensky et al, 2000), the longer-term outcome of CBT interventions for psychosis is not known. In a study by Hogarty et al (1997 Reference Hogarty, Kornblith and Greenwald a , Reference Hogarty, Greenwald and Ulrich b ) of patients recovering from an acute episode of psychosis, individuals receiving an intensive threephase psychosocial intervention over 3 years, known as ‘personal therapy’, showed a significant improvement in social functioning and were significantly less likely to have relapsed at the end of the programme than those receiving supportive therapy or family therapy, providing that they had been residing with their families. In a 15-year follow-up study of patients suffering from non-affective psychosis (Reference Wiersma, Nienhuis and SlooffWiersma et al, 1998), each psychotic episode increased the number of patients experiencing residual positive symptoms; just over 25% of patients showed persistent positive and/or negative symptoms after the first episode, compared with nearly 50% of the sample after the fourth episode. Shepherd et al (Reference Shepherd, Watt and Falloon1989) showed that, in over a third of patients suffering from schizophrenia, each relapse appeared to raise the level of social impairment and residual symptoms in a stepwise fashion. Relapse and residual psychotic symptoms tend to be viewed as separate domains of outcome, whereas here is evidence that they are linked.
This study reports a follow-up of our original cohort of patients 5 years after they had received either a multi-component CBT programme (the CT group) or a social recreational programme with informal support (the ATY group) during an acute phase of their illness (Drury et al, 1996 Reference Drury, Birchwood and Cochrane a , Reference Drury, Birchwood and Cochrane b ). We thought that the occurrence of relapse would have an adverse effect on the level of self-reported delusional beliefs (the primary target of the intervention); and that the reduction in residual delusions shown by the cognitive-behavioural therapy programme CT group when compared with the control ATY group would be maintained only if there had been no more than one relapse between discharge from hospital and follow-up. We also predicted that improvements in certain cognitive variables also targeted during the intervention (attitudes relating to the self and psychosis) would be enduring.
METHOD
Participants and study design
The criteria for selection, and the sociodemographic characteristics, of the patients who took part in a controlled trial of cognitive therapy in acute psychosis have been reported in detail elsewhere (Reference Drury, Birchwood and CochraneDrury et al, 1996a ). The study design and treatment protocols were also described in the same paper. Briefly, 40 hospitalised patients suffering from an acute episode of nonaffective psychosis were allocated, using a stratified sampling technique, to one of two groups : CT or ATY (recreational activities with informal support). The intervention used with the CT group consisted of four individual and group procedures (Reference Birchwood, Drury, Phelan, Strathdee and ThornicroftBirchwood & Drury, 1995; Reference Chadwick, Trower and BirchwoodChadwick et al, 1996; Reference Drury, Birchwood, Fowler and JacksonDrury, 2000) delivered in a staged way over the course of recovery. These were as follows :
-
(a) Individual cognitive therapy in the context of a supportive relationship involving the identification, gentle challenging and empirical testing of evidence for key delusional beliefs.
-
(b) Group cognitive therapy, in small groups of six patients with two facilitators, where patients were encouraged to see how others' delusional beliefs were often supported by flimsy, inconsistent - sometimes contradictory - evidence, and were asked to consider alternative explanations for them. The negative cultural stereotypes of severe mental illness were highlighted and questioned, and blame-free acceptance of illness was encouraged to reduce stigma. Feelings of control and mastery were fostered by helping patients to understand and develop new strategies for coping with positive symptoms and possible relapse, and encouraging ‘integration’ of psychotic experiences.
-
(c) Family psychoeducation and support, which included specific sessions on how to support the patient in attempts to manage their symptoms, particularly delusional beliefs (which were the target of the intervention).
-
(d) An activity programme including lifeskills groups and creative therapies.
The ATY group were encouraged to take part in sports, leisure and social groups carefully matched to their interests and capabilities. They had contact with the same therapists as the CT group, and although queries about symptoms were listened to sympathetically, discussions about the nature of symptoms were not entered into.
Each group received intensive input (mean therapist contact time of 8 h/week) for a maximum of 6 months. Both treatments were an adjunct to standard care. The primary aim of the CBT intervention was to hasten the decay of positive symptoms and to reduce the level of residual delusional beliefs. Secondary aims, particularly through the use of group cognitive therapy, were to encourage the ‘integration’ of psychotic experiences, to improve insight and the self-management of symptoms, and to reduce the sense of isolation and stigma associated with a label of ‘severe mental illness’. Patients in the two groups at entry to the study did not differ in terms of absolute morbidity (i.e. there were no significant differences between the groups in terms of number of episodes, duration of illness or duration of untreated psychosis) or in key risk factors including gender, genetic risk and age at onset.
Patients were followed up after a mean of 5 years. As the original trial spanned a period of 18 months, a few of the patients were followed up after only 4 years. Data regarding relapses and periods in hospital are therefore based on a period of 4 rather than 5 years following discharge from acute hospital care for the index episode. No further formal CBT intervention or booster sessions were provided in the intervening years for any of the patients in the study. In the experimental group (n=20), two patients had left the area and were completely lost to follow-up, and one refused to be interviewed. This left a sample of 17 who agreed to be interviewed. Two of these refused face-to-face contact but agreed to telephone interviews, and completed all of the self-report questionnaires by post. Two patients were unable to complete all the self-report questionnaires because they were too unwell. In the control group (n=20), one patient had left the area and was completely lost to follow-up and two refused to take part. This left a sample of 17 who agreed to be interviewed. Two of these were unable to complete all the self-report questionnaires because they were too unwell. A small financial remuneration was offered to all participants in acknowledgement of their time.
A limitation of the original trial was that the assessors were neither blind to the treatment group nor independent. In an attempt to partly overcome this, all but one of the assessments to be used in the follow-up (as in the original trial) were self-report measures.
Measures
The participants were assessed using four of the measures used for assessment at entry into the study. Measures were administered either by an assistant psychologist who was not involved in the original trial, or by the first author. Neither were blind to treatment group, but both were blind to relapse and rehospitalisation.
Positive symptoms (hallucinations and delusions), thought disorder and negative symptoms (flattened affect, psychomotor retardation and poverty of speech) were assessed using the Psychiatric Assessment Scale (PAS, Reference Krawiecka, Goldberg and VaughanKrawiecka et al, 1977), in which all categories of symptoms are assessed on a 0-4 scale where 0/1 denotes absence of pathology and 2, 3 or 4 indicate that the target symptom is present in increasing severity.
Levels of conviction for the three core delusional beliefs that were elicited in the acute phase were measured using personal questionnaires (Belief and Convictions Scale, Reference Brett-Jones, Garety and HemsleyBrett-Jones et al, 1987). Degree of conviction was rated on a 0-5 scale, where 0 denotes that the belief is no longer held and 5 denotes full conviction in the belief.
Insight was assessed using the self-report Insight Scale (a 12-item scale where a score of 12 denotes full insight) (Reference Birchwood, Smith and DruryBirchwood et al, 1994) and appraisals of self and psychosis were measured using the Personal Beliefs about Illness Questionnaire (PBIQ, Reference Birchwood, Mason and MacmillanBirchwood et al, 1993). The PBIQ assesses the patients' beliefs about their illness and uses the first person (e.g. ‘I know when I am relapsing but I can't do anything about it’). It is divided into five sub-scales : ‘Control over illness’, ‘Expectations’, ‘Awareness of stigma’, ‘Need for containment and social marginalisation’ and ‘Self as illness’. Low scores on these sub-scales indicate favourable attitudes towards the self and psychosis, i.e. a high perceived level of control over illness (low entrapment in psychosis), positive expectations of future performance, particularly with respect to work (high autonomy), low awareness of stigma, little need for containment, and the illness as separate rather than an integral part of the self.
Information about out-patient attendance, medication compliance (rated as full, good but not full, partial or none), relapses and admissions to hospital was collected from the medical notes. ‘Relapse’ was defined as admission to hospital or home treatment with an exacerbation of acute psychotic symptoms, or documentation of early relapse followed by an increase in medication and frequent visits by the keyworker. The case notes were examined after all other data collection had been completed by the first author and an assistant psychologist.
Data analysis
Data summary and analyses were carried out using SPSS for Windows Version 6.1. Dependent variables were compared between groups, using analysis of covariance (ANCOVA) with the corresponding baseline variable as covariate. Since insufficient data were available at week 1, due to difficulties arising from the acute nature of the psychosis, ratings of variables at week 2 were used as the baseline data.
RESULTS
The sample
Thirty-four patients were available to follow-up. At the start of the original study (Drury et al, 1996Reference Drury, Birchwood and Cochrane a , Reference Drury, Birchwood and Cochrane b ), these patients had experienced a mean of 3.4 episodes of illness and had been ill for a mean of 6.6 years. The median age at onset of illness was 24.5 years and the median age at follow-up was 32.5 years. Of the 34 patients available to follow-up, 61.8% were White, 14.7% were Asian, 23.5% were African-Caribbean; 64.7% were male and 35.3% were female; 79.4% were single, 8.8% were married and 11.8% were divorced or separated.
Sample attrition
Six of the 40 patients were lost to follow-up (15%), three from each group : three could not be traced and three refused to be interviewed. These six patients had (at the start of the original study) experienced a mean of 2.2 episodes of illness and had been ill for a mean of 3.5 years. The median age of onset of illness was 24.5 years and the median age at follow-up was 33.5 years. Fifty per cent of this group were White and 50% were African-Caribbean; 50% were male and 50% were female; 85.7% were single and 14.3% were married. The group lost to follow-up did not significantly differ from the group available for follow-up on any of the above variables, nor on delusional conviction or PAS scores at baseline.
Relapse or readmission to hospital
The two groups at follow-up did not differ with regard to number of relapses, number of admissions to hospital or time in acute care (see Table 1). Nor did the cumulative number of relapses recorded at 9 months, 1 year, 2 years and 3 years vary between the groups.
Table I Clinical characteristics of study samples at 4-year follow-up (all P=NS)

| CT (n=18) | ATY (n=19) | |
|---|---|---|
| Mean no. of relapses (s.d.) | 1.4 (1.6) | 1.2 (1.4) |
| Mean no. of admissions to hospital (s.d.) | 1.2 (1.4) | 1.2 (1.4) |
| Median time in acute care (days) | 26.5 | 32.0 |
| Median time to first relapse (days) | 821.0 | 345.0 |
In order to test our hypothesis that the effect of CBT would endure in those who had relapsed no more than once, we examined experimental effects for (a) the group as a whole and (b) those individuals who had relapsed only once, or not at all.
Long-term impact of CBT
(a) For the whole group
Variances and distributions of data across the two groups were found to show a similar pattern (Levene test for homogeneity of variance P>0.05).
Primary analysis : Positive symptoms.
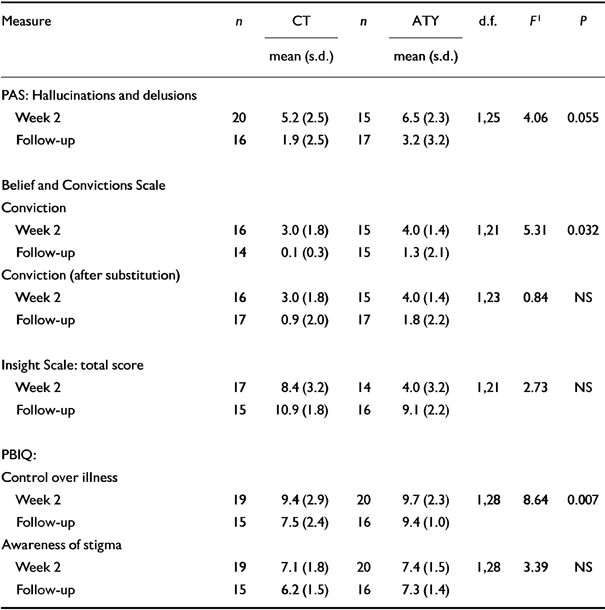
ANCOVAs with the corresponding baseline variable as covariate showed that at followup there was a strong trend towards the CT group reporting significantly fewer positive symptoms (hallucinations and delusions) than the ATY group (P=0.056) as measured by the PAS (see Table 2).
Table 2 Outcome variables at 5-year follow-up which were targeted in the original intervention
| Measure | n | CT | n | ATY | d.f. | F 1 | P |
|---|---|---|---|---|---|---|---|
| mean (s.d.) | mean (s.d.) | ||||||
| PAS : Hallucinations and delusions | |||||||
| Week 2 | 20 | 5.2 (2.5) | 15 | 6.5 (2.3) | 1,25 | 4.06 | 0.055 |
| Follow-up | 16 | 1.9 (2.5) | 17 | 3.2 (3.2) | |||
| Belief and Convictions Scale | |||||||
| Conviction | |||||||
| Week 2 | 16 | 3.0 (1.8) | 15 | 4.0 (1.4) | 1,21 | 5.31 | 0.032 |
| Follow-up | 14 | 0.1 (0.3) | 15 | 1.3 (2.1) | |||
| Conviction (after substitution) | |||||||
| Week 2 | 16 | 3.0 (1.8) | 15 | 4.0 (1.4) | 1,23 | 0.84 | NS |
| Follow-up | 17 | 0.9 (2.0) | 17 | 1.8 (2.2) | |||
| Insight Scale : total score | |||||||
| Week 2 | 17 | 8.4 (3.2) | 14 | 4.0 (3.2) | 1,21 | 2.73 | NS |
| Follow-up | 15 | 10.9 (1.8) | 16 | 9.1 (2.2) | |||
| PBIQ : | |||||||
| Control over illness | |||||||
| Week 2 | 19 | 9.4 (2.9) | 20 | 9.7 (2.3) | 1,28 | 8.64 | 0.007 |
| Follow-up | 15 | 7.5 (2.4) | 16 | 9.4 (1.0) | |||
| Awareness of stigma | |||||||
| Week 2 | 19 | 7.1 (1.8) | 20 | 7.4 (1.5) | 1,28 | 3.39 | NS |
| Follow-up | 15 | 6.2 (1.5) | 16 | 7.3 (1.4) |
Primary analysis : Conviction in targeted delusional beliefs.
For the individuals who were willing and/or able to rate their delusional conviction, self-reported mean delusional conviction (based on the three core beliefs elicited at entry to the study) was significantly lower for the CT group than the ATY group (see Table 2). For those individuals who were contacted but did not rate the conviction of their three original core delusional beliefs (three individuals from the CT group and two individuals from the ATY group), we assumed that lack of cooperation was due to severity of illness rather than other factors, and we therefore conservatively substituted the maximum score of 5 and re-ran the analysis. Following this substitution there was no significant difference between the groups on mean delusional belief conviction (see Table 2).
Primary analysis : Insight, beliefs about the self and psychosis targeted in the intervention.
At the 5-year follow-up, the CT group reported significantly better ‘Control over illness’ than the ATY group (P<0.01), as measured by the PBIQ, in which a lower score is indicative of better perceived control. There were no significant differences between the groups on the Insight Scale or the PBIQ ‘Awareness of stigma’ (see Table 2).
Secondary analysis :
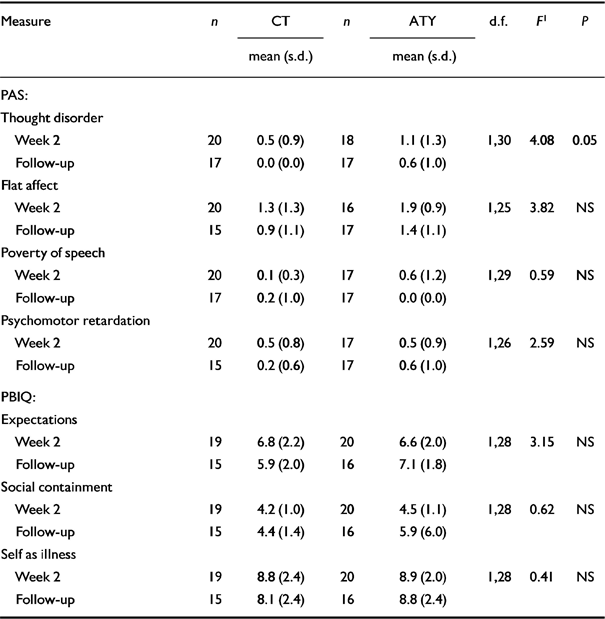
Thought disorder and negative symptoms. The CT group demonstrated significantly less thought disorder than the ATY group (see Table 3); in fact, the CT group showed no evidence of thought disorder at all, and the mean score for the ATY group (0.6) indicates very low levels of thought disorder. Examination of the raw data showed that two individuals had non-pathological levels of thought disorder, three had mild levels and one had moderate levels. As shown in Table 3, there was no significant difference in negative symptoms between the groups as measured by the PAS.
Table 3 Means (s.d.) of measures of outcome : post hoc tests
| Measure | n | CT | n | ATY | d.f. | F 1 | P |
|---|---|---|---|---|---|---|---|
| mean (s.d.) | mean (s.d.) | ||||||
| PAS : | |||||||
| Thought disorder | |||||||
| Week 2 | 20 | 0.5 (0.9) | 18 | 1.1 (1.3) | 1,30 | 4.08 | 0.05 |
| Follow-up | 17 | 0.0 (0.0) | 17 | 0.6 (1.0) | |||
| Flat affect | |||||||
| Week 2 | 20 | 1.3 (1.3) | 16 | 1.9 (0.9) | 1,25 | 3.82 | NS |
| Follow-up | 15 | 0.9 (1.1) | 17 | 1.4 (1.1) | |||
| Poverty of speech | |||||||
| Week 2 | 20 | 0.1 (0.3) | 17 | 0.6 (1.2) | 1,29 | 0.59 | NS |
| Follow-up | 17 | 0.2 (1.0) | 17 | 0.0 (0.0) | |||
| Psychomotor retardation | |||||||
| Week 2 | 20 | 0.5 (0.8) | 17 | 0.5 (0.9) | 1,26 | 2.59 | NS |
| Follow-up | 15 | 0.2 (0.6) | 17 | 0.6 (1.0) | |||
| PBIQ : | |||||||
| Expectations | |||||||
| Week 2 | 19 | 6.8 (2.2) | 20 | 6.6 (2.0) | 1,28 | 3.15 | NS |
| Follow-up | 15 | 5.9 (2.0) | 16 | 7.1 (1.8) | |||
| Social containment | |||||||
| Week 2 | 19 | 4.2 (1.0) | 20 | 4.5 (1.1) | 1,28 | 0.62 | NS |
| Follow-up | 15 | 4.4 (1.4) | 16 | 5.9 (6.0) | |||
| Self as illness | |||||||
| Week 2 | 19 | 8.8 (2.4) | 20 | 8.9 (2.0) | 1,28 | 0.41 | NS |
| Follow-up | 15 | 8.1 (2.4) | 16 | 8.8 (2.4) |
Secondary analysis : Attitudes about the self and psychosis not targeted in the intervention.
There was no significant difference between the groups on ‘Expectations’, ‘Social containment’ and ‘Self as illness’ as measured by the PBIQ (see Table 3).
(b) For those individuals who had at most one relapse
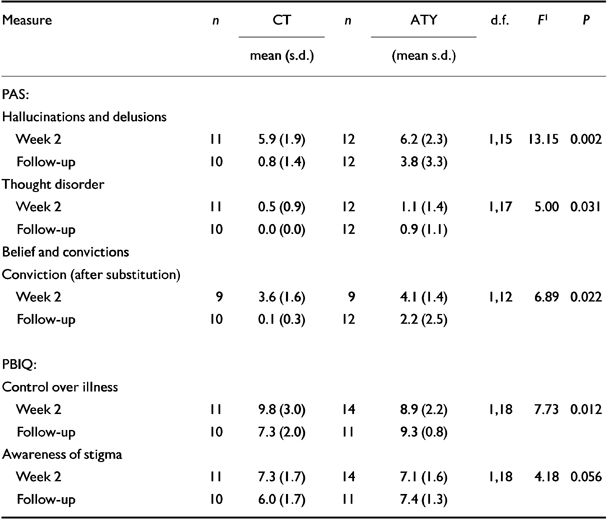
As shown in Table 4, for those individuals who had suffered no relapses, or only one, residual positive symptoms were significantly less in the CT group than in the ATY group. The mean self-reported delusional conviction in the CT group was significantly less than that reported by the ATY group (with the substitution of 5 for one individual in the ATY group who was not able to rate their beliefs). Severity of observer-rated delusional ideation and hallucinations and thought disorder as measured by the PAS also differentiated the groups (higher in controls).
Table 4 Measures of outcome which differentiated between the groups for those individuals who had relapsed once or not at all
| Measure | n | CT | n | ATY | d.f. | F 1 | P |
|---|---|---|---|---|---|---|---|
| mean (s.d.) | (mean s.d.) | ||||||
| PAS : Hallucinations and delusions Week 2 | 11 | 5.9(1.9) | 12 | 6.2(2.3) | 1,15 | 13.15 | 0.002 |
| Follow-up | 10 | 0.8(1.4) | 12 | 3.8(3.3) | |||
| Thought disorder | |||||||
| Week 2 | 11 | 0.5(0.9) | 12 | 1.1(1.4) | 1,17 | 5.00 | 0.031 |
| Follow-up | 10 | 0.0(0.0) | 12 | 0.9(1.1) | |||
| Belief and convictions | |||||||
| Conviction (after substitution) | |||||||
| Week 2 | 9 | 3.6(1.6) | 9 | 4.1(1.4) | 1,12 | 6.89 | 0.022 |
| Follow-up | 10 | 0.1(0.3) | 12 | 2.2(2.5) | |||
| PBIQ : | |||||||
| Control over illness | |||||||
| Week 2 | 11 | 9.8(3.0) | 14 | 8.9(2.2) | 1,18 | 7.73 | 0.012 |
| Follow-up | 10 | 7.3(2.0) | 11 | 9.3(0.8) | |||
| Awareness of stigma | |||||||
| Week 2 | 11 | 7.3(1.7) | 14 | 7.1(1.6) | 1,18 | 4.18 | 0.056 |
| Follow-up | 10 | 6.0(1.7) | 11 | 7.4(1.3) |
In line with the analysis for the whole sample, the total Insight Scale score was not significantly different between the groups. There was a significant difference in perceived ‘Control over illness’ and a strong trend towards a significant difference in ‘Awareness of stigma’ between the groups as measured by the PBIQ, with the individuals in the CT group showing the most adaptive attitudes.
Medication and out-patient attendance
Four individuals from the CT group and five from the ATY were not taking any neuroleptic medication. Apart from one person in the ATY group, this was in each case the patient's rather than the clinician's decision. Four individuals from the CT group (22%) and four from the ATY (16%) were prescribed atypical neuroleptic medication. For the remainder (CT=11; ATY=11), when prescribed medication was converted to chlorpromazine equivalents, following the procedure described in the British National Formulary (British Medical Association, 2000, p. 172), there was no significant difference in the mean daily dose of medication between the groups (CT=440.3 mg, s.d.=750.7; ATY=380.1 mg, s.d.=580.6). One individual from each group was being prescribed mood-stabilishing medication (lithium or carbamazepine) in addition to neuroleptic medication. The percentage of out-patient clinic appointments attended, and the self-reported medication compliance, did not differ significantly between the groups.
DISCUSSION
This is the first long-term follow-up of patients receiving a short-term but intensive CBT programme beginning in the acute phase of a psychotic illness. Some data were obtained on all but three of the original participants, and 28 out of 37 of the remaining participants complied fully with the follow-up assessment battery. This was considered to be an indirect indicator of the satisfaction with the original interventions, since a high refusal rate for follow-up assessments in common with this group of patients (Reference Tarrier, Beckett and HarwoodTarrier et al, 1993).
Main findings
At the 4-year follow-up no significant differences were found between the cognitive intervention group (CT) and the control group (ATY) in relapse rate, time in acute care or time to first relapse following the index episode. The two groups showed a remarkably similar pattern of relapses over the 4 years. Also, observer-rated positive and negative symptoms did not vary significantly between the groups. Thus, although there was a strong trend suggesting a difference in positive symptoms favouring the CT group at follow-up, much of the early improvement shown by this group over the ATY group at 9 months (Reference Drury, Birchwood and CochraneDrury et al, 1996a ) had been lost in the intervening years. There was, however, evidence that self-reported conviction in the three targeted (‘core’) delusional beliefs was significantly lower in the CT group at the 5-year follow-up. These results must be treated with caution, because nine of the original participants failed to cooperate with self-ratings of their delusional beliefs, and three participants were completely lost to followup. Indeed, when the maximum conviction score was substituted for this non-compliant group, the difference between the groups was no longer significant.
Perhaps the most interesting finding of this follow-up study was that, as predicted, cognitive-behavioural therapy led to significant and enduring clinical benefits, provided that the experience of relapse could be avoided or minimised. Both observerrated and self-rated delusional beliefs were significantly lower in the CT group than the ATY group among those individuals who had suffered no relapses, or only one. If we assume that risk factors for relapse (e.g. environmental factors such as life events) are random occurrences that impinge on both groups with the same probability, it appears that the CT group was nevertheless protected against the return of persistent psychotic symptoms to a greater degree than the ATY group, providing they had no more than one relapse. This finding suggests two therapeutic strategies. First, if relapse can be avoided or kept to a minimum, the beneficial effects of a CBT intervention in terms of reduction of residual psychotic symptoms can be maintained. Implementing a strategy of preventing, or minimising, relapses should enhance the durability of CBT (Reference Perry, Tarrier and MorrisPerry et al, 1999). Second, an alternative or complementary strategy might be to offer ‘booster’ CBT sessions at any subsequent relapse.
These findings underscore the critical importance of taking a long-term view, in the context of ongoing vulnerability. Trials of CBT for psychosis have consistently demonstrated short-term benefits (Reference Jones, Cormac, Mota and CampbellJones et al, 1998), but this study shows that re-emergence of the psychotic process can unravel the immediate gains. This theme has been taken up by Hogarty et al (1997 Reference Hogarty, Kornblith and Greenwald a , Reference Hogarty, Greenwald and Ulrich b ) in their trial of ‘personal therapy’ for schizophrenia. This successful approach was implemented over a 3-year time frame and embodied some of the principles of CBT interventions for psychosis such as psychoeducation, stress management, improving coping strategies and help with resolving or reframing difficult interpersonal situations. The authors note that “brief treatment would appear to be less effective than a long-term disorder relevant intervention” (Reference Hogarty, Greenwald and UlrichHogarty et al, 1997b p. 1514). In this context the study by Linszen et al (Reference Linszen, Lenior and de Haan1998) is of particular significance. Their combined family and individual intervention held relapse to 15% over 12 months in a first-episode sample; however, following transfer to standard services, relapse proliferated (64% in the following 2 years). In the present study, on the other hand, among those with minimal relapse, the impact of CBT endured over 5 years. This reinforces the importance of relapse prevention in the early critical period of psychosis, where the seeds of long-term treatment resistance are sown (Reference Birchwood, Fowler and JacksonBirchwood et al, 2000).
Methodological issues
In the initial paper we questioned whether the morbidity of the two groups was comparable. The groups were randomly assigned and comparable on risk factors (gender, untreated illness, ethnicity, number of relapses) and severity of symptoms.
The two groups have continued to relapse at comparable rates, and among those who have relapsed the most, the groups have converged in terms of residual psychotic symptoms. This adds credence to our claim (Reference Drury, Birchwood and CochraneDrury et al, 1996a ) that the two groups did not differ in absolute morbidity and that the results reflected the impact of CBT. We also questioned the blindness and independence of the assessments; but in this follow-up, as in the original trial, this remains an issue. However, reliability checks on the PAS were undertaken in the original trial and the targeted delusional beliefs were all assessed by self-report. In this study, furthermore, we predicted specific interactions with relapse, and these data were not available until the conclusion of the interviews. In fact, in overall terms, no differences emerged between the groups, but only in those with minimal relapse. In our view therefore, the outcomes cannot be accounted for by systematic experimenter bias. Replication is vital, and we anticipate with interest the results of the replication of this study by the ongoing multi-centre soCRATES Medical Research Council trial.
Compared with other long-term followup studies of psychosis, we feel that sample attrition was conservative. After 5 years, only six out of 40 patients (15%) were either untraceable or refused interview. Seventy per cent of the sample completed all the assessments.
Attitudes to self and psychosis
In our 1996a paper we described one of the key aims of the intervention as being the ‘integration’ of psychosis, where the individual develops a curious approach to their illness and views it as something they can exert control over. The group intervention was specifically formulated to address these aspects (and to facilitate response to CBT).
The follow-up shows that the CT group maintained a greater sense of control over their illness, and that those in the CT group (with minimal relapse) were protected against feelings of stigma (both these points were directly addressed in the intervention). A longitudinal study in psychosis (Reference Rooke and BirchwoodRooke & Birchwood, 1998) using the PBIQ suggested that perceived control over psychosis (‘entrapment’) was linked to control over both key symptoms (especially voices) and relapse. We believe these meta-beliefs are crucial in the individual's recovery from, and adjustment to, psychosis and bear upon feelings of hopelessness which are linked to control (Reference Rooke and BirchwoodRooke & Birchwood, 1998) and are so prevalent in first episode psychosis (Reference Aguilar, Haas and ManzaneraAguilar et al, 1997).
CLINICAL IMPLICATIONS AND LIMITATIONS
CLINICAL IMPLICATIONS
-
▪ Short-term benefits of the cognitive therapy programme, applied in the acute phase of a psychotic disorder as an adjunct to standard care, are enduring if relapse is avoided or minimised.
-
▪ Increased perceived control over psychotic illness appears to be an enduring effect of the cognitive intervention.
-
▪ Relapse prevention programmes or ‘booster’ sessions are likely to be an important part of long-term care, especially for first-episode patients.
LIMITATIONS
-
▪ Three-quarters of the original trial participants completed the full battery of assessments at follow-up (although this was controlled for at the data analysis stage).
-
▪ Assessors were blind to some aspects of clinical outcome (number of relapses and admissions to hospital) but were not independent or blind to treatment group.
-
▪ The sample is homogeneous and was from a deprived inner-city area with a high threshold for admission.
ACKNOWLEDGEMENTS
We would like to thank all participants in the study for their cooperation. We are indebted to our consultant psychiatrist and nursing colleagues of Northern Birmingham Mental Health NHS Trust and The Black Country Mental Health NHS Trust and to the staff of the Medical Records Department, All Saints Hospital and the staff of the Psychiatric Out Patient Clinic, Sandwell District General Hospital, for their help and assistance. We would like to thank Simon Kennedy for his help with data collection.









eLetters
No eLetters have been published for this article.