Studies of cohorts with schizophrenia consistently show higher levels of natural and unnatural mortality (Reference BrownBrown, 1997) but lack the clinical detail to explain individual deaths and suggest means of prevention. Lesage et al (Reference Lesage, Trapani and Tansella1990) and Anderson et al (Reference Anderson, Connelly and Johnstone1991) listed causes of death in schizophrenia prevalence cohorts, but neither study examined the circumstances of death in enough detail to identify the exact causes of the excess mortality. Proposed mechanisms of raised natural mortality include unrecognised medical disease (Reference Jeste, Gladsjo and LindamarJeste et al, 1996), unhealthy lifestyle, substance misuse (Reference McCreadie, Macdonald and BlacklockMcCreadie et al, 1998; Reference Brown, Birtwistle and RoeBrown et al, 1999; Reference Kelly and McCreadieKelly & McCreadie, 1999) and poor compliance or refusal of treatment for medical disease (Reference Jeste, Gladsjo and LindamarJeste et al, 1996). There is also a small but significant mortality associated with antipsychotic drug treatment (Reference Mortensen and JuelMortensen & Juel, 1990), while psychoses caused by medical disease with high mortality may be misdiagnosed. Most unnatural deaths are from suicide (Reference BrownBrown, 1997). We describe the mortality of a cohort of 370 patients with schizophrenia followed for 13 years. We examined the circumstances of each death and tried to identify mechanisms behind the increased mortality.
METHOD
The cohort comprised Southampton residents with schizophrenia aged 16-65Footnote 1 living outside hospital, who had had contact with the psychiatric service at the Royal South Hants Hospital between 1 February 1981 and 31 January 1982 (n=370). Subjects were included if: (a) a ‘firm diagnosis of schizophrenia’ had been made by the responsible consultant; (b) there was evidence in their case notes of first-rank symptoms of schizophrenia or persistent non-affective delusions or auditory hallucinations, in the absence of organic brain disease, misuse of alcohol or other substances (Reference Gibbons, Horn and PowellGibbons et al, 1984). Excluded were 47 Southampton residents with persistent schizophrenia, living long-term in the area mental hospital, Knowle Hospital (Reference Gibbons, Horn and PowellGibbons et al, 1984).
Subjects were followed up to 31 December 1994, the cohort census date, and classified as alive, dead or untraced. ‘Alive’ means evidence from records, professional staff, or interview with relatives or patient; ‘dead’ means sight of a death certificate or other official document confirming death; ‘untraced’, neither of these. The untraced were included in the follow-up period until the date they were lost. Medical and psychiatric history, smoking history, personal circumstances, account and cause of death came from the research record of the 1981 study, hospital case notes, relatives, professional staff, coroner's record and death certificate.
Person-years-at-risk by age and gender were calculated, and multiplied by the appropriate mortality rates for England and Wales, in order to obtain the expected number of deaths (Reference Breslow and DayBreslow & Day, 1987; Office of Population Censuses and Surveys, 1981-1994). The number of deaths observed divided by the number of deaths expected and multiplied by 100 gave the standardised mortality ratio (SMR). An increased SMR is statistically significant when the lower confidence interval (CI) (95%) is 100 or more (Reference Gardner and AltmanGardner & Altman, 1989).
We examined the effects of smoking and social disadvantage by comparing the SMR of dichotomous groups, dissimilar for smoking and for factors known to increase mortality in the general population, using χ2 analysis (Reference Breslow and DayBreslow & Day, 1987). Subjects with incomplete data were omitted from the pertinent parts of this analysis.
The effectiveness of medical care was quantified (Reference Rutstein, Berenberg and ChalmersRutstein et al, 1976) by calculating an SMR for those diseases where death is ‘avoidable’ by appropriate treatment, selected for this purpose in the Chief Medical Officer's (CMO's) annual report (Department of Health, 1994). A high SMR for a disease on this list suggests, but does not prove, substandard care.
Individual deaths were assessed by case note audit (by S.B.). Death was considered preventable when an available effective treatment was not given. Details of each death are available from the authors.
RESULTS
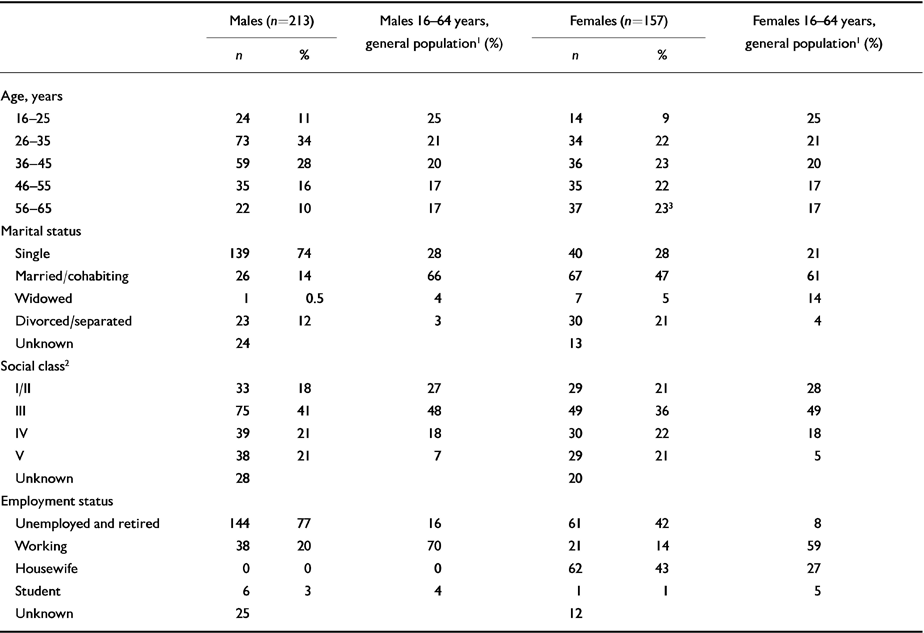
When recruited in 1981 the cohort of 370, whose illness had lasted for a mean of 12 years (range 0-39 years), comprised 213 men and 157 women. The mean age of the men was 39 years (range 19-64) and of the women 43 (range 16-66). The unmarried manual workers, and the unemployed were over-represented (Table 1) compared with the general population (Office of Population Censuses and Surveys, 1984a ). Of the 370 subjects at the census date (31 December 1994) 13 (4%) were untraced, and 79 had died (58 (73%) from natural, 19 (24%) from unnatural and two from unknown causes: these last two died in India and the Philippines).
Table 1 Demographic characteristics at cohort inception of 370 subjects with schizophrenia, compared to the general population of England and Wales
| Males (n=213) | Males 16-64 years, general population1 (%) | Females (n=157) | Females 16-64 years, general population1 (%) | |||
|---|---|---|---|---|---|---|
| n | % | n | % | |||
| Age, years | ||||||
| 16-25 | 24 | 11 | 25 | 14 | 9 | 25 |
| 26-35 | 73 | 34 | 21 | 34 | 22 | 21 |
| 36-45 | 59 | 28 | 20 | 36 | 23 | 20 |
| 46-55 | 35 | 16 | 17 | 35 | 22 | 17 |
| 56-65 | 22 | 10 | 17 | 37 | 233 | 17 |
| Marital status | ||||||
| Single | 139 | 74 | 28 | 40 | 28 | 21 |
| Married/cohabiting | 26 | 14 | 66 | 67 | 47 | 61 |
| Widowed | 1 | 0.5 | 4 | 7 | 5 | 14 |
| Divorced/separated | 23 | 12 | 3 | 30 | 21 | 4 |
| Unknown | 24 | 13 | ||||
| Social class2 | ||||||
| I/II | 33 | 18 | 27 | 29 | 21 | 28 |
| III | 75 | 41 | 48 | 49 | 36 | 49 |
| IV | 39 | 21 | 18 | 30 | 22 | 18 |
| V | 38 | 21 | 7 | 29 | 21 | 5 |
| Unknown | 28 | 20 | ||||
| Employment status | ||||||
| Unemployed and retired | 144 | 77 | 16 | 61 | 42 | 8 |
| Working | 38 | 20 | 70 | 21 | 14 | 59 |
| Housewife | 0 | 0 | 0 | 62 | 43 | 27 |
| Student | 6 | 3 | 4 | 1 | 1 | 5 |
| Unknown | 25 | 12 | ||||
All cause mortality (ICD-9 001-799 and E800-999)
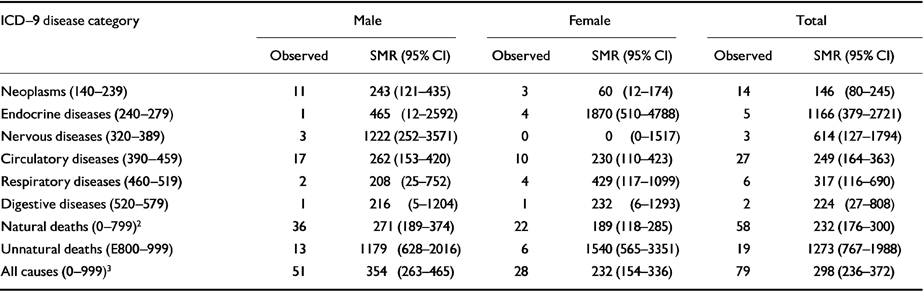
The SMR for all age groups was above the average for the general population, and fell with increasing age. The all-cause SMR was 298 (CI 236-372), a three-fold increase (Table 2), and the SMR for a first episode of illness was 248 (CI 30-896), based on two deaths out of 27 subjects.
Table 2 Cause of death (ICD-9)1 of 79 subjects with schizophrenia with observed deaths, SMRs and 95% CIs, by gender
| ICD-9 disease category | Male | Female | Total | |||
|---|---|---|---|---|---|---|
| Observed | SMR (95% CI) | Observed | SMR (95% CI) | Observed | SMR (95% CI) | |
| Neoplasms (140-239) | 11 | 243 (121-435) | 3 | 60 (12-174) | 14 | 146 (80-245) |
| Endocrine diseases (240-279) | 1 | 465 (12-2592) | 4 | 1870 (510-4788) | 5 | 1166 (379-2721) |
| Nervous diseases (320-389) | 3 | 1222 (252-3571) | 0 | 0 (0-1517) | 3 | 614 (127-1794) |
| Circulatory diseases (390-459) | 17 | 262 (153-420) | 10 | 230 (110-423) | 27 | 249 (164-363) |
| Respiratory diseases (460-519) | 2 | 208 (25-752) | 4 | 429 (117-1099) | 6 | 317 (116-690) |
| Digestive diseases (520-579) | 1 | 216 (5-1204) | 1 | 232 (6-1293) | 2 | 224 (27-808) |
| Natural deaths (0-799)2 | 36 | 271 (189-374) | 22 | 189 (118-285) | 58 | 232 (176-300) |
| Unnatural deaths (E800-999) | 13 | 1179 (628-2016) | 6 | 1540 (565-3351) | 19 | 1273 (767-1988) |
| All causes (0-999)3 | 51 | 354 (263-465) | 28 | 232 (154-336) | 79 | 298 (236-372) |
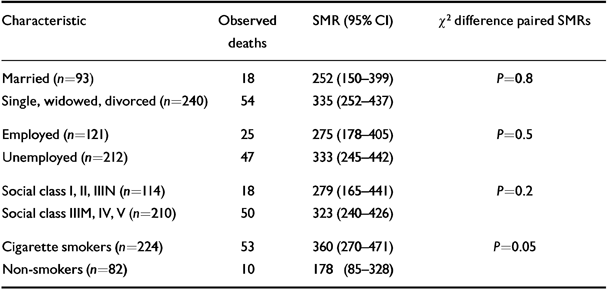
Mortality was higher in males (Table 2), and in the unemployed, the unmarried and patients from lower social classes (Table 3), but the differences in SMR did not reach statistical significance.
Table 3 Standardised mortality ratios (SMRs) for selected dichotomous risk characteristics associated with altered mortality in the general population. (Subjects with incomplete data were omitted from the pertinent part of these analyses.)
| Characteristic | Observed deaths | SMR (95% CI) | χ2 difference paired SMRs |
|---|---|---|---|
| Married (n=93) | 18 | 252 (150-399) | P=0.8 |
| Single, widowed, divorced (n=240) | 54 | 335 (252-437) | |
| Employed (n=121) | 25 | 275 (178-405) | P=0.5 |
| Unemployed (n=212) | 47 | 333 (245-442) | |
| Social class I, II, IIIN (n=114) | 18 | 279 (165-441) | P=0.2 |
| Social class IIIM, IV, V (n=210) | 50 | 323 (240-426) | |
| Cigarette smokers (n=224) | 53 | 360 (270-471) | P=0.05 |
| Non-smokers (n=82) | 10 | 178 (85-328) |
Natural cause mortality (ICD-9 001-799)
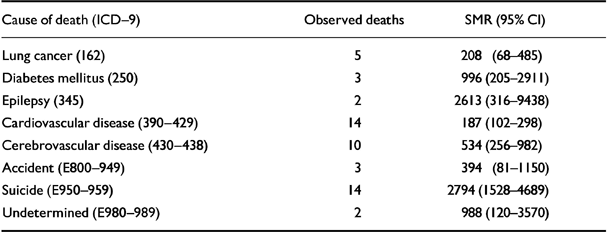
The natural cause SMR (232, CI 176-300), twice that expected, did not change significantly over the follow-up period. Death from natural causes accounted for two-thirds (63%) of the excess mortality: 80% of these deaths were from neoplastic, circulatory or respiratory disease, similar to the distribution of cause of death in the general population (Office of Health Economics, 1992). The SMRs from cerebrovascular disease, diabetes and epilepsy were much increased (Table 4).
Table 4 Standardised mortality ratios (SMRs) for causes of death with two or more deaths
| Cause of death (ICD-9) | Observed deaths | SMR (95% CI) |
|---|---|---|
| Lung cancer (162) | 5 | 208 (68-485) |
| Diabetes mellitus (250) | 3 | 996 (205-2911) |
| Epilepsy (345) | 2 | 2613 (316-9438) |
| Cardiovascular disease (390-429) | 14 | 187 (102-298) |
| Cerebrovascular disease (430-438) | 10 | 534 (256-982) |
| Accident (E800-949) | 3 | 394 (81-1150) |
| Suicide (E950-959) | 14 | 2794 (1528-4689) |
| Undetermined (E980-989) | 2 | 988 (120-3570) |
‘Avoidable’ natural deaths
The SMR (468, CI 172-1020) of those causes designated ‘avoidable’ by the CMO was increased nearly five times. Four of the six ‘avoidable’ deaths, all in people aged 35-64, were from hypertension and/or cerebrovascular disease, and two were from surgical diseases.
The SMR was significantly raised for smokers, but not for non-smokers (Table 3), and for smoking-related disease (SMR 181, CI 112-277; Royal College of Physicians, 1971). The SMR for lung cancer (208, CI 68-485) was twice the expected value.
Audit of the case notes suggested a number of mechanisms underlying the excess natural mortality.
Failed recognition of medical disease by patient or carer
A 41-year-old man died from acute pulmonary oedema shortly after leaving the casualty department, having not waited to see a doctor.
A 63-year-old woman with treatment-resistant schizophrenia and learning disability died in a rest home from acute intestinal obstruction caused by old surgical adhesions.
A 63-year-old man died alone at home from acute intestinal obstruction caused by a scrotal hernia, while on the waiting list for elective repair. He had been managed conservatively in hospital when the hernia obstructed 4 months earlier.
Failed recognition of medical disease is also a plausible explanation for some of the excess cancer mortality, as five cancers were disseminated at presentation: two, in itinerants unregistered with general practitioners (GPs), were detected at psychiatric admission.
Missed medical diagnosis
Two women, resident in long-stay psychiatric wards, died from lobar pneumonia, having been examined by a doctor shortly before death. Neither appeared particularly unwell. In neither case was pneumonia diagnosed or antibiotics prescribed.
A 57-year-old man died in hospital after a cardiac arrest. Psychiatric out-patient notes detailed increasing confusion in the 2 weeks before admission to hospital, stuporous and hypothermic. Hypothyroidism was confirmed by thyroid function tests returned after death.
Poor treatment compliance
A 55-year-old itinerant woman, with known diabetes, not registered with a GP and refusing psychiatric contact, died from diabetic ketoacidosis.
The high SMR from epilepsy, diabetes, cerebrovascular and respiratory diseases (Table 4) may also be at least partly due to poor treatment compliance.
Treatment refusal
A 61-year-old man died a year after refusing potentially curative surgery for bowel cancer. Psychiatrists found no evidence of psychosis but could not persuade him to accept surgery.
A 70-year-old woman died from dehydration after refusing food and drink following a fractured femur.
Lifestyle
A 75-year-old woman died after physicians refused life support treatment, citing poor quality of life. Her elderly husband found her agitation difficult to manage and kept her in bed, inactive and under-stimulated. Psychiatrists were unable to intervene effectively. Bed sores progressed to septicaemia and multiple organ failure.
Mortality from unnatural causes (ICD-9 E800-999)
The unnatural cause SMR was 1273 (CI 767-1988), 12 times that expected. Death from unnatural causes accounted for 33% of the excess mortality. Fourteen of the 19 unnatural deaths were due to suicide, three to accident and in two cases the causes were undetermined. The unnatural deaths occurred in the early years of follow-up: six in year one, 13 by the end of year three. Of the 14 suicides, five died in year one, 12 by the end of year five. Of the ten deaths of subjects aged below 40, nine were unnatural.
Suicide
Ten of the 14 people who committed suicide were under treatment by the psychiatric services at the time of death, three had refused treatment and one had been discharged from hospital without follow-up, 2 weeks before death. Of the ten under treatment, six were in-patients, three were out-patients, and one was a day patient. The six in-patient suicides all used violent methods. Four out-patient suicides used violent methods and four took poison.
Ten of these subjects had previously attempted suicide, five repeatedly. Five had shown evidence of distress or low mood shortly before death. One in-patient killed himself despite regular observation, and one died 2 days after observations were relaxed. None of the other victims had had a recent risk assessment. Case note scrutiny suggested that the in-patient and day patient suicides might have been prevented.
Accident
One out-patient death, from benzatropine toxicity, was probably a missed suicide. Two others, although probably accidental, appeared causally related to schizophrenia.
A 48-year-old man, a heavy smoker living with elderly parents, died of asphyxia in a bedroom fire. Depot anti-psychotic medication had been stopped after years of stability in an attempt to relieve a severe drug-induced extrapyramidal syndrome. He was readmitted because of disorganised conduct but discharged himself, against advice, a week before his death.
A 64-year-old man with mainly negative symptoms, compliant with medication and living quietly in a group home, was found dead from hypothermia in a forest 20 miles away, to which he had apparently walked.
Undetermined cause of death
One undetermined death was probably a suicide. A 55-year-old man with a history of treatment-resistant schizophrenia, substance misuse and attempted suicide died from a self-administered overdose of amitriptyline, which he took at home after absconding from hospital.
The other ‘undetermined’ death was of a 40-year-old man, who died without further psychiatric contact 3 years after recruitment into the study, from a fall or jump from his flat, and this drew an explicit comment from the coroner that there was ‘insufficient evidence of intent to determine causality’.
DISCUSSION
We will discuss the influence of error on the findings, then the findings themselves.
Selection bias
The inclusion criteria were similar to those in most comparable cohorts. The largest source of bias probably came from the use of a prevalence rather than an incidence cohort. This meant that at recruitment, 343 (93%) subjects had already survived the period of greatest excess mortality (Reference Mortensen and JuelMortensen & Juel, 1993). Most were already middle-aged and again at lower risk (Reference BrownBrown, 1997).
Forty-seven potential subjects, who were long-stay hospital patients in 1981 (Reference Gibbons, Horn and PowellGibbons et al, 1984), probably with a relatively low SMR (Reference BrownBrown, 1997), were excluded as they could not be reliably identified. The cohort was further unrepresentative of the local population with schizophrenia in that it excluded patients who were not in contact with the psychiatric services during the index year, those with unrecognised schizophrenia and those with significant drug or alcohol misuse.
Most patients who avoid contact with specialist mental health services for a year will be well and therefore at low risk of premature death. Most with unrecognised schizophrenia probably have early disease and a high SMR (Reference Mortensen and JuelMortensen & Juel, 1993). Patients with comorbid substance misuse also have a high SMR (Reference Harris and BarracloughHarris & Barraclough, 1998). The net effect of these sources of bias was probably to underestimate disease SMR.
Follow-up
We checked with GPs, other health professionals, family and friends to find out whether subjects were dead or alive. Death certificates were matched to National Health Service (NHS) central records, using family and given name, date and place of birth, place of death and NHS number (where we knew it). The matches were then verified, the available detail suggesting that matches were correct. Completeness of follow-up was unexceptional compared to similar studies (Reference Anderson, Connelly and JohnstoneAnderson et al, 1991; Reference Kelly and MacewanKelly et al, 1998).
The causes of death are probably more accurate than one would find in a sample of the general population, as the rates of post-mortem examination (62 and 22%), and coroner's inquests (25 and 3.5%) were many times higher (Home Office Statistical Bulletin, 1994). These rates are explained by the large number of deaths referred to the coroner, either because they were unnatural (n=19) or because no medical officer had seen the deceased in their final illness (n=30).
Statistical analysis
Mortality rates in the south of England are lower than the average for England and Wales (Office of Population Censuses and Surveys, 1996); hence the use of national reference data will have underestimated SMRs.
Calculation of an ‘avoidable’ natural SMR followed the procedure used in the CMO's annual report. Designed to give a rough measure of the quality of medical treatment, this analysis is based on deaths from selected common diseases for which effective treatment is available. It misses potentially preventable deaths from rarer causes, and deaths where the immediate (though not the underlying) cause was treatable, and therefore probably underestimates avoidable mortality.
Smoking histories, obtained from initial case records, may have been unreliable and may have changed over the course of the study. Our results probably followed general population surveys in underestimating the prevalence of cigarette smoking (Reference Bennett, Dodd and FlatleyBennett et al, 1995) and thereby its effect on mortality.
Care assessment
We obtained hospital case notes on all but the two patients who died abroad. Case note audit was retrospective and subject to recorder and investigator bias. Designation of individual deaths as preventable was subjective and conservative; vignettes were chosen to illustrate points rather than as measures of the prevalence of particular mechanisms. We cannot know whether anyone would have survived with better treatment or whether the prevalence of such events differs from that in the general population.
Overall mortality
The SMR was higher than in any previous published cohort of subjects measured at varying points in a schizophrenic illness (Reference BrownBrown, 1997); however, the cohort was relatively small and some SMRs have wide confidence intervals. Previous studies do not contain enough clinical data to know whether the high mortality might be explained by selection or methodology. As in previous studies, about two-thirds of the extra deaths were from natural causes (Reference BrownBrown, 1997).
Kendler's study of twins suggests that most unnatural deaths of subjects with schizophrenia are from suicide, while the pattern of natural mortality is best explained by altered exposure to environmental risk factors (Reference KendlerKendler, 1986). The non-significant variation of SMR with social class, employment and marital status supports previous suggestions from mixed diagnostic cohorts (Reference Babigian and OdoroffBabigian & Odoroff, 1969; Reference BaxterBaxter, 1996) that social disadvantage explains only a small part of the excess mortality. This conclusion requires qualification, as many subjects had declined in the social scale during the follow-up years, and hence analysis, based on status at the outset, probably accentuated differences.
The causes of death were similar to those seen in similar cohorts (Reference Lesage, Trapani and TansellaLesage et al, 1990; Reference Anderson, Connelly and JohnstoneAnderson et al, 1991). Two subjects who died in status epilepticus may have had brain pathology which caused both epilepsy and schizophrenia. No other deaths appeared likely to be due to misclassified organic psychosis. Bronchopneumonia was a particularly common terminal event, usually associated with the underlying pathology. As reference mortality statistics are based on the underlying rather than the immediate cause of death (World Health Organization, 1977), we do not know whether this finding is significant.
‘Preventable’ natural mortality
Analysis of case notes suggests that improved recognition of acute medical disease, better treatment of chronic medical disease and better treatment compliance might prevent some deaths. The vignettes also suggest that some of the ‘avoidable’ deaths would in practice have been very difficult to prevent. Doctors' ability to supervise treatment is limited, while competent patients are entitled to refuse optimal treatment.
Unhealthy lifestyles
Our study suggests that most of the excess natural mortality of modern community samples is due to cigarette smoking, and that helping patients to stop smoking should be a priority for doctors and health service planners. Psychiatrists rarely discuss patients' smoking (Reference Lawrie, Buckley and UlyattLawrie et al, 1995), despite evidence that programmes to help stop smoking can be effective in schizophrenia (Reference Ziedonis and GeorgeZiedonis & George, 1997).
Many patients with schizophrenia eat poor diets and are obese (Reference McCreadie, Macdonald and BlacklockMcCreadie et al, 1998). We did not have the information to assess if diet, self-care and exercise affected the mortality of our subjects. However, when interviewed in 1996, survivors were eating a poor diet and taking little exercise (Reference Brown, Birtwistle and RoeBrown et al, 1999). If survivors were selected for health, then the deceased probably also had unhealthy lifestyles. No deaths were directly due to drug or alcohol misuse, but it must be remembered that the original study criteria excluded patients with significant substance misuse.
Psychiatric treatment
No deaths were unequivocally due to psychiatric treatments. Neuroleptic drugs may have contributed to the death from aspiration pneumonia of a 62-year-old woman with cerebrovascular disease. Similar deaths were noted by both Lesage et al (Reference Lesage, Trapani and Tansella1990) and Anderson et al (Reference Anderson, Connelly and Johnstone1991), a striking finding considering the size of the cohorts. Neuroleptic drugs may also exacerbate diabetes, epilepsy and chronic respiratory disease (Reference Mortensen and JuelMortensen & Juel, 1990).
Unnatural mortality
The unnatural mortality rate was significantly increased. As in other series, most unnatural deaths were from suicide (Reference BrownBrown, 1997), though accidental and undetermined deaths were also increased.
Suicide
The high, but not exceptional, suicide mortality of the Southampton cohort is not explained by its socio-demographic composition. The characteristics of the victims and circumstances of death fit broadly with previous findings, but the numbers were too small for reliable statistical analysis. The high proportion of early in-patient suicides (Reference Barner-RasmussenBarner-Rasmussen, 1986; Reference Heilä, Isometsä and HenrikssonHeilä et al, 1997) may have been due to clustering around psychiatric contact. It may on the other hand reflect the unsettling effects of moving from the area mental hospital to a new non-purpose-built unit in the grounds of an inner-city district general hospital (DGH) shortly before the cohort was first enrolled. Staff had no previous experience of running a DGH unit, and there were probably too few beds.
Case notes suggest that one of four suicides, not in contact with psychiatric services, might have been re-engaged by a more assertive approach. The Care Programme Approach (CPA) might have prevented the suicide of a patient who was discharged from hospital without follow-up. It is unrealistic to expect to prevent all suicides in those with schizophrenia, as some occurred without warning or among patients who rejected psychiatric contact.
Recommendations
Psychiatry, as a branch of medicine, should aim to treat disease. Mortality, the most objective measure of disease outcome and effectiveness of medical treatment, should continue to be monitored, to assess the impact of national policy changes and the performance of local units. Further large, prospective cohort studies are needed to examine the mortality from specific causes and to test hypotheses about aetiology. Individual follow-up studies are needed to identify treatment deficiencies and suggest improvements in clinical practice.
Our findings suggest that most of the excess mortality of schizophrenia can be explained by known mechanisms, and hence should be susceptible to currently available interventions. In particular, psychiatrists should ensure that they maintain their diagnostic skills, and mental health services should be assertive in addressing patients' smoking, alcohol use, diet and other lifestyle factors.
Whether psychiatrists or GPs are best placed to treat medical disease in the seriously mentally ill is uncertain; however, the responsibility for medical treatment should be explicitly allocated. Doctors should consider regular physical examinations of people who might fail to recognise that they were ill and to seek treatment. They should also consider invoking the Mental Health Act when patients' mental state is seriously jeopardising their physical health.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Many of the excess deaths of patients with schizophrenia are potentially preventable by better medical treatment and risk management.
-
▪ The mechanisms of excess natural mortality include unhealthy lifestyle, especially cigarette smoking, failed recognition and poor treatment of medical disease, and poor treatment compliance.
-
▪ Some of the factors which contribute to the excess mortality of schizophrenia are not susceptible to medical intervention. We should nevertheless aim to reduce mortality to a level as close as possible to that of the general population.
LIMITATIONS
-
▪ We describe the experience of a small cohort of mostly middle-aged subjects, originally recruited nearly 20 years ago. These results may not generalise to younger or more recent patients or to different services.
-
▪ Excluding potential subjects with alcohol or drug misuse probably led to an underestimate of substance-related pathology.
-
▪ Care assessment was by retrospective case note examination, and subject to recorder and investigator bias.
ACKNOWLEDGEMENTS
We thank Mrs Jane Gibbons and Professor James Gibbons for comments on the manuscript and foresight in preserving the study records. Sheeley Hutton and Paul Winter of the Medical Research Council Environmental Epidemiology Unit assisted in the calculation of the SMRs; colleagues in the Mental Health Group, University of Southampton advised on the study and the manuscript.









eLetters
No eLetters have been published for this article.