Deliberate self-harm (DSH) is becoming more common (Reference Hawton, Fagg and SimkinHawton et al, 1997; Reference Kapur, House and CreedKapur et al, 1998) and is associated with significant risk of suicide (Reference Hawton and FaggHawton & Fagg, 1988; Reference Nordentoft and RubinNordentoft & Rubin, 1993). Deliberate self-harm occurs for diverse reasons, one important factor being psychiatric disorder. Earlier studies in the UK suggested less psychiatric disorder in self-poisoning patients (Reference Newson-Smith and HirschNewson-Smith & Hirsch, 1979; Reference Urwin and GibbonsUrwin & Gibbons, 1979) than in suicides (Reference Barraclough, Bunch and NelsonBarraclough et al, 1974). More recent studies of DSH from other countries have reported high rates of psychiatric disorder (Reference Ennis, Barnes and KennedyEnnis et al, 1989; Reference Beautrais, Joyce and MulderBeautrais et al, 1996; Reference Suominen, Henriksson and SuokasSuominen et al, 1996; Reference Ferreira de Castro, Cunha and PimentaFerreira de Castro et al, 1998) which resemble those found in suicides (Reference Barraclough, Bunch and NelsonBarraclough et al, 1974; Reference Foster, Gillespie and McClellandFoster et al, 1997). Comorbidity of psychiatric disorders was common in those studies (Reference Beautrais, Joyce and MulderBeautrais et al, 1996; Reference Suominen, Henriksson and SuokasSuominen et al, 1996; Reference Ferreira de Castro, Cunha and PimentaFerreira de Castro et al, 1998). Personality disorders were also frequent (Reference Ennis, Barnes and KennedyEnnis et al, 1989; Reference Suominen, Henriksson and SuokasSuominen et al, 1996; Reference Ferreira de Castro, Cunha and PimentaFerreira de Castro et al, 1998), although few studies have used standardised measures of personality. In this study we used a structured clinical interview and a standardised instrument to investigate the nature and prevalence of psychiatric and personality disorder in a representative sample of DSH patients in the UK.
METHOD
Subjects
The subjects were patients aged 15 years and over who presented to the district general hospital in Oxford following an episode of DSH between 10 February and 1 December 1997. The definition of DSH was as for ‘parasuicide’ in the WHO/Euro Multi-Centre Study on Parasuicide, namely
“an act with non-fatal outcome in which an individual deliberately initiates a non-habitual behaviour, that without intervention from others will cause self-harm, or deliberately ingests a substance in excess of the prescribed or generally recognised dosage, and which is aimed at realising changes that the person desires via the actual or expected physical consequences” (Reference Platt, Bille-Brahe and KerkhofPlatt et al, 1992).
Thus, the definition of DSH included acts of self-poisoning and self-injury, but excluded acts of self-cutting which were part of a repetitive pattern of self-mutilation. Patients were excluded from the study if they were under the age of 15 years, lived outside the Oxford district or were unable to understand or otherwise participate in the study (e.g. medically unfit, severe learning disabilities, severe disturbance of mental state, organic brain syndrome).
The potential sample included all DSH patients who presented to the hospital and were medically fit to be interviewed on recruitment days, which included both weekdays and weekends to ensure the patient sample was distributed throughout the week. The majority of DSH patients (approximately three-quarters) who present to the general hospital in Oxford are assessed by the general hospital psychiatric service (Reference Hawton, Fagg and SimkinHawton et al, 1997). However, efforts were made to recruit patients who had not been seen by the service. Patients were approached in hospital by a member of the research team, generally following assessment by the psychiatric staff. If the patient was discharged before they could be approached, they were sent a letter, which was followed-up by a telephone call. Of 217 patients approached, 150 (69.1%) agreed to participate in the study. The reasons for non-participation (n=67) were: refused (n=42); did not reply to the contact letter (n=16); and agreed, but did not attend the appointment (n=9). The timing of the interviews in relation to the index episode of DSH was within 24 hours (n=4); 1-2 days (n=68); 3-7 days (n=35); 1 week to 1 month (n=39) and >1 month (n=4).
The study sample was compared with all other patients who presented to the hospital during the study period using data from the Oxford Monitoring System for Attempted Suicide, which is used to collect information on all DSH patients presenting to the general hospital, irrespective of whether or not they are assessed by the psychiatric service (Reference Hawton, Fagg and SimkinHawton et al, 1997).
Research instruments
European Parasuicide Study Interview Schedule
The schedule used in the WHO/Euro Multicentre Study on Parasuicide (Reference Kerkhof, Bernasco and Bille-BraheKerkhof et al, 1989) was administered. The schedule includes the following areas of inquiry: demographic, circumstances of current and previous episodes of DSH, life events, social support, contact with health professionals and physical and mental health.
ICD-10 Diagnostic Schedule
The duration and nature of current and past psychiatric symptoms were recorded using a structured interview schedule, based strictly on ICD-10 research diagnostic criteria (World Health Organization, 1993), which was developed by our group (Reference Hawton, Simkin and MalmbergHawton et al, 1998). The assessment was made according to the patient's self-report of symptoms during the period leading up to the index episode of DSH, and observation of the patient during the interview. For each category of disorder the patients were asked screening questions (essential for a diagnosis). Where there was a positive response to one or more of the screening questions, these were followed by the full list of research criteria for the specific diagnosis as listed in ICD-10. The research interviewers were trained by a medical psychiatric researcher who was very experienced in diagnostic interviewing and one researcher who also had previous experience of such interviewing.
Personality Assessment Schedule
Personality was assessed using the self-report version of the Personality Assessment Schedule (PAS) (Reference Tyrer, Alexander, Ferguson and TyrerTyrer et al, 1988), updated according to ICD-10 criteria (World Health Organization, 1993) by Tyrer and colleagues. Ratings within each personality area were classified according to Tyrer et al's (Reference Tyrer, Alexander, Ferguson and Tyrer1988) scheme, where a rating of seven or more indicated personality disorder and a rating of 4-6 trait accentuation. The PAS was completed at the follow-up interview (see below). This allowed us to assess personality when psychiatric disorder was likely to be less prominent (Reference ZimmermanZimmerman, 1994).
Consensus meeting and reliability of ratings
The research team identified psychiatric diagnoses at consensus meetings based on the information obtained from the structured diagnostic interview schedule. In a small number of cases with complex psychiatric histories, psychiatric case notes were examined to aid clarification of the diagnoses. In order to assess reliability, two psychiatrists working on the project independently reviewed the information obtained from the diagnostic interview for 20 cases. One of the psychiatrists made 32 diagnoses. The second psychiatrist was in agreement with all of these diagnoses (F code whole numbers), but also made three further diagnoses. Thus, the overall agreement was 91.4%.
Follow-up interview
Follow-up interviews (n=118) were conducted approximately 12-16 months after the index episode of DSH in 111 cases (94.1%) and between 17-20 months in seven cases (5.9%).
Statistical analyses
The analyses were conducted using the Statistical Package for the Social Sciences (SPSS, 1999) and EpiInfo (Reference Dean, Dean and CoulombierDean et al, 1994). The statistical tests employed were the χ2 (with Yates' correction, where appropriate) and Mann—Whitney U-tests.
RESULTS
Sample
Initial interview
Of the 150 patients included in the study, 92 (61.3%) were female and 58 (38.7%) were male. The majority of patients were Caucasian (97.3%). The social class distribution of the study sample was I and II (16.7%), IIIM and IIINM (35.3%), IV and V (33.3%), armed forces (2.0%) and students (12.7%). Ninety-eight patients (65.3%) were known to have carried out a previous episode of DSH (this includes episodes not resulting in hospital referral). The study sample was representative of the total DSH population which presented to the general hospital during the study period in terms of age, gender, previous history of DSH and whether they were currently in psychiatric care. Patients included in the study were more likely to have self-poisoned (94.0% v. 84.7%; χ2=7.97, P<0.01). This difference is likely to be due to the exclusion of patients who habitually cut themselves from the study as they did not fall within the WHO/Euro Multi-Centre Study definition of DSH.
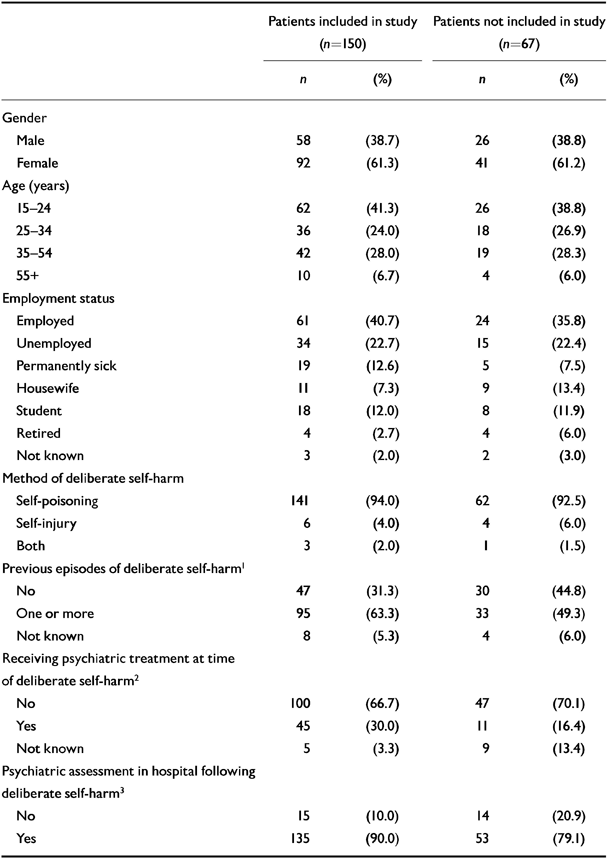
The study sample was also compared with the remaining DSH patients who were approached to be in the study using data from the Oxford Monitoring System for Attempted Suicide in order to ensure the same source of data. The study sample did not differ from the non-included DSH patients in terms of age, gender and employment status. Somewhat more of the included patients had a previous history of DSH and were in psychiatric treatment as the time of the index attempt, although neither difference was statistically significant (see Table 1). Patients who participated in the study were more likely to have been assessed by a member of the hospital psychiatric staff.
Table 1 Comparison of recruited patients with the remainder of potential patients
| Patients included in study (n=150) | Patients not included in study (n=67) | |||
|---|---|---|---|---|
| n | (%) | n | (%) | |
| Gender | ||||
| Male | 58 | (38.7) | 26 | (38.8) |
| Female | 92 | (61.3) | 41 | (61.2) |
| Age (years) | ||||
| 15-24 | 62 | (41.3) | 26 | (38.8) |
| 25-34 | 36 | (24.0) | 18 | (26.9) |
| 35-54 | 42 | (28.0) | 19 | (28.3) |
| 55+ | 10 | (6.7) | 4 | (6.0) |
| Employment status | ||||
| Employed | 61 | (40.7) | 24 | (35.8) |
| Unemployed | 34 | (22.7) | 15 | (22.4) |
| Permanently sick | 19 | (12.6) | 5 | (7.5) |
| Housewife | 11 | (7.3) | 9 | (13.4) |
| Student | 18 | (12.0) | 8 | (11.9) |
| Retired | 4 | (2.7) | 4 | (6.0) |
| Not known | 3 | (2.0) | 2 | (3.0) |
| Method of deliberate self-harm | ||||
| Self-poisoning | 141 | (94.0) | 62 | (92.5) |
| Self-injury | 6 | (4.0) | 4 | (6.0) |
| Both | 3 | (2.0) | 1 | (1.5) |
| Previous episodes of deliberate self-harm1 | ||||
| No | 47 | (31.3) | 30 | (44.8) |
| One or more | 95 | (63.3) | 33 | (49.3) |
| Not known | 8 | (5.3) | 4 | (6.0) |
| Receiving psychiatric treatment at time of deliberate self-harm2 | ||||
| No | 100 | (66.7) | 47 | (70.1) |
| Yes | 45 | (30.0) | 11 | (16.4) |
| Not known | 5 | (3.3) | 9 | (13.4) |
| Psychiatric assessment in hospital following deliberate self-harm3 | ||||
| No | 15 | (10.0) | 14 | (20.9) |
| Yes | 135 | (90.0) | 53 | (79.1) |
Follow-up interview
A total of 118 patients (78.7%) were interviewed at follow-up. Of those who were not interviewed, 10 refused, 14 could not be contacted, seven agreed but did not attend and one committed suicide during the follow-up period. The PAS was completed for 111 patients at follow-up. PAS scores were not obtained for two patients who were too mentally unwell to provide reliable information, nor for five who did not complete the follow-up interview. There was no difference between those for whom the PAS was completed and those where this was not possible with respect to gender, method of DSH, previous self-harm and psychiatric disorder at the time of the index attempt. However, those who were followed-up were somewhat younger (median 26.5 years v. 32.0, U=1448, P<0.05).
Psychiatric disorders
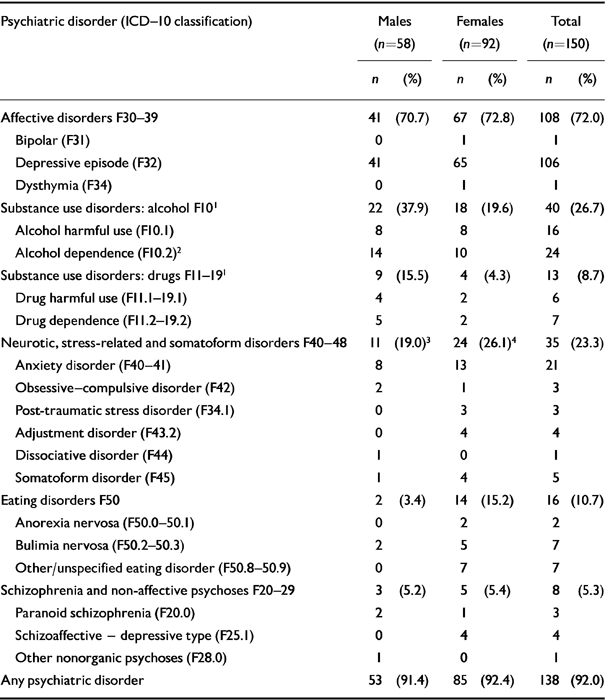
At the time of the index episode of DSH, 138 patients (92.0%) were diagnosed with at least one psychiatric disorder (see Table 2). A single psychiatric disorder was found in 68 patients (45.3%), two disorders in 55 (36.7%) and three or more in 15 (10.0%). Hence, comorbidity of two or more psychiatric disorders was present in 70 cases (46.7%). There was no gender difference in the frequency of comorbidity of psychiatric disorders. Of the 12 patients (8.0%) without a current psychiatric disorder, four had a past history of psychiatric disorder.
Table 2 Psychiatric disorders at time of index episode of deliberate self-harm
| Psychiatric disorder (ICD-10 classification) | Males (n=58) | Females (n=92) | Total (n=150) | |||
|---|---|---|---|---|---|---|
| n | (%) | n | (%) | n | (%) | |
| Affective disorders F30-39 | 41 | (70.7) | 67 | (72.8) | 108 | (72.0) |
| Bipolar (F31) | 0 | 1 | 1 | |||
| Depressive episode (F32) | 41 | 65 | 106 | |||
| Dysthymia (F34) | 0 | 1 | 1 | |||
| Substance use disorders: alcohol F101 | 22 | (37.9) | 18 | (19.6) | 40 | (26.7) |
| Alcohol harmful use (F10.1) | 8 | 8 | 16 | |||
| Alcohol dependence (F10.2)2 | 14 | 10 | 24 | |||
| Substance use disorders: drugs F11-191 | 9 | (15.5) | 4 | (4.3) | 13 | (8.7) |
| Drug harmful use (F11.1-19.1) | 4 | 2 | 6 | |||
| Drug dependence (F11.2-19.2) | 5 | 2 | 7 | |||
| Neurotic, stress-related and somatoform disorders F40-48 | 11 | (19.0)3 | 24 | (26.1)4 | 35 | (23.3) |
| Anxiety disorder (F40-41) | 8 | 13 | 21 | |||
| Obsessive-compulsive disorder (F42) | 2 | 1 | 3 | |||
| Post-traumatic stress disorder (F34.1) | 0 | 3 | 3 | |||
| Adjustment disorder (F43.2) | 0 | 4 | 4 | |||
| Dissociative disorder (F44) | 1 | 0 | 1 | |||
| Somatoform disorder (F45) | 1 | 4 | 5 | |||
| Eating disorders F50 | 2 | (3.4) | 14 | (15.2) | 16 | (10.7) |
| Anorexia nervosa (F50.0-50.1) | 0 | 2 | 2 | |||
| Bulimia nervosa (F50.2-50.3) | 2 | 5 | 7 | |||
| Other/unspecified eating disorder (F50.8-50.9) | 0 | 7 | 7 | |||
| Schizophrenia and non-affective psychoses F20-29 | 3 | (5.2) | 5 | (5.4) | 8 | (5.3) |
| Paranoid schizophrenia (F20.0) | 2 | 1 | 3 | |||
| Schizoaffective — depressive type (F25.1) | 0 | 4 | 4 | |||
| Other nonorganic psychoses (F28.0) | 1 | 0 | 1 | |||
| Any psychiatric disorder | 53 | (91.4) | 85 | (92.4) | 138 | (92.0) |
Affective disorders
Affective disorder was present in 108 patients (72.0%). A depressive episode was present in 106 patients (70.7%). Of the depressive episodes, 50 (47.2%) were severe/psychotic, 45 (42.5%) moderate, three (2.8%) mild and eight (7.5%) other/unspecified. There were no gender differences in the presence or severity of a depressive episode. Of those with a depressive episode, the length of the current episode was 2-4 weeks in 17 cases (16.0%), 2-6 months in 38 (35.9%), 7-12 months in 18 (17.0%) and > 1 year in 32 (30.2%). It was not possible to ascertain the duration in one case. There was a past history of depressive episodes in 41 (38.7%) of those with a current diagnosis of depression and in seven patients (4.7%) without a diagnosis of depression. In addition to the patients with depressive disorders, one patient had dysthymia and another had a bipolar affective disorder which appeared to be in remission.
Disorders with prominent depressive symptoms (depressive episode, F32; dysthymia, F34; schizoaffective disorder—depressive type, F25.1; mixed anxiety and depressive disorder, F41.2; adjustment disorder with depressive symptoms, F43.2) were present in 117 cases (78%).
Substance use disorders
Alcohol dependence or harmful use was present in 40 patients (26.7%). Male patients were significantly more likely to suffer from alcohol dependence or harmful use than female patients (χ2=5.23, P<0.05). Four males were suffering from both alcohol dependence and alcoholic hallucinosis (F10.52). A past history of alcohol dependence or harmful use was present in a further nine patients.
Drug misuse or dependence was present in 13 patients (8.7%) and a further four patients (2.7%) had a past history but no current drug misuse. The most common forms of drug dependency were of heroin (three cases) and benzodiazepines (three cases).
Neurotic, stress-related and somatoform disorders
Twenty-one patients (14.0%) had an anxiety disorder. The most common anxiety disorder was social phobia (n=9, 6.0%) followed by agoraphobia (n=6, 4.0%). Other anxiety disorders present included: generalised anxiety (n=2); mixed anxiety and depression (n=2) and panic disorder (n=1). One patient had an isolated specific phobia and no other psychiatric disorder. No significant gender differences were found in the prevalence of anxiety disorders. Three patients (2.0%) had obsessive—compulsive disorder. Adjustment reactions (n=4, 2.7%) were uncommon. Three patients (2.0%), all female, had post-traumatic stress disorder. One patient had dissociative convulsions. Five patients (3.3%) had somatoform disorders, most commonly somatisation disorder (n=3, 2.0%).
Eating disorders
Eating disorders were present in 16 patients (10.7%), with female patients predominating (χ2=4.01, P<0.05). A past history of an eating disorder was found in nine female patients (6.0%) who did not have a current eating disorder.
Schizophrenia, schizotypal and delusional disorders
Three patients had a diagnosis of schizophrenia. One patient who appeared to be developing a schizophrenic illness was classified as suffering from an ‘other non-organic psychosis’ as the symptoms did not meet the diagnostic criteria for schizophrenia. Four patients (all female) had a schizoaffective illness. Four patients had florid positive psychotic symptoms and four had no positive symptoms. Four were also markedly depressed.
Psychotic symptoms (schizophrenia, F20; schizoaffective disorder, F25; psychotic depression, F32.3; alcoholic hallucinosis, F10.5; and other non-organic psychoses, F28) were present in 14 patients (9.3%).
Conduct disorders
Three patients were diagnosed with conduct disorder, which was 11.5% of those aged 18 years and under.
Personality disorders
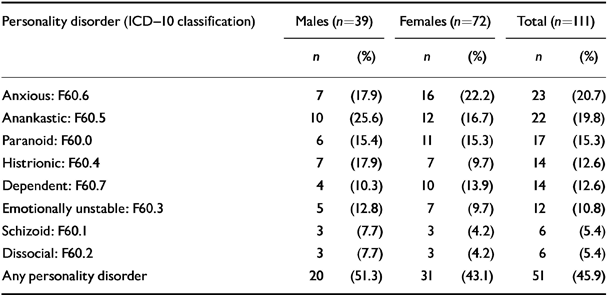
At follow-up the PAS was administered to 74.0% of the original cohort (n=111). Personality disorders were present in 51 cases (45.9%) (see Table 3). Nineteen patients (17.1%) met criteria for one personality disorder, 15 (13.5%) for two and 17 (15.3%) for three or more. The most common disorders were anxious, anankastic and paranoid. Personality trait accentuation was present in 37 patients (33.3%) without a personality disorder. There was no gender difference in the presence or type of personality disorder.
Table 3 Personality disorders at time of follow-up interview
| Personality disorder (ICD-10 classification) | Males (n=39) | Females (n=72) | Total (n=111) | |||
|---|---|---|---|---|---|---|
| n | (%) | n | (%) | n | (%) | |
| Anxious: F60.6 | 7 | (17.9) | 16 | (22.2) | 23 | (20.7) |
| Anankastic: F60.5 | 10 | (25.6) | 12 | (16.7) | 22 | (19.8) |
| Paranoid: F60.0 | 6 | (15.4) | 11 | (15.3) | 17 | (15.3) |
| Histrionic: F60.4 | 7 | (17.9) | 7 | (9.7) | 14 | (12.6) |
| Dependent: F60.7 | 4 | (10.3) | 10 | (13.9) | 14 | (12.6) |
| Emotionally unstable: F60.3 | 5 | (12.8) | 7 | (9.7) | 12 | (10.8) |
| Schizoid: F60.1 | 3 | (7.7) | 3 | (4.2) | 6 | (5.4) |
| Dissocial: F60.2 | 3 | (7.7) | 3 | (4.2) | 6 | (5.4) |
| Any personality disorder | 20 | (51.3) | 31 | (43.1) | 51 | (45.9) |
Comorbidity of psychiatric and personality disorders
Of the 111 patients for which both psychiatric and personality assessments were completed, comorbidity of psychiatric and personality disorders was present in 49 cases (44.1%). Of the 51 patients with a personality disorder, only two did not have a current psychiatric disorder. The frequency of comorbidity of psychiatric and personality disorders did not differ markedly between the two genders.
DISCUSSION
In a representative sample of DSH patients presenting to a general hospital in the UK, we found a high prevalence of both psychiatric (92.0%) and personality (45.9%) disorders, the most common psychiatric disorders being depression, substance use and anxiety disorders. The rates of psychiatric disorder found in this study are considerably higher than those reported in older UK studies which used systematic screening instruments (Reference Newson-Smith and HirschNewson-Smith & Hirsch, 1979; Reference Urwin and GibbonsUrwin & Gibbons, 1979). The rates and profile of psychiatric disorders in this study are more similar to those reported by UK studies of completed suicides (Reference Barraclough, Bunch and NelsonBarraclough et al, 1974; Reference Foster, Gillespie and McClellandFoster et al, 1997). One potential reason for the difference between the findings of this study and those from the 1970s might be a change in the characteristics of the DSH population over time. It is also possible that the use of a structured diagnostic schedule may have resulted in the over-diagnosis of mental disorders in suggestible patients. However, the extent of documented past psychiatric disorder suggests that such an effect, if present, would be small. In addition, discrepancies between the frequency of psychiatric diagnoses in DSH patients based on research interviews and those made in routine clinical consultations have also been reported by Suominen et al (Reference Suominen, Isometsa and Henriksson1999). They found significantly higher rates of depression, alcohol dependence/abuse and comorbidity of psychiatric disorders following research interviews in comparison to routine consultations. They concluded that this finding has important implications for clinical practice. Furthermore, recent studies from other countries have reported similar rates of psychiatric disorders in DSH patients to those found in this study (Reference Ennis, Barnes and KennedyEnnis et al, 1989, 85%; Reference Suominen, Henriksson and SuokasSuominen et al, 1996, 98%; Reference Gupta and TrzepaczGupta & Trzepacz, 1997, 96%; Reference Ferreira de Castro, Cunha and PimentaFerreira de Castro et al, 1998, 86%). Multiple psychiatric disorders were present in nearly half of our sample, which is similar to the findings of Suominen et al (Reference Suominen, Henriksson and Suokas1996).
Psychiatric disorders
We found depression to be by far the most common psychiatric diagnosis, with 70.7% of patients reaching ICD-10 criteria for a depressive episode. Surprisingly, nearly half the depressive episodes were severe or psychotic. Our findings replicate those of Suominen et al (Reference Suominen, Henriksson and Suokas1996), who diagnosed 66.7% of patients with either major depression or depression not otherwise specified, and Beautrais et al (Reference Beautrais, Joyce and Mulder1996), who diagnosed 61.9% with major depression, but are somewhat higher than the rates in other studies (Reference Ennis, Barnes and KennedyEnnis et al, 1989, 31.0%; Reference Gupta and TrzepaczGupta & Trzepacz, 1997; 37.2%). Our low prevalence figure for adjustment disorder (2.7%) is in keeping with the findings of Suominen et al (Reference Suominen, Henriksson and Suokas1996) (3.0%) and Ennis et al (Reference Ennis, Barnes and Kennedy1989) (9.9%), but is lower than that found in other studies (Reference Gupta and TrzepaczGupta & Trzepacz, 1997, 35.8%; Reference Ferreira de Castro, Cunha and PimentaFerreira de Castro et al, 1998, 15.7%).
This study found alcohol dependence and harmful use to be the second most common psychiatric diagnosis (26.7%), but it was not as common as in the Finnish study of Suominen et al (Reference Suominen, Henriksson and Suokas1996) (53.5%) or in the Canadian study of Ennis et al (Reference Ennis, Barnes and Kennedy1989) (33.8%). We found a lower prevalence of drug misuse and dependence (8.7%) than Suominen et al (Reference Suominen, Henriksson and Suokas1996) (12.3%) and Ennis et al (Reference Ennis, Barnes and Kennedy1989) (23.9%). Anxiety disorders were fairly common (14.0%) and of similar frequency to that reported by Suominen et al (Reference Suominen, Henriksson and Suokas1996) (17.5%). The prevalence of eating disorders in this study (10.7%) is much higher than that reported in other studies of DSH patients, for example Ennis et al (Reference Ennis, Barnes and Kennedy1989) and Suominen et al (Reference Suominen, Henriksson and Suokas1996) did not diagnose eating disorders in any of their patients. Schizophrenia and schizoaffective disorder were uncommon in this study, which is similar to the findings of other investigations.
Between-study comparisons with respect to the prevalence of psychiatric disorders are complicated by the use of different diagnostic classifications. We used ICD-10 criteria whereas most other studies have used versions of the DSM classification (Reference Ennis, Barnes and KennedyEnnis et al, 1989; Reference Beautrais, Joyce and MulderBeautrais et al, 1996; Reference Suominen, Henriksson and SuokasSuominen et al, 1996; Reference Gupta and TrzepaczGupta & Trzepacz, 1997; Reference Ferreira de Castro, Cunha and PimentaFerreira de Castro et al, 1998). The main implication for using different diagnostic classifications is the lower threshold for an adjustment disorder diagnosis in DSM and a lower threshold for a mild depressive diagnosis in ICD-10. It is unlikely, however, that our finding of a high prevalence of depressive disorder and a low prevalence of adjustment disorder is due to misdiagnosis because the majority of depressive episodes were moderate or severe (88.7%) and the duration of the depressive symptoms was longer than two months in 83.0% of cases.
Comparison with other studies is further hindered by most having included selected samples. For example, although Suominen et al (Reference Suominen, Henriksson and Suokas1996) in Finland had a systematic approach to identifying suitable patients, only 28% of the patients invited to participate were interviewed. Ennis et al (Reference Ennis, Barnes and Kennedy1989) in Canada studied only those patients who were admitted to an in-patient psychiatric crisis unit. Patients who were not admitted or who were admitted to other psychiatric units were not included, although they constituted nearly three-quarters of the DSH patients. Both Beautrais et al (Reference Beautrais, Joyce and Mulder1996) in New Zealand and Gupta & Trzepacz (Reference Gupta and Trzepacz1997) in the USA included only patients who had made a medically serious suicide attempt. Ferreira de Castro et al (Reference Ferreira de Castro, Cunha and Pimenta1998) studied patients who were attending a suicide prevention facility, but it is unclear how patients were recruited or what proportion agreed to be interviewed.
In the present study there was a relatively high acceptance rate for interview (69.1%). There may have been some bias towards inclusion of patients with greater psychopathology, since a somewhat higher proportion of patients who agreed to participate were in current psychiatric care and had a history of previous DSH compared to those who did not participate (differences not statistically significant). However, the included patients were generally representative of the overall DSH population which presented to the hospital during the study period.
Personality disorders
The proportion of DSH patients in this study with a personality disorder (45.9%) is similar to that found in previous studies (Reference Ennis, Barnes and KennedyEnnis et al, 1989, 57.7%; Reference Suominen, Henriksson and SuokasSuominen et al, 1996, 40.4%; Reference Ferreira de Castro, Cunha and PimentaFerreira de Castro et al, 1998, 50.6%). Borderline personality disorder has been reported as the most common personality disorder in several studies of DSH patients (Reference Ennis, Barnes and KennedyEnnis et al, 1989; Reference Suominen, Henriksson and SuokasSuominen et al, 1996; Reference Gupta and TrzepaczGupta & Trzepacz, 1997). One of its diagnostic features is recurrent threats or acts of self-harm. In this study, emotionally unstable personality disorder, of which borderline personality disorder is a sub-type, was less common than the anxious, anankastic and paranoid disorders. This may reflect insensitivity of the self-report version of the PAS in detecting borderline disorder. However, few studies have screened for the full range of personality disorders. For example, Nordentoft & Rubin (Reference Nordentoft and Rubin1993) only reported on the presence of borderline and antisocial personality disorder. Thus, the previous perceptions of the nature of personality disorder in DSH patients may have been misrepresented. Our findings are similar to those of Dirks (Reference Dirks1998), whose study was the only other one that used a standardised tool for the assessment of personality. He found paranoid and anxious, followed by impulsive, to be the most common personality disorders. The findings regarding personality disorder may have been somewhat different if we had been able to interview other informants (Reference ZimmermanZimmerman, 1994).
Comorbidity
The high prevalence of comorbidity of psychiatric and personality disorders (44.1%) is similar to that reported by Suominen et al (Reference Suominen, Henriksson and Suokas1996) (39.0%) in the only other study which examined comorbidity in a representative patient sample. The importance of comorbidity in suicidal behaviour is apparent from the study by Foster et al (Reference Foster, Gillespie and McClelland1999) in which it increased the risk of suicide over six-fold compared with the risk in individuals with psychiatric disorders alone.
Gender differences
A striking finding of this study is that there were no significant gender differences in the prevalence and severity of depressive disorders, in the prevalence of anxiety disorders or in the frequency of comorbidity of psychiatric and/or personality disorders. However, there were significant gender differences in the rates of alcohol dependence or harmful use and eating disorders.
Implications for the management of deliberate self-harm
The high rates of psychiatric morbidity found in this study suggest that the assessment of DSH patients should include careful screening for psychiatric symptoms. This has implications for staff training. The high prevalence of depressive symptoms and the large number of patients with severe depressive episodes raises the question of whether affective disorders in DSH patients are under-recognised and under-treated. While psychosocial interventions are thought appropriate for a large proportion of patients (Reference Heard, Hawton and van HeeringenHeard, 2000), antidepressant treatment may also be indicated for a sizeable number. Alcohol-related disorders are also very common and require skilled detection and treatment. Deliberate self-harm patients can be non-compliant and difficult to engage in therapy (Reference van Heeringen, Jannes and Buylaertvan Heeringen et al, 1995). The comorbidity of psychiatric and/or personality disorders complicates the management of patients such that effective treatment may require collaboration between multiple agencies.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Psychiatric disorder is very common in deliberate self-harm (DSH) patients and therefore they need careful screening for psychiatric symptoms.
-
▪ Many DSH patients have depression of moderate or severe severity, therefore treatment with antidepressants may often be indicated for these patients.
-
▪ Many DSH patients have comorbid disorders and may need an integrated care package involving multiple agencies.
LIMITATIONS
-
▪ Not all potential subjects could be included in the study and there may have been a small bias towards patients with somewhat greater psychopathology being included in the study sample.
-
▪ Psychiatric disorder was assessed using a structured clinical diagnostic schedule which may have influenced the reporting of symptoms.
-
▪ Personality disorders and traits were only assessed in patients who were interviewed at follow-up.
ACKNOWLEDGEMENTS
This study and the Oxford Monitoring System for Attempted Suicide were funded by Anglia and Oxford NHS Executive Regional Research Committee. Keith Hawton is also supported by Oxfordshire Mental Healthcare Trust. Camilla Haw is supported by St Andrew's Hospital, Northampton. We would like to thank the staff in the Department of Psychological Medicine (Dr Christopher Bass, Karen Carroll, Barbara Chishom, Sharon Codd, Dr Eleanor Feldman, Dave Roberts, Jill Roberts, Heather Weitzel and Linda Whitehead) for their considerable assistance with the study and also Louise Harriss for her help with the analysis of data from the Monitoring System. Oxford is the UK Centre in the WHO/Euro Multicentre Study on Parasuicide.








eLetters
No eLetters have been published for this article.