The possibility that community care may place not only patients but also the public at risk is of much concern. Case management has been proposed as the coordinating mechanism for community care (Reference Holloway, Oliver and CollinsHolloway et al, 1995). In intensive case management a particular emphasis is placed upon small case-loads, typically 10 to 15 patients per case manager, with subsequent increased levels of contact. Adverse outcomes previously measured in case management trials include deaths (Reference Muijen, Cooney and StrathdeeMuijen et al, 1994), imprisonments (Reference Wilson, Tien and EvansWilson et al, 1995) and police contacts (Reference Bond, Miller and KrumwiedBond et al, 1988). Suicidal behaviour, however, has rarely been examined as an adverse outcome. The only published study identified to date reporting the effect of intensive case management compared to standard care on prevalence of suicidal behaviour found no significant effect (Reference Johnson, Leese and BrooksJohnson et al, 1998).
This study addresses two questions:
-
(a) Does intensive case management reduce the prevalence of suicidal behaviour in psychosis compared with standard care?
-
(b) What socio-demographic and clinical factors best predict suicidal behaviour in chronic psychosis?
METHOD
Subjects and setting
The UK700 case management trial is a randomised controlled trial designed to examine the efficacy of intensive compared to standard case management. Patients were recruited from three London centres (King's College Hospital, St George's and St Mary's/St Charles hospitals) and one in Manchester (the School of Psychiatry and Behavioural Sciences, University of Manchester). Recruitment took place at the point of discharge from hospital or in the community. The UK700 trial design (UK700 Group, 1999) and outcomes (Reference Burns, Creed and FahyBurns et al, 1999) are described elsewhere.
Patients had to meet the following inclusion/exclusion criteria:
-
(a) aged 18-65 years;
-
(b) a diagnosis of psychosis, defined as the presence according to the Research Diagnostic Criteria (Reference Spitzer, Endicott and RobinsSpitzer et al, 1978) of delusions, hallucinations or thought disorder;
-
(c) hospitalised for psychotic symptoms at least twice, with the most recent admission being within the past 2 years;
-
(d) absence of organic brain damage;
-
(e) absence of a primary diagnosis of substance misuse.
After giving informed consent and completing a baseline interview, 708 patients were individually randomised to intensive case management (10-15 patients per case manager) or standard care (30 or more patients per case manager). Randomisation was stratified by centre, source of patient at point of randomisation and ethnic origin.
Community teams at each centre were organised into intensive and standard teams, and each patient was assigned an individual case manager from their designated care group. Case managers were mainly community psychiatric nurses but also included occupational therapists, psychologists and social workers. The study was designed so that only one key variable (size of case-load) differed between the experimental and control groups, while all other important variables which might determine outcome were the same. Throughout the trial continuous monitoring of case manager activity was conducted.
Data collection
Subjects were interviewed using a battery of instruments (see below) at baseline and 2-year follow-up.
The main outcome variable was attempted or completed suicide between the baseline and 2-year follow-up interviews. In the World Health Organization (WHO) Life Chart interview (World Health Organization, 1992), individuals were asked whether they had attempted suicide during this time and if so, how often. A suicide attempt was defined as a self-destructive act carried out with the intention of ending one's life. Ratings were based not only on patient report but also on all available sources of information, including case notes and interviews with relatives and case managers. Where a 2-year outcome interview with a subject was not possible, an attempt was made to complete the WHO Life Chart using all other sources of information. Completed suicides were recorded at each centre.
The following socio-demographic and clinical factors, measured at baseline interview, were selected a priori on the basis of previous research, to predict suicidal behaviour during the 2-year follow-up period.
UK700 socio-demographic schedule. This interview measures a variety of socio-demographic and clinical variables, specifically designed for the trial.
Socio-demographic variables are: age, gender, marital status, ethnicity, having children, educational achievement, and social class as determined by occupation of father at birth.
Clinical variables are: previous attempts at suicide (prior to baseline interview), age of onset of psychosis, first admission for psychosis, months since onset of psychosis and months spent as an inpatient since onset of illness to baseline interview.
The Comprehensive Psychopathological Rating Scale. The CPRS (Reference Åsberg, Montgomery and PerrisÅsberg et al, 1978) rates 65 psychopathological items, including acute psychotic symptoms, on a severity scale of 0-3, relating to the week before interview.
Montgomery—Åsberg Depression Rating Scale. This sub-scale of the CPRS (Reference Montgomery and ÅsbergMontgomery & Åsberg, 1979) provides an estimate of the objective level of depression over the previous week.
The Scale for Assessment of Negative Symptoms. The SANS (Reference AndreasonAndreason, 1984) provides a total score for negative symptoms of psychosis based on an observer's judgement of 24 items on a six-point Likert scale.
World Health Organization Life Chart. Socio-demographic variables measured are: employment status, living situation and assaults on others.
Clinical variables are: usual symptom severity, medication use, psychiatric admissions and treatment for substance misuse (drugs and alcohol).
The Operational Criteria Checklist for Psychotic Illness. The OCCPI (Reference McGuffin, Farmer and HarveyMcGuffin et al, 1991) is completed by a psychiatrist from medical case notes to generate lifetime Research Diagnostic Criteria diagnoses.
Clinical variables measured are: psychiatric diagnosis, mode of onset of illness, presence of hallucinations and thought disorder.
Researchers were psychiatrists, research psychologists and a social scientist, all of whom participated in an initial 2-day training course and completed five pilot interview schedules. Training material included lectures, joint patient interviews, case vignettes and video interviews. Completed interview schedules were regularly inspected on site for errors and inconsistencies, and feedback was given to the researchers. Researchers were not blind to the treatment group, the reasons for this being two-fold. First, there was a need for close liaison between case managers and researchers in order to organise interviews with patients who were difficult to contact. Second, researchers were advised to check on the safety of visits with the case manager beforehand.
Statistical methods
The data were initially inspected to examine the baseline demographic characteristics of the UK700 sample. A check was performed for missing values to examine whether any biases had been introduced. Subjects with missing values for the relevant variables were excluded from the analysis.
The 2-year prevalence of suicidal behaviour (the percentage of individuals who had made at least one unsuccessful or a successful attempt at suicide in the 2-year period) was estimated in the total sample and a comparison between treatment groups was made using the chi-squared test. It was not feasible to conduct a survival analysis, as the date of attempts or loss to follow-up was not recorded for many events. Analyses were conducted for those who had attempted suicide but did not succeed in the first instance, and for all individuals irrespective of outcome in the second, and it is the latter results which are presented here.
No follow-up information on parasuicide was available for 45 (6.3%) of the 708 study subjects. Comparisons were made between these individuals and those with outcome information, using chi-squared and Wilcoxon rank sum tests to detect any significant differences in baseline socio-demographic and clinical characteristics.
In order to identify possible predictors, attempters were initially compared on all socio-demographic and clinical variables using chi-squared tests (categorical variables), t-tests (normally distributed continuous variables) and Wilcoxon rank sum tests (skewed continuous variables). Logistic regression was used to generate unadjusted odds ratios along with their 95% confidence intervals for all explanatory variables. A multivariate analysis was then conducted using stepwise methods starting with all univariately significant variables, but allowing these variables to be dropped and other variables to enter the model at later stages using the 5% significance level, so as to find the best model to predict suicidal behaviour. Each risk factor was then assessed in turn by adding it to this final model, to ensure that no significant predictors were missed. Likelihood ratio tests were conducted to assess the significance levels of variables tested and to examine for potential confounders. All variables were adjusted for treatment group. Data were analysed using STATA version 5 (STATA Corporation, 1995).
RESULTS
Randomisation and follow-up
The demographic profile of the UK700 subjects is described elsewhere (Reference Burns, Creed and FahyBurns et al, 1999). Of those approached 13% refused to participate in the trial. A further 7% were not entered for a variety of reasons, including inability to give informed consent and inability to establish contact. It was possible to collect only a limited amount of information on all eligible patients at each site. Some comparisons of basic demographic (age and gender) and clinical characteristics (duration of illness) were made between those who entered the trial and those who did not. The patients who refused to enter were found to be very similar to those who did in terms of socio-demographic and illness history. Three hundred and fifty-three patients (49.8%) were randomised to receive intensive case management and 355 (50.2%) to receive standard care. Follow-up information with regard to suicidal behaviour was available for 663 (94%) of the total group, 334 (95%) in the intensive and 329 (93%) in the standard arm. A comparison between the 45 individuals on whom outcome information on suicidal behaviour was not available with those for whom information was available revealed that those not successfully followed up tended to have less severe forms of illness at baseline (λ2 (3)=7.58, P=0.05) and were significantly more likely to have received treatment for drug misuse in the 2 years prior to interview (λ2 (1)=5.29, P=0.02). No other significant differences were found between the groups among the other 27 variables examined.
During the trial, eight deaths occurred in each treatment arm (intensive - five by suicide, three from natural causes; standard - four by suicide, one murdered and three from natural causes).
Missing values were substantial for occupation of father at birth (119/661=18%), living situation (77/661=11.6%) and mode of onset of illness (151/661=22.8%). No other variable had more than 2% missing values.
Prevalence of suicidal behaviour
Seventy-three (10.3%) subjects attempted suicide in the 2-year follow-up period. A total of 168 attempts were made. The median number of attempts was 1 (90% range 1 to 9). Nine (1.3%) subjects committed suicide, eight males and one female. Fortythree (12.8%) subjects in the intensive arm and 39 (11.8%) in the standard arm of the trial attempted or completed suicide (P=0.69). The odds ratio for suicidal behaviour in the intensive compared to standard groups was 1.09 (95% CI 0.69-1.75).
Predictors of suicidal behaviour
Univariate (unadjusted) analysis
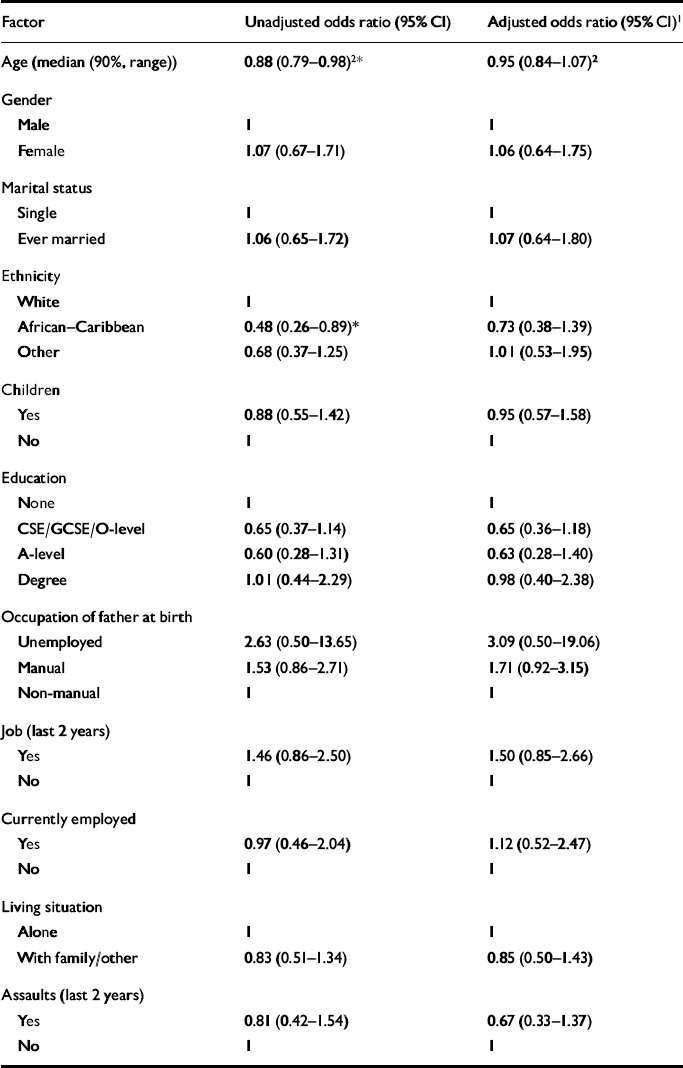
Socio-demographic. Patients who attempted or completed suicide in the 2-year study period differed significantly from those who did not on two of the 11 socio-demographic factors investigated: age and ethnicity. Attempters were significantly younger than non-attempters (OR 0.88 per 5-year increase in age, P=0.03); White subjects were significantly more likely to have made an attempt than African-Caribbean subjects (OR 0.48, P=0.05). Results are presented in Table 1.
Table 1 Unadjusted and adjusted odds ratios for socio-demographic predictors of suicidal behaviour
| Factor | Unadjusted odds ratio (95% CI) | Adjusted odds ratio (95% CI)1 |
|---|---|---|
| Age (median (90%, range)) | 0.88 (0.79-0.98)2 * | 0.95 (0.84-1.07)2 |
| Gender | ||
| Male | 1 | 1 |
| Female | 1.07 (0.67-1.71) | 1.06 (0.64-1.75) |
| Marital status | ||
| Single | 1 | 1 |
| Ever married | 1.06 (0.65-1.72) | 1.07 (0.64-1.80) |
| Ethnicity | ||
| White | 1 | 1 |
| African-Caribbean | 0.48 (0.26-0.89)* | 0.73 (0.38-1.39) |
| Other | 0.68 (0.37-1.25) | 1.01 (0.53-1.95) |
| Children | ||
| Yes | 0.88 (0.55-1.42) | 0.95 (0.57-1.58) |
| No | 1 | 1 |
| Education | ||
| None | 1 | 1 |
| CSE/GCSE/O-level | 0.65 (0.37-1.14) | 0.65 (0.36-1.18) |
| A-level | 0.60 (0.28-1.31) | 0.63 (0.28-1.40) |
| Degree | 1.01 (0.44-2.29) | 0.98 (0.40-2.38) |
| Occupation of father at birth | ||
| Unemployed | 2.63 (0.50-13.65) | 3.09 (0.50-19.06) |
| Manual | 1.53 (0.86-2.71) | 1.71 (0.92-3.15) |
| Non-manual | 1 | 1 |
| Job (last 2 years) | ||
| Yes | 1.46 (0.86-2.50) | 1.50 (0.85-2.66) |
| No | 1 | 1 |
| Currently employed | ||
| Yes | 0.97 (0.46-2.04) | 1.12 (0.52-2.47) |
| No | 1 | 1 |
| Living situation | ||
| Alone | 1 | 1 |
| With family/other | 0.83 (0.51-1.34) | 0.85 (0.50-1.43) |
| Assaults (last 2 years) | ||
| Yes | 0.81 (0.42-1.54) | 0.67 (0.33-1.37) |
| No | 1 | 1 |
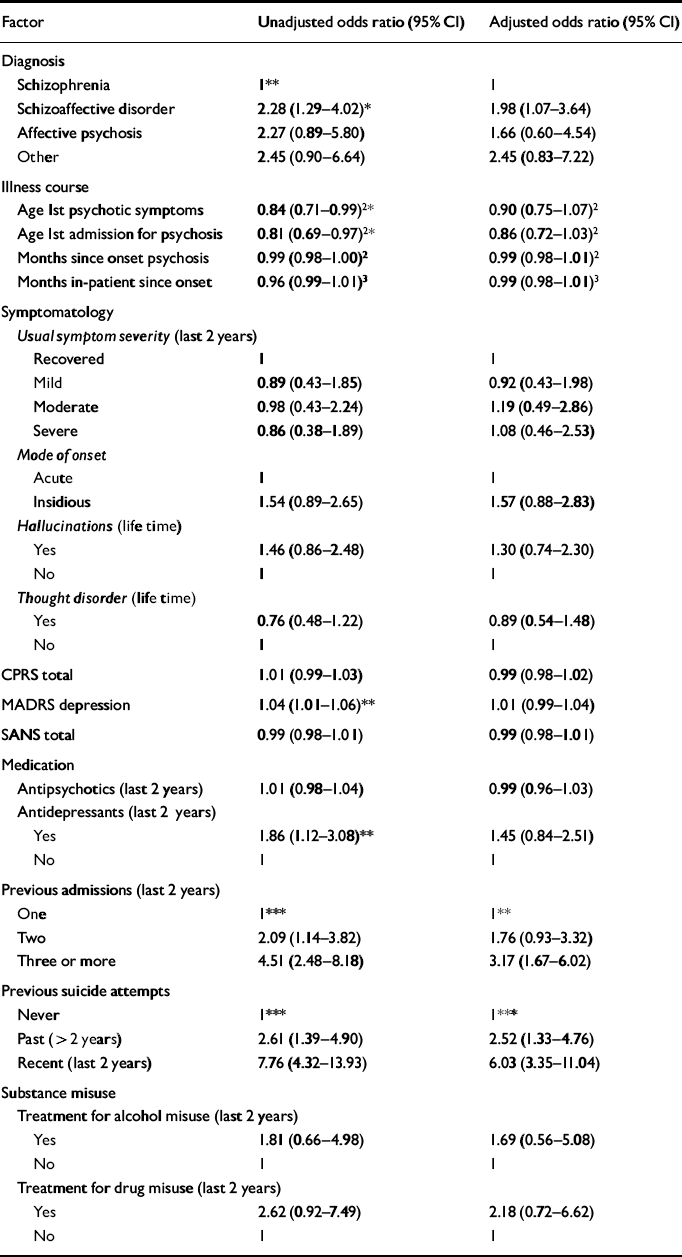
Clinical. Attempters differed significantly from non-attempters in seven of the 19 clinical factors investigated (results are presented in Table 2). They were significantly more likely to have a diagnosis of schizoaffective disorder than schizophrenia (OR 2.28, P=0.03) (the group labelled ‘other’ contained a very mixed set of diagnoses from which little conclusion could be drawn), were significantly younger at onset of illness (OR 0.84 per 5-year increase in age, P=0.02) and at first hospital admission for psychosis (OR 0.81 per 5-year increase in age, P=0.009), had significantly higher MADRS scores (OR 1.04, P=0.01), representing greater levels of objective depression at time of interview, were significantly more likely to have been prescribed antidepressants (OR 1.86, P=0.01) and had been admitted to hospital on multiple occasions in the previous 2 years (OR 4.51, P<0.001). Past attempts at suicide were highly significantly related to parasuicide during the study period (OR 7.76, P<0.001). Only 21 (26%) of those who attempted suicide in the study period had never made a previous attempt, compared to 62% among non-attempters. Nearly 50% (n=36) of attempters had made an attempt in the 2 years prior to interview, compared with only 14% of non-attempters.
Table 2 Unadjusted and adjusted odds ratios for clinical predictors of suicidal behaviour
| Factor | Unadjusted odds ratio (95% CI) | Adjusted odds ratio (95% CI) |
|---|---|---|
| Diagnosis | ||
| Schizophrenia | 1** | 1 |
| Schizoaffective disorder | 2.28 (1.29-4.02)* | 1.98 (1.07-3.64) |
| Affective psychosis | 2.27 (0.89-5.80) | 1.66 (0.60-4.54) |
| Other | 2.45 (0.90-6.64) | 2.45 (0.83-7.22) |
| Illness course | ||
| Age 1st psychotic symptoms | 0.84 (0.71-0.99)2 * | 0.90 (0.75-1.07)2 |
| Age 1st admission for psychosis | 0.81 (0.69-0.97)2 * | 0.86 (0.72-1.03)2 |
| Months since onset psychosis | 0.99 (0.98-1.00)2 | 0.99 (0.98-1.01)2 |
| Months in-patient since onset | 0.96 (0.99-1.01)3 | 0.99 (0.98-1.01)3 |
| Symptomatology | ||
| Usual symptom severity (last 2 years) | ||
| Recovered | 1 | 1 |
| Mild | 0.89 (0.43-1.85) | 0.92 (0.43-1.98) |
| Moderate | 0.98 (0.43-2.24) | 1.19 (0.49-2.86) |
| Severe | 0.86 (0.38-1.89) | 1.08 (0.46-2.53) |
| Mode of onset | ||
| Acute | 1 | 1 |
| Insidious | 1.54 (0.89-2.65) | 1.57 (0.88-2.83) |
| Hallucinations (life time) | ||
| Yes | 1.46 (0.86-2.48) | 1.30 (0.74-2.30) |
| No | 1 | 1 |
| Thought disorder (life time) | ||
| Yes | 0.76 (0.48-1.22) | 0.89 (0.54-1.48) |
| No | 1 | 1 |
| CPRS total | 1.01 (0.99-1.03) | 0.99 (0.98-1.02) |
| MADRS depression | 1.04 (1.01-1.06)** | 1.01 (0.99-1.04) |
| SANS total | 0.99 (0.98-1.01) | 0.99 (0.98-1.01) |
| Medication | ||
| Antipsychotics (last 2 years) | 1.01 (0.98-1.04) | 0.99 (0.96-1.03) |
| Antidepressants (last 2 years) | ||
| Yes | 1.86 (1.12-3.08)** | 1.45 (0.84-2.51) |
| No | 1 | 1 |
| Previous admissions (last 2 years) | ||
| One | 1*** | 1** |
| Two | 2.09 (1.14-3.82) | 1.76 (0.93-3.32) |
| Three or more | 4.51 (2.48-8.18) | 3.17 (1.67-6.02) |
| Previous suicide attempts | ||
| Never | 1*** | 1*** |
| Past (> 2 years) | 2.61 (1.39-4.90) | 2.52 (1.33-4.76) |
| Recent (last 2 years) | 7.76 (4.32-13.93) | 6.03 (3.35-11.04) |
| Substance misuse | ||
| Treatment for alcohol misuse (last 2 years) | ||
| Yes | 1.81 (0.66-4.98) | 1.69 (0.56-5.08) |
| No | 1 | 1 |
| Treatment for drug misuse (last 2 years) | ||
| Yes | 2.62 (0.92-7.49) | 2.18 (0.72-6.62) |
| No | 1 | 1 |
Multivariate analyses
Of the nine variables found to be univariately significant, only two remained so in the multivariate model. Ethnicity was confounded by MADRS score and age at first admission for psychosis by age. Diagnosis, antidepressant use, MADRS score and age were not significant after adjustment for past attempts. Only previous suicide attempts and admissions to hospital in the past 2 years remained independently significant in the multivariate analysis. We then adjusted all other variables for these and treatment group. Following these adjustments, no other variable gained statistical significance. Tables 1 and 2 present the odds ratios for all socio-demographic and clinical variables adjusted for previous suicide attempts, hospital admissions in the last 2 years and treatment group.
DISCUSSION
Prevalence of suicidal behaviour
The first aim of this study was to determine whether intensive case management reduced the prevalence of suicidal behaviour in established psychotic illness. No protective effect of intensive case management was found, with the 2-year prevalence being almost exactly the same in both groups. This verifies the result of the only previous study addressing this question (Reference Johnson, Leese and BrooksJohnson et al, 1998).
Follow-up information on suicidal behaviour was available for only 663 (94%) of the 708 individuals recruited into the trial. Therefore the estimated prevalence of suicidal behaviour is probably an underestimate of the true prevalence in the sample. If all those lost to follow-up had attempted or completed suicide, then the prevalence in the sample would have risen to 18%. Hence the true sample prevalence must lie between 11.6% and 18%.
Apart from the fact that intensive case management may truly have no effect, what other possible explanations may there be for this finding? Although the prevalence of suicidal behaviour was almost exactly the same in both groups, it is possible that more attempts were detected in the intensive group due to the case managers' increased knowledge of the patient, by virtue of increased contact. However, the use of multiple sources of follow-up information, including patients, relatives and case notes, will have minimised this effect. Additionally, we included only those attempts where there was a clear wish to die, and it is likely that most of these more serious attempts will have been detected irrespective of treatment group. There was only a 2% difference in follow-up rates in the two groups; therefore, although some attempts in the standard group may have gone unreported, it is doubtful that this would have made any difference to our findings.
Predictors of suicidal behaviour
The second aim of the study was to identify predictors of suicidal behaviour. As the number of completed suicides was too small for meaningful analyses and it was assumed that attempts and suicides were part of the same continuum, we studied attempts and suicides together. A preliminary analysis of predictors excluding completed suicides revealed similar results. When all socio-demographic and clinical factors investigated in the study were examined in a multivariate model, only previous attempts and multiple admissions in the last 2 years remained significant. Previous attempts at suicide were the strongest predictor of subsequent suicidal behaviour, confirming earlier work (Reference Mann, Waternaux and HassMann et al, 1999; Reference Walsh, Harvey and WhiteWalsh et al, 1999). Examining the relationship further, we found that those who had attempted suicide in the 2 years prior to the study (recent attempts), were six times more likely to attempt suicide during the study period than those who had never made an attempt. Those who had attempted suicide in the distant past — that is, more than 2 years before the study period — were two-and-a-half times more likely to make an attempt than those who had never attempted suicide. Recency of an attempt thus appears to be most important.
Attempters were nearly twice as likely to have been admitted twice and nearly four times more likely to have been admitted three or more times when compared to non-attempters. We do not know the indication for these admissions, and it is possible that some patients were admitted after attempts. However, in our multivariate analysis recent attempts and admissions predicted suicidal behaviour independent of each other.
This study replicated, on univariate analysis, independent associations of suicidality identified previously, including current and past depression (Reference Cohen, Lavelle and RichCohen et al, 1994; Reference Walsh, Harvey and WhiteWalsh et al, 1999) and younger age (Reference Walsh, Harvey and WhiteWalsh et al, 1999). The finding that African—Caribbean patients were significantly less likely to attempt suicide in the univariate analysis lends support to the notion that, although more vulnerable to psychosis, they may be less likely to make attempts (Reference McKenzie, van Os and FahyMcKenzie et al, 1995). We did not replicate previously reported associations between suicidal behaviour and gender (Reference Nyman and JonssonNyman & Jonsson, 1986), mode of onset of illness, thought disorder (Reference Cohen, Lavelle and RichCohen et al, 1994), hallucinations (Reference Kaplan and HarrowKaplan & Harrow, 1996), more severe form of illness (Reference Dassori, Mezzich and KeshavanDassori et al, 1994), antipsychotic use (Reference Walsh, Harvey and WhiteWalsh et al, 1999), assaults or substance misuse (Reference Mann, Waternaux and HassMann et al, 1999).
Missing values for social class may have limited our study's ability to detect differences between the groups on this variable. However, no previous study has identified social class as a predictor. Additionally, a less acute mode of illness onset has been previously identified (Reference Cohen, Lavelle and RichCohen et al, 1994) and the large number of missing values for this variable may also have masked differences. The number of missing values of other variables was too small to have influenced the results presented.
Methodological issues
The multi-centre design allowed recruitment of a large study population, thus providing sufficient statistical power to test hypotheses. The stratified randomised design ensured maximum similarity between the groups on all variables apart from treatment allocation. Selection bias was further minimised by the high rate of follow-up (over 90%).
The main advantage of this study over others, in identification of predictors, was that we were able to measure possible predictors and then record suicidal behaviour prospectively rather than use a retrospective design. The fact that subjects were asked to recall events over a 2-year period may have introduced recall bias, but this was minimised by the use of multiple data sources. Although interviewers were not always blind to treatment group, the use of multiple data sources of information again minimised the possibility of information bias. The use of well-validated questionnaires and continual data monitoring at each centre and centrally will have minimised this bias further. We have no information on those lost to follow-up but a comparison between this group and the other study participants revealed the two groups to be largely similar.
Since the study was conducted in four inner-city areas, it is possible that results may not be generalisable to other settings. However, the multi-site design with a large number of subjects with established psychosis should increase its external validity. The recruitment of only 80% of those approached to participate may introduce further concerns about generalisability of results; those entered were not found to differ significantly on socio-demographic and illness-history variables.
The findings of this study suggest that increasing psychosocial input may not make much difference to outcome with regard to suicidal behaviour in chronic psychosis, and perhaps factors intrinsic to patients are more important. It may be that intensive case management alone is not sufficient and thus consideration must be given to a combination of management approaches. These may include other psychological treatments, such as cognitive—behavioural therapy (Reference Birchwood, Iqbal, Wykes, Tarrier and LewisBirchwood & Iqbal, 1998) and optimal pharmacological management of illness. Clozapine, for example, has been shown to reduce considerably the standardised mortality ratio for suicide in psychosis (Reference Munro, O'Sullivan and AndrewsMunro et al, 1999).
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The 2-year prevalence of suicidal behaviour among a sample of patients with psychosis was 11.6%.
-
▪ Intensive case management does not appear to reduce the prevalence of suicidal behaviour in chronic psychosis compared to standard care.
-
▪ Previous suicide attempts, particularly recent attempts, and recent admissions to hospital best predict future suicidal behaviour.
LIMITATIONS
-
▪ Other aspects of the case manager—patient relationship — for example, quality — may be more important than intensity of contact in producing favourable outcomes in case management.
-
▪ Generalisability of findings may be problematic due to the inclusion of chronic cases only.
-
▪ Subjects were asked to remember suicidal behaviour for the previous 2 years, introducing the possibility of recall bias.
ACKNOWLEDGEMENTS
The UK700 Group is a collaborative study team involving four clinical centres. Manchester Royal Infirmary: Tom Butler, Francis Creed, Janelle Fraser, Peter Huxley, Nicholas Tarrier and Theresa Tattan; King's/Maudsley Hospital, London: Thomas Fahy, Catherine Gilvarry, Kwame McKenzie, Robin Murray, Jim Van Os and Elizabeth Walsh; St Mary's Hospital/St Charles' Hospital, London: John Green, Anna Higgitt, Elizabeth van Horn, Donal Leddy, Catherine Manley, Patricia Thornton and Peter Tyrer; St George's Hospital, London: Robert Bale, Tom Burns, Matthew Fiander, Kate Harvey, Andy Kent and Chiara Samele; Centre for Health Economics, York: Sarah Byford, David Torgerson and Ken Wright; London (Statistics): Simon Thompson (Royal Postgraduate Medical School) and Ian White (London School of Hygiene and Tropical Medicine).







eLetters
No eLetters have been published for this article.