The majority of those who are depressed initially seek help from a primary carer (57-78%) (Reference Lish, Kuzman and LushLish et al, 1997). Most of those who are depressed (60-70%) are expected to be treatable with an antidepressant (Reference AndrewsAndrews, 1994). Depression may occur in one-third of patients seen by general practitioners in a day (Reference MontanoMontano, 1994). The present study concerns the pharmacological treatment of patients with depression and investigates any changes to their quality of life (QOL). At the same time it aims to evaluate the validity and sensitivity of a new, comprehensive assessment of QOL - the World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) (WHOQOL Group, 1994a, 1995, 1998) - by monitoring the initial stages of the natural history of depression. It is vital to the success of evidence-based medicine that the accuracy, reliability and validity of outcome measures are established, otherwise unknown measurement error can unwittingly lead to erroneous conclusions from clinical trials.
METHOD
Design
Around 70% of those with major depression show an excellent response to antidepressants (in appropriate therapeutic doses) administered for 6-8 weeks (Reference NemeroffNemeroff, 1994). To allow the medication to become effective and therefore detect changes in QOL scores, the time-line of this study needed to be a minimum of 6 weeks. A within-subjects, repeated measures design allows aspects of sensitivity or responsiveness to clinical change over time to be investigated. Additional measures were included to enable predictive validity to be assessed. Quota sampling guided the selection of equal gender and age groups; 45 years bisected the age range in a 2 × 2, age by gender design.
Recruitment
General practitioners (GPs) in south-west England were approached, having been selected from rural practices, a major city and suburban areas. Two practices served the armed forces and one was a university medical centre. One hundred and fifteen GPs were invited to participate and 40 doctors agreed to discuss the project, when procedures and patient recruitment criteria were explained. They were asked to recruit 10 consecutive patients to the study if patients complied with the study criteria.
Patient inclusion criteria addressed depression type, severity, medication type and timing, age and gender. English-speaking UK adults (aged 18-65) were approached. The upper limit was set to reduce the incidence of comorbid age-related illnesses, such as dementia, but if cognitive abilities were unimpaired then exceptionally, those above 65 could be included. Patients were screened using DSM-IV 296 (1, 2 or 3) (American Psychiatric Association, 1994) for depressive disorder. Mild to moderately severe depression was identified as the primary presenting condition. It was diagnosed present if patients had low mood or marked loss of interest/pleasure most of the day, most days. Patients also reported at least four of the following: changes in appetite/weight, insomnia/hyperinsomnia, agitation/retardation, fatigue/energy loss, worthlessness/guilt, lack of concentration/indecision or suicide ideation. Patients with anorexia nervosa, mania, delusions/hallucinations, significant social or occupational distress/impairment, drug/medication misuse or medical conditions like hyperthyroidism were excluded.
Patients needed to be at the beginning of a first episode of depression and suited to taking a course of antidepressants. Alternatively, they could be at the start of a new episode of depression and a new course of pharmacological treatment following 3 months of symptom remission. The type of antidepressant prescribed was an independent clinical decision.
For psychometric testing it is unnecessary to control for antidepressant type, size of dose, length of treatment, level of compliance or incidence of comorbidity in the way that would be essential to the success of a clinical trial. For validation/sensitivity tests, it is sufficient to establish that scores of QOL are higher when people are well and lower when their health is worse. Confirmation of these properties enables good measures to be used with confidence in controlled clinical trials.
Procedure
Patients were recruited by GPs at the time of a consultation for depression. Doctors were provided with an eye-catching desk card summarising the symptom criteria. When the screening criteria were met, physicians completed a symptom checklist, obtained informed consent and gave patients an information sheet and questionnaires to complete later. (Researchers assisted patients who were unable to complete the questionnaires alone.) A collector's sheet and procedure summary were provided.
Consent forms returned to the centre enabled patients to be followed up at Time 2. Patients were requested to return their completed questionnaires within a week and were contacted 10 days following issue, if the questionnaires had not been returned. Up to three reminders were issued at 7- to 10-day intervals, as necessary. Six weeks after completion of the first set, a second pack was sent, with a note of thanks.
Instruments
WHOQOL-100
The World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) is a generic measure designed for use with a wide spectrum of psychological and physical disorders. It is a multi-dimensional, multi-lingual profile for subjective assessment. During development, focus groups of patients, health professionals and well people proposed items that were selected and attached to a five-point interval, Likert response scale. They were administered to 320 sick and well people in Britain and, simultaneously, to participants in 14 other centres worldwide (n=4802). The 100 items are organised in 25 facets, subsumed within six domains (WHOQOL Group, 1995, 1998). One of these facets measures overall QOL and general health. High scores (recoded for negatively framed items) indicate good QOL. Respondents judge their quality of life in the previous 2 weeks. Two UK national items are attached to facets on positive and negative feelings respectively. Socio-demographic and current health information is obtained. The international measure as well as the UK national instrument show excellent psychometric qualities of internal consistency, reliability and construct validity (WHOQOL Group, 1995, 1998; Reference SkevingtonSkevington, 1999).
Beck Depression Inventory (BDI)
The revised BDI is a 21-item self-assessment of depression severity. Items score from 0 to 3 and total scores of 0-9 indicate no significant symptoms, 10-18 mild/moderate, 19-29 moderate/severe and 30-63 extremely severe depression. Reliability of internal consistency is good for mixed diagnoses and single- and recurrent-episode major depression. Test-retest reliability for psychiatric patients ranged from 0.48 to 0.86. BDI scores correlate 0.72 with clinical ratings of depression in psychiatric patients (Reference Beck and SteerBeck & Steer, 1987).
Measures of change
Participants completed two transition questions at retest (five-point scales) to indicate how much their general health and depression had changed during treatment. These measures provide independent benchmarks of perceived recovery and are therefore important to tests of validity.
RESULTS
Sample
Twenty-five doctors recruited 106 patients with depression between September 1997 and March 1998. Ten GPs had practices in rural areas, 9 in the suburbs and 6 in urban and inner-city areas. The patient's mean age was 41.4 years (s.d. 12.7) (maximum 78) with a relatively normal distribution. Women (76%) and married people (58%) formed the largest groups, with 14% single, 10% divorced, 9% separated, 7% living as married and 2% widowed. Secondary education was common (43%) with 34% having received further education and 14% university education. Work status assessed at Time 1 showed that 59% were employed and 35% unemployed. Seventy-five per cent had been prescribed selective serotonin reuptake inhibitors (SSRIs), 13% tricyclics and 12% other antidepressants.
When asked about their health at Time 1 it was, on average, neither good nor poor (mean 3.1; s.d. 0.9): 3% reported very poor health, 23% poor, 42% neither poor nor good, 26% good and 4% very good (data were missing for 2%). Fifty-six per cent provided information about co-morbidity; the main groups were chronic nervous/emotional problems (34%), arthritis or rheumatism (10%), high blood pressure (4%) and damaged bones (2%).
Quality of life of patients with depression in primary care
The mean time between test (Time 1) and retest (Time 2) was 55 days (nearly 8 weeks). Over 75% completed a retest in less than 9 weeks. The mean duration of depression was 2 years, 3 months (s.d. 4 years, 4 months) with up to 20 years' recurrent illness. This skewed distribution showed that 69% of patients had been depressed for under a year (80% under 2 years). This was expected for mild to moderate depression where patients were taking a new course of medication. The severity of depression — mean BDI score — was 25.4 (s.d. 11) at the start of treatment, showing that the sample was moderate to severe, and more depressed than expected. At retest, depression had significantly improved: BDI scores had decreased to 15.5 (s.d. 10), indicating a mild or moderate depression (t=9.66, d.f.=79; P=0.0001).
Perceived changes in depression (depression transition question) showed a trend towards improvement (mean 3.8), with 74% reporting that they were better or very much better. Fifty-six per cent felt better, 18% very much better and 15% the same. Nine per cent were worse, with only 1.5% very much worse. Participants also reported that their general health had slightly improved (mean 3.6); 42% thought their general health was the same, 41% felt better and 11% very much better. Only 6% reported that their general health was worse or very much worse. Together these results provide important confirmatory information to show that improvements in health had genuinely occurred.
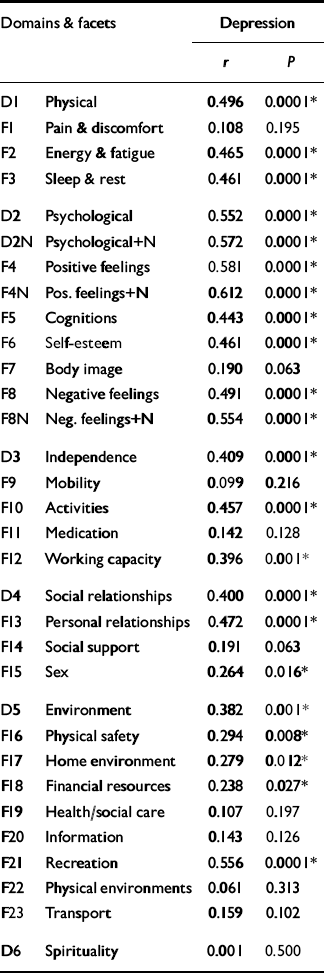
An improvement in depression, as measured by statistical changes in BDI scores during the study, was found to be equivalent to perceived clinical improvements in depression, as recorded by the transition questions (vice versa for deterioration) (Pearson r=-0.469, d.f.=78, P < 0.01). This correlation means that transition scores can be validly substituted as a sensitive measure of clinical change in other depression analyses reported below. (This is preferable to using statistical difference scores that may not tap into the clinical change that has actually been perceived.) It was then possible to find out whether any changes in QOL were significantly associated with perceived changes in depression. Significant correlations would indicate that changes in the WHOQOL-100 scores are closely related to important changes in clinical condition perceived by patients over the same period. The results in Table 4 confirm that improvements in QOL domains are strongly associated with reductions in depression, except for spirituality. Facet analyses showed a similar significant association in 15 facets, but for 9 there was no significant effect (Table 1).
Table 1 Correlations between changes in quality of life with perceived changes in depression on the Beck Depression Inventory
| Domains & facets | Depression | ||
|---|---|---|---|
| r | P | ||
| D1 | Physical | 0.496 | 0.0001* |
| F1 | Pain & discomfort | 0.108 | 0.195 |
| F2 | Energy & fatigue | 0.465 | 0.0001* |
| F3 | Sleep & rest | 0.461 | 0.0001* |
| D2 | Psychological | 0.552 | 0.0001* |
| D2N | Psychological+N | 0.572 | 0.0001* |
| F4 | Positive feelings | 0.581 | 0.0001* |
| F4N | Pos. feelings+N | 0.612 | 0.0001* |
| F5 | Cognitions | 0.443 | 0.0001* |
| F6 | Self-esteem | 0.461 | 0.0001* |
| F7 | Body image | 0.190 | 0.063 |
| F8 | Negative feelings | 0.491 | 0.0001* |
| F8N | Neg. feelings+N | 0.554 | 0.0001* |
| D3 | Independence | 0.409 | 0.0001* |
| F9 | Mobility | 0.099 | 0.216 |
| F10 | Activities | 0.457 | 0.0001* |
| F11 | Medication | 0.142 | 0.128 |
| F12 | Working capacity | 0.396 | 0.001* |
| D4 | Social relationships | 0.400 | 0.0001* |
| F13 | Personal relationships | 0.472 | 0.0001* |
| F14 | Social support | 0.191 | 0.063 |
| F15 | Sex | 0.264 | 0.016* |
| D5 | Environment | 0.382 | 0.001* |
| F16 | Physical safety | 0.294 | 0.008* |
| F17 | Home environment | 0.279 | 0.012* |
| F18 | Financial resources | 0.238 | 0.027* |
| F19 | Health/social care | 0.107 | 0.197 |
| F20 | Information | 0.143 | 0.126 |
| F21 | Recreation | 0.556 | 0.0001* |
| F22 | Physical environments | 0.061 | 0.313 |
| F23 | Transport | 0.159 | 0.102 |
| D6 | Spirituality | 0.001 | 0.500 |
Changes in QOL during treatment
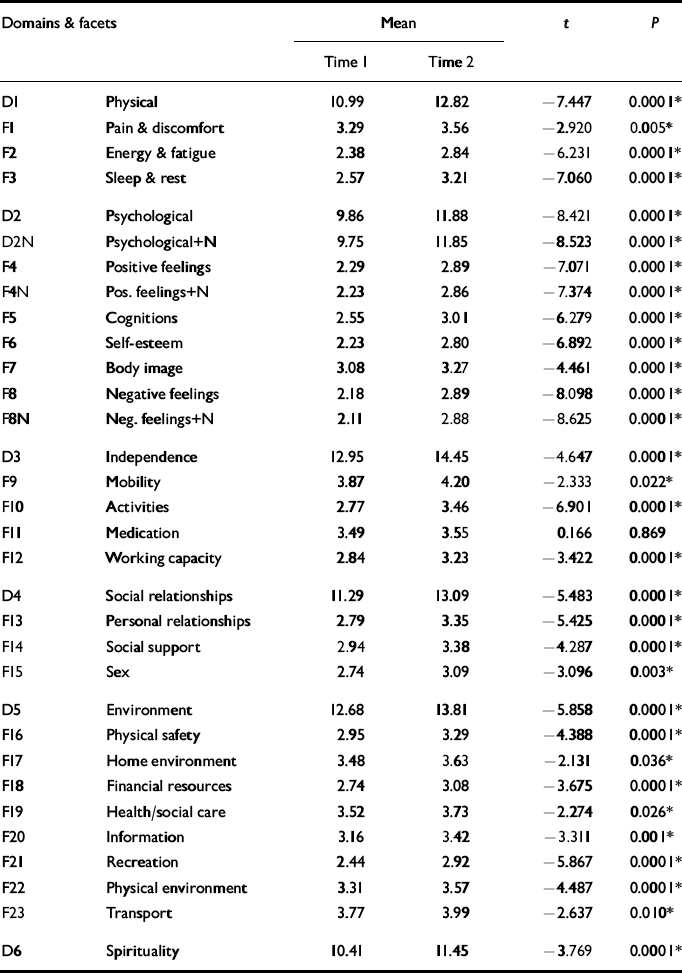
A main aim of this study was to investigate whether antidepressant medication improves different aspects of QOL during the study. Mean test and retest scores for each facet were compared in a matched pairs design (n=84) using Student's t. Twenty-four facets showed a significant increase in QOL scores (P < 0.05) (Table 2), demonstrating that QOL improves in the 8 weeks following the start of antidepressant treatment. This occurs in a broadranging way across all the important aspects of QOL related to health, except dependence on medication and treatments, where no significant change was expected, given the nature of the study. All domains also showed significant improvements in QOL over time. These results provide validation for the WHOQOL-100 and reaffirm that on almost all dimensions, changes in the scores of WHOQOL-100 are responsive to clinical change over time.
Table 2 Student's t-test (matched pairs) showing differences between test and retest for World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) domains and facets
| Domains & facets | Mean | t | P | ||
|---|---|---|---|---|---|
| Time 1 | Time 2 | ||||
| D1 | Physical | 10.99 | 12.82 | -7.447 | 0.0001* |
| F1 | Pain & discomfort | 3.29 | 3.56 | -2.920 | 0.005* |
| F2 | Energy & fatigue | 2.38 | 2.84 | -6.231 | 0.0001* |
| F3 | Sleep & rest | 2.57 | 3.21 | -7.060 | 0.0001* |
| D2 | Psychological | 9.86 | 11.88 | -8.421 | 0.0001* |
| D2N | Psychological+N | 9.75 | 11.85 | -8.523 | 0.0001* |
| F4 | Positive feelings | 2.29 | 2.89 | -7.071 | 0.0001* |
| F4N | Pos. feelings+N | 2.23 | 2.86 | -7.374 | 0.0001* |
| F5 | Cognitions | 2.55 | 3.01 | -6.279 | 0.0001* |
| F6 | Self-esteem | 2.23 | 2.80 | -6.892 | 0.0001* |
| F7 | Body image | 3.08 | 3.27 | -4.461 | 0.0001* |
| F8 | Negative feelings | 2.18 | 2.89 | -8.098 | 0.0001* |
| F8N | Neg. feelings+N | 2.11 | 2.88 | -8.625 | 0.0001* |
| D3 | Independence | 12.95 | 14.45 | -4.647 | 0.0001* |
| F9 | Mobility | 3.87 | 4.20 | -2.333 | 0.022* |
| F10 | Activities | 2.77 | 3.46 | -6.901 | 0.0001* |
| F11 | Medication | 3.49 | 3.55 | 0.166 | 0.869 |
| F12 | Working capacity | 2.84 | 3.23 | -3.422 | 0.0001* |
| D4 | Social relationships | 11.29 | 13.09 | -5.483 | 0.0001* |
| F13 | Personal relationships | 2.79 | 3.35 | -5.425 | 0.0001* |
| F14 | Social support | 2.94 | 3.38 | -4.287 | 0.0001* |
| F15 | Sex | 2.74 | 3.09 | -3.096 | 0.003* |
| D5 | Environment | 12.68 | 13.81 | -5.858 | 0.0001* |
| F16 | Physical safety | 2.95 | 3.29 | -4.388 | 0.0001* |
| F17 | Home environment | 3.48 | 3.63 | -2.131 | 0.036* |
| F18 | Financial resources | 2.74 | 3.08 | -3.675 | 0.0001* |
| F19 | Health/social care | 3.52 | 3.73 | -2.274 | 0.026* |
| F20 | Information | 3.16 | 3.42 | -3.311 | 0.001* |
| F21 | Recreation | 2.44 | 2.92 | -5.867 | 0.0001* |
| F22 | Physical environment | 3.31 | 3.57 | -4.487 | 0.0001* |
| F23 | Transport | 3.77 | 3.99 | -2.637 | 0.010* |
| D6 | Spirituality | 10.41 | 11.45 | -3.769 | 0.0001* |
Mood and quality of life
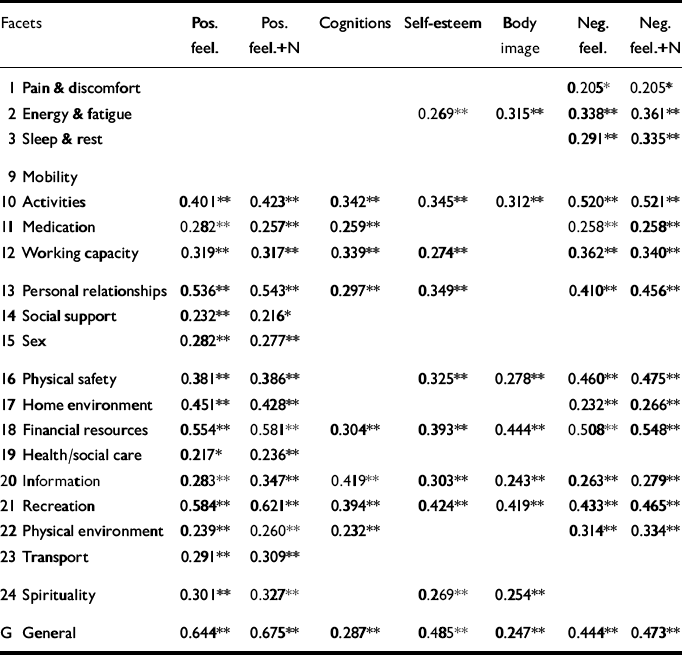
The psychological domain should be especially salient in patients with mild to moderate depression as it contains two measures of mood. A question raised in the literature has been about how mood relates to the way people report their quality of life. To find out, we carried out one-tailed Pearson correlations (P < 0.01) between the five facets of the psychological domain with other facets outside the domain (Table 3). For patients with depression, nearly all facets outside the psychological domain were significantly affected by mood (or vice versa) — namely, by positive feelings, negative feelings or, in the majority of facets, both moods (mobility is the exception). So the way people perceive nearly every important aspect of their QOL is influenced by mood state at the time of completion. Within the time frame of the WHOQOL-100, mood is taken to mean the prevailing affective state during the 2 weeks prior to completion. While perceptions of QOL are clearly influenced by mood, they are not synonymous with it. Within the WHOQOL-100, mood forms two important components of QOL, but development work shows that users believe it to be just two facets among 24. Furthermore, judgements about QOL involve not only an evaluation of subjective, internal state including mood but are also affected in a complex way by the environment, situation or events experienced at the time of rating. Therefore it is not possible to conclude that mood is quality of life.
Table 3 Significant Pearson correlations (1-tailed) (P <0.01) of facets of the psychological domain with other World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) facets
| Facets | Pos. feel. | Pos. feel. + N | Cognitions | Self-esteem | Body image | Neg. feel. | Neg. feel. + N |
|---|---|---|---|---|---|---|---|
| 1 Pain & discomfort | 0.205* | 0.205* | |||||
| 2 Energy & fatigue | 0.269** | 0.315** | 0.338** | 0.361** | |||
| 3 Sleep & rest | 0.291** | 0.335** | |||||
| 9 Mobility | |||||||
| 10 Activities | 0.401** | 0.423** | 0.342** | 0.345** | 0.312** | 0.520** | 0.521** |
| 11 Medication | 0.282** | 0.257** | 0.259** | 0.258** | 0.258** | ||
| 12 Working capacity | 0.319** | 0.317** | 0.339** | 0.274** | 0.362** | 0.340** | |
| 13 Personal relationships | 0.536** | 0.543** | 0.297** | 0.349** | 0.410** | 0.456** | |
| 14 Social support | 0.232** | 0.216* | |||||
| 15 Sex | 0.282** | 0.277** | |||||
| 16 Physical safety | 0.381** | 0.386** | 0.325** | 0.278** | 0.460** | 0.475** | |
| 17 Home environment | 0.451** | 0.428** | 0.232** | 0.266** | |||
| 18 Financial resources | 0.554** | 0.581** | 0.304** | 0.393** | 0.444** | 0.508** | 0.548** |
| 19 Health/social care | 0.217* | 0.236** | |||||
| 20 Information | 0.283** | 0.347** | 0.419** | 0.303** | 0.243** | 0.263** | 0.279** |
| 21 Recreation | 0.584** | 0.621** | 0.394** | 0.424** | 0.419** | 0.433** | 0.465** |
| 22 Physical environment | 0.239** | 0.260** | 0.232** | 0.314** | 0.334** | ||
| 23 Transport | 0.291** | 0.309** | |||||
| 24 Spirituality | 0.301** | 0.327** | 0.269** | 0.254** | |||
| G General | 0.644** | 0.675** | 0.287** | 0.485** | 0.247** | 0.444** | 0.473** |
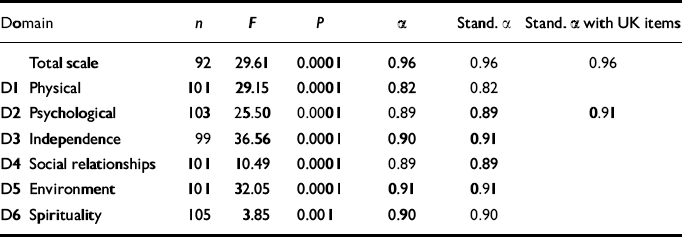
Table 4 Internal consistency of World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) domains (D) for primary care patients with moderate depression
| Domain | n | F | P | α | Stand. α | Stand. α with UK items | |
|---|---|---|---|---|---|---|---|
| Total scale | 92 | 29.61 | 0.0001 | 0.96 | 0.96 | 0.96 | |
| D1 | Physical | 101 | 29.15 | 0.0001 | 0.82 | 0.82 | |
| D2 | Psychological | 103 | 25.50 | 0.0001 | 0.89 | 0.89 | 0.91 |
| D3 | Independence | 99 | 36.56 | 0.0001 | 0.90 | 0.91 | |
| D4 | Social relationships | 101 | 10.49 | 0.0001 | 0.89 | 0.89 | |
| D5 | Environment | 101 | 32.05 | 0.0001 | 0.91 | 0.91 | |
| D6 | Spirituality | 105 | 3.85 | 0.001 | 0.90 | 0.90 | |
Two other results require comment. First, positive mood is not associated with any facets in the physical domain, suggesting that perceptions of physical state are evaluated independently from good mood. Second, some facets outside the psychological domain were significantly associated with all the facets of the psychological domain, notably activities of daily living, financial resources, information and skills, participation and recreation and leisure but also general health and overall quality of life. This result suggests that these ratings are affected by the state of mental health during completion. This has practical implications for the administration of the instrument and interpretation of scores.
Can quality of life predict recovery from depression?
The relationship between depression and QOL was further investigated to find out whether QOL at the start of treatment might predict outcomes of depression later. Facets were first pre-selected for inclusion in a multiple regression by inspecting Pearson correlations between BDI scores (Time 2) and the 24 facets (not G) at Time 1. There were 22 significant, moderate, negative correlations. Owing to the large number of variables and sample size involved, the 22 facets were grouped by parent domain (independent variables) and entered into separate stepwise multiple regression analyses (BDI as dependent variable) to find out which facets were the best predictors in each domain. Facets on energy, positive feelings, dependence on medication, personal relationships, financial resources, physical environments and spirituality, resulting from these domain analyses, were then entered into a second regression of the best facets from all domains. The best single predictor of depression severity after 8 weeks was found to be the level of positive feelings expressed by patients at the beginning of treatment (26%). This provides limited evidence of predictive validity for the WHOQOL-100 facets but does have some practical implications.
Properties of the WHOQOL-100
Reliability (internal consistency)
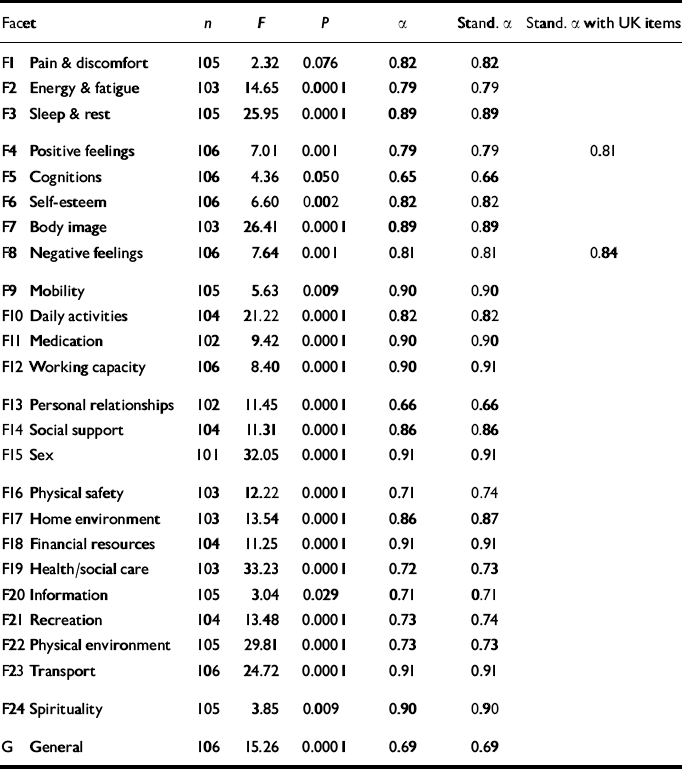
Cronbach's α (and standardised α) were calculated for the total scale of the WHOQOL-100 and obtained an excellent value of 0.96. When the six domains were similarly analysed, internal consistency reliability for independence, environment and spirituality exceeded 0.9, and the other three domains showed very good α values of 0.82-0.89 (Table 4). Six facets exceeded the 0.9 criterion that permits the individual interpretation of scores: mobility, working capacity, sex, finances, transport (to health care), and spirituality (religion and personal beliefs) (Table 5). Three facets showed marginally acceptable results — personal relationships, cognitions and general health — and so scores from these facets should be interpreted carefully. The inclusion of two national items marginally improves the internal consistency of the positive and negative feelings facets. Throughout the results, analyses have been conducted with and without national items to assess their contribution to the UK WHOQOL-100.
Table 5 Internal consistency of World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) facets (F) for patients with moderate depression
| Facet | n | F | P | α | Stand. α | Stand. α with UK items |
|---|---|---|---|---|---|---|
| F1 Pain & discomfort | 105 | 2.32 | 0.076 | 0.82 | 0.82 | |
| F2 Energy & fatigue | 103 | 14.65 | 0.0001 | 0.79 | 0.79 | |
| F3 Sleep & rest | 105 | 25.95 | 0.0001 | 0.89 | 0.89 | |
| F4 Positive feelings | 106 | 7.01 | 0.001 | 0.79 | 0.79 | 0.81 |
| F5 Cognitions | 106 | 4.36 | 0.050 | 0.65 | 0.66 | |
| F6 Self-esteem | 106 | 6.60 | 0.002 | 0.82 | 0.82 | |
| F7 Body image | 103 | 26.41 | 0.0001 | 0.89 | 0.89 | |
| F8 Negative feelings | 106 | 7.64 | 0.001 | 0.81 | 0.81 | 0.84 |
| F9 Mobility | 105 | 5.63 | 0.009 | 0.90 | 0.90 | |
| F10 Daily activities | 104 | 21.22 | 0.0001 | 0.82 | 0.82 | |
| F11 Medication | 102 | 9.42 | 0.0001 | 0.90 | 0.90 | |
| F12 Working capacity | 106 | 8.40 | 0.0001 | 0.90 | 0.91 | |
| F13 Personal relationships | 102 | 11.45 | 0.0001 | 0.66 | 0.66 | |
| F14 Social support | 104 | 11.31 | 0.0001 | 0.86 | 0.86 | |
| F15 Sex | 101 | 32.05 | 0.0001 | 0.91 | 0.91 | |
| F16 Physical safety | 103 | 12.22 | 0.0001 | 0.71 | 0.74 | |
| F17 Home environment | 103 | 13.54 | 0.0001 | 0.86 | 0.87 | |
| F18 Financial resources | 104 | 11.25 | 0.0001 | 0.91 | 0.91 | |
| F19 Health/social care | 103 | 33.23 | 0.0001 | 0.72 | 0.73 | |
| F20 Information | 105 | 3.04 | 0.029 | 0.71 | 0.71 | |
| F21 Recreation | 104 | 13.48 | 0.0001 | 0.73 | 0.74 | |
| F22 Physical environment | 105 | 29.81 | 0.0001 | 0.73 | 0.73 | |
| F23 Transport | 106 | 24.72 | 0.0001 | 0.91 | 0.91 | |
| F24 Spirituality | 105 | 3.85 | 0.009 | 0.90 | 0.90 | |
| G General | 106 | 15.26 | 0.0001 | 0.69 | 0.69 |
Validity
It was important to examine the relationship between domains and between facets to investigate the construct, convergent and divergent validity of the WHOQOL-100. Good construct validity requires that domains and facets should correlate significantly and positively.
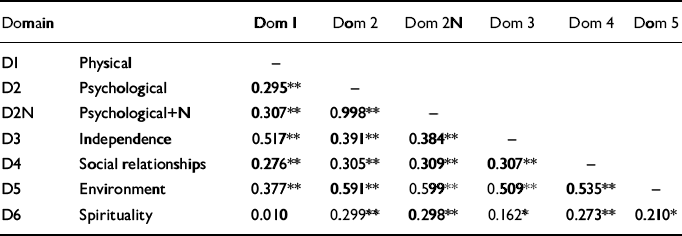
The proposed domain structure for the international WHOQOL-100 was largely confirmed by the UK data (construct validity), except for spirituality, which correlates weakly with physical health and independence (Table 6). Correlations between facets (25 × 25; not shown) were expected to be high within the parent domain (convergent validity) and all facets within Domains 1 to 5 were confirmed to be highly significant and positively correlated with other facets in the parent domain (P<0.01). There were 5 weaker results (P<0.05) but only one non-significant correlation (r=0.13) between home environment and information. Correlations with facets outside the designated domain (divergent validity) were generally weaker than with those inside except where, a priori, an association was expected due to the nature of clinical depression (see section on Mood). Overall, the results show that the WHOQOL-100 domains and facets have high construct, convergent and divergent validity.
Table 6 Pearson's correlations (I-tailed) between World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) domains (D)
| Domain | Dom 1 | Dom 2 | Dom 2N | Dom 3 | Dom 4 | Dom 5 | |
|---|---|---|---|---|---|---|---|
| D1 | Physical | — | |||||
| D2 | Psychological | 0.295** | — | ||||
| D2N | Psychological+N | 0.307** | 0.998** | — | |||
| D3 | Independence | 0.517** | 0.391** | 0.384** | — | ||
| D4 | Social relationships | 0.276** | 0.305** | 0.309** | 0.307** | — | |
| D5 | Environment | 0.377** | 0.591** | 0.599** | 0.509** | 0.535** | — |
| D6 | Spirituality | 0.010 | 0.299** | 0.298** | 0.162* | 0.273** | 0.210* |
Discriminatory power
Are QOL scores different for patients with different levels of depression? If the WHOQOL-100 has high discriminatory power, then patients with the severest depression should provide scores that indicate the worst QOL and those with the mildest depression, better QOL. The sample was divided into four groups on the basis of BDI scores obtained at Time 1: normal functioning (0), mild to moderate (1), moderate to severe (2) and extremely severe depression (3). One-way analysis of variance was performed on facet, then domain scores for these groups (applying a Scheffé post hoc test of comparisons). A significant difference was found between all four categories for four out of six domains: physical, psychological, social relationships and environment. For 15 of the 25 facets, WHOQOL-100 scores significantly discriminate between patients in each category of depression (12 at P=0.0001 level), confirming that those with the poorest QOL were the most severely depressed. Discriminatory power was found for energy, sleep and rest, positive and negative feelings, cognitions, self-esteem, body image, daily activities, dependence on medication/treatments, personal relationships, social support, physical safety, home environment, financial resources, and recreation and leisure. In those facets where significance was not obtained, all means were in the expected direction. As working capacity and sex had up to 5% of missing data, this may have undermined the test of discriminatory power for these facets. The discriminatory power of the WHOQOL-100 was especially good for the psychological domain (as expected from the nature of the sample), particularly positive and negative feelings.
DISCUSSION
Antidepressant medication improves quality of life
An important clinical finding of this study is that QOL improves for moderately depressed patients on 24 out of 25 important dimensions in the 2 months following the start of antidepressant medication. This study of the natural history of depression demonstrates the subjective benefits of pharmacological treatment for those with depression in primary care. Perceived dependence on medication was the only dimension of QOL that did not change during that period. Substantial improvements can be achieved within a relatively short period, and for a majority (74%) of patients the results reaffirm the importance of treating depression in primary care and treating it well. Because depression in primary care is such a common complaint, the findings have widespread applicability and could increase confidence in the use of antidepressants by GPs, thus reducing the number of patients needing in-patient care. Admissions to hospital account for the highest proportion of the treatment bill in depression (Reference Kind and SorensonKind & Sorenson, 1993), so successful drug treatment in primary care that is known to improve QOL could provide a leaner, more cost-effective health service, while simultaneously providing tangible benefits to sufferers.
WHOQOL-100 is valid and sensitive to clinical changes
Validity and sensitivity for the WHOQOL-100 is now established. Clinicians particularly need to know that the scores of a measure show sensitivity to changes in clinical condition. Here it was found that 96% of the WHOQOL-100 facets are responsive to perceived changes in clinical depression. Lack of sensitivity to change has been viewed by some authorities as a relative weakness of generic instruments (compared to disease-specific measures) but here the WHOQOL-100 sensitivity tests perform very highly. These findings should encourage researchers and clinicians to consider using the WHOQOL-100 in preference to less comprehensive instruments with poorer psychometric properties that were designed specifically for depression. Generic instruments enable comparisons to be made between depression and many other types of psychological and physical disorder. Also, the WHOQOL-100 is one of the most comprehensive assessments of QOL available. The UK version of the WHOQOL-100 is shown to have very good construct, convergent and divergent validity and discriminatory power. The power of the WHOQOL-100 scores to discriminate between patients with different levels of depression severity was good in 15 out of 25 facets. Excellent internal consistency reliability is reconfirmed for the UK instrument using this sample (Reference SkevingtonSkevington, 1999). The results show that the UK WHOQOL-100 could be a very useful clinical tool for studies of this disorder, in audit and for clinical governance procedures. As a result of this research, this scale is now ready for use in UK clinical trials.
Restoring happiness and contentment
Lastly, a model of the relationship between QOL and depression may have direct implications for clinical practice. Of interest here was whether aspects of QOL at the end of the study were predictable from the severity of depression at the start of treatment, and it was shown that those with the poorest levels of perceived happiness and contentment at the start were most likely to be depressed later. So the emptiness or void of happiness or contentment in life at the time treatment begins appears to maintain depression, acting as a barrier to later recovery. The monitoring of improvements in happiness and contentment during a course of antidepressants could enable better predictions to be made about whether patients will recover. Counselling and re-orientation therapies might be suitable vehicles for restoring a perceived shortage of the good things in life for those with moderate depression.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The quality of life of primary care patients with moderate depression improves significantly on a wide range of important dimensions (facets) during the 8 weeks following the start of antidepressant medication. Substantial improvements can be achieved for the majority of patients (74%) and within a relatively short time.
-
▪ The World Health Organization Quality of Life Assessment (100-item version) (WHOQOL-100) is validated for use in the UK and can now be used with confidence in clinical work. Most dimensions show sensitivity to changes in clinical condition, such as improvements in symptom severity. It is also reliable.
-
▪ Mood (positive and negative) influences the way patients report many aspects of their quality of life. Positive and negative mood are not synonymous with quality of life but are two of its many important components, as the comprehensive, multi-dimensional assessment of the WHOQOL-100 shows.
LIMITATIONS
-
▪ A study with a larger sample and multiple centres is needed to investigate changes in quality of life following a longer natural history of depression.
-
▪ Patients over 65 years old with depression need a version of the WHOQOL-100 that is specially adapted to their needs; this is in prospect.
-
▪ A different procedure is required to access more patients who did not complete the questionnaires on a second occasion.
ACKNOWLEDGEMENTS
We are greatly indebted to all the general practitioners who helped to make this study possible. Special thanks go to Dr J. Verity, Ludgershall Health Centre, Hants; Dr J. Stone, Castle Street Surgery, Salisbury; Dr M. Mackintosh, Southmead Health Centre, Bristol; Dr R. While, Jubilee Field Surgery, Yatton Keynell, Wilts; Dr G. Walker, Oldfield Surgery, Bath; Dr S. Cembrowicz, Montpellier Health Centre, Bristol; Dr S. Thomas and Dr N. Taylor, Bradgate Surgery, Brentry, Bristol; Dr M. Moore and Dr E. Stanger, Three Swans Surgery, Salisbury, Wilts; and Dr Hodgkinson, Salisbury, Wilts. We would also like to thank practice managers and surgery staff for their help and cooperation. Thanks also to Professor P. Milner, Sarah Walker and Audrie Beaver from Wiltshire Health Authority, Devizes; Dr V. Wood in the Postgraduate Medical School, Bath University and Pat Turton, Dept of Primary Care, University of Bristol, who helped us in the early stages of the research. We acknowledge valued pharmacological advice from Professor P. Redfern, Dept of Pharmacy and Pharmacology, University of Bath.
The paper is based on experience obtained as part of the WHO study to develop a quality of life (QOL) measure (WHOQOL). The collaborators in this study have been at WHO Geneva: Dr J. Orley assisted by Dr Willem Kuyken, Dr Norman Sartorius, Dr R. Billington and Dr Mick Power. In the Field Research Centres, collaborating investigators are Professor Helen Herrman, Dr H. Schofield and Ms B. Murphy, University of Melbourne, Australia; Professor Z. Metelko, Professor S. Szabo and Mrs M. Pibernik-Okanovic, Institute of Diabetes, Endocrinology and Metabolic Diseases and Dept of Psychology, Faculty of Philosophy, University of Zagreb, Croatia; Dr N. Quemada and Dr A. Caria, INSERM, Paris, France; Dr S. Rajkumar and Mrs Shuba Kumar, Madras Medical College, India; Dr S. Saxena, All India Institute of Medical Sciences, Delhi, India; Dr D. Bar-On and Dr M. Amir, Ben Gurion University, Beer Sheeva, Israel; Dr Miyako Tazaki, Dept of Science, Science University of Tokyo, Japan; Dr Ariko Noji, Dept of Community Health Nursing, St Luke's College of Nursing, Japan; Dr G. van Heck and Mrs J. de Vries, Tilburg University, The Netherlands; Professor J. Arroyo-Sucre and Professor Pichard-Ami, University of Panama, Panama; Professor M. Kabanov, Dr A. Lomachenkov and Dr G. Burkovsky, Bekhterev Psychoneurological Institute, St Petersburg, Russia; Dr R. Lucas Carrasco, Barcelona, Spain; Dr Y. Bodharamik and Mr Kitikorn Meesapya, Institute of Mental Health, Bangkok, Thailand; Dr D. Patrick, Ms M. Martin and Ms D. Wild, University of Washington, Seattle, USA; and Professor W. Acuda and Dr J. Mutambirwa, University of Zimbabwe, Harare, Zimbabwe.
An international panel of consultants includes: Dr N. K. Aaronson, Dr P. Bech, Dr M. Bullinger, Dr HeNian Chen, Dr J. Fox-Rushby, Dr C. Moinpur and Dr R. Rosser. Consultants who have advised WHO at various stages of the development of the project have included: Dr D. Buesching, Dr D. Bucquet, Dr L. W. Chambers, Dr B. Jambon, Dr C. D. Jenkinson, Dr D. De Leo, Dr L. Fallowfield, Dr P. Gerin, Dr P. Graham, Dr O. Gureje, Dr K. Kalumba, Dr KerrCorea, Dr C. Mercier, Mr J. Oliver, Dr Y. H. Poortinga, Dr R. Trotter and Dr F. van Dam.











eLetters
No eLetters have been published for this article.