Self-exposure therapy for panic/agoraphobia is effective using exposure to frightening external cues (Reference Marks, Swinson and BasogluMarks et al, 1993) but less tested for exposure to frightening internal (interoceptive) cues (Reference Ito, Noshirvani and BasogluIto et al, 1996). In a randomised controlled trial (RCT), interoceptive exposure decreased panics when it was combined with breathing retraining and cognitive restructuring (Reference Clark, Salkovskis and HackmanClark et al, 1994) but it was not tested alone. In RCTs, interoceptive exposure and breathing retraining given with cognitive restructuring, exposure to external cues, or both combined (Reference Clark, Salkovskis and HackmanClark et al, 1994; Reference Craske, Rowe and LewinCraske et al, 1997) reduced phobic avoidance and panics. No RCT in panic/agoraphobia has yet compared interoceptive exposure on its own with exposure to external cues.
The present study compares self-exposure to external cues, to interoceptive cues, and to both combined, and compares those three self-exposure conditions with a control group. Both interoceptive groups were trained in slow deep breathing after self-exposure to interoceptive cues.
METHOD
Design
Eighty out-patients who had panic disorder plus agoraphobia were randomised to a control group or to one of three groups having self-exposure treatments using (a) external cues (group E), or (b) interoceptive cues (group I) or (c) both external and interoceptive cues (group E+I). Patients in groups E, I and E+I had seven 60-minute sessions over 10 weeks of corresponding self-exposure and were asked to carry out 60 minutes of corresponding daily homework. Control-group patients were offered random reassignment to groups E, I or E+I at week 10. Follow-up was at 24, 36 and 62 weeks after entry. Cell size needed for a power of 80% between group E and the control group was estimated at 5 based on a mean (s.d.) expected improvement in phobic target avoidance of 9 (4), a pre— post-treatment correlation of 0.05, and a significance level of 0.05.
Subjects
These were mostly self-referred (69%) out-patients who sought help after reading an article in the lay press. Inclusion criteria were panic disorder with agoraphobia (semi-structured interview based on DSM—IV criteria; American Psychiatric Association, 1994) for at least 1 year; age 18 to 65; absence of suicidal intent, organic brain disease, past or present psychosis, psychotropic medication or excess alcohol (ingestion of 30 or more alcohol units/week); no response to exposure in the past 2 years; no other current psychotherapy. Patients on benzodiazepines had to withdraw and be drug-free for at least 2 weeks before study entry because of the drugs' negative interaction with exposure treatments. Those on a stable dose of antidepressant without improvement for at least 12 weeks were asked to maintain that dose throughout the study. The study protocol was approved by the university ethics committee.
Referred patients had a 1-hour screening interview for diagnosis and clinical features, and knew they might enter the untreated control group for 10 weeks. Suitable patients gave written consent and were self- and assessor-rated (by L.M.I. and L.A.D.A.) and then randomly assigned in permuted blocks (Reference PocockPocock, 1990) to groups E, I, E+I or control for balance.
Therapists used procedure and treatment manuals (Reference Barlow and CraskeBarlow & Craske, 1988) covering each session for each condition. Groups E, I and E+I patients had seven treatment sessions at weeks 0, 1, 2, 4, 6, 8 and 10.
At week 0, all self-exposure patients (groups E, I and E+I) met the therapist, who explained that panics are part of an anxiety response with behavioural and physical symptoms which can be unpleasant but not dangerous. A self-exposure rationale corresponding to E, I or E+I conditions was also given on a printed sheet that patients were asked to read. Group I and group E+I patients were taught to slow their breathing to lower anxiety after interoceptive exposure exercises.
At sessions 1 and 2 (weeks 0 and 1) the therapist spent 45 minutes with the patient encouraging appropriate exposure and 15 minutes negotiating appropriate homework tasks. Sessions 3-7 lasted 30-45 minutes, with the therapist monitoring and negotiating appropriate self-exposure homework. Groups E, I and E+I patients had the same duration of within-session self-exposure and were asked to do self-exposure homework corresponding to E, I or E+I conditions for 60 minutes daily between sessions. At the end of treatment (week 10), all self-exposure patients were told to continue during follow-up their type of self-exposure homework and to keep a diary of this (to control for the amount of exposure to tasks) to week 62 (1-year follow-up).
Self-exposure to external cues (group E)
At sessions 1 and 2, patients had 45 minutes of therapist-accompanied exposure to feared external situations, until discomfort diminished, and 15 minutes planning homework tasks.
Self-exposure to interoceptive cues (group I)
At sessions 1 and 2, patients had 45 minutes of therapist-accompanied interoceptive exposure exercises and 15 minutes planning interoceptive homework tasks. The therapist showed patients how to induce sensations like those experienced during their panics (e.g. rapid breathing, palpitations, dizziness) by (a) hyperventilating for up to a minute; (b) shaking their head from side to side for 30 seconds; (c) running on the spot for a minute; (d) putting their head between their legs for 30 seconds and then quickly lifting it up; (e) spinning in a chair for a minute. Patients were asked to rate how intense and similar the sensations so induced were to their usual panic feelings. They were told to stop any exercise which produced sensations without anxiety. After each exercise they learned to use slow breathing to return to their baseline anxiety level. Patients were told that their fear would lessen after they induced such sensations repeatedly in a neutral environment.
Self-exposure to both external and interoceptive cues (group E+I)
At sessions 1 and 2, patients had 30 minutes of therapist-accompanied exposure to the frightening external situations while remaining there until discomfort diminished, 15 minutes of therapist-accompanied interoceptive exposure plus training in slow breathing, and 15 minutes negotiating appropriate daily homework tasks comprising 30 minutes of live exposure and 30 minutes of interoceptive exposure.
Control group
At session 1 patients were told that their symptoms could improve without treatment and that they would have to wait for 10 weeks to receive treatment if they still needed it after that period. They could return for advice if their clinical condition worsened.
The therapists
These were four psychiatrists and a psychologist experienced in behaviour therapy for anxiety disorders. A psychiatrist (L.A.D.A.) and a clinical psychologist (L.M.I.) treated most of the patients, each treating similar numbers across the four treatment conditions over 3 years.
ASSESSMENT
Assessors and rating times
At weeks 0, 6, 10, 24 (3-month follow-up), 36 (6-month follow-up) and 62 (1-year follow-up), measures were rated by patients and by two independent blind assessors (L.A.D.A. or L.M.I.). Patients were not assessed by their own therapist and were asked not to reveal any information about their treatment group to their assessor.
Measures
These were validated reliable scales used in past trials. Higher scores denoted more abnormality.
Assessor- and self-ratings were of: two phobic targets (Reference Gelder and MarksGelder & Marks, 1966), for avoidance and for fear (each score range 0-16); four work/social adjustment items (Reference MarksMarks, 1975), each scored 0-8 (total score range 0-32).
Self-ratings were of: Fear Questionnaire (FQT; Reference Marks and MathewsMarks & Mathews, 1979), containing 15 phobic avoidance 0-8 items (total score range 0-120) and including five agoraphobic items making up an agoraphobia subscore (FQAg), range 0-40; Agoraphobic Cognitions Questionnaire (Reference Chambless, Caputo and BrightChambless et al, 1984) for frequency, score range 14-70; diary of panic (DSM-IV criteria) frequency over 2 weeks; Beck Depression Inventory (BDI; Reference Beck, Rial and RickelsBeck et al, 1974), including 21 items, total score range 0-63.
Assessor-ratings were of: Hamilton Anxiety Scale (HAS; Reference HamiltonHamilton, 1959), score range 0-56 and Clinical Global Impression (CGI) scale modified (Reference GuyGuy, 1976): illness severity, score range 0-8 (0=not ill; 8=extremely ill).
Statistics
Multivariate analyses of variance (MANOVAs) compared the four treatment groups on the main outcome measures repeated on five occasions (weeks 0, 6, 10, 36, 62). Analysis of treatment group × time and its interactions tested for significant differences among the three self-exposure groups (E, I and E+I) and the control group across weeks 0-10. The three self-exposure groups were also compared with one another on the main outcome measures from weeks 0-62. χ2 tests for non-parametric and analysis of variance (ANOVA) for parametric data compared groups E, I and E+I on clinical and demographic features at baseline.
RESULTS
Patient flow
Ninety patients met the inclusion criteria and were offered treatment; 20 did not return (9 in group E, 2 in group I, 7 in group E+I, 2 in the control group) and 70 began treatment. The total sample of 80 patients (21 in E, 20 in I, 21 in E+I, 18 in the control group) included 10 of the control group who were re-randomised to groups E, I, or E+I. Five patients (1 in E, 2 in I, 2 in E+I) left treatment during weeks 6-10 and another five (2 in E, 1 in I, 2 in E+I) during follow-up to week 62. Seventy-five patients were included in the statistical analysis to week 10, and 52 patients to week 62.
Baseline features
The 70 patients included in the study resembled those in other panic/agoraphobia studies. Fifty-one (64%) were women. Mean age was 37 (s.d. 11), mean onset age 29 (s.d. 10), and mean illness duration 7 years (s.d. 8). Most were in a stable relationship (67%), 83% were Caucasian and 67% had completed college or university. All had panic disorder with agoraphobia: mean assessor-rated phobic target avoidance was 13 (s.d. 2.8, range 0-16) and FQAg was 21 (s.d. 11, range 0-40). Mean BDI scores were 20 (s.d. 10, range 0-63). Thirty-four patients had comorbid symptoms: depression (17%), general anxiety (17%), social phobia (6%), specific phobia (4%) and mixed (5%) at baseline. Most (67%) had had past psychiatric treatment, mainly for panic/agoraphobia (58%). Half had had antidepressants or benzodiazepines and 33% psychodynamic psychotherapy. Of the 70 patients who began treatment, eight (11%) were on antidepressants, 17 (24%) on benzodiazepines and 5 (7%) on both. Demographic and clinical data did not differ significantly among the four treatment groups on χ2 tests.
Reliability of measures
At week 0, two assessors rated the first 20 patients independently in the same interview on phobic avoidance, fear, and work/social adjustment to check reliability. Pearson and intraclass correlation between the two assessors' ratings were respectively 0.82-0.95 (P<0.001) and 0.94-0.98 (P<0.0001). Self v. assessor reliability was tested at weeks 0 and 10. Pearson correlations for the three measures were highly significant (P<0.0001) at weeks 0 (0.68-0.77) and 10 (0.80-0.85). Intraclass correlations were highly significant (0.54-0.96; P<0.001) for all measures at week 0, at week 10 they were highly significant (0.55-0.84; P<0.001) for phobic avoidance and fear, less so for social adjustment (0.50; P<0.05).
Improvement during treatment
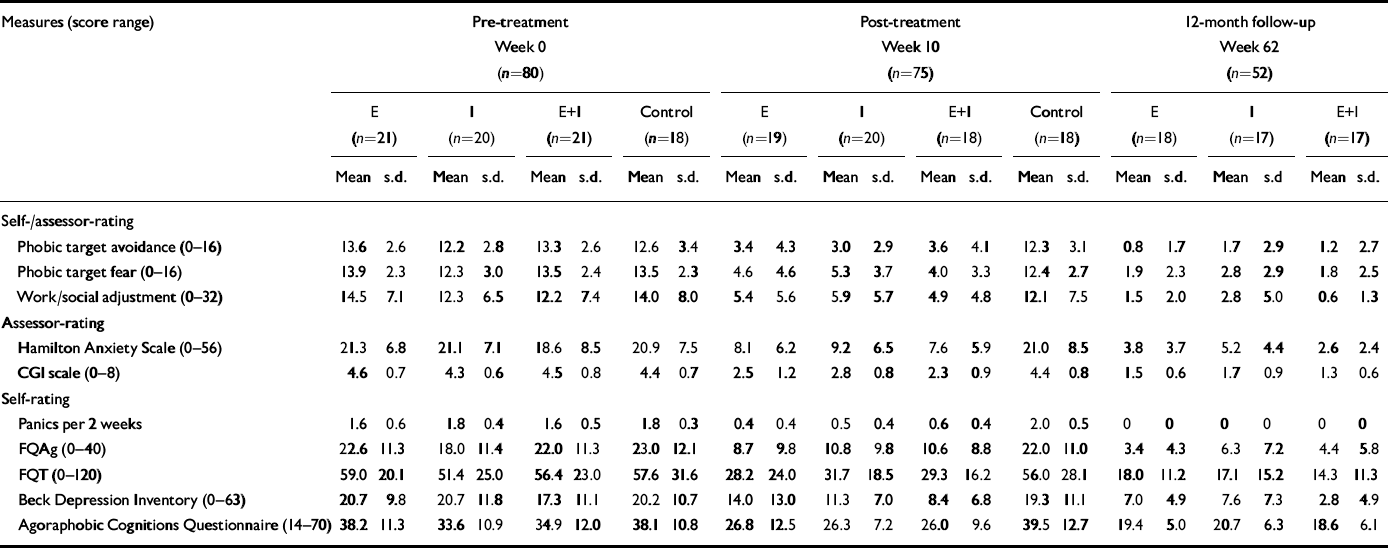
Table 1 shows means (s.d.) of the averaged self- and assessor-ratings for phobic target avoidance, phobic target fear and work/social adjustment and the other outcome measures for the three self-exposure groups and the control group, and Fig. 1 shows means of those four groups at weeks 0, 6, 10, 24, 36 and 62 on target avoidance, the HAS, CGI scale and Agoraphobic Cognitions Scale. Groups E, I or E+I (total n=62) each improved significantly (P<0.001) and similarly (P n.s. on between-group comparisons) and significantly (P<0.001) more than control group patients (n=18) on all 10 outcome measures from weeks 0-10. Effect sizes for the three self-exposure groups were all large in comparison to the control group at post-treatment on phobic target avoidance (E 2.5; I 3; E+I 1.6). The three self-exposure groups were pooled and a percentage of clinical improvement was calculated by subtracting week 0 from week 10 scores and dividing by week 0 scores on the main measures. At week 10 this was 74% for phobic target avoidance and 41% for the CGI scale.

Fig. 1 Main outcome measures by treatment group; fu, follow-up.
Table 1 Treatment group comparisons
| Measures (score range) | Pre-treatment Week 0 (n=80) | Post-treatment Week 10 (n=75) | 12-month follow-up Week 62 (n=52) | |||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| E (n=21) | I (n=20) | E+I (n=21) | Control (n=18) | E (n=19) | I (n=20) | E+I (n=18) | Control (n=18) | E (n=18) | I (n=17) | E+I (n=17) | ||||||||||||
| Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | Mean | s.d. | |
| Self-/assessor-rating | ||||||||||||||||||||||
| Phobic target avoidance (0-16) | 13.6 | 2.6 | 12.2 | 2.8 | 13.3 | 2.6 | 12.6 | 3.4 | 3.4 | 4.3 | 3.0 | 2.9 | 3.6 | 4.1 | 12.3 | 3.1 | 0.8 | 1.7 | 1.7 | 2.9 | 1.2 | 2.7 |
| Phobic target fear (0-16) | 13.9 | 2.3 | 12.3 | 3.0 | 13.5 | 2.4 | 13.5 | 2.3 | 4.6 | 4.6 | 5.3 | 3.7 | 4.0 | 3.3 | 12.4 | 2.7 | 1.9 | 2.3 | 2.8 | 2.9 | 1.8 | 2.5 |
| Work/social adjustment (0-32) | 14.5 | 7.1 | 12.3 | 6.5 | 12.2 | 7.4 | 14.0 | 8.0 | 5.4 | 5.6 | 5.9 | 5.7 | 4.9 | 4.8 | 12.1 | 7.5 | 1.5 | 2.0 | 2.8 | 5.0 | 0.6 | 1.3 |
| Assessor-rating | ||||||||||||||||||||||
| Hamilton Anxiety Scale (0-56) | 21.3 | 6.8 | 21.1 | 7.1 | 18.6 | 8.5 | 20.9 | 7.5 | 8.1 | 6.2 | 9.2 | 6.5 | 7.6 | 5.9 | 21.0 | 8.5 | 3.8 | 3.7 | 5.2 | 4.4 | 2.6 | 2.4 |
| CGI scale (0-8) | 4.6 | 0.7 | 4.3 | 0.6 | 4.5 | 0.8 | 4.4 | 0.7 | 2.5 | 1.2 | 2.8 | 0.8 | 2.3 | 0.9 | 4.4 | 0.8 | 1.5 | 0.6 | 1.7 | 0.9 | 1.3 | 0.6 |
| Self-rating | ||||||||||||||||||||||
| Panics per 2 weeks | 1.6 | 0.6 | 1.8 | 0.4 | 1.6 | 0.5 | 1.8 | 0.3 | 0.4 | 0.4 | 0.5 | 0.4 | 0.6 | 0.4 | 2.0 | 0.5 | 0 | 0 | 0 | 0 | 0 | 0 |
| FQAg (0-40) | 22.6 | 11.3 | 18.0 | 11.4 | 22.0 | 11.3 | 23.0 | 12.1 | 8.7 | 9.8 | 10.8 | 9.8 | 10.6 | 8.8 | 22.0 | 11.0 | 3.4 | 4.3 | 6.3 | 7.2 | 4.4 | 5.8 |
| FQT (0-120) | 59.0 | 20.1 | 51.4 | 25.0 | 56.4 | 23.0 | 57.6 | 31.6 | 28.2 | 24.0 | 31.7 | 18.5 | 29.3 | 16.2 | 56.0 | 28.1 | 18.0 | 11.2 | 17.1 | 15.2 | 14.3 | 11.3 |
| Beck Depression Inventory (0-63) | 20.7 | 9.8 | 20.7 | 11.8 | 17.3 | 11.1 | 20.2 | 10.7 | 14.0 | 13.0 | 11.3 | 7.0 | 8.4 | 6.8 | 19.3 | 11.1 | 7.0 | 4.9 | 7.6 | 7.3 | 2.8 | 4.9 |
| Agoraphobic Cognitions Questionnaire (14-70) | 38.2 | 11.3 | 33.6 | 10.9 | 34.9 | 12.0 | 38.1 | 10.8 | 26.8 | 12.5 | 26.3 | 7.2 | 26.0 | 9.6 | 39.5 | 12.7 | 19.4 | 5.0 | 20.7 | 6.3 | 18.6 | 6.1 |
Follow-up results
Fifty-two patients were followed up from weeks 10-62. During this time most kept their gains or improved further (Fig. 1). The three self-exposure groups did not differ significantly from one another on the main outcome measures from weeks 0-62. Effect sizes increased at 1 year follow-up for groups E, I and E+I, on phobic target avoidance (E 4.7; I 3.5; E+I 3.8), CGI (E 4.1; I 3.3; E+I 4.3) and HAS (E 2.8; I 3.5; E+I 3.4). Clinical improvements additional to those at post-treatment were 17% for phobic target avoidance and 16% for CGI. Eight (2 in E; 2 in I; 4 in E+I) of 52 patients had 1 or 2 booster sessions for anxiety during follow-up.
Assessor blindness
Patients were asked not to tell the assessor anything about their treatment and homework tasks. At week 10 the assessor was asked to guess the patient's treatment condition. Correctness of guesses was 30%, a rate to be expected by chance.
Refusers, drop-outs and non-completers
Twenty patients (9 in E; 2 in I; 7 in E+I; 2 in control group) left the trial before week 4 and were replaced. Of the 18 control group patients assessed at week 10, eight did not return for subsequent self-exposure treatment, four developed depression and had to be referred to pharmacotherapy and four sought treatment elsewhere. Among the three self-exposure groups, five patients (2 in E; 2 in I; 1 in E+I) dropped out between weeks 6 and 10 and another five (1 in E; 2 in I; 2 in E+I) between weeks 10 and 62 - a low total drop-out rate of 12% (3 in E; 3 in I; 4 in E+I). Drop-outs were mainly because of the inconvenience of attending, lack of improvement or depression.
Concurrent use of medication
Thirteen patients were on either antidepressants, benzodiazepines or both at baseline. Five patients were in the control group and three of those were reallocated to the self-exposure groups (n=11: 3 in E, 6 in I, 2 in E+I). Patients who were on antidepressants and those who were not did not differ significantly on t-tests.
Intent-to-treat analyses
This was done for the 90 patients randomised in the trial to test for differences between the four treatment groups regarding improvement from weeks 0 to 10 and weeks 10 to 62. Patients who dropped out before week 4 (20 refusers: 9 in E; 2 in I; 7 in E+I; 2 in control group) and between weeks 6 and 10 (five drop-outs) were considered non-successes. Completers who improved by at least 30% on the CGI scale at week 10 were rated as successes (12 in E; 1 in I; 11 in E+I). The three treatment conditions did not differ significantly on χ2 tests regarding drop-out and success/non-success rates to week 10 or 62.
DISCUSSION
The present study found similar clinical improvement from three forms of self-exposure (to frightening cues that were external (E) or interoceptive (I) or both (E+I)). Gains included change in cognitions (catastrophic thoughts and misinterpretations related to panics), despite the absence of cognitive restructuring instruction. Each of the three self-exposure groups were given the same printed self-exposure rationale. Group E patients had no breathing retraining or other instruction encouraging interoceptive exposure; group I patients had no instructions to do external exposure.
The three self-exposure treatments reduced panic and agoraphobia equally well through weeks 10-62. Although control group patients had no meetings with therapists that might give an ‘attention-placebo’ effect, the three self-exposure groups' similar improvements in agoraphobia were unlikely to be due to an attention-placebo effect, as other panic/agoraphobia studies found little change following attention given with reassurance (Reference Swinson, Soulios and CoxSwinson et al, 1992), relaxation (Reference Marks, Swinson and BasogluMarks et al, 1993), or anti-exposure instructions (Reference Telch, Agras and TaylorTelch et al, 1985). In one study, teaching a control group relaxation techniques (‘relaxation-placebo’) improved panics but not agoraphobia (Reference Marks, Swinson and BasogluMarks et al, 1993).
Perhaps reducing differing elements of the fear network led to similar knock-on improvements in other elements, with the lessening of fear of external cues also lowering fear of internal cues and vice versa. A further possibility is that group I patients improved from the breathing retraining that was present in groups I and E+I but not in group E; this requires further study by giving interoceptive exposure without breathing retraining. Group I had fewer refusals than either groups E or E+I between weeks 0 and 4, which might be due to a smaller rise of anxiety in group I early in treatment (Reference Foa, Steketee, Grayson, Foa and EmmelkampFoa et al, 1983).
Patients in all three self-exposure groups were told briefly that panic and anxiety are not harmful. Shear et al (Reference Shear, Pilkonis and Cloitre1994) found no difference between exposure (external and interoceptive cues) plus cognitive restructuring plus breathing retraining plus relaxation v. a non-prescriptive programme that educated patients about the harmlessness of panic. This alone might reduce panic. Perhaps group I patients learned to cope with panic symptoms, so encouraging them to do E-type homework, but this was not measured in the study. No anti-exposure instructions were given to group I patients that might have stopped them from doing self-exposure to external cues. The role of group E exposure homework deserves more investigation in future research.
A non-significant trend favoured group E+I conditions at post-treatment and at follow-up. Was our sample size too small to detect significant but subtle differences in treatment effects between groups? If so, the clinical meaningfulness of such differences is debatable. Comparisons between exposure and non-exposure groups of patients commonly yield significant differences with cell sizes of merely five, whereas our cell sizes were over thrice that.
Most of the present patients had panic disorder with agoraphobia. It is worth testing whether group I conditions would produce even more improvement in panic disorder without agoraphobia.
Of present patients, 69% were self-referrals. The sample as a whole was severely disturbed on initial main phobic target, FQAg and total phobia (FQT) scores, and moderately depressed on the BDI (as much as mainly doctor-referred patients at I.M.'s unit in London). Their posttreatment improvement, too, resembled that usually obtained in the unit. It would be hard to invoke undetected differences in self- v. doctor-referred patients as explaining the absence of differences between groups, E, I and E+I.
In conclusion, self-exposure to external or to interoceptive cues each improved panic disorder plus agoraphobia significantly and similarly up to 1 year after treatment ended, and each was better than a 10-week waiting-list control condition. Combining the two forms of exposure was not synergistic.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Self-exposure to either external or interoceptive cues can produce lasting clinical benefit in patients with both panic disorder and agoraphobia.
-
▪ The combination of self-exposure to external and to interoceptive cues is not superior to either alone.
-
▪ Self-exposure to external cues is more easily administered and may be better as the first approach.
LIMITATIONS
-
▪ The study did not control for a rationale about panic.
-
▪ External cues exposure homework was not measured in the interoceptive exposure condition.
-
▪ Further studies are required to examine the role of breathing retraining in panic reduction.







eLetters
No eLetters have been published for this article.