The importance of genetic factors in schizophrenia aetiology has long been recognised. As early as the 18th century, the British physician William Battie speculated about heredity as a cause of madness, while in the first years of the 19th century Esquirol regarded 23% (110 of 482) of melancholic patients in the Salpêtrière and 57% (150 of 264) of patients in his private asylum as having hereditary conditions (Reference ShorterShorter, 1997). Since the early 20th century the importance of nature or nurture in relation to human behaviour, whether normal or abnormal, has been heavily debated.
The interest in genes gained momentum after the rediscovery of Mendel's laws around 1900, the year in which Sigmund Freud published Die Traumdeutung. Social Darwinism and later, sociobiology further stressed the importance of biology and genes. Misuse as part of the so-called scientific evidence for Nazi ideology discredited genetics after the Second World War. For the younger generation of psychiatrists the relevance of genetics is self-evident, but many of the generation trained during the 1950s to the 1970s have had to acquire this knowledge from the beginning.
Great efforts are now being concentrated on the identification of specific genes that increase or decrease the risk of psychiatric disorders. Furthermore, genes of importance for treatment response or side-effects of current psychotropic medication, interaction with the environment and personality factors are also being sought, as are others of importance for many aspects of brain function and development.
The development of molecular genetics has greatly strengthened the promise of such investigations, and it is generally believed that information about individual genes obtained by molecular genetic research will be necessary to advance studies on environmental factors involved in psychiatric diseases and their interplay with the involved genes. Research into the environmental components has been somewhat overshadowed, and new approaches are required (Reference Eaton and HarrisonEaton & Harrison, 1998); for example, it is increasingly recognised that the external environment is non-random, in the sense that individuals' interaction with and experience of the external environment also seems to be influenced by their genes. This has been called the ‘nature of nurture’, and interesting studies of genetic influences on experience of life events have been reported (Reference McGuffin, Katz and BebbingtonMcGuffin et al, 1988; Reference Kendler, Neale and KesslerKendler et al, 1993; Reference Kendler and Karkowski-ShumanKendler & Karkowski-Shuman, 1997).
The role of epidemiology in investigating neurobiological causal factors can best be illustrated by an example. In 1988 a now famous paper by Mednick et al was published in the Archives of General Psychiatry. The reported study was the result of clever thinking. We had for many years known about seasonal variations in birth rates of persons later developing schizophrenia, with a higher incidence among those born in winter than in summer in the northern hemisphere, and the reverse occurring in the southern hemisphere. Making the connection from this information to the influenza—schizophrenia theory may now seem obvious, but in fact psychiatry had for many years fumbled for the hypothesis that was first clearly formulated and tested in 1988. As long ago as the 1920s Menninger (Reference Menninger1928) had suggested a connection, but the critical mass of scientific methodology, knowledge and statistical material was not to hand until 60 years later. The Mednick paper was thus a breakthrough in research and stimulated many replications.
The study used case records from the Helsinki Mental Hospital's files. The authors found that individuals whose second trimester of foetal life coincided with the 1957 influenza epidemic had an increased risk of developing schizophrenia later in life. The next step was to design a larger-scale survey, controlling for more of the epidemiological variables.
The Danish National Board of Health has for almost a century registered the incidence of influenza in the whole of Denmark week by week. All these little peaks through the years were registered in a study database. A similar data-set was generated from the Danish Psychiatric Central Register (Reference Munk-J⊘rgensen and MortensenMunk-Jørgensen & Mortensen, 1997), all patients with a diagnosis of schizophrenia and subsequently reported to the register being entered according to date, month and year of birth. By comparing the two data-sets, overlap between gestation periods characterised by high, medium and low influenza incidence and birth cohorts characterised by schizophrenia incidence peaks could be searched for. Adding all the many influenza peaks and the incidence of treated schizophrenia for the corresponding birth cohorts demonstrated a significant correlation between influenza peaks in the population from 1911 to 1950 and an increased schizophrenia risk for those whose gestation coincided with influenza periods, most pronounced for those in the sixth gestation month during the influenza peak periods (Reference Barr, Mednick and Munk-J⊘rgensenBarr et al, 1990). The correlation was significant, but the finding could explain no more than 4% of total variance.
This is an example of how large-scale register epidemiology can be used to examine a statistical trend and to test whether a hypothesis is worth keeping. The various methodological problems connected with this type of epidemiological research will not be discussed here, but the salient point is that one cannot draw conclusions about causation on the basis of such correlations alone. We do not know that the relative excess of patients with schizophrenia in certain years were born to mothers who actually suffered from influenza during their pregnancies. From a statistical point of view it is just as likely that none were affected, and that those responsible for the influenza statistics were men, postmenopausal women, non-pregnant women, or women giving birth to healthy children.
The next step, therefore, was a return to Helsinki Mental Hospital. The authors (Reference Mednick, Huttunen and MachónMednick et al, 1994) read the obstetric records of women pregnant during the 1957 influenza outbreak who gave birth to children later developing schizophrenia, to see whether the women actually had been infected by influenza during the epidemic. Where definite influenza infection was recorded, 87% of women were infected in the second trimester, compared with only 20% infected in the first or the third trimester, a finding supporting the earlier register study. The authors were, however, careful to emphasise that their findings must be interpreted with caution because of the small number of cases (Reference Mednick, Huttunen and MachónMednick et al, 1994).
This comment exemplifies a general epidemiological problem. In large-scale register studies a high statistical power is gained, but the validity of the data can be questioned and the lack of clinical details in the data-sets may be obvious. On the other hand, when this is compensated for by smaller-scale direct investigations, as in the 1994 study by Mednick et al, statistical power tends to be greatly reduced owing to difficulties in obtaining sufficiently large numbers of probands.
There is now an extensive literature on the viral infection—schizophrenia theory. A Medline search performed in January 1998 using the key words INFLUENZA and SCHIZOPHRENIA found 99 entries relating to replication studies, studies testing other types of viral infection, review articles, editorials and journal correspondence, with an annual frequency peaking in 1994 (Fig. 1).
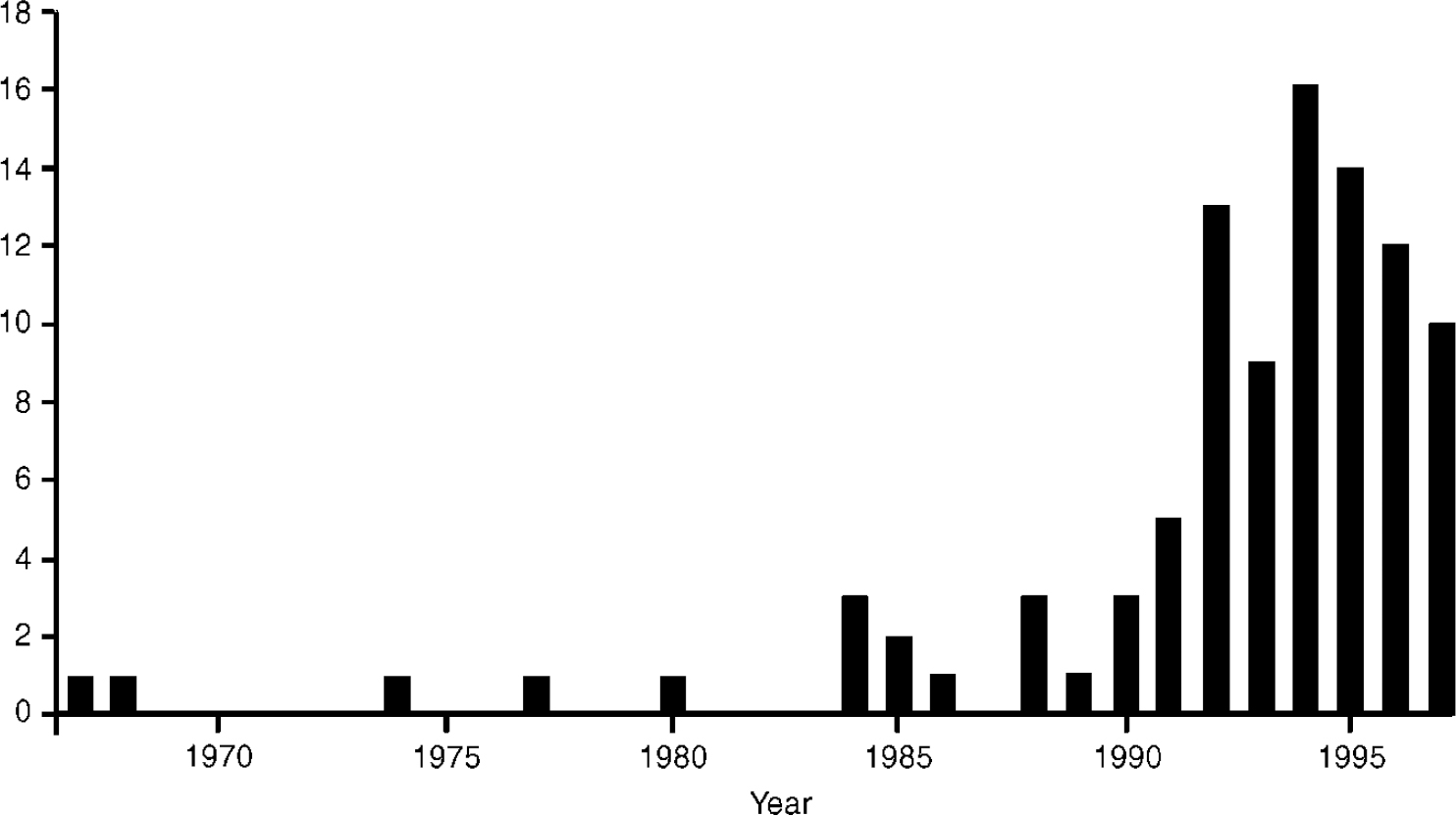
Fig. 1 Number of publications on the schizophrenia—influenza hypothesis.
In summary, the 10-year period of influenza—schizophrenia research in the 1980s and 1990s has provided strong inferential evidence that influenza infection in pregnancy, especially in the second trimester, can cause damage to the immature brain which increases the risk for schizophrenia later in life.
Almost the same story can be told for complications other than viral infections during pregnancy and birth (Reference Geddes and LawrieGeddes & Lawrie, 1995). The influenza hypothesis has become part of a more general theory of the consequences of brain damage during gestation, whether due to viral infections, obstetric complications or nutritional deficiencies, as exemplified by the catastrophe of the Dutch 1944 winter famine (Reference Susser and LinSusser & Lin, 1992; Reference Susser, Neugebauer and HoekSusser et al, 1996), summarised in an anthology edited by Susser et al (Reference Susser, Brown and Gorman1999). However, the initiative now rests largely with researchers in cellular anatomy and neurophysiology, investigating topics such as inhibited cell migration to the cortex, periventricular atrophy and inadequate functioning of the frontal lobes.
One further epidemiological finding, which provides tentative support for the brain-damage theory, is the significant decrease in the incidence of treated schizophrenia in the Western world, which has now been reported by more than 20 studies (Reference Munk-J⊘rgensenMunk-Jørgensen, 1995). There has been much speculation about this phenomenon. The most obvious explanation is the rapid run-down and closure of many psychiatric institutions. However, there is also a possibility that the post-war improvement in maternity welfare and obstetric care, one of the successful preventive developments in Western medicine, may have resulted in a reduction of foetal and perinatal brain damage, and that this could be a partial explanation of the apparent decrease in schizophrenia incidence observed decades later.
It took 10 years to reach the conclusion that influenza in one way or another causes minor damage to the immature brain, increasing the risk of schizophrenia in genetically vulnerable persons. Even today this connection is not firmly established, since some studies have been unable to replicate the association between maternal influenza and schizophrenia (Reference Erlenmeyer-Kimling, Folnegovic and Hrabak-ZerjavicErlenmeyer-Kimling et al, 1994; Reference Susser, Lin and BrownSusser et al, 1994; Reference Cannon, Cotter and CoffeyCannon et al, 1996; Reference Morgan, Castle and PageMorgan et al, 1997).
Perhaps research progress could be expedited by better coordinated use of the available scientific societies and organisations. There are now a number of international bodies, including the epidemiological section of the European Psychiatric Association and the World Psychiatric Association, the Nordic Association for Psychiatric Epidemiology and the International Federation for Psychiatric Epidemiology, each of which is doing valuable work in organising conferences, symposia and workshops for exchanging and spreading knowledge. Such organisations might be useful also in creating knowledge, by actively promoting international collaboration in research: not just descriptive studies as in the past, but studies specifically designed to test causal hypotheses. The influenza—schizophrenia hypothesis can serve as an example of what is needed: multi-centre studies of case records would have given the findings of Mednick, Huttunen and other workers in this field greater statistical power and enabled them to reach more definitive conclusions.






eLetters
No eLetters have been published for this article.