Several recent studies have claimed that being born or brought up in cities is associated with an increased risk of schizophrenia (Reference Lewis, David and AndreassonLewis et al, 1992; Marcelis et al, Reference Marcelis, Navarro-Mateu and Murray1998, Reference Marcelis, Takei and van Os1999; Reference Mortensen, Carsten and WestergaardMortensen et al, 1999). A genuine association between the incidence of schizophrenia and urban dwelling would be profoundly important for the understanding of the aetiology of this disorder. Unfortunately, it is difficult to establish whether or not incidence really does vary, because it is hard to ensure that the conditions and methods of measurement that have been used in different studies are the same for all areas being compared (Reference FreemanFreeman, 1994). We therefore report an urban/rural comparison of first contact rates for schizophrenia using consistently generated diagnoses in two well-defined catchment areas, namely rural Dumfries and Galloway in south-west Scotland and inner-city Camberwell in south-east London. We also assess the impact on this comparison of the significant numbers of non-White individuals living in Camberwell, who when resident in the UK are reported to be at a higher risk of schizophrenia than the White population (Reference Harrison, Owens and HoltenHarrison et al, 1988; Wessely et al, 1991; Reference King, Coker and LeavyKing et al, 1994; Reference van Os, Castle and Takeivan Os et al, 1996).
METHOD
Study areas
Dumfries and Galloway is a rural area in south-west Scotland with a population of around 147 000, 99.6% of whom were classified as White in the 1991 census. It is 2460 square miles in area and has a population density of 60 people per square mile. The local economy is based primarily on agriculture and farming, although there is some tourism and a little light industry. A comprehensive community-based psychiatric service is provided via out-patient clinics throughout the region. These clinics and their associated community psychiatric teams provide a service integrated with primary care and social services. One inpatient facility, situated at the Crichton Royal Hospital in the market town of Dumfries (population of approximately 30 000), serves the area.
Camberwell is an inner-city area in south-east London congruent with the southern portion of the Borough of Southwark. The 1991 census showed it to have a population of approximately 120 000, of whom some 75% are White. It has a population density of some 19 000 persons per square mile, that is, 316 times that of Dumfries and Galloway. Its economy was based historically on manufacturing industries but now is mixed. It contains the wealthy area of Dulwich (approximately 30% of the Camberwell catchment area with 13% of the Camberwell population) but also a number of poor areas. Over the period of the study, its psychiatric service has been provided via the same services based around the Maudsley Hospital but, as in Dumfries and Galloway, the services have moved towards a sectorised integrated community service.
Identification of cases
In both areas, we identified all patients making their first contact with psychiatric services who received a clinical diagnosis of one of a broad range of psychotic disorders. During the study period two different versions of the International Classification of Diseases (ICD) were used for formal coding of the cases: ICD-9 (Reference Wessely, Castle and DerWorld Health Organization, 1978) between 1979 and March 1996; and ICD-10 (Reference Wessely, Castle and DerWorld Health Organization, 1992) thereafter. We reviewed all cases with a clinical diagnosis of schizophrenia (295; F20), schizoaffective disorder (295.6; F25), delusional disorder (297; F22), mania (296.0, 296.2, 296.4; F30, F31.1, F31.2, F31.6), acute, transient or unspecified psychotic disorders (298; F28, F29) or drug induced disorders (292.1; F12.5, F16.6, F19.5, F12.75, F16.75, F19.75) for the years 1979-1984 and 1992-1997. The second period allowed us to carry out a White-only comparison using information specifically about ethnicity that had not been collected before the 1991 census. In Dumfries and Galloway, all patients in contact with the psychiatric services during the study years who were given any of the above clinical diagnoses were identified from two sources: data for all in-patient admissions held centrally by the Information and Statistical Division Scotland (ISD); and data from locally held registers of outpatient contacts, domiciliary visits and emergency referrals.
In Camberwell, the data collection was carried out in two parts. For the years 1979-1984, a list was generated from the Camberwell Cumulative Register for all patients who, within a year of presentation, were given one of the inclusion diagnoses (details given in Reference Castle, Wessely and DerCastle et al, 1991). Cases were identified for the period 1992-1997 by hand-searching the case notes of all patients contacting the community facilities during these years and also via computerised information systems for all admissions to in-patient wards. Patients were divided into White and non-White groups based on information in their case records.
In both areas, cases were excluded if they were not resident in the catchment area, had presented previously with a psychotic episode outwith the study period or had a clear organic cause for their symptoms. For the remaining patients their case records, including medical, nursing, social work and occupational therapy notes together with all correspondence, were examined and the Operational Checklist for Psychotic Disorders (OPCRIT; Reference McGuffin, Farmer and HarveyMcGuffin et al, 1991) was completed for the year following presentation. The OPCRIT is a symptom checklist containing 90 items that explores aspects of the mental state examination and psychiatric history. It has a glossary of clear and explicit descriptions for each constituent item of psychopathology and instructions for coding them. It was designed with case-note review in mind.
Two psychiatrists (J. A. and G. M.) working independently rated the case notes in Dumfries and Galloway. Two psychiatrists rated the Camberwell case notes for the 1979-1984 cases in Camberwell (Reference Castle, Wessely and DerCastle et al, 1991); interrater reliability was shown previously to be high (κ=0.82 for a Research Diagnostic Criteria (RDC) diagnosis of schizophrenia). One psychiatrist (J. K.) worked independently in Camberwell to complete the OPCRIT for the years 1992-1997. Interrater reliability was good for all three raters (J. A., G. M. and J. K.): κ=0.79 for an RDC diagnosis of schizophrenia. The OPCRIT checklists then were used to generate RDC diagnoses (Reference Spitzer, Endicott and RobinsSpitzer et al, 1978) via the associated computer algorithm.
General population data
Data for the general populations stratified by age and gender were obtained in Dumfries and Galloway via the General Register Office Scotland and in Camberwell via the Office of Population Censuses and Surveys (OPCS, 1991) and the London Research Centre (1997). Census data for 1971, 1981 and 1991 were provided as well as population projections for 1997; estimations of the population for the intermediate years were interpolated. The 1991 census recorded information about self-reported ethnicity.
Statistical analysis
We compared first contact rates (service-based incidence rates) for OPCRIT-derived RDC schizophrenia in the two areas for the 12 years 1979-1984 and 1992-1997. First contact rates have been reported previously using different diagnostic criteria in Dumfries and Galloway for the periods 1979-1998 (Reference Allardyce, Morrison and McCreadieAllardyce et al, 2000) and 1979-1984 in Camberwell (Reference Castle, Wessely and DerCastle et al, 1991). To compare the incidence in the two areas we firstly calculated incidence rates stratified by age and gender for Dumfries and Galloway. These rates then were used as our reference or standard population rates. Using the indirect standardisation method, in the STATA statistical program (Stata Corporation, 1999) we applied these rates to the population structure of Camberwell. This allowed us to determine the number of expected cases if the rates were the same in both areas. By dividing the actual observed cases by the expected cases, we calculated the standardised incidence ratio (SIR).
To complement this SIR analysis, we constructed Poisson regression models using the STATA statistical program. In the Poisson regression model, the log of the incidence of schizophrenia is the response (dependent) variable. We examined the effect of the explanatory (independent) variable — urban exposure (residence in Camberwell) — on the incidence of schizophrenia while adjusting for gender, age and time period in the model. The exponentiated regression coefficient is the incidence rate ratio (IRR) (i.e. the incidence rate in Camberwell divided by the rate for Dumfries and Galloway). Previously published work demonstrated a higher incidence of schizophrenia in urban areas, more marked in men than women and higher in the younger age groups (Reference Marcelis, Navarro-Mateu and MurrayMarcelis et al, 1998; Reference Takei, Sham and GloverTakei et al, 1995). We have examined, therefore, the interaction of urban exposure with age and gender and the interaction of age with gender.
RESULTS
Comparison of incidence
In Dumfries and Galloway over the 12 years, 177 cases were identified who fulfilled the OPCRIT-generated RDC criteria for schizophrenia (narrow and broad); all were White. In Camberwell, 265 cases were identified who met the RDC criteria, of whom 128 (50%) were White. When we compared the two areas using indirect standardisation, the SIR was 1.61 (95% CI 1.42-1.81), that is, the risk of schizophrenia was estimated to be 61% higher in Camberwell (Table 1). Stratified analyses showed the SIR varying across different levels of gender, age and time period, suggesting that these factors modify the effect of urban Camberwell residence (Table 2).
Table 1 Standardised incidence ratio (SIR) by comparing Dumfries and Galloway (D+G) with the total population of Camberwell
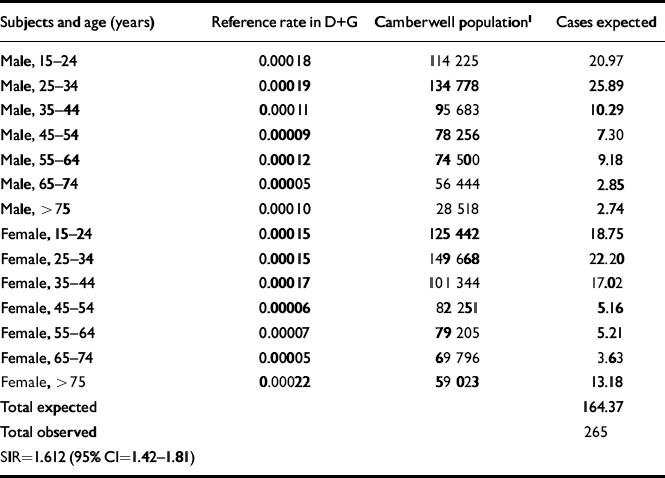
| Subjects and age (years) | Reference rate in D+G | Camberwell population1 | Cases expected |
|---|---|---|---|
| Male, 15-24 | 0.00018 | 114 225 | 20.97 |
| Male, 25-34 | 0.00019 | 134 778 | 25.89 |
| Male, 35-44 | 0.00011 | 95 683 | 10.29 |
| Male, 45-54 | 0.00009 | 78 256 | 7.30 |
| Male, 55-64 | 0.00012 | 74 500 | 9.18 |
| Male, 65-74 | 0.00005 | 56 444 | 2.85 |
| Male, >75 | 0.00010 | 28 518 | 2.74 |
| Female, 15-24 | 0.00015 | 125 442 | 18.75 |
| Female, 25-34 | 0.00015 | 149 668 | 22.20 |
| Female, 35-44 | 0.00017 | 101 344 | 17.02 |
| Female, 45-54 | 0.00006 | 82 251 | 5.16 |
| Female, 55-64 | 0.00007 | 79 205 | 5.21 |
| Female, 65-74 | 0.00005 | 69 796 | 3.63 |
| Female, >75 | 0.00022 | 59 023 | 13.18 |
| Total expected | 164.37 | ||
| Total observed | 265 | ||
| SIR=1.612 (95% Cl=1.42-1.81) |
Table 2 Standardised incidence ratio (SIR) stratified by time period, gender and age (reference rates from Dumfries and Galloway)
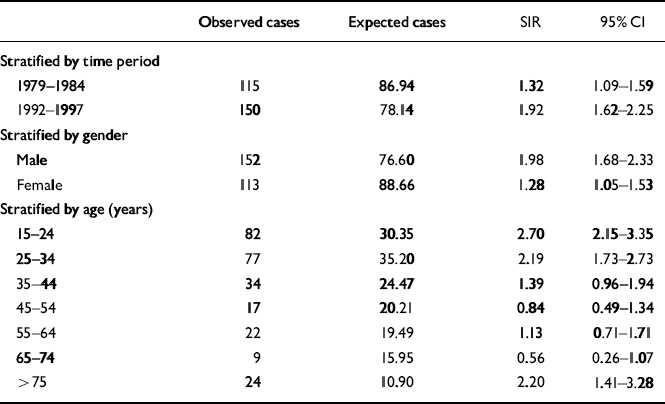
| Observed cases | Expected cases | SIR | 95% Cl | |
|---|---|---|---|---|
| Stratified by time period | ||||
| 1979-1984 | 115 | 86.94 | 1.32 | 1.09-1.59 |
| 1992-1997 | 150 | 78.14 | 1.92 | 1.62-2.25 |
| Stratified by gender | ||||
| Male | 152 | 76.60 | 1.98 | 1.68-2.33 |
| Female | 113 | 88.66 | 1.28 | 1.05-1.53 |
| Stratified by age (years) | ||||
| 15-24 | 82 | 30.35 | 2.70 | 2.15-3.35 |
| 25-34 | 77 | 35.20 | 2.19 | 1.73-2.73 |
| 35-44 | 34 | 24.47 | 1.39 | 0.96-1.94 |
| 45-54 | 17 | 20.21 | 0.84 | 0.49-1.34 |
| 55-64 | 22 | 19.49 | 1.13 | 0.71-1.71 |
| 65-74 | 9 | 15.95 | 0.56 | 0.26-1.07 |
| > 75 | 24 | 10.90 | 2.20 | 1.41-3.28 |
Poisson regression modelling reflected the findings of the SIR analyses. The IRR for ‘Camberwell urban exposure’ was 1.63 (95% CI 1.35-1.98), adjusted for age, year and gender. There was a statistically significant interaction between urban exposure and gender (IRR=0.67; 95% CI 0.46-0.99), that is, the risk of urban residence was greater for males. The statistically significant interaction between gender and age (IRR=1.29; 95% CI 1.16-1.46) shows that the risk of schizophrenia in females in both areas increases with age.
White-only comparison
We then compared the Dumfries and Galloway population with the White population in Camberwell using indirect standardisation for the period 1992-1997; we found no statistically significant difference in the rates (Table 3). The Poisson regression model again was unable to demonstrate any conclusive difference in risk; the IRR was 1.14 (95% CI 0.82-1.58). There were no statistically significant interactions in this model.
Table 3 Standardised incidence ratio (SIR) for the time period 1992-1997 (reference rate from Dumfries and Galloway)

| Observed cases | Expected cases | SIR | 95% Cl | |
|---|---|---|---|---|
| All cases in Camberwell | 150 | 78.14 | 1.92 | 1.62-2.25 |
| White cases only in Camberwell | 62 | 55.58 | 1.12 | 0.86-1.43 |
DISCUSSION
Methodological considerations
Potential sources of bias and confounding
Before interpreting our findings, we must first consider potential sources of bias. We have compared service-based rates but not community rates. This potentially could confound our results if there was any regional difference in help-seeking behaviour. In Ireland a higher threshold for seeking medical advice was shown for neurotic disorders in rural than urban areas, but this was not the case for psychotic disorders (Reference KeatingeKeatinge, 1987). The distance to the psychiatric hospital also has been reported to be related inversely to the admission rates (Reference JarvisJarvis, 1851). The effect is small, however, for severe psychiatric disorders (Reference Davey and GilesDavey & Giles, 1979). The influence of distance on service contact for psychosis is not clear but may be a factor in the level of service utilisation in the relatively distributed population of Dumfries and Galloway, and could be a potential source of bias. We think that this is unlikely because out-patient clinics and community teams are distributed throughout this rural area.
A variation in referral patterns of general practitioners to the different services also could confound our results. However, both areas are within the UK where, if it is suspected that a patient has a psychotic illness, general practitioners will almost invariably arrange a psychiatric referral (Reference Kendell, Malcolm and AdamsKendell et al, 1993; Reference Cooper, Goodhead and CraigCooper et al, 1987). It is conceivable that an occasional patient may be referred to a private practitioner; however, even if this did happen initially, it is very unlikely that someone with a psychotic disorder residing in either of the two areas would have no contact with the National Health Service over the study period. Potential bias due to variations in admission policies between the two centres was avoided by identifying all patients with a first-episode psychosis contacting the respective service, that is, not only those admitted to in-patient facilities but also out-patients, domiciliary visits and emergency contacts.
Case note review may not be an ideal way to make a diagnosis and we cannot exclude the possibility that case notes in the two centres contain different information, perhaps reflecting different clinical traditions. However, the phenomenological tradition in both centres stems from Mayer-Gross, who successively worked at the Maudsley Hospital in Camberwell and The Crichton Royal Hospital in Dumfries (Reference Mayer-Gross, Slater and RothMayer-Grosset al, 1969). The case notes in both areas follow a semi-structured form and it is our experience that in both areas the note-keeping is of a high standard. The OPCRIT-generated RDC diagnosis for schizophrenia demonstrated good interrater reliability, thus ensuring that cases in both areas were diagnosed consistently using a well-established research classification system.
Finally, there was no significant under-enumeration for Dumfries and Galloway in the 1991 census (estimated at around 1%), although under-enumeration may have occurred in Camberwell. It is impossible to know the full extent of this under-enumeration and it is possible that there is some under-counting of the general population, particularly for the non-White groups. We have, however, employed population estimates that now have been corrected for this (London Research Centre, 1997).
Case ascertainment
For the period 1979-1984 there were minor differences in the case ascertainment in the two centres. Cases in Camberwell were identified by their diagnosis in the first year of presentation to psychiatric services, whereas in Dumfries and Galloway it was by first-event psychotic diagnosis. This may have relatively underestimated cases in Camberwell for this period. In the years 1992-1997 the case identification was the same in both centres. Therefore, different methods could not account for the findings in our comparison of White subjects. Owing to the small numbers in the White-only comparison, we were unable to examine interactions with age and gender, which may be masked by the summary measures in this comparison.
Comparison of incidence
We have shown a higher incidence of schizophrenia in urban Camberwell compared with rural Dumfries and Galloway. The risk for urban residence was greatest for males. This is consistent both with recently published work comparing urban/rural variations in (first) admission rates for schizophrenia (Reference SystemaSystema, 1991; Reference Peen and DekkerPeen & Dekker, 1997) and with cohort studies, suggesting that being born or brought up in an urban environment is associated with an increased risk of schizophrenia (Reference Lewis, David and AndreassonLewis et al, 1992; Marcelis et al, Reference Marcelis, Navarro-Mateu and Murray1998, Reference Marcelis, Takei and van Os1999; Reference Mortensen, Carsten and WestergaardMortensen et al, 1999).
White-only comparison
We found no statistically significant difference in the incidence of schizophrenia when the White population in Camberwell was compared with those in Dumfries and Galloway.
This suggests that non-White individuals living in Camberwell account for a large proportion of the increased urban incidence that we have found. The ethnic minority population in Camberwell is a mixed one but the largest group — approximately 11% of the total population — comprise individuals who migrated from the Caribbean together with their children. There is considerable evidence from Camberwell and elsewhere that this population has an incidence of schizophrenia that is four— to sixfold higher than the rest of the British population. This appears to be more prominent in the children of people who have migrated (Reference Harrison, Owens and HoltenHarrison et al, 1988; Wessely et al, 1991; Reference van Os, Castle and Takeivan Os et al, 1996).
Is it possible that recent studies suggesting an increased incidence of schizophrenia in urban areas reflect the different population compositions in urban and rural areas, with migrants and their offspring primarily living in inner-city areas (Reference Herbert and JohnstonHerbert & Johnston, 1976). This seems unlikely because the authors of the various cohort studies assert that their studies, in which an urban place of birth was associated with an increased risk of schizophrenia, were carried out in areas with relatively little external (i.e. from another country) migration.
Why, then, do our results in the White population differ from these cohort studies? First, there may be something atypical about Camberwell, because it contains a relatively rich and predominantly White area (Dulwich), with the non-White people tending to live in the poorer areas; thus, social class and wealth may confound the ethnic division. Second, perhaps it is those individuals in the inner-city who are most disadvantaged and alienated from mainstream society who have an increased incidence of schizophrenia. In south London, African-Caribbeans have taken over this role but it could be that in cities without Black immigrants the low social class Whites occupy this position. Finally, it may be that the cohort studies identified those with only relatively early-onset schizophrenia and missed the later-onset cases, whereas our study identified all first-episode cases of schizophrenia in all age groups in both areas. The onset of schizophrenia may be later in rural areas (Reference EatonEaton, 1974). A longer follow-up period in the cohort studies might, therefore, have identified more rural cases and thus reduced the apparent urban/rural difference. Unfortunately we did not have the power to detect any age and gender interactions in our White population; larger studies should explore these possible interactions.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
• Standardised incidence rates for schizophrenia are higher in urban Camberwell than in rural Dumfries and Galloway.
-
• The increased risk in urban Camberwell is greater in males than females.
-
• Non-White individuals living in Camberwell account for a large proportion of this demonstrated increased incidence.
LIMITATIONS
-
• This is a service-based study.
-
• We have compared only two discrete geographical areas.
-
• Relatively small numbers in the comparison of the White-only population of Camberwell with Dumfries and Galloway hinder the exploration of age and gender interactions in the model.
Acknowledgements
This study was supported by grants from The Stanley Foundation and The Gordon Small Trust. We are grateful to Jennifer Bishop at ISD, the General Register Office (Edinburgh) and the London Research Centre for their help.








eLetters
No eLetters have been published for this article.