Road traffic accidents cause physical injury, can be a frightening threat to life, have major financial consequences and can result in prosecution or prolonged compensation proceedings. Research has focused on physical issues relating to major injury and on whiplash neck injury (Reference Holbrook, Anderson and SieberHolbrook et al, 1999), but there is recent evidence that post-traumatic stress disorder (PTSD) is frequent, disabling and persistent (Reference Hickling and BlanchardHickling & Blanchard, 1999). However, reliance on small selected samples and a narrow view of outcome means that we know little about the consequences for the whole range of those who consult doctors, most of whom suffer no more than minor physical injury. Such knowledge would enable simple procedures to be set up for early recognition of complications and of those at high risk of poor outcome and for the development and evaluation of treatments. This paper reports a prospective study of consecutive attenders aged 17-69 years at a general hospital accident and emergency (A&E) department following road traffic accidents over a 1-year period.
METHOD
Consecutive patients aged 17-69 years who attended the A&E Department of the John Radcliffe Hospital, Oxford, after a road traffic accident and who had not suffered unconsciousness of more than 15 min were asked to complete an initial questionnaire while at the hospital or sent a questionnaire by post. Patients received further questionnaires both 3 months and 1 year after the accident.
The initial questionnaire covered demographic items, memories of the accident, previous travel, previous emotional problems, current feelings and attitudes; it was based on our previous research (Reference Mayou, Bryant and DuthieMayou et al, 1993) and a six-item version of the SF36 scale (Reference Ware, Nelson, Sherbourne, Steward and WareWare et al, 1992). The 3-month and 1-year questionnaires covered present health, consultation and treatment, effects of the accident on finances, work, travel and travel avoidance and also intentions to seek compensation. All subjects were asked to complete the Hospital Anxiety and Depression (HAD) scale (Reference Zigmond and SnaithZigmond & Snaith, 1983) and a self-report of PTSD symptoms (Reference Foa, Riggs and DancuFoaet al, 1993) that provides both a severity score and a DSM-IV (American Psychiatric Association, 1994) diagnosis. We used the standard cut-off on the HAD scale and replies to self-report questions to define categories of anxiety and depression and specific phobia about travel that were similar to standard psychiatric criteria. Information was abstracted from the medical notes, and the Injury Severity Score (ISS) of the Abbreviated Injury Scale (American Association for Automotive Medicine, 1990) was calculated. This standard measure of injury severity, used in trauma research, is based on the summed squares of the three highest scoring injuries across five body regions. A score of 1-3 indicates minor injury, usually soft-tissue injury such as bruises and lacerations but also minor fracture such as a broken finger or nose.
Analysis used χ2 together with logistic regression to identify the predictors of 1-year outcome. The choice of predictors was influenced by theoretical considerations and our previous findings (Reference Ehlers, Mayou and BryantEhlers et al, 1998), but the main concern was to consider variables that might be observed or assessed easily by those providing immediate treatment for accident victims.
RESULTS
There were 1534 attenders aged 17-69 years during the year, of whom seven died in the A&E Department. Of the survivors, 23 were ineligible for the study because they were unconscious for more than 15 min. We further excluded 32 foreign visitors, 8 people unable to complete a questionnaire for language or psychiatric reasons, 11 who were too ill for assessment and 12 who refused to take part. A total of 1441 patients were eligible for the study: 1148 (80%) completed the baseline questionnaire, of whom 865 (75%) completed questionnaires at 3 months and 774 (67%) at 1 year.
Characteristics of the sample
Table 1 shows some of the characteristics of the participants. Just over half were men and half were younger than 30 years old. The great majority of injuries (61%) were minor (ISS score of 1-3, indicating abrasions or lacerations) and 20% were uninjured. Twenty-two per cent (n=278) were admitted, of whom half spent only one night in hospital.
Table 1 Characteristics of participants (n=1148)

| n | % | ||
|---|---|---|---|
| Demographic | |||
| Gender | Male | 631 | 55 |
| Female | 517 | 45 | |
| Age group (years) | Under 30 | 596 | 52 |
| 30+ | 552 | 48 | |
| Living group | Spouse/partner | 565 | 49 |
| Parent | 278 | 24 | |
| Other | 171 | 15 | |
| Alone | 129 | 11 | |
| Not known | 5 | ||
| Employment status | Working | 784 | 68 |
| Off sick | 15 | 1 | |
| Student/trainee | 162 | 14 | |
| Out of work | 84 | 7 | |
| Housekeeper | 71 | 6 | |
| Retired | 32 | 3 | |
| Medical | |||
| ISS (range 0-19) | 0 | 196 | 17 |
| 1 | 540 | 47 | |
| 2 | 158 | 14 | |
| 3 | 37 | 3 | |
| 4+ | 216 | 19 | |
| Admission | Not admitted or no injury | 905 | 79 |
| Admitted 1-2 nights, injury | 137 | 12 | |
| Admitted 3+ nights, injury | 106 | 9 | |
| Accident | |||
| Road user group | Vehicle driver | 600 | 52 |
| Vehicle passenger | 240 | 21 | |
| Motorcyclist | 135 | 12 | |
| Cyclist | 123 | 11 | |
| Pedestrian | 50 | 4 | |
| Memory of accident | Clear | 798 | 70 |
| Patchy | 286 | 25 | |
| None | 56 | 5 | |
| Not known | 6 | ||
| Blames self for accident | No | 808 | 71 |
| Partly | 183 | 16 | |
| Yes | 147 | 13 | |
| Not known | 10 | ||
| Perceived threat of accident | Not frightening | 176 | 15 |
| Mildly frightening | 219 | 19 | |
| Quite frightening | 340 | 30 | |
| Very frightening | 407 | 36 | |
| Not known | 6 |
Non-respondents and drop-outs
To examine for selection bias, the 293 eligible people who did not take part in the study were compared with the 1148 participants. Men were significantly less likely to take part initially (78% v. 82% of women; χ2=4.85, 1 d.f., P<0.05), as were younger people (76% of those aged ≤ 30 years v. 84% of those aged 30+ years; χ2=11.13, 1 d.f., P<0.01) and people who were not admitted to hospital (77% v. 89% of those admitted; χ 2=19.49, 1 d.f., P<0.001). The 375 participants who dropped out of the study during the follow-up year also were compared with the 773 who remained in the study, and again fewer men, younger people and those not admitted completed the 1-year follow-up. Those out of work or off sick at the first assessment also were less likely to stay in the study. However, none of the other variables measured at first assessment or at 3 months were related to subsequent participation.
What are the consequences during the year after the accident?
There was a wide range in immediate reactions. One-third rated the accident as not, or only mildly, frightening and one-fifth did not feel at all distressed. At the other extreme, 36% found the accident very frightening and 27% were highly distressed. Distress was strongly associated with perceived threat but not with injury severity. One-third (35%) felt moderately to extremely angry.
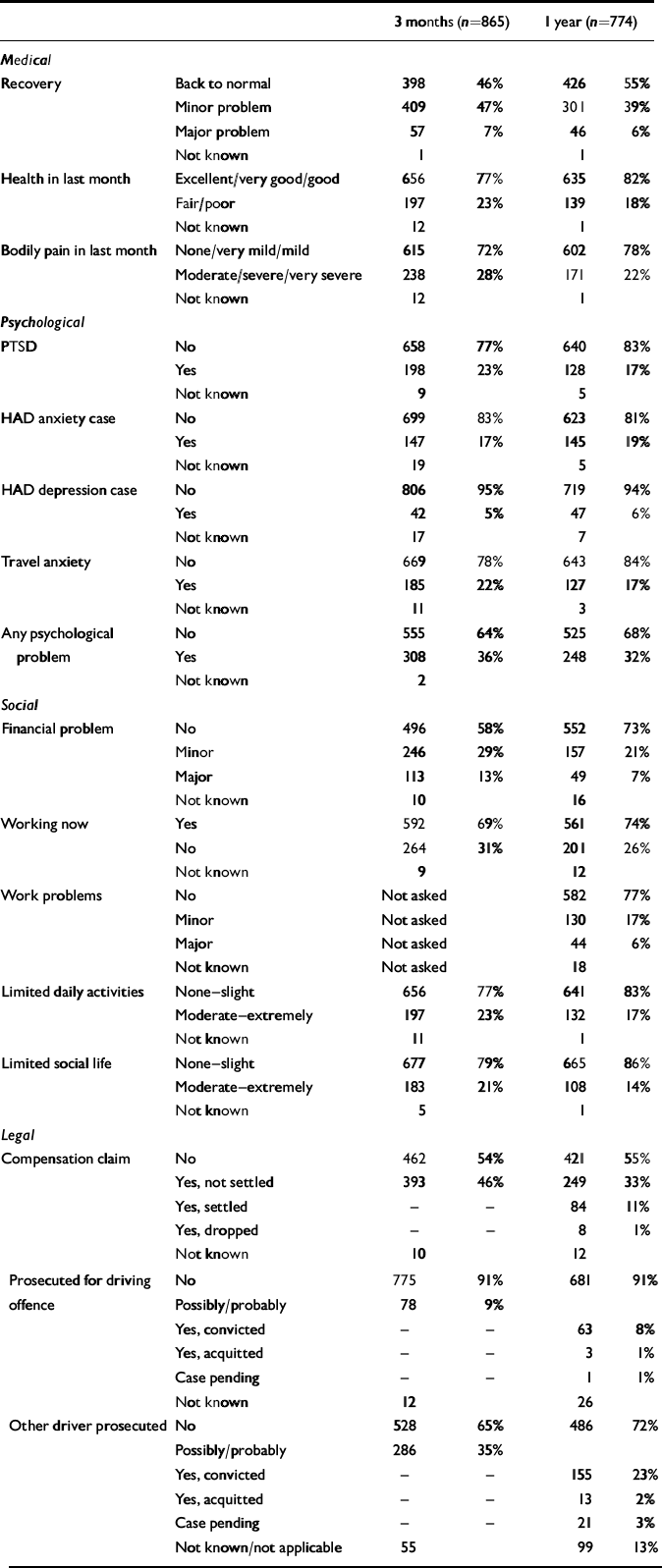
Almost half of the subjects (46%) said that they were physically recovered at 3 months and 55% at 1 year. There was a correlation of 0.355 (n=787; P<0.01) between physical recovery and psychological consequences at 1 year (Table 2).
Table 2 Outcomes for participants at 3 months and 1 year
| 3 months | (n=865) | 1 year | (n=774) | ||
|---|---|---|---|---|---|
| Medical | |||||
| Recovery | Back to normal | 398 | 46% | 426 | 55% |
| Minor problem | 409 | 47% | 301 | 39% | |
| Major problem | 57 | 7% | 46 | 6% | |
| Not known | 1 | 1 | |||
| Health in last month | Excellent/very good/good | 656 | 77% | 635 | 82% |
| Fair/poor | 197 | 23% | 139 | 18% | |
| Not known | 12 | 1 | |||
| Bodily pain in last month | None/very mild/mild | 615 | 72% | 602 | 78% |
| Moderate/severe/very severe | 238 | 28% | 171 | 22% | |
| Not known | 12 | 1 | |||
| Psychological | |||||
| PTSD | No | 658 | 77% | 640 | 83% |
| Yes | 198 | 23% | 128 | 17% | |
| Not known | 9 | 5 | |||
| HAD anxiety case | No | 699 | 83% | 623 | 81% |
| Yes | 147 | 17% | 145 | 19% | |
| Not known | 19 | 5 | |||
| HAD depression case | No | 806 | 95% | 719 | 94% |
| Yes | 42 | 5% | 47 | 6% | |
| Not known | 17 | 7 | |||
| Travel anxiety | No | 669 | 78% | 643 | 84% |
| Yes | 185 | 22% | 127 | 17% | |
| Not known | 11 | 3 | |||
| Any psychological | No | 555 | 64% | 525 | 68% |
| problem | Yes | 308 | 36% | 248 | 32% |
| Not known | 2 | ||||
| Social | |||||
| Financial problem | No | 496 | 58% | 552 | 73% |
| Minor | 246 | 29% | 157 | 21% | |
| Major | 113 | 13% | 49 | 7% | |
| Not known | 10 | 16 | |||
| Working now | Yes | 592 | 69% | 561 | 74% |
| No | 264 | 31% | 201 | 26% | |
| Not known | 9 | 12 | |||
| Work problems | No | Not asked | 582 | 77% | |
| Minor | Not asked | 130 | 17% | ||
| Major | Not asked | 44 | 6% | ||
| Not known | Not asked | 18 | |||
| Limited daily activities | None—slight | 656 | 77% | 641 | 83% |
| Moderate—extremely | 197 | 23% | 132 | 17% | |
| Not known | 11 | 1 | |||
| Limited social life | None—slight | 677 | 79% | 665 | 86% |
| Moderate—extremely | 183 | 21% | 108 | 14% | |
| Not known | 5 | 1 | |||
| Legal | |||||
| Compensation claim | No | 462 | 54% | 421 | 55% |
| Yes, not settled | 393 | 46% | 249 | 33% | |
| Yes, settled | — | — | 84 | 11% | |
| Yes, dropped | — | — | 8 | 1% | |
| Not known | 10 | 12 | |||
| Prosecuted for driving | No | 775 | 91% | 681 | 91% |
| offence | Possibly/probably | 78 | 9% | ||
| Yes, convicted | — | — | 63 | 8% | |
| Yes, acquitted | — | — | 3 | 1% | |
| Case pending | — | — | 1 | 1% | |
| Not known | 12 | 26 | |||
| Other driver prosecuted | No | 528 | 65% | 486 | 72% |
| Possibly/probably | 286 | 35% | |||
| Yes, convicted | — | — | 155 | 23% | |
| Yes, acquitted | — | — | 13 | 2% | |
| Case pending | — | — | 21 | 3% | |
| Not known/not applicable | 55 | 99 | 13% |
Physical
At 3 months, 7% reported ‘major problems’ in physical recovery and there was little improvement at 1 year. Most problems related to serious disabling injuries or to musculo-skeletal complaints that had limited physically demanding work or leisure. At least six patients described severe chronic pain syndromes that appeared out of proportion to the physical impairment. Minor problems (39% at 1 year) were mainly musculo-skeletal complaints.
Psychological
One-third of the responders had at least one of the four psychological conditions (PTSD, phobic travel anxiety, general anxiety, depression) at 3 months (36%) and 1 year (32%). More women than men had at least one of these disorders (3 months: 45% of women v. 28% of men; χ 2=26.90, 1 d.f., n=864; 1 year: 41% of womenv. 24% of men; χ2=23.30, 1 d.f., n=773). There was considerable overlap between these disorders but also a sizeable number of people who had only one or two types of psychological complication. Although there was some improvement during follow-up, with 82 people (12%) getting better between 3 months and 1 year, 66 subjects (9%) suffered late-onset psychological complications.
Social and financial
Most respondents (69%) were working at 3 months, of whom half had been off work for less than a week and four-fifths were back at work within 4 weeks of the accident. Although the proportion in work at 1 year (74%) was similar to before the accident, 23% said that they still suffered work difficulties and four-fifths said that they had financial difficulties as a result. Limitations of travel, both as drivers and as passengers, were conspicuous.
Legal
The 9% of subjects who were prosecuted for driving offences had similar outcomes to the remainder, except that they were significantly less likely to report travel anxiety. Seeking compensation was associated significantly with worse physical, psychological and social outcomes, but claimants also had suffered more severe injury and loss.
Resource use
Although most subjects were discharged from the A&E Department without a follow-up appointment, there was substantial continuing use of health care resources throughout the follow-up year.
Are there differences in outcome according to the severity or type of injuries?
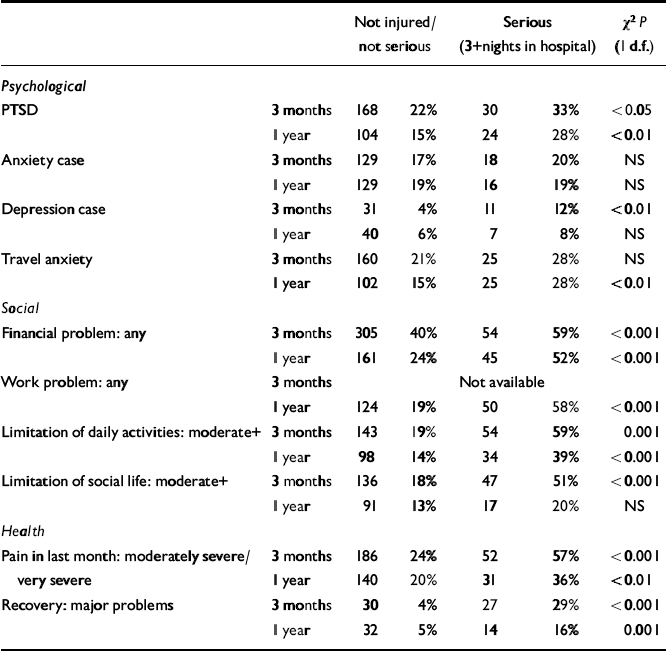
The one-tenth of subjects who suffered medically serious injury (defined in terms of injury resulting in admission for at least 3 nights) had poorer outcomes on almost all measures (physical, psychological and social) at both 3 months and 1 year (Table 3). However, there was little association between clinical classification of severity (no injury, soft tissue or bony), which was highly correlated with ISS score (Spearman's correlation coefficient ρ=0.834, P<0.01) and outcomes. Physical recovery was poorest for those with fractures but there were no differences for psychiatric consequences or for most social outcomes at 3 months or 1 year.
Table 3 Outcomes at 3 months and 1 year by serious injury1
| Not injured/not serious | Serious (3+nights in hospital) | χ 2P (1 d.f.) | ||||
|---|---|---|---|---|---|---|
| Psychological | ||||||
| PTSD | 3 months | 168 | 22% | 30 | 33% | <0.05 |
| 1 year | 104 | 15% | 24 | 28% | <0.01 | |
| Anxiety case | 3 months | 129 | 17% | 18 | 20% | NS |
| 1 year | 129 | 19% | 16 | 19% | NS | |
| Depression case | 3 months | 31 | 4% | 11 | 12% | <0.01 |
| 1 year | 40 | 6% | 7 | 8% | NS | |
| Travel anxiety | 3 months | 160 | 21% | 25 | 28% | NS |
| 1 year | 102 | 15% | 25 | 28% | <0.01 | |
| Social | ||||||
| Financial problem: any | 3 months | 305 | 40% | 54 | 59% | <0.001 |
| 1 year | 161 | 24% | 45 | 52% | <0.001 | |
| Work problem: any | 3 months | Not available | ||||
| 1 year | 124 | 19% | 50 | 58% | <0.001 | |
| Limitation of daily activities: moderate+ | 3 months | 143 | 19% | 54 | 59% | 0.001 |
| 1 year | 98 | 14% | 34 | 39% | <0.001 | |
| Limitation of social life: moderate+ | 3 months | 136 | 18% | 47 | 51% | <0.001 |
| 1 year | 91 | 13% | 17 | 20% | NS | |
| Health | ||||||
| Pain in last month: moderately severe/ | 3 months | 186 | 24% | 52 | 57% | <0.001 |
| very severe | 1 year | 140 | 20% | 31 | 36% | <0.01 |
| Recovery: major problems | 3 months | 30 | 4% | 27 | 29% | <0.001 |
| 1 year | 32 | 5% | 14 | 16% | 0.001 | |
There were few associations between specific type of injury (of which whiplash neck injury was the most frequent) and any aspect of outcome at either 3 months or 1 year. Patients with leg fractures reported more limitation in activities than other subjects at 3 months and 1 year; those with arm fractures were more limited than others at 3 months but not at 1 year.
Are there differences according to the type of accident?
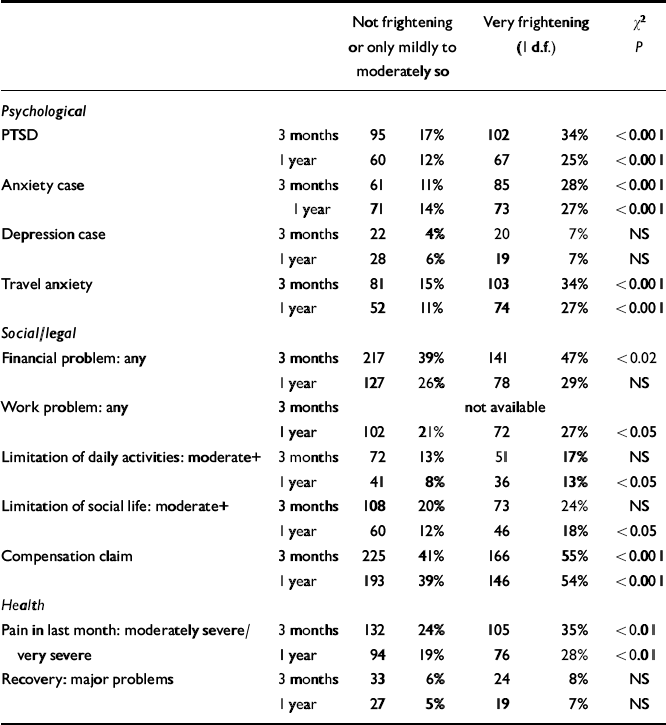
Those who reported immediately after the accident that they had been ‘very frightened’ had significantly worse outcomes at both 3 months and 1 year (Table 4).
Table 4 Outcomes at 3 months and 1 year by perceived threat of accident1
| Not frightening or only mildly to moderately so | Very frightening (1 d.f.) | χ 2 P | ||||
|---|---|---|---|---|---|---|
| Psychological | ||||||
| PTSD | 3 months | 95 | 17% | 102 | 34% | <0.001 |
| 1 year | 60 | 12% | 67 | 25% | <0.001 | |
| Anxiety case | 3 months | 61 | 11% | 85 | 28% | <0.001 |
| 1 year | 71 | 14% | 73 | 27% | <0.001 | |
| Depression case | 3 months | 22 | 4% | 20 | 7% | NS |
| 1 year | 28 | 6% | 19 | 7% | NS | |
| Travel anxiety | 3 months | 81 | 15% | 103 | 34% | <0.001 |
| 1 year | 52 | 11% | 74 | 27% | <0.001 | |
| Social/legal | ||||||
| Financial problem: any | 3 months | 217 | 39% | 141 | 47% | <0.02 |
| 1 year | 127 | 26% | 78 | 29% | NS | |
| Work problem: any | 3 months | not available | ||||
| 1 year | 102 | 21% | 72 | 27% | <0.05 | |
| Limitation of daily activities: moderate+ | 3 months | 72 | 13% | 51 | 17% | NS |
| 1 year | 41 | 8% | 36 | 13% | <0.05 | |
| Limitation of social life: moderate+ | 3 months | 108 | 20% | 73 | 24% | NS |
| 1 year | 60 | 12% | 46 | 18% | <0.05 | |
| Compensation claim | 3 months | 225 | 41% | 166 | 55% | <0.001 |
| 1 year | 193 | 39% | 146 | 54% | <0.001 | |
| Health | ||||||
| Pain in last month: moderately severe/ | 3 months | 132 | 24% | 105 | 35% | <0.01 |
| very severe | 1 year | 94 | 19% | 76 | 28% | <0.01 |
| Recovery: major problems | 3 months | 33 | 6% | 24 | 8% | NS |
| 1 year | 27 | 5% | 19 | 7% | NS | |
There were significant differences between the road user groups in medical outcome at 3 months, but patterns of psychological and social consequences were very similar. The main difference was in the occurrence of phobic travel anxiety. Passengers were more likely than other groups to report travel anxiety at 1 year (28% compared with 20% of motorcyclists, 17% of cyclists, 13% of pedestrians and 12% of drivers, χ2=22.95, 4 d.f.,P<0.01). It was mainly a problem for female passengers, with twice as many female passengers (34%) being classified as suffering from phobic travel anxiety at 1 year than female drivers (17%) and male passengers (16%). Only 7% of male drivers had phobic travel anxiety at 1 year.
Can we identify those who are at risk of chronic problems?
Self-report of physical recovery at 3 months was substantially predicted in a logistic regression by the severity of the accident injuries. However, by 1 year other factors also entered the prediction — psychological complications at 3 months, blame and involvement in compensation proceedings.
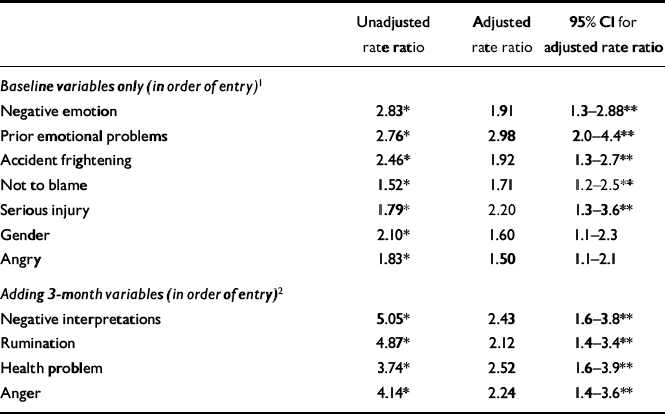
Logistic regression also was used to determine whether those at risk of chronic psychological problems at 1 year could be identified by clinical features that might be assessed easily in the A&E Department or at early follow-up review (Table 5). In the first stage, all the baseline variables included were significant predictors of 1-year outcome when entered on their own. After adjustment for the effects of the other variables and using a strict criterion of significance to take account of the number of variables (Bonferroni correction), negative emotion, prior emotional problems, perceived threat, feeling not to blame and severity of injury remained significant. The proportion of deviance explained was modest. In the second stage a number of 3-month variables, thought likely on theoretical grounds to be associated with later outcome, were added to see if this increased the accuracy of prediction. Continuing medical problems and three of the cognitive maintaining factors at 3 months were significant predictors of 1-year psychological outcome, accounting for an additional 12% of the deviance. In a final stage, ‘any psychological complications at 3 months’ was added to the model as a further predictor variable. This increased the deviance explained to 30% and the proportion of cases correctly classified to 81%.
Table 5 Predictors of psychological complications at 1 year
| Unadjusted rate ratio | Adjusted rate ratio | 95% CI for adjusted rate ratio | |
|---|---|---|---|
| Baseline variables only (in order of entry) 1 | |||
| Negative emotion | 2.83* | 1.91 | 1.3-2.88** |
| Prior emotional problems | 2.76* | 2.98 | 2.0-4.4** |
| Accident frightening | 2.46* | 1.92 | 1.3-2.7** |
| Not to blame | 1.52* | 1.71 | 1.2-2.5** |
| Serious injury | 1.79* | 2.20 | 1.3-3.6** |
| Gender | 2.10* | 1.60 | 1.1-2.3 |
| Angry | 1.83* | 1.50 | 1.1-2.1 |
| Adding 3-month variables (in order of entry) 2 | |||
| Negative interpretations | 5.05* | 2.43 | 1.6-3.8** |
| Rumination | 4.87* | 2.12 | 1.4-3.4** |
| Health problem | 3.74* | 2.52 | 1.6-3.9** |
| Anger | 4.14* | 2.24 | 1.4-3.6** |
DISCUSSION
Over half of the attenders (55%) reported clinically significant medical, psychiatric, social or legal consequences 1 year later. The very small proportion of those who were seriously injured were twice as likely to suffer PTSD, travel anxiety, financial and work problems at 1 year, but the important finding of this study is that many of those in the much larger majority with less serious or no injuries also suffer long-term consequences that are largely unrelated to the type of injury.
The study has the important advantages of being prospective, large size and a representative sample of all attenders following road accident injury, having a comprehensive view of outcome and using systematic emergency department medical data. Although there were high rates of response at each stage for the postal survey, there were some non-respondents. The gender differences (and the small over-representation of women among the participants) mean that overall frequencies of psychiatric disorders should be used with care. Findings also are limited by being based on self-report and by the lack of objective medical assessment at follow-up. However, the validity of our findings is supported by comparison with our previous research (Reference Mayou, Bryant and DuthieMayou et al, 1993) and with an interview subgroup within the present study, both of which had very high response rates throughout and were based on detailed interview. The findings are consistent with previous reports from several countries, both of disability associated with multiple and other very severe injuries (Reference Holbrook, Anderson and SieberHolbrook et al, 1999) and of the psychiatric complications (Reference Hickling and BlanchardHickling & Blanchard, 1999).
Physical and psychological outcomes
Reports of continuing physical problems at 1 year were considerably more common than would have been expected from the nature of the injuries recorded in the A&E Department notes. Written comments and the verbal reports of admitted patients who were interviewed suggest that most were musculo-skeletal complaints. They were often restricting and frustrating for people who had previously had physically demanding work or leisure interests. Psychiatric complications were frequent; there were serious effects on travel and other aspects of daily life. The association between physical and psychological variables suggests that psychiatric complications affect perception of pain and impairment and that interim physical problems may maintain post-traumatic symptoms.
Predicting outcome
The analysis of predictive factors reported here, taken with our report of an earlier cohort (Reference Mayou, Bryant and DuthieMayou et al, 1993) and comparison of detailed analyses of prediction of PTSD (Reference Mayou, Bryant and EhlersMayou et al, 2001) and other psychiatric outcomes (Reference Ehlers, Mayou and BryantEhlerset al, 1998), emphasises the importance of non-medical variables for all domains of outcome. We conclude that a poor outcome following a road traffic accident should be seen as resulting not only from the physical injury but from the psychiatric consequences of a life-threatening experience, financial losses and a system of compensation that perpetuates frustration while delaying resolution. Even though large health, social and legal resources are involved, many difficulties are unrecognised and untreated.
Clinical implications
Improving clinical care has to be considered in a context in which most patients are discharged after a single A&E department attendance, but many of those who see themselves as innocent victims of a very frightening form of trauma are angry about the suffering and the apparent lack of recognition from others. We need to consider the following.
(a) Routine immediate information and advice. Widely recorded and used ‘debriefing’ procedures are unhelpful and even harmful (Reference Mayou, Ehlers and HobbsMayou et al, 2000) but victims' comments suggest that greater efforts to provide information and simple practical help might be helpful.
(b) Early recognition of those needing continuing care. The study suggests predictive variables that could be assessed easily at first attendance or follow-up to identify those at high risk. It is probable that further research could develop a simple clinical instrument.
(c) Access to specialist treatments. Greater access to, and use of, proven psychiatric and psychological care (e.g. cognitive-behavioural treatments and antidepressant medication) are required.
Our account of the outcome for a representative sample of A&E department attenders shows that problems are greater, more varied and more persistent than has been recognised previously. This very large public health and economic problem requires legal and social (Reference Cassidy, Carroll and CoteCassidy et al, 2000) as well as medical answers.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
• Although most road traffic injuries are very minor, a substantial proportion of subjects report persistent adverse consequences at 3 months and 1 year.
• Outcomes at 1 year are predicted by baseline and 3-month psychosocial variables that could be assessed easily in routine clinical care.
• Treatment of associated psychological and social factors could be expected to have substantial benefit.
LIMITATIONS
• Assessment of outcome was by self-report only.
• Eighty per cent completed the baseline questionnaire and there were further non-responders at 3 months and 1 year.
• There was no physical assessment at follow-up.
Acknowledgements
We are grateful for help from: Gail Stockford, who was responsible for the recruitment of subjects and for the collection of initial and follow-up data; Christopher Bulstrode, for advice on design and classification of injury severity; Professor Anke Ehlers, who helped to design the psychological assessments; Ann Day, for data analysis; and the medical and nursing staff of the Accident and Emergency Department of the John Radcliffe Hospital, Oxford.










eLetters
No eLetters have been published for this article.