How can those survivors of traumatic events likely to develop post-traumatic stress disorder (PTSD) be most efficiently identified? Recently studies have investigated the performance of 4-, 6— and 12-item screening instruments requiring respondents to rate the frequency and/or severity of some of the 17 major symptoms contributing to a DSM—III—R (American Psychiatric Association, 1987) or DSM—IV (American Psychiatric Association, 1994) diagnosis (Reference Meltzer-Brody, Churchill and DavidsonMeltzer-Brody et al, 1999; Reference Fullerton, Ursano and EpsteinFullerton et al, 2000). These have shown promising results equivalent to longer 17-item measures, although none has yet been validated on independent samples. Brewin et al (Reference Brewin, Andrews and Rose1999) found that victims of violent crime at high risk of developing PTSD 6 months later could be identified by their reports at 3 weeks post-crime of at least three re-experiencing or arousal symptoms. Our aim in this study was to test a brief 10-symptom screening instrument with survivors of a rail crash and then to validate the findings on our crime victim data.
METHOD
Sample 1: rail crash survivors
Participants
Participants had all been passengers on one of two trains that crashed into one another at Ladbroke Grove, London, on 5 October 1999. There were high levels of injury and loss of life, both from the impact and from smoke inhalation. There were three groups of respondents: 18 patients treated at St Mary's Hospital, Paddington; 15 patients treated at the Royal Berkshire Hospital, Reading; and 8 members of a survivors' group set up after the crash. The sample consisted of 21 men and 20 women with a mean age of 38.3 years (s.d.=10.3 years).
Measures
Screening questionnaire. This was designed for trauma victims in general and consisted initially of a single sheet of 16 items. Of these, five were re-experiencing items and five were arousal items taken from the PTSD Symptom Scale—Self Report version (PSS—SR; Reference Foa, Riggs and DancuFoa et al, 1993). As in our previous work, the threshold for a positive response was designed to correspond to a rating of 2 on the 0-3 scale employed by the original PSS—SR. The PSS—SR instructions were amended as follows: ‘Please consider the following reactions which sometimes occur after a traumatic event. This questionnaire is concerned with your personal reactions to the traumatic event which happened to you. Please indicate whether or not you have experienced any of the following at least twice in the past week.’ Respondents ticked either ‘Yes’ (scored 1) or ‘No’ (scored 0). A further three items enquired about negative emotions and there were three filler items, but analyses involving these items are not reported. The final 10-item version of the Trauma Screening Questionnaire (TSQ) is given in the Appendix.
Clinician-Administered PTSD Scale (CAPS—I; Reference Blake, Weathers and NagyBlake et al, 1995 ). This is a well-validated structured clinical interview designed to elicit the frequency and severity of symptoms and to assign a DSM—IV diagnosis. Interrater and test—retest reliability are good (Reference Blake, Weathers and NagyBlake et al, 1995). In this study a subsample of 28 CAPS interviews were subjected to independent blind rating, which produced 100% agreement on the presence or absence of a PTSD diagnosis with the interviewer rating.
Procedure
In the course of routine clinical follow-up following their involvement in the train crash, teams from the Brent, Kensington, Chelsea & Westminster Mental Health Trust and the Royal Berkshire Hospital contacted patients by letter, inviting them to take part in a study of the care received following major disasters. The 41 respondents agreeing to take part (18 out of 44 contacted from St Mary's; 15 out of 25 contacted from the Royal Berkshire Hospital; no response data available from the survivors' group) were asked to describe their current reactions to the accident and its aftermath by completing the screening questionnaire. They then gave consent for a second interview conducted approximately 1 week later, during which the CAPS was administered. All interviews, which took place between May and November 2000, were conducted by telephone and were tape-recorded. Patients meeting the criteria for PTSD at the second interview were informed of their diagnostic status and treatment options were discussed with them.
Analysis
The performance of the screening instrument was assessed by reference to two standard criteria: sensitivity (i.e. the probability that someone with a PTSD diagnosis will have tested positive) and specificity (i.e. the probability that someone without a PTSD diagnosis will have tested negative). These criteria are independent of the prevalence of the disorder in the population, and so can be compared readily across studies. In practice, the researcher or clinician generally wants to know the answer to two slightly different questions that are sensitive to population prevalence. What is the probability that someone with a positive test will report a diagnosis of PTSD? What is the probability that someone with a negative test will not receive a PTSD diagnosis? The answers to these questions are given by the positive and negative predictive power of the screening test, respectively. The performance of the test was also expressed in terms of the percentage of cases correctly classified as having or not having PTSD (overall efficiency).
Sample 2: crime victims
Participants
We recruited victims of violent crime from police and hospital sources. The 157 participants who entered the study (118 men, 39 women) had an average age of 35 years (s.d.=13 years). Full details of the sample are given in Roseet al (Reference Rose, Brewin and Andrews1999).
Measures
Post-traumatic stress symptoms and diagnoses were assessed using the PSS—SR (Reference Foa, Riggs and DancuFoa et al, 1993). As before, symptoms were counted as present if they were rated at least 2 on the 0-3 scale. A diagnosis of PTSD was assigned if the DSM—III—R criteria of at least one re-experiencing symptom, three avoidance/numbing symptoms and two arousal symptoms were met. Diagnoses based on the PSS—SR have been shown to be highly concordant with diagnoses based on structured interviews (Reference Foa, Riggs and DancuFoa et al, 1993).
Procedure
Participants completed the PSS—SR during interviews that in all cases were conducted within 1 month of the crime (mean 21 days post-crime, range 9-31 days, s.d.=5.6 days). Thus, participants did not fulfil the duration criterion for a DSM—III—R diagnosis of PTSD, although they fulfilled all other criteria.
RESULTS
Sample 1: rail crash survivors
A total of 14 out of the 41 respondents received a CAPS diagnosis of PTSD, which is a prevalence rate of 34%. First we confirmed that a threshold of around three or four re-experiencing and arousal symptoms offered optimum predictive power relative to other possible cut-offs.
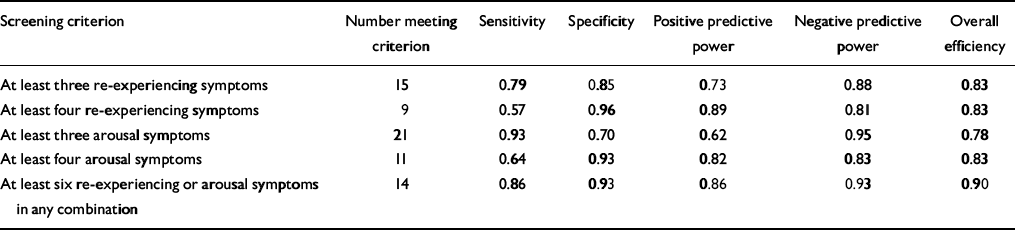
Performance at these two cut-offs is presented in Table 1, which shows that either of these thresholds offers overall efficiency of around 80%. Although both thresholds perform similarly, arguably the threshold of three re-experiencing symptoms offers the best balance of sensitivity and specificity. Using a threshold of four re-experiencing symptoms would improve specificity but at a cost of weaker sensitivity. A threshold of three arousal symptoms would again offer relatively more sensitivity, but the threshold of four arousal symptoms offers relatively better specificity and optimum overall efficiency. Table 1 also shows the diagnostic efficiency of requiring respondents to endorse at least six out of the ten re-experiencing or arousal symptoms in any combination. This cut-off maximised overall efficiency and led to a substantial increase in sensitivity and specificity, with excellent positive and negative predictive power.
Table 1 Sensitivity, specificity and power to predict post-traumatic stress disorder of different symptom combinations in the rail crash sample
| Screening criterion | Number meeting criterion | Sensitivity | Specificity | Positive predictive power | Negative predictive power | Overall efficiency |
|---|---|---|---|---|---|---|
| At least three re-experiencing symptoms | 15 | 0.79 | 0.85 | 0.73 | 0.88 | 0.83 |
| At least four re-experiencing symptoms | 9 | 0.57 | 0.96 | 0.89 | 0.81 | 0.83 |
| At least three arousal symptoms | 21 | 0.93 | 0.70 | 0.62 | 0.95 | 0.78 |
| At least four arousal symptoms | 11 | 0.64 | 0.93 | 0.82 | 0.83 | 0.83 |
| At least six re-experiencing or arousal symptoms in any combination | 14 | 0.86 | 0.93 | 0.86 | 0.93 | 0.90 |
Sample 2: crime victims
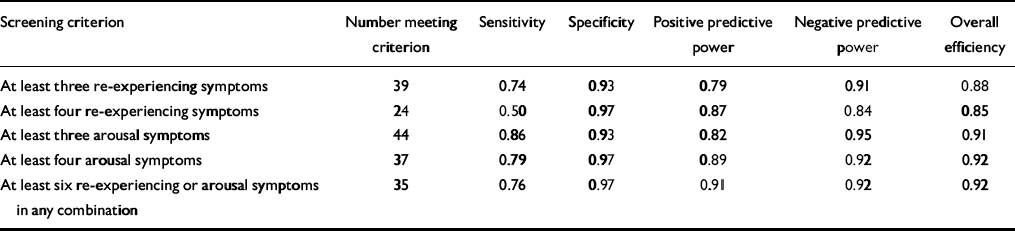
Forty-two respondents received a PSS—SR diagnosis of PTSD, which is a prevalence rate of 26.8%. Performance at the cut-offs of three re-experiencing symptoms and four arousal symptoms again maximised overall efficiency, which ranged from 88% to 92% (Table 2). As with the rail crash survivors, we investigated what was the optimum criterion for endorsing any combination of the ten re-experiencing and arousal symptoms. Once again the optimum cut-off was six symptoms, yielding a comparable level of overall efficiency and excellent positive and negative predictive value.
Table 2 Sensitivity, specificity and power to predict post-traumatic stress disorder of different symptom combinations in the crime victims sample
| Screening criterion | Number meeting criterion | Sensitivity | Specificity | Positive predictive power | Negative predictive power | Overall efficiency |
|---|---|---|---|---|---|---|
| At least three re-experiencing symptoms | 39 | 0.74 | 0.93 | 0.79 | 0.91 | 0.88 |
| At least four re-experiencing symptoms | 24 | 0.50 | 0.97 | 0.87 | 0.84 | 0.85 |
| At least three arousal symptoms | 44 | 0.86 | 0.93 | 0.82 | 0.95 | 0.91 |
| At least four arousal symptoms | 37 | 0.79 | 0.97 | 0.89 | 0.92 | 0.92 |
| At least six re-experiencing or arousal symptoms in any combination | 35 | 0.76 | 0.97 | 0.91 | 0.92 | 0.92 |
DISCUSSION
Performance of the Trauma Screening Questionnaire
There are a number of well-established risk factors for PTSD, such as female gender, previous trauma and previous psychiatric disorder, but few of these risk factors are consistent across different types of study and none of them accounts for a sufficient amount of the variance to be practically useful as predictors (Reference Brewin, Andrews and ValentineBrewin et al, 2000). Most potential screening instruments have therefore focused on symptom patterns to identify and predict cases of PTSD. This study represents the first attempt to cross-validate a brief, symptom-based screening instrument for PTSD in independent samples. In both samples a threshold of around three to four re-experiencing or arousal symptoms provided a reasonably sensitive and specific measure of the presence of PTSD. The level of prediction obtained among the rail crash survivors (83% overall efficiency) when symptoms in each cluster were counted separately was lower than we achieved in our previous study, where the overall efficiency was 85-92%. However, by adopting the strategy of allowing respondents to endorse any combination of six or more re-experiencing and arousal symptoms, efficiency was increased to 90%. Using this criterion, equivalent levels of screening performance were obtained despite the samples differing in the type of trauma, the prevalence of PTSD and the time elapsed since the trauma.
This is a striking result for a number of reasons. One reason is that with the rail crash survivors we were capitalising on post hoc analyses of the data designed to yield optimum prediction, whereas in re-analysing the crime victim data we were replicating previously established cut-off scores. The second reason is that with the crime victims the items used for prediction were also used in the calculation of PTSD, whereas among the rail crash survivors prediction was kept separate from the diagnosis of PTSD. Finally, the crime victims study utilised a questionnaire assessment of PTSD status, whereas with the rail crash survivors we used a structured clinical interview. Despite these promising findings, it will be important to establish the criterion validity of the instrument in other settings and with other traumas in order to overcome any possible sources of bias in the two samples used.
Comparison with existing instruments
Most existing instruments involve the use of rating scales and decision rules, and contain 17 items or more (see Reference Brewin, Rose, Andrews, Ørner and SchnyderBrewin et al, 2002, for a review). They can be scored in two ways, either requiring respondents to meet the diagnostic criteria for PTSD (endorsing at least one re-experiencing symptom, three avoidance/numbing symptoms and two arousal symptoms) or to exceed a cut-off score. Data regarding the performance of such measures have been published by Blanchard et al (Reference Blanchard, Jones-Alexander and Buckley1996) using the PTSD Checklist, by Foa et al (Reference Foa, Cashman and Jaycox1997) using the Post-traumatic Diagnostic Scale, by Davidson et al (Reference Davidson, Book and Colket1997) using the Davidson Trauma Scale and by Başoğlu et al (Reference Başoğlu, Şalcioğlu and Livanou2001) using the Traumatic Stress Symptom Checklist. The performance of briefer screening instruments has been reported by Meltzer-Brody et al (Reference Meltzer-Brody, Churchill and Davidson1999) using the 4-item SPAN, and by Fullerton et al (Reference Fullerton, Ursano and Epstein2000) using the BPTSD-12 and BPTSD-6. However, the performance of some of these brief measures is probably inflated by the use of post hoc cut-off scores and none has yet been adequately validated. When we required the endorsement of at least six re-experiencing or arousal items in any combination, the overall efficiency of the screening instrument in this study was superior to all these measures, of whatever length. Performance was equivalent to that obtained from a comparison of diagnoses yielded by the two most highly regarded interview assessments currently available for PTSD: the Structured Clinical Interview for DSM-IV (SCID; Reference First, Spitzer and GibbonFirst et al, 1996) PTSD module and the CAPS. In a sample of 123 combat veterans, a CAPS total score of 65 was found to have a sensitivity of 0.84 and a specificity of 0.95 relative to a SCID diagnosis (Reference Blake, Weathers and NagyBlake et al, 1995).
General considerations in screening for PTSD
It is quite possible that other combinations of symptoms would be as effective as using the re-experiencing and arousal items. Previously it has been claimed that the avoidance and numbing symptom cluster is likely to be most efficient for screening purposes, because it is less common to reach the threshold for these symptoms than it is for the re-experiencing and arousal symptom clusters (e.g. Reference North, Nixon and ShariatNorth et al, 1999). Our data show that the greater predictive power of the avoidance and numbing cluster is almost certainly due to the fact that more symptoms are required to meet the criterion. If equivalent numbers of re-experiencing or arousal symptoms are required, levels of prediction appear to be just as good. Avoidance and numbing symptoms were not included in our instrument for several reasons. First, there are more of these items, so the length of the instrument would be increased; second, some of the items (e.g. the amnesia and foreshortened future items) are not always well comprehended by respondents.
To be useful, screening instruments ideally should be short and contain the minimum number of items necessary for accurate case identification. They should be simple and preferably not require respondents to ponder over large numbers of alternative scale points. They should be written in a language that is easy to understand. Their purpose should be plain and they should be acceptable to respondents. For ease of administration, self-report questionnaires would appear to be the most flexible solution. If they are to be scored by non-specialists, which would widen their applicability, simple decision rules for determining who passes and fails the screen would be at a premium. Also highly desirable for successful instruments is that they be accurate at detecting both current PTSD and the risk of future PTSD, and that they should work well with different traumas, with different periods of time elapsed post-trauma and with varying prevalence of PTSD.
Our instrument appears to meet most of these criteria. All the items are simple and easy to understand. The use of a clear frequency threshold allied to a Yes/No response format also simplifies matters for respondents, whereas other measures require them to make ratings on four— or five-point scales. Moreover, having a single symptom scale makes our measure extremely practical for use by other health professionals, who may not be familiar with the disorder and with the structure of PTSD symptom clusters. We have shown that among crime and disaster victims excellent levels of prediction can be obtained with as few as ten items, and that enquiring about more PTSD symptoms has little additional value for screening purposes. It should be noted that all these data were collected, on average, 3 weeks post-trauma or later, and our experience is that screening usually should be delayed until this time, because during the initial post-trauma period natural recovery processes are in operation (Reference BrewinBrewin, 2001). The next step is to implement the use of the instrument in primary health care or hospital settings in order to demonstrate that it is effective in improving the identification and treatment rates for cases of PTSD.
CLINICAL IMPLICATIONS
-
• Current post-traumatic stress disorder can be predicted effectively with as few as ten Yes/No questions about re-experiencing and arousal symptoms.
-
• A useful threshold is to ask whether symptoms have occurred at least twice in the past week.
-
• To allow for natural recovery processes, screening probably should not be attempted before 3-4 weeks post-trauma.
LIMITATIONS
-
• The findings should be replicated on larger samples.
-
• The findings should be replicated on samples experiencing different kinds of trauma.
-
• It is possible that other combinations of symptoms will prove to be as effective as using the re-experiencing and arousal items.
APPENDIX
Trauma Screening Questionnaire (TSQ)
Your own reactions now to the traumatic event
Please consider the following reactions which sometimes occur after a traumatic event. This questionnaire is concerned with your personal reactions to the traumatic event which happened to you. Please indicate (Yes/No) whether or not you have experienced any of the following at least twice in the past week.
-
1. Upsetting thoughts or memories about the event that have come into your mind against your will
-
2. Upsetting dreams about the event
-
3. Acting or feeling as though the event were happening again
-
4. Feeling upset by reminders of the event
-
5. Bodily reactions (such as fast heartbeat, stomach churning, sweatiness, dizziness) when reminded of the event
-
6. Difficulty falling or staying asleep
-
7. Irritability or outbursts of anger
-
8. Difficulty concentrating
-
9. Heightened awareness of potential dangers to yourself and others
-
10. Being jumpy or being startled at something unexpected







eLetters
No eLetters have been published for this article.