Several studies, beginning with Huon (Reference Huon1985), have established the potential efficacy of the use of self-help books in the treatment of binge eating (Cooper et al, Reference Cooper, Coker and Fleming1994, Reference Cooper, Coker and Fleming1996; Treasure et al, Reference Treasure, Schmidt and Troop1994, Reference Treasure, Schmidt and Troop1996; Reference Wells, Garvin and DohmWells et al, 1997; Reference Carter and FairburnCarter & Fairburn, 1998; Reference Thiels, Schmidt and TreasureThiels et al, 1998; Reference Loeb, Wilson and GilbertLoeb et al, 2000). A number of self-help books are available (Reference Weiss, Katzman and WolchikWeiss et al, 1986; Schmidt & Treasure, Reference Schmidt and Treasure1993, Reference Schmidt and Treasure1997; Reference CooperCooper, 1995; Reference FairburnFairburn, 1995). They may be used alone but are probably more effective when additional guidance is offered (Reference Fairburn, Carter, Garner and GarfinkelFairburn & Carter, 1997; Reference Loeb, Wilson and GilbertLoeb et al, 2000). Guided self-help may reduce the amount of more intensive therapy that is subsequently required within a stepped care model (Reference Fairburn and PevelerFairburn & Peveler, 1990; Reference Treasure, Schmidt and TroopTreasure et al, 1996). The present study examines the efficacy and effectiveness of two forms of guided self-help through a randomised controlled trial conducted in the context of a specialised secondary eating disorders service for adults. It was predicted that those having either form of help would improve more on average in the first 4 months and need less therapy overall compared with those receiving self-help with minimal guidance or those who were assigned to a waiting list, but that face-to-face guidance would be superior to telephone guidance.
METHOD
The randomised controlled trial compared two forms of guided self-help with each other and with self-help given with minimal guidance. The trial took place over 4 months. There was also a waiting-list comparison group. All groups were followed up for 8 months, during which time further treatment was offered depending upon the patients' clinical state within a rule-governed stepped care programme. The progress of the patients within each of the treatment conditions was compared in terms of both their symptomatic change and their overall service consumption over a 1-year period. The self-help treatment offered within the trial was based upon the book Overcoming Binge Eating, by Christopher Fairburn (Reference FairburnFairburn, 1995). This book offers substantial educational material and a self-help treatment programme based upon the cognitive—behavioural therapy for bulimia nervosa devised by its author and others (Reference Fairburn, Marcus, Wilson, Fairburn and WilsonFairburn et al, 1993). Use of the book with or without guidance has been shown to be helpful in binge eating disorder (Reference Carter and FairburnCarter & Fairburn, 1998; Reference Loeb, Wilson and GilbertLoeb et al, 2000).
Eligible participants were a consecutive series of patients presenting with bulimia nervosa, partial syndromes of bulimia nervosa or binge eating disorder to a specialised secondary eating disorders service for adults. Most were referred directly from primary care to the Leicester Eating Disorders Service, which has a specific catchment area. Diagnoses were made according to DSM—IV (American Psychiatric Association, 1994), and partial syndromes of clinical severity were described as cases of ‘eating disorder not otherwise specified’ within that classification. Exclusion criteria were as follows: significant risk of major self-harm; comorbid psychotic disorder or major substance misuse; severe electrolyte disturbance; major comorbid physical disorder; a body mass index below 18 kg/m2; a rapidly declining weight; and difficulties with spoken English or with reading and writing of a kind that would have impeded the research.
Patients were seen and assessed clinically within the service. Those judged to be eligible and without exclusion criteria were asked whether they were willing to take part in the trial. A written explanation and consent form was used. Those who declined to take part were offered treatment within the service in the usual way. This usually involved being placed on a clinical waiting-list. This list — not to be confused with the waiting-list condition of the trial — typically involved a wait of several months unless there were special circumstances. Those who consented to take part were given an early appointment for a first research assessment. They were subsequently randomly allocated to one of the four conditions.
Some patients were either already taking antidepressant medication, or were deemed to have clinical depression and were prescribed such medication at clinical assessment. These drugs were continued at stable dosage throughout the trial. The participants taking antidepressants were randomised separately so as to ensure their even distribution between the four treatment conditions, as were bulimia nervosa and non-bulimia nervosa cases. Randomisation was from blocks of eight. Eight envelopes with treatment assignments were put in a larger envelope and constituted the pool from which a participant's treatment was drawn. The pool was replenished with a further block of eight when only two envelopes remained.
Outcome measures
The principal measure of eating disorder was the Eating Disorder Examination (EDE; Reference Fairburn, Cooper, Fairburn and WilsonFairburn & Cooper, 1993) and the results reported here are based upon this instrument. This interview was given at intake and at 4, 8 and 12 months. Unfortunately it was not practical for the research assessor to be masked to treatment assignment. Self-report measures were used also but are not reported here.
Outcome was defined in two ways. One was the percentage change in key behavioural symptoms on the following EDE scales: objective binge episodes, self-induced vomiting and the global score. No improvement or a less than 25% reduction in key symptoms was categorised as ‘not improved’. An improvement of 25-75% was categorised as ‘some improvement’ and if there had been more than a 75% reduction in symptoms the patient was categorised as ‘importantly improved’. The other outcome was ‘full behavioural remission’, defined as an absence of either bingeing or vomiting in the month before the relevant assessment.
Treatment conditions
The details of the four treatment conditions were as follows.
Waiting-list
The patient was given an appointment for reassessment after 4 months, with the expectation of then being offered one of the full out-patient therapies available within the service — either cognitive—behavioural therapy or interpersonal psychotherapy (Reference Fairburn, Marcus, Wilson, Fairburn and WilsonFairburn et al, 1993; Reference Fairburn, Garner and GarfinkelFairburn, 1997).
Self-help with minimal guidance
The patient was given a copy of Overcoming Binge Eating together with a brief explanation by a therapist of how to use it (minimal guidance). Patients in this group were also given an appointment for reassessment after 4 months, with the expectation that they would be offered further therapy according to their needs as assessed at that time.
Self-help with face-to-face guidance
The patient was given a copy of Overcoming Binge Eating by a therapist immediately after the research assessment, and then invited for four out-patient guidance sessions spread over 4 months. Typically these sessions lasted about 30 min and occurred 2 weeks, 4 weeks, 2 months and 3 months after the research assessment. Again, the patient was reassessed at 4 months.
Self-help with telephone guidance
Patients were treated in the same way as the face-to-face guidance group except that the guidance was delivered through pre-arranged telephone calls. The telephone sessions were also of about 30 min duration.
In both the face-to-face and telephone guidance conditions the sessions were used to encourage patients and to help them to organise their use of the book. Those offering guidance were nurse therapists experienced in the treatment of eating disorders; however, they confined themselves to offering guidance in the use of the book rather than other advice or therapy.
Follow-up
At the 4-month reassessment appointment, patients were offered further treatment according to their clinical state and the degree to which this had changed since first assessment. Except in the case of unexpected and overriding clinical need, the offer of further treatment was made along the following lines. If there had been little or no improvement (categorised as ‘not improved’) the patient would be offered full therapy (either cognitive—behavioural therapy or interpersonal psychotherapy), as outlined above for participants in the waiting-list condition. Patients categorised as ‘importantly improved’ would be followed up and reassessed, but not given further treatment (although they could keep the book). If improvement fell between 25% and 75% (categorised as ‘some improvement’), the patient would be offered more guided self-help of the kind already experienced.
Participants were subsequently reassessed at 8 months and 12 months. At 8 months, the offer of further treatment was governed by the same rules as applied at 4 months. After the final assessment 12 months after entry to the trial, the patient was offered further treatment as judged necessary by clinical criteria.
Analysis
The outcomes at 4 months for the different treatment conditions were analysed on both a completer basis and an intention-to-treat basis, with the assumption that those dropping out had not improved. The outcome and service consumption measures at 12 months were compared only on an intention-to-treat basis.
RESULTS
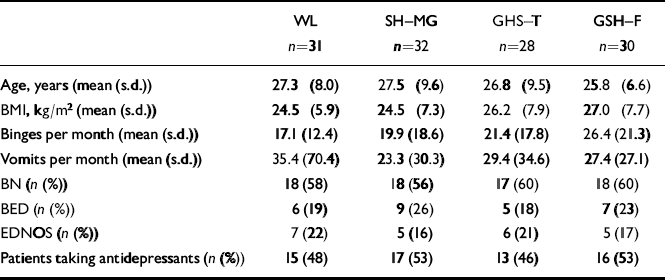
In all, about 150 eligible patients were approached, and about 20% declined to take part or failed to turn up for their first research assessment. (Unfortunately some refusals were not documented and these figures are therefore approximate.) One hundred and twenty-one patients were entered into the trial (Fig. 1). Of these, four were male. Seventy-one (59%) were diagnosed as having bulimia nervosa, 28 (23%) as having binge eating disorder and 22 (18%) as having an eating disorder not otherwise specified. Sixty-one patients (50.4%) were on antidepressant medication at the time of the first research assessment. Table 1 shows the characteristics of the different diagnostic groups. Thirty-one participants were randomised to the waiting-list, 32 to self-help with minimal guidance, 30 to self-help with face-to-face guidance and 28 to self-help with telephone guidance. Table 2 shows the characteristics of the groups on key demographic, diagnostic and symptomatic variables at the beginning of the trial. There was a wide variation in symptom severity, with some notable outliers leading to high standard deviations. However, inspection of the clinical data confirmed these as real rather than spurious, and they were not excluded from the analyses.

Fig. 1 CONSORT diagram. The number of eligible participants assessed clinically was at least 147, but three or four clinical assessments and offers of participation in the trial almost certainly went unrecorded. The reasons for early drop-out were: eight participants moved away from the area, one decided to seek private treatment, one got married and declared herself ‘better’, and for 20 the reasons were unclear. Two people were withdrawn from the follow-up period, one because of relapse into low-weight anorexia nervosa and one because of worsening symptoms. GSH, guided self-help; GSH—F, GSH with face-to-face guidance; GSH—T, GSH with telephone guidance; SH—MG, self-help with minimal guidance; WL, waiting-list.
Table 1 Characteristics of diagnostic groups at start of trial

| BN n=71 | BED n=28 | EDNOS n=22 | |
|---|---|---|---|
| Age, years (mean (s.d.)) | 24.7 (5.8) | 32.9 (10.9) | 26.6 (9.1) |
| BMI, kg/m2 (mean (s.d.)) | 23.2 (4.6) | 34.1 (8.5) | 22.7 (4.1) |
| Binges per month (mean (s.d.)) | 25.2 (19.9) | 14.5 (11.2) | 16.2 (14.2) |
| Vomits per month (mean (s.d.)) | 43.3 (51.4) | 0.4 (1.6) | 17.4 (19.2) |
| Patients taking antidepressants (%) | 55 | 41 | 48 |
Table 2 Comparison of treatment groups at start of trial
| WL n=31 | SH—MG n=32 | GHS—T n=28 | GSH—F n=30 | |
|---|---|---|---|---|
| Age, years (mean (s.d.)) | 27.3 (8.0) | 27.5 (9.6) | 26.8 (9.5) | 25.8 (6.6) |
| BMI, kg/m2 (mean (s.d.)) | 24.5 (5.9) | 24.5 (7.3) | 26.2 (7.9) | 27.0 (7.7) |
| Binges per month (mean (s.d.)) | 17.1 (12.4) | 19.9 (18.6) | 21.4 (17.8) | 26.4 (21.3) |
| Vomits per month (mean (s.d.)) | 35.4 (70.4) | 23.3 (30.3) | 29.4 (34.6) | 27.4 (27.1) |
| BN (n (%)) | 18 (58) | 18 (56) | 17 (60) | 18 (60) |
| BED (n (%)) | 6 (19) | 9 (26) | 5 (18) | 7 (23) |
| EDNOS (n (%)) | 7 (22) | 5 (16) | 6 (21) | 5 (17) |
| Patients taking antidepressants (n (%)) | 15 (48) | 17 (53) | 13 (46) | 16 (53) |
By the time of the first reassessment at 4 months, 30 (25%) had dropped out of treatment. Drop-out rates varied from 22% in the minimal guidance group to 29% for the waiting-list group (Table 3). These differences were not statistically significant. Table 3 shows the numbers who dropped out and who were assigned to each of the improvement categories at 4 months. Analysing these results on an intention-to-treat basis with the assumption that those who dropped out were not improved, and comparing individuals with a negative outcome (drop-out or no improvement) with those who showed either some or important improvement, there was a highly significant linear trend in relation to intensity of treatment. Those who had the most treatment had the greatest chance of improvement. Of those in the waiting-list group only 19% showed at least some improvement, compared with 25% in the minimal guidance group and 36% and 50% in the telephone and face-to-face guidance groups respectively. On partitioning the overall χ2, it was apparent that the heterogeneity of the groups mainly reflects differences in improvement between the face-to-face guidance group and all other groups combined (χ2=5.77, d.f.=1, P=0.016). No other between-group comparison within the partitioning analysis reached statistical significance.
Table 3 Categorical improvement at 4 months by treatment group1

| WL n (%) | SH—MG n (%) | GSH—T n (%) | GSH—F n (%) | |
|---|---|---|---|---|
| Not improved | 16 (52) | 17 (53) | 11 (39) | 8 (27) |
| Some improvement | 4 (13) | 4 (13) | 4 (14) | 7 (23) |
| Importantly improved | 2 (6) | 4 (13) | 6 (22) | 8 (27) |
| Dropped out | 9 (29) | 7 (22) | 7 (25) | 7 (23) |
The efficacy of the individual treatments was examined further by comparing the outcome of each treatment with that of the waiting-list condition using the much more stringent criterion of full behavioural remission — abstinence from both bingeing and vomiting. These individual analyses were performed using data from participants who completed the treatments rather than on an intention-to-treat basis. Results for both the face-to-face and telephone guidance groups were significantly better than the waiting-list group (χ2=4.42 and 4.75 respectively, P<0.05). This was not the case for the minimal guidance group. However, the actual rates of such remission were low. No patient achieved remission while on the waiting-list. Remission occurred in 2 (6%) of the minimal guidance group, 3 (10%) in the face-to-face group and 4 (14%) in the telephone guidance group. Of these 9 participants who had received some form of self-help and were in remission at 4 months, 8 were assessed at 12 months: 7 were found to be still abstinent from both bingeing and vomiting. These patients had received no further therapy and seemed to have achieved lasting remission through self-help alone.
Follow-up
After 4 months, the treatment received by the patients was determined by clinical need and the trial rules rather than randomly by allocation to treatment group. At the 12-month reassessment 77 patients were seen: 64% of the original number. However, 15 (19.5%) of those assessed at 12 months had effectively dropped out of clinical contact (2 had been withdrawn during the later stages of the trial for clinical reasons). Table 4 shows the outcomes and service consumption at 12 months. There was a tendency for the dropout from the study at 12 months to be higher in the waiting-list and minimal guidance groups (42% and 50% respectively) than in the telephone and face-to-face guidance groups (25% and 28% respectively). Drop-out with guided self-help was significantly lower when compared with the other two groups combined (χ2=5.77, P<0.05).
Table 4 Outcome and service consumption at 12 months

| WL | SH—MG | GSH—T | GSH—F | |
|---|---|---|---|---|
| Number in contact at 12 months (% of original group) | 18 (58) | 16 (50) | 21 (75) | 22 (70) |
| Number known to be in full remission (% of original group) | 7 (23) | 7 (22) | 6 (21) | 7 (23) |
| Number receiving additional GSH sessions (% of original group) | 1 (3) | 4 (13) | 4 (14) | 7 (23) |
| Number receiving full therapy (% of original group) | 12 (39) | 15 (47) | 11 (39) | 6 (20) |
| Mean number of clinical contacts of all kinds for total group including drop-outs | 9.2 | 10.6 | 12.5 | 10.5 |
| Total number of sessions needed to lead to one patient known to be in remission at 12 months | 10.7 | 12.9 | 10.1 | 9.3 |
Analysis of outcome at 12 months was made using groups based upon intention-to-treat, since the aim was to compare the effectiveness of the initial treatment approaches as part of an overall treatment package. The outcome criterion was full behavioural remission, in the sense of abstinence from both bingeing and vomiting. There was no significant difference in final outcome between the original treatment groups. The numbers in remission in each of the original treatment groups were 7 (23%) for the waiting-list, 7 (22%) for minimal guidance, 6 (21%) for telephone guidance and 7 (23%) for face-to-face guidance. Moreover, the total numbers of clinical contacts were similar for the different groups. However, the treatment careers of the patients after the first 4 months differed between the groups not only in terms of drop-out rate but also in the type of sessions received. Those in the face-to-face guidance group received more additional sessions of guided self-help and less full therapy. On a group basis, the investment of 10.7 clinical contacts had been necessary to produce each patient abstinent at 12 months in the waiting-list group, compared with 12.9 for the minimal guidance group, 10.1 for the face-to-face guidance group and 9.5 for the telephone guidance group. Again, there was no significant difference between the groups. Neither eating disorder diagnosis at the outset nor the use of anti-depressant drugs predicted outcome at either 4 or 12 months.
DISCUSSION
This study adds to earlier evidence for the efficacy of guided self-help in bulimic disorders but not for the efficacy of providing a self-help book without guidance. Within this study, self-help with minimal guidance was not significantly superior to the waiting-list condition. However, those who received additional guidance, particularly face-to-face, fared better. A substantial minority — around a third of those receiving it — were importantly improved by guided self-help. Such a rate of improvement is of the same order as rates reported for more elaborate treatments (Reference Schmidt, Hoek, Treasure and KatzmanSchmidt, 1998). A smaller proportion went into full remission but their gains were in general sustained over the next 8 months. Drop-out from treatment was high but similar for the different treatment groups.
Is guidance over the telephone as useful as that given face-to-face?
Overall, the study provides substantial evidence for the effectiveness of self-help with face-to-face guidance. On an intention-to-treat analysis, only face-to-face guidance was significantly better than the other interventions. However, telephone guidance does show promise. There was a tendency for more patients who received face-to-face guidance to achieve important improvement compared with those receiving telephone guidance, although with the more stringent criterion of remission they performed equally. Telephone guidance might be useful when face-to-face contact would be difficult to arrange, for instance in rural services where patients or therapists might have to travel long distances. This result adds to preliminary work suggesting a role for treatment delivered over the telephone (Reference Wells, Garvin and DohmWells et al, 1997). It is possible that other technologies such as e-mail or internet chat rooms might be used in a similar fashion (Reference Robinson and SerfatyRobinson & Serfaty, 2001; Reference Zabinski, Wilfley and PungZabinski et al, 2001).
Are the results generalisable?
There are plausible reasons why the present results might have either underestimated or overestimated the benefits of guided selfhelp. The trial might have produced better than expected effects because the guidance was given by nurse therapists experienced in the treatment of people with eating disorders. Such experienced clinicians might have achieved better results than those with less expertise. However, they confined themselves to helping the patients to persevere in using the book that formed the core of the treatment. Similar results would therefore probably be obtainable with less experienced therapists.
The setting of the study in a specialist secondary eating disorders service might have led to some underestimation of the potential benefits of guided self-help. In such a specialised setting, many of the patients might have been expecting rather more elaborate therapy and, furthermore, they were treated within a programme where they knew that they would be offered such therapy later if they required it. This expectation in this setting might have disadvantaged the guided self-help intervention. It is plausible that better results might be obtained in less specialised settings, such as primary care, where a modest intervention might be more valued. Furthermore, it is possible that the case mix included a greater proportion of more severe or treatment-resistant cases than would be typical in some other settings such as primary care. However, all of the patients were from a defined catchment area and nearly all were referred directly from primary care. This is typical of the Leicester Eating Disorders Service, but different from some other specialist services that accept referrals mainly on a tertiary basis.
Was the guidance optimal?
This study used only four sessions of guidance spread out over 4 months. Better results might be obtained with more sessions, or with a different distribution of sessions: clustering of the sessions early in treatment might have been preferable. In practice, where the difficulty of provision is not the lack of overall clinician time but rather the lack of specially trained clinicians, it may well be rational to offer many more guidance sessions. To date there has been no direct comparison of full manual-based cognitive-behavioural therapy with a similar number of sessions of guided self-help delivered by therapists without specialist training in the treatment. A study using trained therapists showed no clear difference between full therapy and guided self-help (Reference Thiels, Schmidt and TreasureThiels et al, 1998). However, it could well be that guided self-help with such substantial guidance might approach the efficacy of full therapy delivered by a specially trained therapist. Furthermore, the experience of providing the guidance would be likely to increase the special competence and confidence of any otherwise experienced clinician delivering the treatment.
Guided self-help as part of a stepped care programme
The most rational use of guided self-help may be as a first step in a stepped care arrangement. Within stepped care, more elaborate, expensive or scarcer treatments are reserved for those who fail to respond to lesser treatments (Reference Fairburn and PevelerFairburn & Peveler, 1990). Such schemes seem to be rational and to promise an efficient use of resources, although there is as yet little evidence that this is so in practice. Indeed, it remains plausible that obliging all patients to undergo lesser treatments before they have a chance to receive more major interventions might even be wasteful of resources. The design of the present study mimics some of the features of a stepped care approach. Most patients received a lesser treatment rather than being offered full therapy. Except for those allocated to the waitinglist condition, only those who failed to respond to self-help with minimal guidance or guided self-help were offered full therapy - or further guided self-help - according to their degree of continuing symptoms.
In this study the total amount of clinical contact and the final results were similar for the different treatment conditions. These results do not support the idea that the use of a stepped care approach within secondary care lessens the overall number of clinical contacts required to achieve each patient in remission 1 year after first assessment. However, there could still be some savings in practice. Those who had guided self-help would have tended to have shorter sessions and their provision would tend to be less demanding of therapeutic skill. Furthermore, some patients did achieve lasting remission with guided self-help. Where skilled therapists are in short supply, it might well be rational for their time to be spent with those people who have not responded to guided self-help.
One criticism of stepped care programmes is that they might lead some patients who could have responded to full treatment to drop out before they have had an opportunity to receive it. It is reassuring to note that those who received guided self-help dropped out of contact less than those who had received self-help with minimal guidance or had been obliged to wait for any treatment. They did not seem to be put off by the nature of their initial contact.
Taken together, the present results suggest that guided self-help might well be a useful and cost-effective first response to people presenting with bulimic disorders in secondary care, especially where the alternative is a long wait for full therapy. It might also be offered in primary care. Indeed, the optimal place for guided self-help within a rational overall response to bulimic disorders may well be in primary care and similar settings.
CLINICAL IMPLICATIONS
-
▪ Self-help based upon a book is an effective treatment for bulimia nervosa and binge eating disorder when accompanied by a few sessions of professional guidance.
Guidance may be useful even when given over the telephone.
-
▪ The experience of initial guided self-help was associated with a lower final drop-out rate compared with that of being on a waiting list.
-
▪ In a specialist secondary care setting, guided self-help did not save overall clinical input in the long run when it was delivered as part of a stepped care programme.
LIMITATIONS
-
▪ The study was carried out in a specialist secondary eating disorder service and the guidance was given by experienced therapists. The results may not generalise to other settings.
-
▪ Better results might have been obtained with more guidance or with guidance that was differently distributed over time.
-
▪ There is a need for further study of the effectiveness of guided self-help delivered in primary care.
Acknowledgements
We acknowledge with gratitude the funding of this study through the Trent National Health Service Research Scheme. We also thank Professor Christopher Fairburn of Oxford University for his interest and support and Helen Doll, also of Oxford, for her statistical advice.










eLetters
No eLetters have been published for this article.