The closure of almost all psychiatric hospitals in England and Wales has revealed that most, but not all, patients can manage without long-term in-patient care. A recent survey of residual populations in four psychiatric hospitals indicated that one-fifth of the patients were not considered for community placement on account of their problematic behaviours or extreme vulnerability (Reference Trieman, Hughes and LeffTrieman et al, 1998). In the post-institutional era, gaps in the provision of in-patient facilities have become apparent in many parts of the country. Despite recent initiatives aiming to increase the availability of 24-hour nursing homes, a relatively small yet enduring sector of patients continues to engage local admission units for protracted periods, partly accounting for the over-occupancy in acute wards nationwide (Reference Lelliott and WingLelliott & Wing, 1994). Many of these ‘new long-stay’ patients are difficult to manage in hospital wards, let alone in community facilities. Specialised facilities known as ‘ward in a house’ (Reference BennettBennett, 1980), ‘ward in the community’, or ‘hospital hostel’ have started to proliferate in recent years, yet these are still relatively scarce in the UK (Reference Lelliott and WingLelliott & Wing, 1994). As they are designed primarily to manage ‘new long-stay’ patients, it remains unclear whether ‘difficult-to-place’ patients treated in such facilities could benefit from the available rehabilitation input, and how many of those could eventually be discharged into the community.
Aim
The reprovision programme for Friern hospital, a large psychiatric institution in north London, provided an opportunity to study this issue on a long-term basis. When the majority of the hospital long-stay population moved into the community, a residual group of patients emerged as too disturbed or too disturbing to be considered for community placement (Reference Trieman and LeffTrieman & Leff, 1996a ). This difficult-to-place group was relocated in four designated facilities, three of which were hospital based (Reference Trieman and LeffTrieman & Leff, 1996b ). The patients were allocated to the different facilities on the basis of their catchment areas and not on the basis of any clinical criteria. The cost of those highly staffed facilities impacted significantly on the overall expenditure of the reprovision programme (Reference HallamHallam, 1996). The aim of this study was to evaluate the efficacy of such facilities by monitoring the long-term outcome for their residents.
METHOD
The care facilities
The basic features of the four facilities have been described elsewhere (Reference Trieman and LeffTrieman & Leff, 1996b ). Briefly, setting A was a ‘ward in the community’ situated within a converted Victorian house in a pleasant residential area. It was administered by a nearby general hospital, which provided services and medical cover. It had 20 places, a staff:patient ratio of 1.7:1 (ratio of full-time equivalent nursing staff to patients), and an ‘environmental index’ (Reference O'Driscoll and LeffO'Driscoll & Leff, 1993) score of 27, indicating that the number of rules and restrictions was equivalent to that in the Friern hospital wards.
Setting B was a ‘hospital hostel’, comprising three purpose-built houses located in the grounds of a small psychiatric hospital, close to a busy neighbourhood. The houses were homely, well designed and had no locked doors. There were 28 places, a staff:patient ratio of 1.7:1, and an environmental index of 10, equal to that in sheltered houses in the community.
Setting C was a ‘special needs’ unit which was part of the psychiatry department of a district general hospital. It provided intensive rehabilitation within a structured milieu. It had 12 places, a staff:patient ratio of 1.3:1, and an environmental index of 30.
Setting D was a ‘continuing care’ ward situated close to C. It contained a group of very withdrawn patients within a traditional institutional setting. There were 24 places, a staff:patient ratio of 1:1, and an environmental index of 22.
The care policies implemented in these facilities varied considerably with regard to the intensity and quality of the therapeutic input. The care environment was meant to be safe but as non-restrictive as possible. However, apart from setting B, these facilities were quite restrictive in their management policy. In general, the staff applied a slow-stream rehabilitation programme aiming to modify inappropriate social behaviour, to improve performance of basic living tasks and to expose the residents to the local community in a graduated manner. In practice, care programmes were not fully individualised, being applied neither consistently nor equitably. One of the facilities, D, offered very little active rehabilitation.
Sample
The study group consisted of 72 patients, all fulfilling the inclusion criteria applied to the long-stay population of Friern hospital by the Team for the Assessment of Psychiatric Services (TAPS) (Reference O'Driscoll and LeffO'Driscoll & Leff, 1993). Designated by the hospital staff as difficult to place, these residual patients were transferred to the specialised facilities in early 1993, as Friern hospital closed. Among the 72 patients were 8 catchment-area patients who were residing at that time in other hospitals, and were incorporated into the Friern reprovision programme.
Assessments
Assessments were carried out at baseline in Friern and other hospitals, shortly before the patients were relocated in 1993, and subsequently after 1 year (1994) and 5 years (1998). The patients were individually assessed by four schedules previously used in the TAPS study (Reference O'Driscoll and LeffO'Driscoll & Leff, 1993). The Present State Examination (PSE; Reference Wing, Cooper and SartoriusWing et al, 1974) and the Social Network Schedule (SNS; Reference Leff, O'Driscoll and DaysonLeff et al, 1990) are both structured interviews administered to the patient by a trained researcher. The Social Behaviour Schedule (SBS; Reference Sturt and WykesSturt & Wykes, 1986) and the Basic Everyday Living Skills (BELS; Reference Leff, Trieman and GoochLeff et al, 1996) schedule obtain information about the patient from senior care staff.
A new schedule, developed as part of this research, was the Special Problems Rating Scale (SPRS; Reference Leff and SzmidlaLeff & Szmidla, 2002). Its design stemmed from a pilot study in which a series of behavioural problems likely to impede placement in the community was compiled (Reference Trieman and LeffTrieman & Leff, 1996a ). It has proved to have a high interrater reliability. Any reported problem was confirmed by medical records and rated positive if severe and persistent over a 3-month period (Reference Trieman and LeffTrieman & Leff, 1996b ). New problems emerging during the follow-up period were rated using the SPRS. Environmental features of the care facilities were formally assessed by the environmental index (Reference O'Driscoll and LeffO'Driscoll & Leff, 1993), which measures the number of restrictions imposed on residents in their living environment.
Basic demographic data, psychiatric history and data pertaining to mortality, residential mobility, criminal offences and medication were obtained from members of staff, ward records and case notes.
Data analysis
The schedules generated both continuous and categorical data. Nine variables, derived from the PSE, BELS, SBS and SNS, were selected prospectively as representative of the major clinical and functional parameters, based on previous analysis of data from the total long-stay population (Reference Leff, Trieman and GoochLeff et al, 1996). For each variable the distribution of continuous data was tested for normality. For variables with skewed distribution, normality was induced by means of a logarithmic transformation. The mean scores were calculated together with the mean differences between the baseline assessment and the 1-year and 5-year follow-ups and 95% confidence intervals of these differences. In the case of categorical variables with dichotomous responses, the proportions were compared between the three points of time together with 95% confidence intervals. The analysis discarded cases for whom data were missing at one or more of the time points.
The total number of problems rated as positive on the SPRS, and the frequency of specific problems, were compared between baseline and the two follow-ups for the whole group.
RESULTS
Patients' demographic data
The mean age of the patients was 45.2 years. Males constituted 65% of the sample. Average length of stay in hospital was 3 years (1 to 12 years). Of the 72 patients, 62 (86%) had a diagnosis of schizophrenia, 4 of affective disorder, 5 of organic psychosis and 1 of personality disorder; four of the patients with a psychotic diagnosis had a secondary diagnosis of borderline IQ.
Administrative outcomes: mortality, vagrancy and crime
Over the 5 years, none of the patients was lost to follow-up or drifted out of contact with mental health services. Over that period 11 patients died, of whom 1 committed suicide (a crude death rate of 30 per 1000 person-years).
Incidents of a disruptive nature provoked by the patients were mostly confined to the premises, being generally well contained by the staff. Inappropriate behaviour in the neighbourhood was relatively uncommon, including a few cases of petty shoplifting, disrobing, urinating in the street and the like. Police were most commonly involved in returning to the facilities patients who absconded. Over 100 informal contacts with police were recorded over the 5-year follow-up, mostly associated with 8 patients presenting recidivistic behaviour. Two-thirds of the sample had not been in contact with the police. Serious assaults numbered 4, of which 2 were targeted at fellow residents and 2 at staff members. Legal charges were dropped in all cases, but the 2 perpetrators involved in these incidents (both from setting B) were transferred to secure wards.
Clinical outcome
The following data pertain to the 61 patients who were still alive at the 5-year follow-up.
Psychiatric state (PSE data)
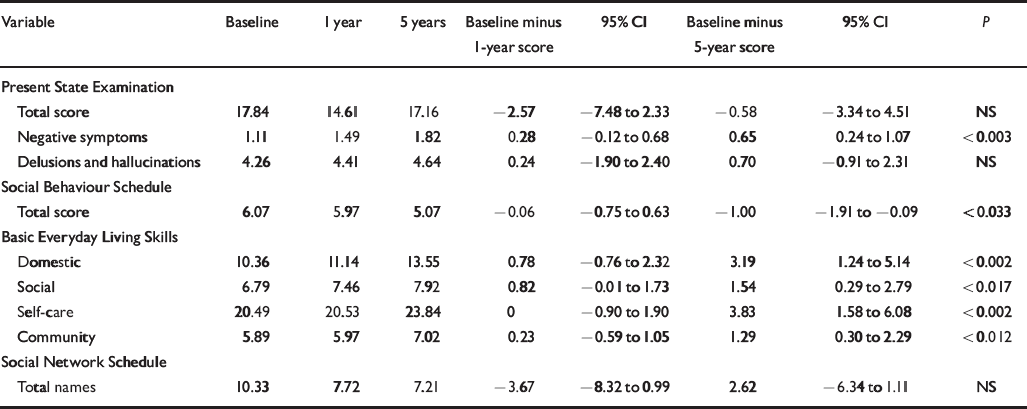
As shown in Table 1, there were no significant changes in the total PSE scores between baseline and the 1-year and 5-year follow-ups. Active psychotic symptoms (delusions and hallucinations sub-score) also remained remarkably stable. However, negative symptoms increased significantly between baseline and the 5-year follow-up.
Table 1 Changes in patients' measures at 1-year and 5-year follow-ups (n=61)1
| Variable | Baseline | 1 year | 5 years | Baseline minus 1-year score | 95% CI | Baseline minus 5-year score | 95% CI | P |
|---|---|---|---|---|---|---|---|---|
| Present State Examination | ||||||||
| Total score | 17.84 | 14.61 | 17.16 | -2.57 | -7.48 to 2.33 | -0.58 | -3.34 to 4.51 | NS |
| Negative symptoms | 1.11 | 1.49 | 1.82 | 0.28 | -0.12 to 0.68 | 0.65 | 0.24 to 1.07 | <0.003 |
| Delusions and hallucinations | 4.26 | 4.41 | 4.64 | 0.24 | -1.90 to 2.40 | 0.70 | -0.91 to 2.31 | NS |
| Social Behaviour Schedule | ||||||||
| Total score | 6.07 | 5.97 | 5.07 | -0.06 | -0.75 to 0.63 | -1.00 | -1.91 to -0.09 | <0.033 |
| Basic Everyday Living Skills | ||||||||
| Domestic | 10.36 | 11.14 | 13.55 | 0.78 | -0.76 to 2.32 | 3.19 | 1.24 to 5.14 | <0.002 |
| Social | 6.79 | 7.46 | 7.92 | 0.82 | -0.01 to 1.73 | 1.54 | 0.29 to 2.79 | <0.017 |
| Self-care | 20.49 | 20.53 | 23.84 | 0 | -0.90 to 1.90 | 3.83 | 1.58 to 6.08 | <0.002 |
| Community | 5.89 | 5.97 | 7.02 | 0.23 | -0.59 to 1.05 | 1.29 | 0.30 to 2.29 | <0.012 |
| Social Network Schedule | ||||||||
| Total names | 10.33 | 7.72 | 7.21 | -3.67 | -8.32 to 0.99 | 2.62 | -6.34 to 1.11 | NS |
Social behaviour problems (SBS data)
There was a significant change in the total SBS score between baseline and the 5-year follow-up (mean difference -1.00, 95% CI -1.9 to -0.09), representing an average reduction of 1 behavioural problem over that period of time. No change was detected at the 1-year follow-up.
Special problems (SPRS data)
Thirteen types of challenging behaviour were rated as present at baseline among members of the difficult-to-place group. By far the most frequent of these was aggression (Reference Trieman and LeffTrieman & Leff, 1996a ). Cumulative data, pertaining to 61 members of the group for whom data were available at the three time points, showed that the total number of 130 problem behaviours recorded at baseline remained quantitatively unchanged after 1 year. However, the total fell to 60 by the end of the 5-year follow-up. A very significant change was detected in physical aggression: the proportion of those exhibiting this behaviour fell from 47% at baseline to 7% at the 5-year follow-up (McNemar test, χ2=12.5, d.f.=1, P<0.001).
Basic everyday living skills (BELS data)
Significant changes in each of the four BELS sub-scores were recorded over the 5-year follow-up, indicating improved performance in all domains, including self-care, domestic chores, activity within the community and social relations. No such changes were apparent at the 1-year follow-up.
Social networks (SNS data)
There was no change in the size of the patients' social networks throughout the 5-year follow-up. On average, each patient had only 5 persons who could be named as acquaintances. Data were obtainable at each assessment for no more than half the sample, while data from all three consecutive assessments were available for only a third of the sample. The likelihood that those refusing interviews were the most socially withdrawn patients (Reference Leff, O'Driscoll and DaysonLeff et al, 1990) implies that the results might not be representative of the whole sample.
Movement between settings
As a result of the improvements in patients' behaviour and skills, by the 5-year follow-up 29 patients had been discharged to a variety of community settings: 24 went to residential care homes, 3 to nursing homes for elderly people with mental health care needs, 1 to an independent flat and 1 to live with family. There was no significant difference between the various facilities in the proportions of patients discharged.
Comparison between discharged and non-discharged patients
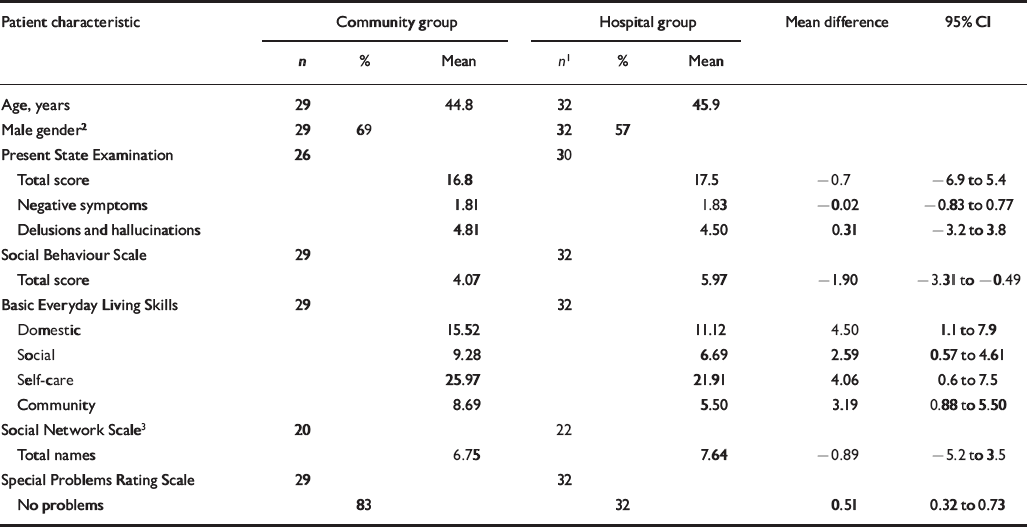
It was of interest to identify features that distinguished patients who were able to move to community homes from those who remained in the specialised facilities. A comparison of ‘movers’ and ‘stayers’, excluding the 11 patients who died during the 5 years, is shown in Table 2.
Table 2 Comparison between patients who remained in the specialised facilities and those who moved to community homes
| Patient characteristic | Community group | Hospital group | Mean difference | 95% CI | ||||
|---|---|---|---|---|---|---|---|---|
| n | % | Mean | n 1 | % | Mean | |||
| Age, years | 29 | 44.8 | 32 | 45.9 | ||||
| Male gender2 | 29 | 69 | 32 | 57 | ||||
| Present State Examination | 26 | 30 | ||||||
| Total score | 16.8 | 17.5 | -0.7 | -6.9 to 5.4 | ||||
| Negative symptoms | 1.81 | 1.83 | -0.02 | -0.83 to 0.77 | ||||
| Delusions and hallucinations | 4.81 | 4.50 | 0.31 | -3.2 to 3.8 | ||||
| Social Behaviour Scale | 29 | 32 | ||||||
| Total score | 4.07 | 5.97 | -1.90 | -3.31 to -0.49 | ||||
| Basic Everyday Living Skills | 29 | 32 | ||||||
| Domestic | 15.52 | 11.12 | 4.50 | 1.1 to 7.9 | ||||
| Social | 9.28 | 6.69 | 2.59 | 0.57 to 4.61 | ||||
| Self-care | 25.97 | 21.91 | 4.06 | 0.6 to 7.5 | ||||
| Community | 8.69 | 5.50 | 3.19 | 0.88 to 5.50 | ||||
| Social Network Scale3 | 20 | 22 | ||||||
| Total names | 6.75 | 7.64 | -0.89 | -5.2 to 3.5 | ||||
| Special Problems Rating Scale | 29 | 32 | ||||||
| No problems | 83 | 32 | 0.51 | 0.32 to 0.73 | ||||
It is evident that those who were discharged showed significantly fewer behavioural problems and had acquired significantly more skills than those who remained. The two groups did not differ in any clinical measure, in gender distribution or in the size of social network. The proportion of each group prescribed novel antipsychotics (‘movers’ 48%, ‘stayers’ 25%) did not differ significantly (χ2=3.57, d.f.=1, P>0.05).
Environmental Index
While at Friern hospital, members of the difficult-to-place group lived in a highly restrictive institutional environment (mean environmental index score 24, s.d.=6.6). Overall, the alternative facilities offered a more permissive environment (mean environmental index score 19 at 1 year, s.d.=8.5). At 5 years, when a high proportion of the former difficult-to-place patients were living in residential homes, the group was subjected to an even lower level of restrictiveness in comparison with that prevailing in Friern hospital (difference in mean environmental index=9; 95% CI -6 to -12).
Medication
In 1993, while still at Friern hospital, only 6 patients were treated with novel antipsychotic medication. At 5-year follow-up, more than 40% of the remaining group were prescribed clozapine, risperidone or olanzapine. The use of polypharmacy and high-dose regimes, which was common practice at Friern, altered to only a modest degree.
DISCUSSION
Clinical and social outcome of difficult-to-place patients
This outcome study of rehabilitation for difficult-to-place patients showed that, despite high staffing levels in the special facilities established for this group, no significant improvements in clinical and social states occurred during year 1 apart from a significant reduction in aggression, which made management of the patients easier (Reference Trieman and LeffTrieman & Leff, 1996b ). However, only 4 were able to move to community homes during this period. Over the succeeding 4 years major changes occurred, although not in all areas measured and not uniformly positive. The patients' mental state as assessed using the PSE remained very stable with one exception: negative symptoms worsened significantly. This is surprising given that the patients gained skills in all areas measured. It is also at variance with the 5-year findings for the rest of the long-stay populations of Friern and Clay-bury hospitals. This large group of patients, numbering 670 on discharge, showed no change in negative symptoms overall (Reference Leff and TriemanLeff & Trieman, 2000) although the earlier cohorts of discharges improved significantly (Reference Leff, Thornicroft and CoxheadLeff et al, 1994). The enduring positive symptoms of the difficult-to-place patients might be proposed as an explanation for the increase in negative symptoms over time, but the other long-stay patients also showed no change in the frequency of positive symptoms over the same period of follow-up.
Improvements in behaviour and skills
There was a significant reduction in the mean number of severe behaviour problems of the difficult-to-place patients, each patient on average losing 1 severe problem. It is highly unlikely that this could have been a response to changes in medication. Although there was a marked increase in the number of patients on novel antipsychotics, the lack of change in delusions and hallucinations combined with the increase in negative symptoms argues against their contribution to the behavioural improvements noted. The highly significant acquisition of skills across all areas of the BELS points to the efficacy of the rehabilitation programmes in the facilities, to which the reduction in severe problems is most plausibly attributable. As with the main group of long-stay patients, difficult-to-place patients were reluctant to complete the SNS: data from all three assessment points were available for only one-third of this sample. These data did not suggest any significant alteration in the quantity or quality of the social networks. Possibly the findings are biased towards a positive view, because patients who do not complete the SNS are more socially restricted than those who do (Reference Leff, O'Driscoll and DaysonLeff et al, 1990).
Factors leading to discharge
The improvement in patients' behaviour and skills enabled many of them to be discharged to sheltered accommodation in the community. At the end of 5 years, 29 (40%) were living in community homes. It is of clinical importance to be able to identify the changes that facilitated these moves. Hence, we compared the patients who were discharged with those who remained in the specialised facilities. It is not surprising that those who were able to leave were significantly more skilled in every area than those who remained, and exhibited fewer problematic behaviours. However, the two groups did not differ on any measure of mental state, in either positive or negative symptoms. Furthermore, there was no difference between the two groups in the proportion prescribed novel antipsychotics. This suggests that psychotic symptoms that are resistant to medication are no impediment to achieving clinically meaningful improvements in patients' behaviour and skills.
The need for rehabilitation facilities
Difficult-to-place patients will not disappear with the closure of the psychiatric hospitals, since a high proportion of them are new long-stay patients (Reference Trieman, Hughes and LeffTrieman et al, 1998). They continue to arise from the population of patients recently diagnosed as suffering from psychosis, and block the beds on admission wards because they need long-term specialised care. The profile of our sample, two-thirds of which were new long-stay, is similar to that of long-stay patients currently accumulating in admission wards in general hospitals. One of the reasons for this accumulation is the scarcity of rehabilitation facilities.
This study has shown that slow-stream rehabilitation in specialised facilities, even if not consistently applied, can produce sufficient improvement in 40% of difficult-to-place patients over 5 years to enable them to move to community homes. The consequent saving of money in the long term justifies the investment in such rehabilitation units (Reference Hallam and TriemanHallam & Trieman, 2001). However, it is our belief that faster progress in preparing such patients for discharge could be made by introducing individualised cognitive—behavioural programmes, and special training for the care staff (Reference Willetts and LeffWilletts & Leff, 1997). We report on an endeavour of this kind in another paper (Reference Leff and SzmidlaLeff & Szmidla, 2002).
CLINICAL IMPLICATIONS
-
▪ Slow-stream rehabilitation can enable a high proportion of difficult-to-place in-patients to be discharged to community homes.
-
▪ Persistent delusions and hallucinations do not preclude improvements in behaviour or the acquisition of living skills.
-
▪ New long-stay in-patients continue to arise from the community, requiring the provision of slow-stream rehabilitation in each district.
LIMITATIONS
-
▪ This group of difficult-to-place patients originated from inner-city areas and may not be representative of such patients nationally.
-
▪ The rehabilitation programmes in the four facilities varied considerably in quality.
-
▪ The unavailability of cognitive—behavioural therapy for psychosis at the time of the study may have resulted in poorer outcomes for this group of drug-resistant patients.







eLetters
No eLetters have been published for this article.