Post-partum depression affects approximately 10-15% of all mothers in Western societies (Reference Kumar and RobsonKumar & Robson, 1984; Reference O'Hara and SwainO'Hara & Swain, 1996). Recent epidemiological inquiries have reported prevalence rates for post-partum depression of 15.8% in Arab women (Reference Ghubash and Abou-SalehGhubash & Abou-Saleh, 1997), 16% in Zimbabwean women (Reference Nhiwatiwa, Patel and AcudaNhiwatiwa et al, 1998), 34.7% in South African women (Reference Cooper, Tomlinson and SwartzCooper et al, 1999), 11.2% in Chinese women (Reference Lee, Yip and ChiuLee et al, 2001), 17% in Japanese women (Reference Yoshida, Yamashita and UedaYoshida et al, 2001) and 23% in Goan women in India (Reference Patel, Rodrigues and DeSouzaPatel et al, 2002). Published reports on the epidemiology of post-partum depression from India are restricted to hospital-based data (Reference John, Seethalakshmi and CharlesJohn et al, 1977; Reference GautamGautam, 1989; Reference Patel, Rodrigues and DeSouzaPatel et al, 2002). To the best of our knowledge, this is the first prospective, community-based inquiry into the incidence of and risk factors for the development of post-partum depression reported from India.
METHOD
Setting
The study was conducted in a rural development block, 4 km from the district head-quarters town of Vellore, in the state of Tamil Nadu in south India. The Department of Community Health of the Christian Medical College at Vellore provides health and development services to the largely agrarian inhabitants of this development block, which is 127 km2 in area and comprises 88 villages and a population of 106 000. Resident health workers and part-time community health workers from the department provide domiciliary antenatal and post-natal care, and assist visiting teams of doctors and nurses in conducting monthly antenatal clinics at these villages. The antenatal programme covers 99.8% of pregnant women, and the department's data collection system includes computerised records of all pregnant women registered with the rural antenatal clinics along with their expected date of delivery. Fifty-two of the 88 villages were selected as representative of the whole area, geographically, demographically and socio-economically, and based on substantial registration of mothers at the antenatal clinics.
Participants
Over a 16-week period we recruited consecutive, consenting pregnant women over 34 weeks of gestation who were registered with the antenatal clinics, and who expected to remain in the area for a minimum of 6 weeks after delivery. We hoped to recruit 436 participants for an anticipated incidence of 18% (based on a pilot study), and 95% confidence intervals that would not exceed a relative precision of 20%.
Design
Health workers encouraged all eligible women to attend the monthly rural antenatal clinics, where one of us (M.C.) assessed the women for the presence and severity of depressive symptoms and risk factors. The interviews were conducted away from the general antenatal clinic with as much privacy as is possible in a rural setting. Participants who were unable to come to the antenatal clinic on the stipulated assessment days were evaluated at home on the same day. These assessments were repeated at the homes of the participants as early as possible after the sixth post-partum week. One of us (P.T.) independently confirmed assessments in a randomly selected proportion of participants and when diagnostic clarification was required. Health workers followed up women who were found to be severely depressed or suicidal at the antepartum assessment, to ascertain the need for referral for management. Mothers who were depressed at the post-partum assessment were entered into a randomised, placebo-controlled trial of fluoxetine therapy v. counselling by trained health workers. The results of this pragmatic trial will be reported elsewhere. Women who were actively psychotic or highly suicidal were referred to the department of psychiatry for immediate treatment. The institution's ethics committee approved the design of the study.
Interviews
Revised Clinical Interview Schedule
The revised Clinical Interview Schedule (CIS—R) is a structured interview for the assessment of common mental disorders in community settings (Reference Lewis, Pelosi and ArayaLewis et al, 1992). We used the Tamil version of the CIS—R (Reference Kuruvilla, Pothen and PhilipKuruvilla et al, 1999) as a standardised interview schedule, generated a symptom checklist, and diagnosed depression in accordance with ICD—10 (World Health Organization, 1992). This interview was conducted at both assessment points.
Assessment of risk factors
We constructed a questionnaire for the assessment of risk factors for post-partum depression, based on previously reported risk factors and factors identified as being of putative significance from a pilot study. This questionnaire was administered to each participant at both assessment points. The questionnaire covered the following areas:
-
(a) Past and family history of psychiatric disorder, including post-partum depression.
-
(b) Obstetric history: number and gender of children; history of miscarriages or stillbirths; pregnancy and delivery complications.
-
(c) Environmental problems: housing, income, financial difficulties.
-
(d) Relationships: family structure (joint or nuclear); support from and problems with husband; husband's alcohol intake; problems with parents and/or in-laws; emotional and physical support from family and others.
-
(e) Adverse life events in the year before delivery.
-
(f) Fears and expectations: wanted/unwanted pregnancy; desired gender of child; pressure to have a male child; worries about the child's health.
Data analyses
We calculated the incidence of post-partum depression, defining cases by the presence of depression according to ICD—10 criteria at post-partum but not antepartum assessment. The risk of depression according to the presence or absence of risk factors was assessed, and risk ratios calculated. We report 95% confidence levels for rates of depression and risk ratios. We also used chi-squared and Fisher's exact tests to assess the significance of these results.
We entered factors that yielded risk ratios greater than 2 and confidence intervals that did not include 1 on univariate analysis, into stepwise forward logistic regression analysis. We aimed for a parsimonious model, selecting only factors that were independent, and omitting factors thought to be influenced by the reporting bias of women with depression. Re-entering the same variables in stepwise backward logistic regression analysis checked the robustness of the final model. We computed odds ratios and confidence intervals for each variable in the final regression model.
As an outcome of secondary interest, we compared risk factors in women with both antepartum and post-partum depression with those who recovered from antepartum depression.
Data were analysed using the Statistical Package for the Social Sciences, version 6.0 (SPSS Inc.) and Epi Info version 5.01 (Centers for Disease Control, Atlanta, GA, USA).
RESULTS
Sample characteristics
Of the 991 pregnant women at various stages of gestation registered during the intake period of the study, 384 had completed 34 weeks of gestation and consented to participate. We assessed all 384, but only 359 (94%) women completed assessments after delivery. The mean duration of follow-up after delivery was 9.8 weeks (s.d. 2.2, range 6-12).
The mean age of the 384 women was 22.8 years (s.d. 3.7, range 17-37). The majority of the women were housewives and only 9% were in paid employment (Table 1). Thirty per cent of the women lived in huts, 67% owned no land and 46% reported a monthly income of less than 1000 rupees (approximately £13). The majority of the women (86%) lived in extended or joint families. One hundred and fifty-four women (40%) were primiparous. Nearly half (49%) of the women had no living children at the time of enrolment, and 30% of the remainder did not have a male child. Seventy-three per cent of the women were delivered at the base hospital of the community health department. Only 7% were delivered by Caesarean section and 9% required assisted deliveries.
Table 1 Social and demographic details of participants assessed before delivery

| Variable | Total (n=384) | Seen post-partum (n=359) | Not seen post-partum (n=25) |
|---|---|---|---|
| Age, years (mean (s.d.)) | 22.8 (3.7) | 22.8 (3.7) | 23.1 (3.5) |
| Years of education (n (%)) | |||
| 0 | 64 (16.7) | 58 (16.2) | 6 (24.0) |
| 1-5 | 75 (19.5) | 72 (20.1) | 3 (12.0) |
| 5-10 | 214 (55.7) | 198 (55.2) | 16 (64.0) |
| > 10 | 31 (8.1) | 31 (8.6) | |
| Family structure (n (%)) | |||
| Nuclear | 51 (13.3) | 47 (13.1) | 4 (16.0) |
| Extended/joint | 334 (86.7) | 312 (86.9) | 21 (84.0) |
| Occupation (n (%)) | |||
| Housewife | 350 (91.1) | 328 (91.6) | 22 (88.0) |
| Other | 34 (8.9) | 30 (8.4) | 3 (12.0) |
| Family income, rupees (n (%)) | |||
| < 1000 | 177 (46.1) | 168 (46.8) | 9 (36.0) |
| ≥ 1000 | 207 (53.9) | 191 (53.2) | 16 (64.0) |
| Type of house (n (%)) | |||
| Thatched roof/hut | 116 (30.2) | 107 (29.8) | 9 (36.0) |
| Tiled/concrete roof | 268 (69.8) | 252 (70.2) | 16 (64.0) |
| Owns land (n (%)) | |||
| No | 256 (66.7) | 233 (64.9)1 | 23 (92.0)1 |
| Yes | 128 (33.3) | 126 (35.1) | 2 (8.0) |
Of the 25 who were lost to follow-up, 16 had left the area; the remaining 9 had not completed a 6-week post-partum period by the close of the study. The demographic characteristics of the 25 women who were lost to follow-up did not significantly differ from the rest of the sample, except for land ownership (Table 1). Four of the 25 women not assessed following delivery were depressed at antepartum assessment, but rates of antepartum depression were similar for the 384 women assessed before delivery and the 359 women followed up after delivery.
We report further results only for the 359 women who completed both sets of assessments.
Prevalence and incidence of post-partum depression
The rates of antepartum and post-partum depression are shown in Table 2. The incidence of depression was 33/301 or 11% among women with no previous depression. Of the 58 women depressed before delivery, 38 were still depressed at the post-partum assessment. The overall prevalence of depression rose from 16% before delivery to 19.8% in the post-partum period.
Table 2 Prevalence and incidence of depression in participants assessed before and after delivery

| Number (n/N) | Rate (%) | 95% CI | |
|---|---|---|---|
| Antepartum depression | |||
| Prevalence | 58/359 | 16.2 | 12.5-19.9 |
| Recovery rate | 20/58 | 34.5 | 22.3-46.7 |
| Post-partum depression | |||
| Prevalence | 71/359 | 19.8 | 15.9-23.7 |
| Incidence | 33/301 | 11.0 | 7.1-14.9 |
Severity of depressive symptoms
The ICD—10 categories of severity of depression and total CIS—R scores for women with antepartum and post-partum depression are detailed in Table 3. Of the 58 women with antepartum depression, 11 out of 21 (52%) women with ICD—10 mild depression, 6 out of 19 (32%) women with moderate depression and 3 out of 19 (16%) women with severe depression recovered after delivery.
Table 3 Depressive episode categories and Clinical Interview Schedule, Revised (CIS—R) scores for women with antepartum and post-partum depression

| Post-partum depression | |||
|---|---|---|---|
| Antepartum depression (n=58) | All cases (n=71) | Incident cases (n=33) | |
| ICD—10 category (n (%)) | |||
| F32.0 Mild | 21 (36.2) | 6 (8.5) | 4 (12.1) |
| F32.1 Moderate | 19 (32.8) | 21 (29.6) | 10 (30.3) |
| F32.2 Severe | 18 (31.0) | 43 (60.5) | 18 (54.6) |
| F32.3 Severe with psychotic symptoms | 1 (1.4) | 1 (3.0) | |
| CIS—R total score (mean (s.d.)) | 12.8 (7.2) | 18.3 (7.4) | 16.6 (7.8) |
Sociocultural and obstetric risk factors
Incident cases of post-partum depression
Obstetric risk factors did not differentiate women with post-partum depression (n=33) from women without depression at either assessment (n=268), nor did most socio-demographic factors assessed (details available from the author upon request). More women with depression than without reported problems in their marital relationship: relative risk (RR) 6.31, 95% CI 3.53-11.26; P<0.001. This was likely to be an artefact of the depressed state, as it was less frequently reported as a problem at the antepartum assessment (RR 1.31, 95% CI 0.21-8.30; P=0.56). Similarly, more women with depression reported concerns about their husband's alcohol use than did those without depression (RR 3.27, 95% CI 1.67-6.38; P=0.003), although this was less frequently of concern at the antepartum assessment (RR 2.46, 95% CI 0.98-6.14; P=0.08).
Of the 33 women with post-partum depression, 18 delivered a male baby, compared with 53 of the 268 women without depression (RR 1.02, 95% CI 0.53-1.95; P=0.82). However, 10 of the 33 women with depression had specifically wanted a male child but were disappointed with the gender of the newborn compared with 32 of the 268 non-depressed women (RR 2.68, 95% CI 1.38-5.2; P=0.004). No significant difference was evident between the depression and non-depression groups in the women's preference for a daughter (not a son) and the gender of the newborn.
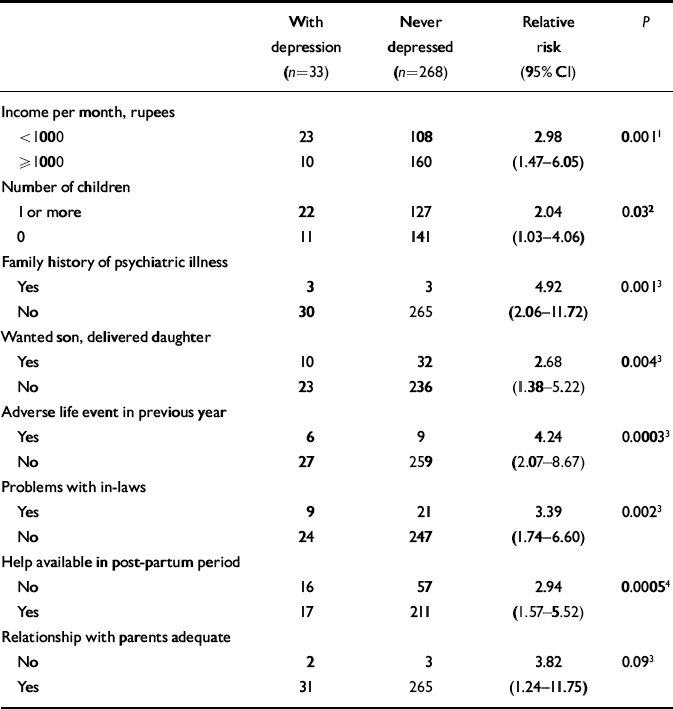
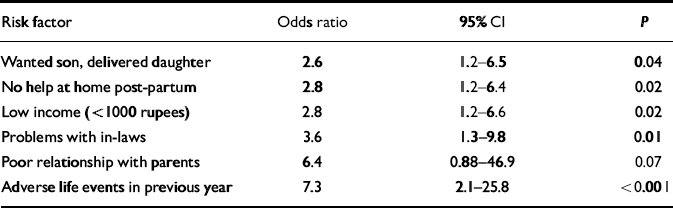
The incidence of depression was associated with the presence of eight risk factors (Table 4). A family history of psychiatric disorder and having one or more living children were excluded in stepwise forward regression analysis, with stepwise backward logistic regression yielding identical results. The final model posits that incident cases of post-partum depression were predicted by low income, an adverse life event in the year preceding delivery, problems with inlaws, poor relationship with parents, birth of a daughter when a son was desired, and lack of physical help at home during the post-partum period (Table 5). This model correctly classified 91% of women who developed depression after delivery. Although each factor individually predicts a more than doubled risk of developing depression post-partum, the presence of more than one factor is likely to have multiplicative effects. There are likely to be interactive effects as well, but these did not emerge as significant in logistic regression, possibly owing to the small number of incident cases of post-partum depression.
Table 4 Risk factors significant by univariate analysis for women with depression only post-partum v. women never depressed
| With depression (n=33) | Never depressed (n=268) | Relative risk (95% CI) | P | |
|---|---|---|---|---|
| Income per month, rupees | ||||
| < 1000 | 23 | 108 | 2.98 | 0.0011 |
| ≥ 1000 | 10 | 160 | (1.47-6.05) | |
| Number of children | ||||
| 1 or more | 22 | 127 | 2.04 | 0.032 |
| 0 | 11 | 141 | (1.03-4.06) | |
| Family history of psychiatric illness | ||||
| Yes | 3 | 3 | 4.92 | 0.0013 |
| No | 30 | 265 | (2.06-11.72) | |
| Wanted son, delivered daughter | ||||
| Yes | 10 | 32 | 2.68 | 0.0043 |
| No | 23 | 236 | (1.38-5.22) | |
| Adverse life event in previous year | ||||
| Yes | 6 | 9 | 4.24 | 0.00033 |
| No | 27 | 259 | (2.07-8.67) | |
| Problems with in-laws | ||||
| Yes | 9 | 21 | 3.39 | 0.0023 |
| No | 24 | 247 | (1.74-6.60) | |
| Help available in post-partum period | ||||
| No | 16 | 57 | 2.94 | 0.00054 |
| Yes | 17 | 211 | (1.57-5.52) | |
| Relationship with parents adequate | ||||
| No | 2 | 3 | 3.82 | 0.093 |
| Yes | 31 | 265 | (1.24-11.75) |
Table 5 Risk factors selected by stepwise logistic regression for incident cases of post-partum depression
| Risk factor | Odds ratio | 95% CI | P |
|---|---|---|---|
| Wanted son, delivered daughter | 2.6 | 1.2-6.5 | 0.04 |
| No help at home post-partum | 2.8 | 1.2-6.4 | 0.02 |
| Low income (< 1000 rupees) | 2.8 | 1.2-6.6 | 0.02 |
| Problems with in-laws | 3.6 | 1.3-9.8 | 0.01 |
| Poor relationship with parents | 6.4 | 0.88-46.9 | 0.07 |
| Adverse life events in previous year | 7.3 | 2.1-25.8 | <0.001 |
Antepartum depression
Of the 71 women with post-partum depression, in 38 (54%) the onset of depression was antenatal. The presence of depression in the last trimester was a strong predictor of depression at post-partum assessment (RR 5.98, 95% CI 4.12-8.67; P<0.001). Of the 58 women with antepartum depression 40 (70%) did not have sons before the current pregnancy. The proportions without sons did not differ significantly between those who recovered following delivery (65%) and those who did not (71%). The proportions of women who wanted sons but were disappointed were similar among women who recovered after delivery (25%) and those who continued to be depressed (21%).
Women with antepartum depression who continued to be depressed after delivery (n=38) were more likely than those who recovered (n=20) to report financial difficulties at the antepartum (RR 1.99, 95% CI 1.09-3.64; P=0.01) and post-partum assessments (RR 2.33, 95% CI 1.26-4.32; P=0.001). No significant difference was evident between these groups of women on other putative risk factors.
DISCUSSION
This study provides information on the incidence of and prospectively assessed risk factors for the development of post-partum depression in a consecutive series of women from a rural area of south India. In this cohort of pregnant women, 11% (95% CI 7.1-14.9) developed depression in the first 3 months after childbirth. The incidence of post-partum depression in this sample is similar to the rates of 7.7% to 14% assessed 9-12 weeks post-partum in the studies by O'Hara et al (Reference O'Hara, Neunaber and Zekoski1984), Kumar & Robson (Reference Kumar and Robson1984), Cooper et al (Reference Cooper, Campbell and Day1988) and Lee et al (Reference Lee, Yip and Chiu2001). The prevalence of depression in this cohort in the last trimester of pregnancy (16.2%, 95% CI 12-19.9) was similar to that in the second and third months after delivery (19.8%, 95% CI 15.9-23.7), although the severity was greater after delivery. These high prevalence and incidence rates in a rural community indicate that both antepartum and post-partum depression are significant public health problems in terms of frequency.
None of these mothers had sought help for their symptoms, although many were functionally impaired and were barely coping with their responsibilities. One possible reason for this low rate of utilisation of health services could be the belief held by mothers, family members and even the area health workers that this state is a normal part of pregnancy and the post-partum period, or a temporary maladjustment that would remit. A screening programme to detect post-partum depression and identify mothers in need of help certainly seems warranted.
Studies have documented the presence of antepartum depression in both Western (Reference Cox, Connor and KendellCox et al, 1982; Reference Kumar and RobsonKumar & Robson, 1984; Reference Cooper, Campbell and DayCooper et al, 1988; Reference Evans, Heron and FrancombEvans et al, 2001) and non-Western societies (Reference Kitamura, Shima and SugaaraKitamura et al, 1993; Reference Patel, Rodrigues and DeSouzaPatel et al, 2002). Some investigators (Reference O'Hara, Neunaber and ZekoskiO'Hara et al, 1984; Reference Nhiwatiwa, Patel and AcudaNhiwatiwa et al, 1998; Reference Najman, Andersen and BorNajman et al, 2000) — but not all (Reference Kumar and RobsonKumar & Robson, 1984) — assert that the presence of antepartum depression predicts the development of post-partum depression. Antepartum depression predicted continuing depression following delivery in a little over two-thirds of women in this study, and identified more than half of the women with post-partum depression. Screening for depression in the last trimester of pregnancy also therefore appears indicated.
Risk factors for developing depression after childbirth
Among women who developed depression only after childbirth in this sample, poverty, problems with in-laws (especially mothers-in-law), strained relations with parents, adverse life events during pregnancy, the birth of a daughter when a son was desired and lack of physical support after delivery were contributory. These risk factors are likely to be interactive as well as multiplicative in effect, although not demonstrable in logistic regression, presumably owing to the smallness of the sample.
In previous studies of adults in developing countries, female gender, low level of education and poverty were strongly associated with common mental disorders (Reference Patel, Araya and LimaPatel et al, 1999). Low educational attainment was not a significant risk factor for depression in the incident cases in this sample, but poverty was associated with depression in women with post-partum depression with or without an antepartum onset. Poverty appears therefore to be a vulnerability factor for the development of depression in women. Pregnancy and childbirth appear to be provoking factors for some women, in the context of a bias against daughters, and conflict with, or poor support from, significant others.
Western research has implicated spousal and parental relationships as risk factors for post-partum depression (Reference O'Hara, Neunaber and ZekoskiO'Hara et al, 1984; Reference Kumar and RobsonKumar & Robson, 1984). Mothers-in-law were specifically implicated in our study. Cultural factors probably underlie this difference. In this study sample, as is common in rural communities in India, most participants were from extended families and lived in the home of their parents-in-law. Problems with mothers-in-law, therefore, assume greater importance as a risk factor for the development of depression after childbirth, and this could be compounded by lack of support from parents, as was apparent in some of the women with depression in this sample.
Many women in this sample were defensive about their relationship with their husbands, especially when privacy was not adequate during interview, and mothers-in-law hovered suspiciously nearby. The common tradition of Indian women to observe pathibakhti (devotion to husbands) could account for their loyalty to their husbands despite strained relationships. One mother in particular repeated the statement, ‘I won't criticise my husband’, to any enquiry about her marital relationship. Thus, it is possible that strained relationships with spouses were underreported in this sample. The finding herein that the frequency of reporting of strained marital relationship (and problem drinking) increased in women with depression after childbirth, but was not significantly different from the rest of the sample when these women were not depressed before delivery, does not entirely support this premise. It is, however, possible that marital disharmony developed after delivery, possibly in relation to excessive alcohol use in this period (and/or in response to disappointment at the birth of a daughter), and these were actually risk factors for depression. Conversely, it is also possible that the frequency of marital disharmony and other subjectively reported risk factors elicited in some previous studies may be over-estimates due to the biased reporting of women with depression.
None of the women in this sample with depression had a previous history of psychiatric disorder related to or separate from the puerperium. A history of depression is likely to increase the risk but is not necessary for post-partum depression to occur. The fact that many other risk factors implicated traditionally were not significantly associated with depression either before or after delivery suggests that risk factors are likely to vary between cultures, and perhaps even within cultures.
The results of this study highlight the association between the pressure upon women to bear sons and the development of post-partum depression. Similar results were obtained in a recent study from Goa (Reference Patel, Rodrigues and DeSouzaPatel et al, 2002), where poverty and marital violence in the context of an infant gender bias were significant risk factors for the prevalence of post-partum depression. In many parts of India, economic and social pressures, and religious traditions associated with funeral rites, make sons much more desirable than daughters. Many communities in India (as in other developing countries) have practised selective abortion of female foetuses and female infanticide for years (Reference Booth, Verma and BeriBooth et al, 1994; Reference Nielsen, Liljestrand and HedegaardNielsen et al, 1997). The proportion of females to males has rapidly declined in India over the past three decades, and in some parts of the country is among the lowest in the world (Reference George, Abel and MillerGeorge et al, 1992). Current legislative and educational efforts to combat these practices need to be supplemented by measures to improve the perceived worth of women, such as higher literacy, equal employment opportunities and economic reforms favouring women, if significant changes in gender-related biases are to occur.
Factors aiding recovery from antepartum depression
Financial hardship was the only risk factor that differentiated women with antepartum depression who continued to be depressed after delivery from those who recovered. Although it was evident that societal and family pressures to have a male child were instrumental in the onset of and recovery from depression in some mothers, the data from this study do not uniformly support the role of this factor in recovery from antepartum depression in all mothers. Studies using larger samples are required to evaluate these relationships further.
Methodological issues
We did not use objective measures or standardised and validated instruments to rate the quality of relationships with significant others, or to elicit adverse life events. The wide confidence intervals of 2.1-25.8 for adverse life events and 0.88-46.9 for strained relationships with parents suggest that the strength of these risk factors should be viewed with caution. The same person (M.C.) assessed risk factors and baseline mental state as well as outcome status, but antepartum assessments were not referred to until analysis of results. Considering the numerous risk factors assessed and the 6-8 week interval between assessments, we do not believe that this biased our results significantly.
A major limitation of this study is that we could not attain the desired sample size in the time allotted to the study. This might have influenced the precision of estimates of risk factors, but is unlikely to have affected the point estimates of prevalence and incidence, which correlated well with published data. Another limitation is that practical constraints prevented assessment of personality and other variables that might be risk factors for post-partum depression, such as childhood sexual abuse and marital violence.
Clinical implications
The major clinical implications of our findings are that both antepartum depression and post-partum depression are common, heterogeneous and largely undetected public health problems. Screening for depression in the last trimester of pregnancy and in the post-partum period, by domiciliary health workers or at the immunisation clinic, is a service that needs to be incorporated into maternal and child health programmes. There is a paucity of research from developing countries addressing the consequences of post-partum depression on the cognitive, emotional and physical health of infants born to women with this disorder. Research aimed at measures to prevent post-partum depression and to elucidate what treatments work best — and are practical in low-income countries — is also urgently required.
CLINICAL IMPLICATIONS
-
▪ Antepartum and post-partum depressive disorders are common conditions.
-
▪ Integrating mental health services with maternal and child health services is indicated.
-
▪ Efforts to combat gender discrimination should be incorporated into public health and socio-economic policies.
LIMITATIONS
-
▪ The relatively small sample size of women with depression might have biased analyses of risk factors.
-
▪ Objective and validated instruments were not used to assess some risk factors, and the list of putative risk factors assessed was not exhaustive.
-
▪ Some risk factors significant on univariate analysis were not analysed with logistic regression since we attributed them to reporting bias; this might have led to an exclusion bias.
Acknowledgements
We are grateful to the mothers who participated and to all the health workers who helped in conducting this study. We thank Mrs Harriet Jeyakumari for help with interviews, Mr Suresh Babu for secretarial assistance, Dr Kurien George for help with identifying eligible participants, and Dr L. Jeyaseelan for statistical support. Dr Abraham Joseph helped with planning this study and constructively evaluated an earlier draft of this paper. This study was supported by an intramural research grant from the fluid research fund of the Christian Medical College, Vellore.










eLetters
No eLetters have been published for this article.