People with severe mental illness may at times be incapable of deciding on appropriate treatment. An advance directive is written while a person is competent to specify what decisions should be made about treatment, were he or she to become mentally incompetent. Although most often used in terminal illness, advance directives are relevant in mental illness where there is alternating competence and incompetence (Applebaum, 1991; Reference GaddGadd, 1998).
Thomas Szasz was among the first to suggest a ‘psychiatric will’ (Reference SzaszSzasz, 1982). This rather narrowly expressed the patient's request for (or refusal of) involuntary psychiatric interventions in the future. However, advance directives may concern wider issues in treatment that have an impact on subsequent hospitalisation. Although patients' views are contravened during an involuntary admission, once insight is recovered patients may be able to define advance directives for their management, should similar circumstances recur. The patients' directives, however, would not prevent their receiving compulsory treatment in the future, as the authority provided by civil commitment orders to treat without consent takes priority. Nevertheless, patient-derived advance directives may have potentially beneficial effects on the process of care such as the therapeutic alliance, communication and continuity in community care (Reference Dawson, King and PapageorgiouDawson et al, 2001). Despite discussion about the role of such directives (Applebaum, 1991; Reference Mester, Toren and GonenMester et al, 1994; Reference BacklarBacklar, 1997; Reference Ritchie, Sklar and SteinerRitchie et al, 1998; Reference GellerGeller, 2000; Reference Swanson, Tepper and BacklarSwanson et al, 2000), there has been no definitive evaluation of their impact on the delivery of mental health services. Our hypothesis was that patient's advance directives, when disseminated in written form to keyworkers and general practitioners and included in patients' case records, would reduce the frequency of compulsory readmissions to hospital.
METHOD
Participants and setting
In-patients receiving compulsory psychiatric treatment were recruited into a randomised trial. All those receiving compulsory treatment (under Sections 2, 3 or 4 of the Mental Health Act 1983 for England and Wales) in two inner-London acute psychiatric services who were due for discharge in the 12 months from October 1997 to October 1998 were eligible to take part. Hospital and community staff were fully briefed about the study, which received research ethical approval. We recruited each patient when staff indicated that discharge from hospital was imminent. Inclusion criteria were age 18 years and over and the ability to read English; exclusion criteria were patients under other specialised sections, those about to be transferred to other orders or to other hospitals, and those with organic brain disease. After complete description of the study to the participants, written informed consent was obtained. Patients were interviewed by A.P. or A.J. on the hospital wards at baseline, and in the patients' home, rehabilitation centre or hospital 12 months after discharge.
We allocated patients randomly using a block design, stratified according to whether this was the patient's first ever or subsequent sectioning. Blocks of twelve random combinations (six experimental, six control) were prepared and sealed in envelopes. Each research assistant telephoned an independent colleague in the trial centre, who chose the next envelope in each case. It was impossible to mask the research assistants to the patients' allocation as they were required to assist patients to make a directive in those allocated to the intervention group. However, systematic bias was unlikely as the primary outcome concerned compulsory hospital admission and was not based on any later assessment by the researcher.
Intervention group — advance directives
The advance directive was provided in the form of a booklet entitled Preferences for Care, which was given to patients in this group. The front page contained the name of the patient and his or her general practitioner, community psychiatric nurse, key-worker, consulting psychiatrist and social worker. We included the trial centre's address in case the booklet became lost. The booklet contained seven statements on future preferences for treatment (see Appendix). The content of the directive was not intended to address compulsory admission directly; rather, it aimed to give patients an opportunity to consider their future treatment on a wider basis, perhaps thereby increasing their trust and compliance and ultimately reducing the need for compulsory treatment. We encouraged patients to complete these and sign the directive. Patients who did not wish to write in the booklet themselves, dictated their preferences to the researcher. A rider printed at the end of the booklet indicated that professionals were not legally bound to comply with the preferences for care, if, for instance, the patient was subsequently recommitted. We asked each patient to keep the booklet in a safe place. We gave copies to the keyworker and general practitioner as well as filing copies with the hospital and general practice records. All patients received standard community psychiatric care.
Control group — usual care
All patients in the control group also received standard community psychiatric care. This consisted of a coordinated care programme in which psychiatric treatment was planned and provided by a multi-disciplinary community psychiatric team.
Outcome measures
In order to evaluate the impact of advance directives on our primary outcome, the rate of compulsory readmissions, we searched the hospital records for data on voluntary and involuntary admissions for the 5 years before baseline and the 12 months of follow-up. However, we also wished to examine their effect on other secondary measures that are an integral part of the objectives of community psychiatric care. These were: time spent in hospital compulsorily or voluntarily; reported symptoms of mental illness; prescribing; patients' satisfaction with service delivery; and patient's ability to take decisions for themselves. Our measures at baseline were:
-
(a) The Basis—32: a self-report questionnaire designed for patients with serious mental illness, including psychoses (Reference Eisen, Dill and GrobEisen et al, 1994).
-
(b) The Hospital Service Satisfaction Scale: an adapted brief version of the Verona Satisfaction Scale (Reference Ruggeri and Dall'agnolaRuggeri & Dall'agnola, 1993).
-
(c) The Health of the Nation Outcome Scales: a measure of patients' functional disabilities, completed by professionals (Reference Wing, Beevor and CurtisWing et al, 1998).
Twelve months after discharge we used:
-
(a) The Basis—32.
-
(b) The Hospital Service Satisfaction Scale for measurement of satisfaction with treatment over the preceding 12 months.
-
(c) The Self-Efficacy Scale (Reference SchwarzerSchwarzer, 1993), which assesses people's ability to make decisions and to conduct their lives.
-
(d) Questions on use of the advance directive.
-
(e) Questions for consultant psychiatrists and keyworkers on their awareness of the directive, its use and whether it could be improved.
We collected data on prescribing from patients' case notes.
Statistical analysis
We analysed the data using the Statistical Package for the Social Sciences (SPSS, 1998). All patients except for those never eventually discharged (see trial profile) were analysed in the group to which they were allocated in an intention-to-treat analysis. Our primary outcome was the number of people compulsorily readmitted under the Mental Health Act during follow-up. In the analysis of other outcomes we made group comparisons using standard t-tests for approximately normal data, Mann—Whitney tests for ordinal non-parametric data and the chi-squared statistic for categorical data. We report grouped medians for ordinal non-parametric data. The grouped median is the median weighted by the frequency of data in the adjacent categories. We used Cronbach's α to test the internal consistency of the adapted Hospital Service Satisfaction Scale (α=0.9). Analyses of variance were performed on log-transformed data. Where data were missing, we performed a sensitivity analysis using the last observation carried forward.
Hospital data for the year before the study indicated that 50% of patients discharged from a compulsory admission were readmitted within 12 months, and that 60% of these readmissions were compulsory. We estimated that detecting a reduction in the rate of compulsory readmission to 10% or less in the advance directives group (compared with 30% in the control group) at 90% power and the 5% level of significance would require 80 patients in each group.
RESULTS
Patient sample
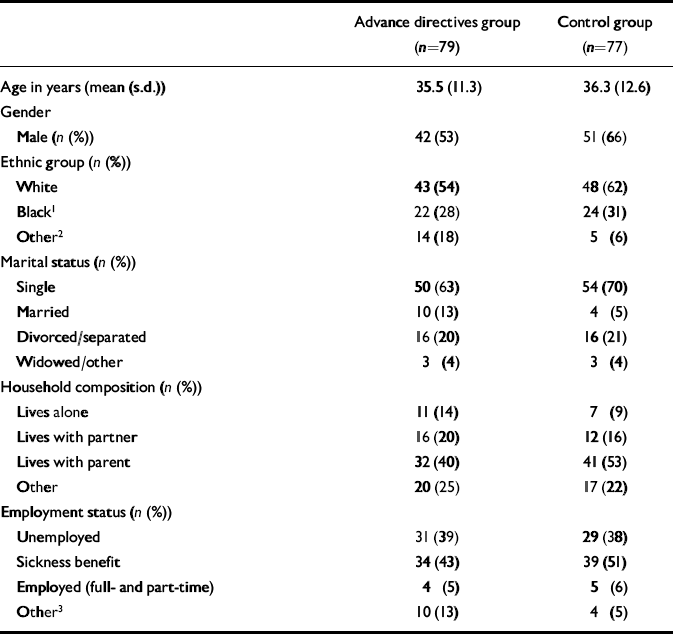
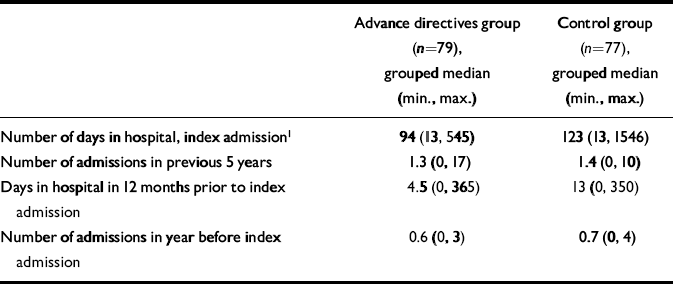
During the period of recruitment, 605 patients were under section of the Mental Health Act, of whom 161 entered the trial (Fig. 1). All but 6 of the 372 not meeting inclusion criteria were transferred to a further commitment order or to another hospital. There was no significant difference in gender or age between those considered and those eventually taking part. Nor was there any baseline difference in age, gender, ethnicity, marital status, house-hold composition or employment between the two arms of the trial (Table 1). There was no difference in previous hospitalisation, diagnosis, symptoms (Basis—32) or satisfaction with services (Tables 2 and 3). Patients in the advance directive group, however, spent less time in hospital during the index admission than those in the control group (Table 2).

Fig. 1 Trial profile.
Table 1 Demographic characteristics of patient groups at baseline
| Advance directives group (n=79) | Control group (n=77) | |
|---|---|---|
| Age in years (mean (s.d.)) | 35.5 (11.3) | 36.3 (12.6) |
| Gender | ||
| Male (n (%)) | 42 (53) | 51 (66) |
| Ethnic group (n (%)) | ||
| White | 43 (54) | 48 (62) |
| Black1 | 22 (28) | 24 (31) |
| Other2 | 14 (18) | 5 (6) |
| Marital status (n (%)) | ||
| Single | 50 (63) | 54 (70) |
| Married | 10 (13) | 4 (5) |
| Divorced/separated | 16 (20) | 16 (21) |
| Widowed/other | 3 (4) | 3 (4) |
| Household composition (n (%)) | ||
| Lives alone | 11 (14) | 7 (9) |
| Lives with partner | 16 (20) | 12 (16) |
| Lives with parent | 32 (40) | 41 (53) |
| Other | 20 (25) | 17 (22) |
| Employment status (n (%)) | ||
| Unemployed | 31 (39) | 29 (38) |
| Sickness benefit | 34 (43) | 39 (51) |
| Employed (full- and part-time) | 4 (5) | 5 (6) |
| Other3 | 10 (13) | 4 (5) |
Table 2 Baseline characteristics concerning hospital care
| Advance directives group (n=79), grouped median (min., max.) | Control group (n=77), grouped median (min., max.) | |
|---|---|---|
| Number of days in hospital, index admission1 | 94 (13, 545) | 123 (13, 1546) |
| Number of admissions in previous 5 years | 1.3 (0, 17) | 1.4 (0, 10) |
| Days in hospital in 12 months prior to index admission | 4.5 (0, 365) | 13 (0, 350) |
| Number of admissions in year before index admission | 0.6 (0, 3) | 0.7 (0, 4) |
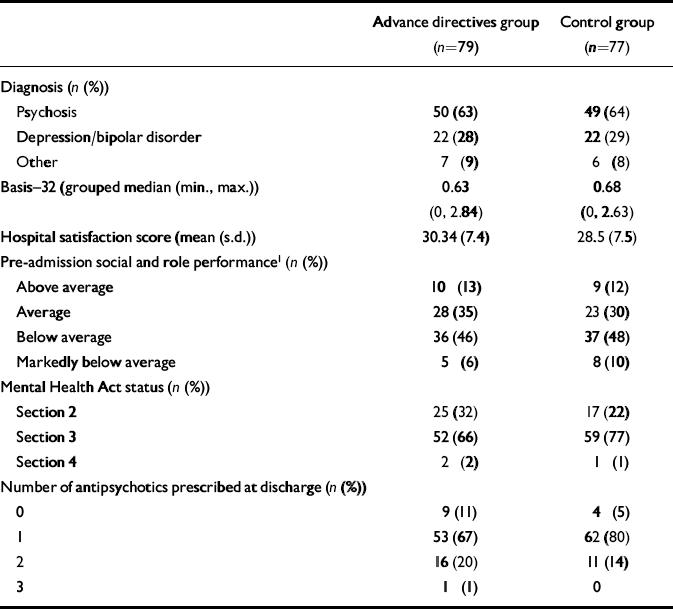
Table 3 Clinical characteristics at recruitment
| Advance directives group (n=79) | Control group (n=77) | |
|---|---|---|
| Diagnosis (n (%)) | ||
| Psychosis | 50(63) | 49(64) |
| Depression/bipolar disorder | 22(28) | 22(29) |
| Other | 7 (9) | 6 (8) |
| Basis—32(grouped median (min., max.)) | 0.63 | 0.68 |
| (0, 2.84) | (0, 2.63) | |
| Hospital satisfaction score (mean (s.d.)) | 30.34(7.4) | 28.5(7.5) |
| Pre-admission social and role performance1 (n (%)) | ||
| Above average | 10 (13) | 9(12) |
| Average | 28(35) | 23(30) |
| Below average | 36(46) | 37(48) |
| Markedly below average | 5 (6) | 8(10) |
| Mental Health Act status (n (%)) | ||
| Section 2 | 25(32) | 17(22) |
| Section 3 | 52(66) | 59(77) |
| Section 4 | 2 (2) | 1 (1) |
| Number of antipsychotics prescribed at discharge (n (%)) | ||
| 0 | 9(11) | 4 (5) |
| 1 | 53(67) | 62(80) |
| 2 | 16(20) | 11(14) |
| 3 | 1 (1) | 0 |
Outcome
We obtained data on our principal outcome for all randomised patients. Five patients were not discharged from hospital during the follow-up period and were removed from the analysis. We conducted face-to-face assessments of 59 (75%) patients in the advance directives arm and 55 (71%) in the usual care arm 12 months after discharge (Fig. 1). There was no difference in gender, age, ethnicity or primary diagnosis between those interviewed at follow-up and those not contacted, nor was there any difference in subsequent rate of involuntary admission between those contacted and those not contacted at follow-up.
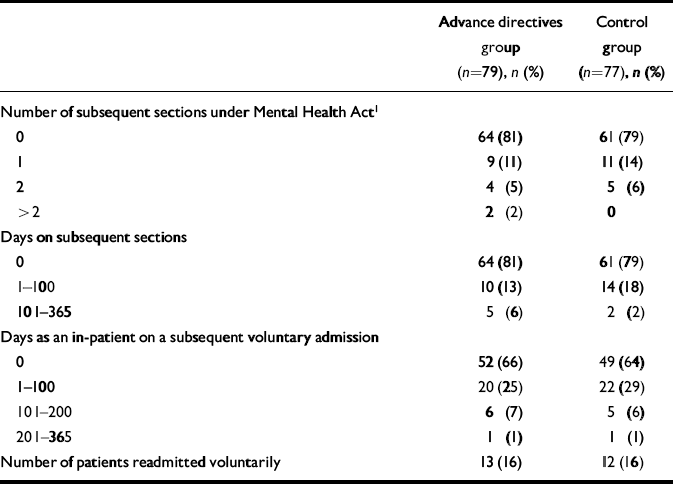
Fifteen participants (19%) in the experimental group and 16 (21%) in the control group were readmitted to hospital under section within 1 year of discharge (χ2=0.08, d.f.=1, P=0.8). There was no significant difference between the groups in the numbers of subsequent compulsory admissions, numbers of patients readmitted voluntarily, or days spent in hospital (Table 4). There was no difference in self-efficacy at follow-up (advance directives grouped median 42.66; control arm grouped median 42.25).
Table 4 Secondary outcome measures
| Advance directives group (n=79), n (%) | Control group (n=77), n (%) | |
|---|---|---|
| Number of subsequent sections under Mental Health Act1 | ||
| 0 | 64(81) | 61(79) |
| 1 | 9(11) | 11(14) |
| 2 | 4 (5) | 5 (6) |
| > 2 | 2 (2) | 0 |
| Days on subsequent sections | ||
| 0 | 64(81) | 61(79) |
| 1-100 | 10(13) | 14(18) |
| 101-365 | 5 (6) | 2 (2) |
| Days as an in-patient on a subsequent voluntary admission | ||
| 0 | 52(66) | 49(64) |
| 1-100 | 20(25) | 22(29) |
| 101-200 | 6 (7) | 5 (6) |
| 201-365 | 1 (1) | 1 (1) |
| Number of patients readmitted voluntarily | 13(16) | 12(16) |
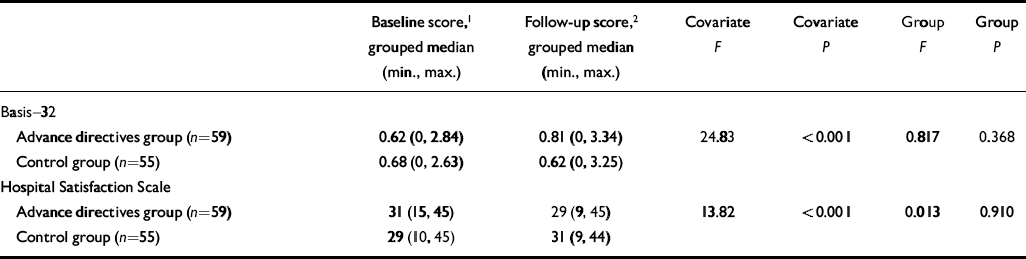
Scores on the Basis—32 were skewed at baseline towards health and at follow-up towards illness. However, there was no indication on other parameters that the patients' clinical state had deteriorated by the time of follow-up. Analysis of covariance (controlling for baseline values) of Basis—32 and Hospital Service Satisfaction scores for those interviewed at baseline and at follow-up showed no significant difference between the groups (Table 5). This finding was largely unchanged in a further analysis of covariance using last observation carried forward to account for missing data.
Table 5 Analyses of covariance (log-transformed data) for Basis—32 and Hospital Satisfaction Scale scores
| Baseline score,1 grouped median (min., max.) | Follow-up score,2 grouped median (min., max.) | Covariate F | Covariate P | Group F | Group P | |
|---|---|---|---|---|---|---|
| Basis—32 | ||||||
| Advance directives group (n=59) | 0.62 (0, 2.84) | 0.81 (0, 3.34) | 24.83 | <0.001 | 0.817 | 0.368 |
| Control group (n=55) | 0.68 (0, 2.63) | 0.62 (0, 3.25) | ||||
| Hospital Satisfaction Scale | ||||||
| Advance directives group (n=59) | 31 (15, 45) | 29 (9, 45) | 13.82 | <0.001 | 0.013 | 0.910 |
| Control group (n=55) | 29 (10, 45) | 31 (9, 44) |
Only 8 (13.5%) of 59 patients in the advance directives group interviewed at follow-up reported that they had found the directive useful. These patients considered that it helped other people to know that they had been ill and when they were relapsing; reminded them of things they could do to make life better; helped with reality testing; and enabled them to evaluate their illness. The consulting psychiatric physicians were concerned that the directives were yet another administrative burden. Although in favour of the trial, they believed that their management already took account of patients' wishes.
DISCUSSION
Evaluation of advance directives
Advance directives have seldom been evaluated in any health field. To our knowledge, this is the first randomised trial of advance directives for psychiatric care (Reference Henderson and LaugharneHenderson & Laugharne, 2000). The use of advance directives involves complex processes and conditions of implementation.
Lack of impact of advance directives
There are several possible explanations for the lack of impact of advance directives on services in our trial. First, were patients competent to understand the role of an advance directive? Although not infallible, specialised competency assessments have been suggested as a means of determining whether patients could use advance directives (Reference BacklarBacklar, 1997; Reference Ritchie, Sklar and SteinerRitchie et al, 1998; Reference Srebnik and La FondSrebnik & La Fond, 1999). Patients entered our trial close to the date of their expected discharge and therefore, although able to consent, might not have had the capacity to make full use of the directives. Despite other clinical signs of recovery, patients were more likely to self-report symptoms on the Basis—32 at follow-up than at baseline. This suggests that near discharge patients had less insight into their problems (or were concerned to present themselves as being well) than 1 year later, when they reported their difficulties more frankly. Thus, their understanding of the directive at recruitment might not have been optimal. Even when the capacity to understand is normal, denial or other psychological mechanisms may prevent people from facing the implications of their illness (Reference Schwartz and BlankSchwartz & Blank, 1986). At follow-up, several patients could not remember the directive, also suggesting a reduced ability to concentrate at recruitment. Against this explanation is that A.P. and A.J. were mental health professionals with extensive experience of managing patients with psychotic disorders, and were able to assess competency adequately at the time patients were recruited.
Second, in both arms fewer patients than expected were compulsorily readmitted. Although this led to lower statistical power than predicted, the difference between trial arms in proportions of patients readmitted compulsorily was so small that inadequate power is unlikely to be an explanation.
Third, although our procedures for introducing the directives and ensuring that staff were aware of them met published recommendations (Reference BacklarBacklar, 1997), professionals may have been unable or unwilling to incorporate them into their clinical work (Reference BacklarBacklar, 1997; Reference Swanson, Tepper and BacklarSwanson et al, 2000). Alternatively, they may already have incorporated patients' views adequately. Although there is evidence that professional staff may not comply with medical advance directives (Reference Srebnik and La FondSrebnik & La Fond, 1999), small studies of mental health advance directives have indicated that compliance can be good (Reference Backlar and McFarlandBacklar & McFarland, 1996; Reference Sutherby, Szmukler and HalpernSutherby et al, 1999). However, the participating psychiatric units suffered the lack of resources typical of inner-city areas and the professionals were struggling to cope with the administration of the Care Programme Approach, which formalises the process of community psychiatric care in England and Wales. Frequent changes of keyworker might have led to confusion about the purpose of the directives or ignorance of their existence. Keyworkers in one psychiatric service were often not allocated before patients were discharged, which might also have reduced the impact of the directives. The directive was sometimes regarded as an administrative burden by staff, who assumed that their management already took account of patients' wishes. These difficulties, however, are not uncommon features of psychiatric services in large metropolitan areas, and are an expected part of any naturalistic setting in which advance directives are implemented.
Mental health services in many countries now prioritise user involvement (Department of Health, 1998). Unfortunately, use of the Mental Health Act may make patients fearful and suspicious of service personnel. Agreeing advance directives with their own mental health professionals may mean that they feel unable to be frank about their care with those who deliver it. In our trial, the directive was therefore drawn up with someone independent of the patient's care. To achieve such independence in routine settings, a patient advocate might be involved. However, this risks diminishing the treating professionals' sense of ‘ownership’ or commitment to honour the terms of the directive.
Fourth, the directives might not have been practical. This is unlikely, as each one was drafted with the patient and any directive considered to be impractical was amended after discussion with staff. However, appropriate requests (such as a single room in hospital) may have been ignored because of limited resources in the service. We speculated that staff, fearing the potential legal implications of the directives, might even increase their use of commitment orders to over-ride instructions they regarded as hard to meet (Reference GellerGeller, 2000; Reference Dawson, King and PapageorgiouDawson et al, 2001). We found, however, that the rate of compulsory readmission for all patients in the trial was lower than expected.
A final explanation for our results may be a lack of sustained awareness of the directives throughout the 12 months of follow-up. As ours was a pragmatic trial, we delegated this process to the clinical team. We suggest that patients' advocates might best keep the directive uppermost in the minds of patients and their professionals.
Overall effects of the trial
Our results suggest that advance directives do not prevent involuntary readmissions to hospital in people with serious mental illness. It is possible, however, that the trial had an overall effect, as the rate for all involuntary admissions went down. Although this drop may simply reflect a secular trend in the trial area, it runs counter to the increased number of involuntary admissions in England — from 23 725 in 1996-1997, to 25 415 in 1997-1998 (Department of Health, 1999). This could be a classic Hawthorne effect: professionals in both arms of the trial might have modified their behaviour in response to being observed in a trial that concerned patients' preferences and subsequent rehospitalisation. However, coupled with our observation that professionals believed that they already took account of their patients' preferences, this finding suggests that hospitalisation rates might be affected simply by increasing providers' sensitivities to patients' wishes.
Explanatory v. pragmatic trial
An explanatory trial might have been a first step in our assessment of advance directives in mental illnesses, but it is difficult to see how it could be conducted. Restricting recruitment to a narrowly defined sample of patients who fully comprehended the process would defeat our aim of reducing undesirable pathways to in-patient care for more vulnerable patients.
Advance directives and outcomes
It appears that mental health care users' advance directives had little impact on compulsory or voluntary readmission rates, clinical status or satisfaction with care over 12 months. Nevertheless, it remains intuitively desirable that patients whose psychiatric symptoms are in remission plan for treatment in the event of loss of mental competence (Reference Rogers and CentifantiRogers & Centifanti, 1991; Reference Nazareth, King and DaviesNazareth et al, 1995; Reference GellerGeller, 2000; Reference Swanson, Tepper and BacklarSwanson et al, 2000), and such planning could form a part of a relapse prevention programme. Since advance directives involve anticipatory planning for the future, they might exert a beneficial effect on such factors as the therapeutic alliance and communication. Even if rates of compulsory treatment were not affected, we cannot rule out such possible beneficial effects. Thus, the impact of advance directives on other aspects of care requires further study (Reference Srebnik and La FondSrebnik & La Fond, 1999; Reference GellerGeller, 2000).
CLINICAL IMPLICATIONS
-
▪ Users' involvement in their own care planning is now regarded as crucial.
-
▪ Advance directives completed by patients about to be discharged from admission under the Mental Health Act appear to have little impact on subsequent compulsory readmission.
-
▪ Advance directives require further examination when integrated as part of the Care Programme Approach.
LIMITATIONS
-
▪ Patients about to be discharged from hospitalisation under the Mental Health Act may not always be able to complete directives of this type.
-
▪ It can be difficult to convince clinical staff of the importance of patients' advance directives.
-
▪ Underfunding of — and high workloads in — community mental health teams militate against the routine use of advance directives.
APPENDIX
Preference statements completed in experimental arm
-
(a) I notice I am becoming ill again when I...
-
(b) Things that happened just before I was placed on a section and/or started to become ill were...
-
(c) If I do seem to be becoming ill again I would like...
-
(d) I would like you to contact...
-
(e) I wouldn't want...
-
(f) If I have to be admitted to hospital again I would like...
-
(g) In hospital I would like...
Acknowledgements
We thank all patients and mental health professionals who took part in the trial. Special thanks are also due to Robert Blizard, who advised on the statistical analysis.
This work was funded by the National Health Service (NHS) Executive, London Research and Development Programme. The views expressed are those of the authors and not necessarily those of the NHS Executive or the Department of Health. A.J. was part-funded by the Priory Hospitals Group. This work was supported by the following trusts: Royal Free Hampstead NHS Trust, the former Haringey Healthcare NHS Trust and Camden and Islington Community NHS Trust.











eLetters
No eLetters have been published for this article.