Studies from the UK and The Netherlands have demonstrated an excess of schizophrenia in immigrants, with particularly high rates in people of African—Caribbean and Surinamese origin (Reference Harrison, Glazebrook and BrewinHarrison et al, 1997; Selten et al, Reference Selten, Slaets and Kahn1997, Reference Selten, Veen and Feller2001). Although the explanation for these findings remains unknown, selective migration is excluded, given the large-scale influx of inhabitants from former colonies (Reference Sharpley, Hutchinson and McKenzieSharpley et al, 2001; Reference Selten, Cantor-Graae and SlaetsSelten et al, 2002). Results from Denmark and Sweden have been less informative, owing to the potential influence of selective migration (Reference Mortensen, Cantor-Graae and McNeilMortensen et al, 1997; Reference Zolkowska, Cantor-Graae and McNeilZolkowska et al, 2001). A question of primary importance is the specificity of the ‘migrant’ risk factor associated with schizophrenia.
Improved record linkage provided the impetus for a new Danish register-based cohort study of the risk of schizophrenia associated with migration. We restricted the cohort to people residing in Denmark by their fifteenth birthday, thus minimising the impact of selective migration. History of foreign residence was examined as a putative risk factor for schizophrenia in people with a Danish background (people born in Denmark of Danish-born mothers).
METHOD
Study group
All live-born children and new residents in Denmark are assigned a unique personal identification number (CPR number), and information about them is recorded in the Danish Civil Registration System (Reference MaligMalig, 1996). We used this information to obtain a large and representative data-set comprising all people born between 1 January 1954 and 31 December 1983 who were resident in Denmark by their fifteenth birthday. For everyone living in Denmark on 1 April 1968 or later, the Danish Civil Registration System contains a record of CPR number, gender, date and country of birth, maternal and paternal CPR number, maternal and paternal date and country of birth, and emigrations and immigrations to and from other countries, together with exact dates for these events. All citizens in Denmark are obliged to inform the authorities about any change of permanent address within 5 days. Failure to supply this information results in an inability to receive supplementary benefit (e.g. unemployment, sickness or disablement benefits, and educational aid from public funds), attend day nursery, nursery school, primary or lower secondary school, obtain free national health care, or obtain a tax deduction card (required for paid work). Therefore, it is very unlikely that migration into Denmark is not reported. Furthermore, it is also unlikely that migration out of Denmark is unreported, since this would make emigrants subject to taxation both in Denmark and in the emigrant country. As paid work is taxed heavily in Denmark, emigrants prefer to be taxed in the emigrant country.
The study population and their mothers and fathers were cross-linked with the Danish Psychiatric Central Register (Reference Munk-J⊘rgensen and MortensenMunk-Jørgensen & Mortensen, 1997), which contains data on all admissions to Danish psychiatric in-patient facilities since April 1969 and out-patient visits to psychiatric departments since 1995. From April 1969 to December 1993 the diagnostic system used was the ICD-8 (World Health Organization, 1967). From January 1994 this was replaced by ICD-10 (World Health Organization, 1992). Cohort members were designated as having schizophrenia if they had been admitted to a psychiatric hospital or received out-patient care with a diagnosis of schizophrenia (ICD-8 code 295 or ICD-10 code F20). Onset was defined as the first day of the first contact with a diagnosis of schizophrenia.
Statistical and data analyses
In total 2.14 million persons were followed up during residence in Denmark from their fifteenth birthday or 1 April 1970, whichever came later, until onset of schizophrenia, death or 31 December 1998, whichever came first. The relative risk of schizophrenia was estimated by log-linear Poisson regression (Reference Breslow and DayBreslow & Day, 1987) with the GENMOD procedure in SAS version 8.1 (SAS Institute, 1999). All relative risks were adjusted for age, gender, interaction between age and gender, and calendar year of diagnosis. Age and calendar year of diagnosis were treated as time-dependent variables (Reference Clayton and HillsClayton & Hills, 1993), whereas all other variables were treated as time-fixed variables unless stated otherwise. To obtain complete confounder control (Reference Breslow and DayBreslow & Day, 1980), age in years was categorised with the following cut-off points: 15, 16, 17, 18, 19, 20, 22, 24, 26, 28, 30, 35 and 40, and calendar year was categorised in 3-year bands in the ICD-8 period and in 1-year bands in the ICD-10 period. Values of P were based on likelihood ratio tests, and 95% confidence limits were calculated by Wald's test (Reference Clayton and HillsClayton & Hills, 1993). The adjusted score test (Reference BreslowBreslow, 1996) suggested that the regression models were not subject to overdispersion.
Country of birth was classified according to geographical region of birth: Denmark, Scandinavia (excluding Denmark), Europe (excluding Denmark and Scandinavia), Asia, the Middle East, Australia, Africa, North America, South America, Greenland, and unknown. Individuals were categorised according to the information in the Danish Civil Registration System concerning maternal country of birth, i.e. maternal reference status. Those born in Denmark were categorised as persons with Danish background (cohort members born in Denmark with mothers born in Denmark), second-generation immigrants (cohort members born in Denmark with mothers born outside Denmark) or other Danish-born (cohort members born in Denmark with no information about maternal country of birth). Individuals born outside Denmark were categorised as possible adoptions (cohort members born outside Denmark with mothers born in Denmark, i.e. either adoptions or children born to Danish women abroad), immigrants migrating with mother (cohort members born outside Denmark with information concerning maternal identity, i.e. mother has a Danish CPR number, meaning that she has been resident in Denmark) or immigrants migrating without mother (cohort members born outside Denmark with no information about maternal identity).
For those born in 1969 or later we have complete information about dates of immigration and emigrations to and from Denmark, and were able to examine the risk of developing schizophrenia in relationship to age at first residence in Denmark and the accumulated number of years lived in Denmark. Age at first residence in Denmark was categorised as: at birth, from birth to the fifth birthday, from the fifth to the tenth birthday, and from the tenth to the fifteenth birthday. The accumulated number of years lived in Denmark was treated as a time- dependent variable and categorised as: 0 to <5 years, ≥ 5 to <10 years, ≥10 to <15 years, ≥15 to <20 years, ≥20 to <25 years, or ≥25 years.
Among persons with a Danish background we examined history of foreign residence (defined as ever residing outside Denmark prior to age 15 years) and the age at which foreign residence occurred, i.e. from post-birth to the fifth birthday, from the fifth to the tenth birthday, and from the tenth to the fifteenth birthday. A person resident abroad during the ages 4-12 years would belong to all three categories. Parental history of psychiatric disorder was examined as a potential modifier or confounder of the risk associated with history of foreign residence. Parents were considered to have a history of psychiatric disorder if they had ever been admitted to hospital or received out-patient care for a psychiatric disorder (any ICD-8 or ICD-10 diagnosis). Parental history of psychiatric disorder was also studied as a potential modifier of schizophrenia risk among second-generation immigrants.
Region of birth and maternal reference status were further examined in relation to age at illness onset (total cohort). For those born in Denmark the most common age at illness onset is 22-23 years (Reference Pedersen and MortensenPedersen & Mortensen, 2001a ). Age in years at illness onset was stratified accordingly as <20, 20-21, 22-23, 24-25 or ≥26, examined in relation to the following categories: Danish background, second-generation immigrants, other Danish-born, and foreign-born.
RESULTS
A total of 10244 persons developed schizophrenia during the 32.6 million person-years of follow-up (Table 1). Foreign birth was associated with an increased risk of developing schizophrenia. The relative risk of developing schizophrenia in persons with any foreign region of birth was 2.45 (95% CI 2.25-2.67) compared with persons with Danish background, i.e. born in Denmark with mothers born in Denmark. The region of birth effect could not be reduced to foreign birth in general, as shown by significant differences in the relative risk of developing schizophrenia across regions of birth (P<0.001).
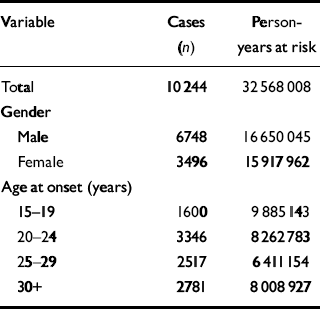
Table 1 Distribution of age and gender for cases of schizophrenia in a population-based cohort of 2.14 million persons resident in Denmark by their fifteenth birthday
| Variable | Cases (n) | Person-years at risk |
|---|---|---|
| Total | 10244 | 32 568 008 |
| Gender | ||
| Male | 6748 | 16 650 045 |
| Female | 3496 | 15 917 962 |
| Age at onset (years) | ||
| 15-19 | 1600 | 9 885 143 |
| 20-24 | 3346 | 8 262 783 |
| 25-29 | 2517 | 6 411 154 |
| 30+ | 2781 | 8 008 927 |
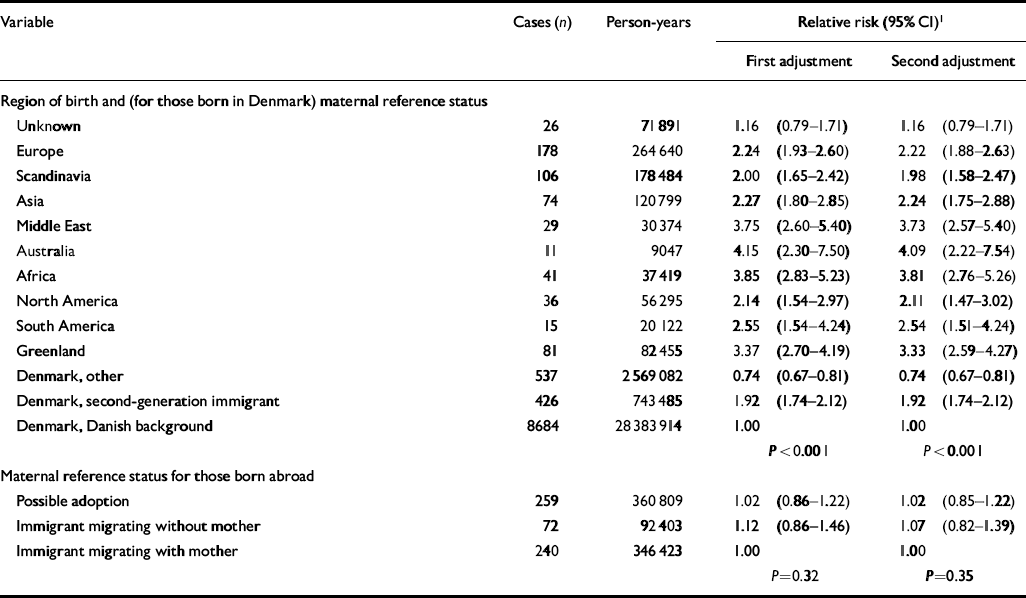
The relative risks obtained for specific categories of region of birth and maternal reference status (Table 2) were adjusted initially for age and its interaction with gender and for calendar year of diagnosis. A second similar adjustment of the relative risk adjusted simultaneously also for region of birth and for maternal reference status. In the foreign-born category, maternal reference status (possible adoption, with or without maternal reference) had no effect upon the risk of developing schizophrenia, nor was there any evidence that the effect of maternal reference status was modified by region of birth (P=0.23). Interestingly, there was no indication that foreign-born possible adoptees are at increased risk compared with foreign-born individuals from the same country. Also, the slightly elevated risk among those with unknown region of birth indicates that this category may represent a combination of Danish-born and foreign-born.
Table 2 Distribution of 10 244 cases of schizophrenia, 32.6 million person-years at risk and estimates of relative risk according to region of birth and maternal reference status
| Variable | Cases (n) | Person-years | Relative risk (95% CI)1 | |||
|---|---|---|---|---|---|---|
| First adjustment | Second adjustment | |||||
| Region of birth and (for those born in Denmark) maternal reference status | ||||||
| Unknown | 26 | 71 891 | 1.16 | (0.79-1.71) | 1.16 | (0.79-1.71) |
| Europe | 178 | 264 640 | 2.24 | (1.93-2.60) | 2.22 | (1.88-2.63) |
| Scandinavia | 106 | 178 484 | 2.00 | (1.65-2.42) | 1.98 | (1.58-2.47) |
| Asia | 74 | 120 799 | 2.27 | (1.80-2.85) | 2.24 | (1.75-2.88) |
| Middle East | 29 | 30 374 | 3.75 | (2.60-5.40) | 3.73 | (2.57-5.40) |
| Australia | 11 | 9047 | 4.15 | (2.30-7.50) | 4.09 | (2.22-7.54) |
| Africa | 41 | 37 419 | 3.85 | (2.83-5.23) | 3.81 | (2.76-5.26) |
| North America | 36 | 56 295 | 2.14 | (1.54-2.97) | 2.11 | (1.47-3.02) |
| South America | 15 | 20 122 | 2.55 | (1.54-4.24) | 2.54 | (1.51-4.24) |
| Greenland | 81 | 82 455 | 3.37 | (2.70-4.19) | 3.33 | (2.59-4.27) |
| Denmark, other | 537 | 2 569 082 | 0.74 | (0.67-0.81) | 0.74 | (0.67-0.81) |
| Denmark, second-generation immigrant | 426 | 743 485 | 1.92 | (1.74-2.12) | 1.92 | (1.74-2.12) |
| Denmark, Danish background | 8684 | 28 383 914 | 1.00 | 1.00 | ||
| P < 0.001 | P < 0.001 | |||||
| Maternal reference status for those born abroad | ||||||
| Possible adoption | 259 | 360 809 | 1.02 | (0.86-1.22) | 1.02 | (0.85-1.22) |
| Immigrant migrating without mother | 72 | 92 403 | 1.12 | (0.86-1.46) | 1.07 | (0.82-1.39) |
| Immigrant migrating with mother | 240 | 346 423 | 1.00 | 1.00 | ||
| P=0.32 | P=0.35 | |||||
Among those born in Denmark, the relative risk of developing schizophrenia differed significantly according to maternal reference status (P<0.001), with an increased relative risk found among second-generation immigrants (Table 2). The increased risk among second-generation immigrants was modified by parental history of psychiatric disorder (P=0.001). In second-generation immigrants with a history of psychiatric disorder in a parent, the relative risk of developing schizophrenia was 1.42 (95% CI 1.20-1.68) compared with Danes with a history of psychiatric disorder in a parent, and in second-generation immigrants with no history of psychiatric disorder in a parent, the relative risk was 2.09 (95% CI 1.85-2.35) compared with Danes with no history of psychiatric disorder in a parent. The effect of second-generation immigrant status was confounded only slightly when adjusting for history of psychiatric disorder in a parent.
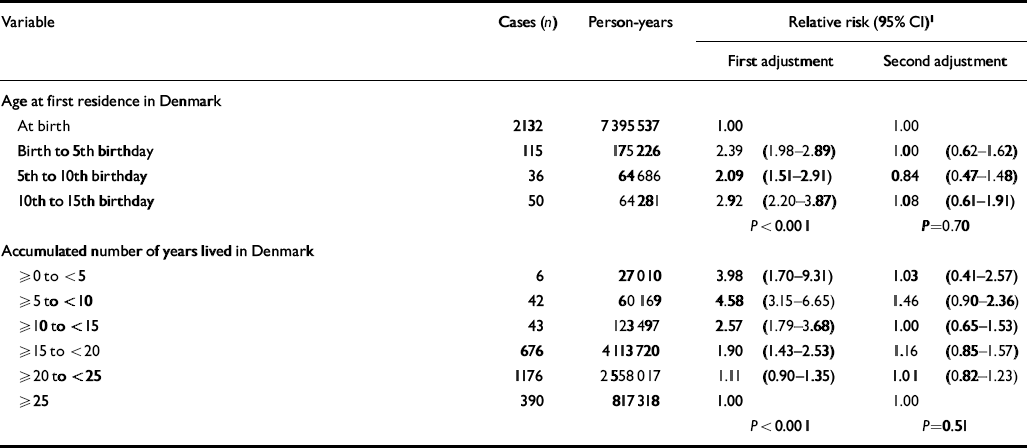
Age at first residence in Denmark and the accumulated number of years lived in Denmark (for those born in 1969 or later) had no effect on the relative risk of developing schizophrenia, after adjustment for region of birth and maternal reference status for those born in Denmark (Table 3). Conversely, the effects of region of birth and maternal reference status among those born in Denmark remained strongly significant (P<0.001), and were not confounded by age at first residence and accumulated number of years of residence in Denmark (results not shown). Age at first residence and the accumulated years of residence in Denmark were thus proxy variables for foreign birth, as the effect of these variables disappeared when the results were also simultaneously adjusted for region of birth and maternal reference status (second adjustment, P=0.70 and P=0.51 respectively).
Table 3 Distribution of 2333 cases of schizophrenia, 7.7 million person-years at risk, and estimates of relative risk according to age at first residence in Denmark and the accumulated number of years lived in Denmark among people born in 1969 or later
| Variable | Cases (n) | Person-years | Relative risk (95% CI)1 | |||
|---|---|---|---|---|---|---|
| First adjustment | Second adjustment | |||||
| Age at first residence in Denmark | ||||||
| At birth | 2132 | 7 395 537 | 1.00 | 1.00 | ||
| Birth to 5th birthday | 115 | 175 226 | 2.39 | (1.98-2.89) | 1.00 | (0.62-1.62) |
| 5th to 10th birthday | 36 | 64 686 | 2.09 | (1.51-2.91) | 0.84 | (0.47-1.48) |
| 10th to 15th birthday | 50 | 64 281 | 2.92 | (2.20-3.87) | 1.08 | (0.61-1.91) |
| P < 0.001 | P=0.70 | |||||
| Accumulated number of years lived in Denmark | ||||||
| ≥ 0 to <5 | 6 | 27 0 10 | 3.98 | (1.70-9.31) | 1.03 | (0.41-2.57) |
| ≥ 5 to <10 | 42 | 60 169 | 4.58 | (3.15-6.65) | 1.46 | (0.90-2.36) |
| ≥ 10 to <15 | 43 | 123 497 | 2.57 | (1.79-3.68) | 1.00 | (0.65-1.53) |
| ≥ 15 to <20 | 676 | 4 113 720 | 1.90 | (1.43-2.53) | 1.16 | (0.85-1.57) |
| ≥ 20 to <25 | 1176 | 2 558 017 | 1.11 | (0.90-1.35) | 1.01 | (0.82-1.23) |
| ≥ 25 | 390 | 817 318 | 1.00 | 1.00 | ||
| P < 0.001 | P=0.51 | |||||
There was no evidence that age at illness onset was modified by region of birth or, for those born in Denmark, by maternal reference status (P=0.36). Furthermore, the age category with the highest risk was age 22-23 years within all groups, thus indicating that illness onset occurs no earlier or later among first- or second-generation immigrants than among people with a Danish background.
Individual with Danish background (i.e. born in Denmark with mothers born in Denmark) and with a history of foreign residence prior to their fifteenth birthday had an increased relative risk of schizophrenia compared with those with Danish background but no such history (Table 4). The effect of history of foreign residence was not modified by age at foreign residence (P=0.36) or by history of parental psychiatric disorder (P=0.82), and was not confounded by history of parental psychiatric disorder.
Table 4 History of foreign residence among people with Danish background born in 1969 or later

| Variable1 | Cases (n) | Person-years | Relative risk (95% CI)2 | |
|---|---|---|---|---|
| No history | 1928 | 6 971 179 | 1.00 | |
| History | 66 | 148 714 | 1.60 | (1.25-2.05) |
| P < 0.001 | ||||
DISCUSSION
Main findings
Foreign birth and foreign background (i.e. second-generation immigrant status) were found to be risk factors for the development of schizophrenia in this population-based cohort of persons residing in Denmark by their fifteenth birthday. Notably, an increased risk of developing schizophrenia also was found among people with a Danish background who had a history of foreign residence prior to their fifteenth birthday.
Limitations
Although the use of register-based diagnostic information may represent a possible methodological limitation, the Danish Psychiatric Central Register has shown good diagnostic validity (Reference Munk-J⊘rgensenMunk-Jørgensen, 1995). Although the findings are based on patients admitted to hospital or in outpatient care, and this may overlook some early episodes of schizophrenia, most of these will eventually present for treatment and be registered. However, although the sample is large and representative, the level of demographic detail may be limited for certain categories; thus, foreign birth is an imprecise designation of ethnic background. Also, it was not possible to further subdivide the category represented by possible adoptees, and some of these individuals may be people born to Danish mothers living abroad.
Migration or ethnicity?
Although we cannot precisely identify the ethnicity of the foreign-born members of our cohort, the results of this study nevertheless have implications for the debate about the excessively high rates of schizophrenia found in people of African—Caribbean origin in the UK (Reference King, Coker and LeaveyKing et al, 1994; Reference Murray, Hutchinson, Gattaz and HäfnerMurray & Hutchinson, 1999; Reference Sharpley, Hutchinson and McKenzieSharpley et al, 2001). Efforts to explain this particular group's vulnerability in terms of ethnicity have been questioned (e.g. Reference Harrison, Glazebrook and BrewinHarrison et al, 1997). Our findings confirm the need for a broader focus on migration in general, and suggest furthermore that mixed migrant populations are potentially informative, despite the obvious difficulties posed by selection factors. The impact of selection bias in mixed migrant samples is aptly illustrated by the difference between the current findings and those from our previous study, in which immigrants from Denmark's neighbouring countries primarily accounted for the increased risk of schizophrenia found among immigrants (Reference Mortensen, Cantor-Graae and McNeilMortensen et al, 1997). It is important to note that in this current, more-restricted cohort — i.e. those residing in Denmark prior to their fifteenth birthday — the increased risk of schizophrenia found among immigrants cannot be ‘explained’ by people migrating during the early stages of their illness. Although we cannot exclude the effects of selective migration operating on the parents of these individuals, it should be observed that the risk associated with second-generation immigrant status was actually lower in second-generation immigrants with a parental history of psychiatric disorder than in those without a parental history of psychiatric disorder.
The results concerning region of birth show subtle but significant variation in risk magnitude across regions, although the pattern of results yields no obvious clues to possible explanatory mechanisms. Thus, for example, the countries of birth represented by regions at the higher end of the risk spectrum (e.g. Australia, Africa, the Middle East, Greenland) have seemingly little in common in terms of geography, climate, level of human development, or difficulties encountered upon arrival in Denmark. The findings concerning immigrants from Greenland may represent an interesting parallel to findings concerning immigrants to Europe from other former colonial regions (Reference Harrison, Glazebrook and BrewinHarrison et al, 1997; Selten et al, Reference Selten, Slaets and Kahn1997, Reference Selten, Veen and Feller2001), namely the Caribbean islands and Surinam. Although information on ethnicity is lacking, most of those born in Greenland are of Inuit extraction.
Recent theorising suggests that adverse social circumstances and ethnic minority disadvantage (Reference Sharpley, Hutchinson and McKenzieSharpley et al, 2001) may have an aetiological role in the ‘migrant’ effect in schizophrenia. Such factors might explain the increased risk of schizophrenia found among second-generation immigrants in this relatively young Danish cohort, and perhaps also some of the subtle regional variation found among first-generation immigrants. Nevertheless, the absence of an effect of age at first residence or duration of residence in Denmark may seem contradictory to the notion of minority-group disadvantage, unless one posits such adversity to be present regardless of how long one has lived in Denmark. It is also possible that the lack of greater regional differences with regard to the relative risks obtained among first-generation immigrants may represent a pattern in and of itself. That is, for people arriving in Denmark before the age of 15 years the experience of being uprooted might be similar regardless of country of origin. Alternatively, the experience of minority-group disadvantage during late puberty (after the age of 15 years) might be more important than specific ethnic identity. As the experience of minority disadvantage could vary according to social class and education, it is possible that further investigation of such factors might be informative for the pattern of regional differences obtained.
Perhaps the most surprising results in the current study are those implicating history of foreign residence as a risk factor for schizophrenia. Thus, migration per se might be a more important component in the ‘migrant’ effect than ethnicity, even when ethnicity is broadly defined (i.e. foreign birth or foreign background). A previous population-based Danish register study found an increased risk of schizophrenia in people born abroad to Danish-born mothers (Reference Mortensen, Pedersen and WestergaardMortensen et al, 1999). In contrast, the current results concern persons who are born in Denmark to Danish-born mothers and who subsequently emigrate and then return to Denmark again. Whatever risk factor may be involved in this process, it is not attributable to birth in a foreign region, to foreign background in one's maternal parentage, or to psychiatric disorder in a parent. A recent study of urban upbringing showed a cumulative risk with each move internally within Denmark and with increasing degree of urbanisation (Reference Pedersen and MortensenPedersen & Mortensen, 2001b ). These parallels notwithstanding, the current risk associated with history of foreign residence is seemingly unaffected by the age at which such residence occurs, whereas the findings of Pedersen & Mortensen (Reference Pedersen and Mortensen2001b ) indicate that the older the age of residential mobility within Denmark, the greater the risk.
As this study primarily concerns people resident in Denmark by their fifteenth birthday, we make no inferences about the risk of schizophrenia in immigrants in general, or in immigrants arriving in Denmark at a later age. However, although the results may not be applicable to all immigrants living in Denmark, it may not be possible to minimise selection bias and simultaneously be able to make inferences about the immigrant population at large. Paradoxically, the information obtained from a sample that might be more representative of immigrants in general would also be more compromised in terms of selection bias, as well as the correctness of the information regarding first-in-lifetime admission for the disorder.
Finally, although we have regarded people with first- and second-generation immigrant status as sharing a ‘commonality’ of migration background, it remains entirely unknown whether a common risk mechanism is indeed involved, and whether such a mechanism is also relevant to history of foreign residence. However, it may be worthwhile to note the lack of differences found concerning age of onset, suggesting that schizophrenia is unaffected by region of birth or background. Our study suggests a need for new hypotheses and for further investigations concerning the nature of the relationship between migration and schizophrenia.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ First- and second-generation immigrants residing in Denmark have an increased risk of schizophrenia that is not attributable to the migration of individuals during the early stages of their illness.
-
▪ First-generation immigrants have an increased risk of schizophrenia that is unlikely to be due to the difficulties encountered upon arrival in Denmark.
-
▪ Migration may confer an increased risk of schizophrenia that is independent of foreign birth or foreign background.
LIMITATIONS
-
▪ Country of birth is an imprecise designation of a person's background, i.e. ethnicity, social class or culture.
-
▪ The category represented by foreign-born possible adoptees might contain individuals who were born abroad to Danish mothers.
-
▪ The findings may not be applicable to immigrants arriving in Denmark after the age of 15 years.
Acknowledgements
The study was supported by the Stanley Medical Research Institute. The National Centre for Register-Based Research is funded by the Danish National Research Foundation.









eLetters
No eLetters have been published for this article.