About 30% of people with a diagnosis of schizophrenia continue to experience psychotic symptoms such as hallucinations and delusions despite treatment with antipsychotic medication (Reference KaneKane, 1996). Current application of cognitive—behavioural therapy aims to help sufferers understand and manage their experience of psychosis in ways that reduce distress and interference with functioning. Meta-analytical reviews support the potential efficacy of cognitive—behavioural therapy for schizophrenia but suggest that evidence for its effectiveness in routine clinical practice is limited (Reference Cormac, Jones and CampbellCormac et al, 2002; Reference Pilling, Bebbington and KuipersPilling et al, 2002). In this paper we report a comparison of cognitive—behavioural therapy, delivered by clinical nurse specialists, with two control conditions: treatment as usual and an analytically based supportive psychotherapy condition delivered by staff in a community mental health team. Recent clinical trials of cognitive—behavioural therapy for psychosis have either not controlled for therapist contact time (Reference Kuipers, Garety and FowlerKuipers et al, 1997; Reference Turkington, Kingdon and TurnerTurkington et al, 2002) or have controlled for it but with the same therapists delivering both treatments (Reference Tarrier, Yusupoff and KinneyTarrier et al, 1998; Reference Sensky, Turkington and KingdonSensky et al, 2000).
METHOD
Overview of recruitment and procedure
This study was conducted at two adjacent mental health services in Tayside and Fife (Scotland) covering a broad mix of urban and rural communities with a total catchment area of about 500 000 people. Patients were recruited by soliciting referrals from psychiatrists and psychiatric nurses working in community mental health teams, in-patient services and community care facilities. Selection criteria were as follows: patients with psychosis and a diagnosis of schizophrenia, schizo-affective disorder or delusional disorder, aged 16-65 years who are known to the psychiatric services as suffering from positive symptoms of persistent and distressing hallucinations or delusions, or both, and who have been stabilised on anti-psychotic medication for at least a 6-month period under the care of a consultant psychiatrist. Exclusion criteria were: primary diagnosis of alcoholism or drug misuse, evidence of organic brain disease and history of violence. All aspects of recruitment, screening and outcome assessment were organised and administered by an experienced psychiatrist (M.G.) over a 4-year period between January 1997 and March 2001. She had some assistance in these tasks during the latter phase of the study from an experienced community psychiatric nurse, who was trained in assessment procedures and was closely supervised.
All referrals were offered an appointment for a screening interview to establish diagnosis (using both ICD—10 (World Health Organization, 1992) and DSM-IV (American Psychiatric Association, 1994) criteria), to determine if selection criteria were met and to obtain consent. Suitable patients who consented were given further structured assessments as detailed below and included in the baseline phase of the study. They were then offered a further assessment interview 3 months later to reassess selection criteria and willingness to participate. The second screening interview was included in order to ensure stability of symptoms and as an added check on suitability for inclusion in the trial. Participants who met the criteria on both occasions were then randomised to one of three treatment conditions (cognitive—behavioural therapy plus treatment as usual — CBT; supportive psychotherapy plus treatment as usual — SPT; treatment as usual — TAU) and entered a 9-month treatment phase. They were then reassessed at the end of treatment and at a 3-month follow-up.
The randomisation procedure (sealed envelope technique) was devised by the project statistician (Cathy Hau) and administered centrally by the non-clinical project coordinator (Jen Petrie). It was carried out separately within each treatment centre using randomised permuted blocking (Reference Johnson, Freeman and TyrerJohnson, 1992). Power calculations were based on the expectation of a reasonably large effect size as found at post-treatment in a clinical trial comparing a coping skills enhancement condition and a problem-solving control (Reference Tarrier, Beckett and HarwoodTarrier et al, 1993). This was the closest example of relevant research when the project was planned. Cohen (Reference Cohen1992) states that having 21 patients in each group gives an 80% power of detecting a large effect size with a two-tailed significance level of 0.05. In retrospect this power calculation was not well founded because large treatment effects have not been reported generally in subsequent clinical trials. On the assumption that about two-thirds of screened patients would consent and be suitable and that about two-thirds of this number would complete, it was calculated that about 150 patients would need to be screened. In fact, these assumptions proved to be unrealistic and only about one-fifth of referrals ended up completing treatment.
Assessments
A broad range of measures were administered as part of structured interviews at initial screening, second screening, post-treatment and 3-month follow-up. Organisation and administration of the work of the independent assessors and therapists were kept strictly separate in order to maintain the blindness of the assessor. Patients also were asked not to mention any details of their treatment during post-treatment assessments, but three patients did. The primary outcome measures were chosen following perusal of the literature on assessment of psychosis (e.g. Reference Barnes and NelsonBarnes & Nelson, 1994) and consultation with clinical research teams experienced in the field. They consisted of standardised assessments of the severity of psychotic symptomatology in general, and delusions and hallucinations in particular. The former was assessed with the Positive and Negative Syndrome Scale (PANSS; Reference Kay, Fiszbein and OplerKay et al, 1987), which has been used frequently in clinical trials with psychosis and is recommended in reviews (e.g. Reference Drake, Haddock, Hopkins, Wykes, Tarrier and LewisDrake et al, 1998). There are three sub-scales (positive symptoms, negative symptoms and general psychopathology) and a total score. The Psychotic Symptom Rating Scale (PSYRATS; Reference Haddock, McCarron and TarrierHaddock et al, 1999) was used to assess specific dimensions of hallucinations and delusions. The hallucination sub-scale consists of items such as frequency, duration, loudness, negative content, intensity of distress and degree of disruption. The delusion sub-scale consists of items such as amount of pre-occupation, degree of conviction, intensity of distress and disruption. Both of these instruments have good internal reliability and validity and provide a comprehensive and clinically useful picture of current mental state that should be sensitive to treatment effects. At the end of the structured interview the assessor completed the Global Assessment Scale (GAS; Reference Endicott, Spitzer and FleissEndicott et al, 1976) and also Clinical Global Improvement (Reference GuyGuy, 1976) in terms of seven categories (marked, moderate or mild deterioration, no change, mild, moderate or marked improvement). Other self-report measures were administered to assess symptom severity, self-esteem and attitude to illness, but these are not central to the main research question and are omitted from this report.
Attitude to treatment was assessed at two time points. At the beginning and middle of therapy patients receiving either of the two psychological therapies were asked to rate the quality of the therapeutic alliance, using the Penn Helping Alliance Questionnaire (Reference Luborsky, Barber and SiquelandLuborsky et al, 1996), to assess their degree of improvement in terms of seven categories (much worse, moderately worse, a bit worse, unchanged, a bit better, moderately better and a lot better) and to rate the suitability of treatment and the degree to which they were learning new ways of coping. These last two measures were on 0-8 Likert scales. These data were collected on those patients receiving therapy who were given the forms to complete and managed to return them (68% in CBT, 63% in SPT). Some bias in the sample may be present. Finally, at the end of the follow-up interview, once all assessments had been completed, patients from all three treatment conditions were administered a brief semi-structured interview to assess the perceived helpfulness of treatment over the course of the trial and the quality of their relationship with their therapist/key worker. The blindness of the independent assessor was broken at this point. As a check on blindness the assessor was asked to guess treatment allocation after the final outcome assessments were completed. Analysis of these guesses found that they were no better than chance (χ2=5.63, d.f.=2, NS).
Treatment conditions
Overview
Participants in all three conditions received the usual care provided by the psychiatric services in Tayside and Fife. Services are well developed in these two areas, with a focus on community care delivered by community mental health teams. Services include regular psychiatric consultation and contact with a key worker (typically a trained community psychiatric nurse), with emergency assessment and hospital admission available as required. Facilities in the community include day care, sheltered work, supported accommodation and volunteer befriending. Specialist psychological intervention for psychosis within a cognitive—behavioural framework, although a limited resource, is offered through clinical psychology and clinical nurse specialists.
All but one of the therapists in the trial saw patients as part of their routine clinical work and it was not possible to follow a rigid protocol in respect of the duration, frequency and location of individual sessions. These aspects of the protocol were kept flexible so as to accommodate the varied needs of individual patients and therapists. The overall aim was to give each patient a maximum of 20 therapy sessions of approximately half an hour in length over a 9-month period. This level of intensity of therapy was the best that could be managed within the constraints of patient concentration and therapist workload.
Therapists
The CBT arm of the trial was delivered by five clinical nurse specialists with extensive professional experience of severe mental disorder. All had completed a recognised post-registration training in Dundee that mainly focuses on standard cognitive—behavioural therapy for common mental disorders but includes a module on psychosis. All were registered as therapists with the British Association of Behavioural and Cognitive Psychotherapy. One of these five (R.V.M.) had developed a specialist interest in cognitive—behavioural therapy for psychosis over several years and took the lead role in developing the treatment protocol, training and supervising the other therapists and treating the majority of patients. He was employed part-time on the research grant. None of the CBT therapists saw patients in the supportive psychotherapy arm of the trial, which was delivered by 16 mental health professionals (mainly nursing but also psychiatry and occupational therapy) who were attached to the clinical teams responsible for the patients referred to the trial and each saw one or two patients as part of their routine clinical work. All had expressed an interest in developing clinical skills in psychotherapy for patients with psychosis and none had received any formal training in cognitive—behavioural therapy. They were given training and supervision by a consultant psychotherapist (L.R.T.), who has consultant responsibility for one of the day hospitals in Dundee and is director of psychotherapy training in Tayside. She took responsibility for developing the supportive psychotherapy protocol and for training and supervising the therapists. All therapists in both treatment conditions were offered bi-weekly supervision for the duration of their contact with patients in the trial, and most participated on a regular basis.
Cognitive—behavioural therapy
The treatment protocol in the CBT condition drew on best practice as exemplified by the treatment manuals of Tarrier (Reference Tarrier, Birchwood and Tarrier1992) and Kingdon & Turkington (Reference Kingdon and Turkington1994). It was strongly influenced by training workshops in cognitive—behavioural therapy for psychosis delivered in Dundee by Tarrier & Turkington. The essential elements were as follows: initial emphasis on engagement, education and building a therapeutic alliance; functional analysis of key symptoms, leading to a formulation and problem list; development of a normalising rationale for the patient's psychotic experiences; exploration and enhancement of current coping strategies; acquisition of additional coping strategies for hallucinations and delusions; and focus on accompanying affective symptomatology using relaxation training, personal effectiveness training and problem-solving as appropriate. The overall aims were: to enhance knowledge and acceptance of illness; to encourage the acquisition of specific coping skills for managing hallucinations and delusions; and to develop an understanding of personal vulnerability and how to mitigate its effects.
Supportive psychotherapy
The treatment protocol in the SPT condition was developed by L.R.T. using the framework described by Garfield in his book Unbearable Affect: A Guide to the Psychotherapy of Psychosis (Reference GarfieldGarfield, 1995). This book provides therapists with vivid case histories and concrete illustrations of therapeutic strategies that give a sense of understanding the nature of psychotic experience and the ways in which talking through these experiences can bring some measure of relief and perspective. The approach is psychodynamic in orientation (cf. Reference De JongheDe Jonghe, 1993) and seeks to understand psychotic experience as a function of being overwhelmed and unable to bear intensely charged emotional experiences. The essential elements of therapy were as follows: provision of a safe and supportive atmosphere in which to raise issues of emotional importance to the patients, with an emphasis on the non-specific factors of warmth, empathy and genuineness; opportunity for the patients to describe the narrative of their lives, including the impact of the illness, so that they can be helped to make sense of the timing of the illness and its nature and content with reference to strong and ‘unbearable’ affect regarding past aspects of personal history; and description and working through of the transference as a process through which an individual transfers onto the analyst and others, past experiences, attitudes and feelings that he or she used to experience in relation to important figures earlier in life (Reference Bateman and HolmesBateman & Holmes, 1995).
Treatment adherence and quality
Treatment protocols in the CBT and SPT conditions required audiotaping of a random selection of early, middle and late sessions. Sessions to be taped were indicated in advance and therapists were encouraged to seek consent for recording at the beginning of treatment. In practice, tapes were not obtained from a sizeable minority of participants (38% in CBT and 35% in SPT), because either consent was refused or the therapist did not feel comfortable asking for consent from a particular patient (e.g. owing to intense paranoia), or because the quality of the recording was too poor to be usable. In total, 65 audiotapes were obtained and coded so as to conceal the therapist's identity. Transcripts of these tapes were made and a representative sample of 45 transcripts of sessions from 23 patients were sent to an independent assessor, D.F., who used the Cognitive Therapy Scale (Reference Vallis, Show and DobsonVallis et al, 1986) and the Cognitive Therapy for Psychosis Adherence Scale (Reference Startup, Jackson and PearceStartup et al, 2002) to examine treatment integrity and quality. Items that were core to both treatments were identified and additional items were included to measure key components of supportive psychotherapy. The same assessment scales were used for all transcripts and tapes.
Transcripts were necessary in order to take account of the different therapists providing treatment in the two conditions. Once the transcripts were assessed for integrity, tapes were provided to assist in the assessment of quality. It was concluded that: the two psychological therapy conditions were clearly distinct, with correct identification of therapy allocation made in 22/23 cases; adequate levels of nonspecific therapy ingredients were present in both conditions, with frequently good levels of interpersonal skill; CBT sessions all involved specific, cognitive—behavioural techniques and received competent ratings on the Cognitive Therapy Scale (Reference Vallis, Show and DobsonVallis et al, 1986). It was also noted that only half of the SPT sessions were rated as having involved a specific psychodynamic approach. Four of thirteen CBT sessions were rated as adherent using the Cognitive Therapy for Psychosis Adherence Scale (Reference Startup, Jackson and PearceStartup et al, 2002). This suggests that relatively few sessions included specific cognitive—behavioural therapy for psychosis techniques of the kind advocated in the Fowler et al (Reference Fowler, Garety and Kuipers1995) treatment manual. This analysis represents one of the first investigations of the nature and quality of cognitive—behavioural therapy delivered in a clinical trial with psychosis patients and points to the existence of different approaches to providing such therapy for this population.
Patient characteristics
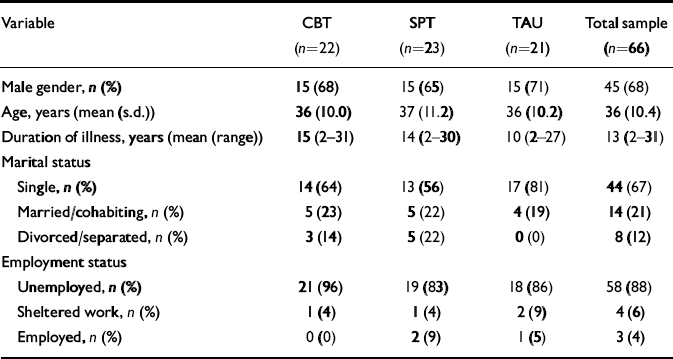
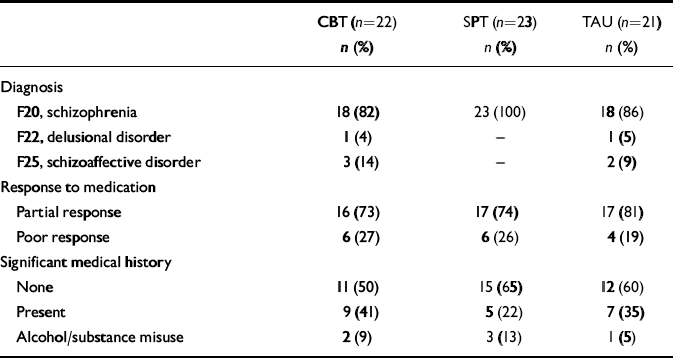
Basic demographic characteristics of the participants are presented in Table 1. In common with other trials of this kind (e.g. Reference Kuipers, Garety and FowlerKuipers et al, 1997) the sample consisted mainly of middle-aged, single, unemployed men with a long history of illness. There were no significant differences in these characteristics across the three treatment groups. The participants as a whole were poorly educated, with 90% having left school at age 16 years or less. At the time of initial referral 85% were living in the community and 15% were in-patients in a psychiatric hospital. Of the 56 participants living in the community, 30 (54%) lived with friends or relatives, 17 (30%) lived alone and the remainder were in supported accommodation. A summary of the diagnostic and clinical status of participants is presented in Table 2.
Table 1 Demographic data on participants who entered the trial
| Variable | CBT (n=22) | SPT (n=23) | TAU (n=21) | Total sample (n=66) |
|---|---|---|---|---|
| Male gender, n (%) | 15 (68) | 15 (65) | 15 (71) | 45 (68) |
| Age, years (mean (s.d.)) | 36 (10.0) | 37 (11.2) | 36 (10.2) | 36 (10.4) |
| Duration of illness, years (mean (range)) | 15 (2-31) | 14 (2-30) | 10 (2-27) | 13 (2-31) |
| Marital status | ||||
| Single, n (%) | 14 (64) | 13 (56) | 17 (81) | 44 (67) |
| Married/cohabiting, n (%) | 5 (23) | 5 (22) | 4 (19) | 14 (21) |
| Divorced/separated, n (%) | 3 (14) | 5 (22) | 0 (0) | 8 (12) |
| Employment status | ||||
| Unemployed, n (%) | 21 (96) | 19 (83) | 18 (86) | 58 (88) |
| Sheltered work, n (%) | 1 (4) | 1 (4) | 2 (9) | 4 (6) |
| Employed, n (%) | 0 (0) | 2 (9) | 1 (5) | 3 (4) |
Table 2 Clinical status at initial screening
| CBT (n=22) n (%) | SPT (n=23) n (%) | TAU (n=21) n (%) | |
|---|---|---|---|
| Diagnosis | |||
| F20, schizophrenia | 18 (82) | 23 (100) | 18 (86) |
| F22, delusional disorder | 1 (4) | - | 1 (5) |
| F25, schizoaffective disorder | 3 (14) | - | 2 (9) |
| Response to medication | |||
| Partial response | 16 (73) | 17 (74) | 17 (81) |
| Poor response | 6 (27) | 6 (26) | 4 (19) |
| Significant medical history | |||
| None | 11 (50) | 15 (65) | 12 (60) |
| Present | 9 (41) | 5 (22) | 7 (35) |
| Alcohol/substance misuse | 2 (9) | 3 (13) | 1 (5) |
Recruitment and attrition
A total of 274 people were referred for possible inclusion in the trial, of whom 95 (35% of initial referrals) fulfilled the initial criteria, entered the baseline assessment phase and were offered a further screening interview 3 months later. Of these, 66 (24% of initial referrals, 38% of 171 potentially suitable referrals) entered the study and were randomised to treatment conditions. Progress through these stages is shown in a CONSORT diagram (see Fig. 1).

Fig. 1 CONSORT diagram (CBT, cognitive—behavioural therapy plus treatment as usual; SPT, supportive psychotherapy plus treatment as usual; TAU, treatment as usual).
Medication
Antipsychotic drug dosages over the course of the trial were available for 22 patients in CBT (100%), 19 in SPT (83%) and 18 in the TAU condition (86%). They were converted to mean daily equivalents of chlorpromazine using standard guidelines (Reference Atkins, Burgess and Bottom leyAtkins et al, 1997) and are summarised in Table 3. The very broad confidence intervals reflect the wide variation in dosages within and between treatment conditions and none of the differences is significant. The increases in dosage post-treatment were a result of increasing use of atypical antipsychotics. Four of the fifteen patients who were started on an atypical were prescribed clozapine. No relationship was found between outcome and commencement of atypical antipsychotics. In order to assess whether or not outcome could be attributed to changes in medication, following randomisation the sample was grouped according to dose change (increased, unchanged, decreased) and an analysis of variance was conducted on difference scores on the primary outcome measure (total PANSS score) from baseline to post-treatment and baseline to follow-up. No significant differences were found at either post-treatment (F (2,55)=0.63, P=0.54) or follow-up (F (2,52)=1.51, P=0.23). The largest decreases in symptom severity were associated with reductions in medication dose.
Table 3 Changes in prescribed antipsychotic drugs

| CBT (n=22) | SPT (n=19) | TAU (n=18) | |
|---|---|---|---|
| Chlorpromazine equivalents, mg/day (mean (95% CI)) | |||
| 1st screening | 691 (441-942) | 711 (522-901) | 575 (302-849) |
| 2nd screening | 604 (392-816) | 747 (527-967) | 630 (333-927) |
| Post-treatment | 833 (512-1155) | 1021 (542-1501) | 865 (303-1427) |
| Follow-up | 627 (371-882) | 961 (486-1437) | 911 (343-1478) |
| Patients changing total antipsychotic drug doses at follow-up evaluation, n (%) | |||
| Reduced | 12 (54) | 7 (37) | 3 (17) |
| Increased | 6 (27) | 7 (37) | 7 (39) |
| Patients changing atypical antipsychotic drug prescription at follow-up evaluation, n (%) | |||
| Discontinued | 1 (4) | 2 (10) | 0 (0) |
| No change | 6 (27) | 7 (37) | 7 (39) |
| Started during study | 6 (27) | 6 (32) | 3 (17) |
RESULTS
Statistical analysis
Comparative efficacy of treatment conditions on the main outcome measures (PANSS, PSYRATS, GAS) was analysed first in terms of changes in mean scores over time, using an average of the baseline scores for each patient as the pre-treatment measure. A second analysis examined the proportion of patients in each treatment condition who showed at least 25% and 50% decreases in symptom severity on the PANSS and PSYRATS at post-treatment and follow-up. Both figures were chosen in order to make meaningful comparisons with the three main clinical trials published in this area, one of which (Reference Kuipers, Garety and FowlerKuipers et al, 1997) used a measure of clinically significant change that broadly equates with the lower figure, whereas the other two (Reference Tarrier, Yusupoff and KinneyTarrier et al, 1998; Reference Sensky, Turkington and KingdonSensky et al, 2000) reported outcomes in terms of the higher figure. Although both figures are arbitrary, most clinicians with experience of chronic schizophrenia would probably regard a 25% improvement as being worthwhile and a 50% improvement as representing an important clinical change. Comparisons were made of the ratings of overall improvement across treatment conditions, from the perspective of both patient and assessor, and of the patient's overall attitude to treatment at follow-up and during therapy. All analyses reported were conducted on available data using SPSS version 10 for Windows. There was a relatively small amount of missing data at post-treatment (9%) and follow-up (14%). The analyses were repeated with the missing values replaced either with previous values carried forward or with group means, and the same pattern of significance was found.
Changes in severity from baseline
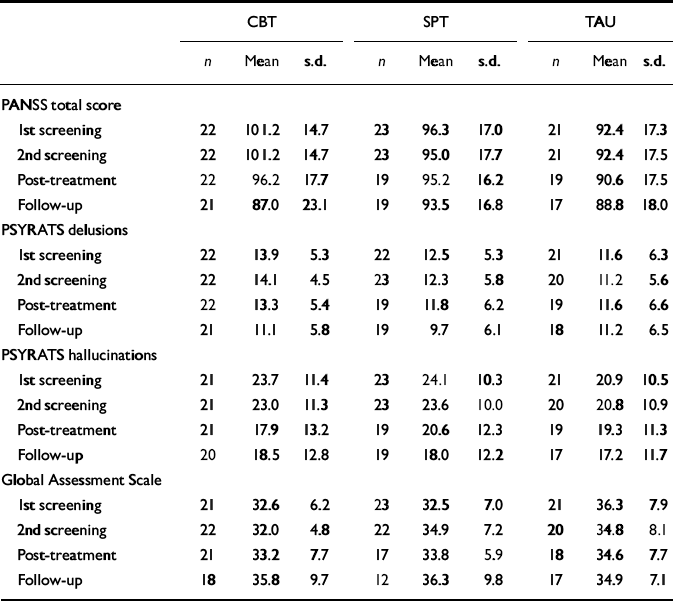
Mean scores across treatment conditions for the four main outcome measures are shown in Table 4. It can be seen that baseline scores are very stable for all measures across all three treatment conditions. An average of the baseline scores was used as the pre-treatment measure. Repeated measures analyses of variance were first conducted with three levels of treatment (CBT v. SPT v. TAU) and three time points (baseline, post-treatment, follow-up). There were significant effects for time for all variables except the GAS but no significant time × treatment interaction effects or contrasts for any of the measures. The analyses were repeated with two levels of treatment, first to provide a more powerful test of CBT effects against an aggregate of the two control conditions (CBT v. SPT and TAU) and, second, to test for the effects of receiving psychological therapy (CBT and SPT v. TAU). The first set of analyses replicated the initial analysis with the exception of the total PANSS score, where there was a significant time × treatment within-subject effect (F(2,106)=3.15, P=0.047). The linear effect of the time × treatment interaction was also significant (F(1,53)=4.14, P=0.047). The degree of overall improvement was greater in the CBT condition than in the other two conditions combined. The second set of analyses again replicated the initial analysis with the exception of the PSYRATS delusions score, where there was a non-significant effect of time (F(2,106)=2.79, P=0.06) but a significant time × treatment within-subject effect (F(2,106)=3.25, P=0.043). The linear effect of time × treatment interaction was also significant (F(1,53)=4.83, P=0.032). The degree of overall improvement in severity of delusions was significantly greater for those patients receiving psychological therapy (either CBT or SPT) than TAU.
Table 4 Mean scores (s.d.) on main outcome measures rated by independent assessor
| CBT | SPT | TAU | |||||||
|---|---|---|---|---|---|---|---|---|---|
| n | Mean | s.d. | n | Mean | s.d. | n | Mean | s.d. | |
| PANSS total score | |||||||||
| 1st screening | 22 | 101.2 | 14.7 | 23 | 96.3 | 17.0 | 21 | 92.4 | 17.3 |
| 2nd screening | 22 | 101.2 | 14.7 | 23 | 95.0 | 17.7 | 21 | 92.4 | 17.5 |
| Post-treatment | 22 | 96.2 | 17.7 | 19 | 95.2 | 16.2 | 19 | 90.6 | 17.5 |
| Follow-up | 21 | 87.0 | 23.1 | 19 | 93.5 | 16.8 | 17 | 88.8 | 18.0 |
| PSYRATS delusions | |||||||||
| 1st screening | 22 | 13.9 | 5.3 | 22 | 12.5 | 5.3 | 21 | 11.6 | 6.3 |
| 2nd screening | 22 | 14.1 | 4.5 | 23 | 12.3 | 5.8 | 20 | 11.2 | 5.6 |
| Post-treatment | 22 | 13.3 | 5.4 | 19 | 11.8 | 6.2 | 19 | 11.6 | 6.6 |
| Follow-up | 21 | 11.1 | 5.8 | 19 | 9.7 | 6.1 | 18 | 11.2 | 6.5 |
| PSYRATS hallucinations | |||||||||
| 1st screening | 21 | 23.7 | 11.4 | 23 | 24.1 | 10.3 | 21 | 20.9 | 10.5 |
| 2nd screening | 21 | 23.0 | 11.3 | 23 | 23.6 | 10.0 | 20 | 20.8 | 10.9 |
| Post-treatment | 21 | 17.9 | 13.2 | 19 | 20.6 | 12.3 | 19 | 19.3 | 11.3 |
| Follow-up | 20 | 18.5 | 12.8 | 19 | 18.0 | 12.2 | 17 | 17.2 | 11.7 |
| Global Assessment Scale | |||||||||
| 1st screening | 21 | 32.6 | 6.2 | 23 | 32.5 | 7.0 | 21 | 36.3 | 7.9 |
| 2nd screening | 22 | 32.0 | 4.8 | 22 | 34.9 | 7.2 | 20 | 34.8 | 8.1 |
| Post-treatment | 21 | 33.2 | 7.7 | 17 | 33.8 | 5.9 | 18 | 34.6 | 7.7 |
| Follow-up | 18 | 35.8 | 9.7 | 12 | 36.3 | 9.8 | 17 | 34.9 | 7.1 |
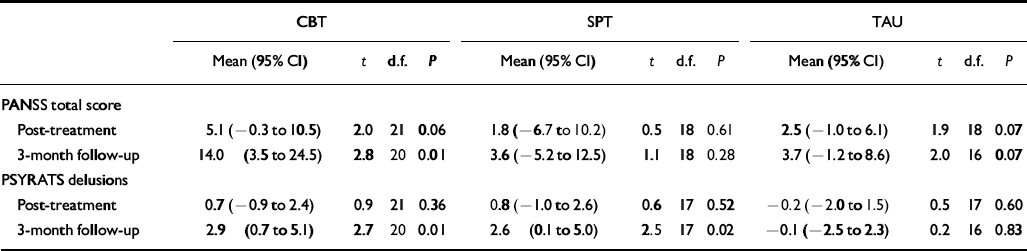
In order to test for the location and magnitude of change in the two outcome measures with significant time × treatment interactions (PANSS total score and PSYRATS delusions), difference scores were calculated between average baseline scores and post-treatment and follow-up scores. The significance of these differences was examined with paired t-tests and the results are summarised in Table 5. It can be seen that the one significant change on the PANSS total score occurs in the CBT condition at follow-up. The changes at post-treatment are generally much smaller and none is significant. Changes on the PSYRATS delusions sub-scale are of a similar magnitude in the CBT and SPT conditions, with small non-significant changes at post-treatment and larger, significant changes at follow-up. Corresponding changes in TAU are very small and non-significant at post-treatment and follow-up.
Table 5 Mean change (95% CI) from baseline at post-treatment and 3-month follow-up on outcome measures with significant overall treatment × time effects
| CBT | SPT | TAU | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean (95% CI) | t | d.f. | P | Mean (95% CI) | t | d.f. | P | Mean (95% CI) | t | d.f. | P | |
| PANSS total score | ||||||||||||
| Post-treatment | 5.1 (-0.3 to 10.5) | 2.0 | 21 | 0.06 | 1.8 (-6.7 to 10.2) | 0.5 | 18 | 0.61 | 2.5 (-1.0 to 6.1) | 1.9 | 18 | 0.07 |
| 3-month follow-up | 14.0 (3.5 to 24.5) | 2.8 | 20 | 0.01 | 3.6 (-5.2 to 12.5) | 1.1 | 18 | 0.28 | 3.7 (-1.2 to 8.6) | 2.0 | 16 | 0.07 |
| PSYRATS delusions | ||||||||||||
| Post-treatment | 0.7 (-0.9 to 2.4) | 0.9 | 21 | 0.36 | 0.8 (-1.0 to 2.6) | 0.6 | 17 | 0.52 | -0.2 (-2.0 to 1.5) | 0.5 | 17 | 0.60 |
| 3-month follow-up | 2.9 (0.7 to 5.1) | 2.7 | 20 | 0.01 | 2.6 (0.1 to 5.0) | 2.5 | 17 | 0.02 | -0.1 (-2.5 to 2.3) | 0.2 | 16 | 0.83 |
Clinically significant improvement
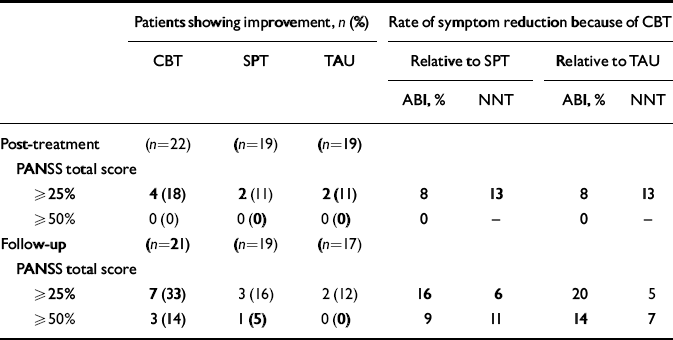
Table 6 summarises the proportion of patients in each treatment condition who showed 25% and 50% improvements on PANSS total scores. The right-hand part of the table shows the difference in these proportions for patients treated with CBT relative to those with either SPT or TAU, from which the ‘number needed to treat’ statistic can be calculated. At post-treatment it can be seen that no patients showed a 50% reduction and relatively small proportions (10-20%) showed a 25% reduction. Although twice as many patients in the CBT condition achieved a 25% improvement, the absolute numbers are small and the differences are not significant. Thus, the number of patients that would need to be treated with CBT in order to achieve a difference of this kind, relative to SPT and TAU, is 13, which is a relatively large number. At follow-up it can be seen that one-third of patients in CBT achieved a 25% reduction, which is more than twice the proportion for SPT and TAU combined, and the number of patients that would need to be treated with CBT in order to achieve a difference of this kind, relative to SPT and TAU, is now six and five, respectively. Only four patients in the study achieved a 50% decrease in overall symptomatology, three of whom were in the CBT condition.
Table 6 Proportion of patients showing greater than 25% and 50% improvement on PANSS total scores at post-treatment and follow-up with absolute benefit increase (ABI) and number needed to treat (NNT)
| Patients showing improvement, n (%) | Rate of symptom reduction because of CBT | ||||||
|---|---|---|---|---|---|---|---|
| CBT | SPT | TAU | Relative to SPT | Relative to TAU | |||
| ABI, % | NNT | ABI, % | NNT | ||||
| Post-treatment | (n=22) | (n=19) | (n=19) | ||||
| PANSS total score | |||||||
| ≥ 25% | 4 (18) | 2 (11) | 2 (11) | 8 | 13 | 8 | 13 |
| ≥ 50% | 0 (0) | 0 (0) | 0 (0) | 0 | - | 0 | - |
| Follow-up | (n=21) | (n=19) | (n=17) | ||||
| PANSS total score | |||||||
| ≥ 25% | 7 (33) | 3 (16) | 2 (12) | 16 | 6 | 20 | 5 |
| ≥ 50% | 3 (14) | 1 (5) | 0 (0) | 9 | 11 | 14 | 7 |
Patient and assessor ratings of overall improvement
Judgements of overall improvement over the course of the trial were made by the independent assessor at the 3-month follow-up. For the patients as a whole, 10% were rated as having some degree of deterioration, 40% as being unchanged and 50% as having improved to some degree. When broken down by treatment condition there was a trend for a greater proportion of patients in the CBT condition being rated as improved to some degree (63%) compared with SPT (36%) and TAU (50%), and also for a larger proportion of CBT patients (15%) to be rated as having deteriorated to some degree in comparison with SPT (6%) and TAU (6%) patients. Judgements of overall improvement made by patients at the 3-month follow-up were broadly similar, although a rather greater proportion rated themselves as being worse (18%), a rather smaller proportion as unchanged (19%) and a rather larger proportion as being better to some degree (64%). None of the differences between treatment conditions was significant.
Patient attitudes to treatment
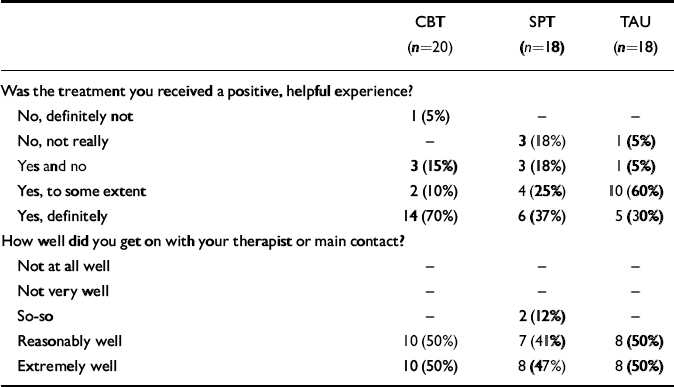
Table 7 summarises patient responses to two questions that were put to them by the independent assessor at the end of the 3-month follow-up interview. There was a broadly positive attitude to treatment across all three conditions but a significant tendency for patients receiving CBT to rate their experience as definitely positive and helpful in comparison with the other two groups (70% CBT, 37% SPT, 30% TAU; χ2=6.93, d.f.=2, P=0.031; CBT v. combined SPT and TAU, χ2=6.72, d.f.=1, P=0.01). This difference is not simply a result of patients in CBT getting on better with their therapist, as indicated by the responses to the second question, which asks about the therapeutic relationship. Responses to this question were broadly positive and almost identical across treatment conditions. It is worth noting in this context that virtually identical ratings were made of the quality of the therapeutic relationship when measured by a sub-scale of the Penn Helping Alliance during the early stage of therapy. This rating was completed by 15 patients in CBT and 12 patients in SPT on a 25-point scale with a minimum of 5 and a maximum of 30 (mean score CBT=25.1, s.d.=3.0, mean score SPT=25.7, s.d.=3.0).
Table 7 Patients' attitudes to treatment received over the course of the trial, assessed at 3-month follow-up
| CBT (n=20) | SPT (n=18) | TAU (n=18) | |
|---|---|---|---|
| Was the treatment you received a positive, helpful experience? | |||
| No, definitely not | 1 (5%) | - | - |
| No, not really | - | 3 (18%) | 1 (5%) |
| Yes and no | 3 (15%) | 3 (18%) | 1 (5%) |
| Yes, to some extent | 2 (10%) | 4 (25%) | 10 (60%) |
| Yes, definitely | 14 (70%) | 6 (37%) | 5 (30%) |
| How well did you get on with your therapist or main contact? | |||
| Not at all well | - | - | - |
| Not very well | - | - | - |
| So-so | - | 2 (12%) | - |
| Reasonably well | 10 (50%) | 7 (41%) | 8 (50%) |
| Extremely well | 10 (50%) | 8 (47%) | 8 (50%) |
Difference in perceived helpfulness of therapy may have been due to differences in ratings of perceived suitability of treatment made by patients in CBT (n=13) in comparison with patients in SPT (n=12). At the first administration of this rating (0-8 scale: 0, not at all suitable; 8, very suitable) there were no significant differences between treatments (mean score CBT=5.5, s.d.=2.1; mean score SPT=5.0, s.d.=2.0), but at the second administration, during the middle stage of therapy, mean ratings of suitability of treatment by patients in CBT were significantly higher than those by patients in SPT (CBT=6.6, s.d.=1.6; SPT=4.9, s.d.=2.1; t=2.27, d.f.=23, P=0.033). There was a similar (although non-significant) trend with regard to ratings of learning new ways of coping with problems and difficulties.
DISCUSSION
Summary of findings
The study provides evidence that cognitive—behavioural therapy in particular and psychological therapy in general give some additional benefit in overall symptom reduction when added to routine care. About one-third of patients in the CBT arm showed a 25% reduction in overall symptomatology. No evidence was found for treatment effects for auditory hallucinations but the CBT and SPT conditions combined produced significantly greater reductions in the severity of delusions than did TAU. Symptomatic improvement following psychological treatment was apparent at follow-up rather than at post-treatment, in line with the findings of a recent meta-analytical review (Reference Pilling, Bebbington and KuipersPilling et al, 2002), and was not associated with changes in overall functioning as assessed by the GAS. From a clinical perspective, the overall reductions in symptomatology were relatively modest but it should be noted that the severity of initial symptoms in the trial and the magnitude of change in the CBT condition, as measured by the PANSS, are comparable with the figures reported in a recent clinical trial of the efficacy of atypical neuroleptics in chronic schizophrenia (Reference Volavka, Czobor and SheitmanVolavka et al, 2002). Notwithstanding symptom change, satisfaction with treatment was generally positive across all three treatment conditions, and expressions of ‘definite satisfaction’ with treatment were significantly higher in the CBT condition (70%) than in SPT (37%) or TAU (2%). The quality of the therapeutic alliance was similar in CBT and SPT but ratings of the suitability of treatment were significantly higher in CBT.
Methodological issues
This clinical trial is one of the first investigations of the efficacy of cognitive—behavioural therapy for psychosis in which treatment was delivered as part of routine clinical practice. The following features have helped to ensure methodological rigour: a 3-month pre-treatment baseline, to ensure the stability of the presenting symptomatology; outcome evaluation with standardised measures by an independent assessor, an experienced psychiatrist, blind to treatment allocation at post-treatment and 3-month follow-up; a credible supportive psychotherapy condition carried out by separate therapists to control for the non-specific effects of CBT; a TAU condition to control for changes over time; an independent evaluation of adherence to psychological treatment protocols and of the quality of therapy delivered; and a research team drawn from nursing, psychiatry and clinical psychology with varying professional commitments to cognitive—behavioural therapy, psychodynamic therapy and biological psychiatry.
Methodological limitations include: lower than expected numbers in each treatment condition as a consequence of a higher than expected proportion of patients refusing to participate at the initial screening (44% of 171 suitable referrals); variable medication regimes between and within treatment conditions following baseline assessment, producing potential biases with the small sample sizes; and a potential confound of treatment condition with differences in therapist experience and expertise in delivering psychological therapy for patients with chronic psychosis. The advantage of CBT over SPT may be a function of the considerable experience and expertise in delivering psychological therapy with this population developed by clinical nurse specialists in cognitive—behavioural therapy over several years. In particular, the construction and presentation of a formulation — a potentially powerful intervention with this population — takes considerable practice. Therapists in the SPT arm were, on the whole, less experienced and found the role of therapist more challenging.
Comparison with other trials
Three other randomised controlled trials have been published that specifically test the efficacy of cognitive—behavioural therapy for chronic psychosis: the London—East Anglia study (Kuipers et al, Reference Kuipers, Garety and Fowler1997, Reference Kuipers, Fowler and Garety1998), the Manchester Wellcome study (Reference Tarrier, Yusupoff and KinneyTarrier et al, 1998) and the London—Newcastle Wellcome study (Reference Sensky, Turkington and KingdonSensky et al, 2000). In common with the present investigation, all three trials found evidence that cognitive—behavioural therapy was more effective than alternatives and associated with low drop-out rates and high patient satisfaction. However, the proportion of patients in cognitive—behavioural therapy judged to be treatment responders at follow-up was found to be 65% in the London—East Anglia study (based on 25% reductions in symptom severity), 33% in the Manchester Wellcome study (based on 50% reductions in symptom severity) and 63% in the London—Newcastle Wellcome study (also based on 50% reductions in symptom severity). Varying operational definitions of a clinically significant treatment response, as well as different measures, timescales and selection procedures, make direct comparisons across studies problematic but it would appear that all three of these trials found higher rates of treatment responders than the 33% found in the present study (based on 25% reductions in symptom severity).
Variable nature of cognitive—behavioural therapy for psychosis
One possible explanation for this apparent difference in outcome may lie in the type of treatment delivered. The analysis of treatment integrity and quality completed by D.F. found that the style of cognitive—behavioural therapy delivered was competent with respect to the standard treatment approach used but included few of the specific adaptations for psychosis advocated in the Fowler et al (Reference Fowler, Garety and Kuipers1995) treatment manual. The variations in practice within cognitive—behavioural therapy for psychosis raise the possibility that some approaches may be more effective than others, and this is an important area for future research. Cognitive—behavioural therapy is a demanding therapy with complex presentations (Reference Durham, Swan and FisherDurham et al, 2000) and there is much scope for better models and illustrations of good practice. Clinicians working with cognitive—behavioural therapy and psychosis do not have the benefit of a range of videotape material demonstrating therapeutic styles and techniques but instead have to work from treatment manuals containing general guidelines and brief transcripts. It is not an easy task to apply this knowledge to the wide variety of clinical presentations of psychosis and it is often hard to know how an ‘expert’ in the field might handle the difficulties that arise. On the other hand, the present study demonstrates that significant benefits in routine clinical practice can result from using standard approaches to cognitive—behavioural therapy for psychotic disorder and that the therapy can be of value even with therapists given relatively brief training (Reference Turkington, Kingdon and TurnerTurkington et al, 2002).
Whatever the explanation for the apparent discrepancy in outcomes between the present study and previous clinical trials, it will be important to conduct further studies in the field to clarify the relationship between the nature and quality of therapy delivered and clinically significant outcomes. The current debate on this issue tends to be polarised between those who believe that cognitive—behavioural therapy is clearly efficacious and those who seem sceptical of any incorporation of specialised psychological intervention into routine care. Our own view of the evidence is that people with chronic psychosis should be given the opportunity to engage in systematic psychological therapy on the grounds that most will find this of some value and a few will be able to use the opportunity to make a significantly better adjustment for the future.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Cognitive—behavioural therapy delivered by clinical nurse specialists gives modest but clinically significant improvements in severity of overall symptomatology in about one-third of patients with chronic psychosis who are willing to attend therapy sessions.
-
▪ Cognitive—behavioural therapy and supportive psychotherapy both give modest but significant improvements in the severity of delusions but there is no evidence for a psychological treatment effect for hallucinations.
-
▪ Treatment manuals for psychological therapy for chronic psychosis need to be supplemented by videotape demonstrations of therapy with representative samples of patients.
LIMITATIONS
-
▪ Forty-four per cent of 171 suitable referrals refused to participate, giving relatively small numbers in each treatment condition.
-
▪ Medication regimes between and within treatment conditions following baseline assessment were uncontrolled.
-
▪ Psychological treatment conditions were confounded, with differences in therapist expertise in psychological therapy with chronic psychosis.
Acknowledgements
The preparation of this article was made possible by a grant to R.C.D., R.V.M. and D.A.R. by the Chief Scientist Office, Scottish Home and Health Department, Edinburgh, whose financial support is gratefully acknowledged. Cathy Hau provided statistical advice in the early phase of the project and Susan Schooling provided research assistance during the later phase of the project. Jen Petrie coordinated all phases of the project with unfailing efficiency and good humour. We are grateful to Dr Andrew Reid, Consultant Psychiatrist, for his clinical support and encouragement and to all the therapists who took part.













eLetters
No eLetters have been published for this article.