Depersonalisation is an underreported and underresearched clinical phenomenon. The disorder was first described in the late-19th century (Reference Sierra and BerriosSierra & Berrios, 1998) and there have been several classic descriptions since then (Reference Shorvon, Hill and BurkittShorvon et al, 1946; Reference AcknerAckner, 1954). The reported prevalence of significant symptoms is 2.4-20% (Reference Ross, Joshi and CurrieRoss et al, 1990; Reference Kihlstrom, Gilsky and AngiuloKihlstrom et al, 1994; Reference Aderibigbe, Bloch and WalkerAderibigbe et al, 2001). Depersonalisation disorder is defined in the DSM—IV (American Psychiatric Association, 1994) as an ‘alteration in the perception or experience of the self so that one feels detached from and as if one is an outside observer of one's mental processes or body’. Derealisation is defined as an ‘alteration in perception or experience of the world so that it seems unreal’ (American Psychiatric Association, 1994). Both sets of symptoms can occur in the context of other psychiatric illnesses, particularly panic disorder (Reference Segui, Maruez and GarciaSegui et al, 2000) and depression (Reference SedmanSedman, 1966), but may be considered primary as long as they do not occur exclusively in this context. Depersonalisation also may be associated with neurological conditions (Reference Lambert, Sierra and PhillipsLambert et al, 2002; Reference Sierra, Lopera and LambertSierra et al, 2002a ), head injury (Reference Grigsby and KayeGrigsby & Kaye, 1993), illicit drug use (Reference McGuire, Cope and FahyMcGuire et al, 1994), ‘near death’ experiences (Reference Noyes and KlettiNoyes & Kletti, 1977) and post-traumatic stress disorder (Reference Mayou, Bryant and EhlersMayou et al, 2001). Depersonalisation disorder (severe depersonalisation associated with functional impairment) is classified with four essential criteria as one of the dissociative disorders in the DSM—IV (American Psychiatric Association, 1994) but as a neurotic condition in the ICD—10 (World Health Organization, 1992). Nevertheless, the two sets of criteria are remarkably similar, although explicit mention of impairment is not included in the ICD—10. There are no accepted treatments but many have been tried (Reference Simeon and HollanderSimeon & Hollander, 1993). The aetiology of depersonalisation is unknown but recent studies have pointed to neurocognitive (Reference Simeon, Gross and GuralnikSimeon et al, 1997; Reference Lambert, Senior and PhillipsLambert et al, 2001b ) and physiological abnormalities (Reference Phillips, Medford and SeniorPhillips et al, 2001a ; Reference Sierra, Senior and DaltonSierra et al, 2002b ). Early studies had the strength of rich clinical description. However, they were based on small case series and so lacked the necessary information needed to derive ‘typical’ features and demographic associations. A recent series of 30 cases published by Simeon et al (Reference Simeon, Gross and Guralnik1997) went some way to redressing this. We report a much larger series assessed in a UK clinic (Reference Phillips, Sierra and HunterPhillips et al, 2001b ). We analysed the group in terms of age of onset, gender, associated psychiatric and medical conditions, precipitating factors and course.
As well as describing the cohort, we sought to address two main questions:
-
(a) Are there identifiable clinical subtypes that might point to specific aetiological factors?
-
(b) Is there a meaningful distinction between primary and secondary depersonalisation?
METHOD
We carried out a questionnaire and interview survey of a cohort of consecutive eligible cases who made contact with a recently established depersonalisation disorder clinic based at the Maudsley Hospital, London.
Participants
A total of 204 people with a putative diagnosis of depersonalisation disorder seeking help or information were recruited via clinical referrals to the Depersonaliation Research Unit at the Institute of Psychiatry, London (n=130), and through the Unit's website (n=55), media announcements (n=14) and patient support organisations (n=5).
Assessments
Demographic details, along with medical and psychiatric history, were obtained from all participants. A detailed history of the nature and course of their depersonalisation was also obtained. A total of 124 referrals had a full psychiatric interview and assessment at the request of the individual and their referring clinician. The clinical assessment incorporated the Present State Examination (PSE; Reference Wing, Cooper and SartoriusWing et al, 1974). An additional 22 participants had a telephone interview using the key PSE items and the remaining 58 supplied detailed written information on a clinic form and by completing several questionnaires. The PSE includes items for depersonalisation and derealisation. To summarise definitions given in the glossary, for each item: 0=not present; 1=moderately intense or transient; and 2=intense and persistent. Our case definition required a total score of ≥2 without an obvious additional clinical diagnosis or prominent non-dissociative symptomatology. This has been shown previously to have good sensitivity and specificity when measured against a new and established self-report measure (see below) (Reference Lambert, Senior and PhillipsLambert et al, 2000). A final clinical diagnosis was made according to DSM—IV criteria, with the PSE items being used to help define the core symptoms of depersonalisation and derealisation.
Self-report questionnaires
The Beck Anxiety Inventory (BAI; Reference Beck, Epstein and BrownBeck et al, 1988a ) and the Beck Depression Inventory (BDI; Reference Beck, Steer and GarbinBeck et al, 1988b ) were used. A score of ≤10 on either scale is considered within the ‘normal’ range and a score of ≥30 above is ‘severe’.
The Dissociative Experiences Scale, version II (DES; Reference Bernstein and PutnamBernstein & Putnam, 1986; Reference Carlson and PutnamCarlson & Putnam, 1993), was also used. This is a 28-item self-report questionnaire with a cut-off score of 30 for severe dissociative disorders (Reference Carlson and PutnamCarlson & Putnam, 1993). Factor analysis shows this scale to have three main sub-scales: ‘depersonalisation/derealisation’ (DES—DP/DR); ‘amnesia’ for dissociative experiences (DES—Amnesia); and ‘absorption’ and imaginative involvement (DES—Absorption) (Reference Carlson, Putnam, Ross, Braun and CarlsonCarlson et al, 1991). Eight items make up the ‘taxon’ sub-scale (DES—Taxon) (Reference Simeon, Guralnik and GrossSimeon et al, 1998); this is sensitive to the detection of depersonalisation disorder, with a cut-off score of 13.
RESULTS
Demographic characteristics
The mean age of the 204 participants (112 males and 92 females) was 36.3 years, range 16-74 (Table 1). Around two-thirds were from the greater London area. Others came from the rest of the UK or mainland Europe (n=16), North America and Canada (n=15) and Australasia (n=3). Fifty-one per cent were single, 38% were cohabiting and 11% were separated/divorced/widowed. Fifty-four per cent had some form of higher education; 38% were not working or were unemployed.
Table 1 Mean (s.d.) age, age at onset and duration of depersonalisation disorder in all participants

| All participants (n=204) | Male (n=112) | Female (n=92) | |
|---|---|---|---|
| Age (years) | 36.3 (12.77) | 35.2 (11.59) | 37.5 (14.03) |
| Age at onset (years) | 22.8 (11.94) | 21.5 (9.67) | 24.3 (14.14) |
| Duration (years) | 13.9 (13.43) | 13.2 (12.4) | 14.7 (14.62) |
| DES—Mean score | 23.84 (14.94) | 22.89 (13.83)1 | 24.98 (16.17)1 |
| DES—Taxon score | 24.78 (16.25) | 23.75 (15.10)2 | 26.01 (17.53)2 |
Course
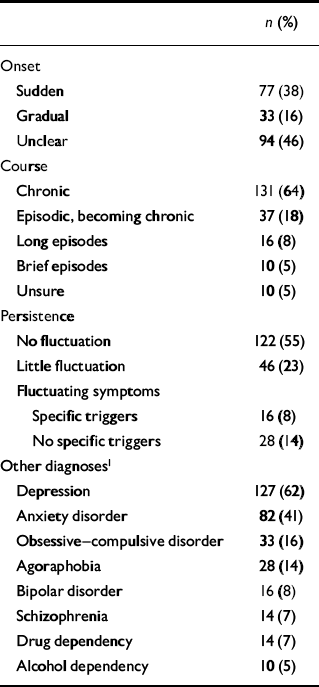
The most common description of the lifetime pattern of depersonalisation was ‘chronic’ (64%) and with little or no fluctuation (78%) (Table 2). The longest single episode for the majority (69%) was 1 year or more. Seventy-nine per cent of participants reported impaired social and/or work functioning (see Appendix for clinical descriptions).
Table 2 Associated diagnoses, onset and course in depersonalisation disorder (n=204)
| n (%) | |
|---|---|
| Onset | |
| Sudden | 77 (38) |
| Gradual | 33 (16) |
| Unclear | 94 (46) |
| Course | |
| Chronic | 131 (64) |
| Episodic, becoming chronic | 37 (18) |
| Long episodes | 16 (8) |
| Brief episodes | 10 (5) |
| Unsure | 10 (5) |
| Persistence | |
| No fluctuation | 122 (55) |
| Little fluctuation | 46 (23) |
| Fluctuating symptoms | |
| Specific triggers | 16 (8) |
| No specific triggers | 28 (14) |
| Other diagnoses1 | |
| Depression | 127 (62) |
| Anxiety disorder | 82 (41) |
| Obsessive—compulsive disorder | 33 (16) |
| Agoraphobia | 28 (14) |
| Bipolar disorder | 16 (8) |
| Schizophrenia | 14 (7) |
| Drug dependency | 14 (7) |
| Alcohol dependency | 10 (5) |
Onset and duration
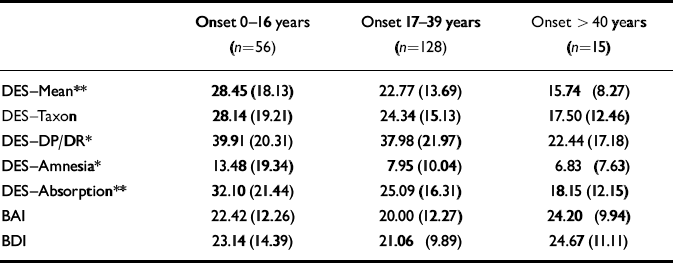
The mean age at onset of depersonalisation was 22.8 years, range 4-69 (Table 1), although 30% reported the onset before the age of 16 years. We divided the sample into one of three groups, depending upon age at onset: early (0-16 years); mid (17-39 years) and late (40+ years). One-way analysis of variance (ANOVA) revealed that the early-onset group scored significantly more highly than the mid-onset group, who in turn scored more highly than the late-onset group (see Table 3) on all the DES sub-scales and nearly significantly on DES—Taxon (F=2.748, d.f.=195, P=0.07). No effect of age at onset was observed for the BDI, BAI or PSE ratings (see Appendix).
Table 3 Mean (s.d.) scores from Dissociative Experiences Scale (DES), Beck Anxiety Inventory (BAI) and Beck Depression Inventory (BDI) for early-, mid- and late-onset participants and correlation of duration of illness with all measures (n=199; some missing data)
| Onset 0-16 years (n=56) | Onset 17-39 years (n=128) | Onset > 40 years (n=15) | |
|---|---|---|---|
| DES—Mean** | 28.45 (18.13) | 22.77 (13.69) | 15.74 (8.27) |
| DES—Taxon | 28.14 (19.21) | 24.34 (15.13) | 17.50 (12.46) |
| DES—DP/DR* | 39.91 (20.31) | 37.98 (21.97) | 22.44 (17.18) |
| DES—Amnesia* | 13.48 (19.34) | 7.95 (10.04) | 6.83 (7.63) |
| DES—Absorption** | 32.10 (21.44) | 25.09 (16.31) | 18.15 (12.15) |
| BAI | 22.42 (12.26) | 20.00 (12.27) | 24.20 (9.94) |
| BDI | 23.14 (14.39) | 21.06 (9.89) | 24.67 (11.11) |
Dissociative Experiences Scale (DES)
Mean scores from the DES (Tables 1 and 3) showed that female participants tended towards higher scores across all sub-scales than the males, but none reached statistical significance. Eighty per cent of participants scored on or above the DES—Taxon cut-off score of 13 for depersonalisation disorder and 90% scored on or above 8 on the DES—DP/DR sub-scale (76% >15 and 69% >20), with only 30% scoring in the dissociative disorders range. Scores on the DES—Amnesia sub-scale were noticeably lower than in other groups of patients with mixed dissociative disorders (Reference Dubester and BraunDubester & Braun, 1995; Reference Putnam, Carlson and RossPutnam et al, 1996).
The early- and late-onset groups were more likely to report hearing voices (χ2=14.47, d.f.=4, P=0.006) than the mid-onset group but were no more likely to use alcohol or drugs, have other psychiatric diagnoses, to have been hospitalised or to have suffered head trauma (90% thought that the voices were not ‘real’). The mean reported duration of depersonalisation was 13.9 years, range 0.5-69 (see Table 1). There were no significant correlations between length of illness (all r<0.1) and other clinical variables.
Subjects found it difficult to categorise the onset of their disorder, although just over one-third (38%) described a sudden onset (Table 2). These participants were more likely to experience seeing flashes of light (χ2=4.671, d.f.=1, P=0.04) and had a significantly lower mean score of 6.7 (s.d.=8.6) on the DES—Amnesia sub-scale compared with the gradual and unclear onset groups: mean DES—Amnesia=12.3 (s.d.=14.7), t=2.68 and P=0.008. No other sub-scale scores from the DES were significantly different.
Clinical assessment and PSE ratings
Comparisons were made between participants who were assessed clinically with an interview (n=124) and the remainder (n=80). There were no significant differences between the two groups on age (t=-0.56, P=0.58), gender (χ2=0.47, P=0.49), duration of illness (t=0.93, P=0.35), age at onset (t=-0.45, P=0.65), DES—Mean (t=0.34, P=0.74), DES—Taxon (t=0.62, P=0.54) and any sub-scale. There was no difference on the BDI score (t=-0.48, P=0.63) but there was a trend for slightly higher BAI anxiety scores (t=1.7, P=0.09) in the non-interviewed group. There were no differences between those participants with PSE ratings (including telephone interviewees) and those without. The main reasons why some subjects did not have a clinical assessment were: problems traveling to the clinic; lack of a responsible clinician to sanction the referral; and the need not to complicate existing clinical care.
Of those clinically assessed or with PSE ratings, formal diagnosis by a qualified psychiatrist in the clinic (according to DSM—IV) revealed 71% with primary depersonalisation disorder, 18% with depersonalisation secondary to major depression or dysthymic disorder, generalised anxiety disorder, agoraphobia (with and without panic) and obsessive—compulsive disorder, 3% with transient depersonalisation and 8% who were not assigned or where the diagnosis was unsure. Mann—Whitney tests revealed that PSE scores were significantly higher for participants designated with primary depersonalisation disorder, including transient cases (n=108; 74%), compared with those designated with secondary depersonalisation or other disorder (n=38) for both ‘depersonalisation’ (P<0.001; depersonalisation mean= 1.65, median=2; secondary: mean=1.44, median=1) and ‘derealisation’ ratings (P<0.001; derealisation mean=1.46, median=2; secondary: mean=0.79, median=1). There were no differences in terms of age or gender.
According to PSE ratings, depersonalisation was ‘present’ in 96% and ‘intense’ in 66% of cases. Symptoms of derealisation were ‘present’ in 80% and ‘intense’ in 49% of cases. Seventy-three per cent reported symptoms of depersonalisation and derealisation, 21% reported depersonalisation symptoms only and 6% reported derealisation symptoms only.
Attributions
Many participants (n=111) gave causal attributions for depersonalisation. Factors identified were psychological (15%), traumatic event (14%), substance misuse (14%), multiple (20%) and none obvious (27%). Participants were asked about factors that improved depersonalisation symptoms: 27% reported none, 19% physical (diet/exercise), 13% psychological, 8% social, 8% situational, 5% alcohol/drugs and the remaining 20% identified multiple factors. Psychological stress (16%), environmental lighting (10%) and physical stressors such as fatigue (12%) were identified as factors known to worsen depersonalisation.
Past medical and psychiatric history
Of all the participants, 62% reported no significant previous or current (60%) medical condition. Conditions mentioned included head injury (n=5), asthma (n=5), irritable bowel syndrome (n=4) and thyroid problems (n=3). Forty-two per cent reported undergoing a ‘brain scan’. Sixteen participants (8%) attributed a physical illness, specifically a viral infection, as the cause of the depersonalisation disorder. Tinnitus was mentioned in 29% of respondents and migraine in 31%, one-third of whom believed that their headaches and depersonalisation were connected.
For all participants (n=204), 50% reported a previous psychiatric diagnosis. The biggest single diagnostic category was depression in 62% (Table 2); 42% had experienced psychiatric hospitalisation and, of these, 57% had had more than one admission. The primary reason cited was major depression in (35%). Seventy-three per cent reported current ‘panic attacks’ and 59% said they were ‘afraid to go out alone’. The majority (72%) described persistent thoughts (mainly about depersonalisation) but only 26% said that they carried out any associated behaviours, for example checking or rituals. Seventy per cent of participants were currently taking psychotropic medication and these included the gamut of antidepressants and anxiolytics.
Alcohol and drugs
Of the participants who answered questions relating to alcohol and illicit drug use (n=154), six reported being previously treated for alcohol misuse (one current) and eight for drug misuse (two current). Forty-six people said that they had used illegal drugs in the past, with the majority reporting cannabis use only (n=20) and the remainder LSD, ecstasy, cocaine and various combinations of drugs. Forty participants reported using illicit drugs and 28 using alcohol just before the initial onset of depersonalisation; the role of drugs and alcohol in depersonalisation will be reported separately.
Family history
There was a suggestive family history (first- or second-degree relative) of depersonalisation disorder in 10% of cases. For all participants (n=204), 30% reported a history of some psychiatric disorder in a first-degree relative. The largest single diagnostic category was depression (28%), followed by alcohol misuse (15%) and panic (14%).
Anxiety and depression
The mean BAI score was 21.1 (s.d.=12.2) and the mean BDI score 22.0 (s.d.=11.5) for the entire sample. The BAI scores correlated significantly (r=0.25-0.41; all P<0.05), as did the BDI scores (r=0.35-0.52; all P<0.01), with all sub-scale scores from the DES. We used BDI and BAI scores to define operationally both primary and secondary depersonalisation. One-way ANOVA showed that participants scoring in the ‘normal’ range (0-11) on both the BAI and BDI had significantly lower mean scores on all sub-scales of the DES (except DES—Amnesia, which was generally low) than all other groups. Out of the 19 with no depression or anxiety, seven (37%) scored more than the DES—Taxon cut-off of 13 and may be said to have ‘pure depersonalisation’. Their mean (s.d.) DES—Taxon score compared with the remaining 185 subjects was 12.0 (12.1) v. 39.7 (21.5); F 5.54; P<0.001. Out of 57 with no or minimal depression or anxiety (scores of ≤18 on the BAI and BDI, respectively), 22 (38.6%) had ‘pure depersonalisation’.
DISCUSSION
Depersonalisation disorder is probably not as rare as is commonly assumed. We have amassed over 200 cases, slightly more men than women, from a single clinic over 4 years — the largest cohort of people with depersonalisation/derealisation described to date. The results both complement and enhance those of earlier reports (Reference Simeon, Gross and GuralnikSimeon et al, 1997; Reference Lambert, Senior and FewtrellLambert et al, 2001a ).
Limitations
The main limitation of this study was the criterion used to detect depersonalisation: 61% of the sample underwent a full psychiatric examination whereas the remainder were assessed on the basis of completed questionnaires (supplemented by a telephone interview in some). However, there were no significant differences between the two groups on a number of demographic and clinical variables. In addition, this sample was not epidemiologically based. Various biases will have affected self- and practitioner referrals. The option of contact through the internet may have biased the sample towards relatively high educational attainment and perhaps male gender (Reference Senior, Phillips and DavidSenior et al, 1997) and less depression (Reference Lambert, Senior and PhillipsLambert et al, 2000), although a similar gender ratio was reported by Simeon et al (Reference Simeon, Gross and Guralnik1997) in the USA, whose clinic attracts patients via ‘media advertisements’. Furthermore, family and past psychiatric history were based on self-report and an unstructured clinical interview without independent corroboration.
Clinical course
There was no uniform pattern to the mode of onset. Sudden onset did not appear to mark out a distinct subgroup. Depersonalisation disorder tended to occur around 23 years of age (range 4-69), which is somewhat later than Simeon et al's 1997 series but similar to older series (e.g. Reference SedmanSedman, 1966). With our larger sample we were able to separate an early-onset group (5-16 years) who appeared to have a more severe disorder in that they were more likely to report higher depersonalisation disorder symptomatology and greater levels of anxiety and depression (see also Reference Brauer, Harrow and TuckerBrauer et al, 1970). They also endorsed a question regarding hallucinations of voices. However, it is reassuring that in most cases several years had passed without any suggestion of a psychotic illness developing. These phenomenological differences between early and late onset were not accounted for by a greater use of illicit drugs or alcohol underlying the psychiatric diagnosis. Depersonalisation symptoms in general appear to improve with age (Reference SedmanSedman, 1966), but in line with classical descriptions and Simeon et al's findings (Reference Simeon, Gross and Guralnik1997) we found that depersonalisation disorder tends to run a chronic and unremitting course (see Appendix).
Depersonaliation and derealisation
Seventy-three per cent of participants reported symptoms of both depersonalisation and derealisation, the latter as a single phenomenon being rare (see also Reference SedmanSedman, 1966). The majority of participants were designated as having a clinical diagnosis of ‘primary depersonalisation disorder’ (DSM—IV depersonalisation disorder). The main symptoms focused on emotional and sensory/perceptual disturbances such as self-reported ‘flattening or blunting of affect’, ‘feeling as if the world and/or the self was unreal’ or ‘like seeing the world through a goldfish bowl’. This supports the placing together of depersonalisation and derealisation as in the ICD—10 classification and not their separation as in the DSM—IV. Pure derealisation does exist and may well have a distinct neurophysiological basis because it resembles the syndrome of visual hypoemotionality (Reference Sierra, Lopera and LambertSierra et al, 2002a ). However, current and previous work have failed to show any clinical factors unique to ‘idiopathic’ derealisation (Reference Lambert, Senior and PhillipsLambert et al, 2000).
Associations: other psychiatric disorders
Clues to aetiology come from some of the clinical associations. Just under half of all participants reported ‘seeing flashes of light’, suffered from tinnitus and/or migraine. Patients with migraine have been noted to experience symptoms of depersonalisation, suggesting that this association may not be due to chance (Reference Lambert, Sierra and PhillipsLambert et al, 2002). Indeed, such an association (38%) was noted by Shorvon et al in 1946. No cases of temporal lobe disorder were uncovered, although further specific tests such as electroencephalography and magnetic resonance imaging were not carried out (see Reference Lambert, Sierra and PhillipsLambert et al, 2002). Trauma (including physical/sexual abuse) was recorded as a contributing factor in 14% of cases compared with the 43% reported by Simeon et al (Reference Simeon, Gross and Guralnik1997) who had been subjected to childhood abuse including domestic violence. Again, specific study of such antecedents may be worthwhile. Factors that were identified by some to improve depersonalisation, such as diet, exercise, alcohol and fatigue, were listed by others as worsening the condition.
The main risk factor was a past (and family) psychiatric history, although this was non-specific. Half of the sample reported being diagnosed formally with one or more psychiatric disorders (besides depersonalisation disorder), the most common being depression and/or anxiety (Reference DixonDixon, 1963). The majority of participants reported having ‘panic attacks’ (Reference Cassano, Petracca and PerugiCassano et al, 1989; Reference Segui, Maruez and GarciaSegui et al, 2000), prompting a reevaluation of Roth's ‘phobic anxiety—depersonalisation syndrome’ concept (Reference RothRoth, 1959), generalised anxiety, low or flat mood (Reference AcknerAckner, 1954; Reference Brauer, Harrow and TuckerBrauer et al, 1970; Reference SedmanSedman, 1970) as well as symptoms specific to depersonalisation disorder.
Other comorbid diagnoses were not made using a structured clinical interview but scores on the BAI and BDI will enable comparison with other case series. Correlations between depersonalisation-specific symptoms from the DES were highest with depression ratings, suggesting a degree of overlap. On the other hand, it has been shown that prognosis of anxiety disorder, particularly panic, is worsened if accompanied by depersonalisation (Reference Segui, Maruez and GarciaSegui et al, 2000). The reasons why some people develop depersonalisation as a complication of another neurotic disorder deserves further investigation.
Clearly, the clinical distinction between primary and secondary depersonalisation seems easy to make but is not absolute. We were able to extract a small group who had no symptoms of either depression or anxiety, more than one-third of whom scored above a validated cut-off for depersonalisation disorder. Links with anxiety and depression appear to be stronger than ‘dissociation’, given the low scores on amnesia items in the DES (Reference Dubester and BraunDubester & Braun, 1995). Many authorities regard ‘amnesia’ — recurrent discontinuities in conscious awareness — as the hallmark of dissociation (Reference Putnam, Carlson and RossPutnam et al, 1996). The relatively low level of childhood abuse in this cohort again supports a separation from other dissociative disorders, as does the lack of significant female preponderance in this and other series (Reference Shorvon, Hill and BurkittShorvon et al, 1946; Reference Simeon, Guralnik and SchmeidlerSimeon et al, 2001). All in all, these clinical features favour placing depersonalisation disorder with anxiety and mood disorders (as in the ICD—10) rather than with dissociative disorders (as in the DSM—IV).
Comorbidity may arise from attempts to cope with depersonalisation, such as anxious or obsessive ‘checking’ of symptoms change leading to compulsive behaviours (Reference Simeon and HollanderSimeon & Hollander, 1993), cognitive and behavioural avoidance of potential exacerbating factors or, instead, feelings of hopelessness. Differing appraisals currently are being explored through the development of theoretical cognitive—behavioural models, and in practice using a variety of therapeutic techniques including ‘attention training’ (Reference Senior, Hunter and LambertSenior et al, 2001). In view of the chronicity and persistence of the condition, research into its aetiology and possible treatments, both pharmacological and psychological, is urgently required.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Depersonalisation disorder tends to be chronic and persistent.
-
▪ Early onset is associated with a more severe disorder.
-
▪ Depersonalisation disorder has stronger affiliations with anxiety and depression than with dissociation.
LIMITATIONS
-
▪ Not all participants had a full clinical examination.
-
▪ The survey was based on clinic rather than community cases.
-
▪ Longitudinal data are not reported.
APPENDIX
Brief presentation of six ‘typical’ cases of depersonalisation disorder
The following case descriptions are anonymised, reconstructed vignettes incorporating statements similar to those made by individuals from the sample studied.
Case 1
A 26-year-old male student with depersonalistion disorder for 9 years who failed to complete his studies owing to illness.
Onset and attribution Acute onset following illicit drug use at a party. Believes that cannabis was ‘spiked’ with unknown chemical.
Subjective description Reported feeling emotionally numb and cut-off from other people. Visual disturbance of ‘hands and feet appearing to increase and decrease in size when I stare at them’. Said that he felt ‘as if I am living in a film — it's all black and white and 2D. I know that it is not real but that is how it feels’.
Diagnosis The disorder is constant and chronic. Previous psychiatric differential diagnoses were of anxiety, panic, depression and schizophrenia.
Case 2
A 30-year-old male journalist with depersonalistion disorder for 15 years.
Onset and attribution Acute onset following alcohol binge at a party when aged 15 years. Patient believes that parental abuse was a contributing factor.
Subjective description ‘I'm Unreal and truly alone — like an outsider looking in... When I walk down the street I feel as if I am swaying and the pavement is moving. I feel as if I can't connect normally to people on a mental level. I just don't feel anything — I think I have gone mad.’
Diagnosis The disorder is constant and chronic, with a previous psychiatric diagnosis of depression.
Case 3
A 29-year-old female sales manager with depersonalistion disorder for 6 months who is married with a family business.
Onset and attribution Current episode: gradual onset following recent marriage. Previous episode: acute onset at age 20 years following a prolonged period of stress (duration of disorder=5 years).
Subjective description ‘I don't know who I am — of course I am **** but I feel like a robot, like I am listening to someone else talking, like I am looking at myself from the outside, but it is not another voice or body — it is mine, it is me, it just doesn't feel like it... I spend all day trying to figure it out. Maybe I am too analytical. Nothing makes it better but being with other people makes it worse.’
Diagnosis The disorder is episodic and becoming chronic. There was no previous psychiatric diagnosis.
Case 4
A 54-year-old married female barrister with depersonalistion disorder for 30 years.
Onset and attribution Unsure of onset. Patient recalls feeling the disorder all of her life.
Subjective description ‘I feel nothing — never have. When my children were born — nothing. I am not sure what love is, I have been married 30 years, it drives my husband mad when I talk about it. I just feel nothing — not pain, not anxiety, not happiness. I am not depressed — I am nothing.’
Diagnosis The disorder is constant and chronic, with a previous psychiatric diagnosis of depression.
Case 5
A 40-year-old divorced male with depersonalistion disorder for 2 years who is unemployed.
Onset and attribution Gradual onset over 6 months for two separate episodes. Both episodes attributed to unhappy relationships.
Subjective description ‘These feelings are unbearable. It is like walking around with a goldfish bowl on your head... I can't drive, can't work. You try taking photos when everything you look at feels... like it is the wrong colour and depth is all wrong... When you try and tell people they think you're mad.’
Diagnosis The disorder is constant and chronic within each episode. There was a previous diagnosis of anxiety and depression.
Case 6
A 28-year-old male, unemployed shop assistant with depersonalistion disorder for 4 years.
Onset and attribution Gradual onset over several months with each separate episode becoming more intense. No attribution made or significant life events reported.
Subjective description ‘This sounds mad but I am not me. I look in the mirror and I don't see me. I don't know who it is that I see and I don't know where the real me has gone. Logically that cannot be the case, but that is how it feels. I spend all day checking myself and it's never me. I panic and try to solve where I am. I feel so depressed, like I can't go on living this way but I live in hope that one day I will wake up and it will be me.’
Diagnosis The disorder is constant and chronic with anxiety and depression. There was a previous psychiatric diagnosis of panic and obsessive—compulsive disorder.
Acknowledgement
The authors acknowledge the support of the Pilkington Family Trusts.








eLetters
No eLetters have been published for this article.