The evaluation of withdrawal programmes of long-term benzodiazepine use has been limited, as none of the reported studies included a control condition to correct for the number of people able to discontinue those drugs without any support, and none of them identified all long-term users before starting recruitment, limiting generalisability (Reference Oude Voshaar, Gorgels and MolOude Voshaar et al, 2001). In this study we recruited participants known to their general practitioner to be long-term benzodiazepine users, and included a control group receiving usual care. Because Cormack et al (Reference Cormack, Sweeney and Hughes-Jones1994) found that after written advice from their general practitioner 18% of people using benzodiazepines quit by themselves, this intervention was used as a pre-selection. Our objectives were to investigate the effects of tapering off long-term benzodiazepine use in patients who did not quit after written personal advice to do so; the value of additional group cognitive–behavioural therapy (CBT); and the feasibility of using both taper programmes in general practice.
METHOD
Design
The study was a randomised, controlled trial comparing tapering off long-term benzodiazepine use alone with tapering off combined with group CBT and with a control group receiving usual care. In order to include only those who were unable to quit of their own accord, all patients who were long-term users were sent a letter by the participating general practitioner in which they were advised to discontinue their benzodiazepine use. The study received ethical approval from the University Medical Centre, Nijmegen, and took place from 1998 to 2001.
Retirement
Long-term benzodiazepine use was identified by means of a computerised search for benzodiazepine prescriptions at 30 general practices (58 doctors; 118 082 patients). The practices were chosen to maximise the variety of locations throughout the Netherlands – 12 were urban (Amsterdam, Nijmegen and Almere) and 18 rural (villages near Nijmegen) – and of organisation type (4 health centres, 11 group practices and 15 solo practices). ‘Long-term use’ was defined as benzodiazepine use for at least 3 months with a prescribed amount sufficient for at least 60 days of consumption in accordance with the recommended dosage. Exclusion criteria were current psychiatric treatment; current treatment for drug or alcohol dependence; medical history of psychosis; epilepsy; insufficient mastery of the Dutch language; or terminal illness. Furthermore, some people were excluded specifically at general practitioner's request because of severe comorbidity or for psychosocial reasons. People who met this definition of long-term benzodiazepine use were sent a letter by their general practitioner advising them to quit gradually and inviting them to the surgery 3 months later to evaluate the effect of the letter. At this consultation the doctor enquired whether the patient had been able to achieve complete abstinence and if not, whether the patient would participate in this study. All participants provided written informed consent.
Sample size and randomisation
The aim was to increase the success rate after the pre-selection procedure (i.e. the letter from the general practitioner) from an expected 55% through tapering off alone, to 80% by combining tapering off with group CBT (Reference Otto, Pollack and SachsOtto et al, 1993). Based on a chi-squared test, this effect size required a sample size (two-sided α=0.05, β=0.20) of 52 participants in each experimental group, or 62 participants based on a corrected chi-squared or Fisher's exact test (Reference Dupont and PlummerDupont & Plummer, 1990). Participants were randomised in a ratio of 2:2:1 to achieve maximum discriminative power between the two experimental groups. Computerised randomisation took place after at least ten participants within a geographic cluster had given informed consent, in order to form CBT groups with a minimum of four participants at a location near to the participants' homes.
Intervention
Tapering off
Participants who were not using diazepam were transferred to an equivalent dose of diazepam for 2 weeks by their own doctor, using the conversion table of Zitman & Couvée (Reference Zitman and Couvée2001). For participants taking more than one benzodiazepine, the dosages were added together. The daily dose of diazepam was reduced by 25% a week during four weekly visits. In accordance with Schweizer et al (Reference Schweizer, Rickels and Case1990) participants had the opportunity to divide the last step into two steps of 12.5% for 4 days. The last visit took place 2 weeks after the last reduction step. The general practitioner filled in a case record form to monitor progress and any adverse events during the intervention period. Two months later, we evaluated participant and doctor satisfaction and the feasibility of the withdrawal programme by means of a postal questionnaire.
Group cognitive–behavioural therapy
The participants who were randomised to tapering off combined with group CBT attended five weekly 2-h sessions of group CBT in addition to the dose reduction visits to their general practitioner. The sessions started halfway through the tapering-off period and finished 2 weeks after the conclusion of the withdrawal programme. The aim of the group therapy was to support the participants during the tapering-off process and to prevent relapse thereafter. The therapy programme included:
-
(a) psychoeducation concerning the advantages and disadvantages of long-term benzodiazepine use;
-
(b) teaching and practising relaxation exercises by means of progressive relaxation;
-
(c) cognitive restructuring of the interpretation of withdrawal symptoms.
The sessions were led by registered psychologists, experienced in CBT, who received training and a detailed manual of the therapy. The therapists documented participation and reasons for non-participation at each session. Tape-recordings of a random sample of sessions 3 and 5 were judged by an independent assessor using previously defined criteria, and did not show any protocol violations. Two months later, we evaluated patient satisfaction with the group therapy by means of a postal questionnaire.
Usual care
Participants in the usual care control group were informed about the randomisation by letter. They did not receive any help with benzodiazepine reduction.
Measurements
Participants received a baseline assessment after giving informed consent, and they received an outcome assessment 3 months after the start of the intervention. Structured interview assessments were carried out at the participants' homes by a trained research assistant, who explored the self-reported use of benzodiazepines, administered the 15-words test, and assessed the circumstances of filling in the self-report questionnaires.
Primary outcome measure
The primary outcome measure was the proportion of participants who successfully discontinued long-term benzodiazepine use, defined as no benzodiazepine use at the outcome self-report assessment. We checked self-reported discontinuation of benzodiazepine use in the general practitioners' prescription databases, which showed that less than 5% of the participants who reported successful discontuation had received a benzodiazepine prescription in the month before the outcome assessment.
Secondary outcome measures
Secondary outcome measures were the reduction in daily benzodiazepine dosage by participants who did not successfully discontinue drug use; the use of alcohol (including the number of problem drinkers, based on the 18-item list of Reference Cornel, Knibbe and Van ZutphenCornel et al, 1994); psychological well-being assessed by the General Health Questionnaire 12-item version (GHQ–12; Reference Goldberg and BlackwellGoldberg & Blackwell, 1970); memory (delayed recall of the 15-words test; Reference Saan and DeelmanSaan & Deelman, 1986); mood (the scales of depression, anger, fatigue, vigour and tension of the 32-item shortened Profile of Mood States; Reference Wald and MellenberghWald & Mellenbergh, 1990); and the number and severity of benzodiazepine withdrawal symptoms (Benzodiazepine Withdrawal Symptom Questionnaire; Reference Tyrer, Murphy and RileyTyrer et al, 1990).
Statistical analysis
To check for baseline differences between the three groups, a series of univariate analyses of variance (ANOVAs) or nonparametric equivalents were performed on psychiatric status and demographic variables. The primary outcome measurements were analysed with a chi-squared test (number of participants who discontinued successfully). A forward logistic regression analysis with correction for treatment group was performed to identify independent predictors (all baseline characteristics) of discontinuation success.
The dosage reduction in participants who failed to discontinue diazapam was analysed with one-way ANOVA (dosage quotient at outcome and baseline after natural log-transformation). Repeated-measures ANOVAs were performed on the other secondary outcome variables for continuous variables and chi-squared tests for dichotomous variables. Significant main effects were further analysed with pairwise comparisons.
Analyses were performed on an intent-to-treat basis. In the case of a missing outcome value, the last observation was carried forward to serve as the outcome measurement (whole sample, n=180). The analyses were repeated after excluding all those who had left the study at the outcome assessment (completers sample, n=141). A substantial number of participants had discontinued their use of benzodiazepines before the intervention started. For this reason, we also carried out a per protocol analysis on the participants who had been fully compliant with both the treatment programme and the outcome measurement (per protocol sample, n=78). We excluded the control group from this analysis, because only data on the experimental groups were available at the start of the intervention.
RESULTS
Study profile
Of the 2964 persons identified as long-term users of benzodiazepines, 2004 were advised to stop their benzodiazepine use; 1036 were eligible for the trial (Fig. 1). The participation rate was low: 180 out of 1036 (17.4%). Participants (n=180) and non-participants (n=876) did not differ with respect to age, gender or benzodiazepine dosage used. Of the 146 participants assigned to one of the withdrawal programmes, 23 discontinued their benzodiazepine use while waiting for the intervention to begin. In order to start therapy groups with at least 4 participants, the mean (s.d.) delay between baseline assessment and intervention was 71 (45) days (range 0–223 days). Thirty-nine participants refused to take part in the outcome assessment. The numbers leaving the study at this stage did not differ significantly across the three groups (χ2=1.85, d.f.=2, P=0.40). Of the 85 participants compliant with the entire intervention programme (tapering off alone or tapering off with group CBT), 78 were assessed at outcome.

Fig. 1 CONSORT diagram. BZD, benzodiazepine; CRF, case record form; GP, general practitioner.
Characteristics of the study participants
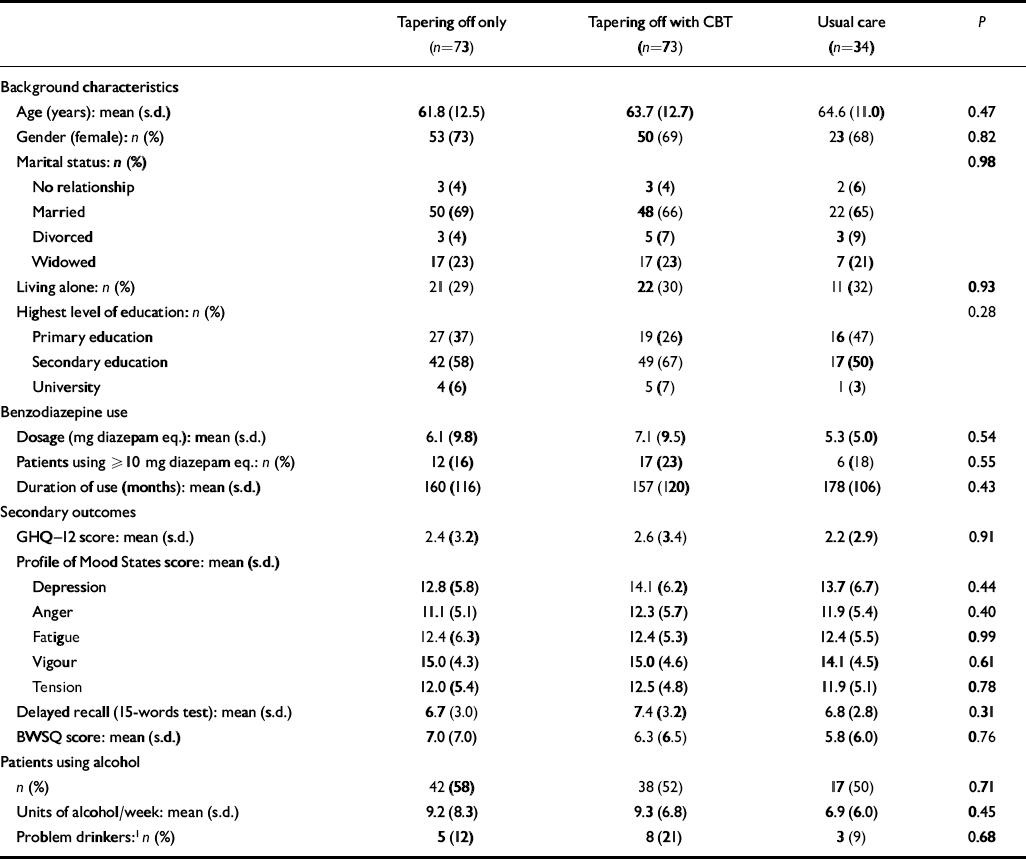
Comparisons of the three groups did not reveal any significant differences in baseline characteristics (Table 1). In addition, no significant difference in baseline characteristics was observed between those leaving and those completing the study. In the sample as a whole, the decile scores on the 15-words test did not differ from the norm. Sub-analyses revealed that participants who were using 10 mg diazepam equivalents or more per day (n=35) had significantly worse scores than the participants who were using less than 10 mg per day (t=2.25, d.f.=178, P=0.03) and the norm population (t=5.93, d.f.=34, P<0.001).
Table 1 Characteristics of the study participants (n=180) at baseline assessment
| Tapering off only (n=73) | Tapering off with CBT (n=73) | Usual care (n=34) | P | |
|---|---|---|---|---|
| Background characteristics | ||||
| Age (years): mean (s.d.) | 61.8 (12.5) | 63.7 (12.7) | 64.6 (11.0) | 0.47 |
| Gender (female): n (%) | 53 (73) | 50 (69) | 23 (68) | 0.82 |
| Marital status: n (%) | 0.98 | |||
| No relationship | 3 (4) | 3 (4) | 2 (6) | |
| Married | 50 (69) | 48 (66) | 22 (65) | |
| Divorced | 3 (4) | 5 (7) | 3 (9) | |
| Widowed | 17 (23) | 17 (23) | 7 (21) | |
| Living alone: n (%) | 21 (29) | 22 (30) | 11 (32) | 0.93 |
| Highest level of education: n (%) | 0.28 | |||
| Primary education | 27 (37) | 19 (26) | 16 (47) | |
| Secondary education | 42 (58) | 49 (67) | 17 (50) | |
| University | 4 (6) | 5 (7) | 1 (3) | |
| Benzodiazepine use | ||||
| Dosage (mg diazepam eq.): mean (s.d.) | 6.1 (9.8) | 7.1 (9.5) | 5.3 (5.0) | 0.54 |
| Patients using ≥ 10 mg diazepam eq.: n (%) | 12 (16) | 17 (23) | 6 (18) | 0.55 |
| Duration of use (months): mean (s.d.) | 160 (116) | 157 (120) | 178 (106) | 0.43 |
| Secondary outcomes | ||||
| GHQ—12 score: mean (s.d.) | 2.4 (3.2) | 2.6 (3.4) | 2.2 (2.9) | 0.91 |
| Profile of Mood States score: mean (s.d.) | ||||
| Depression | 12.8 (5.8) | 14.1 (6.2) | 13.7 (6.7) | 0.44 |
| Anger | 11.1 (5.1) | 12.3 (5.7) | 11.9 (5.4) | 0.40 |
| Fatigue | 12.4 (6.3) | 12.4 (5.3) | 12.4 (5.5) | 0.99 |
| Vigour | 15.0 (4.3) | 15.0 (4.6) | 14.1 (4.5) | 0.61 |
| Tension | 12.0 (5.4) | 12.5 (4.8) | 11.9 (5.1) | 0.78 |
| Delayed recall (15-words test): mean (s.d.) | 6.7 (3.0) | 7.4 (3.2) | 6.8 (2.8) | 0.31 |
| BWSQ score: mean (s.d.) | 7.0 (7.0) | 6.3 (6.5) | 5.8 (6.0) | 0.76 |
| Patients using alcohol | ||||
| n (%) | 42 (58) | 38 (52) | 17 (50) | 0.71 |
| Units of alcohol/week: mean (s.d.) | 9.2 (8.3) | 9.3 (6.8) | 6.9 (6.0) | 0.45 |
| Problem drinkers:1 n (%) | 5 (12) | 8 (21) | 3 (9) | 0.68 |
Benzodiazepine usage
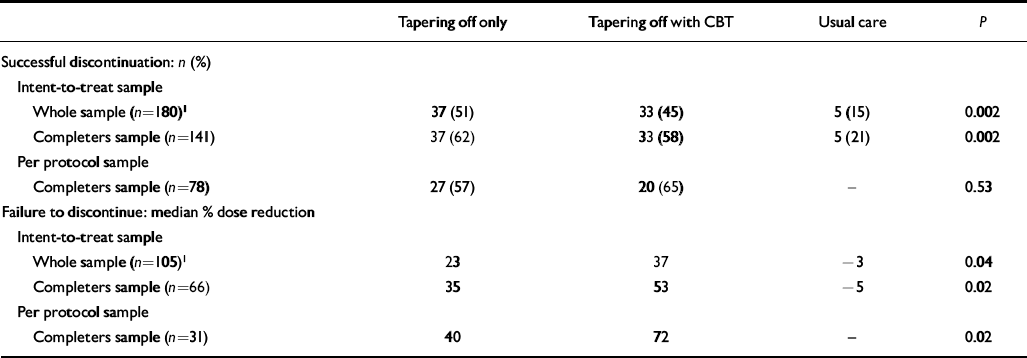
The proportions of participants who successfully discontinued benzodiazepine use differed significantly between the three groups in the intent-to-treat analysis (Table 2). Subsequent pairwise comparisons revealed that the two experimental groups did not differ significantly from each other in the intent-to-treat analysis (whole sample P=0.51, completers sample P=0.68). However, the two experimental groups were significantly more successful than the control group: tapering off alone (whole sample P<0.001; completers sample P=0.001) and tapering off combined with group CBT (whole sample P=0.002; completers sample P=0.002). Corroborating these findings, the per protocol analysis did not show any significant difference between the two experimental conditions (P=0.53). Logistic regression analysis yielded benzodiazepine dosage as the only independent predictor of successful discontinuation (OR=4.5, 95% CI 2.0–10.2). Patients who used 10 mg diazepam equivalents or more had a significantly lower chance of successful discontinuation than patients using less than 10 mg (35% v. 64%, P=0.009).
Table 2 Benzodiazepine use at 3 months' follow-up
| Tapering off only | Tapering off with CBT | Usual care | P | |
|---|---|---|---|---|
| Successful discontinuation: n (%) | ||||
| Intent-to-treat sample | ||||
| Whole sample (n=180)1 | 37 (51) | 33 (45) | 5 (15) | 0.002 |
| Completers sample (n=141) | 37 (62) | 33 (58) | 5 (21) | 0.002 |
| Per protocol sample | ||||
| Completers sample (n=78) | 27 (57) | 20 (65) | - | 0.53 |
| Failure to discontinue: median % dose reduction | ||||
| Intent-to-treat sample | ||||
| Whole sample (n=105)1 | 23 | 37 | -3 | 0.04 |
| Completers sample (n=66) | 35 | 53 | -5 | 0.02 |
| Per protocol sample | ||||
| Completers sample (n=31) | 40 | 72 | - | 0.02 |
Among those failing to quit, dose reduction differed significantly across the three groups (whole sample F 2,102=3.33, P=0.04; completers sample F 2,62=3.98, P=0.02). Tukey HSD post hoc tests showed a significant difference in dosage reduction between tapering off combined with group CBT and usual care (whole sample P=0.03; completers sample P=0.02).
Secondary outcome measures
We used repeated-measure ANOVAs across the three groups to evaluate the effects of the severity of withdrawal symptoms, psychological distress, mood, memory and problem alcohol use. There was a significant time effect only for the delayed recall of the 15-words test, which indicated an improvement. However, no significant interaction effect emerged for any of the secondary outcome measures, thus these measures were fairly comparable in the three groups (Table 3). Moreover, comparing participants who successfully discontinued benzodiazepine use with those who failed to do so did not result in significant time×outcome interaction effects for any of the secondary outcome measures. Neither the prevalence of alcohol use, nor the amount consumed by alcohol users, changed.
Table 3 Secondary outcome measures at 3 months' follow-up in the intent-to-treat sample (last observation carried forward, n=180)

| Tapering off only | Tapering off with CBT | Usual care | P | |
|---|---|---|---|---|
| GHQ—12 score: mean (s.d.) | 1.8 (2.5) | 2.4 (3.0) | 1.8 (3.0) | 0.83 |
| Profile of Mood States score: mean (s.d.) | ||||
| Depression | 12.6 (5.2) | 13.8 (6.9) | 13.0 (7.5) | 0.86 |
| Anger | 11.5 (5.5) | 12.0 (6.2) | 10.7 (5.1) | 0.22 |
| Fatigue | 12.7 (6.4) | 12.7 (5.9) | 11.7 (7.0) | 0.68 |
| Vigour | 14.9 (4.9) | 15.0 (4.7) | 15.3 (5.9) | 0.39 |
| Tension | 11.4 (4.9) | 12.6 (5.8) | 11.1 (5.6) | 0.46 |
| Delayed recall (15-words test): mean (s.d.) | 7.2 (2.9) | 8.1 (3.4) | 7.6 (2.5) | 0.83 |
| BWSQ score: mean (s.d.) | 6.2 (6.8) | 6.8 (7.5) | 5.8 (7.3) | 0.57 |
| Patients using alcohol | ||||
| n (%) | 42 (58) | 40 (55) | 18 (53) | 0.81 |
| Units of alcohol/week: mean (s.d.) | 10.0 (11.0) | 8.3 (6.4) | 7.3 (6.4) | 0.63 |
| Problem drinkers: n (%)1 | 5 (12) | 10 (14) | 5 (15) | 0.71 |
Doctor and patient views of the tapering-off strategy
Participants (n=103) who entered the withdrawal programme visited their general practitioner an average of 5.6 times (s.d.=1.4, range 1–9). The average number of visits did not differ between the participants assigned to tapering off alone and those assigned to tapering off combined with group CBT, and there was no difference between the participants who successfully discontinued benzodiazepine fully use and those who did not. A total of 43 out of the 58 participating doctors actually supervised the patients during the tapering-off process; 42 of them returned the postal evaluation questionnaire. Analysis of these questionnaires showed that 37 doctors (88%) had found the protocol feasible at their own practice, 35 (83%) would encourage other general practitioners to taper off long-term benzodiazepine use with the aid of the withdrawal protocol, and 22 (52%) had already started using this protocol for patients not included in the trial. No major adverse event during the reduction period (such as epileptic seizure or psychotic episode) was reported in the case record forms.
A total of 91 (88%) of the 103 participants who entered the withdrawal programme returned the postal evaluation questionnaire. The results showed that 78 (86%) of those who responded were satisfied with the ‘treatment’ received; 66 (73%) would be willing to follow the same treatment again if necessary. With respect to their supervision, 65 (76%) preferred treatment by their own general practitioner, 6 (7%) preferred referral to a specialised treatment setting, 12 (14%) preferred no support with tapering off and 3 (3%) had no preference.
Attrition rates and participants' views on group CBT
Seven (10%) of the 73 participants assigned to CBT discontinued their benzodiazepine use before the start of the intervention. In order to prevent relapse, we invited these participants to the therapy sessions; however, only two actually participated. Of the participants who began the tapering-off process combined with group CBT, only 34 (65%) attended three or more sessions (Fig. 1). The discontinuation success rates did not differ significantly between the patients who were compliant with CBT and those who were not: 20/31 (65%) ν 6/15 (40%), P=0.12. The postal evaluation questionnaire was returned by 30 (88%) of the 34 compliant participants: 14 (47%) of them would have preferred more sessions; 28 (93%) were satisfied with the group therapy in general. The degree of satisfaction with group CBT was not related to taper success.
DISCUSSION
Tapering off was an effective strategy for the discontinuation of long-term benzodiazepine use, even after pre-selection with a letter containing advice to stop, achieving its highest success rates in patients using less than 10 mg diazepam equivalents. Adding group CBT did not increase the proportion of those who successfully discontinued. Although the study was marginally lacking power for some analyses, this is irrelevant since the success rate for patients receiving group CBT was numerically lower than that for the group assigned to tapering off alone. Of those who failed to discontinue benzodiazepine use, those assigned to additional group CBT reduced their dosage significantly more than the participants in the control group. Both withdrawal programmes proved to be feasible in general practice. After the intervention, we did not find any significant differences between the three groups in the presence and severity of withdrawal symptoms, symptoms reflecting psychological distress, and mood disturbances. Neither the prevalence of problem drinking or alcohol use, nor the amount of alcohol consumed, was influenced by the intervention type or tapering off, which indicates that none of our participants replaced benzodiazepine use with alcohol.
Efficacy of tapering off
This was the first study to show the efficacy of tapering off long-term benzodiazepine use by including a ‘usual care’ control condition. Although we pre-selected patients by sending a letter advising them to stop their use, our success rates were comparable with those of other benzodiazepine withdrawal studies (Reference Schweizer, Rickels and CaseSchweizer et al, 1990; Reference Zitman and CouvéeZitman & Couvée, 2001). In the control group, 21% of the participants stopped their benzodiazepine use spontaneously. In addition, 23 (16%) of the 146 participants assigned to the experimental groups discontinued benzodiazepine use without any professional help while waiting for the interventions to start. At first we considered this to be a methodological (but inevitable) problem of our study, because it took some time to fill the therapy groups. However, it appeared to be a cost-effective strategy in view of the 60% success rate among those still using benzodiazepines, as was shown by the per protocol analysis. The proportions of participants who stopped spontaneously were much higher than the estimated 6%. Several explanations can be put forward. First, actually taking part in a discontinuation trial could provide an extra incentive to discontinue benzodiazepine use independently, even if a previous attempt was not successful. Second, owing to the selection process, the proportion of participants in discontinuation trials who are able to stop their use without any professional help might be higher than in long-term users in general.
Generalisability
A participation rate of 17.4% presumes significant selection processes. Although patients gave a variety of reasons for non-participation, dependence on benzodiazepines might have played an important part. Kan et al (Reference Kan, Breteler and Zitman1997) found that 40% of all those prescribed benzodiazepines in general practice were dependent on benzodiazepines according to DSM–III–R criteria (American Psychiatric Association, 1987), and Linden et al (Reference Linden, Bar and Geiselmann1998) found that two-thirds of those who were long-term benzodiazepine users rejected a drug ‘holiday’. Reluctance to enter group therapy as well as reluctance to hold interview sessions at home might have also contributed to the small number of participants. In clinical practice a higher recruitment rate might be achieved if the patients are not asked to participate in a randomised trial. As participants were representative with respect to not only age and gender, but also to the (only) independent predictor of success, benzodiazepine dosage, it is unlikely that we excluded treatment-resistant patients. As we identified all patients who were long-term users before we recruited participants, it is not possible to compare our attrition rate with that of other studies that recruited referred participants from specialised settings or by advertisement.
Efficacy of group CBT
In our study, adjunctive group CBT focused on the management of withdrawal symptoms did not have any additional value. Previous studies evaluating simultaneous psychological treatment to improve these success rates have considerable methodological problems. Two studies did not compare the efficacy of additional CBT ν tapering off alone (Reference Sanchez-Craig, Cappell and BustoSanchez-Craig et al, 1987; Reference Elsesser, Sartory and MaurerElsesser et al, 1996); the other studies did not use a controlled design (Reference Cormack and SinnottCormack & Sinnott, 1983; Reference Schmauss, Apelt and EmrichSchmauss et al, 1987; Reference Crouch, Robson and HallstromCrouch et al, 1988; Reference Joughin, Tata and CollinsJoughin et al, 1991), did not randomise participants over the conditions (Reference Higgitt, Golombok and FonagyHiggitt et al, 1987) or studied a sample of fewer than 10 participants (Reference Tyrer, Murphy and OatesTyrer et al, 1985; Reference Nathan, Robinson and CherekNathan et al, 1986). The two studies without these methodological problems were restricted to participants who met the criteria for panic disorder; here the addition of CBT to tapering off significantly increased the proportion who successfully discontinued benzodiazepine use (Reference Otto, Pollack and SachsOtto et al, 1993; Reference Spiegel, Bruce and GreggSpiegel et al, 1994). These results are difficult to generalise, as the prevalence of panic disorder among those who are long-term benzodiazepine users has been estimated to be at most 27% (Reference Rickels, Case and SchweizerRickels et al, 1986). Our success rate for CBT might have been increased by a priori selection on psychiatric morbidity and by introducing disorder-specific elements. A disadvantage of this strategy is that the programme cannot then be used easily in general practice.
The lack of additional value might also be due to the limited number of sessions provided. However, the efficacy of brief psychotherapy in alcohol dependence and somatisation disorder in general practice has been supported by the results of randomised, controlled trials (Reference Sandahl and RonnbergSandahl & Ronnberg, 1990; Reference LidbeckLidbeck, 1997). In view of the relapse rate in the benzodiazepine withdrawal study by Zitman & Couvée (Reference Zitman and Couvée2001), and the delayed effects of psychotherapy in the treatment of cocaine dependence (Reference Carroll, Rounsaville and NichCarroll et al, 1994) and in the tapering off of alprazolam in panic disorder (Reference Otto, Pollack and SachsOtto et al, 1993), a long-term follow-up study is planned. Another possibility is to give CBT after instead of during tapering off. In our opinion, however, this strategy is of limited value in clinical practice: only two of the seven participants who stopped their use before the intervention could be motivated to attend the therapy sessions to help them remain benzodiazepine-free in the future.
Adherence to group CBT
Adherence to group therapy was poor, which may reflect an overall resistance to group therapy among people who are long-term benzodiazepine users. This is in line with findings in other studies (Reference Cormack and SinnottCormack & Sinnott, 1983; Reference Nathan, Robinson and CherekNathan et al, 1986) and with our interpretation of the personal reasons why patients refused to attend group therapy sessions. Moreover, individual CBT sessions to restructure dysfunctional cognition might be more successful. However, the poor adherence cannot explain the lack of success, as the success rate of patients who were compliant with CBT (n=34) was 65%. Although sub-analyses lack statistical power, it is unlikely this would be superior to the 57% success rate of tapering off alone.
Feasibility in general practice
Tapering off was tolerated well in general practice: the general practitioners did not report any major adverse event during or after the tapering-off process. The good compliance and high level of satisfaction with the programme among both doctors and participants further strengthen the feasibility of tapering off as a strategy to discontinue long-term benzodiazepine use in general practice.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ This study is the first to evaluate additional psychotherapy in a randomised, controlled fashion.
-
▪ Gradual tapering-off is an effective way of discontinuing benzodiazepine use.
-
▪ Additional psychotherapy does not seem to increase the success rate of the gradual tapering-off approach.
LIMITATIONS
-
▪ Only one in six patients in this study were willing to take part in a withdrawal programme.
-
▪ Treatment adherence in psychotherapy was limited.
-
▪ Patients received no diagnostic psychiatric screening, which made sub-analyses in specific diagnostic groups impossible.









eLetters
No eLetters have been published for this article.