Childhood maltreatment and abusive experiences in adulthood are major problems which lead to high levels of psychiatric morbidity and social difficulties. Studies have indicated that many women who were abused as children are later abused as adults, with evidence that childhood abuse independently increases the risk of adult abuse (Reference Coid, Petruckevitch and FederCoid et al, 2001). Independent associations with psychiatric morbidity and substance misuse in adulthood are as strong for those who have experienced recent abuse as for those who have experienced childhood physical or sexual abuse (Reference McCauley, Kern and KolodnerMcCauley et al, 1997). Some studies detecting these associations have used broad categories of abusive experience over a woman's lifetime. As different types of abuse tend to co-occur in women's lives, the effect of one experience on subsequent psychiatric morbidity may be confounded by others.
Most studies of the relationship between early abusive experiences and adult mental health have focused on the role of sexual abuse, although some have attempted to examine the independent contributions of childhood sexual and physical abuse (Reference Mullen, Martin and AndersonMullen et al, 1993; Reference Hill, Davis and ByattHill et al, 2000; Reference Dube, Anda and FelittiDube et al, 2001). Most studies investigating the differential impact of abusive experiences in both childhood and adulthood are characterised by small sample sizes or a limited number of clinical outcome measures. Previous investigators have not been able to differentiate independent effects of multiple abusive experiences over the lifetime on mental health outcomes.
We carried out a survey of adult women attending primary care in east London to:
-
(a) measure the prevalence of a range of self-reported childhood and adult abusive experiences;
-
(b) measure the prevalence of psychiatric morbidity, using a range of categorical measures, including anxiety, depression, post-traumatic stress disorder (PTSD), deliberate self-harm and substance misuse;
-
(c) analyse associations between demographic variables and measures of mental health;
-
(d) analyse associations between individual childhood and adult abusive experiences and mental health outcomes.
METHOD
Between January and December 1999, we surveyed adult female patients (16 years old or over) in 13 general practices in the London borough of Hackney from a random list of all general practice surgeries. All consecutive eligible female patients attending the surgeries were invited to take part in the survey and recruitment took place during seven randomised sessions per week over a 2–4 week period for each practice. Women were eligible to participate if they were registered with the practice and were able to read English, Turkish or Bengali. Those observed to be holding an infant or who were too ill to participate were excluded.
If an adult female patient was eligible to participate, a research assistant introduced the woman to the survey and the purpose of the study was explained. Women were told that participation was voluntary and that all information disclosed would be confidential and would not be given to their doctor or entered in their medical records. Doctors had been given an information pack which detailed local support and housing services for abused women before the start of the study. The survey questionnaire also included an information sheet explaining the study in detail, a list of local support services for women, and a written consent form. Women were encouraged to take the information and support services sheet away with them.
The self-administered questionnaire was specifically developed for this survey and translated into Bengali and Turkish. It included enquiries about demographic details; the Hospital Anxiety and Depression Scale (HADS), rating the presence of anxiety and depression (score of 11 or more) in the past week (Reference Zigmond and SnaithZigmond & Snaith, 1983); the CAGE (Reference Mayfield, McLeod and HallMayfield et al, 1974) questions to assess current and past alcohol misuse; self-reported use of any illicit (street) drugs, and whether the woman had had difficulty reducing or controlling her drug use; and questions about attempted suicide and episodes of self-harm without suicidal intent. Questions on violence in relationships, unwanted sexual experiences in childhood and adulthood, the person's attitude to being questioned by the general practitioner or practice nurse about domestic violence and sexual abuse, and self-reported criteria for DSM–IV post-traumatic stress disorder (American Psychiatric Association, 1994) were also included. An algorithm was applied to these PTSD data as developed by Breslau et al (Reference Breslau, Peterson and Kessler1999), in which a score of four symptoms or more on a seven-symptom screening scale defined positive cases of PTSD.
Six measures of abusive experience included both physical and sexual abuse in childhood and adulthood. These comprised:
-
(a) domestic violence, defined using the criteria of a previous US survey (Reference McCauley, Kern and KolodnerMcCauley et al, 1997), consisting of an affirmative answer to either (i) one or more of a series of questions involving physical assault, or (ii) an enquiry whether the woman had been forced to have sex by a present or any previous partner (in this study, women were asked whether any of the above had occurred during their lifetime or in the past year);
-
(b) unwanted sexual intercourse with anyone when the respondent was a child (under 16 years old);
-
(c) unwanted sexual activities, but not including sexual intercourse (under age 16 years);
-
(d) severe beating by a parent, step-parent or carer when a child (under age 16 years) on one, or more than one, occasion;
-
(e) rape, at age 16 years or over;
-
(f) sexual assault, but not rape, at age 16 years or over.
Statistical methods
Data analysis was performed using SAS statistical software, version 6.12 (SAS, Institute, 1997). Logistic regression modelling was used to examine the associations between demographic variables and mental health measures. A stepwise procedure with backward elimination was used to select those variables that remained independently associated with the psychiatric outcome of interest. The variables selected by the stepwise procedure were used in subsequent analyses to adjust the associations of abusive experience variables with psychiatric outcome for any significant demographic characteristics.
Odds ratios relative to a baseline category were estimated for the different levels of categorical variables. The values for odds ratios are such that values greater than 1 indicate an increased risk of a psychiatric outcome and values less than 1 a reduced risk.
RESULTS
The survey aimed to recruit 5% of the total number of women registered at each practice and this was achieved in 11 of the 13 practices. Women completed the questionnaire in the waiting room at each practice and were requested not to take it home. During the study period, 2592 women attended; 243 (9%) were not approached because of severe illness or the presence of an infant, and 157 (6%) were ineligible because of language difficulties. Of the 2192 women who were approached in the waiting rooms, 781 (36%) declined to complete the questionnaire; 1411 (64%) consented and were eligible to take part in the survey. However, 204 (9%) eligible women did not complete the questionnaire sufficiently to be included, 169 because they were called to see their doctor or practice nurse. A total of 1207 (55%) of the women approached were finally recruited and completed the questionnaire (Reference Richardson, Coid and PetruckevitchRichardson et al, 2002). Not all items were completed by all responders, so the denominators for the numbers reported below vary.
Demographic characteristics
The ages of the 1207 women respondents ranged from 16 years to 85 years, with a mean age of 37.2 years (s.d.=15.9). A total of 569 (49%) reported that they or their family owned the property in which they lived, and 597 (50%) owned or lived with someone who owned a car. Four hundred and seventeen (35%) were born outside the UK, 634 (54%) were White; 443 (38%) were single, 413 (35%) married, 151 (13%) divorced or separated, 35 (3%) widowed, and 123 (11%) cohabiting; 593 (51%) were currently living with a partner or spouse, 321 (28%) lived alone, and 250 (21%) were living in other circumstances; 730 (61%) had children.
Prevalence of abusive experiences
Experiences of childhood abuse (at age less than 16 years) included 88 (9%) women who reported unwanted sexual intercourse; 116 (11%) unwanted sexual activities, but not intercourse; 48 (5%) severely beaten by a parent or carer on one occasion and 112 (12%) severely beaten more than once; 53 (5%) experiencing both unwanted sexual intercourse and other unwanted sexual activities. Among the women reporting that they had been severely beaten on more than one occasion, 23 (21%) reported experiencing unwanted sexual intercourse and 29 (27%) unwanted sexual activities. A total of 17 (2%) reported all three forms of abusive experience before age 16 years.
Reported adult (16 years and above) abusive and traumatic experiences included 425 (41%) women who fulfilled the study definition for domestic violence, 61 (17%) with more than one partner; 79 (8%) reported that they had been raped; 87 (9%) reported that they had been sexually assaulted (but not raped). Excluding women who reported that they had at some time been forced to have sex by a partner, 33 (4%) reported that they had been raped. The questionnaire did not identify the perpetrator of the rape.
Within the sample surveyed, all childhood abusive experiences were closely interrelated, tending to co-occur in the lives of individual participants: 53 (67%) of the women who had experienced unwanted sexual intercourse prior to age 16 years had also experienced other unwanted sexual activities (OR=30.3; 95% CI 17.7–52.0; P<0.001); 28 (39%) of the same subgroup had been beaten on one or more occasions (OR=3.5; 95% CI 2.1–5.8; P<0.001) and 35 (35%) of women who had experienced unwanted sexual activities (not intercourse) before age 16 years had been severely beaten on one or more occasions (OR=3.0; 95% CI 1.9–4.7; P<0.001). In addition, adult experiences of abuse and trauma co-occurred: 55 (14%) of the women who experienced domestic violence also reported rape (OR=4.7; 95% CI 2.76–8.11; P<0.001); 54 (14%) sexual assault other than rape (OR=3.34; 95% CI 2.06–5.41; P<0.001). Forty-one (59%) women who reported being raped reported other forms of sexual assault (OR=30.03; 95% CI 16.99–53.09; P<0.001) (Reference Coid, Petruckevitch and FederCoid et al, 2001).
Prevalence of psychiatric morbidity
A total of 301 (27%) women scored 11 or more on the anxiety scale, and 105 (9%) scored 11 or more on the depression scale of the HADS; 144 (13%) had made a suicide attempt, and 104 (9%) had deliberately injured themselves, but without suicidal intention; 708 (62%) reported that they drank alcohol. Of this latter subgroup, 209 (30%) had at some time felt that they should cut down on their drinking, 82 (12%) reporting that people had annoyed them by criticising their drinking; 112 (16%) had at some time felt bad or guilty about their drinking, and 46 (6%) had drunk alcohol first thing in the morning to steady their nerves or get rid of a hangover. Within the subgroup of drinkers, 27 (4%) also reported that they had had a problem with their drinking in the past 12 months, 35 (5%) before the past 12 months. Of the total sample of women, 132 (12%) screened positive for alcohol misuse (affirmative response to two or more of the CAGE questions); 222 (20%) women reported that they had at some time used illicit (street) drugs. Of these, 31 (14%, which is 3% of the total sample) had at some time been unable to reduce their use of these drugs. A total of 95 women (8%) were observed to be suffering from PTSD based on the criteria of Breslau et al (Reference Breslau, Peterson and Kessler1999).
Within this population all the mental health measures were closely associated, confirming a high level of comorbidity between anxiety, depression, illicit drug use, alcohol problems, parasuicide, selfharm and PTSD. All associations demonstrated statistical significance at the P<0.001 level, except for depression and illicit use of drugs, for which the association was not significant.
Demographic associations with mental health measures
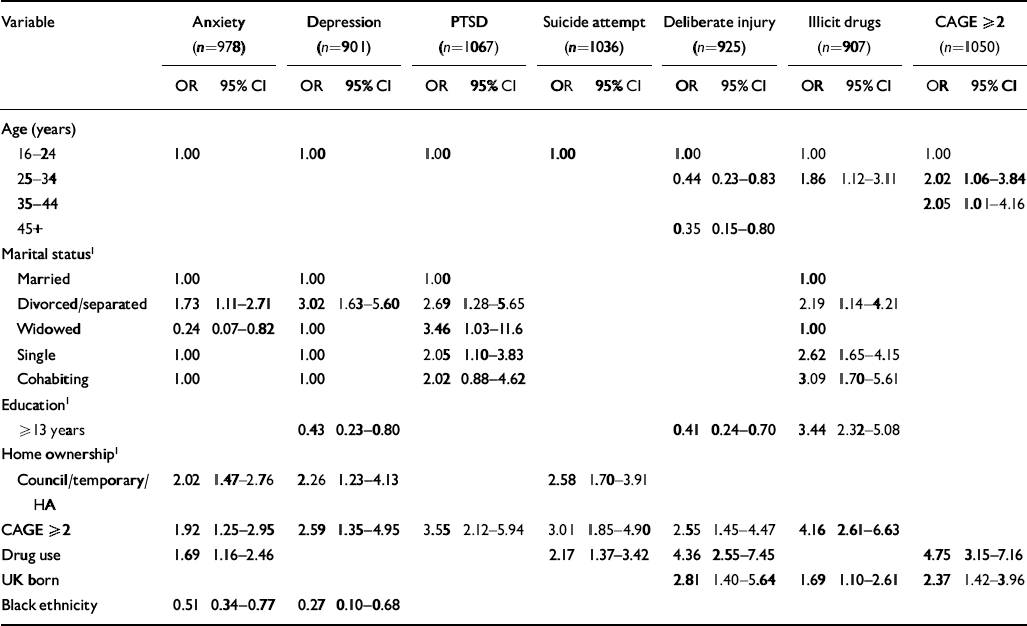
Table 1 shows the independent associations between the demographic characteristics of the women in the survey and mental health measures. All models were adjusted for age, which was significantly associated only with reported use of illicit drugs (more prevalent in the 25–34 year age group), and alcohol misuse (more prevalent between the ages of 25 years and 44 years). Marital status had several important independent associations with mental outcomes: being divorced or separated was independently associated with anxiety, depression, PTSD and illicit drug use. Illicit drug use was also associated with single marital status and cohabitation. Being widowed was associated with a lower prevalence of anxiety.
Table 1 Demographic variables independently associated with mental health outcomes for women primary care attenders
| Variable | Anxiety (n=978) | Depression (n=901) | PTSD (n=1067) | Suicide attempt (n=1036) | Deliberate injury (n=925) | Illicit drugs (n=907) | CAGE ≥ 2 (n=1050) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | |
| Age (years) | ||||||||||||||
| 16-24 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | |||||||
| 25-34 | 0.44 | 0.23-0.83 | 1.86 | 1.12-3.11 | 2.02 | 1.06-3.84 | ||||||||
| 35-44 | 2.05 | 1.01-4.16 | ||||||||||||
| 45+ | 0.35 | 0.15-0.80 | ||||||||||||
| Marital status1 | ||||||||||||||
| Married | 1.00 | 1.00 | 1.00 | 1.00 | ||||||||||
| Divorced/separated | 1.73 | 1.11-2.71 | 3.02 | 1.63-5.60 | 2.69 | 1.28-5.65 | 2.19 | 1.14-4.21 | ||||||
| Widowed | 0.24 | 0.07-0.82 | 1.00 | 3.46 | 1.03-11.6 | 1.00 | ||||||||
| Single | 1.00 | 1.00 | 2.05 | 1.10-3.83 | 2.62 | 1.65-4.15 | ||||||||
| Cohabiting | 1.00 | 1.00 | 2.02 | 0.88-4.62 | 3.09 | 1.70-5.61 | ||||||||
| Education1 | ||||||||||||||
| ≥ 13 years | 0.43 | 0.23-0.80 | 0.41 | 0.24-0.70 | 3.44 | 2.32-5.08 | ||||||||
| Home ownership1 | ||||||||||||||
| Council/temporary/HA | 2.02 | 1.47-2.76 | 2.26 | 1.23-4.13 | 2.58 | 1.70-3.91 | ||||||||
| CAGE ≥ 2 | 1.92 | 1.25-2.95 | 2.59 | 1.35-4.95 | 3.55 | 2.12-5.94 | 3.01 | 1.85-4.90 | 2.55 | 1.45-4.47 | 4.16 | 2.61-6.63 | ||
| Drug use | 1.69 | 1.16-2.46 | 2.17 | 1.37-3.42 | 4.36 | 2.55-7.45 | 4.75 | 3.15-7.16 | ||||||
| UK born | 2.81 | 1.40-5.64 | 1.69 | 1.10-2.61 | 2.37 | 1.42-3.96 | ||||||||
| Black ethnicity | 0.51 | 0.34-0.77 | 0.27 | 0.10-0.68 | ||||||||||
Having further education (more than 13 years) was associated with self-reported use of illicit drugs, but was negatively associated with depression and deliberate self-injury. Living in council or temporary accommodation was associated with anxiety, depression and a history of parasuicide. Women who had been born in the UK were more likely to have deliberately injured themselves and used illicit drugs than women born outside the UK. Black women were less likely to suffer from anxiety or depression than other ethnic groups.
Associations between abusive experiences and mental health measures
Table 2 demonstrates the independent associations between abusive experiences reported by the women and seven mental health outcomes after adjusting for significant demographic characteristics. Bivariate analyses showed associations with all mental health measures. Following logistic regression, however, neither form of childhood sexual abuse was associated with any of the mental health measures, except for PTSD where women reporting sexual activities before age 16 years were five times more likely to be rated as a PTSD sufferer. However, being beaten by a parent or carer in childhood was strongly and independently associated with several measures: beating on more than one occasion was independently associated with anxiety, depression, PTSD, parasuicide and deliberate self-injury, but not drug or alcohol misuse. Table 2 also highlights the influence of this repetitive form of childhood physical maltreatment. The odds ratios are higher for those reporting beating on more than one occasion.
Table 2 Independent associations between childhood maltreatment, adult abusive experiences and mental health outcomes for women primary care attenders

| Variable | Anxiety1 (n=679) | Depression2 (n=629) | PTSD3 (n=716) | Suicide attempt4 (n=719) | Deliberate injury5 (n=716) | Illicit drugs6 (n=641) | CAGE ≥ 27 (n=718) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Adjusted OR | 95% CI | Adjusted OR | 95% CI | Adjusted OR | 95% CI | Adjusted OR | 95% CI | Adjusted OR | 95% CI | Adjusted OR | 95% CI | Adjusted OR | 95% CI | |
| Sexual activity before age 16 years | 1.12 | 0.56-2.23 | 1.61 | 0.56-4.66 | 5.40 | 2.50-11.7 | 1.71 | 0.63-3.83 | 1.32 | 0.58-2.99 | 1.97 | 0.99-3.90 | 1.72 | 0.83-3.55 |
| Sexual intercourse before age 16 years | 1.09 | 0.45-2.63 | 0.23 | 0.05-1.00 | 0.56 | 0.19-1.61 | 2.32 | 0.94-5.75 | 1.42 | 0.56-3.61 | 1.37 | 0.58-3.24 | 0.54 | 0.21-1.36 |
| Beaten once | 2.69 | 1.19-6.05 | 1.54 | 0.45-5.32 | 1.37 | 0.41-4.59 | 2.24 | 0.82-6.11 | 1.75 | 0.56-5.44 | 0.99 | 0.37-2.67 | 1.03 | 0.35-3.03 |
| Beaten more than once | 3.89 | 2.16-7.01 | 2.34 | 1.00-5.47 | 3.62 | 1.74-7.56 | 4.74 | 2.44-9.19 | 2.99 | 1.42-6.31 | 1.03 | 0.53-2.00 | 1.37 | 0.67-2.80 |
| Sexual assault aged 16+ years | 0.49 | 0.21-1.13 | 1.32 | 0.42-4.16 | 1.07 | 0.39-2.91 | 1.08 | 0.43-2.72 | 1.43 | 0.59-3.45 | 2.69 | 1.30-5.59 | 2.61 | 1.25-5.46 |
| Raped aged 16+ years | 2.18 | 0.97-4.88 | 2.71 | 0.91-8.05 | 3.95 | 1.51-10.3 | 4.41 | 1.80-10.8 | 2.30 | 0.89-5.92 | 1.75 | 0.74-4.15 | 1.75 | 0.75-4.07 |
| Domestic violence (ever) | 3.31 | 2.25-4.86 | 2.76 | 1.41-5.41 | 3.27 | 1.73-6.18 | 2.18 | 1.27-3.73 | 1.40 | 0.77-2.52 | 2.19 | 1.41-3.41 | 2.44 | 1.48-4.02 |
Independent associations between sexual abuse in adulthood and mental health problems also differed according to the severity of the experience. Table 2 shows contrasts between the odds ratios for sexual assault and rape and individual mental health measures: independent associations with sexual assault included illicit drug and alcohol misuse, but not anxiety, depression, PTSD, parasuicide or deliberate self-injury; rape was independently associated with PTSD and parasuicide, but not with anxiety, depression, deliberate self-injury, or misuse of drugs or alcohol.
Women experiencing domestic violence were more likely to report all forms of psychiatric morbidity except for deliberate self-injury. The effect of current abuse was examined by separating women who reported domestic violence in the past 12 months from those who reported it only in the period prior to the past 12 months. Adjusted odds ratios demonstrated stronger associations with most mental health measures for domestic violence occurring during the past 12 months than for violence occurring prior to the past 12 months, including anxiety (OR=3.6, 95% CI 2.2–6.0 v. OR=2.4, 95% CI 1.5–3.9), depression (OR=3.9, 95% CI 1.7–8.5 v. OR=2.1, 95% CI 0.9–4.6), PTSD (OR=2.52, 95% CI 1.15–5.52 v. OR=1.94, 95% CI 0.91–4.14), parasuicide (OR=2.23, 95% CI 1.14–4.38 v. OR=1.95, 95% CI 1.01–3.75) and alcohol misuse (OR=2.58, 95% CI 1.39–4.79 v. OR=1.86, 95% CI 1.04–3.33), but with associations in the opposite direction for illicit drug use (OR=1.83, 95% CI 1.01–3.33 v. OR=2.52, 95% CI 1.49–4.24).
DISCUSSION
Our study measured a broad range of lifetime abusive experiences and psychiatric measures in a large sample, from a random sample of general practice populations. Non-English speakers were included and there was no indication of a systematic bias in response that might have distorted associations between abuse and mental health. However, the study did not take into account other important aetiological factors that might have acted independently or in combination with factors we measured to determine psychiatric morbidity, including low parental care and high control, and parental indifference and neglect (Reference Bifulco, Brown and HarrisBifulco et al, 1987). Another potential limitation of our study is the recruitment of participants from primary care. There is evidence that primary care attenders have higher reported prevalences of childhood abuse and depression (Reference Newman, Clayton and ZuelligNewman et al, 2000).
Although a cross-sectional survey cannot determine the direction of causation in adulthood, we found strong associations between certain abusive experiences in both childhood and adulthood and adult mental ill health. Furthermore, we observed important differential effects between individual abusive experiences at different stages in a woman's life and over her lifetime on the mental health measures. Severity and repetition of certain abusive experiences also led to increased levels of association with psychiatric morbidity.
Child maltreatment
In contrast to previous research, our study demonstrated that childhood abuse in the form of a severe beating by a parent or carer was independently associated with several adverse mental health measures, whereas childhood sexual abuse was not associated. These findings also confirmed a dose–response relationship between repetition of physical abuse and anxiety, depression, PTSD, parasuicide and other deliberate self-harm. There is an important divergence between our findings and other studies which found associations between childhood sexual abuse and psychiatric morbidity in adulthood (Reference Bagley and RamsayBagley & Ramsay, 1986; Reference Burnam, Stein and GoldingBurnam et al, 1988; Reference Mullen, Romans-Clarkson and WaltonMullen et al, 1988; Reference Peters, Wyatt and PowellPeters, 1988; Reference Stein, Golding, Siegel, Wyatt and PowellStein et al, 1988; Reference Winfield, George and SwartzWinfield et al, 1990; Reference Bifulco, Brown and AdlerBifulco et al, 1991; Reference Bushnell, Wells and Oakley-BrowneBushnell et al, 1992; Reference Mullen, Martin and AndersonMullen et al, 1993; Reference Fergusson, Horwood and LynskeyFergusson et al, 1996; Reference Kessler, Davis and KendlerKessler et al, 1997; Reference Hill, Davis and ByattHill et al, 2000). It is possible that our measures of childhood sexual abuse were insufficiently precise and were different from several of these studies. We obtained our sample from a primary care setting in the community and did not carry out clinical interviews with the participants to explore in depth the nature of their abusive experiences. However, previous studies might have missed a confounding effect of childhood physical abuse, either by not measuring it (Reference Mullen, Romans-Clarkson and WaltonMullen et al, 1988; Reference Bushnell, Wells and Oakley-BrowneBushnell et al, 1992; Reference Fergusson, Horwood and LynskeyFergusson et al, 1996) or by not including it in a logistic regression model (Reference Bagley and RamsayBagley & Ramsay, 1986; Reference Mullen, Martin and AndersonMullen et al, 1993; Reference Fergusson, Horwood and LynskeyFergusson et al, 1996; Reference Hill, Davis and ByattHill et al, 2000), although some controlled for childhood neglect (Reference Bifulco, Brown and AdlerBifulco et al, 1991; Reference Mullen, Martin and AndersonMullen et al, 1993; Reference Fergusson, Horwood and LynskeyFergusson et al, 1996; Reference Kessler, Davis and KendlerKessler et al, 1997). Our results are concordant with a study by Mulder et al (Reference Mulder, Beautrais and Joyce1998), which found a relationship between childhood physical abuse and adult dissociative symptoms but did not find an association with childhood sexual abuse. Similarly, Ernst et al (Reference Ernst, Angst and Foldenyi1993) found that adult depression was more strongly associated with a range of early familial risk factors, including physical abuse, than with early sexual abuse.
We did not make any prior assumption that childhood sexual abuse was the primary abusive experience associated with the psychopathological symptoms measured in adulthood. The analysis in our study assumed that all abusive experiences had an equal chance of association with these measures. As there was a high level of diagnostic comorbidity, and a marked tendency for the abusive experiences to co-occur over the lifetime for certain participants, it was essential to examine the differential associations. In doing so, the effect of childhood sexual abuse on adult mental health proved to be considerably less important than we had expected.
Associations between childhood sexual abuse and measures of morbidity in previous studies may not reflect causation. Social, family and contextual factors associated with childhood sexual abuse and increased risk of adult psychopathological disorder may have been confounded because childhood sexual abuse is more prevalent in dysfunctional families, with impaired parent–child relationships and parental psychopathology (Reference Mullen, Martin and AndersonMullen et a 1994; Reference Paradise, Rose and SleeperParadise et al, 1994; Reference Stern, Lynch and OatesStern et al, 1995; Reference Fergusson, Horwood and LynskeyFergusson et al, 1996). Associations between childhood sexual abuse and certain forms of adult psychiatric disorder could have been due to these factors (of which severe beating by carers constituted an additional and more important component) rather than a result of direct effects of sexual abuse. However, studies that have examined the severity of sexual abuse, indicated by attempted or completed penetration, long duration, and where physical violence and restraint are an integral part, tend to show an association with later psychopathological disorder (Reference Mullen, Martin and AndersonMullen et al, 1993; Reference Fergusson, Horwood and LynskeyFergusson et al, 1996; Reference Dinwiddie, Heath and DunneDinwiddie et al, 2000; Reference Bulik, Prescott and KendlerBulik et al, 2001).
An alternative hypothesis could be tested in future research which might explain the absence of the expected association. Both childhood physical and sexual abuse substantially and independently increase the risks of further physical and sexually abusive experiences in adulthood (Reference Coid, Petruckevitch and FederCoid et al, 2001). The apparent associations found in studies that have not measured adult abusive experiences could therefore be confounded within a three-stage process, in which the childhood abusive experience independently leads to the adult abusive experience, which in turn independently leads to adult psychopathological disorder.
Sexual assault and rape in adulthood
Sexual violence towards women in adulthood contrasted with sexually abusive experiences in childhood in demonstrating associations with the mental health outcomes. The more severe experience of rape in adulthood demonstrated stronger associations than sexual assault. Associations between sexual assault (but not rape) and substance misuse are consistent with other studies, suggesting that although substance misuse may be associated with unwanted physical and sexual experience in adulthood, this is independent of childhood abusive experiences (Reference Merrill, Newell and ThomsonMerrill et al, 1999). It is possible that women who had experienced sexual assault (but not rape) continued to take more risks than women who had been raped. It has been observed that sexual encounters characterised by heavy drinking are more likely to involve sexual aggression (Reference Muehlenhard and LintonMuehlenhard & Linton, 1987). Furthermore, women with more sexual partners may be at increased risk of victimisation through greater contact with a larger number of men who have the potential to become sexually aggressive (Reference Koss and DineroKoss & Dinero, 1989). We did not collect data on the sexual behaviour of respondents to test this hypothesis.
The question remains as to why rape was not associated with substance misuse. There was no difference in the mean age at which rape and sexual assault had occurred in this sample of women, both experiences occurring at a mean age of 21 years. There are two possible explanations. First, women who were raped and women who were sexually assaulted could have constituted two distinct subgroups. This is unlikely, because both experiences cooccurred in the lives of a substantial proportion of the participants, with 59% of those who had been raped reporting that they had been sexually assaulted. Furthermore, the demographic characteristics of women who had experienced these two forms of abuse were similar. The second – more likely – explanation was that rape, which constituted a more serious trauma in the lives of these women, had led to substantial changes in their subsequent lifestyle, as previously observed by Mezey & Taylor (Reference Mezey and Taylor1988). Presenting symptoms soon after rape do not predict outcome. Some women experience severe impairment, including depression (Reference Ellis, Atkeson and CalhounEllis et al, 1981; Reference Nadelson, Notman and ZacksonNadelson et al, 1982), sexual dysfunction (Reference Feldman-Summers, Gordon and MeagherFeldman-Summers et al, 1977), impaired task performance (Burgess & Holmstrom, Reference Burgess and Holmstrom1974a , Reference Burgess and Holmstrom b ; Reference Walker and BrodskyWalker & Brodsky, 1976) and social adjustment (Reference Resick, Culhoun and AtkesonResick et al, 1981). Associations with PTSD and suicide attempts in our respondents who had been raped suggest that many had been unable to resolve and recover from these traumatic experiences, in contrast to women who had been sexually assaulted but not raped. Their psychiatric sequelae are likely to have further impaired their social adjustment, so that they were less likely to engage in social situations that might involve substance misuse. The strong association between parasuicide and rape in this survey underlines the importance of identifying this traumatic experience for future interventions to prevent suicide.
Domestic violence
The findings of our study are generally consistent with a recent meta-analysis of the literature on intimate partner violence and mental disorder, which suggests that depression, parasuicide, PTSD, and alcohol and drug misuse are common among battered women (Reference GoldingGolding, 1999). Domestic violence was associated with a wider range of mental health measures than any other abusive experience in this study. Domestic violence had a stronger association than rape with anxiety and depression. It is possible that these findings were an artefact, in that the trauma of domestic violence had been more recent, or was ongoing, at the time of the survey (Reference McCauley, Kern and KolodnerMcCauley et al, 1995). This contrasted with rape, which had predated the survey by several years for most women and where some may have shown partial resolution of their symptoms. Golding (Reference Golding1999) suggests that depression tends to remit following cessation of violence, and both depression and PTSD are influenced by the severity of women's violent experiences.
The associations between domestic violence and illicit drug use and alcohol misuse are not explained by our study. Substance misuse in this sample could have been the outcome of the domestic violence, but can also be understood in the context of the abusive partner's substance misuse. Substance misuse may become a feature of the couple's relationship, further increasing the risk of violence between them (Reference Giles-Sims, Jasinski and WilliamsGiles-Sims, 1998).
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Women abused in childhood and adulthood are at risk of further abuse. These experiences have differential effects on the women's subsequent adult psychopathological state.
-
▪ Experiencing physical violence from carers during childhood may be a more important risk factor than sexual abuse, depending on its severity.
-
▪ Women should be questioned about ongoing and recent abusive experiences as well as those that occurred in childhood.
LIMITATIONS
-
▪ The cross-sectional method precluded examination of the direction of the associations found in the study.
-
▪ Information on most of these abusive experiences was entirely retrospective.
-
▪ There was limited exploration of the temporal associations between abusive experiences and the onset of psychopathological symptoms.
Acknowledgements
The study was funded by National Health Service Research and Development (North Thames). We thank the practices in east London that allowed us to. recruit in their waiting rooms. Anna Koenig also obtained data. The survey was. piloted at Lower Clapton Group Practice, part of the East London and Essex. Network of Researchers.







eLetters
No eLetters have been published for this article.