Studies reporting on the toxicity of different antidepressants in overdose indicate that, compared with selective serotonin reuptake inhibitors (SSRIs), tricyclic antidepressants, particularly amitriptyline and dothiepin, are associated with an increased risk from overdose (Reference Henry, Alexander and SenerHenry et al, 1995; Reference Shah, Uren and BakerShah et al, 2001). Although this information has aided in the choice of antidepressants prescribed, several questions remain about the profile of toxicity of different antidepressants. First, studies on antidepressant-related deaths have failed to distinguish between accidental deaths and deaths with suicidal intent. Furthermore, no studies have examined whether certain antidepressant drugs are more likely to be used in multiple drug overdoses, particularly in combination with other antidepressants or other psychoactive drugs. With this in mind, the aims of this paper were: to investigate the relative toxicity of the major classes of antidepressant drugs, with the specific objective of assessing the cause of death as either accidental or intentional; and to analyse deaths where other drugs were present in combination with antidepressants.
METHOD
Sources of data
The np-SAD database on drug-related deaths
In July 1997 the National Programme of Substance Abuse Deaths (np-SAD; Reference Ghodse, Oyefeso and WebbGhodse et al, 2002) was established after the Home Office's index of addicts closed. Data are collected from coroners in England and Wales where licit or illicit psychoactive drugs are implicated in death. Coroners supply demographic data and information regarding the drugs implicated in these fatalities.
Prescription cost analysis
Prescription cost analysis provides details on the total quantity, number of prescription items and net ingredient cost of all antidepressant prescriptions dispensed in the community by doctors in England (Department of Health, Statistics Division 1E, Prescription Cost Analysis system) and Wales (Prescribing Services Unit, Health Solutions, Wales) during 1998–2000. Prescriptions written by hospital doctors are also included provided that they were dispensed in the community. Prescription cost analysis uses the concept of the ‘defined daily dose’, which is an international system developed by the World Health Organization, and is defined as ‘the assumed average maintenance dose per day for a drug used on its main indication in adults’. It also collects information on ‘average daily quantity’ for antidepressants, a concept developed by an expert group convened by the Prescribing Support Unit and used to reflect more adequately general practitioner prescribing in England, based on several measures, including defined daily doses and British National Formulary information. Prescription cost analysis does not cover items dispensed in hospitals or on private prescriptions. However, because 90–98% of patients with depression are seen by general practitioners rather than psychiatrists (Reference Thompson and ThompsonThompson & Thompson, 1989; Reference McCarthyMcCarthy, 1993; Reference Donoghue and TyleeDonoghue & Tylee, 1996; Reference Dunn, Donoghue and OzminkowskiDunn et al, 1999; Reference Middleton, Gunnell and WhitleyMiddleton et al, 2001), the exclusion of private prescriptions and hospital-dispensed prescriptions from our analysis should not appreciably affect the outcome of this study.
Study population
The study population consisted of cases reported by coroners in England and Wales to the np-SAD for deaths occurring during the 3-year period 1998–2000. Cases for the study were those who had a current prescription for antidepressant drugs at the time of the fatality and where antidepressant drugs were implicated in the cause of death. Contribution to fatalities is defined by the np-SAD as being when substances are specifically mentioned in the cause of death by the coroner, or when the drug type in the cause of death is not specified (e.g. ‘polydrug toxicity’) but the coroner reports that drugs were present post-mortem. Cases are classified as intentional in the np-SAD database according to the coroner's verdict of ‘suicide’ or ‘open’ where suicide is likely. For the purposes of this study, ‘accidental’ includes deaths by accidental overdose, traumatic accident or acute medical conditions. Cases are also classified as those with or without a drug misuse history.
Data analysis
Antidepressants were assigned to four therapeutic classes according to the British National Formulary: tricyclic antidepressants, monoamine oxidase inhibitors (MAOIs), selective serotonin reuptake inhibitors (SSRIs) and other antidepressant drugs. The antidepressants included in each therapeutic class can be seen in Table 2. For each of the above classes of antidepressant, the following variables were analysed:
-
(a) frequencies of drug mentions per million prescriptions; the observed number of mentions was compared with the expected number of mentions, which was calculated by standardising for the number of prescriptions;
-
(b) frequencies of mentions in deaths by single drug or in combination with other drugs;
-
(c) other drugs most likely to be implicated in deaths in combination with antidepressants;
-
(d) history of drug misuse or dependence;
-
(e) the incidence of antidepressants by class in accidental and intentional deaths.
Statistical analysis
We used prevalence ratios and their 95% confidence intervals (CIs) to compare differences in proportions. Standardised mortality ratios and their 95% CIs were used to compare observed and expected number of deaths when standardised for the number of prescriptions for antidepressant drugs. The χ2 statistical test was used to test for differences between the antidepressant therapies. All analyses were undertaken using the Statistical Package for the Social Sciences for Windows version 1.0 and CLINISTAT (Reference BlandBland, 1990).
RESULTS
Antidepressant classes implicated in death compared with the number of prescriptions
During the study period there were 4167 drug-related deaths, of which 468 had an antidepressant implicated in the deaths. Therefore, 11.2% of all drug-related deaths involved antidepressant drugs. Among the 468 fatalities there were 473 mentions of antidepressants by class implicated in the deaths. A total of 285 cases had a single antidepressant class implicated in the deaths and there were 186 cases where two or more specific drug types were implicated: an antidepressant class and another drug or multiple mentions of antidepressants with or without other drugs. There were 498 mentions of specific antidepressants and there were 10 cases that had a mention of both nortriptyline and amitriptyline. Because nortriptyline is a metabolite of amitriptyline (Reference Sanchez and HyttelSanchez & Hyttel, 1999) these cases were included in fatalities associated with amitriptyline only.
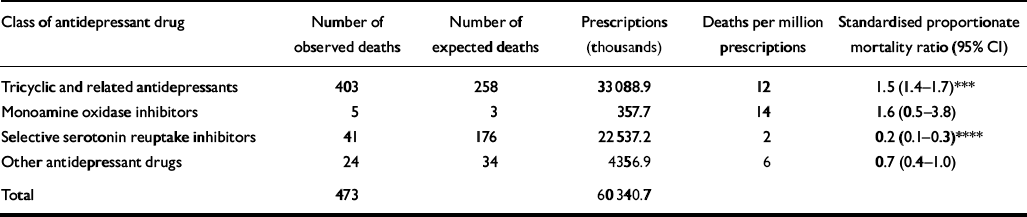
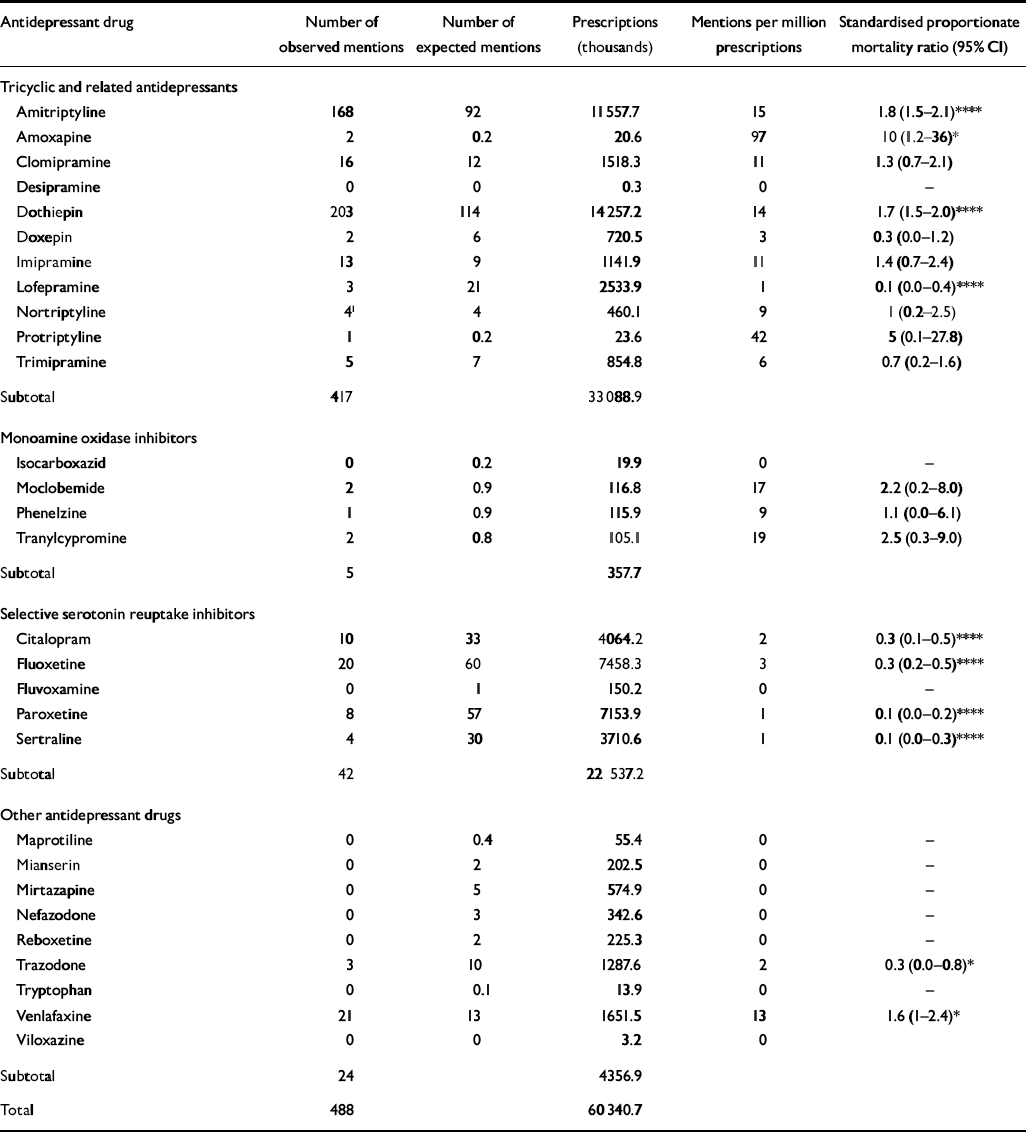
There was a substantial variation in the risk of death from the different antidepressant classes when compared with the number of prescriptions. As can be seen from Table 1, the tricyclics (12 mentions per million prescriptions) and the MAOIs (14 mentions per million prescriptions) had a higher number of mentions per million prescriptions compared with the SSRIs (2 mentions per million prescriptions). The tricyclics prescribed most frequently were dothiepin, amitriptyline and lofepramine. Both dothiepin and amitriptyline were associated with significantly more deaths than would be expected when standardised for the number of prescriptions but lofepramine was associated with significantly fewer mentions. In contrast to amitriptyline and dothiepin, the SSRIs were associated with significantly fewer mentions than would be expected (P<0.0001) when standardised for the number of prescriptions, and this was the case for the four most widely prescribed SSRIs: fluoxetine, paroxetine, citalopram and sertraline (Table 2). For the class of other antidepressant drugs, 88% of fatalities were due to venlafaxine and the remainder were due to trazodone, which was associated with significantly fewer mentions than would be expected (P<0.05) when standardised for the number of prescriptions. Venlafaxine, however, had a mortality rate not dissimilar to that seen with the tricyclics, and there were 13 mentions per million prescriptions of this drug (see Table 2).
Table 1 Number of mentions of antidepressants by class per million prescriptions in England and Wales, 1998-2000
| Class of antidepressant drug | Number of observed deaths | Number of expected deaths | Prescriptions (thousands) | Deaths per million prescriptions | Standardised proportionate mortality ratio (95% CI) |
|---|---|---|---|---|---|
| Tricyclic and related antidepressants | 403 | 258 | 33 088.9 | 12 | 1.5 (1.4-1.7)*** |
| Monoamine oxidase inhibitors | 5 | 3 | 357.7 | 14 | 1.6 (0.5-3.8) |
| Selective serotonin reuptake inhibitors | 41 | 176 | 22 537.2 | 2 | 0.2 (0.1-0.3)**** |
| Other antidepressant drugs | 24 | 34 | 4356.9 | 6 | 0.7 (0.4-1.0) |
| Total | 473 | 60 340.7 |
Table 2 Number of drug mentions by specific drug and per million prescriptions in England and Wales, 1998-2000
| Antidepressant drug | Number of observed mentions | Number of expected mentions | Prescriptions (thousands) | Mentions per million prescriptions | Standardised proportionate mortality ratio (95% CI) |
|---|---|---|---|---|---|
| Tricyclic and related antidepressants | |||||
| Amitriptyline | 168 | 92 | 11 557.7 | 15 | 1.8 (1.5-2.1)**** |
| Amoxapine | 2 | 0.2 | 20.6 | 97 | 10 (1.2-36)* |
| Clomipramine | 16 | 12 | 1518.3 | 11 | 1.3 (0.7-2.1) |
| Desipramine | 0 | 0 | 0.3 | 0 | — |
| Dothiepin | 203 | 114 | 14 257.2 | 14 | 1.7 (1.5-2.0)**** |
| Doxepin | 2 | 6 | 720.5 | 3 | 0.3 (0.0-1.2) |
| Imipramine | 13 | 9 | 1141.9 | 11 | 1.4 (0.7-2.4) |
| Lofepramine | 3 | 21 | 2533.9 | 1 | 0.1 (0.0-0.4)**** |
| Nortriptyline | 41 | 4 | 460.1 | 9 | 1 (0.2-2.5) |
| Protriptyline | 1 | 0.2 | 23.6 | 42 | 5 (0.1-27.8) |
| Trimipramine | 5 | 7 | 854.8 | 6 | 0.7 (0.2-1.6) |
| Subtotal | 417 | 33 088.9 | |||
| Monoamine oxidase inhibitors | |||||
| Isocarboxazid | 0 | 0.2 | 19.9 | 0 | — |
| Moclobemide | 2 | 0.9 | 116.8 | 17 | 2.2 (0.2-8.0) |
| Phenelzine | 1 | 0.9 | 115.9 | 9 | 1.1 (0.0-6.1) |
| Tranylcypromine | 2 | 0.8 | 105.1 | 19 | 2.5 (0.3-9.0) |
| Subtotal | 5 | 357.7 | |||
| Selective serotonin reuptake inhibitors | |||||
| Citalopram | 10 | 33 | 4064.2 | 2 | 0.3 (0.1-0.5)**** |
| Fluoxetine | 20 | 60 | 7458.3 | 3 | 0.3 (0.2-0.5)**** |
| Fluvoxamine | 0 | 1 | 150.2 | 0 | — |
| Paroxetine | 8 | 57 | 7153.9 | 1 | 0.1 (0.0-0.2)**** |
| Sertraline | 4 | 30 | 3710.6 | 1 | 0.1 (0.0-0.3)**** |
| Subtotal | 42 | 22 537.2 | |||
| Other antidepressant drugs | |||||
| Maprotiline | 0 | 0.4 | 55.4 | 0 | — |
| Mianserin | 0 | 2 | 202.5 | 0 | — |
| Mirtazapine | 0 | 5 | 574.9 | 0 | — |
| Nefazodone | 0 | 3 | 342.6 | 0 | — |
| Reboxetine | 0 | 2 | 225.3 | 0 | — |
| Trazodone | 3 | 10 | 1287.6 | 2 | 0.3 (0.0-0.8)* |
| Tryptophan | 0 | 0.1 | 13.9 | 0 | — |
| Venlafaxine | 21 | 13 | 1651.5 | 13 | 1.6 (1-2.4)* |
| Viloxazine | 0 | 0 | 3.2 | 0 | |
| Subtotal | 24 | 4356.9 | |||
| Total | 488 | 60 340.7 |
Antidepressants in combination with other drugs implicated in mortality
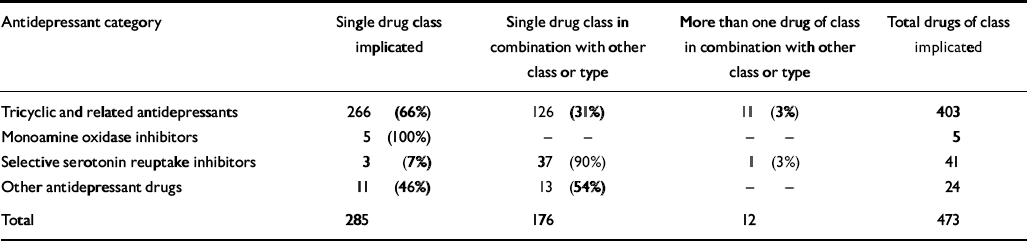
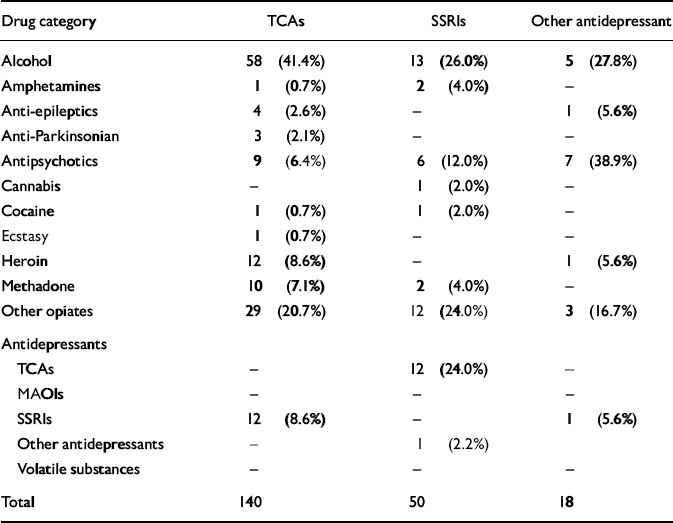
Of 468 deaths in which antidepressant drugs were implicated, 60% had antidepressants solely implicated in death, whereas antidepressants in combination with other drugs were implicated in 40% of cases. There was a significant relationship between whether antidepressants were implicated alone or in combination with other drugs and the type of antidepressant (χ2=55.39, P<0.0001), and antidepressant-related fatalities involving multiple drug mentions were almost three times more likely to occur in SSRI-related cases than in tricyclic-related cases (percentage ratio=2.7, 95% CI 2.3–3.2; see Table 3). As can be seen from Table 4, the most frequently mentioned drugs in combination with SSRIs were alcohol (26%), tricyclic antidepressants (24%) and other opiates (24%). Antipsychotics (12%) were also implicated. When tricyclics were found in combination with other drugs in antidepressant-related deaths, the other drugs most likely to be implicated were alcohol (41.4%), other opiates (20.7%), SSRIs (8.6%), heroin (8.6%) and methadone (7.1%). A different profile emerged for the class of other antidepressants, where antipsychotics (38.9%), alcohol (27.8%) and other opiates (16.7%) were most likely to be found in combination.
Table 3 Classes of antidepressant drugs implicated in deaths between 1998 and 2000 either alone or in combination with other drugs
| Antidepressant category | Single drug class implicated | Single drug class in combination with other class or type | More than one drug of class in combination with other class or type | Total drugs of class implicated |
|---|---|---|---|---|
| Tricyclic and related antidepressants | 266 (66%) | 126 (31%) | 11 (3%) | 403 |
| Monoamine oxidase inhibitors | 5 (100%) | - - | - - | 5 |
| Selective serotonin reuptake inhibitors | 3 (7%) | 37 (90%) | 1 (3%) | 41 |
| Other antidepressant drugs | 11 (46%) | 13 (54%) | - - | 24 |
| Total | 285 | 176 | 12 | 473 |
Table 4 Frequencies of antidepressants by class associated with other common psychoactive drugs and other antidepressants1
| Drug category | TCAs | SSRIs | Other antidepressant |
|---|---|---|---|
| Alcohol | 58 (41.4%) | 13 (26.0%) | 5 (27.8%) |
| Amphetamines | 1 (0.7%) | 2 (4.0%) | - |
| Anti-epileptics | 4 (2.6%) | - | 1 (5.6%) |
| Anti-Parkinsonian | 3 (2.1%) | - | - |
| Antipsychotics | 9 (6.4%) | 6 (12.0%) | 7 (38.9%) |
| Cannabis | - | 1 (2.0%) | - |
| Cocaine | 1 (0.7%) | 1 (2.0%) | - |
| Ecstasy | 1 (0.7%) | - | - |
| Heroin | 12 (8.6%) | - | 1 (5.6%) |
| Methadone | 10 (7.1%) | 2 (4.0%) | - |
| Other opiates | 29 (20.7%) | 12 (24.0%) | 3 (16.7%) |
| Antidepressants | |||
| TCAs | - | 12 (24.0%) | - |
| MAOIs | - | - | - |
| SSRIs | 12 (8.6%) | - | 1 (5.6%) |
| Other antidepressants | - | 1 (2.2%) | |
| Volatile substances | - | - | - |
| Total | 140 | 50 | 18 |
Drug misuse status of antidepressant-implicated deaths
Deaths related to antidepressant use in combination with other drugs were more likely to occur among drug misuse cases than non-drug misuse cases (χ2=20.87, P<0.0001). However, among these ‘combination’ deaths there was no evidence that being a drug misuser was related to a particular class of antidepressant (χ2=1.55, P=0.4).
Accidental and intentional antidepressant deaths
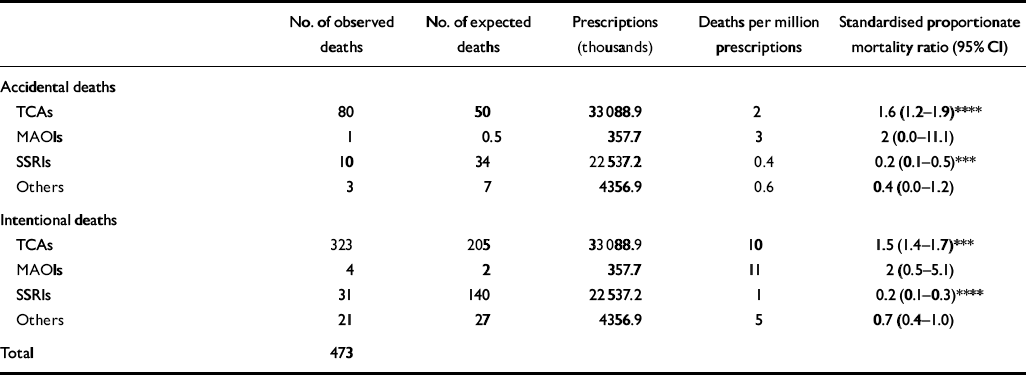
As can be seen from Table 5, 20% of mentions were associated with accidental deaths whereas 80% of mentions were associated with intentional deaths, suggesting that most deaths from antidepressant drugs are due to suicide. Tricyclic antidepressants are associated with a higher number of accidental and intentional deaths, and significantly more accidental (P<0.0001) and intentional (P<0.001) deaths were observed with the tricyclics than would be expected when standardised for the number of prescriptions. The SSRIs were associated with significantly fewer accidental (P<0.0001) and intentional (P<0.0001) deaths than would be expected when standardised for the number of prescriptions. For the other antidepressant drugs there was no significant difference between the number of observed and expected mentions when standardised for the number of prescriptions. Finally, there was no evidence of a relationship between type of antidepressant and the occurrence of an intentional or accidental death.
Table 5 Frequencies of drug mentions by class in accidental and intentional deaths
| No. of observed deaths | No. of expected deaths | Prescriptions (thousands) | Deaths per million prescriptions | Standardised proportionate mortality ratio (95% CI) | |
|---|---|---|---|---|---|
| Accidental deaths | |||||
| TCAs | 80 | 50 | 33 088.9 | 2 | 1.6 (1.2-1.9)**** |
| MAOIs | 1 | 0.5 | 357.7 | 3 | 2 (0.0-11.1) |
| SSRIs | 10 | 34 | 22 537.2 | 0.4 | 0.2 (0.1-0.5)*** |
| Others | 3 | 7 | 4356.9 | 0.6 | 0.4 (0.0-1.2) |
| Intentional deaths | |||||
| TCAs | 323 | 205 | 33 088.9 | 10 | 1.5 (1.4-1.7)*** |
| MAOIs | 4 | 2 | 357.7 | 11 | 2 (0.5-5.1) |
| SSRIs | 31 | 140 | 22 537.2 | 1 | 0.2 (0.1-0.3)**** |
| Others | 21 | 27 | 4356.9 | 5 | 0.7 (0.4-1.0) |
| Total | 473 |
DISCUSSION
Fatalities related to tricyclic antidepressants
The present study suggests that up to 80% of deaths from antidepressants are suicides, and confirms previous findings that the tricyclics most likely to be implicated in antidepressant-related deaths are amitriptyline and dothiepin. Although the antidepressant properties of tricyclics are attributed to their ability to inhibit both noradrenalin and serotonin reuptake, it has been suggested that the increased toxicity of these drugs in overdose may be due to modulation of ion channel function within the myocardium. Indeed the tricyclics, particularly amitriptyline, have been associated with the inhibition of both cardiac sodium (Na+) channels and potassium (K+) channels, which is associated with an increased risk of cardiac arrthymias and sudden death (Reference Freeman, Mundy and BeattieFreeman et al, 1969; Reference Marshall and ForkerMarshall & Forker, 1982; Reference Ma and HenryMa & Henry, 2001; Reference Witchel, Hancox and NuttWitchel et al, 2003). Lofepramine was the only tricyclic associated with a lower incidence of mortality. Although the mechanism of the lower toxicity of this drug has yet to be clarified, its membrane-stabilising activities (which may increase the risk of cardiac arrthythmias) are much lower than those of amitriptyline and desipramine (Reference Darcy, Kelly and LeonardDarcy et al, 2002).
Fatalities related to selective serotonin reuptake inhibitors
In contrast to amitriptyline and dothiepin, this study clearly suggests that the SSRIs when taken on their own are safer in overdose and are less likely to be implicated in both intentional and accidental deaths. In addition to the treatment of depression, antidepressant drugs have been used for many other indications. In particular, SSRIs have been used in the treatment of generalised anxiety disorders, obsessive–compulsive disorders, social phobia, premenstrual dysphoric disorder and post-traumatic stress disorder (Reference Ables and BaughmanAbles & Baughman, 2003). Because these disorders are likely to carry a lower risk of suicide than depressive illnesses, this could also account for the reduced toxicity of these drugs in overdose. The present study suggests that when SSRIs are implicated in death they are mostly found in combination with other drugs, especially with tricyclics. In clinical practice, augmentation therapy involving the prescription of an antidepressant alongside another antidepressant drug of the same or different pharmacological class has largely been used in patients with treatment-resistant depression or in patients who only partially respond to antidepressants (Reference FavaFava, 2001). Therefore, a possible explanation for the increased number of combination deaths with SSRIs is that these individuals were suffering from a treatment-resistant depression and tricyclics may have been prescribed concurrently, accounting for the fatal outcome. The SSRIs have been shown also to differ in the extent of their inhibition of the cytochrome P-450 enzymes of the liver, which are crucial in the metabolism of numerous drugs (Reference RichelsonRichelson, 1997), raising the possibility of drug–drug interactions in patients taking multiple medications. Enzyme CYP2D6 is considered the principal P-450 cytochrome enzyme in the clearance of tricyclics, and data from in vitro studies suggest that the rank order of potency for inhibition of CYP2D6 by antidepressants is paroxetine ≥ fluoxetine > sertraline > fluvoxamine > venlafaxine > mirtazapine (Reference VaughanVaughan, 1988; Reference Crewe, Lennard and TuckerCrewe et al, 1992). Therefore, it is possible that by inhibiting CYP2D6 the SSRIs may increase plasma levels of tricyclics, thereby increasing the toxic effects associated with these drugs. This could be an explanation for the present findings of increased risk of death from SSRIs in combination with tricyclics, although the data at present do not seem to support this hypothesis because higher rates of deaths involving SSRIs such as fluoxetine and paroxetine were not found. Although we do not know what percentage of the combination deaths from SSRIs and tricyclics occurred as a result of prescription within the normal clinical guidelines, the present findings do suggest that the clinical efficacy of augmentation therapy in SSRI-resistant patients should be monitored carefully because of the risk of suicide.
Antidepressant-related deaths and drug misuse
The present study is the first to demonstrate that cases involving antidepressants with other drugs are significantly more likely to involve drug addicts. The other drugs that are most likely to be implicated in combination with the antidepressants were alcohol and opiate-based drugs. These findings suggest that general practitioners and psychiatrists should screen for drug use/misuse patterns in patients being prescribed antidepressants and should prescribe cautiously for these individuals.
Venlafaxine-related fatalities
This study suggests that, of the miscellaneous group of antidepressants, venlafaxine may be more toxic in overdose than other drugs in this class. This finding supports evidence from a recent study published by Buckley & McManus (Reference Buckley and McManus2002). Venlafaxine is a serotonin and noradrenalin reuptake inhibitor and at low doses is very similar to SSRIs in that it predominantly inhibits the reuptake of serotonin, although at higher doses noradrenalin reuptake inhibition is predominant. Furthermore, recent case studies have suggested a link between cardiac illness/failure and venlafaxine, and there is evidence that this drug blocks Na+ channels (Reference Blythe and HackettBlythe & Hackett, 1999; Reference Khalifa, Daleau and TurgeonKhalifa et al, 1999; Reference Reznik, Rosen and RosenReznik et al, 1999; Reference Drent, Singh and GorgelsDrent et al, 2003). However, the other drugs most likely to be found in combination with venlafaxine were antipsychotics, which were implicated in 38.9% of cases in this group. The higher rate of antipsychotic prescribing with venlafaxine suggests that a different patient group may have been involved, possibly the seriously depressed or dual-diagnosis patients who are difficult to treat and possibly at a greater risk from suicide.
Limitations and summary
It is important to note that there are several reasons apart from the toxicity of antidepressant medication that can lead to a fatal overdose. These include treatment-resistant depression, non-response to the antidepressant therapy, medication non-compliance, duration of illness, history of antidepressant treatments and undertreatment of depression. Previously it has been suggested that in primary care practice tricyclic antidepressants are frequently prescribed at doses below those that are shown to be efficacious in randomised controlled clinical trials (Reference Donoghue and TaylorDonoghue & Taylor, 2000), with studies showing that up to 88% of patients receiving tricyclics were on doses below those recommended in the national guidelines (Reference Donoghue and TyleeDonoghue & Tylee, 1996). However, a recent meta-analysis of randomised controlled clinical trials comparing the effects of low-dose and standard-dose tricyclics suggests that low dosage regimes are more effective than placebo in the treatment of depression, and may or may not be as effective as standard dosage regimes but that the drop-out rate is lower because they produce fewer side-effects (Reference Furukawa, McGuire and BarbuiFurukawa et al, 2002). This is in contrast to the SSRIs, which are associated with the lowest level of mortality and are almost always prescribed at efficacious doses in primary care settings (Reference Donoghue and TyleeDonoghue & Tylee, 1996; Reference Dunn, Donoghue and OzminkowskiDunn et al, 1999). Furthermore, not all coroners report to the np-SAD database, although the response rate from the coroners in England and Wales has been estimated to be as high as about 95% (Reference Oyefeso, Ghodse and ClancyOyefeso et al, 1999). Despite these limitations, the present study clearly suggests that, although tricyclic antidepressants are more toxic in overdose, the SSRIs are largely implicated in death in combination with other drugs, especially tricyclics, suggesting either a treatment-resistant depression or non-response to pharmacotherapy. Therefore, suicide risk should be monitored carefully when augmentation therapy is used in SSRI-resistant patients. Furthermore, all patients prescribed antidepressants should be screened routinely for a history of drug use/misuse.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Because 80% of deaths from antidepressants are intentional, suicide risk needs to be monitored carefully in all patients prescribed antidepressant drugs.
-
▪ Although selective serotonin reuptake inhibitors (SSRIs) are safer in overdose than the tricyclic antidepressants, deaths in which SSRIs are implicated are most likely to be in combination with other drugs, particularly tricyclics. Therefore, the efficacy and safety of augmentation therapy in SSRI-resistant patients should be monitored carefully.
-
▪ Deaths in which antidepressants are implicated in combination with other drugs are more likely to happen in drug misusers. Therefore, all patients prescribed antidepressants should be screened routinely for a history of drug use/misuse.
LIMITATIONS
-
▪ Because not all coroners report to the National Programme of Substance Abuse Deaths database, the number of deaths in which antidepressant drugs are implicated is likely to be underestimated.
-
▪ Factors other than the antidepressant medication, such as medication non-compliance, undertreatment of depression and non-response to antidepressant therapy, may have led to the fatal outcome.
-
▪ Toxicology reports on the quantity of drug detected at post-mortem examination were not available.










eLetters
No eLetters have been published for this article.