Approximately a fifth of people over 55 years old have mental disorders unrelated to the normal ageing process (Reference MalmgrenMalmgren, 1994). Older people have the highest suicide rate of any group, reaching 20 per 100 000 at age 85 years in the USA. In France rates are particularly high, reaching 148 per 100 000 for men and 24 per 100 000 for women over 85 years old. Consumption of psychotropic drugs is four times higher than in neighbouring European countries, reaching 23% to 39% according to region (Reference Allard, Artero and RitchieAllard et al, 2003). The Enquête de Santé Psychologique - Risques, Incidence et Traitement (ESPRIT) Project is the first longitudinal study of psychiatric disorder undertaken in France; its principal aim is the construction of a comprehensive database incorporating clinical, biological, genetic and environmental risk factors. The first results reported here estimate prevalence in order to determine whether rates of psychiatric morbidity are indeed higher in France than elsewhere.
METHOD
Participants were recruited from people aged 65 years and over living in the community, by random selection from the 15 electoral rolls of the Montpellier district between March 1999 and February 2001. Of the people initially drawn at random, more than a quarter (27.3%) did not participate (of these, 3.3% were excluded owing to severe disability). Those who refused to participate were replaced by another person drawn at random from the same electoral division, so that each division was equally represented. Those who refused were slightly older and more likely to be living alone than those who agreed. A total of 1873 persons were included in the study.
Participants were asked to attend a half-day examination at the Gui de Chauliac Neurology Hospital (with taxi transport where necessary), to undergo the assessments described below. Housebound participants were examined at home by a nurse and neurologist with training in psychogeriatrics. In each case the neurologist contacted the person's general practitioner, permitting verification of information where necessary. This paper reports results obtained from the psychiatric examination only.
Health interview
A standardised health interview covered present state of health; individual and family medical history; medication use (participants were asked to bring their medication to the centre); past and present hormonal therapy for women; exposure to adverse environmental factors (including pesticides, electromagnetic fields, anaesthesia, adverse life events); and sleep disorders. Exposure to adverse life events was assessed using the Gospel Oak questionnaire (Reference Harwood, Prince and MannHarwood et al, 1998). The Activities of Daily Living (ADL; Reference Katz, Ford and MoskowitzKatz et al, 1963), Instrumental Activities of Daily Living (IADL; Reference LawtonLawton, 1988) and the Rosow & Breslau (Reference Rosow and Breslau1966) scales were completed for assessment of disabilities.
Neurological examination
A standardised neurological examination based on ICD-10 criteria (World Health Organization, 1992) was used to detect possible organic causes of behavioural disorder. The examination also included measures of sitting and standing blood pressure and a cognitive examination.
Psychiatric interview
A standardised psychiatric interview was used to investigate lifetime and current psychiatric disorder; this was the Mini International Neuropsychiatric Interview (MINI, French version 5.00), previously validated within the general population setting (Reference Lecrubier, Sheehan and WeillerLecrubier et al, 1997). This interview, which has been widely used in many clinical and research settings in France, provides an extensive symptomatological examination. Diagnostic algorithms may then be applied to assess ‘caseness’. The interviewers (nurses or psychologists) were trained using video recordings of interviews by the clinicians responsible for the development of the French version of the MINI. Following training, the interviewers administered the examination over a 1-month period under the supervision of psychiatrists in the department of adult psychiatry at Montpellier University. Regular meetings were conducted with clinicians to discuss problems, and dual interviews were randomly conducted to minimise interviewer ‘drif’. Cases detected by the MINI, i.e. those meeting DSM-IV criteria (American Psychiatric Association, 1994), were reviewed at the research site by an international panel of three psychiatrists and a psychologist, taking into account the observations of the neurologist and the participant's medication and medical history, in order to validate the initial diagnosis. The MINI explores lifetime and current DSM-IV Axis I psychiatric disorders, and a pilot study conducted on 20 persons by two of the ESPRIT interviewers within a geriatric hospital showed it to be well accepted, even by extremely old and frail people and by those with mild cognitive impairment. In the case of mild cognitive or sensory difficulties the MINI is administered with the assistance of a close relative or carer. The MINI does not use a hierarchical approach and comorbidity was recorded under each disorder. Severity of anxiety and depressive symptoms was examined using the State and Trait versions of the Spielberger Anxiety Scales (Reference SpielbergerSpielberger, 1983) and the Center for Epidemiologic Studies - Depression (CESD) scale (Reference RadloffRadloff, 1977). Interviews were occasionally conducted in tandem to reduce drift.
Biological measures
Stress reactivity was measured by cortisol levels taken over 2 days, one stressful and one non-stressful, and blood samples were taken at home on the day after the clinical examination to constitute a specimen (serum, plasma, DNA). The results of these analyses are not reported here.
RESULTS
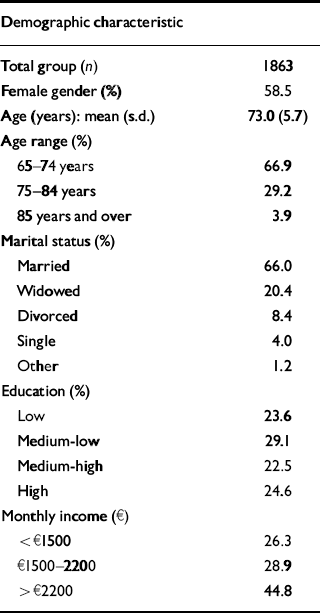
Of the 1873 persons examined, 10 were excluded from the analyses because of moderate or severe dementia (diagnosed by the neurologist) as they were unable to provide adequate information. Cases of early dementia and mild cognitive impairment were retained, with information being verified by the family and general practitioner. The mean age of the whole sample was 73 (s.d.=6) years and it comprised 58.5% women and 41.5% men. Regional data on 5-year-band age distribution suggest that the sample corresponded closely to the actual population up to age 80 years, but there was underrepresentation of those aged over 80. The socio-demographic characteristics of the sample are given in Table 1.
Table 1 Characteristics of the study population
| Demographic characteristic | |
|---|---|
| Total group (n) | 1863 |
| Female gender (%) | 58.5 |
| Age (years): mean (s.d.) | 73.0 (5.7) |
| Age range (%) | |
| 65–74 years | 66.9 |
| 75–84 years | 29.2 |
| 85 years and over | 3.9 |
| Marital status (%) | |
| Married | 66.0 |
| Widowed | 20.4 |
| Divorced | 8.4 |
| Single | 4.0 |
| Other | 1.2 |
| Education (%) | |
| Low | 23.6 |
| Medium-low | 29.1 |
| Medium-high | 22.5 |
| High | 24.6 |
| Monthly income (€) | |
| <€1500 | 26.3 |
| € 1500–2200 | 28.9 |
| >€ 2200 | 44.8 |
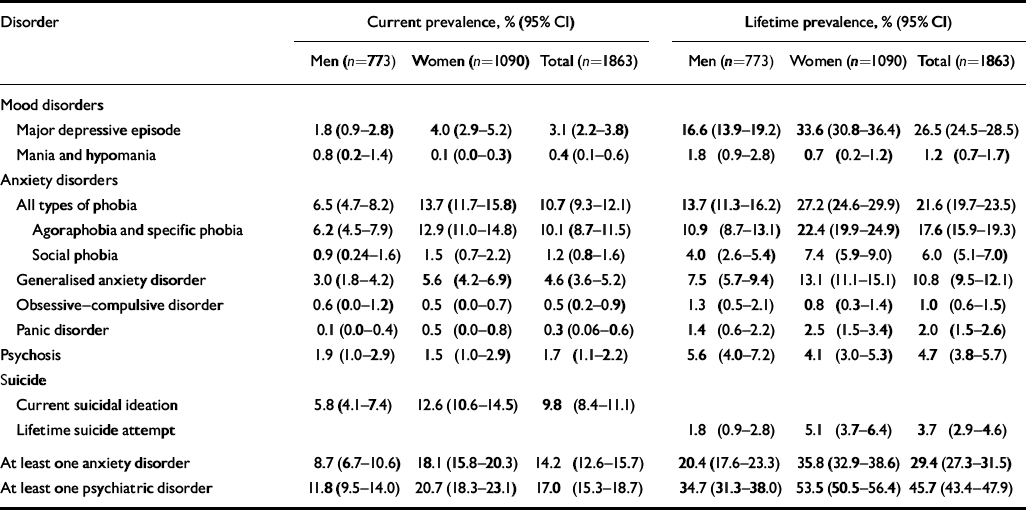
Table 2 gives current and lifetime prevalence rates and confidence intervals for each DSM-IV disorder in men and women. Overall, 45.7% of the population sampled had experienced at least one psychiatric disorder in their lifetime and 17.4% were currently suffering from such a disorder. Anxiety disorders were the most frequent, with a lifetime prevalence of 29.4%, and a lifetime history of mood disorders was reported by 26.5% of the sample. Comorbidity rates are given in Table 3.
Table 2 Current and lifetime prevalence of DSM-IV psychiatric disorders in elderly men and women
| Disorder | Current prevalence, % (95% CI) | Lifetime prevalence, % (95% CI) | ||||
|---|---|---|---|---|---|---|
| Men (n=773) | Women (n=1090) | Total (n=1863) | Men (n=773) | Women (n=1090) | Total (n=1863) | |
| Mood disorders | ||||||
| Major depressive episode | 1.8 (0.9-2.8) | 4.0 (2.9-5.2) | 3.1 (2.2-3.8) | 16.6 (13.9-19.2) | 33.6 (30.8-36.4) | 26.5 (24.5-28.5) |
| Mania and hypomania | 0.8 (0.2-1.4) | 0.1 (0.0-0.3) | 0.4 (0.1-0.6) | 1.8 (0.9-2.8) | 0.7 (0.2-1.2) | 1.2 (0.7-1.7) |
| Anxiety disorders | ||||||
| All types of phobia | 6.5 (4.7-8.2) | 13.7 (11.7-15.8) | 10.7 (9.3-12.1) | 13.7 (11.3-16.2) | 27.2 (24.6-29.9) | 21.6 (19.7-23.5) |
| Agoraphobia and specific phobia | 6.2 (4.5-7.9) | 12.9 (11.0-14.8) | 10.1 (8.7-11.5) | 10.9 (8.7-13.1) | 22.4 (19.9-24.9) | 17.6 (15.9-19.3) |
| Social phobia | 0.9 (0.24-1.6) | 1.5 (0.7-2.2) | 1.2 (0.8-1.6) | 4.0 (2.6-5.4) | 7.4 (5.9-9.0) | 6.0 (5.1-7.0) |
| Generalised anxiety disorder | 3.0 (1.8-4.2) | 5.6 (4.2-6.9) | 4.6 (3.6-5.2) | 7.5 (5.7-9.4) | 13.1 (11.1-15.1) | 10.8 (9.5-12.1) |
| Obsessive-compulsive disorder | 0.6 (0.0-1.2) | 0.5 (0.0-0.7) | 0.5 (0.2-0.9) | 1.3 (0.5-2.1) | 0.8 (0.3-1.4) | 1.0 (0.6-1.5) |
| Panic disorder | 0.1 (0.0-0.4) | 0.5 (0.0-0.8) | 0.3 (0.06-0.6) | 1.4 (0.6-2.2) | 2.5 (1.5-3.4) | 2.0 (1.5-2.6) |
| Psychosis | 1.9 (1.0-2.9) | 1.5 (1.0-2.9) | 1.7 (1.1-2.2) | 5.6 (4.0-7.2) | 4.1 (3.0-5.3) | 4.7 (3.8-5.7) |
| Suicide | ||||||
| Current suicidal ideation | 5.8 (4.1-7.4) | 12.6 (10.6-14.5) | 9.8 (8.4-11.1) | |||
| Lifetime suicide attempt | 1.8 (0.9-2.8) | 5.1 (3.7-6.4) | 3.7 (2.9-4.6) | |||
| At least one anxiety disorder | 8.7 (6.7-10.6) | 18.1 (15.8-20.3) | 14.2 (12.6-15.7) | 20.4 (17.6-23.3) | 35.8 (32.9-38.6) | 29.4 (27.3-31.5) |
| At least one psychiatric disorder | 11.8 (9.5-14.0) | 20.7 (18.3-23.1) | 17.0 (15.3-18.7) | 34.7 (31.3-38.0) | 53.5 (50.5-56.4) | 45.7 (43.4-47.9) |
Table 3 Rates of psychiatric comorbidity

| Current comorbid condition, % (n) | |||||
|---|---|---|---|---|---|
| At least one cormorbid condition | Major depressive episode | Generalised anxiety disorder | All types of phobia | Suicidal ideation | |
| Major depressive episode (n=58) | 70.7 (41) | 22.4 (13) | 34.5 (20) | 48.3 (28) | |
| Generalised anxiety disorder (n=84) | 46.4 (39) | 15.5 (13) | 32.1 (27) | 28.6 (24) | |
| All types of phobia (n=199) | 29.1 (58) | 10.1 (20) | 13.6 (27) | 17.1 (34) | |
| Suicidal ideation (n=182) | 34.1 (62) | 15.4 (28) | 13.2 (24) | 18.7 (34) | |
Mood disorders
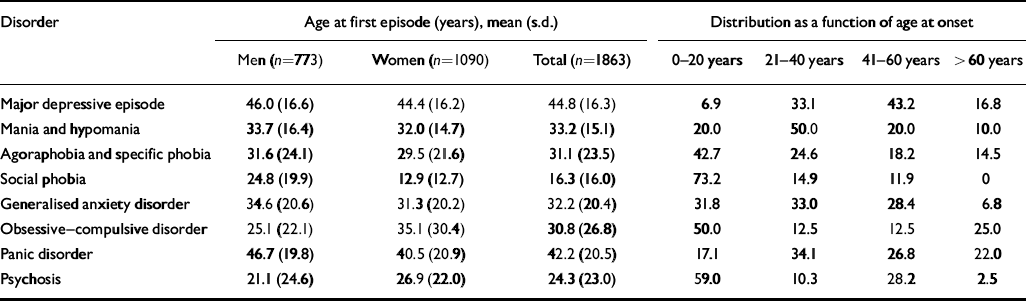
The prevalence of current (during the past 15 days) depressive illness in the Montpellier district was 3.1% and the lifetime prevalence of major depression was 26.5%. Both lifetime and current prevalence were twice as high in women than in men. Around 10% admitted to current suicidal ideation (during the past month) and 3.7% had made at least one suicide attempt. Table 4 shows the mean age at first-reported episode for each psychiatric disorder. In order to distinguish between late-onset and early-onset disorders, prevalence rates are also given according to the period of onset (under 20 years, 21-40 years, 41-60 years, 61 years and over) roughly corresponding to periods of childhood and adolescence, young adulthood, old adulthood and old age.
Table 4 Mean age at first reported episode for each psychiatric disorder and distribution as a function of age at onset
| Disorder | Age at first episode (years), mean (s.d.) | Distribution as a function of age at onset | |||||
|---|---|---|---|---|---|---|---|
| Men (n=773) | Women (n=1090) | Total (n=1863) | 0-20 years | 21-40 years | 41-60 years | > 60 years | |
| Major depressive episode | 46.0 (16.6) | 44.4 (16.2) | 44.8 (16.3) | 6.9 | 33.1 | 43.2 | 16.8 |
| Mania and hypomania | 33.7 (16.4) | 32.0 (14.7) | 33.2 (15.1) | 20.0 | 50.0 | 20.0 | 10.0 |
| Agoraphobia and specific phobia | 31.6 (24.1) | 29.5 (21.6) | 31.1 (23.5) | 42.7 | 24.6 | 18.2 | 14.5 |
| Social phobia | 24.8 (19.9) | 12.9 (12.7) | 16.3 (16.0) | 73.2 | 14.9 | 11.9 | 0 |
| Generalised anxiety disorder | 34.6 (20.6) | 31.3 (20.2) | 32.2 (20.4) | 31.8 | 33.0 | 28.4 | 6.8 |
| Obsessive-compulsive disorder | 25.1 (22.1) | 35.1 (30.4) | 30.8 (26.8) | 50.0 | 12.5 | 12.5 | 25.0 |
| Panic disorder | 46.7 (19.8) | 40.5 (20.9) | 42.2 (20.5) | 17.1 | 34.1 | 26.8 | 22.0 |
| Psychosis | 21.1 (24.6) | 26.9 (22.0) | 24.3 (23.0) | 59.0 | 10.3 | 28.2 | 2.5 |
Mean age at first major depressive episode was 44.8 years, and was similar for men and women. There is a progressive increase in the proportion of first episodes of major depression up to age 60 years. In more than 76% of the diagnosed cases of major depression, the age of onset was 21-60 years; however, late episodes are not uncommon, since 16.8% of first episodes occurred after age 60 years. The current prevalence rate for manic episodes is 0.4%, and 1.2% of participants had experienced an episode during their lifetime. Prevalence rates in men were 2.6 and 8 times higher than those in women for current and lifetime episodes, respectively. For both men and women, the mean age at first manic episode was 33.2 years and first onset of mania appeared more frequently before age 40 years (only one case of mania was reported after age 60, in a man).
Anxiety disorders
The prevalence of all anxiety disorders in the cohort has been estimated to be 14.2% and 29.4% for current (during the past month) prevalence. Phobia was the most prevalent anxiety disorder, currently affecting 10.7% of the cohort (1.2% of these phobias were classified as social phobia). The lifetime prevalence of phobia was 21.6% (social phobia 6%). The prevalence of current generalised anxiety disorder in the cohort has been estimated at 4.6%. Lifetime generalised anxiety disorder accounted for 10.8% of total psychiatric disorders. Generalised anxiety and phobia states are seen to be almost twice as common in women than in men for both current and lifetime prevalence. Obsessive-compulsive disorders were diagnosed in 0.5% of the population; lifetime prevalence was 1%, with a slightly higher prevalence in men (1.3%) than in women (0.8%). Current panic attacks were found in 0.3% of the cohort, principally in women, and the lifetime prevalence rate for panic disorder was 2%. All anxiety disorders had their mean age of onset primarily before the age of 50 years in this population (mean age at first episode is generally 31-42 years). Earlier median ages at illness onset are found only for social phobia (16.3 years), which occurs much earlier than other phobias (31.1 years). The first episode generally occurred at the same age or slightly earlier for women than for men except for social phobia. Irrespective of the type of phobia, for both men and women there was a gradual decline with age in the proportion of first episodes. Regarding social phobia, most of the episodes (73.2%) occurred before age 20 years, and after age 60 years there was no case of social phobia onset, whereas a significant proportion of agoraphobia (14.5%) occurred after age 60 years. Generalised anxiety disorder follows a different pattern: there is roughly the same proportion (around 30%) of first episodes in each of the age ranges 20, 20-40 years and 40-60 years, and only 6.8% of onset occurs after age 60 years. For obsessive-compulsive disorder, the first episode occurred later in women (35.1 years) than in men (25.1 years) and half of the participants experienced their first episode before the age of 20 years. In contrast, irrespective of gender, 61% of panic first episodes occurred between the ages of 21 years and 60 years, and a large proportion (22%) occurred after age 60 years.
Psychosis
Psychosis as defined by the MINI refers to the presence of delusions, hallucinations and thought disorder, permitting a DSM-IV diagnosis of schizophrenia and mood disorder with psychotic features. The lifetime prevalence of psychosis in the Montpellier study was 4.7%, and 1.7% of the study sample currently suffered from this disorder. A slightly higher prevalence was observed for men than for women (differing by less than 1.4-fold). The mean age at onset was 24 years, with an earlier onset for men than for women (21 years v. 26.9 years). Most of the participants (especially men) had their onset primarily before the age of 20 years, and after age 60 years there was only one case of first onset (male).
DISCUSSION
This first general population survey of the full range of DSM-IV psychiatric disorders in elderly people in France reveals that almost half (45.7%) of the population have experienced a mental disorder in their lifetime, and around 4% have made a suicide attempt. More than 17% of the population studied were currently suffering from a psychiatric disorder, excluding dementia. These high rates globally concur with the results of the Epidemiologic Catchment Area (ECA) study (Reference Robins and RegierRobins & Regier, 1991), which reported a 6-month prevalence rate of 20% for the same disorders in people aged over 55 years, and also with those of the National Comorbidity Survey, in which nearly half of respondents reported at least one lifetime disorder and there was a 1-year prevalence rate of 30% in adults (Reference Kessler, McGonagle and ZhaoKessler et al, 1994).
Mood disorders
Major depression is the most frequent mood disorder reported by other studies in Western cultures, with variable lifetime prevalence rates ranging from 3-7% using the DSM-III version of the Diagnostic Interview Schedule (DIS; Reference Robins, Helzer and WeissmanRobins et al, 1984) to 15-19% using DSM-III-R and the Composite International Diagnostic Interview (CIDI; Reference Lepine, Lellouch and LovellLepine et al, 1989; Reference Kessler, McGonagle and ZhaoKessler et al, 1994). Using DSM-IV criteria for depression, Forsell et al (Reference Forsell, Jorm and von Strauss1995) reported a 7.9% prevalence of major depressive episode in Swedish nonagenarians. In the Montpellier district (using DSM-IV criteria) we noted a significantly higher lifetime prevalence of major depression: 26.5%. The current prevalence rate of 3.1% is, however, comparable with rates reported elsewhere in Europe, which range between 2% and 4.3%, and also in the USA (1-3.8%).
There are few reports of the prevalence of manic disorder in elderly people. It has been estimated that episodes of mania occur in less than 2% of the elderly population (0-2.2%) (Reference Robins, Helzer and WeissmanRobins et al, 1984; Reference Kessler, McGonagle and ZhaoKessler et al, 1994; Reference AngstAngst, 1995) with no reported gender differences (Reference Kessler, McGonagle and ZhaoKessler et al, 1994). In our study the current prevalence rate was in the same range (0.4%), with a higher prevalence in men than in women, although the numbers are too small to draw conclusions on this point. First onset of mania appeared more frequently before age 40 years, and after age 60 years only one case of mania was diagnosed (a man).
Suicide attempts and suicidal ideation
Seventy-six per cent of the diagnosed cases of major depression had their onset between the ages of 21 and 60 years. Given the relatively higher rates of suicide, especially among older men in France, it is possible that the lifetime prevalence of major depression at higher ages reported here are underestimates due to suicide-related mortality. The suicide rates in the Languedoc-Roussillon region of France where this study was conducted (3.9% for men and 1% for women) are twice the national rates (2% and 0.6%). Our study shows a high rate of current suicidal ideation - 9.8% compared with the estimated 0.7-1.2% reported from the USA by Callahan et al (Reference Callahan, Hendrie and Nienaber1996). In Sweden, Skoog et al (Reference Skoog, Aevarsson and Beskow1996) noted an increase of suicidal ideation in people aged over 85 years (9.6% in men and 18.7% in women). Findings in our Montpellier sample were similar, with rates of suicidal ideation over the past month in people aged over 80 years of 11.3% for men and 21.4% for women. During their lifetime, 3.7% of our cohort had made at least one suicide attempt, and this was 2.8 times more frequent for women than for men. This gender difference may be due to a survival effect, as men make attempts that are more seriously life-threatening.
Anxiety disorders
Anxiety disorders are the most common psychiatric disorders in this elderly population. In the present study, the prevalence of all anxiety disorders has been estimated at 14.2% and 29.4% for current and lifetime prevalence, respectively. Other epidemiological surveys also reveal that up to 30% of individuals will experience an anxiety disorder in their lifetime (Reference Robins, Helzer and WeissmanRobins et al, 1984; Reference Kessler, McGonagle and ZhaoKessler et al, 1994). In our sample, phobias were the most common anxiety disorder, generalised anxiety disorder was relatively common and obsessive-compulsive disorder and panic were quite rare. The MINI only deals with agoraphobia and social phobia. The differential diagnosis between agoraphobia and specific phobia is sometimes difficult to establish, and we have thus not distinguished between these disorders, although social phobia was estimated separately. The lifetime prevalence for phobia was 21.6% with 6% corresponding to social phobia. Around 11% of participants were currently experiencing phobias.
Previously reported prevalences for phobic disorders are highly variable - from 0.7% to 12% for current rates (Reference Krasucki, Howard and MannKrasucki et al, 1998) - essentially because of the use of different diagnostic systems, through different hierarchical diagnostic rules and severity criteria (Reference Lindesay and BanerjeeLindesay & Banerjee, 1993; Reference Krasucki, Howard and MannKrasucki et al, 1998). More specifically, estimates of prevalence for agoraphobia vary from 1% to 8% (Reference Robins, Helzer and WeissmanRobins et al, 1984; Reference Kessler, McGonagle and ZhaoKessler et al, 1994; Reference Manela, Katona and LivingstonManela et al, 1996). The lowest prevalence figures probably result from the combination of the use of DSM-III hierarchical exclusion criteria in the DIS, which require that agoraphobia not be diagnosed in the presence of major depressive disorder, and a different threshold for caseness resulting from the use of different anxiety instruments. On the other hand, the agoraphobia dimension on the Anxiety Disorder Scale includes two items - fear of being with and fear of meeting other people - that could be construed as establishing the presence of social phobia rather than agoraphobia (Reference Krasucki, Howard and MannKrasucki et al, 1998).
There is also considerable variation in prevalence findings for social phobia, from fairly low rates of 2-3% (Reference Robins, Helzer and WeissmanRobins et al, 1984) to considerably higher estimates (13-16%; Reference Kessler, McGonagle and ZhaoKessler et al, 1994; Reference Manela, Katona and LivingstonManela et al, 1996; Reference Lecrubier, Wittchen and FaravelliLecrubier et al, 2000). The lowest estimates, notably found in the ECA study (0.6%), are probably an underestimation due to the use of the DSM-III version of the DIS, which assessed only a limited range of social fears as part of the ‘simple phobia’ section. This problem has been corrected in the World Health Organization's CIDI, and the lifetime prevalence of social phobia in the general population is estimated to be at least 7% (Reference Lecrubier, Wittchen and FaravelliLecrubier et al, 2000). Unfortunately, as yet there are few (if any) exhaustive epidemiological studies using DSM-IV diagnostic criteria.
In our survey, lifetime generalised anxiety disorder accounted for 10.8% of total psychiatric disorders, which is higher than the 4-6% generally reported (Reference Robins, Helzer and WeissmanRobins et al, 1984; Reference Kessler, McGonagle and ZhaoKessler et al, 1994). We estimated the prevalence of current generalised anxiety disorder at 4.6%, which corresponds to the highest rates reported elsewhere (generally between 1% and 4.7%; see for review Reference Krasucki, Howard and MannKrasucki et al, 1998). Obsessive-compulsive disorder was diagnosed in 0.5% of our population and its lifetime prevalence was 1%. Other European and US studies report comparable rates for current (0.1-1.5%) and lifetime 1-3% prevalence (Reference Robins, Helzer and WeissmanRobins et al, 1984; Reference Copeland, Dewey and WoodCopeland et al, 1987; Reference Bland, Newman and OrnBland et al, 1988). Current panic attacks were found in 0.3% of the cohort. The lifetime prevalence for panic disorder was 2%, which is in the 0.1-3.5% range reported by other epidemiological studies (Reference Robins, Helzer and WeissmanRobins et al, 1984; Reference Copeland, Dewey and WoodCopeland et al, 1987; Reference Bland, Newman and OrnBland et al, 1988; Reference Lepine, Lellouch and LovellLepine et al, 1989; Reference Kessler, McGonagle and ZhaoKessler et al, 1994; Reference Krasucki, Howard and MannKrasucki et al, 1998).
Generalised anxiety disorder is generally reported to be rare in adolescence and early adulthood and more common in older adults, especially women aged 50-79 years (Reference Krasucki, Howard and MannKrasucki et al, 1998; Reference PigottPigott, 1999). The peak incidence for panic disorder generally occurs in men aged 18-44 years, and slightly later in women (30-64 years), whereas in those aged over 65 years, no new case has been reported (Reference Krasucki, Howard and MannKrasucki et al, 1998). This contrasts with our population, in whom an equal distribution (around 30%) of onset of the disorder was observed in the 0-20, 21-40 and 41-60 year age groups, and in whom a constant sustained rate for panic disorder was observed even after age 60 years. This could result from the fact that this elderly population had been exposed to several successive wars between 1914 and 1962: the First World War for the oldest, the Second World War for all of them, the war in Indochina for a small proportion, and for more than a quarter of our population, the Algerian conflict. This could also explain the high lifetime prevalence rates observed for most mood and anxiety disorders in this population. Unfortunately, regional statistics do not record the proportion of the population resettled from postwar Algeria, and thus it is not known to what extent this might constitute a risk factor specific to this region. In subsequent waves of the study, detailed information was obtained on war exposure, early life events and immigration, which may help us to determine the relative weight of such risk factors in disease onset. In our sample we observed similar rates for mood and anxiety disorders (around 30%); however, point prevalence rates were quite different, with 5% of participants currently manifesting mood disorders and 15% currently suffering from anxiety disorders. This might be due to differential attrition rates in depression across the life span (in particular through suicide), and/or more successful current treatment of depression.
Psychosis
The lifetime and current prevalence rates for psychosis are 1.7% and 4.7% respectively, and in 70% of cases onset was before the age of 40 years. Little information is available concerning the prevalence of psychotic episodes in elderly people. These rates are much higher than the 0.6% found in the ECA study (Reference Robins and RegierRobins & Regier, 1991). Training sessions with the MINI suggested that the module concerning psychoses caused the most problems. Although in some cases indirect validation was possible by reference to treatment, these questions posed the most difficulty for the interviewees. The clinical panel found that most people reporting psychotic symptoms were also classified by the neurological examination as having mild cognitive impairment (a pre-dementia syndrome). Follow-up of these individuals will allow us to determine whether the current psychotic symptoms recorded by interviewers on the MINI were in fact dementia-related neuropsychiatric signs.
Gender differences
In our sample there was a general trend for a female predominance in depression (but not in mania) and in anxiety disorders (except obsessive-compulsive disorder), which has also been reported in US and European studies (Reference Robins, Helzer and WeissmanRobins et al, 1984; Reference Lepine, Lellouch and LovellLepine et al, 1989; Reference Kessler, McGonagle and ZhaoKessler et al, 1994; Reference Krasucki, Howard and MannKrasucki et al, 1998), and an age-related decline for some anxiety disorders (especially phobia). This downward age-related trend could be due to an excess anxiety-related mortality (for example from suicide, or from cardiovascular or cerebrovascular causes) and could possibly contribute to the lower prevalence in men than in women (Reference Krasucki, Howard and MannKrasucki et al, 1998). Numbers are too small to examine gender differences in psychotic disorder.
Study limitations and future research
The study has a number of shortcomings which might have led us to underestimate the true prevalence: institutionalised elderly people were not included; registration on the electoral roll is voluntary, and no information is available on non-registered populations (which may include a large number of residents who have moved to the region, and illegal immigrants); and there was undersampling of the oldest age group, in which suicide rates are highest. Although costly cross-sectional population studies are now considered to add little to current knowledge, longitudinal observations of mental disorder are still undertaken in almost all European countries to permit monitoring of changes in prevalence, to develop dynamic models of disease onset, establish causality, describe patterns of care utilisation and to assess the impact of therapeutic innovations (Reference Ritchie and MannRitchie & Mann, 2001). This first French prospective epidemiological study of psychiatric disorders in elderly people shows a very high lifetime prevalence of major depression, and relatively high rates of current generalised anxiety disorder and phobia. Longitudinal follow-up of this population will permit the construction of aetiological hypotheses concerning the causes of psychiatric disorder in elderly people, to determine whether these high rates of morbidity may be attributed to biological determinants, environmental exposures or differences in clinical management.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The lifetime prevalence of major depression appears to be higher in France than that reported in other general population studies in Western countries.
-
▪ Four per cent of the study population reported a suicide attempt and 10% had persistent suicidal ideation.
-
▪ Seventeen per cent of elderly people in France are currently suffering from psychiatric disorders, of which generalised anxiety disorder and phobia are the most common.
LIMITATIONS
-
▪ Sampling methods might have led to an underestimation of current prevalence.
-
▪ Many participants had experienced the Algerian war, which might have increased the rates of psychiatric order compared with those in other generations or regions of France.
-
▪ Data were not obtained for people living in institutions.
Acknowledgements
The ESPRIT Project is financed by the regional government of. Languedoc—Roussillon and an unconditional grant from Novartis.









eLetters
No eLetters have been published for this article.