A great deal of research has been carried out into violence among psychiatric in-patients (Reference FottrellFottrell, 1980; Reference ShepherdShepherd, 2001). When managing violence, staff have a number of techniques available to deal with an incident, such as psychological interventions, giving emergency medication and using physical restraint or seclusion (Reference Drinkwater, Gudjonsson, Howells and HollinDrinkwater & Gudjonsson, 1989). There are a number of factors that are likely to determine what techniques staff apply when managing violent incidents but the possible influence of ethnic background of the violent patient has been little researched (Reference Gudjonsson, Rabe-Hesketh and WilsonGudjonsson et al, 2000). This is important because some ethnic minority groups, particularly those of African–Caribbean origin, are more frequently arrested, imprisoned or detained in a psychiatric hospital following offending behaviour (Reference Coid, Kahtan and GaultCoid et al, 2000; Reference Farrington and ShepherdFarrington, 2001). In one study carried out in south London, the ethnic differences in compulsory psychiatric admission to hospital were found to be independent of psychiatric diagnosis and sociodemographic differences (Reference Davies, Thornicroft and LeeseDavies et al, 1996), with Black Caribbean and Black African patients being overrepresented. There is also some evidence that Black patients may be managed differently by nursing staff when involved in an ‘untoward incident’ (Reference Flaherty and MeagherFlaherty & Meagher, 1980; Reference Gudjonsson, Rabe-Hesketh and WilsonGudjonsson et al, 2000). Our hypothesis was that ethnic differences would be found in the management of the patients after a violent incident, but that these differences would, at least in part, be explained by other variables such as the patient's age, gender, the nature and circumstances of the violence, the extent of injuries inflicted, Mental Health Act 1983 status and staff perceptions of the patient's disturbance and potential danger.
METHOD
The study consisted of an analysis of ‘untoward’ incident forms completed over a period of three years (1994, 1996 and 1998) within the Maudsley and Bethlem Royal Hospitals in south London. For the 3-year period there was a total of 4464 untoward incidents recorded. The focus in this paper is on violent incidents on the 14 general adult wards, representing over one-third of all the violent incidents recorded in the two hospitals.
Each untoward incident in the hospital is recorded on a standard hospital incident form by a member of staff. Details include the name of the patient involved, location of incident, date, time of day, type of incident (e.g. violence, arson, self-harm), extent of injury inflicted (none apparent, minor, major), age, gender and ethnic background of the patient and the target of the assault. It is also recorded whether it was thought that the ‘incident had potential for being dangerous irrespective of the actual nature of the injury’. A brief description of the antecedents to the incident is recorded (including any contributory factors, warning signs and causes), as well as what happened during the incident (threat of violence, violence towards others or property) and the outcome (including how the incident was resolved). As far as management of the incident is concerned, it is noted whether emergency medication was given, whether physical restraint was used and whether the patient was secluded.
Self-injurious behaviour and suicide attempts (i.e. violence towards self) were excluded from the analysis, because the focus of the study was on aggression towards others or towards property.
Statistical analysis
The main research question is whether there are differences in the management of Black patients involved in violent incidents compared with White patients and, if so, whether these are present after adjusting for confounders treated as covariates. Three management decisions were considered - medication, restraint and seclusion - each rated as yes (1) or no (0). For each of these variables, logistic regression was used to estimate the odds ratio that the corresponding decision was taken for Black patients compared with White patients after adjusting for covariates. Each patient could contribute several incidents to the analysis and the corresponding management decisions are likely to be correlated owing to unobserved patient-specific variables such as the patient's personality. The models therefore included a random effect for patients representing this effect of unobserved patient-specific variables on the management decision (e.g. Reference Diggle, Liang and ZegerDiggle et al, 1994). The resulting model is a mixed logistic regression model with a normally distributed random effect for patients and fixed effects for Black v. White, Other v. White and the other covariates. All analyses were carried out in Stata 7 (StataCorp, 2001).
Initially, the unadjusted difference between Black and White patients was tested. The other variables were then considered for entry in the model in blocks, starting with other demographics, then antecedents and, finally, incident-specific variables:
-
(a) ethnicity: Black, White, Other or missing;
-
(b) other demographics: gender, age, diagnosis, section type;
-
(c) antecedent: interaction with others, staff denial of a patient request, patient described as agitated, patient attempting to abscond, no warning;
-
(d) incident-specific: perception of potential danger, injury inflicted, drug or alcohol described as a contributory factor, target of assault (nurse, patient, other person, property), type of violence (threat of violence, actual violence, damage to property).
For each block, a forward selection procedure with a 5% level of significance was used for including variables in the model, retaining all variables selected from previous blocks.
RESULTS
Incidents
Most (1515; 34%) of the 4464 untoward incidents recorded were on the 14 general adult wards, 1380 (31%) were in learning disability, 756 (17%) were on the children's wards, 256 (6%) were on the specialist wards, 256 (6%) were on the forensic wards, 195 (4%) were on wards for the elderly, 76 (2%) were community based and 29 (<1%) were on the addiction wards.
Patient characteristics
The 1515 incidents on the 14 general wards involved 422 patients. As far as ethnic background is concerned, 186 (44%) were White, 202 (48%) were Black (74% were African–Caribbean and 26% were African) and 34 (8%) were of another ethnicity or information concerning ethnic background was missing.
The majority (958; 63%) of the 1515 untoward incidents involved male patients, with 557 (37%) incidents involving female patients.
As far as the patients’ status under the Mental Health Act 1983 was concerned, 1137 incidents (75%) involved patients on a civil section, 45 (3%) involved patients on a criminal section and for 333 incidents (22%) the patient was informal or data were missing.
Of the 1515 incidents, data regarding psychiatric diagnosis were missing for 594 (39%) incidents. For the remainder the most common diagnoses were psychosis (766), learning disability (91) and personality disorder (64).
Rate of incidents
Out of the total of 1403 violent incidents where ethnic background was recorded as either ‘White’ or ‘Black’, 597 (43%) involved White patients and 806 (57%) involved Black patients.
Antecedents
The most common antecedents noted on the untoward incident form were: agitation (487; 32%), specific interaction with patients or staff (397; 24%), staff refusal of patient's request or patient's refusal to take medication (242; 16%) and patient attempting to abscond (96; 7%).
Association between explanatory variables and ethnic group
Black patients involved in violent incidents tended to be younger than White patients (mean age averaged over the incidents was 30.0 years for Black patients and 36.4 years for White patients). Incidents by Black patients were more likely to be committed by males (67% of Black patients involved in incidents were male compared with 59% of White patients; odds ratio=1.37) and more likely to be associated with a diagnosis of psychosis than incidents by White patients (59% compared with 42%; odds ratio=2.03). In contrast, incidents by White patients were more associated with personality disorder (9% compared with 1%; odds ratio=0.10). Incidents by Black patients were more commonly associated with being on a civil section (78% compared with 74%; odds ratio=1.25) and less likely to be by patients who were informal (or involve missing information) (17% compared with 26%; odds ratio=0.59).
Violent incidents by Black patients were slightly more likely to be considered to involve potential for danger (86% compared with 81%; odds ratio=1.43) or to be preceded by a staff denial of a request (17% compared with 13%; odds ratio=1.39) and less likely to have occurred without warning (11% compared with 15%; odds ratio=0.69). Incidents by Black patients were less likely to involve damage to property (12% compared with 19%; odds ratio=0.56) but similarly likely to result in physical injury (29% and 31%, respectively; odds ratio=0.91).
As far as the target of assault is concerned, incidents by Black patients were more likely to involve patients (37% compared with 20%; odds ratio=2.39), less likely to target property (15% compared with 23%; odds ratio=0.59) and similarly likely to target a nurse (60% and 62%, respectively; odds ratio=0.90).
Management of incidents
We first considered simple unadjusted odds ratios for each form of post-incident management by ethnicity. Then the effect of potential confounders was taken into account to produce adjusted odds ratios for ethnicity (i.e. the effect of ethnicity on each of the three management techniques after controlling for each potential confounder). Also presented are the significant factors contributing to the management of violence for the group as a whole.
Simple unadjusted odds ratios for Black v. White patients
Black patients are more likely to be given medication after a violent incident than are White patients (P=0.02), with unadjusted odds ratio estimate of 1.54 (95% CI 1.08–2.20). The unadjusted odds ratio for physical restraints when comparing Black with White patients was not significant (odds ratio=1.15, 95% CI 0.79–1.67, P=0.47). Black patients are more likely to be secluded following an incident than are White patients (unadjusted odds ratio=2.86, 95% CI 1.64–5.00,P<0.001).
Adjusted odds ratios for Black v. White patients
Tables 1, 2, 3 give odds ratios for each variable associated with the management of violent incidents when adjusted for all other variables in the model. The first column gives the odds ratios for each variable for the total group of patients. The last column gives the odds ratios for Black v. White patients when each variable is controlled for individually. Comparing this odds ratio with the unadjusted odds ratio at the foot of the table shows the strength of confounding by that variable.
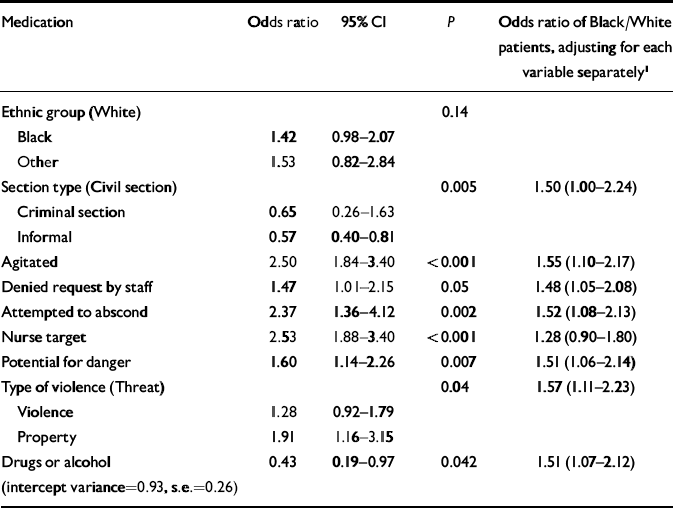
Table 1 Parameter estimates for final model for medication (the last column reports the odds ratio for Black v. White patients when only the variable on the left is controlled for)
| Medication | Odds ratio | 95% CI | P | Odds ratio of Black/White patients, adjusting for each variable separately1 |
|---|---|---|---|---|
| Ethnic group (White) | 0.14 | |||
| Black | 1.42 | 0.98-2.07 | ||
| Other | 1.53 | 0.82-2.84 | ||
| Section type (Civil section) | 0.005 | 1.50 (1.00-2.24) | ||
| Criminal section | 0.65 | 0.26-1.63 | ||
| Informal | 0.57 | 0.40-0.81 | ||
| Agitated | 2.50 | 1.84-3.40 | <0.001 | 1.55 (1.10-2.17) |
| Denied request by staff | 1.47 | 1.01-2.15 | 0.05 | 1.48 (1.05-2.08) |
| Attempted to abscond | 2.37 | 1.36-4.12 | 0.002 | 1.52 (1.08-2.13) |
| Nurse target | 2.53 | 1.88-3.40 | <0.001 | 1.28 (0.90-1.80) |
| Potential for danger | 1.60 | 1.14-2.26 | 0.007 | 1.51 (1.06-2.14) |
| Type of violence (Threat) | 0.04 | 1.57 (1.11-2.23) | ||
| Violence | 1.28 | 0.92-1.79 | ||
| Property | 1.91 | 1.16-3.15 | ||
| Drugs or alcohol | 0.43 | 0.19-0.97 | 0.042 | 1.51 (1.07-2.12) |
| (intercept variance=0.93, s.e.=0.26) |
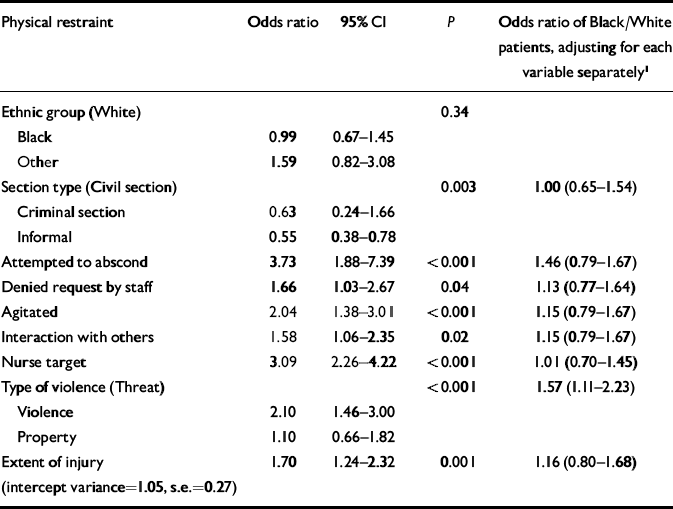
Table 2 Parameter estimates for final model for physical restraint (the last column reports the odds ratio for Black v. White patients when only the variable on the left is controlled for)
| Physical restraint | Odds ratio | 95% CI | P | Odds ratio of Black/White patients, adjusting for each variable separately1 |
|---|---|---|---|---|
| Ethnic group (White) | 0.34 | |||
| Black | 0.99 | 0.67-1.45 | ||
| Other | 1.59 | 0.82-3.08 | ||
| Section type (Civil section) | 0.003 | 1.00 (0.65-1.54) | ||
| Criminal section | 0.63 | 0.24-1.66 | ||
| Informal | 0.55 | 0.38-0.78 | ||
| Attempted to abscond | 3.73 | 1.88-7.39 | <0.001 | 1.46 (0.79-1.67) |
| Denied request by staff | 1.66 | 1.03-2.67 | 0.04 | 1.13 (0.77-1.64) |
| Agitated | 2.04 | 1.38-3.01 | <0.001 | 1.15 (0.79-1.67) |
| Interaction with others | 1.58 | 1.06-2.35 | 0.02 | 1.15 (0.79-1.67) |
| Nurse target | 3.09 | 2.26-4.22 | <0.001 | 1.01 (0.70-1.45) |
| Type of violence (Threat) | <0.001 | 1.57 (1.11-2.23) | ||
| Violence | 2.10 | 1.46-3.00 | ||
| Property | 1.10 | 0.66-1.82 | ||
| Extent of injury | 1.70 | 1.24-2.32 | 0.001 | 1.16 (0.80-1.68) |
| (intercept variance=1.05, s.e.=0.27) |
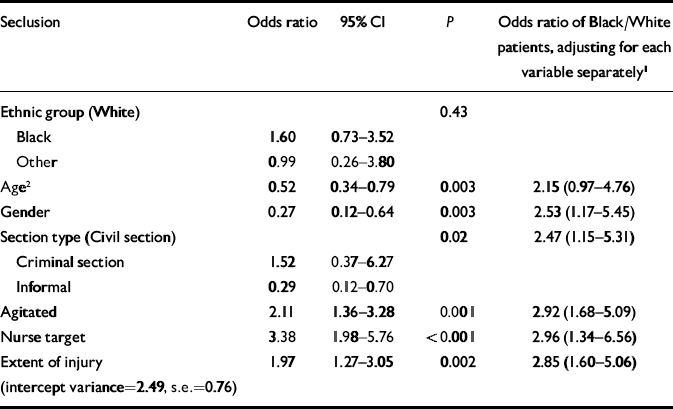
Table 3 Parameter estimates for final model for seclusion (the last column reports the odds ratio for Black v. White patients when only the variable on the left is controlled for)
| Seclusion | Odds ratio | 95% Cl | P | Odds ratio of Black/White patients, adjusting for each variable separately1 |
|---|---|---|---|---|
| Ethnic group (White) | 0.43 | |||
| Black | 1.60 | 0.73-3.52 | ||
| Other | 0.99 | 0.26-3.80 | ||
| Age2 | 0.52 | 0.34-0.79 | 0.003 | 2.15 (0.97-4.76) |
| Gender | 0.27 | 0.12-0.64 | 0.003 | 2.53 (1.17-5.45) |
| Section type (Civil section) | 0.02 | 2.47 (1.15-5.31) | ||
| Criminal section | 1.52 | 0.37-6.27 | ||
| Informal | 0.29 | 0.12-0.70 | ||
| Agitated | 2.11 | 1.36-3.28 | 0.001 | 2.92 (1.68-5.09) |
| Nurse target | 3.38 | 1.98-5.76 | <0.001 | 2.96 (1.34-6.56) |
| Extent of injury | 1.97 | 1.27-3.05 | 0.002 | 2.85 (1.60-5.06) |
| (intercept variance=2.49, s.e.=0.76) |
Table 1 gives the odds ratios for emergency medication. An inspection of the adjusted odds ratios in the last column does not suggest that ‘Black’ v. ‘White’ is strongly confounded with any of the variables included in the model (i.e. the odds ratios are stable, ranging from 1.28 to 1.57, compared with an unadjusted odds ratio of 1.54). The strongest effect is that of a nurse being the target of aggression. However, although the unadjusted effect of ethnicity is statistically significant (P=0.02; odds ratio=1.54), adjusting for all variables included in the model renders the effect non-significant (P=0.14; odds ratio=1.42). Considering all incidents, for the total patient group the largest adjusted odds ratios for emergency medication are a nurse being the target of the violent incident (odds ratio=2.53), the patient rated as being agitated (odds ratio=2.50), attempts to abscond (odds ratio=2.37), being on a civil section (odds ratio=1.53 compared with criminal section and 1.75 compared with informal section) and involvement of drugs or alcohol (odds ratio=0.43).
Table 2 gives the odds ratios for physical restraint. There was no significant unadjusted effect of ethnic background. Ethnic background remained non-significant when other variables were controlled for. For all incidents, for the total patient group the strongest predictors of physical restraint were attempts to abscond (odds ratio=3.73), a nurse being a target (odds ratio=3.09), the patient being rated as agitated (odds ratio=2.04), being on a civil section (odds ratio=1.59 compared with a criminal section and 1.82 compared with being informal) and violence (odds ratio=2.10 compared with threat of violence and 1.91 compared with damage to property).
Table 3 gives the odds ratios for seclusion. The highly significant unadjusted effect of ethnic background (P<0.001; odds ratio=2.86) becomes non-significant (P=0.43; odds ratio=0.99) once the other variables have been entered into the model. The adjusted odds ratios in the last column suggest a considerable confounding effect of age because the adjusted odds ratio decreases to 2.15 when adjusting for age, compared with the unadjusted odds ratio of 2.86. Gender and section type also had some confounding effect. The strongest predictors of seclusion for the total group of patients are the gender of the patient (odds ratio=0.27), a nurse being the target (the adjusted ethnic odds ratio=3.38), the patient rated as being agitated (odds ratio=2.11), extent of injury (odds ratio=1.97), age of patient (odds ratio=0.52) and being on a civil section (odds ratio=3.45 compared with informal status and 0.66 compared with a criminal section).
DISCUSSION
This study is based on a very large number of violent incidents, covering all those recorded in an entire hospital trust for 3 years. At first sight it appears that Black patients were more likely than White patients to be given emergency medication and/or secluded after a violent incident, but this was not so for physical restraint. However, after controlling for potential confounding factors, such as age, gender, the target of assault and the Mental Health Act 1983 status of the patient, the effect of ethnic background of the patient was no longer significant. The confounding effects were strongest in relation to seclusion. The age of the patient, with Black patients tending to be younger than White patients, was the strongest confounding variable, followed by gender and section type. The main confounder in the case of emergency medication was a nurse being the target of the violence.
The current study is largely consistent with the findings of Gudjonsson et al (Reference Gudjonsson, Rabe-Hesketh and Wilson2000), which also examined these three forms of post-incident management. Whereas in the previous study the findings were limited to one medium secure unit, in the present study incidents over 3 years (1994, 1996, 1998) were analysed for 14 general wards in a large psychiatric hospital. As in our study, ethnic differences were not found for physical restraint. However, in contrast to the previous study, there was a significant difference found for seclusion. This could be explained by the fact that the patients on the medium secure unit were more homogeneous in those characteristics shown in our study to demonstrate differences in the rate of seclusion. The previous study found, as we did, that there were ethnic differences in relation to emergency medication after a violent incident. In that study, however, the significant difference persisted despite taking confounders into account. This may be because fewer potential confounders were examined compared with the present study, or it may be that practice in a medium secure setting is influenced by different factors.
Explaining ethnic differences
Our results do not support the idea that ethnic differences in post-incident management reflect a form of racial bias (Reference Sabshin, Diesenhaus and WilkersonSabshin et al, 1970; Reference SashidharanSashidharan, 2001). A concern that this might be occurring was the main impetus for our study; if such a bias is operating, then it needs to be acknowledged and action should be taken to eliminate it.
Rather than being a reflection of racial bias, ethnic differences found in the treatment of patients may be confounded by a range of differences between ethnic patient groups on demographic variables (e.g. age, gender), the nature of the psychiatric illness (e.g. psychosis v. personality disorder), the type of legal section they are detained under (e.g. civil section v. criminal or informal status) and incident-related characteristics (e.g. the patient's level of disturbance, attempting to abscond, the target of the violence, the extent of the injury). Also to be noted in evaluating differences in the use of ‘coercive’ measures on in-patient units is the possibility of earlier, pre-admission or ‘upstream’ events that may have been influenced by ethnic differences and might have resulted in admission to hospital under more coercive circumstances, for example on a compulsory order. This may have been an important factor contributing to the use of seclusion. However, once on the ward, nurses’ responses showed no evidence of racial bias.
The present findings indicate that, in explaining ethnic differences, confounding influences were powerful in the case of seclusion and sufficiently evident in relation to emergency medication to make the differences non-significant. Of note is that for what are arguably the more ‘coercive’ managements - seclusion and physical restraint - there was either no ethnic difference or it was explained by clear demographic differences. In the case of emergency medication a range of confounders was evident, each making small contributions. The strongest confounder was a nurse being the target of violence. We cannot be sure whether, within this assessment by staff who completed reports on the incidents, an element of stereotyping did or did not play a role. It is possible that Black patients might have been perceived as more threatening to staff. Against this is the finding that ‘potential for danger’ associated with the incident, assessed by staff, was not an important confounder.
Determinants of management of violent incidents for the patient group as a whole
We also considered the determinants of the management of violent incidents for the patient group as a whole, regardless of ethnicity. Different factors appear to be related to different methods of managing violent incidents, although there was a marked overlap. The most significant factor across all three management techniques was a nurse being the target of the violence. Particular concerns have been raised by some authors about assaults on staff in mental health services (Reference Cembrowicz, Ritter, Wright and ShepherdCembrowicz et al, 2001), with about two-thirds of all violent incidents being directed at nursing staff (Reference Gournay, Ward and ThornicroftGournay et al, 1998). When a potentially violent situation arises, or where there is actual violence, staff have to defuse and control the situation. Assaults on staff may be perceived as being particularly unsafe, irrespective of the actual injury inflicted, because staff are required to prevent an escalation of violence and to manage a situation threatening to undermine their control.
The most important other predictors of emergency medication were a mental state described as ‘agitation’ and attempts to abscond. This was also the case for physical restraint and seclusion. It is not clear what was encompassed by the term ‘agitation’ but it probably referred to a wide range of disturbed behaviours.
Historical variables, such as age, section type, target of assault and attempts to abscond, are less problematic in interpretation than retrospective descriptions of agitation and potential for violence. We do not know, for example, the extent to which a certain management technique, once implemented by nursing staff, influenced subsequent perceptions and ratings of agitation and potential for danger. Further research using a finer-grained examination and a less retrospective approach is needed to clarify which patient behaviours are associated with particular staff responses, and how they are interpreted by those staff. Our findings indicate that interactions preceding the violent incident, for example refusing a request, also may be important in determining what emergency actions will be taken.
There is a consistent association between patients being on a civil section and increased use of emergency medication, seclusion and physical restraint. It is known that patients admitted on a civil section are more likely to have been involved in violent incidents than those on a criminal section (Reference Agarwal and RobertsAgarwal & Roberts, 1996; Reference Gudjonsson, Rabe-Hesketh and WilsonGudjonsson et al, 1999).
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ ▪ National Health Service trusts have a duty of care to patients and need to research and address ethnic issues relating to the management of violent incidents.
-
▪ ▪ In this study, ethnic differences in the way violent incidents were managed could be explained by a number of confounding factors that did not suggest a racial bias.
-
▪ ▪ A number of factors have been identified in this large study that predict the way in which staff manage violent incidents. Finer-grained studies are necessary for a clearer characterisation of these factors and their interactions.
LIMITATIONS
-
▪ ▪ The study relies on retrospective data of violent incidents.
-
▪ ▪ The data analysed are restricted by the nature of the data collected on a standard hospital incident form.
-
▪ ▪ Because this is a study of the management of violent incidents in one trust, there may be limitations to how far the findings can be generalised.
Acknowledgements
Claire Wilson and Joanna Mary assisted with computerising the incident. forms.








eLetters
No eLetters have been published for this article.