Postnatal depression affects between 10% and 15% of new mothers. It is associated with adverse consequences for the mother's mental health and functioning (Reference Kumar and RobsonKumar & Robson, 1984; Reference Marks, Wieck and CheckleyMarks et al, 1992), with deterioration of the marital relationship and of the psychological health of the partner (Reference Lovestone and KumarLovestone & Kumar, 1993; Reference Ballard and DaviesBallard & Davies, 1996), and has an adverse long-term impact on the cognitive and social development of the infant (Reference Hay, Pawlby and SharpHay et al, 2001; Reference Murray, Cooper and GoodyerMurray & Cooper, 2003). Despite growing recognition of the problem of postnatal depression, no research has yet linked analyses of its origins and consequences with studies of service provision in different national health and social service systems. For such research to be achieved, methods of assessment are required that take into account the particular characteristics and needs of women perinatally and that have been modified and tested in cross-national contexts.
Transcultural Study of Postnatal Depression
The primary aim of the Transcultural Study of Postnatal Depression (TCS-PND) was to develop (or modify), translate and validate research instruments that could be used in future studies of postnatal depression in different countries and cultures. The instruments were chosen to assess key aspects of the maternity experience; namely, clinical diagnosis, the psychosocial context of pregnancy and motherhood, maternal attachment style, mother-infant interaction, the child's environment, and health service structure, use and its associated costs. The modified and translated research tools were then piloted to test how well they worked in a perinatal setting and in other languages and populations.
Ten centres in eight countries took part in testing the study instruments: Bordeaux (France), Dublin (Ireland), Florence (Italy), Iowa City (USA), Keele (UK), London (UK), Paris (France), Porto (Portugal), Vienna (Austria) and Zurich (Switzerland). Several additional centres contributed to a qualitative study which aimed to inform the work on instrument development by exploring the cross-cultural equivalence of the concept of postnatal depression.
Five of the companion papers in this supplement describe the study instruments and report details of modifications, translations and the results of pilot testing. One paper reports on the qualitative study.
METHOD
Study instruments
Seven research instruments were piloted in this study. Two instruments were first adapted for use in perinatal research, and then translated and piloted: the Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I; Reference First, Spitzer and GibbonFirst et al, 1994) and the Client Service Receipt Inventory (CSRI; Reference Beecham, Knapp, Thornicroft, Brewin and WingBeecham & Knapp, 1992). A further five instruments - the Edinburgh Postnatal Depression Scale (EPDS; Reference Cox, Holden and SagovskyCox et al, 1987), the Contextual Assessment of the Maternity Experience (CAME; Reference Bernazzani, Bifulco and MarksBernazzani et al, 1998), the Attachment Style Interview (ASI; Reference Bifulco, Lillie and BallBifulco et al, 1998), the Global Ratings Scales of mother-infant interaction (Reference Murray, Fiori-Cowley and HooperMurray et al, 1996) and the Infant-Toddler version of the Home Observation for the Measurement of the Environment (IT-HOME, Reference Caldwell and BradleyCaldwell & Bradley, 1984) - were modified where necessary, translated and piloted.
Assessment of clinical diagnoses for women in the perinatal period
The SCID-I is a semi-structured interview for making the major DSM-IV diagnoses (American Psychiatric Association, 1994). In this study a research version of SCID-I designed for use with non-patient populations (SCID-I/NP; Reference First, Gibbon and SpitzerFirst et al, 1996), was modified to produce an instrument for assessing postnatal depression in different cultural contexts: the SCID-PND (Reference Gorman, O'Hara and FigueiredoGorman et al, 2004, this supplement).
The EPDS is a ten-item self-completion scale used to screen for postnatal depression. Although the scale cannot be used as a diagnostic tool, a score of 12 or more is usually taken to indicate the likely presence of depression.
Psychosocial context of pregnancy and motherhood
Psychosocial adversity is a robust predictor of postnatal depression (Reference O'Hara and SwainO'Hara & Swain, 1996). The Contextual Assessment of Maternity Experience was developed to assess the social environment relevant to the maternity experience in different cultural settings (Bernazzani et al, Reference Bernazzani, Gorman and Marks2000, Reference Bernazzani, Conroy and Marks2004, this supplement). Contextual rating aims to capture the meaning of an experience based on team consensus about the likely emotional reaction of most people in biographical circumstances similar to that of the interviewee. Such consensus judgements are embodied in extensive training manuals for European settings. Reliability is ensured by interviewer training, reference to manualised examples (Reference Bernazzani, Bifulco and MarksBernazzani et al, 1998) and consensus team judgements. The CAME includes assessment of social and practical support, recent adversity, the emotional context (feelings about the pregnancy, and about motherhood and parenting), and the woman's roles and activities.
Attachment style
The Attachment Style Interview (Reference Bifulco, Figueiredo and GuedeneyBifulco et al, 2004, this supplement) is a semistructured interview to identify attachment styles which increase vulnerability to major depression (Bifulco et al, Reference Bifulco, Moran and Ball2001a ,Reference Bifulco, Moran and Ball b ). Ratings are made by interviewers from transcribed, tape-recorded interview material. Reliability is ensured by prior interviewer training, reference to manualised examples (Reference Bifulco, Lillie and BallBifulco et al, 1998) and consensus team judgements. Overall attachment style is based on eight sub-scales assessing avoidant behaviour, dependence, emotional constraints on closeness, and judgement of ability to make and maintain relationships. The ASI generates five attachment style ratings: ‘enmeshed’, ‘angry-dismissive’, ‘fearful’, ‘withdrawn’ and ‘clearly standard’.
Child assessments (interaction and environment)
The Global Rating Scales (Reference Murray, Fiori-Cowley and HooperMurray et al, 1996; Reference Gunning, Fiori-Cowley and MurrayGunning et al, 1999) were developed to assess differences in mother-infant interaction between women who were or were not depressed. The scales globally assess the quality of maternal and infant behaviours and the overall interaction between the two, during a 5 min video-recorded assessment of free play.
The Infant-Toddler version of the Home Observation for the Measurement of the Environment assesses the quality and quantity of stimulation and support available to the child in the home environment. The 45-item binary choice scale is administered in the home, with some items scored from observation and some from interview (Reference Caldwell and BradleyCaldwell & Bradley, 1984).
Service use and costs
The Client Service Receipt Inventory - Postnatal Depression version (CSRI-PND; Reference Chisholm, Conroy and Glangeaud-FreudenthalChisholm et al, 2004, this supplement) is a service use measure for women with postnatal depression which provides information for economic evaluation of the mental health care they received. The instrument is a derivation of the Client Socio-demographic and Service Receipt Inventory - European version (Reference Chisholm, Knapp and KnudsenChisholm et al, 2000), which itself is an adaptation of the CSRI (Reference Beecham, Knapp, Thornicroft, Brewin and WingBeecham & Knapp, 1992). The CSRI-PND enables the comprehensive costing of care packages for women who have recently had a child, with a view to determining the excess need and service uptake of women with postnatal depression. Information is collected on the use of a range of health care, social care and other services over a defined retrospective period. Unit costs for each of these services can then be calculated to give the total costs associated with each individual's use of services.
Study sites
Ireland (Dublin)
For funding and administrative purposes, Ireland is divided into eight health board regions, directly responsible for providing acute general hospital, obstetric and psychiatric care in rural Ireland. In the Dublin area, voluntary organisations, directly funded by the Department of Health, have traditionally provided these services along-side those run by the health board. About a third of the population carries a medical card provided by the local health board. This card entitles the bearer to the full range of medical services free of charge on grounds of financial hardship. The remaining two-thirds of the resident population have limited eligibility for public health care.
A maternity and infant scheme, operated through general medical practitioners, provides free antenatal care for expectant mothers and medical care for mothers and infants for up to 6 weeks after the birth. Normally, women choose their own general practitioner (GP) and make at least six visits before delivery and two visits afterwards. An option of combined care is also available antenatally, with monitoring by both the hospital and the GP. Public hospital obstetric care is available free of charge to all. Domiciliary births are infrequent, the rate being 0.4% in 1998. A general community nursing service is provided through public health nurses trained in community nursing and midwifery. A public health nurse carries out a home visit soon after notification of birth is received and ideally again at 3 months and 7 months. With many nursing posts currently vacant, visits may now be less frequent, but the initial home visit almost always takes place, and mothers are well informed and pursued to have their infant's developmental checks carried out.
Psychiatric care has been progressively de-institutionalised, and a community care model with acute care provided in general hospital psychiatric units is now becoming the norm. The number of in-patient beds has steadily declined from the mid-1980s, made possible by growth in the number of community residences and day hospitals. There are no dedicated mother and baby facilities in Irish psychiatric hospitals but each of the Dublin maternity hospitals has a psychiatric liaison service, which partially meets the psychiatric needs of their patients.
Italy (Florence)
The National Health System, which provides health care for the entire population, is organised into three levels: basic medical services, supplied by general practitioners, paediatricians and emergency services; specialised care, including out- patient clinics and laboratories; and hospital care. The GP has a crucial role, both supplying first-level care and acting as a filter for patients' access to National Health System specialists and hospital care.
A pregnancy certificate entitles a woman to access public health services for routine screenings included in the National Pregnancy Protocol and provided by each Italian region. Family health centres provide care for mothers and infants from gynaecologist-obstetricians, midwives, psychologists, social workers, paediatricians and legal advisers. The majority of deliveries (80%) take place in a public hospital, with the rest in a private hospital or, rarely, at home. If all is well, the woman is discharged on the third day following delivery. Women are entitled to request three postnatal domiciliary visits by a National Health System midwife, who is able to advise on managing the baby and to assess the woman's physical and mental health.
The Mental Health Department coordinates psychiatric care. Mental health centres, with multi-disciplinary teams of psychiatrists, psychologists, nurses and educators, coordinate community services, offer out-patient units and domiciliary visits, and act as a filter for hospitalisation, psychotherapy and welfare activity. The psychiatric departments of general hospitals have in-patient facilities for patients in an acute phase. Greater Florence is subdivided into four areas, each with the above facilities. An individual may approach these services directly or be referred by a GP. In addition, the department of neurology and psychiatry at the University of Florence provides specialised hospital facilities for voluntary patients, and also functions as a day hospital and out-patient clinic. Psychiatric care facilities in the private sector exist but are difficult to quantify.
France (Bordeaux and Paris)
Most French people have state health insurance which reimburses most of the costs of medical care, and many have additional insurance to complete the reimbursement of care. Uninsured people with no income are entitled to free state assistance. Despite open access to specialist and hospital services, many French people visit a family physician (GP) for general health matters.
All women are entitled to free health care during pregnancy, although the majority have insurance. A distinctive feature of perinatal care is that specific conditions must be fulfilled in order to obtain the large financial maternity allowance. Women must obtain a pregnancy certificate before 15 weeks from their doctor or midwife and attend all seven state recommended antenatal visits and all required postnatal checks for the baby. Three postnatal checks are required, at 8 days, 9 months and 24 months, and these obligatory visits are free. A free examination, by a gynaecologist or GP, is recommended for the woman at 6-8 weeks post-partum. Many women are prescribed ten free abdominal and/or perineum ‘re-education’ sessions, conducted either by a kinesitherapist or a midwife. Two-thirds of all deliveries are led by midwives, approximately 6% as home deliveries. About half of all maternity care takes place within the private sector and half within the public sector, with a tendency for women with high-risk pregnancies and those requiring specialised care to be delivered in public-sector hospitals.
At the centre of the delivery of psychiatric care is a multi-disciplinary mental health team consisting of psychiatrists, psychiatric nurses, psychologists, social workers and a wide range of other paramedical mental health workers. In the Îlede-France (Paris and suburbs) most public general psychiatric care takes place on an out-patient or community basis (81%), with 17% of care provided to in-patients and 2% to day patients. A number of psychiatric mother and baby units offer acute or prophylactic pregnancy and postnatal in-patient admissions, including one in Bordeaux and several in Paris.
USA (Iowa City)
Although there is no universal national health care system in the USA, the government programme Medicaid covers health care costs for the poorest and most vulnerable. In 1997, about 10% of the Iowa population received care through Medicaid. Those not covered by government health care programmes are typically covered by private health insurance plans.
The maternity health care system is variable throughout the USA, depending on the setting and resources. The state of Iowa funds a system of maternal health care centres which provide prenatal services for women with low incomes. The majority of pregnant women begin prenatal care during the first trimester of pregnancy; obstetricians, family practice physicians and GPs are the main providers of obstetric care. Foetal testing procedures and surgical deliveries are relatively common. Physicians deliver the majority of babies in hospital (99% of births in 1993). Typically, women stay in hospital for 48 h following an uncomplicated delivery, and 3 days following a Caesarean delivery. There is virtually no provision for post-partum care at home. Most hospitals provide information about infant care or post-partum difficulties through a call-in telephone line, and some provide lactation consultants for women experiencing breast-feeding difficulties. Women typically return for a final follow-up visit to their obstetrician or family practice physician at 4-6 weeks post-partum.
Mental health care service delivery in the USA is highly complex and rapidly changing and there is currently no unified or comprehensive mental health care policy. There is a range of mental health facilities, including community mental health centres, state and county mental hospitals, private psychiatric hospitals, psychiatric units in general hospitals, residential treatment centres, multi-service mental health organisations, and free-standing psychiatric clinics. Services are also provided in private practice settings and in educational, occupational and other organisational settings. Access to mental health services depends upon many factors, including geographical location, economic status and health insurance coverage. Primary care physicians are frequently the sole source of care, particularly in rural areas. In 1997 about 22% of people in Iowa lacked access to mental health care services, almost twice the national rate (Reference Morgan and MorganMorgan & Morgan, 1999). There is no specialised mental health care service for pregnant and post-partum women.
Portugal (Porto)
During pregnancy, about half of Portuguese women are cared for by a general practitioner in their local community health service; the other half are cared for by private gynaecologists or obstetricians. Women with high-risk pregnancies see an obstetrician at the hospital; those with uncomplicated pregnancies attend either a GP or a private gynaecologist or obstetrician. In 1999, over 99% of deliveries took place in a public or private hospital, while less than 1% took place at home. Women receive a post-partum check-up 4-5 weeks after delivery. Approximately half receive this from a GP and half from a private obstetrician.
About 80% of women with mental health problems are treated initially by public-sector services. The first contact may be with either a GP or a psychiatrist from the emergency service of the local hospital, who will refer, if necessary, to a psychiatric ward or day hospital. Private psychiatrists initially see about 20% of women with mental health problems and they also will refer on, if necessary, to the same services. There is no specialised service for post-partum mental illness in mothers.
UK (Keele and London)
The National Health Service (NHS) provides the majority of health care, although the private sector is steadily growing and becoming increasingly integrated with the NHS, which buys in some of its services. Every UK citizen has a right to be registered with a local GP who supplies first-level care and acts as a filter for access to NHS specialists and hospital care.
A pregnant woman is usually first seen by her GP and then booked for antenatal care either in a hospital or in a community midwifery booking clinic. Antenatal care is usually shared between hospital, GP and community midwife, although high-risk pregnancies receive mostly hospital care while very low-risk pregnancies may receive only community care. Ninety-eight per cent of deliveries take place in hospital. Following a normal delivery, women typically stay in hospital for less than 48 h (5 days after a Caesarean section). Midwifery home visits are made for 10 days after delivery and up to 28 days if circumstances require. A health visitor sees the mother at home at around 10-14 days, with subsequent contacts at a child health clinic, general practice surgery, or at home. Health visitors have a preventive role in relation to both maternal and child health. Women routinely have a 6-week postnatal check with the GP or the hospital.
Community mental health services for people with more severe mental health problems are provided by multi-disciplinary teams, typically consisting of a psychiatrist, psychiatric nurses, social workers and an occupational therapist. General practitioners and health visitors treat most women with postnatal depression. Several areas in the UK have a perinatal psychiatric service catering specifically for the mental health needs of pregnant and postpartum women, and there are a number of in-patient mother and baby units, for acute or prophylactic postnatal admissions.
Austria (Vienna)
The provision of health services in Austria is mainly a public task under the control of federal, provincial and communal authorities. Social and health insurance (SHI) is obligatory, financed with contributions from the consumer and the employer. Members have the right to consult any GP or medical specialist who has a contract with the SHI. Community medical services are mainly provided by independent GPs and medical specialists. The former provide primary medical care and are usually the first point of contact, although patients can also approach specialists or out-patient hospital wards directly.
There is a standardised prevention programme to ensure maternal and child health, consisting of obligatory free medical check-ups for pregnant women and their children until the age of 4 years. Information about the mother's health during pregnancy, the birth process and well-baby visits are recorded in the ‘mother-child passport’. The first contact for a pregnant woman is typically her gynaecologist, who gives her the passport and informs her about the programme. In rural areas with few specialists the woman's first contact may be her GP. Ninety-eight per cent of deliveries take place in hospital. If the woman leaves the hospital within 24 h after childbirth, she is entitled to the service of a midwife for the first week at home, with the costs covered by health insurance.
Vienna is divided into eight psychosocial service areas, each equipped with a community-based out-patient department. In addition to these and several associated day clinics, within each service area psychiatric in-patient departments offer 24 h out-patient services. These facilities offer treatment free of charge, including counselling, support for family members, rehabilitation programmes, financial support, self-help groups and assisted living services, primarily serving patients with chronical illness. There are also several residential facilities offering programmes for patients with chronical illness. At present there is no facility for women with mental illness to be admitted with their babies.
Switzerland (Zurich)
Typically, a pregnant woman will register with a gynaecologist or, less frequently, a GP whom she already knows; however, if medical complications are identified, the woman is usually referred to one of the large maternity hospitals. Seven antenatal checks are required by the general medical guidelines approved by the health insurance and two ultrasound scans are paid for by health insurance. Ninety-nine per cent of deliveries take place in hospital and health insurance pays for up to 5 days of hospital care after delivery. After birth, the woman remains in the care of her private obstetrician or GP, with an entitlement to 10 days of midwifery care. On the perinatal ward, mothers are encouraged to register their baby with a paediatrician or GP for future routine checks.
A network of mostly free advice centres provide advice and assistance prenatally and postnatally on breast-feeding, nutrition, sleep problems, maternal and paternal emotional and psychological problems, and problems with older siblings. Individual counselling by nurses and psychologists, social workers and other professionals may be provided, and referral to psychiatric services or day support services may be organised if necessary. There is no specialised psychiatric unit for pregnant women or mothers with babies, but some obstetric departments provide prolonged or preventive in-patient treatment for women with psychiatric needs, and many psychiatric hospitals try to arrange joint mother and baby admissions on general wards.
Protocol
The study instruments were all originally developed in English and so had to be translated into four other languages (Portuguese, Italian, French and German). To ensure that translations were conceptually valid and to enable researchers to reach appropriate levels of interrater reliability, training and supervision workshops were conducted at regular intervals throughout the study. These began with an initial 12-day training workshop held at the University of Keele, UK, in 1998, followed by consensus workshops in France (1998), Austria (1999), Italy (2000), UK (2000) and Ireland (2001).
Sample
Eligible women were approached in antenatal clinics and classes by a researcher who obtained informed consent from those who agreed to take part. The only criterion for recruitment was that women had to be in the second or third trimester of pregnancy - except in Paris, Bordeaux and Vienna, where women were also required to have the nationality of the country. The size of the sample recruited varied for each centre (Table 1). In total, 296 women were interviewed antenatally, of whom 261 were interviewed again postnatally.
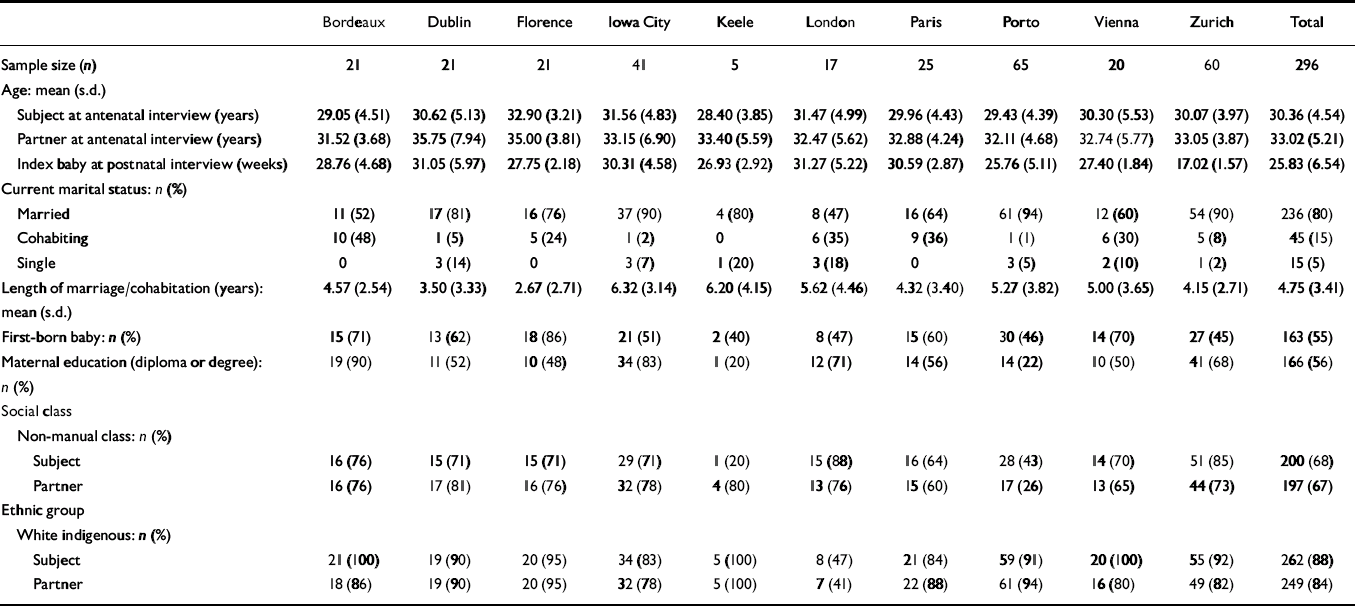
Table 1 Demographic characteristics of sample in each study site
| Bordeaux | Dublin | Florence | Iowa City | Keele | London | Paris | Porto | Vienna | Zurich | Total | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Sample size (n) | 21 | 21 | 21 | 41 | 5 | 17 | 25 | 65 | 20 | 60 | 296 |
| Age: mean (s.d.) | |||||||||||
| Subject at antenatal interview (years) | 29.05 (4.51) | 30.62 (5.13) | 32.90 (3.21) | 31.56 (4.83) | 28.40 (3.85) | 31.47 (4.99) | 29.96 (4.43) | 29.43 (4.39) | 30.30 (5.53) | 30.07 (3.97) | 30.36 (4.54) |
| Partner at antenatal interview (years) | 31.52 (3.68) | 35.75 (7.94) | 35.00 (3.81) | 33.15 (6.90) | 33.40 (5.59) | 32.47 (5.62) | 32.88 (4.24) | 32.11 (4.68) | 32.74 (5.77) | 33.05 (3.87) | 33.02 (5.21) |
| Index baby at postnatal interview (weeks) | 28.76 (4.68) | 31.05 (5.97) | 27.75 (2.18) | 30.31 (4.58) | 26.93 (2.92) | 31.27 (5.22) | 30.59 (2.87) | 25.76 (5.11) | 27.40 (1.84) | 17.02 (1.57) | 25.83 (6.54) |
| Current marital status: n (%) | |||||||||||
| Married | 11 (52) | 17 (81) | 16 (76) | 37 (90) | 4 (80) | 8 (47) | 16 (64) | 61 (94) | 12 (60) | 54 (90) | 236 (80) |
| Cohabiting | 10 (48) | 1 (5) | 5 (24) | 1 (2) | 0 | 6 (35) | 9 (36) | 1 (1) | 6 (30) | 5 (8) | 45 (15) |
| Single | 0 | 3 (14) | 0 | 3 (7) | 1 (20) | 3 (18) | 0 | 3 (5) | 2 (10) | 1 (2) | 15 (5) |
| Length of marriage/cohabitation (years): mean (s.d.) | 4.57 (2.54) | 3.50 (3.33) | 2.67 (2.71) | 6.32 (3.14) | 6.20 (4.15) | 5.62 (4.46) | 4.32 (3.40) | 5.27 (3.82) | 5.00 (3.65) | 4.15 (2.71) | 4.75 (3.41) |
| First-born baby: n (%) | 15 (71) | 13 (62) | 18 (86) | 21 (51) | 2 (40) | 8 (47) | 15 (60) | 30 (46) | 14 (70) | 27 (45) | 163 (55) |
| Maternal education (diploma or degree): n (%) | 19 (90) | 11 (52) | 10 (48) | 34 (83) | 1 (20) | 12 (71) | 14 (56) | 14 (22) | 10 (50) | 41 (68) | 166 (56) |
| Social class | |||||||||||
| Non-manual class: n (%) | |||||||||||
| Subject | 16 (76) | 15 (71) | 15 (71) | 29 (71) | 1 (20) | 15 (88) | 16 (64) | 28 (43) | 14 (70) | 51 (85) | 200 (68) |
| Partner | 16 (76) | 17 (81) | 16 (76) | 32 (78) | 4 (80) | 13 (76) | 15 (60) | 17 (26) | 13 (65) | 44 (73) | 197 (67) |
| Ethnic group | |||||||||||
| White indigenous: n (%) | |||||||||||
| Subject | 21 (100) | 19 (90) | 20 (95) | 34 (83) | 5 (100) | 8 (47) | 21 (84) | 59 (91) | 20 (100) | 55 (92) | 262 (88) |
| Partner | 18 (86) | 19 (90) | 20 (95) | 32 (78) | 5 (100) | 7 (41) | 22 (88) | 61 (94) | 16 (80) | 49 (82) | 249 (84) |
Demographic details of participants for each centre are shown in Table 1. The mean age of participants was 30.4 years, slightly older than the European average age of all mothers giving birth which was 28.9 in 1995 (Eurostat, 1997). Samples from each centre were similar with respect to women's age (range 28-32 years) and partner's age (range 31-35 years) at antenatal interview. Duration of marriage or cohabitation ranged from 2.6 years to 6.3 years, with a mean of 4.75 across centres. Overall, four-fifths of the sample were married, one-sixth was cohabiting and only 1 in 20 was single, although there was some variation in this between centres. Samples were predominantly middle-class, with over two-thirds of women and their partners in non-manual employment, except in Porto where less than half of the women and their partners were non-manual workers. Nearly half the sample had a previous child or children, the least in Florence (14%), and the most in Zurich (55%).
Procedure
Women were interviewed during the third trimester of pregnancy (mean gestation 7.97 months, s.d.=0.91). Postnatal interviews were conducted at around 6 months following delivery (mean 6.03 months, s.d.=1.59), except in Zurich where interviews took place at around 4 months. In most centres a number of participants were lost to follow-up at the time of the postnatal interviews, mostly owing to women moving house and becoming uncontactable. Interviews took place at a time and location convenient for the woman, usually her own home or the hospital.
Qualitative study
In parallel with and informing the instrument development work, a qualitative study was conducted to explore the cross-cultural equivalence of the concept of postnatal depression and to seek views on appropriate remedies and services (Reference Oates, Cox and NeemaOates et al, 2004, this supplement). Data from focus groups with postnatal women were supplemented with the views of relatives (partners and grandmothers) and those of health service professionals. In addition to the study sites that undertook instrument testing, three other European centres (Nottingham and Manchester, UK, and Gothenburg, Sweden) and two outside Europe (Kampala, Uganda and Kyushu, Japan) were able to conduct this part of the study. In two of the UK sites, lay informants came from an Asian ethnic minority group. This wider participation allowed a broader exploration of whether postnatal depression is recognised in only certain countries and cultures.
RESULTS
The papers in this supplement describe more fully the research instruments used in the study, and report details of modifications, translations and the results of their testing on pilot samples in the different centres.
DISCUSSION
The general approach with regard to the quantitative measures reported in this supplement (with the exception of the CSRI-PND) is to examine results for both the pooled samples overall and for individual centre samples. Gorman et al (Reference Gorman, O'Hara and Figueiredo2004, this supplement) report that the overall rate of depression during pregnancy and the postnatal period was consistent with rates reported in previous studies, suggesting that the SCID-I was successfully adapted for this context. However, rates of perinatal depression varied substantially between centres and the authors suggest possible explanations for this, including differences between centre samples in history of previous depression, social class, recent life adversity, emotional support, attitudes towards the pregnancy, and maternal attachment style. More than a quarter (28%) of the pooled sample had a history of previous depression, with centre rates varying from 8% to 56%, and previous depression was strongly associated overall with perinatal depression. Rates of severe adversity ranged from 40% to 71% across centres, with a rate of 53% in the pooled sample. A quarter of the pooled sample had a poor relationship with either their partner or a significant other, with individual centre rates varying from 11% to 59%. Attitudes towards the pregnancy also varied by centre. All three of these variables predicted onset of depression during the perinatal period (Reference Bernazzani, Conroy and MarksBernazzani et al, 2004, this supplement). Rates of insecure maternal attachment style ranged from 19% to 76% across centres, with a rate of 55% for the pooled sample, similar to that found in a previous London study. Insecure attachment style was also associated with onset of both antenatal and postnatal depression (Reference Bifulco, Figueiredo and GuedeneyBifulco et al, 2004, this supplement).
Results from testing the measures of mother-infant interaction and the home environment are reported by Gunning et al (Reference Gunning, Conroy and Valoriani2004, this supplement). Centre differences in social class explained variations in global ratings of mother-infant interaction across centres but not variations in IT-HOME scores. In the pooled sample, women with both postnatal depression and poor postnatal emotional support had less sensitive interactions with their babies, whereas poor support alone was related to lower IT-HOME scores. Gunning et alconcluded that the Global Ratings Scales were effectively applied by participating centres but that there was less evidence for the usefulness of the IT-HOME in these small pilot samples.
Any future cross-cultural study of postnatal depression would need to take into account local health service provision and use. Chisholm et al (Reference Chisholm, Conroy and Glangeaud-Freudenthal2004, this supplement) report on the successful adaptation of a service use measure which demonstrated the varied and often limited use of care within these small pilot samples.
Oates et al (Reference Oates, Cox and Neema2004, this supplement) describe the novel method of the qualitative study and report on some of the commonalities and differences that were apparent between participating centres. Informants in all centres recognised ‘morbid unhappiness’ as a common phenomenon following childbirth, describing signs and symptoms compatible with a diagnosis of postnatal depression. Lay informants viewed the causes and remedies as lying in the psychosocial domain, emphasising family relationships and social support. A need for intervention by health professionals was not universally recognised, but where a need was seen, talking therapies were the preferred option. Although health professionals in all centres shared the psychosocial view of the aetiology of the condition, they viewed the remedies as improved health service intervention. Oates et al conclude that the future of cross-cultural research lies in combining both quantitative and qualitative approaches.
No conclusion about the aetiology of perinatal depression can be drawn from these small pilot samples. However, reliable, culturally valid and harmonised methods for diagnosing depression and assessing the maternity experience in a cross-cultural context are now available in English, French, German, Italian and Portuguese, enhancing the potential for future comparative research into postnatal depression within different health systems and countries.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Reliable methods for diagnosing postnatal depression, assessing the maternity experience and evaluating service use and costs, in a cross-cultural context, are now available.
-
▪ These methods enhance the potential for future comparative research into postnatal depression within different health systems and countries.
-
▪ Such research is likely to lead to improvements in the detection and treatment of women with postnatal depression.
LIMITATIONS
-
▪ Samples within in each centre were small, and not always representative.
-
▪ No reliable conclusion about observed differences between centres could therefore be drawn.
-
▪ Methods for assessing the longer-term implications of postnatal depression for the mother, the infant and the family were not included.






eLetters
No eLetters have been published for this article.