Attachment theory in relation to experiences associated with childbirth has been invoked mainly in relation to the impact of the mother's interaction with the newborn baby (Reference Stein, Gath and BucherStein et al, 1991; Reference Hipwell, Goossens and MelhuishHipwell et al, 2000). Much of the emphasis has been on the child's development of secure attachment in relation to the mother's sensitivity as observed in dyadic study (Reference Murray, Stanley and HooperMurray et al, 1996). The development of secure attachment early in life is a key developmental task that influences the child's representations of self and others. This dictates aspects of the ‘internal working model’ which influences future expectations of self and others, and determines strategies for processing attachment-related thoughts and feelings (Bowlby, Reference Bowlby1973, Reference Bowlby1980). Insecure attachment strategies primarily involve either minimising the expression of attachment (avoidant styles) or maximising such expression (anxious/enmeshed styles). These strategies relate to maternal behaviours identified, respectively, as distant and withdrawn, or intrusive and punitive - behaviours that are more common in mothers with depression and in those living in conditions of social adversity (Reference Murray, Stanley and HooperMurray et al, 1996).
Research into attachment style in relation to adult psychopathological disorder is relatively new and has followed separate strands investigating the influence of attachment on either social interaction or states of mind (Reference Dozier, Stovall, Albus, Cassidy and ShaverDozier et al, 1999). The former is the focus of the present study. A number of studies using this approach have now explored the association of adult attachment style with depression (Reference Hammen, Burge and DaleyHammen et al, 1995; Reference Gerlsma and LuteijnGerlsma & Luteijn, 2000), and with vulnerability associated with depression, such as poor support and adverse childhood experience (Reference Muller and LemieuzMuller & Lemieuz, 2000). Investigation of psychosocial risks for postnatal disorder has largely paralleled that for major depression (Reference Brown, Bifulco and AndrewsBrown et al, 1990), with the wider context of the pregnancy and birth examined in terms of maternal life stressors, quality of marriage, and social support (Reference Bernazzani, Saucier and DavidBernazzani et al, 1997). In addition, interpersonal psychotherapy, proved to aid recovery in major depression, has been shown similarly to effect recovery from postnatal depression (Reference O'Hara, Stuart and GormanO'Hara et al, 2000). However, such investigation has not yet been extended to studying maternal attachment style in relation to postnatal risk. Given the importance of close adult attachments in the development of depression associated with childbirth, it is highly plausible that attachment style, defined in terms of ability to access and utilise social support, will also play a part in the development of antenatal or postnatal depression.
One reason for the slow integration of attachment theory into psychopathology is the limited measurement options. The study of attachment style-related states of mind has relied on assessments of defensive processes such as the Adult Attachment Interview (Reference George, Kaplan and MainGeorge et al, 1984). Although this measure has been used for some postnatal studies, for example involving the loss of a child (Reference Hughes, Turton and HopperHughes et al, 2001), it is labour-intensive and its complex, discourse-based scoring methods are potentially problematic for reliability in psychiatric series and in translation. In contrast, the study of attachment style in terms of social interaction has largely relied on self-report questionnaire assessments (Reference Stein, Jacobs and FergusonStein et al, 1998), which have been validated in the context of either adolescent development (Reference Bartholomew and HorowitzBartholomew & Horowitz, 1991) or romantic relationships (Reference Hazan and ShaverHazan & Shaver, 1994) and mainly in normal populations with little attention to pathological outcomes. This makes the self-report assessments less amenable both to the antenatal context and to cross-cultural settings.
The recent development of the Attachment Style Interview (ASI; Reference Bifulco, Moran and BallBifulco et al, 2002a ) has allowed intensive measurement of adult attachment style in psychiatric epidemiological series. Specifically, it has been tested in community-based studies of women and in relation to onset of major depression (Bifulco et al, Reference Bifulco, Moran and Ball2002a ,Reference Bifulco, Moran and Ball b ). The measure has been designed to identify not only attachment profiles ('enmeshed’,'fearful’,'angry-dismissive’ and'withdrawn’, in addition to'secure’) but also the extent to which such styles are dysfunctional (markedly, moderately or mildly insecure) compared with ‘secure’ (or clearly standard). Although rates of any level of insecure style of around 49% were found, similar to rates found with self-report assessments (Reference Mickelson, Kessler and ShaverMickelson et al, 1997), rates with more dysfunctional styles (markedly or moderately insecure) accounted for only 18%. Only these levels of insecurity consistently predicted major depression prospectively when controls were included for initial disorder, with rates of 44% compared with 17% of those with ‘standard’ ratings (either secure or mildly insecure). Markedly or moderately insecure attachment was also closely related to other depression vulnerability factors such as conflict in marriage, poor support and low self-esteem, as well as childhood experience of neglect and abuse, all consistent with attachment theory hypotheses (Reference Bifulco, Moran and BallBifulco et al, 2002b ).
The ASI is an investigator-based measure, where the researcher rather than the respondent makes the judgement in scoring the characteristics of attachment style and support, based on full narrative information collected with probing questions for full details. Rating thresholds are determined by prior training and reference to a manual of precedent benchmarked examples. The ASI measure combines both support assessment (quality of support from partner and at least one person defined as ‘very close’) and attachment attitudes reflecting anxiety/ambivalence (e.g. desire for engagement with others; intolerance of separation; fear of intimacy) and avoidance/distance (e.g. mistrust; constraints on closeness; self-reliance; anger) in maintaining relationships. A judgement of overall attachment style is based both on the ability to make intimate relationships as evidenced by interaction with partner and close support figures, and on the pervasiveness of avoidant or anxious attitudes. Higher insecurity is rated for those who have no supportive others, or who are in conflictful and unsupportive relationships and who have distorted attitudes to closeness and/or self-reliance.
Transcultural Study of Postnatal Depression
The aim of the Transcultural Study of Postnatal Depression (TCS-PND) was to develop (or modify), translate and validate research instruments that could be used in future studies of postnatal depression in different countries and cultures. The instruments were chosen to assess key aspects of the maternity experience, namely clinical diagnosis, the psychosocial context of pregnancy and motherhood, maternal attachment style, mother-infant interaction, the child's environment, and health service structure, use and its associated costs. The modified and translated research tools were piloted to test how well they worked in a perinatal setting and in different languages and populations. The piloting of the ASI to assess maternal attachment style, reported in the present paper, is part of the TCS-PND.
METHOD
Study sites
Nine centres in eight countries participated in the adult attachment component of the study: Bordeaux (France), Dublin (Ireland), Florence (Italy), Iowa City (USA), Keele (UK), Paris (France), Porto (Portugal), Vienna (Austria) and Zurich (Switzerland). Researchers from these centres were trained in the use of the ASI. Details are given in the paper by Asten et al (Reference Asten, Marks and Oates2004, this supplement).
Sample
Full details of the sample selection are also given by Asten et al (Reference Asten, Marks and Oates2004, this supplement). The series was not established as representative of the population of all study centres; women were approached at antenatal clinics or classes and invited to participate. All were provided with information about the study and asked to give signed consent to comply with local ethics committee requirements. Sample sizes varied in each centre, with a total of 296 participating in the study as a whole. The ASI was administered to a subsample of 204 women antenatally and to 96 of the 174 women seen postnatally.
For comparative purposes a London-based study of a series of 80 women, interviewed with the ASI in the 1990s, is referred to when examining the prevalence of insecure attachment style in the series as a whole. Unlike the current sample these women were not pregnant, but were selected from a questionnaire screening of women aged 20-45 registered with general practitioners in north London. Full details of the sample are given elsewhere (Reference Bifulco, Moran and BallBifulco et al, 2002a ).
Interview procedure
Interviews were undertaken in the third trimester of pregnancy. The existing English version of the ASI was used by three centres, and the measure was translated into four languages: French, German, Portuguese and Italian. Five centres also administered the ASI at follow-up 6 months postnatally (Bordeaux, Paris, Vienna, Zurich and Porto). Attrition rates were similar across centres.
Other measures
The Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I; Reference First, Spitzer and GibbonFirst et al, 1994) is a semi-structured interview used for DSM-IV depression diagnoses (American Psychiatric Association, 1994). In this study a research version designed for use with non-patient populations, the SCID-I/NP (Reference First, Gibbon and SpitzerFirst et al, 1996), was modified to produce an instrument for assessing postnatal depression in different cultural contexts, the SCID-PND (Reference Gorman, O'Hara and FigueiredoGorman et al, 2004, this supplement). The SCID-PND was administered at both antenatal and postnatal interviews, thus providing a continuous assessment of depressive disorder from the beginning of pregnancy up to 6 months postnatally. Diagnoses were made of both major and minor depression according to DSM-IV, and time of onset was recorded. A combined variable of either major or minor episodes is used here as the dependent variable.
Training and reliability
A 2-day training course was provided at the beginning of the study. All trainees were provided with a manual of precedent rating examples to aid reliability. Each team was required to send back to the London team ratings for their first five interviews, which were checked (by A.B.), and any difference in rating reported back. Teams were encouraged to e-mail questions about difficult ratings, to ensure consistency. In addition, face-to-face meetings were held with team leaders, when requested, to discuss ratings.
Analyses
The Statistical Package for the Social Sciences version 9 was used for statistical analysis, with reliability and stability correlations using Cohen's κ, Pearson's r and γ. Chi-squared testing with Yates' correction was used to examine differences in social factors and disorder rates between those with and without insecure attachment. Binary logistic regression was used to examine type of attachment style in relation to disorder outcomes controlling for study centre.
RESULTS
Reliability of ASI
Two characteristics of the ASI measure were examined: interrater reliability between the study centres and the London rating thresholds, and stability of ratings between the antenatal and postnatal interviews. Although the latter does not necessarily constitute a standard test-retest reliability given the potential for change due to the baby's birth, nevertheless moderate stability would be expected given the short (9-month) follow-up period, the relatively low risk of the women in the series and the stability of attachment style reported in other studies (Reference Sagi, van Ijzendoorn and ScharfSagi et al, 1994; Reference ScharfeScharfe, 1994; Reference Stein, Jacobs and FergusonStein et al, 1998).
Interrater reliability
Formal interrater reliability testing was undertaken on 35 participants from seven centres. Each of the centres chose five consecutive participants (excluding those checked in the training procedure), including at least one with a ‘highly insecure’ attachment rating. All the attachment material was sent in translation by e-mail to the London team and rated (masked to original scorings) by a researcher trained in the ASI but not involved in the study. Later, the original scorings were collated and compared with the London ratings. Levels of agreement for the derived overall attachment style variables used in the analysis were satisfactory. Using weighted κ, ‘degree of insecurity of attachment’ reached 0.72, type of attachment at any level of insecurity 0.74, type of markedly insecure style 0.84, and anxious style v. avoidant or secure style, 0.73. The relative γ ratings ranged from 0.81 to 1.00 and Pearson's r from 0.74 to 0.93. All were significant at P<0.0001.
Stability
The ASI was administered postnatally to just over half of the mothers seen at follow-up (96 of 174). Attachment style proved to be relatively stable. When the scale was dichotomised, the same level of insecurity as indicated by’ marked/moderate’ v.'mild/none’ held for 85% of women (82 of 96) at both interviews. The small number who changed were equally likely to develop greater security (n=8) or insecurity (n=6) after the baby's birth. When any level of insecurity, including mild levels (i.e.'marked’ through to'mild’), v.'clearly’ secure was examined at both interviews, 77% (74 of 96) retained the same classification. Here there was greater movement towards security postnatally (n=17) than to insecurity (n=5). Correlations between antenatal and postnatal ASI ratings ranged from 0.50 to 0.59 for weighted κ values, with γ from 0.67 to 0.90 and Pearson r from 0.57 to 0.63. All were significant at P<0.0001.
Prevalence of insecure attachment
Degree of insecure attachment
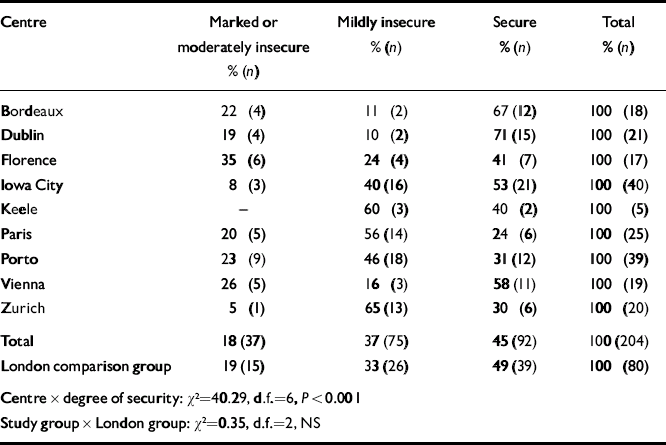
The total prevalence of insecure attachment was examined in the series as well as by study centre. The aim was to see whether the pooled series had comparable rates to those previously obtained in the London series. Because of the small numbers in each centre and their varying demographic composition, no attempt was made to account for differences between centres. Table 1 shows the distribution of insecure attachment ratings across the series. Although variation between centres existed, the average rates of 18% for marked or moderate insecurity and 36% for mild insecurity proved almost identical to the London rates shown in the last row of the table. However, given that differences between study centres were statistically significant (P<0.001) and that the purpose of the analysis was to examine the series as a whole and not by study centre, this element was controlled in final analyses of insecure attachment and depression, to guard against possible bias from unaccounted differences in samples in the various sites.
Table 1 Prevalence of insecure attachment in nine study centres: degree of insecure attachment style
| Centre | Marked or moderately insecure % (n) | Mildly insecure % (n) | Secure % (n) | Total % (n) |
|---|---|---|---|---|
| Bordeaux | 22 (4) | 11 (2) | 67 (12) | 100 (18) |
| Dublin | 19 (4) | 10 (2) | 71 (15) | 100 (21) |
| Florence | 35 (6) | 24 (4) | 41 (7) | 100 (17) |
| Iowa City | 8 (3) | 40 (16) | 53 (21) | 100 (40) |
| Keele | - | 60 (3) | 40 (2) | 100 (5) |
| Paris | 20 (5) | 56 (14) | 24 (6) | 100 (25) |
| Porto | 23 (9) | 46 (18) | 31 (12) | 100 (39) |
| Vienna | 26 (5) | 16 (3) | 58 (11) | 100 (19) |
| Zurich | 5 (1) | 65 (13) | 30 (6) | 100 (20) |
| Total | 18 (37) | 37 (75) | 45 (92) | 100 (204) |
| London comparison group | 19 (15) | 33 (26) | 49 (39) | 100 (80) |
Type of insecure attachment
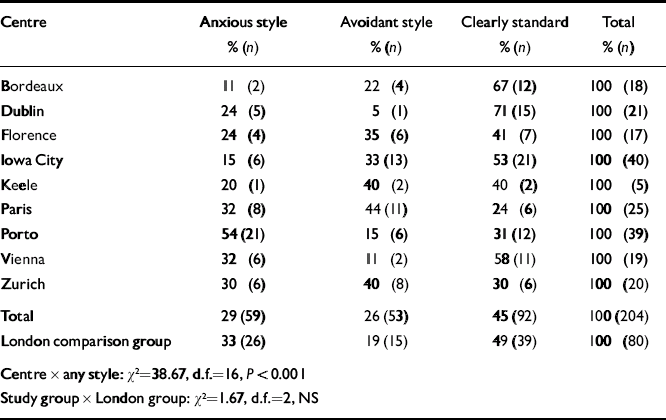
When insecure attachment style was examined using the full five-style classification there were substantial differences between centres (P<0.005). However, in the pooled series, just under half of the women were found to be clearly standard/secure (45%), with fairly equal distribution between the other styles ranging from 13% for’ enmeshed’, 15% for'fearful’, 10% for’ angry-dismissive’ and 16% for'withdrawn’. These rates proved to be statistically similar to the London rates of 9%, 6%, 24% and 13%, respectively. Because of small numbers per study centre, the styles were grouped into'anxious’ style (enmeshed or fearful at marked to mild levels) and'avoidant’ style (angry-dismissive or withdrawn at marked to mild levels) and compared with secure/clearly standard. This simplified classification is consistent with a number of other attachment measures which use a threefold scheme (anxious, avoidant and secure style), and the results of factor meta-analysis of different instruments (Reference Brennan, Clark, Shaver, Simpson and RholesBrennan et al, 1998). Table 2 shows the distribution of these styles by study centre. Again, differences were evident (P<0.001), but overall the total rates were statistically similar to those found in the London comparison study. There was fairly equal distribution of 29%'anxious’ and 26%’ avoidant’ ratings but the majority (45%) were rated secure. When only those markedly or moderately insecure were examined separately, 10% were rated as'anxious’ and 8% as'avoidant’, compared with 82%'secure’ (including mildly insecure). These were almost identical to the London rates (11%, 8% and 81% respectively, NS).
Table 2 Prevalence of insecure attachment in nine study centres: type of insecure style
| Centre | Anxious style % (n) | Avoidant style % (n) | Clearly standard % (n) | Total % (n) |
|---|---|---|---|---|
| Bordeaux | 11 (2) | 22 (4) | 67 (12) | 100 (18) |
| Dublin | 24 (5) | 5 (1) | 71 (15) | 100 (21) |
| Florence | 24 (4) | 35 (6) | 41 (7) | 100 (17) |
| Iowa City | 15 (6) | 33 (13) | 53 (21) | 100 (40) |
| Keele | 20 (1) | 40 (2) | 40 (2) | 100 (5) |
| Paris | 32 (8) | 44 (11) | 24 (6) | 100 (25) |
| Porto | 54 (21) | 15 (6) | 31 (12) | 100 (39) |
| Vienna | 32 (6) | 11 (2) | 58 (11) | 100 (19) |
| Zurich | 30 (6) | 40 (8) | 30 (6) | 100 (20) |
| Total | 29 (59) | 26 (53) | 45 (92) | 100 (204) |
| London comparison group | 33 (26) | 19 (15) | 49 (39) | 100 (80) |
Attachment style and social risk variables
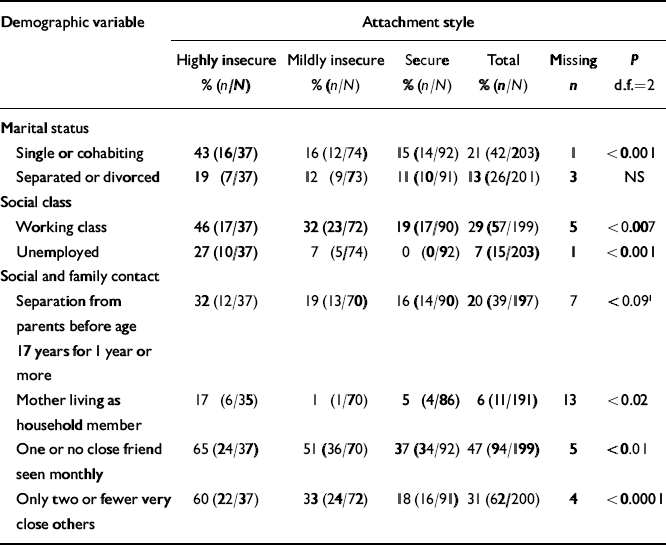
Attachment style was examined in relation to demographic characteristics such as social class and employment, as well as to marital status and social and family contact. Expected associations would confer criterion validation to the attachment measure and construct. Table 3 shows that degree of insecure attachment was significantly related not only to economic factors (lower social class and unemployment) but also to marital status (being single or cohabiting). However, insecure attachment style was not significantly related to prior marital separation. Those with highly insecure attachment were more likely to have their mother living in the household, more likely to have fewer than two others named as’ very close’ and less likely to see a friend at least monthly.
Table 3 Insecurity of attachment style and social factors
| Demographic variable | Attachment style | |||||
|---|---|---|---|---|---|---|
| Highly insecure % (n/N) | Mildly insecure % (n/N) | Secure % (n/N) | Total % (n/N) | Missing n | P d.f.=2 | |
| Marital status | ||||||
| Single or cohabiting | 43 (16/37) | 16 (12/74) | 15 (14/92) | 21 (42/203) | 1 | <0.001 |
| Separated or divorced | 19 (7/37) | 12 (9/73) | 11 (10/91) | 13 (26/201) | 3 | NS |
| Social class | ||||||
| Working class | 46 (17/37) | 32 (23/72) | 19 (17/90) | 29 (57/199) | 5 | <0.007 |
| Unemployed | 27 (10/37) | 7 (5/74) | 0 (0/92) | 7 (15/203) | 1 | <0.001 |
| Social and family contact | ||||||
| Separation from parents before age 17 years for 1 year or more | 32 (12/37) | 19 (13/70) | 16 (14/90) | 20 (39/197) | 7 | <0.091 |
| Mother living as household member | 17 (6/35) | 1 (1/70) | 5 (4/86) | 6 (11/191) | 13 | <0.02 |
| One or no close friend seen monthly | 65 (24/37) | 51 (36/70) | 37 (34/92) | 47 (94/199) | 5 | <0.01 |
| Only two or fewer very close others | 60 (22/37) | 33 (24/72) | 18 (16/91) | 31 (62/200) | 4 | <0.0001 |
Only one measure of childhood experience was included - that of separation from either parent before age 17 years. This is known to be highly related to the more toxic experiences of neglect and abuse that relate to adult depressive disorder (Reference Bifulco and MoranBifulco & Moran, 1998). An association was confirmed. Although separation from parents fell short of statistical significance when examined with the threefold security rating (P<0.09, see Table 3), when dichotomised, those with marked or moderate levels of insecurity were more likely to have lost a parent in childhood (31%; 12 of 39) than those with lower levels of insecurity (16%; 25 of 158, P<0.03).
Attachment style and depression
Fifteen per cent of women (22 of 147) had an onset of major or minor depression in pregnancy. A similar percentage (19%; 33/174) had an onset in the first 6 months postnatally. When the 9 women with depression at antenatal interview were excluded, this constituted 15% (24/165) of women with a new onset postnatally. Onset of major depression postnatally was rare at only 4% (8 women), and major and minor onsets of depression were therefore combined in this analysis. Those with an insecure attachment style in the third trimester of pregnancy were significantly more likely to have onset of depression in pregnancy, with a'dose-response’ effect observed for degree of insecurity and onset of depression (Table 4). The same results held when those depressed at first interview when the ASI was administered were excluded.
Table 4 Insecure attachment style and depression in pregnancy

| Attachment style | Onset of major or minor depression in pregnancy % (n/N) |
|---|---|
| Degree of insecurity | |
| Marked/moderate | 22 (8/37) |
| Mild | 12 (9/74) |
| None | 6 (5/91) |
| P<0.02, d.f.=2 | |
| Anxious style | |
| Marked/moderate | 15 (3/20) |
| Mild | 5 (2/38) |
| Not anxious | 12 (17/144) |
| NS, d.f.=2 | |
| Avoidant style | |
| Marked/moderate | 29 (5/17) |
| Mild | 19 (7/36) |
| Not avoidant | 7 (10/149) |
| P<0.003, d.f.=2 |
Antenatal depression
Attachment style was examined in relation to depression in pregnancy. A significant correlation was found only for'withdrawn’ style (r=0.22, P<0.001), but this held when both withdrawn and angry-dismissive groups were combined in the avoidant category (r=0.23, P<0.001). No association was found for the anxious category (r=0.01, NS), nor for its component styles (both enmeshed and fearful, r=0.10, NS) and depression in pregnancy. The analysis was repeated using χ2 to test the association between avoidant style and depression in pregnancy, and the findings were confirmed (P<0.003, Table 4). Anxious style was again shown to be unrelated to depression in pregnancy (Table 4). Logistic regression confirmed that the avoidant style provided the best predictor of onset of depression in pregnancy, even when controlling for study centre (Table 5).
Table 5 Logistic regression (outcome: onset of depression in pregnancy)1

| Variable | Odds ratio | Wald test | d.f. | P |
|---|---|---|---|---|
| Anxious style2 | 1.58 | 1.45 | 1 | NS |
| Avoidant style2 | 2.95 | 10.72 | 1 | 0.001 |
| Study centre | 0.96 | 1.32 | 1 | NS |
Postnatal depression
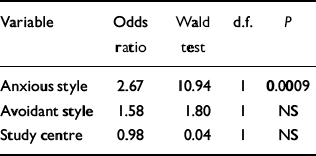
Finally, the analysis was repeated for postnatal onset of depression once those with depression at the point of antenatal interview were excluded (Table 6). Again, insecurity of attachment was related to postnatal onset (P<0.009). In terms of attachment style, correlational analysis showed that'enmeshed’ style (r=0.18, P<0.01) and'fearful’ style (r=0.20, P<0.009) were both significantly related to postnatal onset. Neither'angrydismissive’ (r=0.02, NS) nor'withdrawn’ (r=0.02, NS) styles were related to postnatal depression. Chi-squared analysis confirmed that those with anxious attachment styles were significantly more likely to experience depression postnatally (P<0.004, Table 6), but not those with avoidant styles. Logistic regression confirmed that only anxious attachment style was required to predict postnatal depression, with controls applied for study centre (Table 7).
Table 6 Attachment style and postnatal depression (major or minor depression)

| Attachment style | Onset of depression postnatally % (n/N) |
|---|---|
| Degree of insecurity | |
| Marked/moderate | 31 (9/29) |
| Mild | 26 (16/62) |
| None | 10 (8/83) |
| P<0.009, d.f.=2 | |
| Anxious style | |
| Marked/moderate | 38 (6/16) |
| Mild | 33 (11/33) |
| None | 13 (16/125) |
| P<0.004, d.f.=2 | |
| Avoidant style | |
| Marked/moderate | 23 (3/13) |
| Mild | 17 (5/29) |
| None | 19 (25/132) |
| NS, d.f.=2 |
Table 7 Logistic regression (outcome: onset of depression 6 months postnatally)1
| Variable | Odds ratio | Wald test | d.f. | P |
|---|---|---|---|---|
| Anxious style | 2.67 | 10.94 | 1 | 0.0009 |
| Avoidant style | 1.58 | 1.80 | 1 | NS |
| Study centre | 0.98 | 0.04 | 1 | NS |
DISCUSSION
The study demonstrates successful use of the Attachment Style Interview in European and US settings. Interrater reliability was high and ASI ratings were relatively stable across antenatal and postnatal interviews. Almost no modification of the measure was required in its administration across nine different centres and in five languages. Insecure attachment style was related to more adverse social conditions: to lower social class and unemployment, being single or cohabiting, having less support and fewer social contacts, and more disrupted childhood experience.
The study confirms an association of insecure attachment style with both antenatal and postnatal depression. Specificity of style and the timing of depression were found, with subjects exhibiting avoidant styles (angry-dismissive or withdrawn) more likely to have an onset of depression in pregnancy, and those exhibiting anxious styles (enmeshed or fearful) to suffer depression postnatally. Despite variations of attachment style in different study centres, the association with depression remained when controls were included for centre status.
Limitations of the study
The small samples at most centres were potentially unrepresentative of the wider population and precluded meaningful analysis of cultural differences in attachment style. The London series used for partial comparison was an imprecise match, given that it was not an antenatal series nor was it closely matched for demographic characteristics. The possibility of bias needs to be considered, given that the interviewer was aware of antenatal or postnatal status and of attachment style and depression during the course of the interview. However, given the nature of the standardised interview measures used, the reliability and stability of the ASI over time and the lack of a prior hypothesis relating to the timing of attachment style and disorder, it is difficult to see how this would have influenced findings in any consistent way.
The combining of styles into'anxious’ and ‘avoidant’ was done largely for pragmatic reasons because of the small numbers with particular insecure styles and to give a more compact analysis of results across study centres. Although repeating the analysis on the full five-style classification seemed consistent with the abbreviated three-style grouping, further investigation on larger numbers may indicate yet more subtle associations between each of the styles and different experiences and risks associated with pregnancy and birth. Thus, although both ‘enmeshed’ and ‘fearful’ styles do involve anxious elements in attachment and on this basis merit being combined, other bases for combining could be conceptualised: for example, ‘fearful’ and ‘withdrawn’ styles both involve behavioural avoidance, and ‘enmeshed’ and ‘angry-dismissive’ styles both involve ambivalence. The grouping used in this analysis should not preclude future exploration of styles individually or in other combinations.
The combining of both minor and major depression as the outcome variable might have blurred the association of attachment style with the more pernicious clinical level disorder. Previous analysis of the ASI has only examined its status as a vulnerability factor for major depression. In this analysis both major and minor levels of depression were combined, largely because of the low rates of disorder. Further study of the relationship of attachment style with minor and subclinical level disorder is required in order to establish threshold effects.
Merits of the study
The merits of the study include its use of interview assessments of both attachment style and depression (which militate against biased self-reporting), the high levels of reliability achieved, the prospective nature of the study with controls applied for depression at time of assessment, and the relatively large number in the sample overall.
Explanation of the study findings
The finding that differential timing of depression applies to those with avoidant and anxious attachment styles needs further investigation. A cognitive-emotional explanation is that women with avoidant styles might experience the pregnancy itself as intrusive, given their barriers to forming close ties and sustaining close contact with others. Thus, the pregnancy could be seen as causing psychological conflict which, in turn, produces symptoms. After the birth, boundaries and relative distance can be reestablished, resulting in symptom reduction. In contrast, for women with anxious styles, a baby in the womb may fulfil needs for enmeshing closeness and fear of separation, which would be threatened by even brief separations from the child once born, thus increasing symptom levels postnatally. An alternative explanation concerns social support. This could identify disorder as associated with changes in the marital and supportive context associated with pregnancy and birth, which will have different effects depending on the individual's attachment style. For example, neediness expressed by those with anxious styles might be more difficult for support figures to satisfy when there is competition for attention from the new baby. This might lead to jealousy and conflicts with partner and/or close others in attending to the baby. In contrast, those with avoidant styles might feel physically more vulnerable in pregnancy and need support, but be impeded in eliciting it by their prior typically independent, autonomous behaviour. Existing support arrangements might not be readily responsive to changed levels of neediness. Further investigation of this is possible within this sample. Another issue requiring further investigation - and only briefly touched on in this analysis - is the move towards greater security of attachment for 18% of women after the baby's birth. This needs to be explored in a larger series in which the ASI is used routinely at both antenatal and postnatal contacts. In the current analysis numbers precluded investigation of the impact of depressive symptoms on changes in attachment status at follow-up.
Future applications of the ASI
The study has shown that the ASI can be used successfully in different European and US centres. The centres all expressed satisfaction with the psychometric properties of the measure and (given that the researchers were all clinicians) most found the blend of quantitative and qualitative elements meaningful for investigating psychosocial risks in pregnancy. At least three centres are in the process of using the measure on new series with further training sessions provided for their research teams locally.
This analysis has taken a universal (etic) approach to cross-cultural assessment, expecting similarities in social attachment behaviour across cultures (Reference Van Ijzendoorn, Sagi, Cassidy and Shavervan Ijzendoorn & Sagi, 1999). This is justified by a number of studies showing similar patterns of attachment behaviour across diverse cultural contexts, and is useful in cross-cultural psychopathological studies in showing that dysfunctional styles similarly relate to depressive disorder. However, this is not to deny the relevance of emic approaches, which seek to find different social and behavioural configurations specific to culture. The Western European and US cultures represented in this series would not be expected to show large variations in social behaviour, given the similarities in marital and family patterns, social class and religious affiliation. For example, nearly all women in this series were living in a nuclear family, with a partner who was the father of the baby - few lived with their extended family, and only 6% had their mother living in the household. However, rates of different attachment styles did vary substantially between study centres, and it is possible that interesting cultural differences were masked by the study procedure and would benefit from further investigation.
Given the preliminary success in using the ASI, further interesting analyses are possible: for example, the question of whether insecure attachment style as denoted by inability to access support related to inappropriate service use - in particular whether anxious and avoidant styles relate to different patterns of service use, and to use at different points in the childbearing process. Another topic worth investigating is whether insecure parent attachment style relates to impaired interactions with the baby, involving distance or intrusiveness, over and above those related to depressive disorder. The use of the ASI in further investigation of maternal risk related to childbirth will allow the exploration of such issues.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Insecure attachment style in pregnant women in significantly associated with depressive disorder and predicts onset of depression postnatally.
-
▪ The association of type of attachment style, poor support and timing of depression in relation to childbirth has implications for the type of intervention offered at different points during pregnancy and postnatally.
-
▪ The reliable use of the Attachment Style Interview in different European and US centres indicates it can be used as an assessment of risk for postnatal depression in varied international contexts.
LIMITATIONS
-
▪ Samples were not representative of each centre investigated.
-
▪ The relationship of insecure attachment style to major v. minor depressive disorder was not ascertained owing to relatively low disorder rates.
-
▪ Investigation of cultural differences in attachment style across different centres was not possible.
Acknowledgement
We thank Catherine Jacobs who undertook ASI reliability ratings in. London.












eLetters
No eLetters have been published for this article.