Some physical illnesses, particularly diabetes and coronary heart disease, occur with increased frequency in patients with schizophrenia and major depression (Reference Peet and EdwardsPeet & Edwards, 1997; Reference Ryan and ThakoreRyan & Thakore, 2002). These physical illnesses share some epidemiological features with mental disorders. Thus, the outcome of schizophrenia is generally better in developing countries than in more ‘developed’ nations (Reference Hopper and WanderlingHopper & Wanderling, 2000). Similarly, diabetes and heart disease are regarded as diseases of Western industrialised nations and are less common in developing countries (Reference Tucker and BuranapinTucker & Buranapin, 2001). It is well recognised that the pattern of food intake is of substantial importance in the aetiology of diabetes and heart disease. In view of the clinical and epidemiological association between these mental and physical illnesses, it is surprising that there has been little research interest in the relationship between nutrition and mental illness. The present study is an ecological analysis of international variations in food supply in relation to epidemiological data on the outcome of schizophrenia and on the prevalence of depression.
METHOD
Existing databases on international variations in the outcome of schizophrenia, the prevalence of depression and patterns of food usage were identified. For the outcome of schizophrenia, 2-year outcome data from the International Pilot Study of Schizophrenia (IPSS; World Health Organization, 1979) and the Determinants of Outcome of Severe Mental Disorders (DOSMED) study (Reference Jablensky, Sartorius and EmbergJablensky et al, 1992) were used. From the IPSS study, data on mean days out of hospital and percentage of patients with severe social impairment were used as outcome variables, as well as a total outcome score, as described by Christensen & Christensen (Reference Christensen and Christensen1988). This total outcome score is a composite score that takes into account all outcome measures in the IPSS study. In the DOSMED study, data on percentage of patients never hospitalised and percentage of patients with little social impairment were used for analysis. Where data for urban and rural populations were given separately, the urban data were used for analysis. In addition, a ‘total best outcome’ score was calculated from all the outcome measures listed in Table 4.10 from Jablensky et al (Reference Jablensky, Sartorius and Emberg1992). This was calculated by adding together the percentages of patients with ‘best possible’ outcomes as defined by Jablensky et al (Reference Jablensky, Sartorius and Emberg1992), namely: remitting course with full remissions; in psychotic episodes, 1–5% of follow-up period; in complete remission, 76–100% of follow-up period; on no antipsychotic medication throughout follow-up; never hospitalised; and unimpaired social functioning for 76–100% of follow-up period. The use of this composite outcome score ensured that all outcome variables were taken into account. Data on international variations in the prevalence of depression in the population were taken from the study of Weissman et al (Reference Weissman, Bland and Canino1996), plus data from Japan as used in the analysis by Hibbeln (Reference Hibbeln1998).
The countries included in the analysis were: Denmark, India, Colombia, Nigeria, UK, USSR, USA and Czechoslovakia for the IPSS study; Denmark, India, Colombia, Ireland, USA, Nigeria, USSR, Japan, UK and Czechoslovakia for the DOSMED study; and New Zealand, Canada, Germany, France, USA, USSR, Taiwan and Japan for the depression study. No data on social outcome were available for Japan. Data on food usage were taken from the FAOSTAT database (Food and Agriculture Organization, 2002), which records the apparent national food consumption. This is estimated from the total domestic production of food (including non-commercial production and production from kitchen gardens) plus imports, minus exports, taking into account changes in stocks such as stored grain and minus the food lost to waste during commercial processing. The following foodstuffs were included in the analysis: meat (including beef, mutton, goat, pig and poultry); fish and seafood; eggs; dairy products (milk, cheese, butter and ghee); vegetable oil, vegetables; cereals (excluding beer); fruits (excluding wine); starchy roots; refined sugar; pulses; nuts; coffee; and alcoholic beverages. All were expressed as supply in kilograms per capita per year. Food consumption data were taken for the year that approximated to the time when the clinical studies were conducted (1970 for the IPSS study, 1980 for the DOSMED study and 1990 for the depression prevalence study). It was not considered necessary to analyse more than one year because national food consumption patterns change slowly over decades and there is little variation from year to year.
Each foodstuff group was correlated with each of the clinical databases. Stepwise multiple regression was then carried out using the Statistical Package for the Social Sciences for Windows, Version 11.5, with the clinical measures as dependent variables and dietary measures as independent variables.
RESULTS
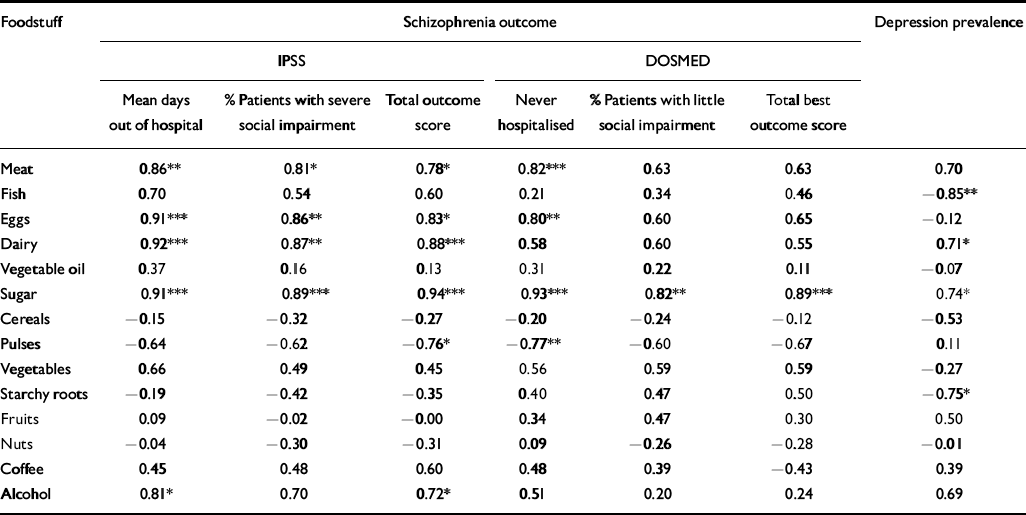
The results of the multiple (Pearson) correlations are shown in Table 1. The most consistent finding is that a greater consumption of refined sugar is associated with a worse outcome of schizophrenia and a greater prevalence of depression. In the schizophrenia data-sets, a high correlation with sugar consumption was seen both for outcome measures based on hospital admission and those based on social outcome. Other correlations that were found in both schizophrenia data-sets but not necessarily for both admission and social outcome measures included the consumption of meat and eggs (adverse relationship) and the consumption of pulses (beneficial relationship). Dairy products and alcohol consumption were associated with a poor outcome in the IPSS study but not in the DOSMED database. With regard to depression, the strongest association was between a high dietary intake of fish and seafood and reduced prevalence of depression. A high intake of dairy products and sugar was associated with an increased prevalence of depression, whereas a high intake of starchy roots was associated with a reduced prevalence of depression.
Table 1 Pearson correlation coefficients between both the schizophrenia 2-year outcome variables and depression prevalence and the composition of the national diet
| Foodstuff | Schizophrenia outcome | Depression prevalence | |||||
|---|---|---|---|---|---|---|---|
| IPSS | DOSMED | ||||||
| Mean days out of hospital | % Patients with severe social impairment | Total outcome score | Never hospitalised | % Patients with little social impairment | Total best outcome score | ||
| Meat | 0.86** | 0.81* | 0.78* | 0.82*** | 0.63 | 0.63 | 0.70 |
| Fish | 0.70 | 0.54 | 0.60 | 0.21 | 0.34 | 0.46 | — 0.85** |
| Eggs | 0.91*** | 0.86** | 0.83* | 0.80** | 0.60 | 0.65 | — 0.12 |
| Dairy | 0.92*** | 0.87** | 0.88*** | 0.58 | 0.60 | 0.55 | 0.71* |
| Vegetable oil | 0.37 | 0.16 | 0.13 | 0.31 | 0.22 | 0.11 | — 0.07 |
| Sugar | 0.91*** | 0.89*** | 0.94*** | 0.93*** | 0.82** | 0.89*** | 0.74* |
| Cereals | — 0.15 | — 0.32 | — 0.27 | — 0.20 | — 0.24 | — 0.12 | — 0.53 |
| Pulses | — 0.64 | — 0.62 | — 0.76* | — 0.77** | — 0.60 | — 0.67 | 0.11 |
| Vegetables | 0.66 | 0.49 | 0.45 | 0.56 | 0.59 | 0.59 | — 0.27 |
| Starchy roots | — 0.19 | — 0.42 | — 0.35 | 0.40 | 0.47 | 0.50 | — 0.75* |
| Fruits | 0.09 | — 0.02 | — 0.00 | 0.34 | 0.47 | 0.30 | 0.50 |
| Nuts | — 0.04 | — 0.30 | — 0.31 | 0.09 | — 0.26 | — 0.28 | — 0.01 |
| Coffee | 0.45 | 0.48 | 0.60 | 0.48 | 0.39 | — 0.43 | 0.39 |
| Alcohol | 0.81* | 0.70 | 0.72* | 0.51 | 0.20 | 0.24 | 0.69 |
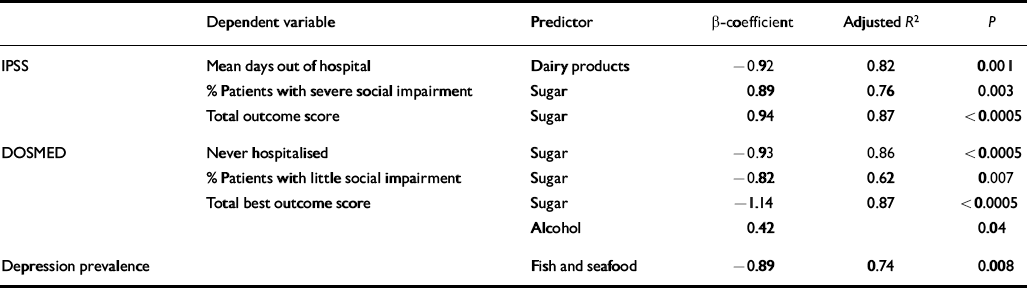
The results of the multiple regression analysis are shown in Table 2. The most striking relationship in the schizophrenia databases is between sugar consumption and outcome. This was an independent predictor of poor outcome of schizophrenia as judged by both social and hospital admission criteria, as well as the total outcome score. An exception to this was the hospital admission data from the IPSS study, in which increased intake of dairy products predicted fewer days spent out of hospital. Also, alcohol consumption was found to be an additional weak but significant positive predictor of overall ‘total best outcome’ in the DOSMED study, although this accounted for only a very small part of the variance relative to sugar. All of these associations predicted the majority of variance in the outcome of schizophrenia.
Table 2 Multiple regression analysis of food categories in the national diet as predictors of the outcome of schizophrenia and prevalence of depression
| Dependent variable | Predictor | β -coefficient | Adjusted R 2 | P | |
|---|---|---|---|---|---|
| IPSS | Mean days out of hospital | Dairy products | — 0.92 | 0.82 | 0.001 |
| % Patients with severe social impairment | Sugar | 0.89 | 0.76 | 0.003 | |
| Total outcome score | Sugar | 0.94 | 0.87 | <0.0005 | |
| DOSMED | Never hospitalised | Sugar | — 0.93 | 0.86 | <0.0005 |
| % Patients with little social impairment | Sugar | — 0.82 | 0.62 | 0.007 | |
| Total best outcome score | Sugar | — 1.14 | 0.87 | <0.0005 | |
| Alcohol | 0.42 | 0.04 | |||
| Depression prevalence | Fish and seafood | — 0.89 | 0.74 | 0.008 |
The sole independent predictor of depression prevalence emerging from the multiple regression analysis was the consumption of fish and seafood, which predicted the prevalence of depression with an adjusted R 2 of 0.74.
DISCUSSION
The results of this analysis allow the hypothesis that the outcome of schizophrenia and prevalence of depression are influenced by dietary factors.
Diet and outcome of schizophrenia
The finding that the outcome of schizophrenia is better in developing than in developed countries has never been satisfactorily explained and does not appear related simply to confounding factors such as diagnostic differences and selective outcome measures (Reference Hopper and WanderlingHopper & Wanderling, 2000). Christensen & Christensen (Reference Christensen and Christensen1988) reported a correlation between international variations in outcome of schizophrenia according to the IPSS study and the ratio in the diet of animal (mainly saturated) fat to fish and vegetables (mainly polyunsaturated) fats. This was reflected in the present study, where correlations were shown between a higher consumption of meat and dairy products and a worse outcome of schizophrenia. However, strong intercorrelations are found between various dietary constituents, and on multiple regression analysis it was sugar consumption that was the predominant predictor of poor outcome in schizophrenia. Exceptions to this were that the consumption of dairy products predicted hospital admission in the IPSS study, and alcohol was a weak predictor of global good outcome in the DOSMED study. Therefore, the dominant and robust finding of this analysis is the predictive value of sugar consumption.
Diet and prevalence of depression
There has been recent interest in the relationship between fish consumption and depression. Hibbeln & Salem (Reference Hibbeln and Salem1995) noted that the increased prevalence of depression in the 20th century parallels the increased rates of coronary heart disease that are thought to be associated with altered dietary patterns, including reduced dietary intake of omega-3 polyunsaturated fatty acids. Hibbeln (Reference Hibbeln1998) has subsequently demonstrated striking correlations between dietary fish intake and international variations in major depression. Using the same depression database as Hibbeln (Reference Hibbeln1998), we have confirmed the relationship between fish consumption and international variations in rates of depression, and also found that sugar consumption relates to the prevalence of depression. This had been noted previously by Westover & Marangell (Reference Westover and Marangell2002). However, multiple regression analysis shows that fish and seafood consumption provides the strongest and most robust independent predictor of depression prevalence.
Limitations
Association does not prove causation. Diet is partly determined by sociocultural factors, so diet could be a proxy for other social variables. Correlation studies of this type, particularly when taken in conjunction with other sources of information, have their greatest value in generating hypotheses. Issues of cause and effect can be clarified only by intervention studies in which diet is manipulated, by either supplementation or restriction, and mental health outcome is assessed.
Correlations are only as good as the data-sets utilised. The national apparent food consumption data are the best available but they are inexact and do not necessarily reflect the dietary practices of individuals or of population subgroups. This can be done only by case–control or cohort studies in which individual dietary practices are recorded. There are several large prospective studies relating diet to subsequent heart disease, diabetes and cancer, but there are no large prospective studies relating diet to subsequent mental health problems.
The databases used for schizophrenia outcome are well accepted and often cited. The data on major depression prevalence reported by Weissman et al (Reference Weissman, Bland and Canino1996) are derived from rigorous methodologies and are among the most reliable cross-national data available.
It is well recognised that the use of multiple correlations can give rise to spurious associations by chance. Also, multiple regression analysis can be sensitive to the exact regressors entered. However, the breadth of data used in this study has enabled patterns to be identified and this was strengthened by the robust findings from the use of multiple regression analysis.
Implications
Diabetes, coronary heart disease and other related conditions that cluster together have been conceptualised as manifestations of the ‘metabolic syndrome’ (Reference De Fronzo and FerranniniDe Fronzo & Ferrannini, 1991; Reference HansenHansen, 1999). Because these diseases also cluster with schizophrenia and depression, it has been proposed that these mental disorders may share some aetiological factors with physical diseases that constitute the metabolic syndrome (Reference Peet and EdwardsPeet & Edwards, 1997; Reference Ryan and ThakoreRyan & Thakore, 2002). A fundamental abnormality in the metabolic syndrome is insulin resistance (Reference HansenHansen, 1999). Abnormal glucose utilisation reflecting insulin resistance has been demonstrated in patients with depression (Reference Peet and EdwardsPeet & Edwards, 1997). In schizophrenia, abnormalities of glucose utilisation were demonstrated before the introduction of modern antipsychotic drugs (Reference Ryan and ThakoreRyan & Thakore, 2002). Insulin resistance is altered by diet. Regular consumption of significant quantities of foodstuffs with a high ‘glycaemic load’, such as sugar and white bread, which rapidly release glucose into the blood-stream, gives rise to insulin resistance and subsequent susceptibility to diabetes and cardiovascular disease (Reference LudwigLudwig, 2002). A high dietary intake of saturated fat leads to increased insulin resistance, whereas substitution of saturated fat with polyunsaturated fat can reverse this effect and may be protective against future development of insulin resistance (Reference Summers, Fielding and BradshawSummers et al, 2002). The risk of mortality from coronary heart disease is decreased by regular consumption of fish and pulses (Reference MannMann, 2002). Thus, dietary patterns that influence insulin resistance and lead to diseases of the metabolic syndrome are reflected by the dietary predictors of outcome of schizophrenia and prevalence of depression in the present study. It can therefore be hypothesised that insulin resistance and associated metabolic disturbances resulting from dietary factors may account for the clinical association between depression, schizophrenia and the physical diseases of the metabolic syndrome.
An obvious practical consequence of this hypothesis is the possibility that mental health could be improved by dietary manipulation. There have been few controlled trials of nutrition in the treatment of psychiatric disorders. If food with a high glycaemic load is of importance in determining the outcome of schizophrenia, then modification of glycaemic load or its metabolic consequences should be beneficial in the management of schizophrenia. Diets with a low glycaemic load were promoted decades ago as being potentially useful in the treatment of schizophrenia but have been supported only by anecdotal evidence (Reference Meiers, Hawkings and PaulingMeiers, 1973).
With regard to depression, the overriding association was between fish and seafood consumption and prevalence of depression, which supports previous epidemiological data (Reference HibbelnHibbeln, 1998). This leads directly to the proposition that depression should be treatable with omega-3 fatty acids. This proposition has been tested recently, with strong positive antidepressant benefits reported and confirmed (Reference Nemets, Stahl and BelmakerNemets et al, 2002; Reference Peet and HorrobinPeet & Horrobin, 2002). This is now a matter of intense further research.
It is premature to speculate on molecular mechanisms, save to note that a number of potential mechanisms do exist. Insulin receptors are widely distributed in the brain where they are involved in cell signalling and modulate the actions of other neurotransmitters (Reference KyriakiKyriaki, 2003). Also, a high-fat, refined sugar diet has been shown to reduce levels of brain-derived neurotrophic factor in rat hippocampus (Reference Molteni, Barnard and YingMolteni et al, 2002): brain-derived neurotrophic factor promotes a variety of neuromodulatory processes during early development and adulthood and has been implicated in schizophrenia (Reference Durany, Michell and ZochlingDurany et al, 2001).
In conclusion, this study has shown that national dietary factors predict international variations in the outcome of schizophrenia and prevalence of depression. The nutritional predictors are similar to those reported for other ‘Western’ diseases such as diabetes and coronary heart disease, which are more common in people with mental health problems. Whether the relationship between nutritional factors and mental health is causal can be determined only by intervention studies. Initial treatment studies with omega-3 fatty acids in depression are encouraging but other nutritional strategies should be explored.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Variations in the national diet predict international variations in the outcome of schizophrenia and the prevalence of depression.
-
▪ The dietary predictors for mental health are the same as those that are known to be of causal importance for physical health problems, including coronary heart disease and diabetes.
-
▪ These findings allow the hypothesis that nutrition is important in the genesis and maintenance of mental ill health.
LIMITATIONS
-
▪ Data for the national diet are crude and approximate.
-
▪ Diet is partly determined by social factors, so diet could be a proxy for other sociocultural variables.
-
▪ Association does not prove causation. Further dietary intervention studies are required to test the hypothesis.







eLetters
No eLetters have been published for this article.