Cognitive-behavioural therapy involving exposure is effective for anxiety disorders such as phobia and panic (Department of Health, 2001), yet only a small minority of people with these conditions are treated (Reference Bebbington, Brugha and MeitzerBebbington et al, 2000), largely because of fear of stigma, problems in finding a therapist and difficulties in travelling to attend appointments. The computer-aided exposure self-help system FearFighter enabled therapists to treat more patients effectively by offering easy access to FearFighter on stand-alone computers in self-help clinics (Reference Kenwright, Liness and MarksKenwright et al, 2001; Reference Marks, Kenwright and McDonoughMarks et al, 2004). The system was modified to allow internet access at home. This short paper of an open pilot reports the first outcome study of the internet version.
METHOD
Design
We examined the outcomes of the first 10 cases referred for treatment of phobia or panic in which the internet version of FearFighter was used in August 2001, and then, in an uncontrolled, non-randomised comparison, outcomes of the 17 referrals who used the stand-alone FearFighter in a clinic from December 2000 to December 2001.
Procedure
Self-referrals to a computer-aided self-help clinic in west London (Reference Marks, Mataix-Cols and KenwrightMarks et al, 2003) were assessed for suitability using a questionnaire and a 30 min telephone interview. Suitability criteria were presence of phobia or panic disorder (based on an interview checklist of ICD-10 diagnostic criteria; World Health Organization, 1992); motivation to try self-help, and absence of substance misuse, psychosis or active suicidal plans.
Exposure guidance by internet at home
After the telephone interview, suitable candidates who had internet access at home were given unlimited access to FearFighter on the internet for a 12-week period. They never saw the therapist or attended the clinic. The therapist (M.K.) scheduled seven live 10 min support sessions by telephone at weeks 1, 2, 4, 6, 8, 10 and 12.
Exposure guidance on a stand-alone computer at a clinic
After the telephone screening interview, all suitable candidates without home internet access were given appointments to use FearFighter on a stand-alone computer in the clinic at weeks 1, 2, 4, 6, 8, 10 and 12. The therapist gave support at the start and end of each session, for a total of 10 min per session.
Measures
At weeks 0, 12 and 16 (1-month follow-up), patients rated the Fear Questionnaire (FQ; Reference Marks and MathewsMarks & Mathews, 1979), the Work and Social Adjustment scale (Reference Mundt, Marks and ShearMundt et al, 2002) and the Beck Depression Inventory (Reference Beck, Epstein and BrownBeck et al, 1988). Therapists recorded time and content of patient support.
RESULTS
Patient flow
Of the 266 people referred to the clinic, screening identified 56 (21%) who met suitability criteria for treatment of phobia or panic with FearFighter and 154 who were suitable for the clinic's other computer-aided self-help systems for depression, general anxiety and obsessive-compulsive disorder (Reference Marks, Kenwright and McDonoughMarks et al, 2004). A further 56 people were unsuitable for computer-aided treatment and were referred to other services. Of the 56 people suitable for FearFighter, nearly a quarter (13) refused self-help. Of the 43 people who began using FearFighter, 16 (37%) dropped out before completion of treatment - all after using FearFighter at the clinic.
Participants
The 4 women and 6 men given home internet access to FearFighter said they would have problems travelling to the clinic because of their phobia. Six patients had agoraphobia with panic, 3 had social phobia, and 1 had both insect phobia and claustrophobia; 5 patients also had a comorbid condition - 3 depression, 2 generalised anxiety disorder. Mean age was 37 years, and mean problem severity was 6.0 (FQ global phobia 0-8 scale), indicating marked severity. Five patients were employed full-time, 5 used computers quite often, 3 occasionally and 2 hardly at all. All 10 patients completed end-of-treatment ratings.
Of the 8 women and 9 men guided by the stand-alone version of FearFighter in the west London clinic, 7 had a specific phobia, 5 had agoraphobia with panic, 4 had social phobia, 1 had panic with generalised anxiety; 7 patients also had a comorbid condition - 2 depression, 2 social phobia, 2 generalised anxiety disorder and 1 obsessive-compulsive disorder. Mean age was 36 years, and mean problem severity was 5.4 (0-8 scale), indicating moderate to marked severity. Thirteen patients were employed full-time, 5 used computers quite often, 7 occasionally and 5 hardly at all or never.
Use of computer system, outcome and satisfaction
Of 11 candidates offered the internet therapy one declined because of lack of computer experience. The 10 internet FearFighter users said they used it a mean of 16 times (s.d.=11) in all, over 66 days (s.d.=25). Internet users had slightly more therapist support time than stand-alone computer users - 113 min (s.d.=28.1) v. 99 min (s.d.=11.4) - for extra treatment advice and for technical support, although this difference was not significant (t=-1.42, P=0.16). Users of the stand-alone system spent a mean total of 237 min (s.d.=57) at the clinic.
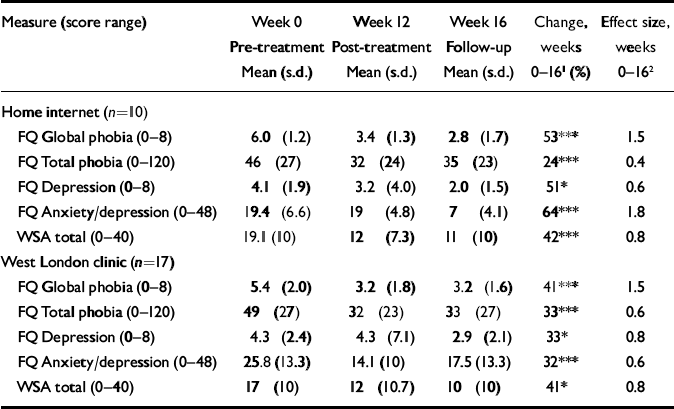
All 10 internet FearFighter users gave outcome ratings at week 12. Paired two-tailed t-tests were used for outcome analyses with significance set at P<0.05. The internet FearFighter users improved significantly to the end of treatment and to 1-month follow-up (Table 1). Their gains were also clinically significant as judged by effect size on the global phobia and anxiety/depression sub-scales of the FQ, and on the Work and Social Adjustment scale. Their improvement resembled that of stand-alone FearFighter users who had brief face-to-face therapist support in the west London clinic (Table 1, Reference Marks, Mataix-Cols and KenwrightMarks et al, 2003), and of stand-alone users in a randomised controlled trial at a clinic in south-east London (Reference Marks, Kenwright and McDonoughMarks et al, 2004).
Table 1 Computer-aided exposure therapy: comparison of outcomes of home internet treatment with stand-alone therapy
| Measure (score range) | Week 0 | Week 12 | Week 16 | Change, | Effect size, |
|---|---|---|---|---|---|
| Pre-treatment | Post-treatment | Follow-up | weeks | weeks | |
| Mean (s.d.) | Mean (s.d.) | Mean (s.d.) | 0—161 (%) | 0—162 | |
| Home internet (n=10) | |||||
| FQ Global phobia (0—8) | 6.0 (1.2) | 3.4 (1.3) | 2.8 (1.7) | 53*** | 1.5 |
| FQ Total phobia (0—120) | 46 (27) | 32 (24) | 35 (23) | 24*** | 0.4 |
| FQ Depression (0—8) | 4.1 (1.9) | 3.2 (4.0) | 2.0 (1.5) | 51* | 0.6 |
| FQ Anxiety/depression (0—48) | 19.4 (6.6) | 19 (4.8) | 7 (4.1) | 64*** | 1.8 |
| WSA total (0—40) | 19.1 (10) | 12 (7.3) | 11 (10) | 42*** | 0.8 |
| West London clinic (n=17) | |||||
| FQ Global phobia (0—8) | 5.4 (2.0) | 3.2 (1.8) | 3.2 (1.6) | 41*** | 1.5 |
| FQ Total phobia (0—120) | 49 (27) | 32 (23) | 33 (27) | 33*** | 0.6 |
| FQ Depression (0—8) | 4.3 (2.4) | 4.3 (7.1) | 2.9 (2.1) | 33* | 0.8 |
| FQ Anxiety/depression (0—48) | 25.8 (13.3) | 14.1 (10) | 17.5 (13.3) | 32*** | 0.6 |
| WSA total (0—40) | 17 (10) | 12 (10.7) | 10 (10) | 41* | 0.8 |
The internet users were generally satisfied and felt comfortable using the system (further information available from the authors upon request). However, three said they would have preferred face-to-face-guided self-help to internet-guided self-help.
DISCUSSION
In this preliminary study, ten people with phobia or panic disorder who treated themselves with computer-aided exposure therapy at home via the internet, improved by the end of treatment and at 1-month follow-up. Their improvement resembled that of patients who completed computer-aided exposure therapy in a clinic. Most of the internet group had primary agoraphobia or social phobia which prevented them attending the clinic, and only one patient used it for a specific phobia. In contrast, 7 users of the stand-alone version (40%) had a primary specific phobia, which did not restrict travel to the clinic.
This pilot study has obvious limitations. It had few patients and no masked assessor. It was uncontrolled, with assignment to groups depending not on randomisation but on patient choice and home internet access.
Computer-aided self-exposure guidance using the internet at home, with brief advice from a clinician on a live helpline, may help some people with phobia or panic disorders to overcome barriers to treatment such as the scarcity of qualified therapists and having to travel to see the therapist in person. A randomised controlled trial of the home internet FearFighter system is nearing completion.
Acknowledgements
The west London clinic was funded by the Hillingdon Primary Care Trust and. a grant from London Region Research and Development, and was co-directed by. Professor Steven Hirsch. We thank Lina Gega and David Mataix-Cols for their. work as part of the clinic team.






eLetters
No eLetters have been published for this article.