Traumatic events and the way in which people subsequently cope with them have a crucial role in the development of post-traumatic stress disorder (PTSD) and also in the development of major depression. Reported studies tend to follow one of two separate lines of research: some studies report exclusively on the aetiology of major depression with regard to childhood trauma (e.g. Reference Kendler, Gardner and PrescottKendler et al, 2002), whereas studies in general populations focus on the development of PTSD (Reference Kessler, Sonnega and BrometKessler et al, 1995; Reference Breslau, Kessler and ChilcoatBreslau et al, 1998; Reference Perkonigg, Kessler and StorzPerkonigg et al, 2000). Guided by a developmental psychopathological perspective (Reference Maercker, Maercker, Schutzwohl and SolomonMaercker, 1999), we assume that development of PTSD requires a certain maturation of memory organisation and arousal modulation which is not achieved before adolescence (Reference Pynoos, Steinberg and PiacentiniPynoos et al, 1999). The very nature of intrusions requires the recording, processing and analysing of sensory information with kinaesthetic and somatic registration, which depends on frontocortical dominance. This developmental perspective suggests that there are age-differential vulnerabilities for trauma-related disorders. There are indications that the age at which a person experiences a traumatic event is an important predictor for the severity or prevalence of PTSD. Green et al (Reference Green, Korol and Grace1991) found fewer PTSD symptoms after a disaster in the youngest age group compared with an adolescent group. Maercker (Reference Maercker, Maercker, Schutzwohl and Solomon1999) found higher PTSD prevalence rates in traumatised adolescents than in young adults, in a study of former victims of political violence. Our study on a population-based sample of young women investigates whether childhood traumas are related in particular to major depression and whether traumas in adolescence and early adulthood are primarily related to PTSD. Furthermore, we investigated whether trauma and PTSD prevalence rates in our sample correspond with those found in other representative studies (Reference Kessler, Sonnega and BrometKessler et al, 1995; Reference Breslau, Kessler and ChilcoatBreslau et al, 1998; Reference Perkonigg, Kessler and StorzPerkonigg et al, 2000). Finally, the comorbidity rate for PTSD and major depressive disorder was estimated.
METHOD
Sample
The data used in this report derive from a large epidemiological study of mental disorders of young women in the city of Dresden in Germany. The sample has been described in detail by Becker et al (Reference Becker, Margraf and Turke2001) and Hoyer et al (Reference Hoyer, Becker and Neumer2002). The representative sampling by age and city area was done with the support of the city government registry of residents. The age criterion for participants was 18–24 years. Initially, 5204 women were identified and deemed eligible for the study, of whom 2064 (39.7%) agreed to take part. After a complete description of the study to the participants, written informed consent was obtained.
For the purposes of the current analysis, the sample was further restricted. Participants who failed to supply data concerning the time of the trauma (n=67) or who had an episode of depression before experiencing a trauma (n=31) were withdrawn from the analysis. The final sample for our analysis therefore consisted of 1966 women, and the mean age was 21.8 years (s.d.=1.80).
The majority of the women in the final sample had a stable intimate partner (62.1%); 4.2% were married and 0.5% were separated or divorced. About half (51.8%) were living with their parents at the time of the study, about a third with a partner or spouse (26.2%) and 6.8% with spouse or partner and children. With regard to educational level, 93.2% had completed school education, with 6.7% having had the lowest level of school education (Hauptschule), about a third (30.1%) having had the medium level of schooling (Realschule or Polytechnische Oberschule) and about half (55.5%) having left school with the qualification that allows German students to attend university (Abitur).
Assessment
The data on traumatic events, symptoms and disorder onsets were gathered retrospectively. Diagnostic assessment was done using the Diagnostisches Interview bei psychischen Störungen – Forschungsversion (F–DIPS; Reference Margraf, Schneider and SoederMargraf et al, 1996), a structured interview for diagnosing DSM–IV disorders (American Psychiatric Association, 1994). The F–DIPS is a modified version of the Anxiety Disorder Interview Schedule for DSM–IV – Lifetime version (ADIS–IV–L; Reference Di Nardo, Brown and BarlowDiNardo et al, 1994), which is widely used for the assessment of anxiety disorders and shows excellent psychometric properties (Reference Brown, Di Nardo and LehmanBrown et al, 2001). The modification consisted of the addition of comprehensive diagnostic modules for affective and childhood disorders according to DSM–IV criteria.
Interviewers were either psychology students in their last year of training in clinical psychology, psychologists or medical doctors. All underwent extensive training totalling approximately 40 h and received biweekly supervision. For control and supervisory purposes, all interviews were audiotaped and randomly selected tapes were assessed by supervisors. Interviews took place either in the participant's home or in the university department of psychology. There was no financial reimbursement for participants in the study.
Traumatic events
The DSM–IV A1 criterion of trauma was assessed with an open question: ‘Have you ever experienced a traumatic or life-threatening event? (Examples of such events are physical assaults, severe injuries, rape, killing, combat actions, accidents, natural disasters and man-made catastrophes.)’ Participants were then asked whether they had witnessed such an event happening to others. Any number of traumatic events could be noted, and the respondent's age at the time the event occurred was recorded for each example. The following question was asked specifically for childhood trauma: ‘Can you remember events of this kind that took place in your childhood?’ Again, an unlimited number of events were noted, together with the dates of their occurrence. The next question addressed ‘personal experience of intense fear, helplessness, or horror’ (the DSM–IV A2 criterion of trauma), and in the concluding question participants were asked to identify one event that was most upsetting – the worst trauma of their lives.
Assessment of PTSD and major depression
The F–DIPS structured interview evaluated all DSM–IV criteria for PTSD and major depressive disorder in the order listed in the DSM. For appropriate PTSD symptoms (e.g. loss of interest, sense of restricted future, irritability), questions were followed by the prompt, ‘Did this occur only in the aftermath of the event?’ The F criterion (clinically significant distress) was assessed by asking, ‘Did the disturbances cause any significant distress or handicap in your professional life or other areas like family life or leisure?’ All symptoms or criteria were rated on a nine-point scale from 0 (not present) to 8 (extreme). Only symptom endorsement values of 4–8 were counted as symptom presence.
Major depression was assessed according to the DSM–IV algorithm asking introductory questions and questions regarding current and past episodes. In the introductory section, the main question was: ‘Has there ever been a phase lasting a minimum of 2 weeks in which you felt depressed, sad, or hopeless or in which you lost interest or pleasure in all your usual activities?’ This was followed by the childhood-specific question: ‘Was there a phase of 2 weeks in your life before age 18 where you were in a very irritable mood?’ Participants were subsequently asked to indicate how long such phases lasted. Current and past episodes were assessed by asking single symptom questions relating to the current and the most distressing past episode. Finally, patients were asked to disclose any excluding symptom criteria according to DSM–IV (e.g. drug misuse, medication, physiological conditions).
Psychosocial functioning
Psychosocial functioning was assessed by the clinicians’ rating of DSM Axis V (Global Assessment of Functioning, GAF; Reference Endicott, Spitzer and FleissEndicott et al, 1976) separately for current and past years of general assessment of functioning (GAF scale rating range 1–100).
Data analysis
Trauma categories
The idiosyncratic terms for traumatic events given by the participants were noted by the assessors. In a subsequent step they were grouped into nine categories of traumatic events, according to previously published trauma category lists (Reference Breslau, Davis and AndreskiBreslau et al, 1991; Reference Kessler, Sonnega and BrometKessler et al, 1995). Raters were given descriptions of the categories as follows:
-
(a) ‘serious accident’ included motor vehicle, other traffic, home, occupational, or leisure accidents;
-
(b) ‘physical attack’ included attempts or acts of intentional physical violence, e.g. severe beating, physical family violence, violent robbery assaults, hate crimes;
-
(c) ‘molestation’ included all sexual assaults without accomplished intercourse, e.g. molested by family members, friends, or strangers, or having been inappropriately ‘touched’ or having witnessed ejaculation;
-
(d) ‘rape’ comprised sexual assaults or abuse (whether as single, multiple or long-lasting events);
-
(e) ‘sudden death/death threat to associate’ included reports of losses or feared losses of loved ones (parents, siblings, close friends, close family members) e.g. through fatal accident, crime or disease;
-
(f) ‘serious illness’ comprised own life-threatening disorders;
-
(g) ‘disaster/fire’ included explosions, large-scale catastrophes and fires;
-
(h) ‘witnessing trauma’ included having witnessed major violent or life-threatening acts (whether or not family members were involved);
-
(i) the category ‘don't want to talk about it’ applies when participants refused to answer.
Three clinically experienced members of the research group categorised a total of 761 idiosyncratic terms into the above categories. There was agreement across all categories and raters of 77.5%, and dyadic kappa coefficients ranged from 0.88 to 0.94. The category showing least agreement was ‘witnessing trauma’ (average agreement 55.6%) and the category with the highest agreement was ‘rape’ (96.8%). In the case of non-agreement, the idiosyncratic term was assigned to the category endorsed by two of the three raters. In cases of total disagreement (22 of 761 trauma terms), all three raters discussed it until a consensus was reached.
Post hoc group divisions
The sample was divided into subgroups according to the age at which an individual's worst trauma took place or began. Following conventional distinctions of childhood and adolescence derived from developmental psychology (Reference BornsteinBornstein, 1999) and previous research (Reference Mullen, Martin and AndersonMullen et al, 1993), we assigned participants who experienced a traumatic event at age 12 years or younger to the childhood trauma group, whereas a traumatic event occurring after age 13 years qualified the participant for the adolescent trauma group. Finally, we divided the sample according to DSM–IV diagnosis, ending up with a pure PTSD group, a pure major depression group and a comorbid (mixed) PTSD and major depression group.
Statistical analyses
Data were analysed using the Statistical Package for Social Sciences, version 10.x for PC. Statistical tests included analyses of variance, χ2 tests and relative risk estimates.
RESULTS
Exposure to traumatic events
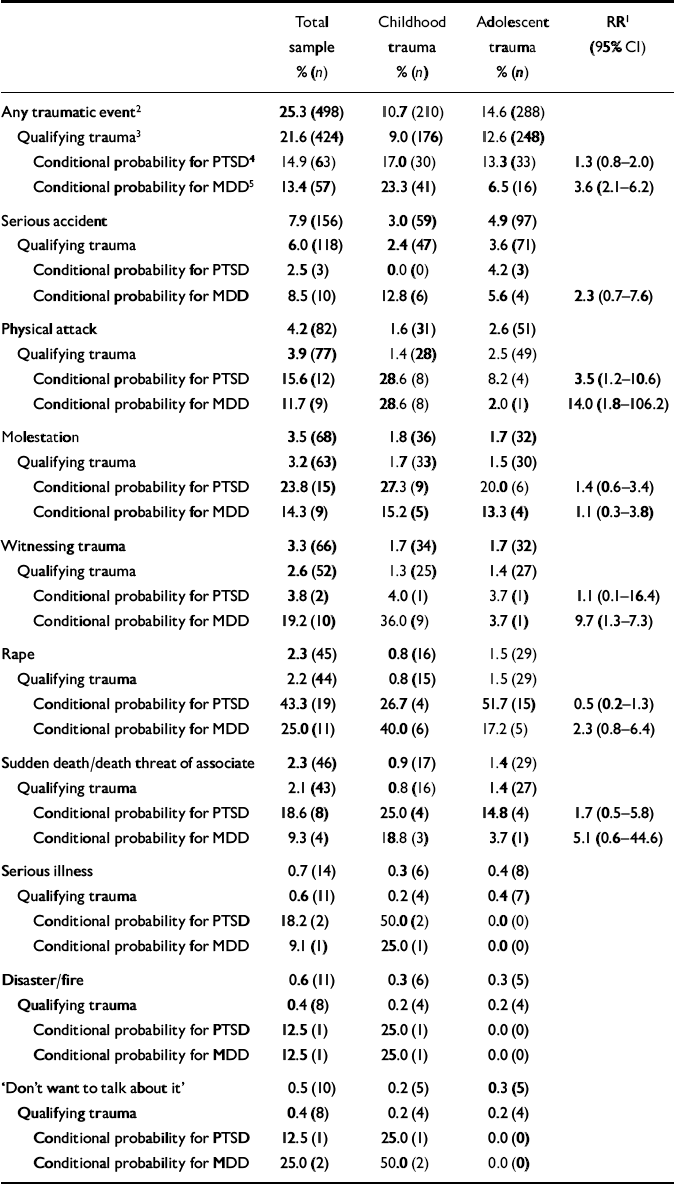
A quarter of the total group reported having experienced at least one A1 event at some time in their life (Table 1), and a fifth fulfilled both the A1 and the A2 criteria for DSM–IV PTSD by reporting events that caused horror or helplessness (qualifying trauma). ‘Serious accident’ was the most common trauma category, with 7.9% and 6.0% prevalences of A1 criterion and A1+A2 criteria respectively, followed by physical attack (4.2% for A1 and 3.9% for A1+A2). The trauma category with the highest number of A2 criteria reports was ‘rape’ (97.8% participants with A1 also endorsed A2), and the category with the lowest concordance was ‘disaster/fire’ (72.7%). Table 1 lists the prevalences of traumatic events in descending order.
Table 1 Prevalence rates of traumatic events, conditional probabilities and relative risks for post-traumatic stress disorder and major depressive disorder when trauma occurred in childhood or adolescence
| Total sample % (n) | Childhood trauma % (n) | Adolescent trauma % (n) | RR1 (95% CI) | |
|---|---|---|---|---|
| Any traumatic event2 | 25.3 (498) | 10.7 (210) | 14.6 (288) | |
| Qualifying trauma3 | 21.6 (424) | 9.0 (176) | 12.6 (248) | |
| Conditional probability for PTSD4 | 14.9 (63) | 17.0 (30) | 13.3 (33) | 1.3 (0.8–2.0) |
| Conditional probability for MDD5 | 13.4 (57) | 23.3 (41) | 6.5 (16) | 3.6 (2.1–6.2) |
| Serious accident | 7.9 (156) | 3.0 (59) | 4.9 (97) | |
| Qualifying trauma | 6.0 (118) | 2.4 (47) | 3.6 (71) | |
| Conditional probability for PTSD | 2.5 (3) | 0.0 (0) | 4.2 (3) | |
| Conditional probability for MDD | 8.5 (10) | 12.8 (6) | 5.6 (4) | 2.3 (0.7–7.6) |
| Physical attack | 4.2 (82) | 1.6 (31) | 2.6 (51) | |
| Qualifying trauma | 3.9 (77) | 1.4 (28) | 2.5 (49) | |
| Conditional probability for PTSD | 15.6 (12) | 28.6 (8) | 8.2 (4) | 3.5 (1.2–10.6) |
| Conditional probability for MDD | 11.7 (9) | 28.6 (8) | 2.0 (1) | 14.0 (1.8–106.2) |
| Molestation | 3.5 (68) | 1.8 (36) | 1.7 (32) | |
| Qualifying trauma | 3.2 (63) | 1.7 (33) | 1.5 (30) | |
| Conditional probability for PTSD | 23.8 (15) | 27.3 (9) | 20.0 (6) | 1.4 (0.6–3.4) |
| Conditional probability for MDD | 14.3 (9) | 15.2 (5) | 13.3 (4) | 1.1 (0.3–3.8) |
| Witnessing trauma | 3.3 (66) | 1.7 (34) | 1.7 (32) | |
| Qualifying trauma | 2.6 (52) | 1.3 (25) | 1.4 (27) | |
| Conditional probability for PTSD | 3.8 (2) | 4.0 (1) | 3.7 (1) | 1.1 (0.1–16.4) |
| Conditional probability for MDD | 19.2 (10) | 36.0 (9) | 3.7 (1) | 9.7 (1.3–7.3) |
| Rape | 2.3 (45) | 0.8 (16) | 1.5 (29) | |
| Qualifying trauma | 2.2 (44) | 0.8 (15) | 1.5 (29) | |
| Conditional probability for PTSD | 43.3 (19) | 26.7 (4) | 51.7 (15) | 0.5 (0.2–1.3) |
| Conditional probability for MDD | 25.0 (11) | 40.0 (6) | 17.2 (5) | 2.3 (0.8–6.4) |
| Sudden death/death threat of associate | 2.3 (46) | 0.9 (17) | 1.4 (29) | |
| Qualifying trauma | 2.1 (43) | 0.8 (16) | 1.4 (27) | |
| Conditional probability for PTSD | 18.6 (8) | 25.0 (4) | 14.8 (4) | 1.7 (0.5–5.8) |
| Conditional probability for MDD | 9.3 (4) | 18.8 (3) | 3.7 (1) | 5.1 (0.6–44.6) |
| Serious illness | 0.7 (14) | 0.3 (6) | 0.4 (8) | |
| Qualifying trauma | 0.6 (11) | 0.2 (4) | 0.4 (7) | |
| Conditional probability for PTSD | 18.2 (2) | 50.0 (2) | 0.0 (0) | |
| Conditional probability for MDD | 9.1 (1) | 25.0 (1) | 0.0 (0) | |
| Disaster/fire | 0.6 (11) | 0.3 (6) | 0.3 (5) | |
| Qualifying trauma | 0.4 (8) | 0.2 (4) | 0.2 (4) | |
| Conditional probability for PTSD | 12.5 (1) | 25.0 (1) | 0.0 (0) | |
| Conditional probability for MDD | 12.5 (1) | 25.0 (1) | 0.0 (0) | |
| ‘Don't want to talk about it’ | 0.5 (10) | 0.2 (5) | 0.3 (5) | |
| Qualifying trauma | 0.4 (8) | 0.2 (4) | 0.2 (4) | |
| Conditional probability for PTSD | 12.5 (1) | 25.0 (1) | 0.0 (0) | |
| Conditional probability for MDD | 25.0 (2) | 50.0 (2) | 0.0 (0) |
Conditional risks of PTSD and major depressive disorder
Table 1 also shows the conditional risks of PTSD and major depressive disorder for the total sample. ‘Rape’ and ‘serious accident’ had the highest and lowest probability of PTSD respectively, with ‘rape’ having a PTSD probability of 43.3% and ‘serious accident’ having a PTSD probability of 2.5%. The categories ‘rape’ and ‘Don't want to talk about it’ had the highest probability of major depressive disorder (both 25.0%), followed by ‘molestation’, which had a PTSD probability of 23.8%. ‘Serious accident’ had the lowest probability of major depressive disorder (8.5%).
In a comparison of the PTSD and major depressive disorder conditional probabilities, the only trauma category with a significant probability difference was ‘witnessing trauma’ (χ2(1)=5.33, P<0.05) with a probability of 3.8% for PTSD and 19.2% for major depressive disorder. Accordingly, for the comprehensive category ‘any traumatic event’, there was no significant difference between conditional probability for PTSD (14.9%) and conditional probability for major depressive disorder (13.4%; χ2(1)=0.30, P=0.58).
Overall, the PTSD prevalence rate of the total sample was 3.2%. The prevalence for trauma-related major depression in the total sample was 3.0%; however, if trauma is not taken into consideration, the overall (non-trauma-related) prevalence of major depression in the total sample was 10.3% (n=203).
Age specific risks of PTSD and major depressive disorder
Table 1 also includes comparisons of the two age groups. In accordance with our prediction, the probabilities for A1 criterion of any traumatic event differed between the age groups (χ2(1)=12.22, P<0.001), with more cases in the adolescent group than in the child group (288 v. 210). The conditional probability of PTSD for any traumatic event did not differ between the age groups (17.0% v. 13.3%; χ2(1)=0.14, P=0.71), with a non-significant relative risk of 1.3. For major depressive disorder, both the estimated relative risk (3.6; 95% CI 2.09–6.22) and the conditional probability (23.3% v. 6.5%; χ2(1)=12.07, P=0.001) indicated a higher risk of developing major depression when trauma occurred in childhood. The trauma category ‘witnessing trauma’ had a relative risk of 9.7 for subsequent major depressive disorder, with 36.0% conditional risk for the younger group and 3.7% for the older group (χ2(1)=6.40, P=0.01). For physical attack the relative risk was 14.0, with significant differences in conditional probabilities for the different age groups (childhood trauma 28.6% v. adolescent trauma 2.0%; χ2(1)=5.44, P=0.02).
The sample was then divided into three groups: PTSD only (‘pure PTSD’), trauma-related major depressive disorder only (‘pure major depressive disorder’) and a mixed PTSD/trauma-related major depressive disorder group. Table 2 shows the odds ratios of these groups for the two age groups. In accordance with our prediction, the odds ratio for pure major depressive disorder is increased in the childhood trauma group and decreased in the adolescent trauma group. There was no difference in odds ratios between the age groups for pure PTSD.
Table 2 Age-related risk for disorders, mean age at trauma and general assessment of functioning in three diagnostic groups

| Diagnostic group | |||
|---|---|---|---|
| PTSD (n=45) | PTSD/MDD (n=18) | MDD (n=43) | |
| Risk of disorders: [OR (95% CI)] | |||
| Trauma ≤ 12 years | 0.91 (0.48-1.69) | 2.85 (1.05-7.71) | 5.18 (2.49-10.78) |
| Trauma ≥ 13 years | 1.10 (0.59-2.06) | 0.35 (0.13-0.95) | 0.19 (0.09-0.40) |
| Age at trauma, years: mean (s.d.) | 13.8* (4.41) | 9.9 (5.31) | 9.8† (4.48) |
| GAF score: mean (s.d.)1 | |||
| Past year1 | 76.5* (13.48) | 66.7 (12.72) | 73.4 (11.65) |
| Current1 | 79.5* (12.56) | 68.4 (14.12) | 79.9* (9.55) |
The age-dependence hypothesis is further corroborated by the difference between the diagnostic groups of pure PTSD and pure major depressive disorder with regard to the mean age at trauma, with an age for the PTSD group of 13.8 years compared with 9.8 years for the major depressive disorder group and 9.9 years for the mixed group (F (2,103)=8.36, P<0.001).
Finally, analyses of psychosocial functioning (GAF rating) during the current and previous year revealed significant differences between the three groups (Table 2). For current GAF, analysis of variance indicated significant group differences (F (2,100)=6.83, P=0.002). In post hoc analyses, the comorbid group showed the lowest level compared with the PTSD or major depressive disorder groups, whereas the GAF ratings of the pure PTSD and pure major depressive disorder groups did not differ.
DISCUSSION
Age-differential pathways
The main goal of this study was to investigate age-differential conditional probabilities of developing either major depression or PTSD after traumatisation. We were able to show that experiencing a traumatic event in childhood (up to age 12 years) is related to higher rates of major depression than is experiencing a traumatic event in adolescence (after age 13 years). This age-related difference could not be found for PTSD. In other words, there is a higher probability of developing major depressive disorder if a trauma is suffered during childhood than if the trauma occurs in adolescence. The finding of childhood trauma being related to affective disorder is in line with results from neurobiology (Reference Heim and NemeroffHeim & Nemeroff, 2001) and developmental psychopathology (Reference Pynoos, Steinberg and PiacentiniPynoos et al, 1999). Developmental psychological studies of the generation of intense negative emotions indicate ways in which childhood traumatic experiences might challenge maturing mechanisms of emotional or mood regulation. Thus, the findings indicate that traumatic experiences in children are processed differently from those in adults, resulting in a slightly different phenotype and sequelae of childhood PTSD (Reference Pynoos, Steinberg and PiacentiniPynoos et al, 1999). Heim & Nemeroff (Reference Heim and Nemeroff2001) found that severe stress early in life is related to greater sensisitivity of the hypothalamic–pituitary–adrenal axis to stress in adulthood, which underlies greater vulnerability to major depression. Furthermore, epidemiological research has confirmed the aetiological role of childhood trauma in later psychopathological disorder: Kendler et al (Reference Kendler, Gardner and Prescott2002) showed childhood sexual abuse to be a major aetiological pathway within a multifactorial model.
A complementary explanation of our results could refer to the fact that the length of time elapsing between the reported trauma and the assessment of psychopathological state can also affect the degree of depression. The natural history of response to trauma seems to indicate that the response begins with anxiety symptoms and then – possibly mediated by functional impairment and resulting vulnerabilities – evolves towards depression (Reference Wittchen, Kessler and PfisterWittchen et al, 2000). However, we consider this explanation to be of limited value, as it does not explain why the group of respondents traumatised in childhood separate into a pure major depressive disorder group and a comorbid PTSD and major depressive disorder group.
Prevalences of trauma and PTSD
The rates of exposure to traumatic events and prevalences for PTSD can be seen as meaningful with regard to previous studies (Reference Kessler, Sonnega and BrometKessler et al, 1995; Reference Breslau, Kessler and ChilcoatBreslau et al, 1998; Reference Perkonigg, Kessler and StorzPerkonigg et al, 2000). Our population-based sample of young women (aged 18–24 years) showed a trauma prevalence (DSM A1 criterion) of 25.3% and a PTSD prevalence rate of 3.4%. Another study in Germany (Reference Perkonigg, Kessler and StorzPerkonigg et al, 2000) with a sample aged 14–24 years found a somewhat lower trauma prevalence (DSM A1 criterion) of 17.7% and a PTSD prevalence rate of 2.2% for female participants.
In the USA the National Comorbidity Survey, using the somewhat more liberal DSM–III–R algorithm, reported a trauma prevalence of 51.2% and a PTSD prevalence of 10.3% for women aged 15–24 years (Reference Kessler, Sonnega and BrometKessler et al, 1995). Breslau et al (Reference Breslau, Davis and Andreski1991) reported similarly high prevalence rates for PTSD in a sample of mainly middle-aged women in Detroit: trauma prevalence was 40% and PTSD prevalence was 13.8%. Only the study by Cuffe et al (Reference Cuffe, Addy and Garrison1998) on older adolescents in the USA reported lower prevalence rates, comparable with the range of findings from studies in Germany. The greater differences of the National Comorbidity Survey and Detroit area studies may reflect substantial changes in the definition of PTSD from DSM–III–R to DSM–IV, as well as true differences between study populations, such as considerably lower event rates of natural disasters, threat with weapons, and witnessing such events, in the different geographical regions of the studies. Interestingly, our study showed similar conditional risks of developing PTSD for the particular trauma event categories to those reported by Kessler et al (Reference Kessler, Sonnega and Bromet1995), Breslau et al (Reference Breslau, Davis and Andreski1991) and Perkonigg et al (Reference Perkonigg, Kessler and Storz2000): for example, for rape the risks were 55%, 49% and 52%, respectively, compared with 52% in the adolescent group in the present study.
Major depression and comorbidity with PTSD
For trauma-related major depression there are fewer published studies available. In the study by Mullen et al (Reference Mullen, Martin and Anderson1993) on childhood sexual abuse before age 13 years, only 13% of participants reported a major depressive disorder; our study shows a prevalence of major depressive disorder of 40% after rape and 15% after molestation. It could be speculated that these differences are due to diagnostic algorithms and definitions of events. In addition, the data of Mullen et al (Reference Mullen, Martin and Anderson1993) suggest that greater severity, frequency and duration of abuse result in an increased likelihood of subsequently developing depression. This might lead to the conclusion that our definition of rape or molestation as trauma may be significantly different from theirs.
In our sample, we found relatively low comorbidity rates of PTSD and major depression: 29% of the women with PTSD also had major depressive disorder, and 32% of the women with major depressive disorder also had PTSD. This indicates lower comorbidity rates than in other studies (Reference Bleich, Koslowsky and DolveBleich et al, 1997; Reference Goenjian, Steinberg and NajarianGoenjian et al, 2000). In our sample, comorbidity rates may not be as marked because of the young age of the participants. Wittchen et al (Reference Wittchen, Kessler and Pfister2000) provided evidence that comorbid disorders are developed and maintained particularly in extended, untreated, chronic courses, typical of middle-adulthood samples (Reference Deering, Glover and ReadyDeering et al, 1996). Our finding of the lowest levels of psychosocial functioning in the comorbid group may point to the fact that young women suffering from more than one trauma-related disorder may struggle with a larger range of mental health problems and their distal stress consequences (Reference Pynoos, Steinberg and PiacentiniPynoos et al, 1999).
Limitations
There are various limitations to the present study. First, the sample consisted entirely of women, and it has been shown that the aftermath of trauma differs substantially between the genders (e.g. Reference Springer and PadgettSpringer & Padgett, 2000). Second, the response rate of the study was less than 40%. The main reason for this low response rate is probably rooted in the macrocontext of the study, which was conducted in Dresden, in the eastern part of Germany. Because of economic and other problems relating to the transformation of the political system following the demise of communism, many of those living in this part of the country are unwilling to participate in psychiatric studies (Reference Maercker and HerrleMaercker & Herrle, 2003). Specific reasons for non-participation include the scarcity of telephones at the time of the assessment (mid-1990s), high levels of economic migration to other parts of Germany, and a general reluctance to allow personal data to be reported – the legacy of years of surveillance by the East German secret security police. A third limitation was that we assessed trauma retrospectively from adults; numerous studies have suggested that such data are subject to recall bias (Reference Maughan and RutterMaughan & Rutter, 1997). If the errors introduced in our assessment were random, this would attenuate the true associations. However, biases that would exaggerate the true associations are also possible. Fourth, the methodology differed somewhat from previous epidemiological studies on trauma consequences. Although we used DSM–IV criteria, we used the more uncommon structured interview version, originally developed for the assessment of anxiety disorders (ADIS–IV–L). Trauma categories were first assessed by using the participants’ idiosyncratic terms and later classified into categories. There is no information available concerning the reliability of this method for assessing personal trauma in an epidemiological study, although the trauma prevalence rates in our study were comparable in range to those previously published. Fifth, although our study had the advantage of applying an age limit between childhood and adolescence based on developmental psychological literature, the inflexible application of this limit remains largely conventional. In developmental psychology age is regarded as a carrier variable for various psychodevelopmental processes. Further research should look for more appropriate markers (e.g. maturation of emotional or physiological regulation) in childhood and adolescent development to explain differential effects. Furthermore, since PTSD symptoms decrease over time and depression normally increases in this age group, the study may overemphasise depression as an outcome of traumatic stress in the younger age group. Finally, psychopathological outcomes other than PTSD and major depressive disorder were not investigated. Other important sequelae of childhood traumatisation (e.g. alcohol and drug misuse, anxiety disorders, borderline personality disorder) would be worth following up in a similar age-stratified study design.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ People with a history of childhood or adolescent trauma may develop not only post-traumatic stress disorder (PTSD) but also major depression, either alone or in combination with PTSD.
-
▪ In patients with persistent major depression, clinicians should also enquire about traumatic experiences in childhood in order to obtain a comprehensive record of possible aetiological factors.
-
▪ The probability of developing PTSD after exposure to a traumatic event varies with other epidemiological findings, from about 4% after serious accidents to about 50% after rape experienced in adolescence.
LIMITATIONS
-
▪ The sample was entirely female, and it has been previously shown that the psychiatric sequelae of trauma differ between the genders.
-
▪ The retrospective nature of the trauma report may affect the reliability of the study.
-
▪ The low response rate of less than 40% limits the generalisability of results.
Acknowledgements
The study was carried out in Dresden, Germany, supported by grant DLR. 01EG9410 from the Federal Ministry of Education and Science. The authors. acknowledge the support in conducting the study provided by Simon Neumer, PhD, and Ulrich Soeder, MSc.







eLetters
No eLetters have been published for this article.