During the past decade acute and maintenance treatment of depression has switched towards the use of newer anti-depressant drugs such as the selective serotonin reuptake inhibitors (SSRIs), serotonin–noradrenaline reuptake inhibitors (SNRIs) and selective noradrenaline reuptake inhibitors (selective NARIs). It is claimed that compliance with these drugs is better than compliance with tricyclic antidepressant therapy (Reference Mourilhe and StokesMourilhe & Stokes, 1998; Reference Masand and GuptaMasand & Gupta, 1999; Reference Keller, Hirschfeld and DemyttenaereKeller et al, 2002) because of the former's more favourable profile of side-effects, and that the risk of cycle acceleration may be lower (Reference Masand and GuptaMasand & Gupta, 1999). It remains to be investigated whether the longitudinal course is improved in naturalistic studies following the introduction of these drugs. We have previously found that the risk of recurrence increased with every episode in patients discharged from their first-ever admission with a diagnosis of depression or mania during a period from 1971 to 1993 in Denmark (Reference KessingKessing, 1998; Reference Kessing, Andersen and MortensenKessing et al, 1998). The SSRIs were introduced in Denmark in 1987 and the SNRIs and selective NARIs have been used since 1990. The aim of our study was to investigate the rate of relapse, expressed as the rate of readmission after successive discharges, for patients hospitalised for depression, recurrent depression, mania or bipolar affective disorder at their first-ever admission following 1993. As in prior studies, we used the Danish Psychiatric Central Register as the database and used survival analysis (including so-called ‘frailty’ methods) to take account of the individual liability to relapse.
METHOD
The register
The Danish Psychiatric Central Research Register is nationwide, with registration of all psychiatric admissions in Denmark for the country's 5.3 million inhabitants (Reference Munk-Jorgensen and MortensenMunk-Jorgensen & Mortensen, 1997). All the inhabitants of Denmark have a unique personal identification number, the Civil Person Registration number, which can be logically checked for errors, so it can be established with great certainty if a patient has been admitted previously, irrespective of changes in name. Data on death can also be established with equal certainty, as the same identification number is used across all public registration systems.
The ICD–10 (World Health Organization, 1992) has been used in Denmark since January 1994. Information on treatment intervention is not available.
The sample
The study sample was defined as all in-patients with a diagnosis of depression or recurrent depression (ICD–10 codes F32–33.9) or a diagnosis of manic episode or bipolar affective disorder (codes F30–31.6, F38.00), at first discharge ever during the period 1 January 1994 to 31 December 1999. According to the diagnostic hierarchy in ICD–10, patients who were given a main diagnosis of organic disorder (codes F00–09), schizophrenia (codes F20–20.9) or schizoaffective disorder (codes F25–25.9) at later discharges were included in the analysis until this diagnostic alteration and thereafter censored from further analysis, since from this point these patients were no longer considered to have a primary affective disorder. Patients who were given other diagnoses (lower in the hierarchy) at later discharges were still regarded as suffering from affective disorder, which is why all data from these admissions were included.
The sample was divided dynamically into two according to the type of affective disorder at a given time. Thus, patients were classified as having a depressive disorder as long as they had not been discharged with a diagnosis of manic episode or bipolar affective disorder, but once they had received such a diagnosis they were reclassified as having bipolar disorder. The type of disorder was thus time-dependent.
It is well known that a proportion of psychiatric patients are temporarily discharged to a somatic ward for the elucidation or treatment of somatic illness and then readmitted to the psychiatric ward for further treatment of their psychiatric illness. Since the scope of our investigation was to study episodic relapse, the two admission periods were added together and counted as a single episode if readmission occurred within 3 days of discharge. Relapse was thus defined as readmission after being discharged for 3 days. Time to relapse was estimated, censoring if death occurred or if relapse had not occurred before 31 December 1999. The follow-up period thus varied between 1 day and 6 years.
Statistical analysis
The Kaplan–Meier method for estimation with censored observations was used for calculating the probability of remaining well (i.e. the probability of remaining discharged after 3 days). Episodes were categorised into 1, 2, 3, 4, 5, 6, 7–8, 9–10, 11–12 and 13 or more episodes. Additionally, a frailty model was used to take account of the individual liability toward relapse. The frailty model is an extended Cox regression model (Reference Andersen, Borgan and GillAndersen et al, 1993). The time variable was time since the latest episode and the event was relapse, censoring at death and if relapse did not occur before 31 December 1999. Gender, age at first episode leading to hospitalisation, type of disorder, calendar period and the episode number were included as co-variables. Calendar period was categorised as the periods 1994–1995, 1996–1997 and 1998–1999. Age in years at first episode leading to hospitalisation was categorised as age < 30, 30–44, 45–59, 60–79 and 80 or over. Finally, the rate of relapse was adjusted for the effect of frailty, as previously described by Kessing et al (Reference Kessing, Olsen and Andersen1999). Patients with a large frailty value tend to have a high rate of relapse after any episode, whereas patients with a small frailty value have a low rate of relapse. The frailty is assumed to follow a ‘gamma’ distribution across the population of patients, and the variance of this distribution is thus a measure of the heterogeneity of the patients. Finally, it was tested whether models including prior episodes and calendar period as quantitative variables described data sufficiently well compared with when these variables were included as categorised variables as described above.
All values of P were based on likelihood ratio tests and all confidence intervals on Wald tests (except for the frailty variance, for which likelihood ratio tests were used). The statistical software used was S-PLUS (Reference Becker, Chambers and WilksBecker et al, 1988).
RESULTS
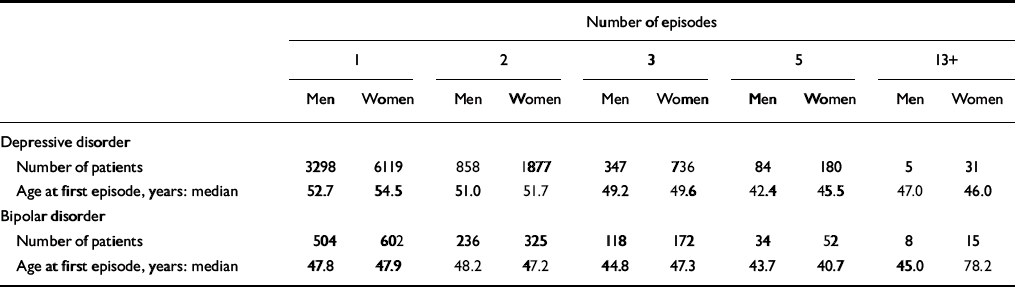
A total of 9417 patients had a diagnosis of depressive disorder and 1106 patients had a diagnosis of mania or bipolar affective disorder, at first-ever discharge during the period 1994–1999. Information on patient gender and numbers of episodes leading to hospitalisation is given in Table 1. Patients with many episodes were younger at first episode leading to hospitalisation.
Table 1 Number of patients with depressive or bipolar disorder according to number of episodes leading to hospitalisation and age at first episode
| Number of episodes | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 5 | 13+ | ||||||
| Men | Women | Men | Women | Men | Women | Men | Women | Men | Women | |
| Depressive disorder | ||||||||||
| Number of patients | 3298 | 6119 | 858 | 1877 | 347 | 736 | 84 | 180 | 5 | 31 |
| Age at first episode, years: median | 52.7 | 54.5 | 51.0 | 51.7 | 49.2 | 49.6 | 42.4 | 45.5 | 47.0 | 46.0 |
| Bipolar disorder | ||||||||||
| Number of patients | 504 | 602 | 236 | 325 | 118 | 172 | 34 | 52 | 8 | 15 |
| Age at first episode, years: median | 47.8 | 47.9 | 48.2 | 47.2 | 44.8 | 47.3 | 43.7 | 40.7 | 45.0 | 78.2 |
Figure 1 presents the rates of relapse leading to hospitalisation (after being discharged for more than 3 days) following the first, second, third, fourth and fifth discharges for men and women with depressive or bipolar affective disorders, respectively. As can be seen, the risk of relapse increased successively with the number of episodes for both genders and for both types of disorder.

Fig. 1 Rate of relapse leading to hospitalisation (after being discharged for at least 3 days) following first, second, third, fourth and fifth discharges for (a) men with depressive disorder, (b) women with depressive disorder, (c) men with bipolar affective disorder and (d) women with bipolar affective disorder.
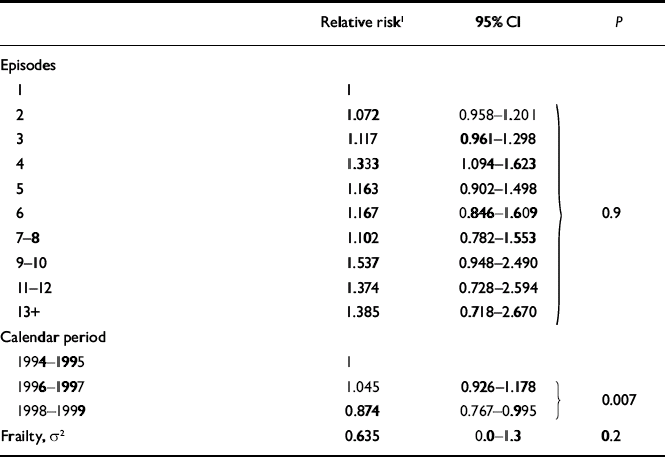
In further analyses the rate of relapse was adjusted for the effect of the individual liability toward recurrence in frailty models. Table 2 presents for men the relative risks (RR) following successive episodes adjusted for the effect of type of disorder at first discharge (depressive v. bipolar), age at onset leading to hospitalisation, calendar period and frailty. Men with a diagnosis of mania or bipolar disorder at first discharge had significantly greater rate of relapse than men with a diagnosis of depressive disorder at first discharge (RR=1.39, 95% CI 1.22–1.57) and the rate of relapse decreased with age at first episode (age < 30, RR=1; age 30–44, RR=0.840; age 45–59, RR=0.727; age 60–79, RR=0.701; age 80+, RR=0.669; d.f.=4, P < 0.0001). The rate of relapse differed significantly for patients discharged in various calendar periods (1994–1995, 1996–1997, 1998–1999) but without a systematic trend in time (Table 2). However, no interaction was found between the effect of episodes on the rate of relapse and type of disorder (χ2=0.01, d.f.=1, P=0.9), age at first episode (χ2=4.6, d.f.=4, P=0.3) or calendar period (χ2=1.4, d.f.=2, P=0.5), respectively. Consequently, a common effect of episodes is presented in Table 2 for male patients with depressive and bipolar disorders, regardless of age and calendar period. For men, the relative risk of relapse tended to increase with the number of episodes leading to hospitalisation, albeit non-significantly. The rate of relapse increased from a 7.2% greater rate for patients with two episodes v. patients with one episode, to a 38.5% greater rate for patients with 13 or more episodes.
Table 2 Men: effect of episodes in depressive and bipolar disorder
| Relative risk1 | 95% CI | P | |
|---|---|---|---|
| Episodes | |||
| 1 | 1 | ||
| 2 | 1.072 | 0.958–1.201 | 0.9 |
| 3 | 1.117 | 0.961–1.298 | |
| 4 | 1.333 | 1.094–1.623 | |
| 5 | 1.163 | 0.902–1.498 | |
| 6 | 1.167 | 0.846–1.609 | |
| 7–8 | 1.102 | 0.782–1.553 | |
| 9–10 | 1.537 | 0.948–2.490 | |
| 11–12 | 1.374 | 0.728–2.594 | |
| 13+ | 1.385 | 0.718–2.670 | |
| Calendar period | |||
| 1994–1995 | 1 | ||
| 1996–1997 | 1.045 | 0.926–1.178 | 0.007 |
| 1998–1999 | 0.874 | 0.767–0.995 | |
| Frailty, σ2 | 0.635 | 0.0–1.3 | 0.2 |
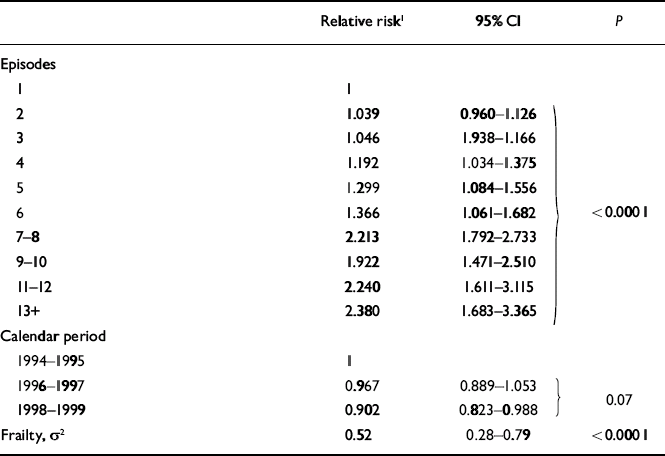
As for men, women with a diagnosis of mania or bipolar affective disorder at first discharge had greater rate of relapse than women with a diagnosis of depressive disorder at first discharge, albeit non-significantly (RR=1.10, 95% CI 0.995–1.220; P=0.063) and the rate of relapse decreased significantly with age at first episode (age < 30, RR=1; age 30–44, RR=0.887; age 45–59, RR=0.701; age 60–79, RR=0.686; age 80+, RR=0.617; d.f.=4, P < 0.0001). A trend of decreasing rates of relapse in recent calendar periods was found, but these rates did not differ significantly (Table 3). As for men, no interaction was found between the effect of episodes on the rate of relapse and type of disorder (χ2=0.16, d.f.=1, P=0.7), age at first episode (χ2=3.14, d.f.=4, P=0.07) or calendar period (χ2=2.0, d.f.=2, P=0.4). Consequently, as for men, a common effect of episodes is presented in Table 3 for female patients with depressive and bipolar disorders, regardless of age and calendar periods. The rate of relapse leading to hospitalisation differed significantly following various numbers of episodes (P < 0.0001), with an increasing rate with the number of episodes.
Table 3 Women: effect of episodes in depressive and bipolar disorder
| Relative risk1 | 95% CI | P | |
|---|---|---|---|
| Episodes | |||
| 1 | 1 | ||
| 2 | 1.039 | 0.960–1.126 | <0.0001 |
| 3 | 1.046 | 1.938–1.166 | |
| 4 | 1.192 | 1.034–1.375 | |
| 5 | 1.299 | 1.084–1.556 | |
| 6 | 1.366 | 1.061–1.682 | |
| 7–8 | 2.213 | 1.792–2.733 | |
| 9–10 | 1.922 | 1.471–2.510 | |
| 11–12 | 2.240 | 1.611–3.115 | |
| 13+ | 2.380 | 1.683–3.365 | |
| Calendar period | |||
| 1994–1995 | 1 | ||
| 1996–1997 | 0.967 | 0.889–1.053 | 0.07 |
| 1998–1999 | 0.902 | 0.823–0.988 | |
| Frailty, σ2 | 0.52 | 0.28–0.79 | <0.0001 |
Finally, models including prior episodes and calendar periods as quantitative variables confirmed the above estimations. Models including prior episodes as a quantitative variable gave an adequate description of data (men: χ2=3.5, d.f.=8, P=0.9; women: χ2=13.4, d.f.=8, P=0.1). For men, the rate of relapse leading to readmission increased 1.019 times (95% CI 0.98–1.06) and for women 1.091 times (95% CI 1.05–1.12). For men, a model including calendar period as a quantitative variable described data significantly less well than when calendar period was included as a categorical variable (χ2=4.4, d.f.=1, P=0.04), but for women calendar period included as a quantitative variable gave an adequate description (χ2=2.3, d.f.=1, P=0.1). For women, the rate of relapse leading to readmission decreased 0.979 times (95% CI 0.957–1.002) for every calendar year, but (as can be seen from the confidence intervals) this was not significant.
DISCUSSION
The study showed that despite the introduction of new antidepressants the risk of relapse leading to hospitalisation increases with every new episode for patients with depressive disorder and for patients with bipolar affective disorder. For men, this effect of episodes was not statistically significant. The rate of relapse was not reduced significantly within the investigating period. The study comprised a nationwide, naturalistic follow-up of all patients discharged with a diagnosis of depressive or bipolar affective disorder from their first psychiatric hospitalisation in the period 1994–1999. We have no information about their treatment, but a recent study found that new-generation antidepressants constituted 69.4% of the total antidepressants prescribed for patients discharged from psychiatric hospitals in Denmark with a diagnosis of affective disorder in 1998 (Reference Hansen, Soendergaard and VachHansen et al, 2004). Thus, the majority of patients with depressive disorder might have been treated with newer antidepressants during both acute and maintenance phases. Similarly, patients with bipolar affective disorder might have been treated with SSRIs for depressive episodes in accordance with recommendations in Danish national guidelines (Reference Licht, Kessing and LarsenLicht et al, 2002) and other guidance.
Methodological considerations
The study included diagnoses recorded in the Danish Psychiatric Central Research Register. It should be recalled that the diagnoses in the register originate from different clinicians all over Denmark and are not standardised for research purposes. The validity of the ICD–10 diagnoses of affective disorder has not been investigated and indeed clinicians may have heterogeneous ways of handling diagnoses.
It should be noted that the findings pertain to the proportion of patients with more severe depressive or bipolar disorders, as only patients who had passed the threshold for admission to psychiatric care were included in the study. Thus, the findings may not be generalisable to the general population or to patients who are treated by general practitioners or in private psychiatric practice without hospitalisation.
Data were analysed in a historical prospective way, as in prior studies of the course of illness of affective disorders (Reference Kessing, Andersen and MortensenKessing et al, 1998). Patients with depressive disorder may develop a bipolar disorder with time and in the analyses the type of disorder was thus time-dependent. Censoring was done if patients with affective disorders developed disorders higher in the diagnostic hierarchy (organic disorders or schizophrenia). Additionally, the risks of relapse following successive episodes were adjusted for the individual tendency toward relapse with inclusion of a frailty parameter in extended Cox's regression analyses, as in prior studies (Reference Kessing, Olsen and AndersenKessing et al, 1999).
The advantages of the study are that it comprises observation over a period of 6 years of the whole Danish population (5.3 million) and that this population is ethnically and socially homogeneous and has a very low migration rate. Psychiatric care is well developed, so that people with a moderate to severe affective disorder can easily come into contact with a psychiatric hospital. Because all psychiatric in-patient treatment in Denmark is free of charge, and as no private psychiatric in-patient facility exists, the study is not biased by socio-economic differences.
Comparisons with prior studies
Three prior studies have taken the individual liability toward recurrence into account in analyses of the rate of recurrence following successive episodes of affective disorders (Kessing et al, Reference Kessing, Olsen and Andersen1999, Reference Kessing, Hansen and Andersen2004; Reference Solomon, Keller and LeonSolomon et al, 2000). In the 10-year prospective study, initiated in the early 1980s, by the US National Institute of Mental Health (Clinical Research Branch) Collaborative Program on the Psychobiology of Depression, the risk of recurrence was found to increase with each successive episode for both in-patients and out-patients treated in five psychiatric units for major depressive disorder, taking the individual propensity toward recurrence into account (Reference Solomon, Keller and LeonSolomon et al, 2000); this increase in risk remained when data for men and women were analysed separately, although it was not significant (Reference Kessing and AndersenKessing & Andersen, 2001).
In re-analyses of data from the Zurich study by Jules Angst of patients who were admitted to psychiatric hospital between 1959 and 1963 and followed up to 1997, the rate of subsequent recurrence was found to increase with the number of episodes when adjusting for the individual liability toward recurrence in frailty models similar to those used in our study (Reference Kessing, Hansen and AndersenKessing et al, 2004). The effect of number of episodes was the same in depressive and bipolar disorders and for men and women. In our earlier register study of recurrence in affective disorder we found no (significant) effect of episodes for men with depressive disorder when adjusting for the individual liability toward recurrence (Reference Kessing, Olsen and AndersenKessing et al, 1999). In the present study, a non-significant effect of episodes was found for men with depressive as well as bipolar disorders, adjusting for individual heterogeneity. In both of these studies, the frailty parameter was larger for men than for women, reflecting greater heterogeneity in the course of illness for men. Thus for men, the findings of a successively increasing risk of relapse with the number of episodes (see Fig. 1a,c) may partly be due to the proportion of patients who already had a high risk of relapse following the first episode.
In the register study with data from the period 1971–1993, diagnoses were made in accordance with ICD–8 (Reference Kessing, Andersen and MortensenKessing et al, 1998) in contrast to the ICD–10 diagnoses used in the period 1994–1999. The diagnostic change from ICD–8 (World Health Organization, 1974) to ICD–10 hampers the possibility of analysing changes in the risk of relapse according to calendar time across the two periods. Additionally, it is difficult to compare results in detail for the two studies because outcomes were defined in different ways. In the study reported here, outcome was relapse defined as readmission following 3 days of discharge, whereas in the earlier study the outcome was recurrence defined as readmission following 8 weeks of discharge. We did not use the latter definition of outcome in this study, since following the publication of the ICD–10 and DSM–IV (American Psychiatric Association, 1994) it has become increasingly clear that it often takes more than 8 weeks to reach remission. However, keeping this in mind, for patients discharged from their first-ever admission with a diagnosis of affective disorder, the rate of relapse in this study did not differ substantially from the rate of recurrence leading to readmission in our earlier study (Reference Kessing, Andersen and MortensenKessing et al, 1998): for depressive disorder, 25% of patients discharged from first hospitalisation with depression developed a relapse leading to readmission within 0.7 years in the present study, whereas 25% developed recurrence leading to readmission within 1.7 years in the earlier study; for bipolar disorder, 50% of patients discharged from first hospitalisation with depression developed a relapse leading to readmission within 3.6 years in the present study, whereas 50% developed recurrence leading to readmission within 3.8 years in the earlier study.
Interpretation of results from the present study
This is the first study to analyse the rate of relapse following successive episodes for patients who presented with onset of depressive or bipolar disorder in the period following the introduction of newer anti-depressants. During the study period (1994–1999), newer antidepressants were increasingly used in Denmark, and the majority of patients with depressive disorders were treated with these newer drugs by 1998 (Reference Hansen, Soendergaard and VachHansen et al, 2004). However, the risk of relapse leading to hospitalisation was not reduced during the study period. No other major change affecting the treatment of patients with affective disorders took place during the investigation period. Patients with bipolar affective disorder were treated with older antipsychotics, lithium or anticonvulsants and mainly SSRIs during depressive episodes (Licht et al, Reference Licht, Kessing and Larsen2002, Reference Licht, Vestergaard and Kessing2003). Atypical antipsychotics for treatment of acute mania or as maintenance treatment for bipolar disorder were introduced in Denmark in 2000. No major organisational change has taken place in the treatment of patients with affective disorders and the number of available psychiatric in-patient beds in Denmark was stable throughout the investigating period.
As in prior studies, the risk of relapse was found to increase with the number of episodes in depressive and bipolar disorders in our study, suggesting that in clinical practice the availability of newer antidepressants did not alter the progressive deteriorating course of the illness. It is reasonable to assume that the majority of patients in the study were treated in the acute depressive phase (patients with depressive or bipolar affective disorders) or in the maintenance phase (patients with depressive disorder) with newer antidepressants, but a possible better compliance and reduced cycle acceleration related to these drugs did not improve the course of illness substantially. In accordance with our findings, a recent study from Iceland showed that the rate of out-patient visits and admission rates increased during the period 1989–2000 despite a dramatic increase in the sales of antidepressants (Reference Helgason, Tomasson and ZoegaHelgason et al, 2004).
The possibility cannot be excluded that the course of depressive or bipolar illness has ameliorated in recent times in terms of measures other than those used in our study. It might be that newer antidepressants improve the course of illness without this being reflected in a reduction in the rate of relapse leading to hospitalisation and in the effect of episodes. It is possible that newer antidepressants in naturalistic settings might reduce the number of milder depressive episodes not leading to hospitalisation, and improve psychosocial outcome. The effect of treatment on the course of illness of depressive and bipolar disorders in daily clinical life warrants further research.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Patients with recent-onset depressive or bipolar disorder will on average experience increasing risk of relapse with the number of successive episodes.
-
▪ The availability of newer antidepressant drugs does not seem to stop the progressive worsening of these illnesses.
-
▪ There is a need for research into methods of early intervention in depressive and bipolar disorders.
LIMITATIONS
-
▪ The diagnoses were not validated.
-
▪ The results relate to patients who had been admitted to a psychiatric hospital at least once.
-
▪ The results relate to readmission rather than to relapse.
Acknowledgement
The study was supported by the Lundbeck Foundation.









eLetters
No eLetters have been published for this article.