‘My mother told our neighbours that I was one of her relatives, not her daughter. I was upset in the past when she first treated me like that, but now I'm used to it’ (28-year-old Chinese woman with a history of schizophrenia).
Studies on psychiatric stigma have often focused on public attitudes. Because these collective attitudes vary in their impact on individuals, and stigma is ultimately an intersubjective experience, they provide at best an approximate guide to how stigma causes difficulties to individuals with mental illness. In contrast, understanding patients' subjective experiences of stigma attunes us to what is at stake in their lived local worlds, i.e. the everyday, non-trivial interpersonal transactions involving family members, partners, friends and colleagues (Reference Kleinman and KleinmanKleinman & Kleinman, 1997). Western studies on subjective stigma suggested that hurtful media representations, offensive comments, patronising attitudes and being shunned or rejected were common experiences for people with schizophrenia (Reference WahlWahl, 1999; Reference Schulze and AngermeyerSchulze & Angermeyer, 2003; Reference Dinos, Stevens and SerfatyDinos et al, 2004). Since Chinese society has routinely been said to privilege interpersonal bonding over individualism, it is instructive to examine the nature, magnitude and impact of Chinese patients' experience of stigma in their local worlds.
METHOD
Instrument
Four focus groups comprising 31 psychiatric out-patients in total were conducted to formulate a conceptual framework and to devise items for examining subjective stigma. In probing stigma, we asked participants about the attitudes, reactions and treatment that they perceived to be unfair or prejudicial and believed to be due to their having a psychiatric illness. Based on a thematic analysis of the transcribed responses of the focus groups, a 137-item Psychiatric Stigma Experience Questionnaire (PSEQ), in Chinese, was constructed.
The PSEQ was an exploratory tool that covered stigma in the areas of work, family, social relationships and medical treatment. Its items were grouped into several domains:
-
(a) ‘work-related stigma’ consisted of items such as ‘Did your employer fire you because of your illness?’
-
(b) ‘interpersonal stigma’ included items related to stigma from family members, friends and partners, e.g. ‘Did your family members dislike/despise you because of your illness?’
-
(c) ‘concealment and anticipated stigmatisation’ included items such as, ‘If your friends knew about your illness, they might deliberately distance you.’
-
(d) ‘emotional reactions to stigmatisation’ included items such as ‘Have you ever thought of ending your life because of the stigmatisation and unfairness resulting from your illness?’
The study reported here focused on items about stigma related to work, family and social relationships and the impact of stigma on patients' well-being.
Participants
Convenience sampling was used to recruit a total of 480 participants (age range 17-62 years, mean 40.2). They included 320 out-patients with schizophrenia (217 men, 103 women) who resided in 28 ‘halfway houses’ and 160 out-patients with diabetes mellitus (78 men, 82 women) attending a public clinic. Because of the practical difficulty of administering a protracted questionnaire at the diabetes clinic, a shortened 28-item version containing salient domains of stigma that we considered applicable to both groups of patients was used.
Procedure
Each patient gave informed consent and participated voluntarily and anonymously. Owing to a low level of literacy among some of the participants with schizophrenia, a research assistant read out the questionnaire to groups of about 20 patients in the halfway houses. Sufficient interpersonal space was provided so that they could complete the questionnaire undisturbed. Because this group approach was not feasible at the diabetes clinic, participants there completed the questionnaire on their own in a quiet room. Participants were encouraged to ask for clarification throughout the data collection process.
Analyses
Dependent variables were defined dichotomously, with ‘yes/no’ measures of whether participants had had actual stigma experience before, and ‘agree/disagree’ measures of whether participants anticipated stigmatisation if certain incidents had occurred. The independent variable consisted of two levels: patients with schizophrenia and patients with diabetes mellitus. Bivariate analyses were conducted using chi-squared statistical significance tests and t-tests in order to examine associations between schizophrenia and stigma experience. Data were analysed using the Statistical Package for the Social Sciences (SPSS) 11.0 computer package for Windows. Missing data were excluded listwise.
RESULTS
Reliability
Cronbach's alpha coefficients for the long and short forms of the PSEQ were both satisfactory, being 0.93 and 0.79 respectively.
Socio-demographic profile
Independent sample t tests showed no significant difference in age (mean 39.7 years, s.d.=9.05 v. 41.0 years, s.d.=9.16; t=-1.47, P>0.05), duration of illness (mean 9.35 years, s.d.=3.59 v. 9.50 years, s.d.=4.08; t=-0.40, P>0.05) and educational level (mean 3.34 years, s.d.=1.20 v. 3.39 years, s.d.=1.20; t=-0.46, P>0.05) between the patients with schizophrenia and those with diabetes. Those with schizophrenia earned a significantly lower income than those with diabetes (t=-13.14; P<0.001): whereas 68.6% of the former earned less than US $500 per month, 62.5% of the latter earned more than US $500 per month. Four-fifths of the patients with schizophrenia were single, whereas two-thirds of the diabetes group were married. Significant association existed between having schizophrenia and being unmarried (χ2=133.50; P<0.001).
Work-related stigma
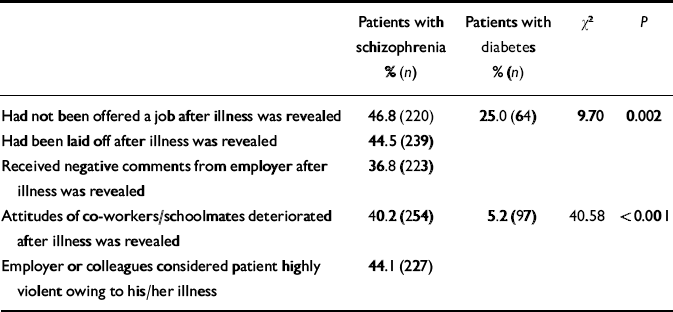
More than a third of patients with schizophrenia received negative comments from employers after their illness was revealed (Table 1). Many indicated that their colleagues' or schoolmates' attitudes deteriorated after such disclosure. Significantly more people with schizophrenia than diabetes had been refused a job because of their illness, and almost half of patients with schizophrenia reported having been laid off upon disclosure.
Table 1 Work-related stigma experience of patients with schizophrenia and diabetes mellitus
| Patients with schizophrenia % (n) | Patients with diabetes % (n) | χ2 | P | |
|---|---|---|---|---|
| Had not been offered a job after illness was revealed | 46.8 (220) | 25.0 (64) | 9.70 | 0.002 |
| Had been laid off after illness was revealed | 44.5 (239) | |||
| Received negative comments from employer after illness was revealed | 36.8 (223) | |||
| Attitudes of co-workers/schoolmates deteriorated after illness was revealed | 40.2 (254) | 5.2 (97) | 40.58 | < 0.001 |
| Employer or colleagues considered patient highly violent owing to his/her illness | 44.1 (227) |
Interpersonal stigma
Family members
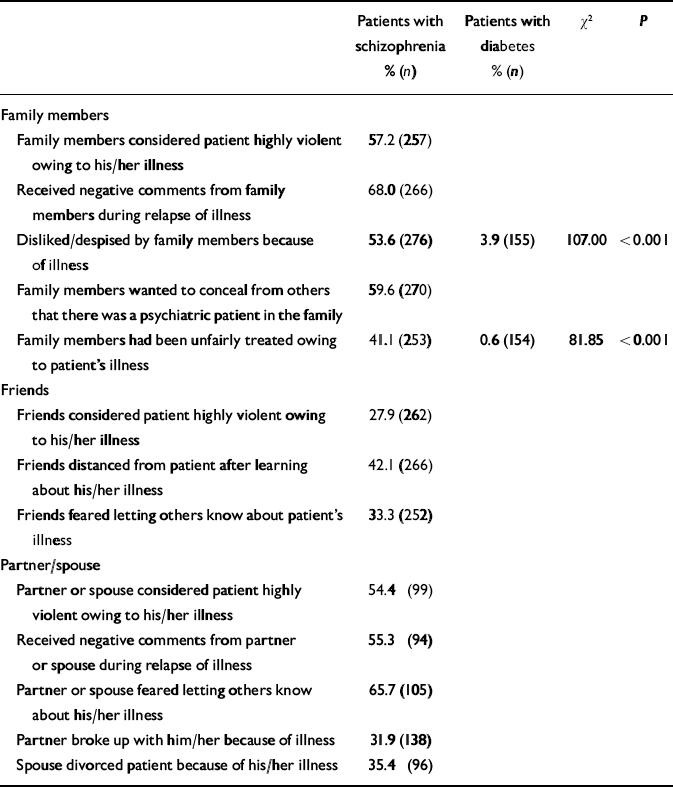
Stigma from parents, siblings or close relatives was frequent; 57.2% of the patients with schizophrenia reported that family members considered them highly violent (Table 2). The majority received negative remarks from family members during relapse. More than half (53.6%) of them, compared with only 3.9% of patients with diabetes, felt disliked or despised by family members; 59.6% also indicated that family members wanted to conceal from others the presence of a psychiatric patient in the family. A much higher percentage of patients with schizophrenia than with diabetes reported that their family members had been unfairly treated owing to their illness.
Table 2 Interpersonal stigma experience of patients with schizophrenia and diabetes mellitus
| Patients with schizophrenia % (n) | Patients with diabetes % (n) | χ2 | P | |
|---|---|---|---|---|
| Family members | ||||
| Family members considered patient highly violent owing to his/her illness | 57.2 (257) | |||
| Received negative comments from family members during relapse of illness | 68.0 (266) | |||
| Disliked/despised by family members because of illness | 53.6 (276) | 3.9 (155) | 107.00 | < 0.001 |
| Family members wanted to conceal from others that there was a psychiatric patient in the family | 59.6 (270) | |||
| Family members had been unfairly treated owing to patient's illness | 41.1 (253) | 0.6 (154) | 81.85 | < 0.001 |
| Friends | ||||
| Friends considered patient highly violent owing to his/her illness | 27.9 (262) | |||
| Friends distanced from patient after learning about his/her illness | 42.1 (266) | |||
| Friends feared letting others know about patient's illness | 33.3 (252) | |||
| Partner/spouse | ||||
| Partner or spouse considered patient highly violent owing to his/her illness | 54.4 (99) | |||
| Received negative comments from partner or spouse during relapse of illness | 55.3 (94) | |||
| Partner or spouse feared letting others know about his/her illness | 65.7 (105) | |||
| Partner broke up with him/her because of illness | 31.9 (138) | |||
| Spouse divorced patient because of his/her illness | 35.4 (96) |
Friends
In the schizophrenia group, 42.1% of patients reported that their friends distanced themselves after finding out about the patient's illness, and 33.3% indicated that their friends feared letting others know about their illness.
Partner
More than half of patients with schizophrenia who were married or in a sexual relationship reported that their partner considered them to be highly violent, and a similar proportion received negative comments from their partners during relapse; two-thirds reported that their partner avoided letting others know about their illness, and about a third reported that their partner broke up with them because of their mental illness or attributed their divorce to their illness (Table 2).
Concealment and anticipated stigma
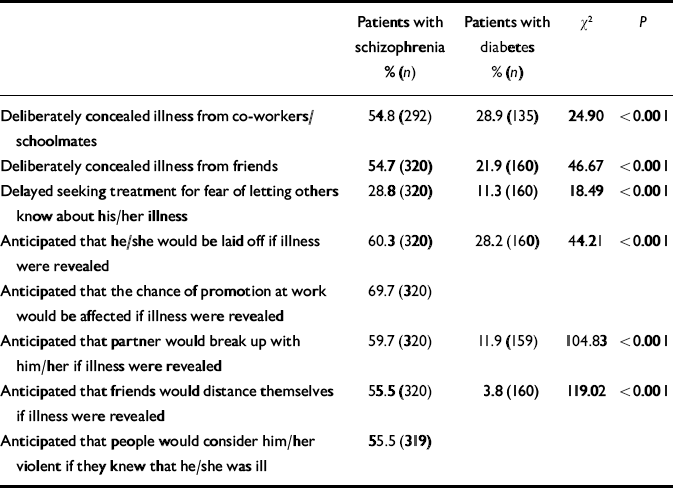
Compared with patients with diabetes, patients with schizophrenia were much more likely to conceal their illness from others and to anticipate discreditation during social exposure (Table 3). At work, almost 70% anticipated that their chance of getting promoted would be affected if their illness were revealed and significantly more patients with schizophrenia than with diabetes anticipated that they would be laid off. Regarding unmarried patients with partners, more than half of the schizophrenia group expected that the latter would leave them should their illness be revealed; only 11.9% of the diabetic group thought this would occur. Significantly more people in the schizophrenia group (55.5%) than in the diabetes group (3.8%) predicted that friends would distance themselves if the latter knew about their illness. Patients with schizophrenia made more effort to conceal their illness: over half of them did so from both colleagues or schoolmates and friends. In contrast, only a fifth of patients with diabetes concealed their illness from friends.
Table 3 Concealment of illness and anticipated stigmatisation
| Patients with schizophrenia % (n) | Patients with diabetes % (n) | χ2 | P | |
|---|---|---|---|---|
| Deliberately concealed illness from co-workers/schoolmates | 54.8 (292) | 28.9 (135) | 24.90 | < 0.001 |
| Deliberately concealed illness from friends | 54.7 (320) | 21.9 (160) | 46.67 | < 0.001 |
| Delayed seeking treatment for fear of letting others know about his/her illness | 28.8 (320) | 11.3 (160) | 18.49 | < 0.001 |
| Anticipated that he/she would be laid off if illness were revealed | 60.3 (320) | 28.2 (160) | 44.21 | < 0.001 |
| Anticipated that the chance of promotion at work would be affected if illness were revealed | 69.7 (320) | |||
| Anticipated that partner would break up with him/her if illness were revealed | 59.7 (320) | 11.9 (159) | 104.83 | < 0.001 |
| Anticipated that friends would distance themselves if illness were revealed | 55.5 (320) | 3.8 (160) | 119.02 | < 0.001 |
| Anticipated that people would consider him/her violent if they knew that he/she was ill | 55.5 (319) |
Emotional reactions to stigmatisation
The perception of stigmatisation and anxiety over disclosure caused emotional distress in a considerable proportion of patients with schizophrenia - over half felt that they were of a lower class or worthless because of their illness (Table 4); 40.6% deliberately avoided most social contacts and 43.8% had thought of ending their lives.
Table 4 Emotional reactions to stigmatisation of patients with schizophrenia

| Patients with schizophrenia % (n) | |
|---|---|
| Felt lower class or lower status | 50.2 (319) |
| Wanted to end his/her life as a result of stigmatisation and injustice | 43.8 (320) |
| Felt that being ill was his/her own fault | 35.4 (319) |
| Avoided interpersonal contact as a result of stigmatisation and injustice | 40.6 (320) |
| Felt bad about concealing his/her illness | 38.8 (258) |
DISCUSSION
Actual and anticipated interpersonal stigma experiences were substantially more common among patients with schizophrenia than among those with diabetes, even though both schizophrenia and diabetes are chronic and treatable physical diseases - of the brain in the former case, and of the endocrine system in the latter. One correlate of pervasive stigma was social marginalisation, as reflected by the poorer occupational and marital status of patients with schizophrenia.
Stigma in the local world
According to vignette and self-report studies, increased personal contact with psychiatric patients could reduce people's stigmatising attitudes (Reference Alexander and LinkAlexander & Link, 2003; Reference Couture and PennCouture & Penn, 2003), presumably through the mechanism of exposure-induced reduction of negative stereotypes about mental illness. However, our findings contradicted this experimentally demonstrated positive impact of exposure - the very people who were in most frequent contact with the psychiatric patients could also be significant sources of stigma. This paradox suggests that certain factors could be more powerful than negative stereotypes in interpersonal stigmatisation.
In Chinese culture, where interdependence is highly valued, kinship and friendship have been said to act as a potent reservoir of support for psychiatric patients (Reference KirmayerKirmayer, 1989). Our study, unfortunately, showed that stigma from significant others was pervasive. Stigma from such closely bonded individuals was much more hurtful than that arising in the public domain, where mental illness was easier to conceal. Its traumatising impact on patients' well-being and course of illness could hardly be overemphasised (Reference Kleinman and KleinmanKleinman & Kleinman, 1997). As anecdotal evidence, one of our study participants, a 36-year-old man, reported having been shouted at by his younger sister, ‘Crazy people shouldn't live with normal ones! I'll sever any connection with you! If you don't move out, I'll just throw away all your belongings!’ Another 50-year-old participant reported having been abandoned: his wife and his daughter did not visit him in hospital, and a few months later he received a letter demanding a divorce. He never saw them again.
Clearly, a collectivist culture such as that of the Chinese does not protect psychiatric patients against familial stigma. The intrafamilial and social connections of moral favour (renqing) and relationship (guanxi) can break down in the face of the powerful forces of stigma (Reference Kleinman and KleinmanKleinman & Kleinman, 1997). Thus, studies in China indicated that families might ultimately abandon a member with schizophrenia (Reference Xiong, Phillips and HuXiong et al, 1994). Such abandonment was particularly distressing because unmarried adults are generally expected to live with their parents and siblings in Chinese society.
Chinese culture and courtesy stigma
Albeit universal, psychiatric stigma is likely to exert a context-specific impact (Reference LeeLee, 2002). In Chinese society, it has been suggested that psychiatric stigma is attached as much to the family as to the individual (Reference KirmayerKirmayer, 1989). Consequently, an entire family takes up the shame and burden of having a mentally ill member throughout the course of the illness. In order to avoid public shame and marginalisation, Chinese families frequently conceal the mental illness of their members (Reference Lin and LinLin & Lin, 1981).
Our study provides empirical evidence for the presence of such familial ‘courtesy stigma’ (Reference GoffmanGoffman, 1968) and deliberate concealment. For example, about 40% of the patients with schizophrenia had family members who had been unfairly treated because of the patients' illness, and over 60% reported that their family members and partners would attempt to cover up the presence of a relative with schizophrenia. Concealment was thus a common response and a strategy of de-stigmatisation that, nonetheless, could induce anxiety among family members as it involved, strictly speaking, the telling of lies. Thus, family members acted as both stigmatisers and victims of stigmatisation themselves. Because of this paradoxical role dualism, family members might project their anger towards a patient for causing them added suffering. This negative affective state, we suspect, could heighten the chronic burden of care. It could also lead to the displacement of frustration on to the patient, even though family members could already have learned through intimate contact that psychiatric patients were neither violent nor inhuman.
Although research data are lacking, intrafamilial stigma could be connected with high levels of expressed emotion, which worsens the outcome of schizophrenia (Reference Leff and VaughnLeff & Vaughn, 1985). In Beijing, one recent study demonstrated that 40.3% of the family members of in-patients with schizophrenia exhibited high expressed emotion (Reference Xu, Phillips and WengXu et al, 2003), and another showed that high expressed emotion was correlated with subjective (non-familial) stigma experience among people with schizophrenia (Reference Phillips, Pearson and LiPhillips et al, 2002). The interactions between high expressed emotion and intrafamilial stigma in different ethnic communities therefore warrant further research.
Implications for stigma reduction
Anti-stigma community campaigns have usually emphasised the transmission of medical knowledge and the normalising of media coverage of psychiatric patients (Reference Hayward and BrightHayward & Bright, 1997; Reference Corrigan and PennCorrigan & Penn, 1999; Reference CrispCrisp, 2001). In Hong Kong, more attention has recently been given to the harm of stigmatising public attitudes. However, few programmes have been devised to tackle stigma arising from patients' significant others.
Our study suggests that family support cannot be assumed during the typically chronic course of schizophrenia. Consequently, psychiatric care must move beyond symptom control to diminish blatant as well as subtle forms of stigmatisation in the patients' social life. Since stigma may build up over time, opportune intervention is required to turn families into long-term resources or even advocates for psychiatric care (Reference LeeLee, 2002); that might in turn buffer patients and their caregivers against stigma in the public domain. Regarding the reduction of work-related stigma, we believe that a combination of corporate education programmes, legal measures and advocacy efforts are needed.
Limitations and future studies
Our study had certain limitations. First, our participants were not representative of the entire population of patients with schizophrenia in Hong Kong; our sample was biased toward ‘halfway house’ inmates, who might have experienced more family rejection than patients with disease of recent onset who lived with their family. Although having a mental illness may even be a positive experience (Reference Dinos, Stevens and SerfatyDinos et al, 2004), our findings reflected at least the situation of the large number of patients with a socially deprived status. Second, the study examined only the subjective experience of patients. Although stigma defies a gold standard of measurement, its comprehensive understanding requires a multi-dimensional framework in which the perspectives of the stigmatiser, the stigmatised and the context of stigmatisation are considered in parallel (Reference Dovidio, Major and CrockerDovidio et al, 2000). Third, although we found the family to be a source of stigma, we have not examined the conflictual duality of family members being both stigmatisers and victims of courtesy stigma. Fourth, the PSEQ provided a quantifiable but none the less exploratory account of stigma experience. Further studies are needed to develop a psychometrically robust instrument for studying stigma quantitatively.
Ethnographic approaches that probe more deeply into interpersonal interactions, political economy and embedded meanings of stigma over time are needed to examine the deep and unique experience of stigma. Future studies should investigate other sources of stigmatisation, such as that arising from psychiatric diagnosis and treatment, and the impact of stigma on the outcome of schizophrenia.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Stigma experience is pervasive: it deeply affects the social, occupational and emotional well-being of patients with schizophrenia and should be included in clinical management.
-
▪ Family support for Chinese patients with schizophrenia should not be taken for granted and needs to be nurtured.
-
▪ Family programmes should start early to reduce stigma from significant others and to transform the family into a long-term resource for psychiatric rehabilitation.
LIMITATIONS
-
▪ The study findings may not be generalisable to patients with a shorter duration of illness and residing with family members.
-
▪ The perspectives of stigmatisers and the context of stigmatisation were not studied.
-
▪ No examination was made of the impact of interpersonal stigma on illness outcome.
Acknowledgements
The study was funded by the Equal Opportunities Commission and the. Department of Psychiatry of The Chinese University of Hong Kong.









eLetters
No eLetters have been published for this article.