Many studies in the UK have found that African–Caribbean and Black African patients are more likely than White patients to come into contact with mental health services compulsorily and by adversarial routes, such as those involving the police and other criminal justice agencies (Reference Bhui, Stansfeld and HullBhui et al, 2003). However, the reasons for these differences – and the points at which they develop – remain poorly understood, and two recent reviews have highlighted a number of methodological limitations that characterise much of the previous research in this area (Reference Bhui, Stansfeld and HullBhui et al, 2003; Reference Morgan, Mallett and HutchinsonMorgan et al, 2004). These include use of crude ethnic categories (e.g. Black, White); small sample sizes; heterogeneous samples (e.g. all diagnostic groups, or those with first onset and chronic illness); and limited adjustment for potential confounding factors. For example, the importance of distinguishing between first and subsequent presentations to services is highlighted in the two most recent studies among patients with a first episode of psychosis. In contrast to most research, neither of these studies found a difference in compulsory admissions between White and Black patients (Reference Cole, Leavey and KingCole et al, 1995; Reference Burnett, Mallett and BhugraBurnett et al, 1999). However, both these studies were small, and in the study by Cole et al (Reference Cole, Leavey and King1995) ethnic groups were crudely defined as White or Black. Therefore, the extent to which these findings can be generalised is unclear.
We therefore sought to investigate the relationship between ethnicity and pathways to mental health services in two UK centres in a large cohort of patients with a first episode of psychosis. In this paper our focus is specifically on ethnicity and compulsory admission, the aim being to test the hypothesis that there is an association between compulsory admission and ethnicity at first presentation, independent of socio-demographic characteristics, aspects of clinical presentation and how patients came into contact with services.
METHOD
This research forms part of the Aetiology and Ethnicity in Schizophrenia and Other Psychoses (ÆSOP) study. This is a three-centre epidemiological study, conducted over a 2-year period, of all patients with a first episode of psychosis (codes F20–29 and F30–33 in ICD–10; World Health Organization, 1992a ) who presented to secondary and tertiary services within tightly defined catchment areas in south-east London, Nottingham and Bristol. Potential patients were screened for inclusion using the Screening Schedule for Psychosis (Reference Jablensky, Sartorius and ErnbergJablensky et al, 1992). Each patient who screened positive was approached to take part in the study and permission was sought to interview a relative who had been in recent contact with the patient. In south-east London and Nottingham patients were recruited over a 2-year period, and in Bristol over a 9-month period. The data reported here relate to the London and Nottingham arms of the study, the two centres for which data were available for a 2-year period. Exclusion criteria were age under 16 years or over 65 years; evidence of psychotic symptoms precipitated by an organic cause; and transient psychotic symptoms resulting from acute intoxication as defined by ICD–10. No patient included in the study had an IQ of less than 65.
Data collection
Socio-demographic characteristics
Data on ethnicity, gender, educational level achieved, employment status, living circumstances and relationship status were collected by interview with patients or (for patients not interviewed) from case notes, using the Medical Research Council Socio-demographic Schedule (Reference MallettMallett, 1997).
Clinical data
Clinical data were collected using the Schedules for Clinical Assessment in Neuropsychiatry (SCAN; World Health Organization, 1992b ) and the Personal and Psychiatric History Schedule (PPHS; World Health Organization, 1996). The SCAN incorporates the Present State Examination version 2.0, which was used to elicit symptom-related data at the time of presentation. Where an interview with the patient was not possible, case notes were used to complete the Item Group Checklist part of the SCAN. Diagnoses according to ICD–10 criteria were determined using the SCAN data on the basis of consensus meetings involving one of the ÆSOP study's principal investigators (J.L. or R. Murray in London and P.J. in Nottingham) and other members of the research team. For the analysis, patients were grouped into three diagnostic categories: broad schizophrenia and other psychoses (codes F20–29), manic psychosis (F30–31) and depressive psychosis (F32–33). There was an assessment for possible bias between the principal psychiatrists. Each independently formulated a diagnosis for 20 patients based on the same summary SCAN information; there was 80% agreement on diagnostic category (κ=0.63–0.75, P<0.001).
The PPHS, previously used in World Health Organization multicentre studies of the incidence and outcome of schizophrenia (Reference Jablensky, Sartorius and ErnbergJablensky et al, 1992) and in previous studies of pathways to care (Reference Burnett, Mallett and BhugraBurnett et al, 1999), was used to collate further clinical data, specifically relating to duration of untreated psychosis and reasons for admission. Duration of untreated psychosis was defined as the period from the first clear description of psychotic phenomena, from any source, to first contact with statutory mental health services; it was analysed as a dichotomous variable, cut into ‘short’ and ‘long’ around the median of 66 days. Reasons for admission considered in the analysis were act of self-harm, perceived risk to self, act of violence and perceived risk to others.
Pathways to care
Data relating to pathways to care and mode of contact with services were collated using the PPHS. The section on pathways to care was extended to include an item on who initiated help-seeking and to allow a detailed narrative description of the pathway to care. The relevant variables derived from these data were: the person who initiated help-seeking; involvement of criminal justice agencies (police, courts, prisons) and general practitioners in the pathway; source of referral to services; and mode of contact (non-compulsory v. compulsory).
Ethnicity
Patients assigned to one of the following four ethnic groups were included in the analysis:
-
(a) White British: all White patients with at least one parent born in the UK;
-
(b) African–Caribbean: all Black patients born in the Caribbean or born in the UK with at least one parent of Caribbean origin;
-
(c) Black African: all Black patients born in sub-Saharan Africa or born in the UK with at least one parent of sub-Saharan African origin;
-
(d) other White: all White patients with no parent born in the UK.
There was no patient of mixed Caribbean–African parentage in the study, and patients of other ethnicities were excluded from the analysis.
In assigning patients to ethnic groups, a number of data sources were used. The primary source was self-ascribed ethnicity, collected as part of the socio-demographic interview. If this was not available other sources were used, including other informants and case notes. Where there was ambiguity, a consensus rating was made by members of the research team; this always included those with long-standing expertise in the study of ethnicity and mental health (R. Mallett, G.H.).
Analysis
Chi-squared tests were used to compare ethnic groups in each study centre according to the key study variables. The data were stratified by study centre at this point to assess whether there were any marked differences between the samples drawn from the two distinct service settings. Logistic regression was used to analyse the relationship between ethnicity and compulsory admission while controlling for potential confounders, thereby addressing the primary study hypothesis. A logistic regression model was constructed, with compulsory admission as the dependent variable, using the following steps. First, to identify crude associations between compulsory admission and other variables, unadjusted odds ratios were calculated. Second, using Mantel–Haenszel analyses with the test for homogeneity, potential effect modifiers for the association between ethnicity and compulsory admission were identified. Third, a logistic regression model with the primary outcome (compulsory admission), exposure (ethnicity) and a variable for study centre was fitted, and variables found to be crudely associated with compulsory admission at P<0.10 were added one by one, starting with the strongest. Finally, interaction terms for ethnicity and potential effect modifiers, identified using Mantel–Haenszel analyses, were fitted. For each new variable or interaction term fitted, a likelihood ratio test was conducted by checking each nested model against the new potential model. Variables and interaction terms were retained in the model if the P value for the likelihood ratio test was <0.10. At each point, a liberal value of P=0.10 was used as a cut-off point to ensure that potentially important factors were not removed from the analysis. All analyses were conducted using STATA version 8 (Stata, 2003).
RESULTS
During the 2-year study period a total of 512 patients with a first episode of psychosis presented to services: 309 in south-east London and 203 in Nottingham. Of these, 92% (469) were White British, other White, African–Caribbean or Black African. For seven patients, information relating to the primary study outcome (mode of contact) was not available (six in south-east London, one in Nottingham), and these cases were also excluded from the analysis. The small number of patients for whom other data were missing, for example who initiated help-seeking (34 missing values), were included and the missing values are noted in the relevant tables. Where data were missing this was primarily due to absence of clear information in the case notes. There was no evidence that the proportion of missing values varied systematically between key groups in the sample.
Of the 462 patients included in the analysis, 301 (65.2%) were interviewed. Of those not interviewed, 66 (14.3%) were included in a leakage study that was conducted at the end of the period of patient recruitment to pick up all patients meeting the inclusion criteria who were not initially identified. There was no consistent reason why patients identified as part of the leakage study were initially missed, and these patients were not approached to be interviewed. Ninety-five (20.5%) could not be successfully contacted following presentation or refused to be interviewed. Of the 301 patients interviewed, 118 (39.2%) had a close relative with whom they had been in recent contact and who agreed to be interviewed. Case notes were scrutinised for all patients. The basic socio-demographic, clinical and pathway-related variables were compared between those who were interviewed and those were not interviewed, and between those with and those without a relative interview, to assess whether they differed in any key respects. There were no statistically significant differences between the groups. In particular, there was no difference in the proportions of patients or relatives interviewed in each ethnic group.
Sample characteristics
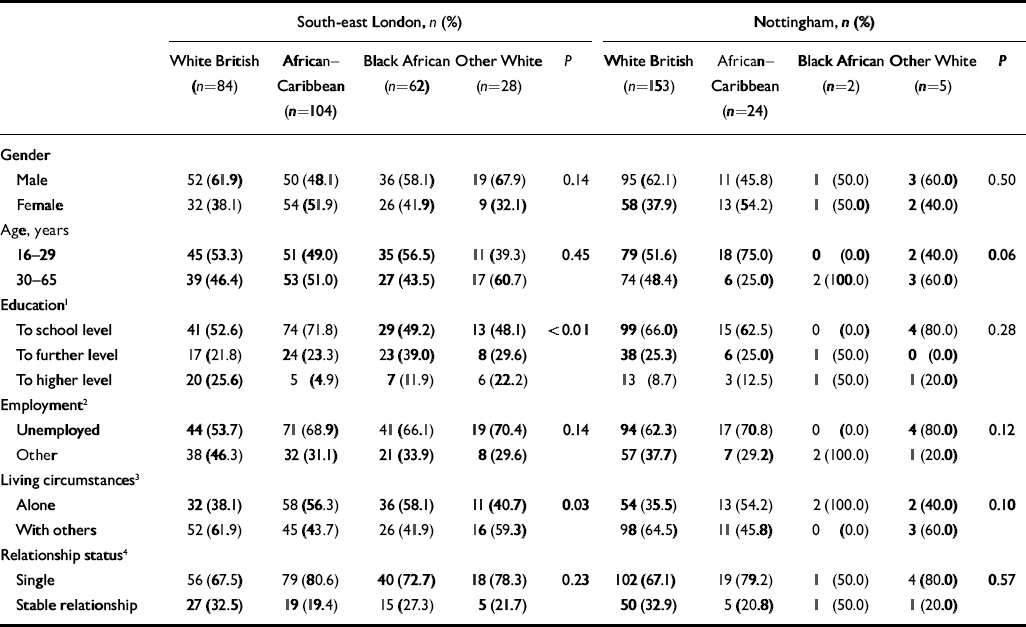
Socio-demographic and clinical characteristics of the sample are summarised by study site and ethnicity in Tables 1 and 2.
Table 1 Socio-demographic characteristics by study centre and ethnicity
| South-east London, n (%) | Nottingham, n (%) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| White British (n=84) | African-Caribbean (n=104) | Black African (n=62) | Other White (n=28) | P | White British (n=153) | African-Caribbean (n=24) | Black African (n=2) | Other White (n=5) | P | |
| Gender | ||||||||||
| Male | 52 (61.9) | 50 (48.1) | 36 (58.1) | 19 (67.9) | 0.14 | 95 (62.1) | 11 (45.8) | 1 (50.0) | 3 (60.0) | 0.50 |
| Female | 32 (38.1) | 54 (51.9) | 26 (41.9) | 9 (32.1) | 58 (37.9) | 13 (54.2) | 1 (50.0) | 2 (40.0) | ||
| Age, years | ||||||||||
| 16-29 | 45 (53.3) | 51 (49.0) | 35 (56.5) | 11 (39.3) | 0.45 | 79 (51.6) | 18 (75.0) | 0 (0.0) | 2 (40.0) | 0.06 |
| 30-65 | 39 (46.4) | 53 (51.0) | 27 (43.5) | 17 (60.7) | 74 (48.4) | 6 (25.0) | 2 (100.0) | 3 (60.0) | ||
| Education1 | ||||||||||
| To school level | 41 (52.6) | 74 (71.8) | 29 (49.2) | 13 (48.1) | <0.01 | 99 (66.0) | 15 (62.5) | 0 (0.0) | 4 (80.0) | 0.28 |
| To further level | 17 (21.8) | 24 (23.3) | 23 (39.0) | 8 (29.6) | 38 (25.3) | 6 (25.0) | 1 (50.0) | 0 (0.0) | ||
| To higher level | 20 (25.6) | 5 (4.9) | 7 (11.9) | 6 (22.2) | 13 (8.7) | 3 (12.5) | 1 (50.0) | 1 (20.0) | ||
| Employment2 | ||||||||||
| Unemployed | 44 (53.7) | 71 (68.9) | 41 (66.1) | 19 (70.4) | 0.14 | 94 (62.3) | 17 (70.8) | 0 (0.0) | 4 (80.0) | 0.12 |
| Other | 38 (46.3) | 32 (31.1) | 21 (33.9) | 8 (29.6) | 57 (37.7) | 7 (29.2) | 2 (100.0) | 1 (20.0) | ||
| Living circumstances3 | ||||||||||
| Alone | 32 (38.1) | 58 (56.3) | 36 (58.1) | 11 (40.7) | 0.03 | 54 (35.5) | 13 (54.2) | 2 (100.0) | 2 (40.0) | 0.10 |
| With others | 52 (61.9) | 45 (43.7) | 26 (41.9) | 16 (59.3) | 98 (64.5) | 11 (45.8) | 0 (0.0) | 3 (60.0) | ||
| Relationship status4 | ||||||||||
| Single | 56 (67.5) | 79 (80.6) | 40 (72.7) | 18 (78.3) | 0.23 | 102 (67.1) | 19 (79.2) | 1 (50.0) | 4 (80.0) | 0.57 |
| Stable relationship | 27 (32.5) | 19 (19.4) | 15 (27.3) | 5 (21.7) | 50 (32.9) | 5 (20.8) | 1 (50.0) | 1 (20.0) | ||
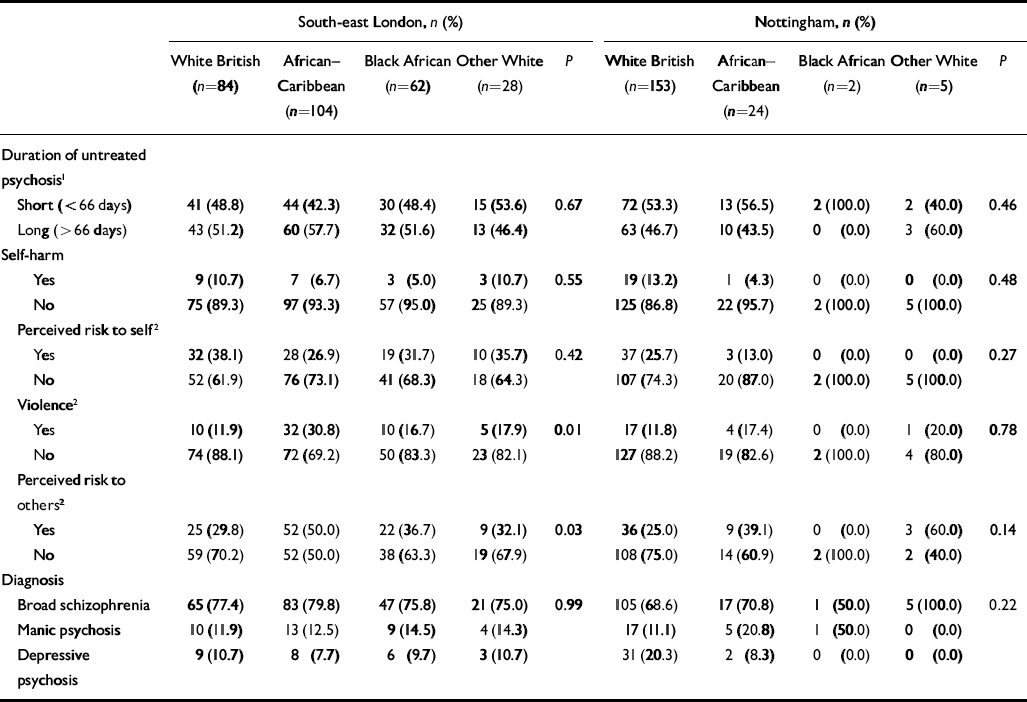
Table 2 Clinical characteristics by study centre and ethnicity
| South-east London, n (%) | Nottingham, n (%) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| White British (n=84) | African—Caribbean (n=104) | Black African (n=62) | Other White (n=28) | P | White British (n=153) | African—Caribbean (n=24) | Black African (n=2) | Other White (n=5) | P | |
| Duration of untreated psychosis1 | ||||||||||
| Short (<66 days) | 41 (48.8) | 44 (42.3) | 30 (48.4) | 15 (53.6) | 0.67 | 72 (53.3) | 13 (56.5) | 2 (100.0) | 2 (40.0) | 0.46 |
| Long (>66 days) | 43 (51.2) | 60 (57.7) | 32 (51.6) | 13 (46.4) | 63 (46.7) | 10 (43.5) | 0 (0.0) | 3 (60.0) | ||
| Self-harm | ||||||||||
| Yes | 9 (10.7) | 7 (6.7) | 3 (5.0) | 3 (10.7) | 0.55 | 19 (13.2) | 1 (4.3) | 0 (0.0) | 0 (0.0) | 0.48 |
| No | 75 (89.3) | 97 (93.3) | 57 (95.0) | 25 (89.3) | 125 (86.8) | 22 (95.7) | 2 (100.0) | 5 (100.0) | ||
| Perceived risk to self2 | ||||||||||
| Yes | 32 (38.1) | 28 (26.9) | 19 (31.7) | 10 (35.7) | 0.42 | 37 (25.7) | 3 (13.0) | 0 (0.0) | 0 (0.0) | 0.27 |
| No | 52 (61.9) | 76 (73.1) | 41 (68.3) | 18 (64.3) | 107 (74.3) | 20 (87.0) | 2 (100.0) | 5 (100.0) | ||
| Violence2 | ||||||||||
| Yes | 10 (11.9) | 32 (30.8) | 10 (16.7) | 5 (17.9) | 0.01 | 17 (11.8) | 4 (17.4) | 0 (0.0) | 1 (20.0) | 0.78 |
| No | 74 (88.1) | 72 (69.2) | 50 (83.3) | 23 (82.1) | 127 (88.2) | 19 (82.6) | 2 (100.0) | 4 (80.0) | ||
| Perceived risk to others2 | ||||||||||
| Yes | 25 (29.8) | 52 (50.0) | 22 (36.7) | 9 (32.1) | 0.03 | 36 (25.0) | 9 (39.1) | 0 (0.0) | 3 (60.0) | 0.14 |
| No | 59 (70.2) | 52 (50.0) | 38 (63.3) | 19 (67.9) | 108 (75.0) | 14 (60.9) | 2 (100.0) | 2 (40.0) | ||
| Diagnosis | ||||||||||
| Broad schizophrenia | 65 (77.4) | 83 (79.8) | 47 (75.8) | 21 (75.0) | 0.99 | 105 (68.6) | 17 (70.8) | 1 (50.0) | 5 (100.0) | 0.22 |
| Manic psychosis | 10 (11.9) | 13 (12.5) | 9 (14.5) | 4 (14.3) | 17 (11.1) | 5 (20.8) | 1 (50.0) | 0 (0.0) | ||
| Depressive | 9 (10.7) | 8 (7.7) | 6 (9.7) | 3 (10.7) | 31 (20.3) | 2 (8.3) | 0 (0.0) | 0 (0.0) | ||
| psychosis | ||||||||||
Socio-demographic characteristics
In south-east London, African–Caribbean patients were significantly less likely than the other three ethnic groups to be educated beyond school level, this being particularly evident in the small number of African–Caribbean patients who were educated at university level. Levels of unemployment were higher in all ethnic minority groups than in the White British group, although this only reached statistical significance for the African–Caribbean group. Both African–Caribbean and Black African patients were significantly more likely to live alone than White British patients, and African–Caribbean patients were significantly more likely to be single than White British patients. In the Nottingham sample, there were similar differences between White British and African–Caribbean patients, but the relatively small number of the latter meant these differences did not reach statistical significance.
Clinical data
For the clinical variables considered, there were few ethnic differences in either centre; for example, there was no difference between the ethnic groups in duration of untreated psychosis. The main difference between the ethnic groups in south-east London was in the reasons for admission, with African–Caribbean patients being significantly more likely than all other groups to be involved in a violent incident and/or be perceived as threatening by others. This was less evident in the Nottingham sample, although African–Caribbean patients were more likely to be perceived as threatening (39.1% v. 25.0%; χ2=2.01, d.f.=1, P=0.16).
Mode of contact and pathways to care
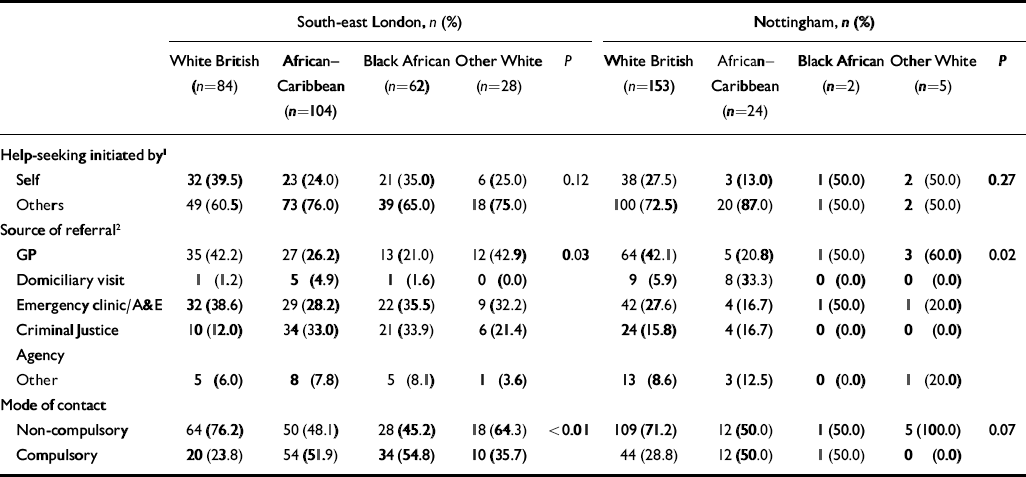
Data relating to pathways to care and mode of contact with services are presented in Table 3.
Table 3 Pathways to care by study centre and ethnicity
| South-east London, n (%) | Nottingham, n (%) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| White British (n=84) | African—Caribbean (n=104) | Black African (n=62) | Other White (n=28) | P | White British (n=153) | African—Caribbean (n=24) | Black African (n=2) | Other White (n=5) | P | |
| Help-seeking initiated by1 | ||||||||||
| Self | 32 (39.5) | 23 (24.0) | 21 (35.0) | 6 (25.0) | 0.12 | 38 (27.5) | 3 (13.0) | 1 (50.0) | 2 (50.0) | 0.27 |
| Others | 49 (60.5) | 73 (76.0) | 39 (65.0) | 18 (75.0) | 100 (72.5) | 20 (87.0) | 1 (50.0) | 2 (50.0) | ||
| Source of referral2 | ||||||||||
| GP | 35 (42.2) | 27 (26.2) | 13 (21.0) | 12 (42.9) | 0.03 | 64 (42.1) | 5 (20.8) | 1 (50.0) | 3 (60.0) | 0.02 |
| Domiciliary visit | 1 (1.2) | 5 (4.9) | 1 (1.6) | 0 (0.0) | 9 (5.9) | 8 (33.3) | 0 (0.0) | 0 (0.0) | ||
| Emergency clinic/A&E | 32 (38.6) | 29 (28.2) | 22 (35.5) | 9 (32.2) | 42 (27.6) | 4 (16.7) | 1 (50.0) | 1 (20.0) | ||
| Criminal Justice | 10 (12.0) | 34 (33.0) | 21 (33.9) | 6 (21.4) | 24 (15.8) | 4 (16.7) | 0 (0.0) | 0 (0.0) | ||
| Agency | ||||||||||
| Other | 5 (6.0) | 8 (7.8) | 5 (8.1) | 1 (3.6) | 13 (8.6) | 3 (12.5) | 0 (0.0) | 1 (20.0) | ||
| Mode of contact | ||||||||||
| Non-compulsory | 64 (76.2) | 50 (48.1) | 28 (45.2) | 18 (64.3) | <0.01 | 109 (71.2) | 12 (50.0) | 1 (50.0) | 5 (100.0) | 0.07 |
| Compulsory | 20 (23.8) | 54 (51.9) | 34 (54.8) | 10 (35.7) | 44 (28.8) | 12 (50.0) | 1 (50.0) | 0 (0.0) | ||
Mode of contact
In both south-east London and Nottingham, African–Caribbean patients were significantly more likely to be compulsorily admitted than White British patients. The proportion of patients in each of these ethnic groups who were compulsorily admitted was remarkably similar in the two centres: in south-east London, 23.8% White British v. 51.9% African–Caribbean (unadjusted odds ratio 3.46; 95% CI 1.84–6.51, P<0.01); in Nottingham, 28.8% White British v. 50.0% African–Caribbean (unadjusted odds ratio 2.48; 95% CI 1.03–5.93; P=0.04). Given this similarity, for stratified and multivariable analyses focusing on ethnicity and compulsory admission, data from the two centres were combined. In south-east London, the proportion of Black African patients who were compulsorily admitted was even higher than for African–Caribbean patients, at 54.8% (unadjusted odds ratio 3.89; 95% CI 1.91–7.89; P<0.01).
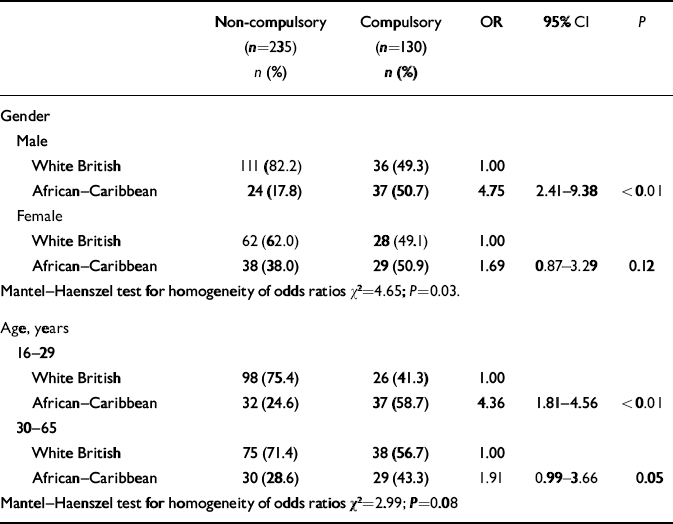
When proportions of compulsory admissions among the different ethnic groups are broken down by gender and age the picture becomes more complex. The odds of compulsory admission among African–Caribbean patients in south-east London varied by age and gender, variations that held when the data were combined with those from Nottingham. Across the two sites, the odds ratio for compulsory admission, with White British patients as the baseline group, was 4.75 for African–Caribbean men and 1.69 for African–Caribbean women (Table 4). The odds ratio for compulsory admission was 4.36 for African–Caribbean patients aged 16–29 years and 1.91 for African–Caribbean patients aged 30–65 years (Table 4). There was no evidence of similar effects for gender and age on the relationship between Black African ethnicity and compulsory admission in south-east London.
Table 4 Ethnicity (White British and African—Caribbean only) and compulsory admission, by gender and age
| Non-compulsory (n=235) n (%) | Compulsory (n=130) n (%) | OR | 95% CI | P | |
|---|---|---|---|---|---|
| Gender | |||||
| Male | |||||
| White British | 111 (82.2) | 36 (49.3) | 1.00 | ||
| African—Caribbean | 24 (17.8) | 37 (50.7) | 4.75 | 2.41-9.38 | <0.01 |
| Female | |||||
| White British | 62 (62.0) | 28 (49.1) | 1.00 | ||
| African—Caribbean | 38 (38.0) | 29 (50.9) | 1.69 | 0.87-3.29 | 0.12 |
| Mantel—Haenszel test for homogeneity of odds ratios χ2=4.65; P=0.03. | |||||
| Age, years | |||||
| 16-29 | |||||
| White British | 98 (75.4) | 26 (41.3) | 1.00 | ||
| African—Caribbean | 32 (24.6) | 37 (58.7) | 4.36 | 1.81-4.56 | <0.01 |
| 30-65 | |||||
| White British | 75 (71.4) | 38 (56.7) | 1.00 | ||
| African—Caribbean | 30 (28.6) | 29 (43.3) | 1.91 | 0.99-3.66 | 0.05 |
| Mantel—Haenszel test for homogeneity of odds ratios χ2=2.99; P=0.08 |
The proportions compulsorily admitted did not vary significantly within the south-east London sample between African–Caribbean patients born in the UK and those born in the Caribbean (57.3% v. 41.2%; χ2=2.38, d.f.=1, P=0.12). There was a trend for Black African patients born in the UK to be compulsorily admitted more often than those born in Africa (73.3% v. 46.3%; χ2=3.28, d.f.=1, P=0.07). The number of non-UK-born African–Caribbean patients in Nottingham was too small for comparisons to be made (n=4).
Pathways to care
In terms of the pathway to care, further differences were apparent (see Table 3 for selected pathways data). These data are of particular interest here as potential confounders of the relationship between ethnicity and compulsory admission.
Compulsory admission and ethnicity
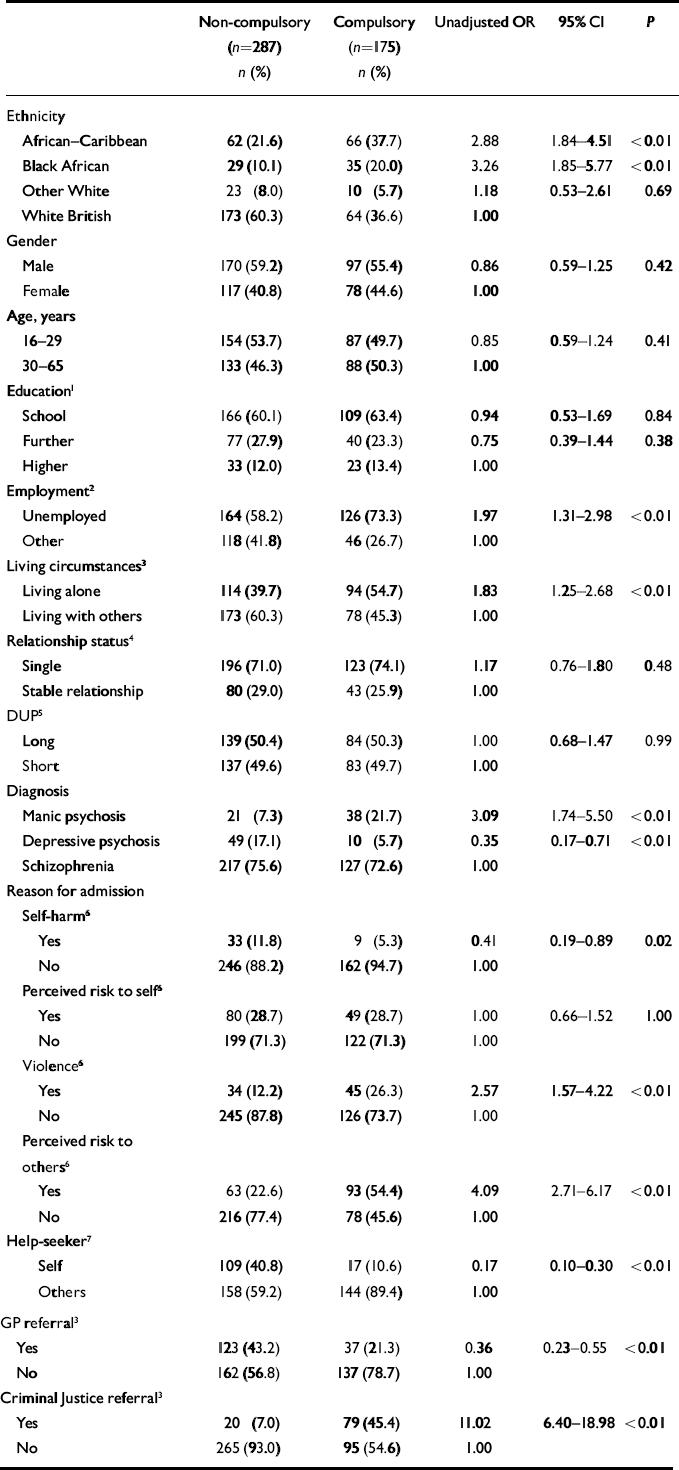
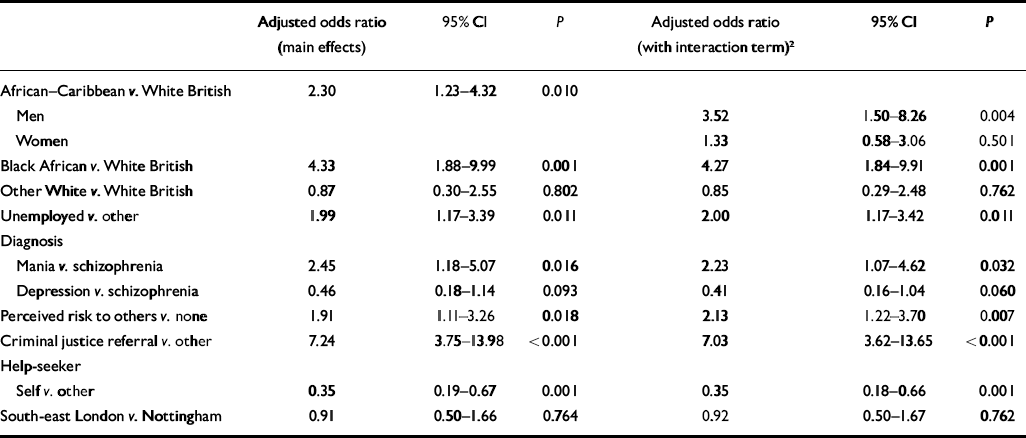
Table 5 presents the unadjusted odds ratios for compulsory admission by each independent variable using combined data for south-east London and Nottingham. It shows that, in addition to ethnicity, nine variables were associated with an increase or decrease in the odds of compulsory admission, at P<0.10. A logistic regression model was fitted, as detailed above. Following this procedure, five of the nine variables crudely associated with compulsory admission were selected for inclusion: being unemployed, criminal justice referral, perceived risk to others, self-initiated help-seeking and diagnosis. As there was evidence that the relationship between African–Caribbean ethnicity and compulsory admission was modified by gender and age, interaction terms were fitted, first for gender and African–Caribbean ethnicity and second for age and African–Caribbean ethnicity. A likelihood ratio test was conducted to assess whether each interaction term significantly improved the model; on this basis, an interaction term for gender and African–Caribbean ethnicity was included in the final model (χ2=3.02, d.f.=1, P=0.08), but not for age and African–Caribbean ethnicity (χ2=1.96, d.f.=1, P=0.16). Table 6 presents the final logistic regression model both with main effects only and with the interaction term included. This shows that, when adjusting for the other variables in the model, the odds of compulsory admission are 3.5 times greater for African–Caribbean male patients than for White British male patients. There is some attenuation of the unadjusted odds ratio, suggesting some confounding by the other variables in the model. However, among men, African–Caribbean ethnicity retains a strong independent effect on the odds of compulsory admission. The increased odds of compulsory admission observed among African–Caribbean men do not hold for African–Caribbean women. Black African ethnicity also retains a strong independent effect on the odds of compulsory admission after adjusting for the other variables in the model. The other factors that were independently associated with increased or decreased odds of compulsory admission were being unemployed, criminal justice referral, perceived risk to others, self-initiated help-seeking and a diagnosis of mania.
Table 5 Unadjusted odds ratios for compulsory admission
| Non-compulsory (n=287) n (%) | Compulsory (n=175) n (%) | Unadjusted OR | 95% CI | P | |
|---|---|---|---|---|---|
| Ethnicity | |||||
| African—Caribbean | 62 (21.6) | 66 (37.7) | 2.88 | 1.84-4.51 | <0.01 |
| Black African | 29 (10.1) | 35 (20.0) | 3.26 | 1.85-5.77 | <0.01 |
| Other White | 23 (8.0) | 10 (5.7) | 1.18 | 0.53-2.61 | 0.69 |
| White British | 173 (60.3) | 64 (36.6) | 1.00 | ||
| Gender | |||||
| Male | 170 (59.2) | 97 (55.4) | 0.86 | 0.59-1.25 | 0.42 |
| Female | 117 (40.8) | 78 (44.6) | 1.00 | ||
| Age, years | |||||
| 16-29 | 154 (53.7) | 87 (49.7) | 0.85 | 0.59-1.24 | 0.41 |
| 30-65 | 133 (46.3) | 88 (50.3) | 1.00 | ||
| Education1 | |||||
| School | 166 (60.1) | 109 (63.4) | 0.94 | 0.53-1.69 | 0.84 |
| Further | 77 (27.9) | 40 (23.3) | 0.75 | 0.39-1.44 | 0.38 |
| Higher | 33 (12.0) | 23 (13.4) | 1.00 | ||
| Employment2 | |||||
| Unemployed | 164 (58.2) | 126 (73.3) | 1.97 | 1.31-2.98 | <0.01 |
| Other | 118 (41.8) | 46 (26.7) | 1.00 | ||
| Living circumstances3 | |||||
| Living alone | 114 (39.7) | 94 (54.7) | 1.83 | 1.25-2.68 | <0.01 |
| Living with others | 173 (60.3) | 78 (45.3) | 1.00 | ||
| Relationship status4 | |||||
| Single | 196 (71.0) | 123 (74.1) | 1.17 | 0.76-1.80 | 0.48 |
| Stable relationship | 80 (29.0) | 43 (25.9) | 1.00 | ||
| DUP5 | |||||
| Long | 139 (50.4) | 84 (50.3) | 1.00 | 0.68-1.47 | 0.99 |
| Short | 137 (49.6) | 83 (49.7) | 1.00 | ||
| Diagnosis | |||||
| Manic psychosis | 21 (7.3) | 38 (21.7) | 3.09 | 1.74-5.50 | <0.01 |
| Depressive psychosis | 49 (17.1) | 10 (5.7) | 0.35 | 0.17-0.71 | <0.01 |
| Schizophrenia | 217 (75.6) | 127 (72.6) | 1.00 | ||
| Reason for admission | |||||
| Self-harm6 | |||||
| Yes | 33 (11.8) | 9 (5.3) | 0.41 | 0.19-0.89 | 0.02 |
| No | 246 (88.2) | 162 (94.7) | 1.00 | ||
| Perceived risk to self6 | |||||
| Yes | 80 (28.7) | 49 (28.7) | 1.00 | 0.66-1.52 | 1.00 |
| No | 199 (71.3) | 122 (71.3) | 1.00 | ||
| Violence6 | |||||
| Yes | 34 (12.2) | 45 (26.3) | 2.57 | 1.57-4.22 | <0.01 |
| No | 245 (87.8) | 126 (73.7) | 1.00 | ||
| Perceived risk to others6 | |||||
| Yes | 63 (22.6) | 93 (54.4) | 4.09 | 2.71-6.17 | <0.01 |
| No | 216 (77.4) | 78 (45.6) | 1.00 | ||
| Help-seeker7 | |||||
| Self | 109 (40.8) | 17 (10.6) | 0.17 | 0.10-0.30 | <0.01 |
| Others | 158 (59.2) | 144 (89.4) | 1.00 | ||
| GP referral3 | |||||
| Yes | 123 (43.2) | 37 (21.3) | 0.36 | 0.23-0.55 | <0.01 |
| No | 162 (56.8) | 137 (78.7) | 1.00 | ||
| Criminal Justice referral3 | |||||
| Yes | 20 (7.0) | 79 (45.4) | 11.02 | 6.40-18.98 | <0.01 |
| No | 265 (93.0) | 95 (54.6) | 1.00 |
Table 6 Adjusted odds ratios for compulsory admission1
| Adjusted odds ratio (main effects) | 95% CI | P | Adjusted odds ratio (with interaction term)2 | 95% CI | P | |
|---|---|---|---|---|---|---|
| African—Caribbean v. White British | 2.30 | 1.23-4.32 | 0.010 | |||
| Men | 3.52 | 1.50-8.26 | 0.004 | |||
| Women | 1.33 | 0.58-3.06 | 0.501 | |||
| Black African v. White British | 4.33 | 1.88-9.99 | 0.001 | 4.27 | 1.84-9.91 | 0.001 |
| Other White v. White British | 0.87 | 0.30-2.55 | 0.802 | 0.85 | 0.29-2.48 | 0.762 |
| Unemployed v. other | 1.99 | 1.17-3.39 | 0.011 | 2.00 | 1.17-3.42 | 0.011 |
| Diagnosis | ||||||
| Mania v. schizophrenia | 2.45 | 1.18-5.07 | 0.016 | 2.23 | 1.07-4.62 | 0.032 |
| Depression v. schizophrenia | 0.46 | 0.18-1.14 | 0.093 | 0.41 | 0.16-1.04 | 0.060 |
| Perceived risk to others v. none | 1.91 | 1.11-3.26 | 0.018 | 2.13 | 1.22-3.70 | 0.007 |
| Criminal justice referral v. other | 7.24 | 3.75-13.98 | <0.001 | 7.03 | 3.62-13.65 | <0.001 |
| Help-seeker | ||||||
| Self v. other | 0.35 | 0.19-0.67 | 0.001 | 0.35 | 0.18-0.66 | 0.001 |
| South-east London v. Nottingham | 0.91 | 0.50-1.66 | 0.764 | 0.92 | 0.50-1.67 | 0.762 |
DISCUSSION
This study moves beyond previous research in at least two important respects. First, it is the largest study to compare modes of contact with mental health services in a sample of patients with a first episode of psychosis, with the consequent advantage of increased statistical power to detect differences and to control for confounding. Second, it is the first such study conducted in two different settings simultaneously using the same methodology.
Ethnicity and compulsory admission at first contact
In contrast to the findings of Cole et al (Reference Cole, Leavey and King1995) and Burnett et al (Reference Burnett, Mallett and Bhugra1999), we found important differences in proportions of compulsory admissions between ethnic groups in both south-east London and Nottingham at first presentation to services. The most striking of these relate to African–Caribbean men. When a range of factors that might explain these high proportions are adjusted for, including criminal justice referral, the odds of compulsory admission for African–Caribbean men remain over 3 times greater than for White British men. Other studies have reported an excess of compulsory admissions among African–Caribbean men. Bebbington et al (Reference Bebbington, Feeney and Flannigan1994), for example, reported compulsory admissions for African–Caribbean men to be respectively 13 and 8 times greater than for White men in two London boroughs; for African–Caribbean women the proportions were 3 and 5 times greater than for White women. Most previous studies, however, have included both first and subsequent admissions, and the studies by Cole et al (Reference Cole, Leavey and King1995) and Burnett et al (Reference Burnett, Mallett and Bhugra1999) did not report proportions of compulsory admission in different ethnic groups by age and gender.
The proportion of Black African patients compulsorily admitted in south-east London was similar to that of African–Caribbean patients; there was, however, no variation by age or gender. When other factors were controlled for, the odds of compulsory admission for Black African patients were over 4 times greater than those for White British patients. Only a small number of studies have reported levels of compulsory admission among specifically Black African patients. These have also tended to find high levels of compulsory admissions among this group. Davies et al (Reference Davies, Thornicroft and Leese1996), for example, in a study of a representative sample of patients with a psychotic mental illness in contact with services during a 1-year period, found that Black African patients were almost 3 times more likely to be compulsorily admitted than White patients.
Taken together, these findings point to there being an increased risk of compulsory admission for African–Caribbean and Black African patients with a psychotic mental illness at first contact with mental health services, contrary to the conclusions drawn by Cole et al (Reference Cole, Leavey and King1995) and Burnett et al (Reference Burnett, Mallett and Bhugra1999).
Explaining the differences
Clinical presentation
One of the earliest explanations put forward to account for the high proportion of compulsory admissions among African–Caribbean patients was that, for some reason, they presented as more disturbed than White patients (Reference RwegelleraRwegellera, 1980). Defining severity of disturbance at presentation is far from straightforward and previous researchers have used different indicators, including challenging behaviour, violence and poor insight. The evidence has been mixed (e.g. Reference Owens, Harrison and BootOwens et al, 1991; Reference Pipe, Bhat and MatthewsPipe et al, 1991). We collected data relating to a number of possible indicators of disturbance at presentation, including diagnosis, violence and perceived threat; a diagnosis of manic psychosis and both actual and perceived risk of violence were associated with compulsory admission. However, although diagnosis and perceived risk were independently associated with compulsory admission after adjustment for other factors, neither accounted for the excess of compulsory admissions among either African–Caribbean men or Black African patients.
Social isolation
A number of previous studies have found compulsory admission to be associated with socio-demographic variables such as unemployment and living alone (Reference Szmukler, Bird and ButtonSzmukler et al, 1981). Both Cole et al (Reference Cole, Leavey and King1995) and Burnett et al (Reference Burnett, Mallett and Bhugra1999) found such variables to be particularly important in predicting aversive pathways to care and compulsory admission at first contact. One interpretation of these data is that such variables are proxies for social isolation, and that the absence of significant others to facilitate help-seeking increases the risk of compulsory admission. In relation to this, it is also noteworthy that we found absence of family involvement in seeking help was associated with compulsory admission. In this study, African–Caribbean patients in both centres and Black African patients in south-east London were more likely to live alone and be unemployed than White British patients. Both of these variables, moreover, were associated with compulsory admission. However, although being unemployed was independently associated with compulsory admission, this did not account for the ethnic variations in proportions of compulsory admission in either centre: that is, although this study confirms the association between compulsory admission and variables such as living alone and unemployment, these at best account for only a small proportion of the variance between ethnic groups. Further, there was no difference between African–Caribbean and White patients in either study centre in levels of family involvement in the pathway to care, although White patients were more likely to seek help themselves.
The pathway to care
Intuitively, the route by which a patient is referred to services will influence the nature of the contact. For example, criminal justice agency involvement or referral is already suggestive of resistance to intervention and, from the point of view of an assessing psychiatrist, referral through the police suggests a possible need for restraint and containment. It is not surprising, then, that criminal justice agency involvement and referral should be very strongly – and independently – correlated with compulsory admission. Conversely, successful general practitioner referral signifies a willingness on the part of the patient to accept intervention by mental health services. The expected influence of source of referral is found, to a degree, in our study. In particular, criminal justice agency referrals were more common among the African–Caribbean and Black African patients and general practitioner referrals were less common. However, again these differences in the source of referral do not fully account for ethnic variations in compulsory admissions. The question thus remains: what processes are operating prior to – or at the point of – first contact with mental health services that increase the risk of compulsory admission for African–Caribbean patients, particularly men, and Black African patients? Extending the analysis to consider the pathway to first contact with mental health services may offer some further clues (see Part 2: Reference Morgan, Mallet and HutchinsonMorgan et al, 2005, this issue).
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ African–Caribbean and Black African patients are more likely to be compulsorily admitted at first contact with services, independent of service setting.
-
▪ African–Caribbean men are the most likely to be compulsorily admitted at first contact with services.
-
▪ Diagnosis, socio-demographic characteristics and how patients come into contact with services do not explain the high levels of compulsory admission among African–Caribbean and Black African patients.
LIMITATIONS
-
▪ For a proportion of patients the only available data were drawn from case notes. Although the information obtained was factual and likely to be routinely recorded, errors might have arisen through inaccuracies and incomplete information in these notes.
-
▪ Data relating to clinical presentation were limited and did not include direct measures of clinical severity or insight.
-
▪ The number of African–Caribbean patients in the Nottingham sample was small.
Acknowledgements
We are grateful to mental health services and patients in Bristol, Nottingham and south-east London for their cooperation and support, and to the. UK Medical Research Council and the Stanley Medical Research Institute for. funding. We are also grateful to Morven Leese for statistical advice.
Members of the ÆSOP Study Group are as follows. Bristol: G. Harrison, F. Muga and J. Holloway. Cambridge: A. Fung, J. Mietunen, M. Ashby and H. Hayhurst. London: J. Leff, R. Murray, T. Craig, R. Mallett, P. Fearon, C. Morgan, K. Morgan, P. Dazzan, J. MacCabe, C. Samele, M. Sharpley, S. Vearnals, G. Hutchinson, R. Burnett, J. Boydell, K. Orr, J. Salvo, K. Greenwood, M. Lambri, S. Auer, P. Rohebak and L. McIntosh. Nottingham: P. Jones, G. Doody, J. Tarrant, S. Window, P. Williams, T. Lloyd, H. Bagalkote, B. Dow, D. Boot, A. Farrant, S. Jones, J. Simpson, R. Moanette, S. Suranim, M. Ruddell, J. Brewin and I. Medley.











eLetters
No eLetters have been published for this article.