Major depressive disorder among inpatients carries about a 20-fold risk of completed suicide (Reference Osby, Brandt and CorreiaOsby et al, 2001) and about half of people who complete suicide have attempted suicide at least once before (Reference Isometsa, Henriksson and AroIsometsä et al, 1994). The lifetime risk of a non-fatal suicide attempt among patients with major depressive disorder is estimated at about 40% (Reference Malone, Haas and SweeneyMalone et al, 1995), and may be an important proxy outcome when investigating risk factors for suicide. In the few published prospective studies, risk factors for suicide attempt (Reference Paykel and DieneltPaykel & Dienelt, 1971; Reference Duggan, Sham and LeeDuggan et al, 1991; Reference Bronisch and HechtBronisch & Hecht, 1992; Reference Oquendo, Kamali and EllisOquendo et al, 2002) or completed suicide (Reference Fawcett, Scheftner and FoggFawcett et al, 1990; Reference Nordström, Åsberg and Åberg-WistedtNordström et al 1995; Reference Hansen, Wang and StageHansen et al, 2003) have included a history of suicide attempt by the patient or suicide in the family (Reference Paykel and DieneltPaykel & Dienelt, 1971; Reference Fawcett, Scheftner and FoggFawcett et al, 1990; Reference Bronisch and HechtBronisch & Hecht, 1992; Reference Nordström, Åsberg and Åberg-WistedtNordström et al, 1995), high severity of depression (Reference Oquendo, Kamali and EllisOquendo et al, 2002; Reference Hansen, Wang and StageHansen et al, 2003), comorbid personality disorder (Reference Paykel and DieneltPaykel & Dienelt, 1971; Reference Hansen, Wang and StageHansen et al, 2003), comorbid alcohol dependence or misuse (Reference Fawcett, Scheftner and FoggFawcett et al, 1990; Reference Duggan, Sham and LeeDuggan et al, 1991; Reference Bronisch and HechtBronisch & Hecht, 1992), comorbid chronic physical illness (Reference Duggan, Sham and LeeDuggan et al, 1991), younger age (Reference Paykel and DieneltPaykel & Dienelt, 1971), hopelessness and suicidal ideation (Reference Fawcett, Scheftner and FoggFawcett et al, 1990). However, most of these prospective studies have been conducted exclusively within in-patient settings (Reference Duggan, Sham and LeeDuggan et al, 1991; Reference Bronisch and HechtBronisch & Hecht, 1992; Reference Nordström, Åsberg and Åberg-WistedtNordström et al, 1995; Reference Oquendo, Kamali and EllisOquendo et al, 2002; Reference Hansen, Wang and StageHansen et al, 2003), have had relatively small (n<100) sample sizes (Reference Duggan, Sham and LeeDuggan et al, 1991; Reference Bronisch and HechtBronisch & Hecht, 1992) or have investigated populations with diagnostically mixed affective disorders (Reference Fawcett, Scheftner and FoggFawcett et al, 1990; Reference Nordström, Åsberg and Åberg-WistedtNordström et al, 1995). Therefore the generalisability of their findings to other settings or populations, or their power to detect risk factors, may have been limited. Previously we have reported factors cross-sectionally associated with suicidal ideation and attempts among psychiatric patients with major depressive disorder (Reference Sokero, Melartin and RytsäläSokero et al, 2003). In the present prospective study we hypothesised that presence and severity of depression, comorbid substance use, cluster B personality and anxiety disorders, and social support and history of previous suicide attempts would each independently predict suicide attempts.
METHOD
Setting
The background and methodology of the Vantaa Depression Study have been described in detail elsewhere (Melartin et al, Reference Melartin, Rytsälä and Leskelä2002, Reference Melartin, Rytsälä and Leskelä2004). In brief, the Vantaa Depression Study is a collaborative depression research project between the Department of Mental Health and Alcohol Research of the National Public Health Institute, Helsinki, Finland, and the Department of Psychiatry of the Peijas Medical Care District, Vantaa, Finland. Vantaa is the fourth largest city in Finland, with a population of 169 000 in 1997, and provides psychiatric services to all its citizens free of charge. The Vantaa Depression Study was accepted by the ethical committee of the Peijas Medical Care District in December 1996.
Screening, diagnostic evaluation and baseline measurements
In the first phase, all patients (n=806) at the Department of Psychiatry of the Peijas Medical Care District were screened for a possible new episode of DSM–IV (American Psychiatric Association, 1994) major depressive disorder between 1 February 1997 and 31 May 1998 (Reference Melartin, Rytsälä and LeskeläMelartin et al, 2002). Patients with a positive screen were fully informed about the study project and their participation was requested. Of the 703 eligible patients, 542 (77%) agreed and gave written informed consent.
In the second phase a researcher using SCAN 2.0 (Reference Wing, Babor and BrughaWing et al, 1990) interviewed the 542 consenting patients, 269 of whom were diagnosed with DSM–IV major depressive disorder and were included in the study; the diagnostic reliability was excellent (k=0.86, 95% CI 0.58–1.0) (Reference Melartin, Rytsälä and LeskeläMelartin et al, 2002). The Structured Clinical Interview for DSM–III–R personality disorders (SCID–II; Reference Spitzer, Williams and GibbonSpitzer et al, 1987) was used to assess diagnoses on Axis II. The cohort baseline measurements included the 17-item Hamilton Rating Scale for Depression (HRSD; Reference HamiltonHamilton, 1960), 21-item Beck Depression Inventory (Reference Beck, Ward and MendelsonBeck et al, 1961), Beck Anxiety Inventory (Reference Beck, Brown and EpsteinBeck et al, 1988), Beck Hopelessness Scale (Reference Beck, Weissman and LesterBeck et al, 1974), Scale for Suicidal Ideation (Reference Beck and KovacsBeck & Kovacs, 1979), Social and Occupational Functioning Assessment Scale of DSM–IV (American Psychiatric Association, 1994: pp. 760–761), Interview for Recent Life Events (Reference PaykelPaykel, 1983), Interview Measure of Social Relationships (Reference Brugha, Sturt and MaccarthyBrugha et al, 1987) and the Perceived Social Support Scale – Revised (Reference Blumenthal, Burg and BraefootBlumenthal et al, 1987).
Follow-up
Of the 269 individuals with current major depressive disorder initially included in the study, 198 were still alive at the end of the study period, their depression had remained unipolar and they could be followed up (Reference Melartin, Rytsälä and LeskeläMelartin et al, 2004). At baseline, the majority (154/198, 78%) were receiving antidepressants at normal adult doses. The patients whose diagnosis switched to bipolar disorder during the follow-up (13/269, 5%) were analysed separately. The outcome of major depressive disorder and the comorbid disorders was investigated at 6 and 18 months by repeated SCAN 2.0 and SCID–II interviews, observer- and self-report scales and medical and psychiatric records. A detailed life chart was created, with time after baseline divided into three classes: state of full remission (none of the nine criteria symptoms for major depressive episode), partial remission (one to four symptoms); and major depressive episode (five or more symptoms). We used two different definitions for duration of the index episode: the uninterrupted duration of the episode in the state of major depression (time with full criteria) and time to the first onset of state of full remission that lasted at least 2 consecutive months (time to full remission) (Reference Melartin, Rytsälä and LeskeläMelartin et al, 2004).
Occurrence of a suicide attempt before the baseline interview and during the follow-up was based on both the interview and psychiatric records. By definition, a suicide attempt had to involve at least some degree of intent to die; self-harm with no suicidal intention was not included. Patient-months were calculated based on the life chart. Information about the deaths among all the 269 patients during the follow-up was obtained from the official records of Statistics Finland.
For the validity of the results it is essential to verify that there were no more suicidal patients among those who did not complete the study than among those followed up. This did not seem to be the case. Patients who could not be followed up did not differ from the patients who were followed up, in terms of suicide attempts before the index episode (18% v. 14%), suicide attempt during the index episode (25% v. 23%) or suicidal ideation (38% v. 39%). However, they were somewhat younger, were more often living alone, had a higher score on the Eysenck Personality Inventory neuroticism scale (Reference Eysenck and EysenckEysenck & Eysenck, 1964) and more often had comorbid dysthymia (Reference Melartin, Rytsälä and LeskeläMelartin et al, 2004).
Statistical methods
Logistic regression models were created, classifying suicide attempt during the follow-up as the dependent variable. The statistical methods included non-parametric and parametric univariate analyses (the t-test, χ2-test, Fisher's exact test, analysis of variance (ANOVA), the Mann–Whitney test and the Kruskal–Wallis test) and logistic regression models; the Statistical Package for the Social Sciences software, version 11.0, was used.
RESULTS
During the 18-month follow-up, 16 (8%) patients reported at least one suicide attempt but in total there were 41 discrete suicide attempts. Four occurred during a period of full remission, 12 during partial remission and 25 during a major depressive episode. Thus, the risk of a suicide attempt was 4/1201 patient-months during full remission, 12/1441 patient-months (relative risk 2.50) during partial remission and 25/995 patient-months (relative risk 7.54) during a major depressive episode (χ2=24.3, d.f.=2, P<0.001). Patients who switched to bipolar disorder and patients who died were not included. Of all the 269 patients in the cohort, eight patients (3%) died during the 18 months after baseline, three (1%) of them by suicide.
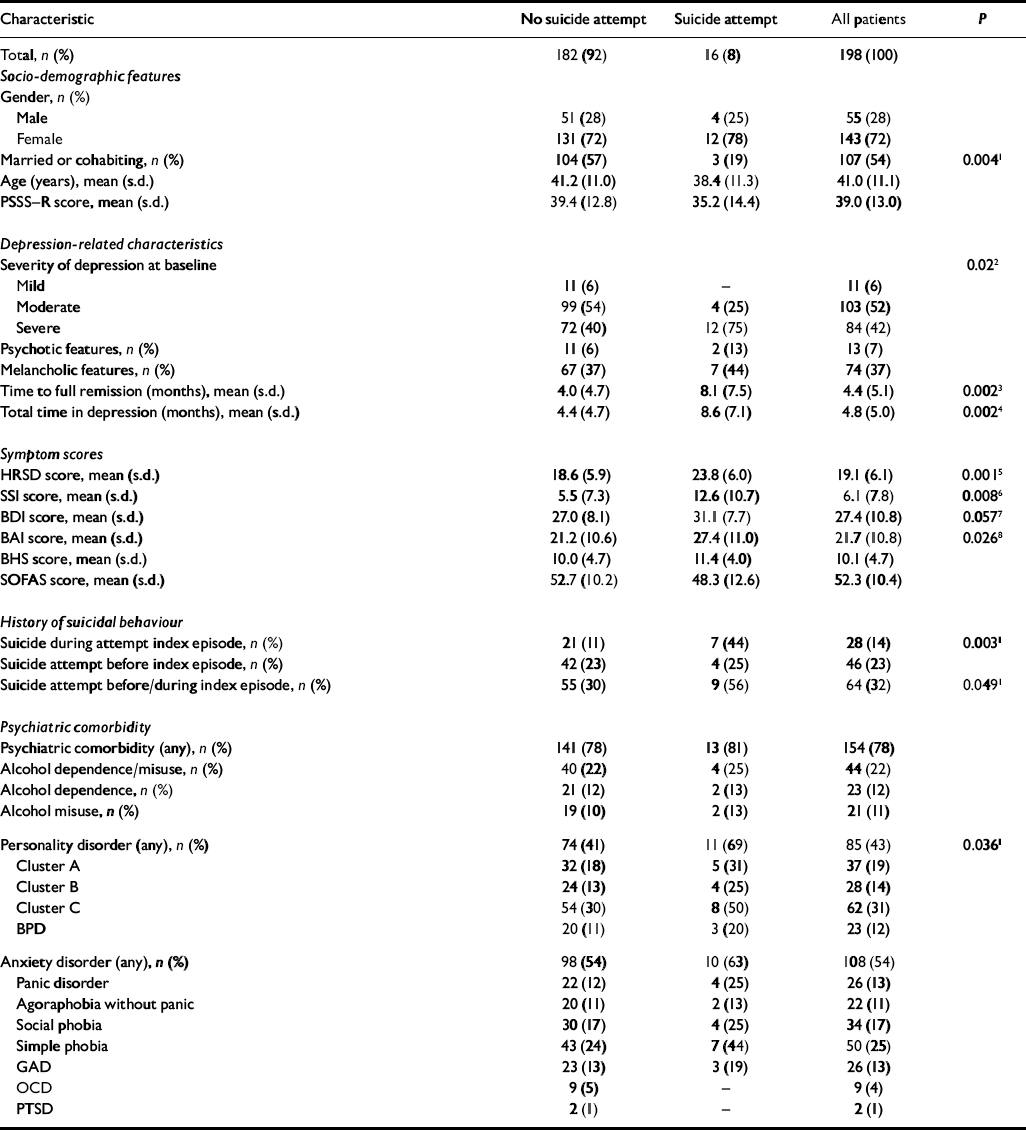
We found significant differences between those attempting suicide and those not attempting suicide (Table 1) in terms of: severity of index episode of depression; amount of suicidal ideation and anxiety; prevalence of personality disorder; prevalence of suicide attempts during the index episode; time to full remission and total time spent in a major depressive episode; and marital status (lack of partner). Patients with cluster B or borderline personality disorder had more attempts (Mann–Whitney test: Z=–2.146, P=0.032, and Z=–2.165, P=0.030, respectively).
Table 1 Differences in characteristics between those who did and did not attempt suicide out of the 198 patients with unipolar major depressive disorder during the 18-month prospective follow-up
| Characteristic | No suicide attempt | Suicide attempt | All patients | P |
|---|---|---|---|---|
| Total, n (%) | 182 (92) | 16 (8) | 198 (100) | |
| Socio-demographic features | ||||
| Gender, n (%) | ||||
| Male | 51 (28) | 4 (25) | 55 (28) | |
| Female | 131 (72) | 12 (78) | 143 (72) | |
| Married or cohabiting, n (%) | 104 (57) | 3 (19) | 107 (54) | 0.0041 |
| Age (years), mean (s.d.) | 41.2 (11.0) | 38.4 (11.3) | 41.0 (11.1) | |
| PSSS—R score, mean (s.d.) | 39.4 (12.8) | 35.2 (14.4) | 39.0 (13.0) | |
| Depression-related characteristics | ||||
| Severity of depression at baseline | 0.022 | |||
| Mild | 11 (6) | - | 11 (6) | |
| Moderate | 99 (54) | 4 (25) | 103 (52) | |
| Severe | 72 (40) | 12 (75) | 84 (42) | |
| Psychotic features, n (%) | 11 (6) | 2 (13) | 13 (7) | |
| Melancholic features, n (%) | 67 (37) | 7 (44) | 74 (37) | |
| Time to full remission (months), mean (s.d.) | 4.0 (4.7) | 8.1 (7.5) | 4.4 (5.1) | 0.0023 |
| Total time in depression (months), mean (s.d.) | 4.4 (4.7) | 8.6 (7.1) | 4.8 (5.0) | 0.0024 |
| Symptom scores | ||||
| HRSD score, mean (s.d.) | 18.6 (5.9) | 23.8 (6.0) | 19.1 (6.1) | 0.0015 |
| SSI score, mean (s.d.) | 5.5 (7.3) | 12.6 (10.7) | 6.1 (7.8) | 0.0086 |
| BDI score, mean (s.d.) | 27.0 (8.1) | 31.1 (7.7) | 27.4 (10.8) | 0.0577 |
| BAI score, mean (s.d.) | 21.2 (10.6) | 27.4 (11.0) | 21.7 (10.8) | 0.0268 |
| BHS score, mean (s.d.) | 10.0 (4.7) | 11.4 (4.0) | 10.1 (4.7) | |
| SOFAS score, mean (s.d.) | 52.7 (10.2) | 48.3 (12.6) | 52.3 (10.4) | |
| History of suicidal behaviour | ||||
| Suicide during attempt index episode, n (%) | 21 (11) | 7 (44) | 28 (14) | 0.0031 |
| Suicide attempt before index episode, n (%) | 42 (23) | 4 (25) | 46 (23) | |
| Suicide attempt before/during index episode, n (%) | 55 (30) | 9 (56) | 64 (32) | 0.0491 |
| Psychiatric comorbidity | ||||
| Psychiatric comorbidity (any), n (%) | 141 (78) | 13 (81) | 154 (78) | |
| Alcohol dependence/misuse, n (%) | 40 (22) | 4 (25) | 44 (22) | |
| Alcohol dependence, n (%) | 21 (12) | 2 (13) | 23 (12) | |
| Alcohol misuse, n (%) | 19 (10) | 2 (13) | 21 (11) | |
| Personality disorder (any), n (%) | 74 (41) | 11 (69) | 85 (43) | 0.0361 |
| Cluster A | 32 (18) | 5 (31) | 37 (19) | |
| Cluster B | 24 (13) | 4 (25) | 28 (14) | |
| Cluster C | 54 (30) | 8 (50) | 62 (31) | |
| BPD | 20 (11) | 3 (20) | 23 (12) | |
| Anxiety disorder (any), n (%) | 98 (54) | 10 (63) | 108 (54) | |
| Panic disorder | 22 (12) | 4 (25) | 26 (13) | |
| Agoraphobia without panic | 20 (11) | 2 (13) | 22 (11) | |
| Social phobia | 30 (17) | 4 (25) | 34 (17) | |
| Simple phobia | 43 (24) | 7 (44) | 50 (25) | |
| GAD | 23 (13) | 3 (19) | 26 (13) | |
| OCD | 9 (5) | - | 9 (4) | |
| PTSD | 2 (1) | - | 2 (1) |
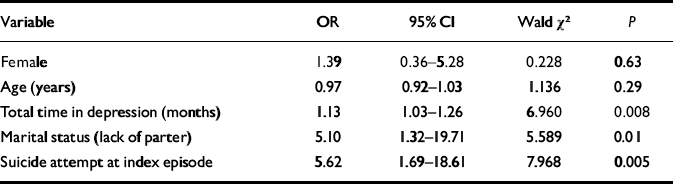
In the logistic regression model predicting suicide attempts during the follow-up (Table 2), the predetermined covariates comprised gender, age, marital status, HRSD score, alcohol dependence or misuse, Beck Anxiety Inventory score, personality disorder (any), cluster B personality disorder, suicide attempt during the index episode and time spent in major depressive episodes. After removing the non-significant variables, three factors were strongly associated with suicide attempt: months spent in major depressive episodes (OR=1.13), suicide attempt during the index episode (OR=5.62) and lack of partner (OR=5.10).
Table 2 Logistic regression model for suicide attempts during 18-month follow-up (n=198)
| Variable | OR | 95% Cl | Wald χ2 | P |
|---|---|---|---|---|
| Female | 1.39 | 0.36-5.28 | 0.228 | 0.63 |
| Age (years) | 0.97 | 0.92-1.03 | 1.136 | 0.29 |
| Total time in depression (months) | 1.13 | 1.03-1.26 | 6.960 | 0.008 |
| Marital status (lack of parter) | 5.10 | 1.32-19.71 | 5.589 | 0.01 |
| Suicide attempt at index episode | 5.62 | 1.69-18.61 | 7.968 | 0.005 |
Patients who switched to bipolar disorder (13/269, 5%) formed a particularly suicidal subgroup. They reported more suicidal ideation before the index episode (9 (69%) v. 97 (38%); Fisher's exact test, P=0.039) and had more suicide attempts before the index episode (8 (62%) v. 56(22%); Fisher's exact test, P=0.003) but this was nonsignificant during the follow-up (2 (22%) v. 16 (8%); Fisher's exact test, P=0.17).
DISCUSSION
Main findings
During the 18-month prospective followup, 8% of patients with major depressive disorder attempted suicide. The risk of an attempt was almost eightfold during a major depressive episode compared with a period of full remission. Although many factors from various domains were associated with this risk, it was effectively predicted by three independent factors: lack of a partner, history of previous suicide attempts and time spent in major depressive episodes.
To our knowledge, the present study is the first prospective investigation to employ a life chart to place the suicide attempts, allowing us to identify important disparities in risk between periods with different levels of depressive symptoms. We interpret these robust findings as evidence for the causal role of depression per se in the aetiology of suicide attempts. Given the high level of comorbidity with anxiety, substance use and personality disorders in the patient population (Reference Melartin, Rytsälä and LeskeläMelartin et al, 2002), all factors that are related independently to suicidal behaviour, the finding is far from self-evident.
Strengths, limitations and generalisability
The present study has some major methodological strengths. It involved a relatively large (n=269) cohort of both out- and inpatients with major depressive disorder, effectively representing all psychiatric patients with a new episode of major depressive disorder in a Finnish city. Based on an epidemiological survey, we have estimated (Reference Rytsala, Melartin and LeskelaRytsälä et al, 2001) that two-thirds of all individuals with major depressive disorder in the general population of the city of Vantaa seeking treatment from psychiatrists are treated in the Peijas Medical Care District. The patients were diagnosed carefully using structured interviews with excellent reliability (κ=0.86) for the diagnosis of major depressive disorder, plus information on all comorbid Axis I and II disorders at baseline and later interviews. The total rate of losses to the study was low, because 87% of participants could be interviewed at least once after baseline. However, owing to deaths, diagnostic switch to bipolar disorder and patients who left the study after 6 months, those included in the present report represent 74% of the original 269 patients. These patients do not differ in terms of baseline suicidal behaviour from those who could not be included. The study took place during the era of current antidepressants (1997–1999) in a modern community psychiatric setting; at baseline, 78% of the patients received antidepressants at adequate levels in the acute phase, in compliance with the American Psychiatric Association's Practice Guidelines. Methodological details are discussed more fully in earlier reports (Reference Melartin, Rytsälä and LeskeläMelartin et al, 2002; Reference Sokero, Melartin and RytsäläSokero et al, 2003; Reference Melartin, Rytsälä and LeskeläMelartin et al, 2004). The most important limitation of the present study is that, despite a large cohort of patients, the number of suicide attempts was moderate and the number of patients attempting was small during the followup. Although the main findings are statistically robust, some degree of type II error may have occurred and some risk of spurious findings also exists. Finally, the density of psychiatrists per population in Finland is among the highest in Europe, and psychiatric settings treat about half of all individuals seeking treatment for depression from healthcare providers (Reference Hämäläinen, Isometsä and LaukkalaHämäläinen et al, 2004). Nevertheless, the characteristics of patients in the Vantaa Depression Study do not differ in terms of comorbidity and symptom severity from the few other studies that have reported them comprehensively (Reference Zimmerman, McDermut and MattiaZimmerman et al, 2000; Reference Tedlow, Smith and NeaultTedlow et al, 2002), supporting the generalisation of our findings to other settings.
Predictors of suicide attempt
Preceding the follow-up phase, 15% of the cohort had attempted suicide during the index episode and 24% before that (Reference Sokero, Melartin and RytsäläSokero et al, 2003). The prevalence of those attempting suicide during the follow-up (8%) in our study is similar to another report (Reference Bronisch and HechtBronisch & Hecht, 1992) but lower than in two others with populations apparently at higher risk (Reference Duggan, Sham and LeeDuggan et al, 1991; Reference Oquendo, Kamali and EllisOquendo et al, 2002). Our univariate analysis findings are also in line with risk factor findings in our own baseline analysis (Reference Sokero, Melartin and RytsäläSokero et al, 2003) and in the other studies. Marital status (Reference Bronisch and HechtBronisch & Hecht, 1992), major depressive disorder (Reference Bronisch and HechtBronisch & Hecht, 1992; Reference Oquendo, Kamali and EllisOquendo et al, 2002; Reference Hansen, Wang and StageHansen et al, 2003; Reference Sokero, Melartin and RytsäläSokero et al, 2003), anxiety (Reference Fawcett, Scheftner and FoggFawcett et al, 1990; Reference Sokero, Melartin and RytsäläSokero et al, 2003), personality disorder (Reference Paykel and DieneltPaykel & Dienelt, 1971; Reference Hansen, Wang and StageHansen et al, 2003; Reference Sokero, Melartin and RytsäläSokero et al, 2003) and suicidal behaviour (Reference Paykel and DieneltPaykel & Dienelt, 1971; Reference Fawcett, Scheftner and FoggFawcett et al, 1990; Reference Bronisch and HechtBronisch & Hecht, 1992; Reference Nordström, Åsberg and Åberg-WistedtNordström et al, 1995; Reference Oquendo, Kamali and EllisOquendo et al, 2002; Reference Sokero, Melartin and RytsäläSokero et al, 2003) were all associated with suicide attempts. In contrast to our cross-sectional findings (Reference Sokero, Melartin and RytsäläSokero et al, 2003), substance use disorder, age, chronic physical illness and hopelessness did not, independently, predict suicide attempts. Finally, the small group of patients who switched to bipolar disorder during the follow-up appeared to be a particularly ‘suicidal’ subgroup. However, the number of cases was too small to evaluate risk factors for their suicidal behaviour.
Clinical implications
The clinical implications of our findings are clear. Suicide attempts among patients with major depressive disorder are strongly associated temporarily with the presence of depressive symptoms and robustly predicted by lack of a partner, previous suicide attempts and time spent depressed. Reducing the duration of a depressed state is likely to be an effective preventive measure for suicide attempts.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Psychiatric in- and out-patients with major depressive disorder have a high level of comorbidity with anxiety, substance use and personality disorder, all of which independently implicate elevated risk for suicide attempts. Nevertheless, risk for suicide attempt is about eightfold during a major depressive episode compared with full remission.
-
▪ Risk for suicide attempts during follow-up is predicted independently and strongly by the time spent in major depressive episodes, suicide attempt during the index episode and lack of partner.
-
▪ Reducing the time spent depressed is a credible preventive measure.
LIMITATIONS
-
▪ Total number of suicide attempts in the study was 41, made by only 16 (8%) patients followed up. However, despite vulnerability to type II error, the main findings were highly significant statistically.
-
▪ Owing to deaths, diagnostic switch to bipolar disorder and dropping out, the patients interviewed represent 74% of the population at the baseline. Those who dropped out did not differ from those who remained, in terms of suicidal behaviour evaluated at baseline.
-
▪ The generalisability of the findings from psychiatric settings in Finland to psychiatric settings in other countries needs to be confirmed.







eLetters
No eLetters have been published for this article.