Treatment of psychotic disorders should be a combination of psychopharmacological therapy, psychological treatment and rehabilitation efforts. Antipsychotic drugs help in reducing the acute symptoms of schizophrenia, whereas psychological interventions and rehabilitation efforts can help patients and their relatives cope with the consequences of having schizophrenia (Reference Birchwood, Spencer, May and SartoriusBirchwood & Spencer, 1999). An increasing number of studies have shown that cognitive–behavioural therapy combined with standard psychiatric care, including antipsychotic medication, results in significant clinical benefits over standard care alone (Reference Pilling, Bebbington and KuipersPilling et al, 2002). However, no study has been conducted with in-patients experiencing treatment-resistant psychotic symptoms. Our study examines the effects of cognitive–behavioural therapy combined with standard care, compared with supportive counselling and standard care, in a population receiving long-term in-patient care, whose illness had proved resistant to other treatments including adequate atypical antipsychotic medication. We predicted that cognitive–behavioural therapy would be more effective than supportive counselling in reducing auditory hallucinations and delusional beliefs.
METHOD
Study design
The study was a randomised controlled trial of cognitive–behavioural therapy compared with supportive counselling in an in-patient population with chronic schizophrenia. Patients were randomly allocated to one of the two treatment conditions. For the selection procedure, the project coordinator had two baskets: a ‘treatment’ basket which contained sealed envelopes with lots for each of the two treatment conditions and a ‘used’ basket where the drawn lots could be placed. To ensure the anonymity of the participants, each individual was given a code, and the coordinator used a form to communicate the results of the random assignment to the local therapist. The study took place in various mental health hospitals across The Netherlands and in one in Belgium. The study was supervised by Professor Tarrier of the University of Manchester in the UK, and it originated from his previous work in this area (Tarrier et al, Reference Tarrier, Beckett and Harwood1993, Reference Tarrier, Yusupoff and Kinney1998, Reference Tarrier, Wittkowski and Kinney1999, Reference Tarrier, Kinney and McCarthy2000). Psychologists specialising in cognitive–behavioural therapy who were working with patients with schizophrenia were invited to participate in the study as therapists. To control for non-specific therapy and therapist effects, cognitive–behavioural therapy was compared with supportive counselling plus psycho-education. Both types of intervention were offered by all therapists. Each centre had a local assessor masked to the participants’ identity to conduct the assessment. All participants experienced psychotic symptoms refractory to atypical antipsychotic medication. The same selection criteria and assessment instruments were used in all participating centres. Oral and written information about the study was given to the patients and written informed consent was obtained. After the baseline assessment patients were randomly allocated to receive 22 weeks of their cognitive–behavioural therapy or supportive counselling, comprising 16 h of therapy: sessions 1–12 took place once a week, sessions 13–15 every 2 weeks and session 16 after 4 weeks. Assessment was repeated a week after the final therapy session and again at follow-up after 6 months (from the last session).
Sample
The Netherlands has a population of 16 million people, about 100 000 of whom have schizophrenia. Hospital admission is needed for more than 11 000 patients each year (Schizofrenie Platform, 2000). Depending on the course of the disease, patients can be discharged to receive home-based care, day care or assertive community treatment. Patients can also choose a sheltered living facility or, if severely affected, live in long-stay housing in the hospital grounds. According to the DSM–IV (American Psychiatric Association, 1994), positive symptoms appear to reflect an excess or distortion of normal functions and can be divided into two dimensions: the psychotic dimension, including delusions and hallucinations, and the disorganisation dimension, including disorganised speech and behaviour (American Psychiatric Association, 1994: pp. 274–275). In this study we wanted to focus on the psychotic dimension, and the aim of the study was to test the efficacy of cognitive–behavioural therapy for an in-patient population. The sample size of 72 patients (two groups of 36) was determined with an a priori sample size calculation (α=0.05; power 0.80; effect size 0.60). Participants were recruited from the in-patient population of the participating institutes if they met the following inclusion criteria:
-
(a) age 18–70 years;
-
(b) diagnosis of schizophrenia according to DSM–IV criteria;
-
(c) residual delusions or auditory hallucinations experienced for at least 3 months;
-
(d) a stable medication regimen (last medication change more than 6 weeks prior to recruitment).
A confirmed resistance to psychopharmacological treatment was established according to the following conventional criteria: symptoms unresponsive to at least two different antipsychotic compounds including an atypical antipsychotic, taken for enough time and in an acceptable dosage, as advised in the prescription guidelines (Reference Kane, Honigfeld and SingerKane et al, 1988). To exclude patients experiencing predominantly symptoms from the disorganisation dimension, the following exclusion criteria were also applied:
-
(a) conceptual disorganisation;
-
(b) stereotypic thinking;
-
(c) disorientation, measured by the Positive and Negative Syndrome Scale (PANSS; Reference Kay, Fiszbein and OplerKay et al, 1987), items P2≥4, N7≥3 and G10≥2;
-
(d) drug or alcohol addiction as a primary diagnosis (patients using drugs or alcohol below the level of this criterion were included);
-
(e) mental retardation (premorbid IQ≥80);
-
(f) organic conditions;
-
(g) cognitive–behavioural therapy given for persistent psychotic symptoms in the past.
The authors wanted to ensure that any changes in symptoms were due to the psychological intervention provided and not to a change in medication, therefore anti-psychotic medication remained unchanged during the experimental period. If a considerable change in antipsychotic medication was necessary, the patient was withdrawn from the study.
Interventions
Cognitive–behavioural therapy
A comprehensive treatment manual was written (by the first three authors) and the participating therapists were trained in using this protocol. The therapy begins with an engagement phase which stresses the development of a collaborative relationship between therapist and patient; their mutual goal becomes reducing the distress that accompanies delusional beliefs, instead of each trying to convince the other that the belief is or is not true. This approach reduces reactance and facilitates the challenging of the beliefs in the next phase of therapy (Reference Kingdon and TurkingtonKingdon & Turkington, 1994). In the second phase a shared case formulation is drawn up, based on a detailed assessment of the problems experienced by the patient. The aim is to establish a link between thoughts and emotions and between thoughts and behaviour. Specific techniques are then used aiming at a reduction of the symptoms and a reduction of the distress that accompanies the symptoms. With auditory hallucinations the aim is to change the beliefs about the origin, power and dangerousness of voices (Reference Chadwick and BirchwoodChadwick & Birchwood, 1994). In delusions, the focus is on challenging the dysfunctional beliefs and learning to make more balanced conclusions. In the last phase of therapy, treatment gains are consolidated and attention is given to relapse prevention strategies. Some adaptations have to be taken into account when working with patients with chronic schizophrenia: to cope with the attention and memory problems the pace of the session is slower, the therapist asks frequently for feedback on what was just discussed and frequently summarises relevant information. Many patients cannot concentrate for an hour, so a break of 5–10 min is introduced halfway through the session, and relevant information is written down for the patient to read between sessions.
Supportive counselling
The supportive counselling protocol was a conventional method previously used in other studies (Reference Tarrier, Yusupoff and KinneyTarrier et al, 1998; Reference Lewis, Tarrier and HaddockLewis et al, 2002). The therapist shows non-critical acceptance, warmth, genuineness and empathy. The following basic skills are applied: listening (to hear both the content and the feelings behind the patient's message), reflecting, empathising and summarising. Patients are asked about a subject they would like to talk about during the session. However, in our study patients had spent long periods in hospital and often found it hard to find a subject they wanted to discuss. If this was the case the therapist could ask questions about current living circumstances, illness and current problems, daily routine, social contacts, family, and personal history. In addition, the therapist offered the patients psycho-education about schizophrenia; however, most patients declined this offer on the basis that they had received it in the past.
Outcome measures
To quantify the primary hypothesis the following main outcome measures of positive symptoms were selected: the Positive and Negative Syndrome Scale and the Psychotic Symptoms Rating Scale (PSYRATS; Reference Haddock, McCarron and TarrierHaddock et al, 1999). The PANSS has three sub-scales, measuring positive symptoms, negative symptoms and general psychopathology. The PSYRATS consists of two scales: the auditory hallucination scale and the delusion scale. The 11 items of the auditory hallucination scale assess different dimensions of auditory hallucinations over the past week and can be clustered in three factors: a physical characteristics factor (frequency, duration, location and loudness), an emotional characteristics factor (amount and degree of negative content and of distress) and a cognitive interpretation factor (disruption, belief about origin and attribution of control). The delusion scale consists of six items which can be clustered in two factors: a cognitive interpretation factor (amount and duration of preoccupation, conviction and disruption) and an emotional characteristics factor (amount and intensity of distress). The psychometric properties of the PSYRATS have been researched, and both the auditory hallucination scale and the delusion scale have excellent interrater reliability and good validity (Reference Haddock, McCarron and TarrierHaddock et al, 1999). Relapse was defined as an increase of more than 10 in the score on the positive symptom sub-scale of the PANSS with the deterioration in symptoms lasting longer than 3 days.
Treatment fidelity
To ensure treatment fidelity, all therapists received training in the standardised protocols that were used in the study. In the first year of the trial therapists met once a month for supervision; later, the meetings were held once every 6 weeks. M.v.d.G. was the main supervisor, and N.T. came to The Netherlands every 6 months for an extra supervision meeting. Both therapeutic conditions were recorded to control adherence to protocol. Two audiotapes for each condition for each therapist were selected at random; these tapes were scored independently by the first author and by another therapist who was not involved in the research, using an adapted version of the Cognitive Therapy Scale for Psychosis (Reference Haddock, Devane and BradshawHaddock et al, 2001).
Statistical analysis
Results were analysed using the Statistical Package for the Social Sciences (SPSS) version 10 (SPSS, 1999). Differences between the two conditions with regard to the main hypothesis were calculated using analysis of covariance (ANCOVA), baseline assessment results were used as covariates, and the condition was used as fixed factor. Levene's test of equality was used to control sphericity (equality of variances of the differences between the two treatment conditions). A violation of sphericity means a loss of power and uncertain test results (Reference FieldField, 2000). Analysis was by intention to treat. Post-therapy and follow-up missing data were calculated using the missing value analysis option of SPSS, which estimates missing values using multiple linear regression (Reference HillHill, 1997). Effect sizes were calculated using Cohen's formula (Reference CohenCohen, 1988). Numbers needed to treat were calculated regarding the variables used to represent the primary hypothesis. Pearson's correlation was used to analyse the results of the scoring of the tapes done to ensure treatment fidelity.
RESULTS
Participants
Recruitment lasted 3 years. The flow of participants during the stages of the study is illustrated in Fig. 1. In total 66 patients were assessed for eligibility. Two patients declined to participate and two did not meet the inclusion criteria because they scored too highly on the disorganisation dimension. A total of 62 patients were randomly allocated to either cognitive–behavioural therapy (n=36) or supportive counselling (n=26). There is no explanation other than chance to account for the difference in numbers between the two treatment groups. A total of 50 patients received the complete allocated intervention. During the study only three patients relapsed, two in the cognitive–behavioural therapy group and one in the supportive counselling group. Post-treatment assessment was possible with 50 participants and follow-up was completed by 42 patients. One therapist withdrew from the study because he changed employer; this led to loss of the data for two patients. One of the assessors involved in the research lost the assessment data of two other patients. As the complete data-sets for these four patients were lost, no baseline data were available for these individuals, who were thus excluded from the intention-to-treat analyses. Owing to these losses, 58 participants were included in the analysis. According to the CONSORT statement, calculating the statistical power after the study has been completed is not useful; in such cases the power is better expressed by confidence intervals (Reference AltmanAltman, 1998).
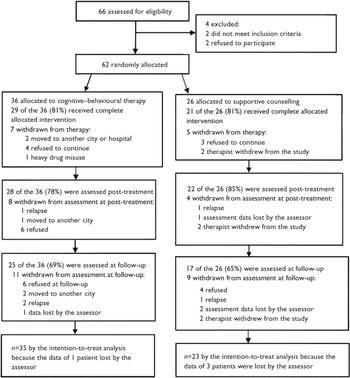
Fig. 1 Flow of the participants through the study.
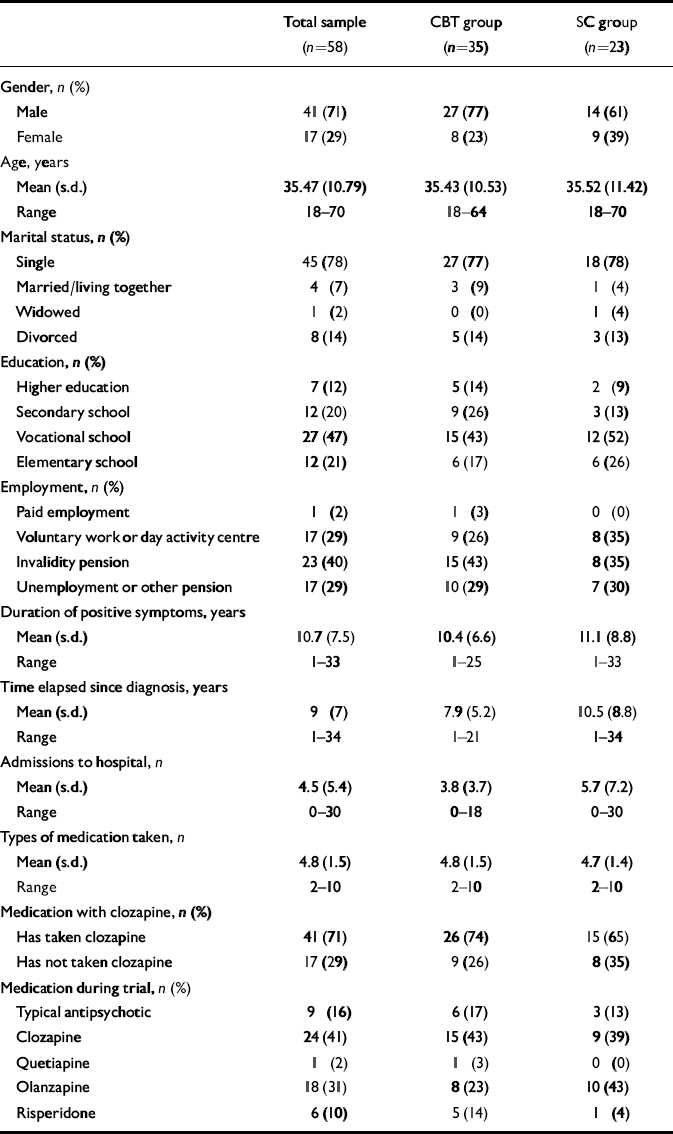
The baseline demographic characteristics of the participants are summarised in Table 1. The participants were predominately adult men, the large majority were single and only one patient was in paid employment. On average patients had been experiencing psychotic symptoms for the previous 11 years and had been admitted to hospital five times in the past 9 years. Depending on the type of variable, independent t-tests or chi-squared tests were carried out to control for differences in demographical variables between the two conditions. No significant difference was found between the two groups. With regard to the baseline assessment, the two randomised groups largely overlapped. Independent t-tests showed that there was a significant difference between the two groups regarding factor 2 of the auditory hallucination scale, ‘emotional characteristics’ (two-tailed P=0.044). The supportive counselling group reported more emotional distress related to the auditory hallucinations.
Table 1 Demographic and clinical characteristics of the sample
| Total sample (n=58) | CBT group (n=35) | SC group (n=23) | |
|---|---|---|---|
| Gender, n (%) | |||
| Male | 41 (71) | 27 (77) | 14 (61) |
| Female | 17 (29) | 8 (23) | 9 (39) |
| Age, years | |||
| Mean (s.d.) | 35.47 (10.79) | 35.43 (10.53) | 35.52 (11.42) |
| Range | 18-70 | 18-64 | 18-70 |
| Marital status, n (%) | |||
| Single | 45 (78) | 27 (77) | 18 (78) |
| Married/living together | 4 (7) | 3 (9) | 1 (4) |
| Widowed | 1 (2) | 0 (0) | 1 (4) |
| Divorced | 8 (14) | 5 (14) | 3 (13) |
| Education, n (%) | |||
| Higher education | 7 (12) | 5 (14) | 2 (9) |
| Secondary school | 12 (20) | 9 (26) | 3 (13) |
| Vocational school | 27 (47) | 15 (43) | 12 (52) |
| Elementary school | 12 (21) | 6 (17) | 6 (26) |
| Employment, n (%) | |||
| Paid employment | 1 (2) | 1 (3) | 0 (0) |
| Voluntary work or day activity centre | 17 (29) | 9 (26) | 8 (35) |
| Invalidity pension | 23 (40) | 15 (43) | 8 (35) |
| Unemployment or other pension | 17 (29) | 10 (29) | 7 (30) |
| Duration of positive symptoms, years | |||
| Mean (s.d.) | 10.7 (7.5) | 10.4 (6.6) | 11.1 (8.8) |
| Range | 1-33 | 1-25 | 1-33 |
| Time elapsed since diagnosis, years | |||
| Mean (s.d.) | 9 (7) | 7.9 (5.2) | 10.5 (8.8) |
| Range | 1-34 | 1-21 | 1-34 |
| Admissions to hospital, n | |||
| Mean (s.d.) | 4.5 (5.4) | 3.8 (3.7) | 5.7 (7.2) |
| Range | 0-30 | 0-18 | 0-30 |
| Types of medication taken, n | |||
| Mean (s.d.) | 4.8 (1.5) | 4.8 (1.5) | 4.7 (1.4) |
| Range | 2-10 | 2-10 | 2-10 |
| Medication with clozapine, n (%) | |||
| Has taken clozapine | 41 (71) | 26 (74) | 15 (65) |
| Has not taken clozapine | 17 (29) | 9 (26) | 8 (35) |
| Medication during trial, n (%) | |||
| Typical antipsychotic | 9 (16) | 6 (17) | 3 (13) |
| Clozapine | 24 (41) | 15 (43) | 9 (39) |
| Quetiapine | 1 (2) | 1 (3) | 0 (0) |
| Olanzapine | 18 (31) | 8 (23) | 10 (43) |
| Risperidone | 6 (10) | 5 (14) | 1 (4) |
Medication use
Participants had tried five different anti-psychotics on average (if the same medication was taken twice, it was counted as one medication taken). All patients had taken at least one atypical antipsychotic and more than two-thirds of them (n=41) had taken clozapine (Table 1). All patients were taking antipsychotic medication during the trial, and the majority were on atypical antipsychotic regimens. Nine patients were using a typical compound during the trial because they had been given depot medication. The medication regimens were kept stable during the study. Three patients experienced a relapse and their medication had to be changed; these patients were considered to have withdrawn from the study.
Treatment fidelity
A total of 40 tapes were scored. The mean score of the cognitive–behavioural therapy tapes scored by the first rater was 48.8 (s.d.=4.3) and the mean score of the supportive counselling tapes was 15.6 (s.d.=2.3). The second rater's mean scores were 53.7 (s.d.=3.7) and 15.4 (s.d.=1.5) respectively. A Pearson's correlation calculated between the two raters was 0.990 (P<0.001), indicating that the therapies were delivered according to protocol.
Outcome measures
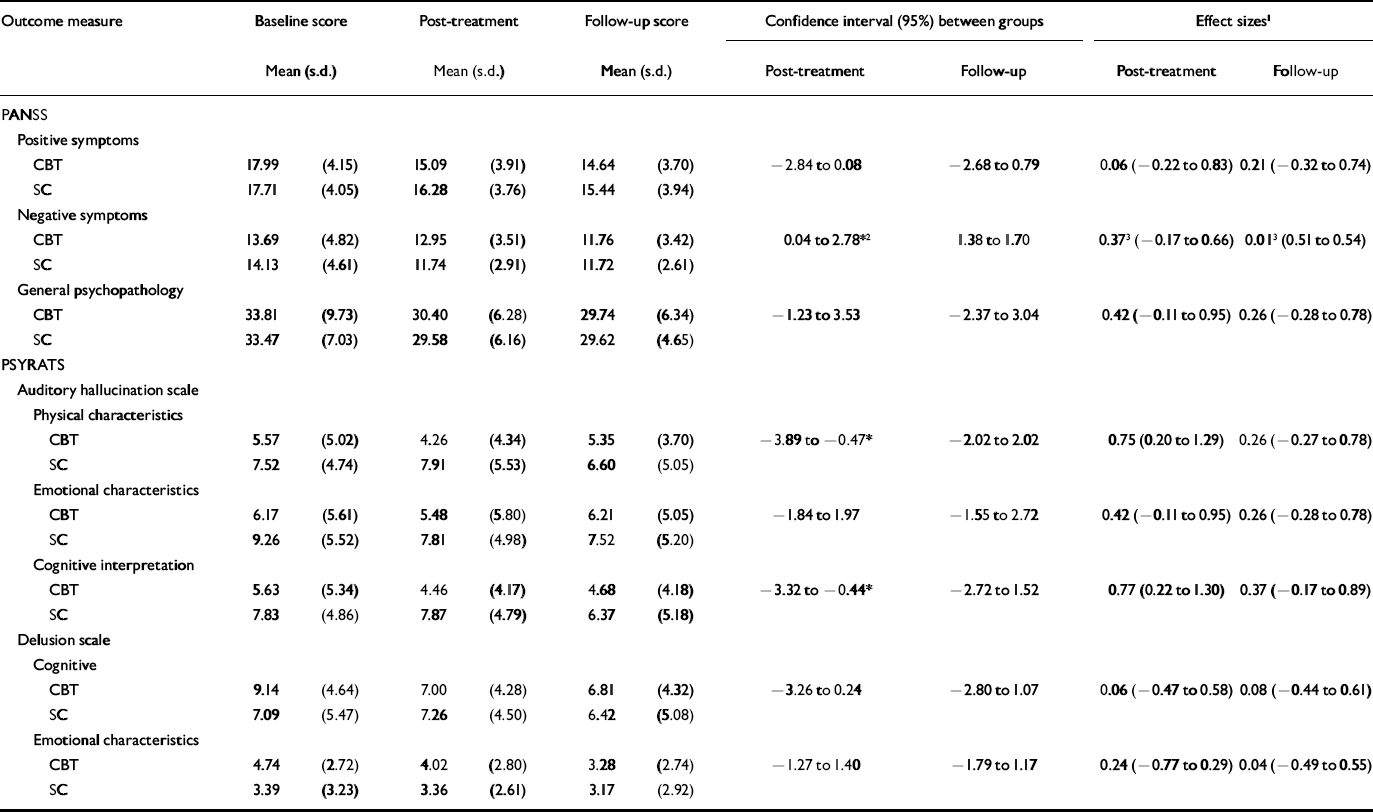
Table 2 shows the baseline, post-treatment and follow-up scores with regard to the primary hypothesis. At the post-treatment assessment the score on the positive subscale of the PANSS showed a non-significant effect of therapeutic condition (F(1,57)=3.58, P=0.064). Cognitive–behavioural therapy was more effective than supportive counselling on factor 1, physical characteristics, of the auditory hallucination scale (F(1,57)=6.43, P=0.014) and factor 3, cognitive interpretation (F(1,57)=6.86, P=0.011), but had no significant influence on factor 2, emotional characteristics. No significant effect of the therapeutic condition was found regarding the delusion scale factor 1, cognitive interpretation, and factor 2, emotional characteristics. In the follow-up results no significant effect of therapeutic condition on the score of any of the scales used to assess positive symptoms was found.
Table 2 Baseline, post-treatment and follow-up results for the cognitive–behavioural therapy group (n=35) and the supportive counselling group (n=23)
| Outcome measure | Baseline score | Post-treatment | Follow-up score | Confidence interval (95%) between groups | Effect sizes1 | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Mean (s.d.) | Mean (s.d.) | Mean (s.d.) | Post-treatment | Follow-up | Post-treatment | Follow-up | ||||
| PANSS | ||||||||||
| Positive symptoms | ||||||||||
| CBT | 17.99 | (4.15) | 15.09 | (3.91) | 14.64 | (3.70) | -2.84 to 0.08 | -2.68 to 0.79 | 0.06 (-0.22 to 0.83) | 0.21 (-0.32 to 0.74) |
| SC | 17.71 | (4.05) | 16.28 | (3.76) | 15.44 | (3.94) | ||||
| Negative symptoms | ||||||||||
| CBT | 13.69 | (4.82) | 12.95 | (3.51) | 11.76 | (3.42) | 0.04 to 2.78*2 | 1.38 to 1.70 | 0.373 (-0.17 to 0.66) | 0.013 (0.51 to 0.54) |
| SC | 14.13 | (4.61) | 11.74 | (2.91) | 11.72 | (2.61) | ||||
| General psychopathology | ||||||||||
| CBT | 33.81 | (9.73) | 30.40 | (6.28) | 29.74 | (6.34) | -1.23 to 3.53 | -2.37 to 3.04 | 0.42 (-0.11 to 0.95) | 0.26 (-0.28 to 0.78) |
| SC | 33.47 | (7.03) | 29.58 | (6.16) | 29.62 | (4.65) | ||||
| PSYRATS | ||||||||||
| Auditory hallucination scale | ||||||||||
| Physical characteristics | ||||||||||
| CBT | 5.57 | (5.02) | 4.26 | (4.34) | 5.35 | (3.70) | -3.89 to -0.47* | -2.02 to 2.02 | 0.75 (0.20 to 1.29) | 0.26 (-0.27 to 0.78) |
| SC | 7.52 | (4.74) | 7.91 | (5.53) | 6.60 | (5.05) | ||||
| Emotional characteristics | ||||||||||
| CBT | 6.17 | (5.61) | 5.48 | (5.80) | 6.21 | (5.05) | -1.84 to 1.97 | -1.55 to 2.72 | 0.42 (-0.11 to 0.95) | 0.26 (-0.28 to 0.78) |
| SC | 9.26 | (5.52) | 7.81 | (4.98) | 7.52 | (5.20) | ||||
| Cognitive interpretation | ||||||||||
| CBT | 5.63 | (5.34) | 4.46 | (4.17) | 4.68 | (4.18) | -3.32 to -0.44* | -2.72 to 1.52 | 0.77 (0.22 to 1.30) | 0.37 (-0.17 to 0.89) |
| SC | 7.83 | (4.86) | 7.87 | (4.79) | 6.37 | (5.18) | ||||
| Delusion scale | ||||||||||
| Cognitive | ||||||||||
| CBT | 9.14 | (4.64) | 7.00 | (4.28) | 6.81 | (4.32) | -3.26 to 0.24 | -2.80 to 1.07 | 0.06 (-0.47 to 0.58) | 0.08 (-0.44 to 0.61) |
| SC | 7.09 | (5.47) | 7.26 | (4.50) | 6.42 | (5.08) | ||||
| Emotional characteristics | ||||||||||
| CBT | 4.74 | (2.72) | 4.02 | (2.80) | 3.28 | (2.74) | -1.27 to 1.40 | -1.79 to 1.17 | 0.24 (-0.77 to 0.29) | 0.04 (-0.49 to 0.55) |
| SC | 3.39 | (3.23) | 3.36 | (2.61) | 3.17 | (2.92) | ||||
At follow-up the results of the analysis of covariance showed no significant effect on any of the variables measured. The effect sizes confirm the findings of the analysis of covariance.
Numbers needed to treat
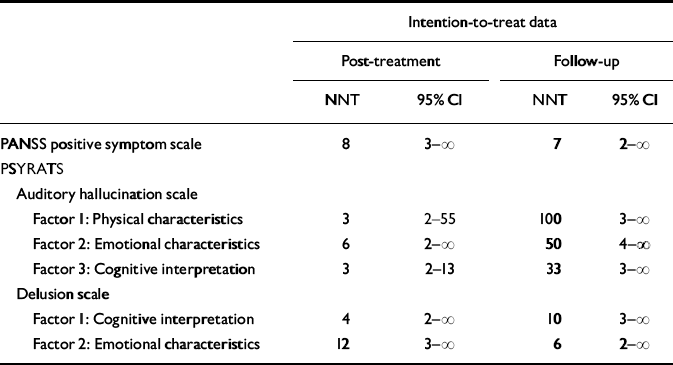
Using the same criteria as in a previous study (Reference Tarrier, Kinney and McCarthyTarrier et al, 2000), numbers needed to treat were calculated on a 20% symptom improvement for the positive sub-scale of the PANSS and for the factors of the PSYRATS. Table 3 displays the NNT and 95% confidence intervals at post-treatment and follow-up for the intention-to-treat analysis. The lack of statistical significance of the results is reflected in the confidence intervals of the NNTs. If the treatment effect is not statistically significant at the 5% level, the 95% confidence intervals include infinity (Reference AltmanAltman, 1998).
Table 3 Numbers needed to treat
| Intention-to-treat data | ||||
|---|---|---|---|---|
| Post-treatment | Follow-up | |||
| NNT | 95% CI | NNT | 95% CI | |
| PANSS positive symptom scale | 8 | 3-∞ | 7 | 2-∞ |
| PSYRATS | ||||
| Auditory hallucination scale | ||||
| Factor 1: Physical characteristics | 3 | 2-55 | 100 | 3-∞ |
| Factor 2: Emotional characteristics | 6 | 2-∞ | 50 | 4-∞ |
| Factor 3: Cognitive interpretation | 3 | 2-13 | 33 | 3-∞ |
| Delusion scale | ||||
| Factor 1: Cognitive interpretation | 4 | 2-∞ | 10 | 3-∞ |
| Factor 2: Emotional characteristics | 12 | 3-∞ | 6 | 2-∞ |
DISCUSSION
The aim of our study was to assess the effectiveness of cognitive–behavioural therapy and supportive counselling in an inpatient population with chronic schizophrenia refractory to treatment. To the authors’ knowledge this study is the first of its kind to include in-patients with chronic illness who did not benefit from atypical medication, and the first to keep the medication regimen stable during the trial.
Limitations
The first limitation of the study is that the strict inclusion and exclusion criteria led to a selective sample of patients. To be included in the study, participants had to have tried at least two antipsychotic compounds, including at least one atypical agent. Problems with recruitment were mainly due to the inefficient application of medication protocols in some of the institutes that participated in the study, which made it difficult to find patients who met the strict inclusion criteria with regard to drug-therapy resistance. A second limitation lies in the small sample size, which led to a lack of statistical power. Because of this lack of power, improvements that might have been significant with a large sample size were not found with the available data (type 2 error). A third limitation could be the loss of significant results at follow-up. A possible explanation for this loss could be that the patients included in the study had serious cognitive disabilities and that 16 sessions might not have been sufficient to produce stable results. Mueser et al (Reference Mueser, Drake and Bond1997) identified five characteristics of successful psychiatric interventions in chronic illness: they are direct and behavioural; produce specific effects on related outcomes and do not generalise to other domains; are long-term interventions; are delivered in the patients’ environment; and combine skills training and environmental support. Our intervention might have been too short; furthermore, it did not involve the environment of the patients.
Psychotic symptoms
The between-group analyses showed that cognitive–behavioural therapy was more effective than supportive counselling at the post-treatment assessment in reducing the physical characteristics and cognitive interpretation of auditory hallucinations. This indicates that the group receiving cognitive–behavioural therapy experienced a reduction in the frequency, duration, location and loudness of auditory hallucinations. The disruption of life associated with auditory hallucinations, belief about the origin of hallucinations and the attribution of control improved in this intervention group. No difference was found with regard to the emotional characteristics of auditory hallucinations. Contrary to previous results (e.g. Reference Sensky, Turkington and KingdonSensky et al, 2000), in our study the differences post-treatment with regard to auditory hallucinations were not maintained at follow-up. No between-group difference was found regarding delusions. A larger percentage of participants in the cognitive–behavioural condition showed a 20% reduction in symptoms on the positive sub-scale of the PANSS.
Numbers needed to treat
The research was conducted in a population with long-term illness that had proved resistant to other treatments including clozapine. To appreciate the relevance of the NNT found in this research, the reader might be interested in knowing that clozapine is effective in 32% of cases (NNT=5, 95% CI 4–7) in producing a clinical improvement (Reference Wahlbeck, Cheine and EssaliWahlbeck et al, 2002). Patients taking clozapine showed fewer relapses in the short term (NNT=20, 95% CI 17–38); no data are available for relapse prevention in the long term. Previous randomised controlled trials of the effect of cognitive–behavioural therapy on symptoms, when compared with other psychological interventions, show an NNT of 5 (National Institute for Clinical Excellence, 2003).
Clinical implications
The results of our trial showed that psychological treatment could induce a change in psychotic symptoms in in-patients with chronic illness. Excluding patients from psychological help on the grounds that they are too ill to benefit from therapy is not justified by these findings. Cognitive–behavioural therapy for psychotic symptoms should therefore be available in inpatient facilities.
The therapists and assessors who participated in the study were therapists from standard mental health services, not specialised research staff. As a result, cognitive–behavioural therapy for psychosis is now widely used in the participating institutes. Based on the experience accumulated during the course of the trial, a comprehensive teaching tool kit was produced (Reference van der Gaag, Valmaggia and van MeerGaag et al, 2000). In the subsequent years there has been an increasing demand for training in the use of this tool kit, and some therapists involved in the research have become involved as trainers.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The result of this randomised controlled trial showed that psychological treatment could induce a change in psychotic symptoms in in-patients with chronic illness.
-
▪ Excluding patients from psychological help on the expectation that they are too ill to benefit from therapy is not justified by these findings.
-
▪ Cognitive–behavioural therapy for psychotic symptoms should be available in inpatient facilities.
LIMITATIONS
-
▪ The study's strict inclusion and exclusion criteria led to a selective sample of patients.
-
▪ The small sample size resulted in a lack of statistical power.
-
▪ The intervention offered might have been too short; furthermore, it did not involve the environment of the patients.
Acknowledgements
The study was funded by a grant from the Stanley Medical Research. Institute. Further financial support was provided by GGZ-Drenthe and by the. Stichiting Bennenkom. We thank all the patients and therapists who. participated in the study.









eLetters
No eLetters have been published for this article.