The foetal origins hypothesis (Reference Barker, Winter and OsmondBarker et al, 1989; Reference BarkerBarker, 1998) has suggested a link between early life factors and adult health. Often quoted are studies showing a relationship between low birth weight and coronary heart disease (Reference Leon, Lithell and VageroLeon et al, 1998) or non-insulin-dependent diabetes mellitus (Reference Lithell, McKeigue and BerglundLithell et al, 1996). There is also evidence suggesting a link between markers of foetal growth and hypoxic brain damage, most notably low birth weight and schizophrenia (Reference Cannon, Jones and MurrayCannon et al, 2002). Evidence from three birth cohorts has suggested that low birth weight may act as a risk factor for common affective disorder across a range of ages (26 years (Reference Gale and MartynGale & Martyn, 2004); 23, 33 and 42 years (Reference Cheung, Khoo and KarlbergCheung et al, 2002); and 68 years (Reference Thompson, Syddall and RodinThompson et al, 2001)), but disparity exists. Thompson et al (Reference Thompson, Syddall and Rodin2001) reported an increased risk of depression at age 68 years for men born of low birth weight but not women, whereas Gale & Martyn (Reference Gale and Martyn2004) reported an increased risk of depression in women at 26 years, but not men.
Early life factors, such as birth weight, influence cognition (Reference BreslauBreslau, 1995; Reference Richards, Hardy and KuhRichards et al, 2001) and behaviour (Reference Kelly, Nazroo and McMunnKelly et al, 2001) in childhood, and childhood cognitive deficit and psychiatric disorders are associated with psychiatric disorder in adulthood (Reference van Os, Jones and Lewisvan Os et al, 1997). An indirect pathway linking low birth weight and adult psychiatric morbidity via childhood cognition and/or behavioural problems may therefore be proposed, but it is possible that, in addition to or instead of this indirect effect, early life factors may have a direct effect on the occurrence of common affective disorder in later life. Using data from the Aberdeen Children of the 1950s study (Reference Batty, Morton and CampbellBatty et al, 2004), we examined the association between birth weight and adult psychological distress at age 45-51 years. Our aim was to determine whether childhood factors (specifically, cognition and behavioural problems) mediate the association between early life factors and adult psychological distress.
METHOD
The Aberdeen Children of the 1950s cohort study
Full details of the Aberdeen Children of the 1950s study have been described elsewhere (Reference Batty, Morton and CampbellBatty et al, 2004). In brief, this cohort comprises children born in Aberdeen, Scotland, UK between 1950 and 1956 who participated in the Aberdeen Child Development Survey (ACDS). This was a cross-sectional survey of learning disability in all children attending a primary school in Aberdeen in December 1962. Obstetric and perinatal data (including preeclampsia, birth weight and length of gestation) were available by reference to the Aberdeen Maternal and Neonatal Databank (AMND), established in 1948. Father's social class at the time of birth was derived from the occupational status listed on obstetric records. Details of maternal age, parity and whether the child was a singleton birth were also available from AMND records. At baseline, data were available for 12 150 children.
Results of IQ tests (assessed using the Moray House Picture Intelligence Test; Reference Birch, Richardson and BairdBirch et al, 1970) routinely administered in Aberdeen schools at 7 years of age were extracted from school records for children taking part in the ACDS. Teachers also completed the Rutter Scale B (Reference RutterRutter, 1967) of behaviour disorder for each child. On the Rutter scale, a score of 9 or more is indicative of a childhood behavioural disorder. Further classification into neurotic or antisocial disorder can be made using the sub-scale scores. If neither sub-scale score dominates, the disorder is deemed ‘undifferentiated'.
In 1998 over 97% of the original cohort were traced and the majority still resided in Scotland. In May 2001, a questionnaire was mailed to surviving cohort members who were believed to be resident in the UK (n=11 282); 7183 cohort members responded (63.7% participation rate). A variety of socio-demographic data were recorded as part of this questionnaire, including marital status and current occupation, from which social class (I, II, III, IV or V) was assigned using the Standard Occupational Classification (Office of Population Censuses and Surveys, 1991).
In addition, participants were asked about psychological distress using 4 items from the 12-item General Health Questionnaire (GHQ; Reference Goldberg and WilliamsGoldberg & Williams, 1988).
These items were: have you (i) been able to enjoy your day-to-day activities; (ii) been feeling unhappy and depressed; (iii) been losing confidence in yourself; and (iv) been feeling reasonably happy, all things considered. It is known that long questionnaires reduce response rates (Reference Edwards, Roberts and ClarkeEdwards et al, 2002). Such practical considerations were behind the decision to limit the number of GHQ items included. Previous work has shown that the difference in the percentage of variation explained by any subset of four GHQ questions was less than 5% (Reference Jacobsen, Hasvold and HoyerJacobsen et al, 1995). Therefore, the four items included were based on an unrotated principal-components analysis of the data from the first sweep of the British Household Panel Survey (Reference Weich and LewisWeich & Lewis, 1998). The total score for the GHQ4 was derived using the GHQ scoring method (0, 0, 1, 1), giving total scores between 0 and 4. A score of 1 or more was taken to indicate adult psychological distress.
Data-set available for analysis
Of the 7183 participants who completed the 2001 follow-up questionnaire, data from 80 proxy respondents were excluded. Of the remaining 7103 individuals, 7033 had completed all four GHQ questions and, of these, 5572 had information recorded on AMND data: maternal age, father's social class at the time of birth, parity, whether the child was a singleton, pre-eclampsia during pregnancy, length of gestation and birth weight; ACDS reading survey data: gender, IQ at age 7 years and Rutter B scores; 2001 follow-up questionnaire data: marital status and adult social class.
Statistical analysis
All analyses were conducted using Stata version 8 for PC. Logistic regression was used to examine the relationship between obstetric and perinatal factors (birth weight for gestational age and pre-eclampsia) and adult psychological distress (GHQ4≥1). Odds ratios (ORs) and their 95% confidence intervals (95% CIs) are reported. Because of the presence of siblings within the data-set, the cluster option for logistic regression was used in all analyses.
Associations were initially adjusted for multiple birth, with subsequent adjustment for other potential confounding factors (gender, father's social class, parity and maternal age). Additional adjustment was then made for potential confounders identified in adulthood (marital status and social class recorded on the 2001 survey questionnaire).
The primary analysis dichotomised birth weight (using a cut-point of 5.5 lb or approximately 2500 g) and gestational age (≥38 weeks' gestation) in order to determine the effect of low birth weight by gestational age. However, in an attempt to provide a more sensitive estimate of the association, Z-scores (Reference Armitage, Berry and MatthewsArmitage et al, 2002) were calculated. The Z-score expresses birth weight in standard deviation units according to gestational age. Within the Aberdeen data-set, each completed week of gestation is recorded, with the exception of the extremes of the distribution (≤33 weeks and ≥43 weeks), similarly birth weight is recorded in categories of 0.5 lb except for extreme values (<2.5 lb and ≥9.5 lb). Z-scores were therefore calculated by estimating the mean birth weight category for each completed week of gestation, and the estimate of variance was adjusted using Sheppard's correction (Reference Armitage, Berry and MatthewsArmitage et al, 2002) to allow for the use of grouped data.
In order to test the hypothesis that early life factors have a direct effect on adult psychological distress, the logistic regression models were further adjusted for cognition (IQ at age 7 years) and Rutter neurotic and antisocial sub-scale scores. If the effect of early life factors on adult mental health was mediated through such intermediaries, then any association between early life factors and adult mental health would be attenuated.
Finally, given that missing data on the GHQ outcome variable meant that the above analyses involved just under half the original cohort, the validity of the study findings might be in doubt. To address this, a weighted analysis using probability weights (Reference Brick and KaltonBrick & Kalton, 1996) was conducted. Probability weights were constructed using a logistic regression model where the outcome was having or not having GHQ4 data. The influence of father's social class, maternal age, parity, multiple birth and gender were assessed individually and then combined in a multivariable model. The results of unweighted and weighted analyses were then compared to assess whether exclusion of subjects (because of missing data) had influenced the study findings. Further discussion of the representativeness of the study cohort can be found elsewhere (Reference Batty, Morton and CampbellBatty et al, 2004).
RESULTS
Description of the study cohort
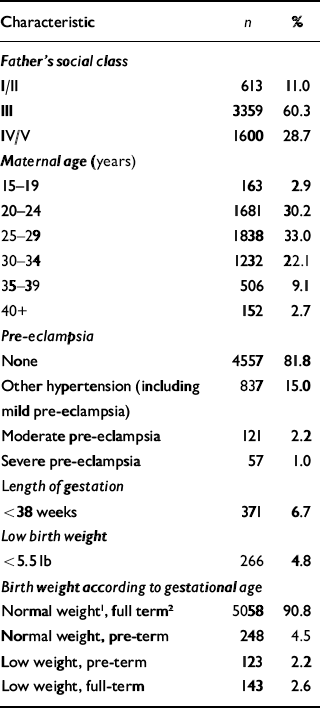
Of the 5572 participants, 2890 (51.9%) were female and 2682 (48.1%) were male. The majority of fathers (60.3%) were in social class III at the time of their child's birth (Table 1). Mothers were most commonly between the ages of 25 and 29 years at the birth of their child. This was the first child for just over a third of women (n=1901). Almost all the children (98%) were singletons.
Table 1 Characteristics of the study cohort
| Characteristic | n | % | |
|---|---|---|---|
| Father's social class | |||
| I/II | 613 | 11.0 | |
| III | 3359 | 60.3 | |
| IV/V | 1600 | 28.7 | |
| Maternal age (years) | |||
| 15-19 | 163 | 2.9 | |
| 20-24 | 1681 | 30.2 | |
| 25-29 | 1838 | 33.0 | |
| 30-34 | 1232 | 22.1 | |
| 35-39 | 506 | 9.1 | |
| 40+ | 152 | 2.7 | |
| Pre-eclampsia | |||
| None | 4557 | 81.8 | |
| Other hypertension (including mild pre-eclampsia) | 837 | 15.0 | |
| Moderate pre-eclampsia | 121 | 2.2 | |
| Severe pre-eclampsia | 57 | 1.0 | |
| Length of gestation | |||
| <38 weeks | 371 | 6.7 | |
| Low birth weight | |||
| <5.5 lb | 266 | 4.8 | |
| Birth weight according to gestational age | |||
| Normal weight 1 , full term 2 | 5058 | 90.8 | |
| Normal weight, pre-term | 248 | 4.5 | |
| Low weight, pre-term | 123 | 2.2 | |
| Low weight, full-term | 143 | 2.6 | |
1. Normal weight=birth weight of 5.5 lb or more.
2. Full-term=gestational length of 38 weeks or longer.
Prevalence of pre-eclampsia, pre-term birth and low birth weight
Table 1 shows that 18.2% of mothers had problems with hypertension, pre-eclampsia or eclampsia during pregnancy; 371 children (6.7%) were born before 38 weeks of gestation and almost 5% were born weighing less than 5.5 lb (or 2537 g).
Almost 3% of children were born at full term (≥38 weeks) but were of low weight (<5.5 lb) (Table 1).
Adult psychological distress
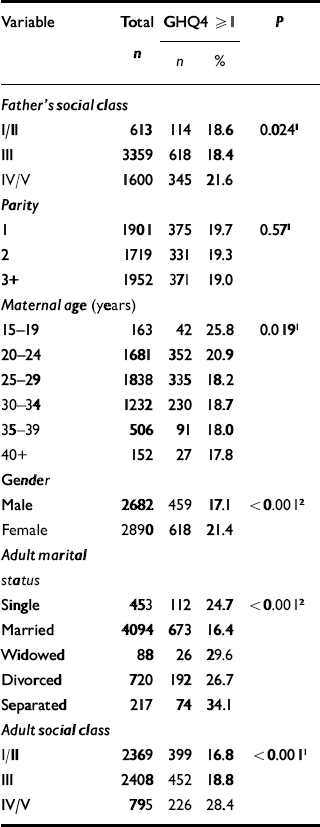
Nineteen per cent of the cohort (95% CI 18.3-20.4%) (n=1077) were categorised as having psychological distress (GHQ4≥1) at the time of the follow-up survey; 434 participants (7.8%) scored above two on the GHQ4 and 193 (3.5%) answered positively to all four questions. As expected, women were more likely to be distressed (21.4%) than men (17.1%) (Table 2). Furthermore, those whose fathers or who were themselves in social class IV or V were more likely to be distressed. Those who were married at the time of the 2001 survey were less likely to be distressed. There was also a tendency for those children born to young mothers to be more likely to report psychological distress in adulthood (Table 2).
Table 2 Childhood and adult factors and psychological distress in adulthood
| Variable | Total | GHQ4 ≥ 1 | P | ||
|---|---|---|---|---|---|
| n | n | % | |||
| Father's social class | |||||
| I/II | 613 | 114 | 18.6 | 0.024 1 | |
| III | 3359 | 618 | 18.4 | ||
| IV/V | 1600 | 345 | 21.6 | ||
| Parity | |||||
| 1 | 1901 | 375 | 19.7 | 0.57 1 | |
| 2 | 1719 | 331 | 19.3 | ||
| 3+ | 1952 | 371 | 19.0 | ||
| Maternal age (years) | |||||
| 15-19 | 163 | 42 | 25.8 | 0.019 1 | |
| 20-24 | 1681 | 352 | 20.9 | ||
| 25-29 | 1838 | 335 | 18.2 | ||
| 30-34 | 1232 | 230 | 18.7 | ||
| 35-39 | 506 | 91 | 18.0 | ||
| 40+ | 152 | 27 | 17.8 | ||
| Gender | |||||
| Male | 2682 | 459 | 17.1 | <0.001 2 | |
| Female | 2890 | 618 | 21.4 | ||
| Adult marital | |||||
| status | |||||
| Single | 453 | 112 | 24.7 | <0.001 2 | |
| Married | 4094 | 673 | 16.4 | ||
| Widowed | 88 | 26 | 29.6 | ||
| Divorced | 720 | 192 | 26.7 | ||
| Separated | 217 | 74 | 34.1 | ||
| Adult social class | |||||
| I/II | 2369 | 399 | 16.8 | <0.001 1 | |
| III | 2408 | 452 | 18.8 | ||
| IV/V | 795 | 226 | 28.4 | ||
1. χ2 test for trend.
2. χ2 test for association.
Associations between obstetric and perinatal factors and childhood IQ and behavioural disorder
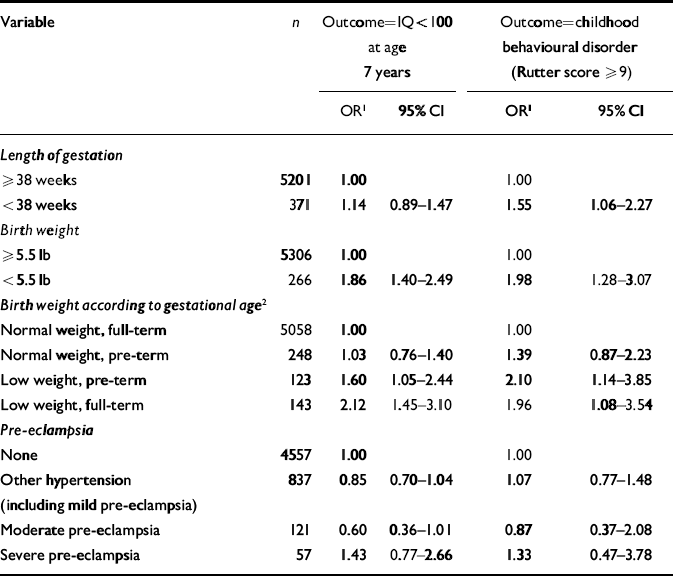
As in previous studies, low birth weight (<5.5 lb) was associated with an increased odds of cognitive deficit (IQ <100) at age 7 years and childhood behavioural disorder (Table 3). This effect was observed among both those born early (<38 weeks' gestation) and those born at term. There was no such increase for the children of mothers who had severe pre-eclampsia during pregnancy, although this was based on small numbers.
Table 3 Associations between obstetric and perinatal factors and childhood IQ and behavioural disorder
| Variable | n | Outcome=IQ < 100 at age 7 years | Outcome=childhood behavioural disorder (Rutter score ≥ 9) | ||||
|---|---|---|---|---|---|---|---|
| OR 1 | 95% CI | OR 1 | 95% CI | ||||
| Length of gestation | |||||||
| ≥ 38 weeks | 5201 | 1.00 | 1.00 | ||||
| < 38 weeks | 371 | 1.14 | 0.89-1.47 | 1.55 | 1.06-2.27 | ||
| Birth weight | |||||||
| ≥ 5.5 lb | 5306 | 1.00 | 1.00 | ||||
| <5.5 lb | 266 | 1.86 | 1.40-2.49 | 1.98 | 1.28-3.07 | ||
| Birth weight according to gestational age 2 | |||||||
| Normal weight, full-term | 5058 | 1.00 | 1.00 | ||||
| Normal weight, pre-term | 248 | 1.03 | 0.76-1.40 | 1.39 | 0.87-2.23 | ||
| Low weight, pre-term | 123 | 1.60 | 1.05-2.44 | 2.10 | 1.14-3.85 | ||
| Low weight, full-term | 143 | 2.12 | 1.45-3.10 | 1.96 | 1.08-3.54 | ||
| Pre-eclampsia | |||||||
| None | 4557 | 1.00 | 1.00 | ||||
| Other hypertension | 837 | 0.85 | 0.70-1.04 | 1.07 | 0.77-1.48 | ||
| (including mild pre-eclampsia) | |||||||
| Moderate pre-eclampsia | 121 | 0.60 | 0.36-1.01 | 0.87 | 0.37-2.08 | ||
| Severe pre-eclampsia | 57 | 1.43 | 0.77-2.66 | 1.33 | 0.47-3.78 | ||
OR, odds ratio; CI, confidence interval.
1. Adjusted for father's social class, multiple birth, parity, maternal age, gender.
2. Normal weight means birth weight of 5.5 lb or more and full-term means gestational length of 38 weeks or longer.
Associations between childhood IQ and behavioural disorder and adult psychological distress
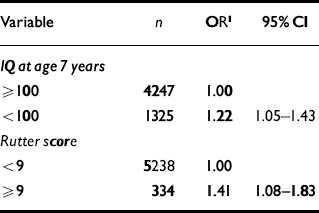
IQ <100 at age 7 years was associated with an increased odds of psychological distress in adulthood (Table 4). A score of 9 or above on the Rutter scale was associated with a 40% increased odds of adult psychological distress (Table 4).
Table 4 Associations between childhood IQ and behavioural disorder and adult psychological distress (GHQ4≥1)
| Variable | n | OR 1 | 95% CI |
|---|---|---|---|
| IQ at age 7 years | |||
| ≥ 100 | 4247 | 1.00 | |
| <100 | 1325 | 1.22 | 1.05-1.43 |
| Rutter score | |||
| <9 | 5238 | 1.00 | |
| ≥ 9 | 334 | 1.41 | 1.08-1.83 |
OR, odds ratio; CI, confidence interval.
1. Adjusted for father's social class, gender, multiple birth, parity, maternal age.
Associations between obstetric and perinatal factors and adult psychological distress
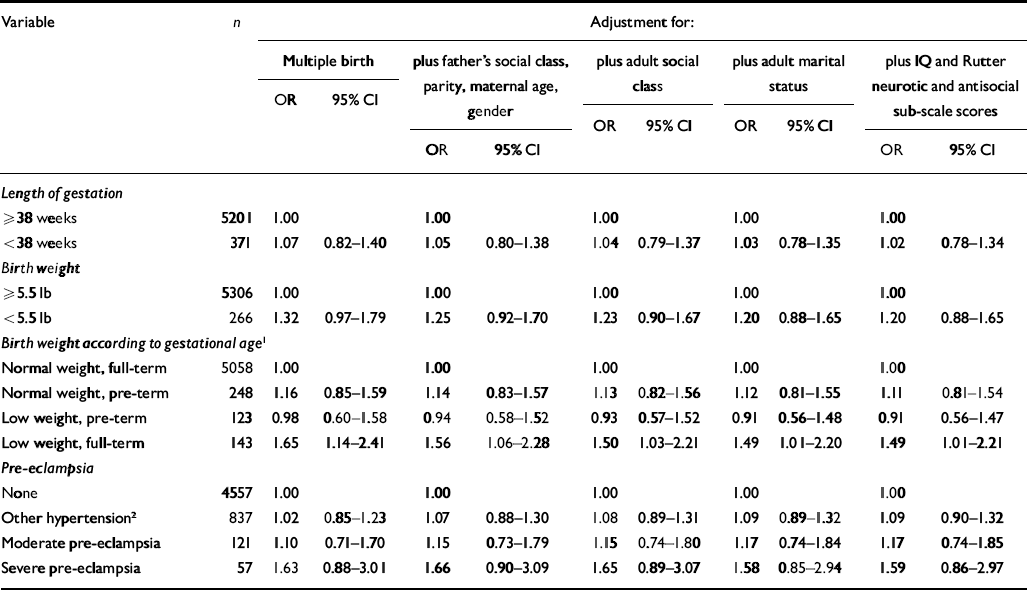
Neither pre-term delivery (<38 weeks' gestation) nor low birth weight (<5.5 lb) was associated with an increased odds of psychological distress in adulthood (Table 5). However, those children who were born weighing less than 5.5 lb but at full term (i.e. born after at least 38 weeks of gestation) had an increased odds (1.65 (95% CI 1.14-2.41)) of experiencing psychological distress at age 45-51 years (Table 5). After adjustment for potential confounders (father's social class, parity, maternal age, gender, adult social class and adult marital status), this association persisted (OR=1.49 (95% CI 1.01-2.21)). No increase in odds was observed for those of low birth weight who were born early (before 38 weeks). Similarly, pre-term delivery was not associated with an increased odds of psychological distress in adulthood among those of normal birth weight (Table 5).
Table 5 Associations between obstetric and perinatal factors and adult psychological distress (GHQ4≥I)
| Variable | n | Adjustment for: | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Multiple birth | plus father's social class, parity, maternal age, gender | plus adult social class | plus adult marital status | plus IQ and Rutter neurotic and antisocial sub-scale scores | ||||||||||||||||
| OR | 95%CI | OR | 95%CI | OR | 95%CI | OR | 95%CI | OR | 95%CI | |||||||||||
| Length of gestation | ||||||||||||||||||||
| ≥ 38 weeks | 5201 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | ||||||||||||||
| <38 weeks | 371 | 1.07 | 0.82-1.40 | 1.05 | 0.80-1.38 | 1.04 | 0.79-1.37 | 1.03 | 0.78-1.35 | 1.02 | 0.78-1.34 | |||||||||
| Birth weight | ||||||||||||||||||||
| ≥ 5.5 Ib | 5306 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | ||||||||||||||
| <5.5 Ib | 266 | 1.32 | 0.97-1.79 | 1.25 | 0.92-1.70 | 1.23 | 0.90-1.67 | 1.20 | 0.88-1.65 | 1.20 | 0.88-1.65 | |||||||||
| Birth weight according to gestational age 1 | ||||||||||||||||||||
| Normal weight, full-term | 5058 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | ||||||||||||||
| Normal weight, pre-term | 248 | 1.16 | 0.85-1.59 | 1.14 | 0.83-1.57 | 1.13 | 0.82-1.56 | 1.12 | 0.81-1.55 | 1.11 | 0.81-1.54 | |||||||||
| Low weight, pre-term | 123 | 0.98 | 0.60-1.58 | 0.94 | 0.58-1.52 | 0.93 | 0.57-1.52 | 0.91 | 0.56-1.48 | 0.91 | 0.56-1.47 | |||||||||
| Low weight, full-term | 143 | 1.65 | 1.14-2.41 | 1.56 | 1.06-2.28 | 1.50 | 1.03-2.21 | 1.49 | 1.01-2.20 | 1.49 | 1.01-2.21 | |||||||||
| Pre-eclampsia | ||||||||||||||||||||
| None | 4557 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | ||||||||||||||
| Other hypertension 2 | 837 | 1.02 | 0.85-1.23 | 1.07 | 0.88-1.30 | 1.08 | 0.89-1.31 | 1.09 | 0.89-1.32 | 1.09 | 0.90-1.32 | |||||||||
| Moderate pre-eclampsia | 121 | 1.10 | 0.71-1.70 | 1.15 | 0.73-1.79 | 1.15 | 0.74-1.80 | 1.17 | 0.74-1.84 | 1.17 | 0.74-1.85 | |||||||||
| Severe pre-eclampsia | 57 | 1.63 | 0.88-3.01 | 1.66 | 0.90-3.09 | 1.65 | 0.89-3.07 | 1.58 | 0.85-2.94 | 1.59 | 0.86-2.97 | |||||||||
OR, odds ratio; CI, confidence interval.
1. Normal weight means birth weight of 5.5 lb or more and full-term means gestational length of 38 weeks or longer.
2. Includes mild pre-eclampsia.
Excluding the multiple births from the data-set would result in significant loss of power for our analysis as this group has greater exposure. However, we have undertaken a stratified analysis by multiplicity and found that the low weight at term category was at greatest risk of adult psychological distress among both singletons and multiple-birth infants (data not shown). Moreover, there was no evidence of an interaction between birth weight by gestational age and multiplicity (P=0.19).
After adjustment for confounders, the children of those mothers who had experienced severe pre-eclampsia or eclampsia during pregnancy also had an increased odds of psychological distress in adulthood. However, this may be due to chance (Table 5).
Additional modelling demonstrated that the observed association between low birth weight at full term and adult psychological distress was independent of pre-eclampsia (data not shown). While a formal test of interaction was inconclusive (P=0.25), analysis stratified by gender showed stronger associations for men than women for low birth weight at full term (ORmen=2.85 (95% CI 1.40-5.78) v. ORwomen=1.16 (95% CI 0.72-1.88)).
The direct effect of low birth weight at full term on adult psychological distress was examined by further adjusting the logistic regression models for IQ at age 7 years and Rutter sub-scale scores (Table 5). Little change in the size of the effect estimates following this adjustment was observed, suggesting that low birth weight at full term has a direct effect on adult mental health. Although we have examined the mediating role of childhood IQ and behaviour in this data-set, we cannot exclude the possibility that other factors may mediate this relationship.
Using Z-scores, an increased odds of adult psychological distress was observed for those of low birth weight for gestational age. For a standard deviation decrease in birth weight for gestational age, there was a 4% increased odds of psychological distress in adulthood (OR=1.04, 95% CI 0.97-1.12). The strength of this association increased when restricted to infants born at term (OR=1.06 (95% CI 0.98, 1.14)). Again, additional adjustment for childhood IQ and behavioural disorder (Rutter scores) did not attenuate this association (data not shown).
Differences between those with and without GHQ outcome data
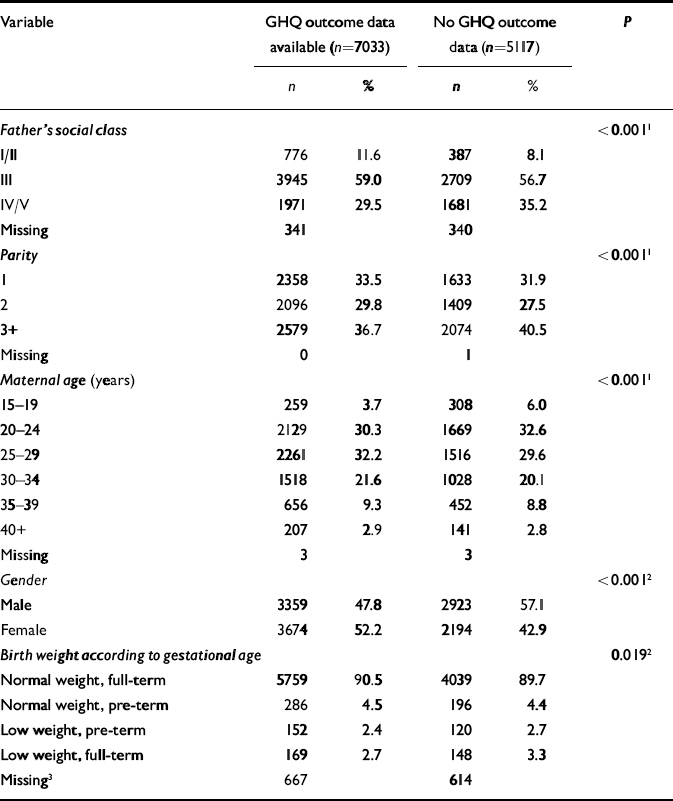
There were a number of differences in the baseline characteristics among those who did and did not complete the GHQ items included in the 2001 follow-up questionnaire (Table 6). Those who did not complete the GHQ were more likely to be male and have fathers of lower social class. However, there was no difference in the birth weight for gestational age profile among those who did or did not have GHQ outcome data.
Table 6 Comparison of characteristics of those with and without GHQ outcome data
| Variable | GHQ outcome data available (n=7033) | No GHQ outcome data (n=5117) | P | ||||
|---|---|---|---|---|---|---|---|
| n | % | n | % | ||||
| Father's social class | <0.001 1 | ||||||
| I/II | 776 | 11.6 | 387 | 8.1 | |||
| III | 3945 | 59.0 | 2709 | 56.7 | |||
| IV/V | 1971 | 29.5 | 1681 | 35.2 | |||
| Missing | 341 | 340 | |||||
| Parity | <0.001 1 | ||||||
| 1 | 2358 | 33.5 | 1633 | 31.9 | |||
| 2 | 2096 | 29.8 | 1409 | 27.5 | |||
| 3+ | 2579 | 36.7 | 2074 | 40.5 | |||
| Missing | 0 | 1 | |||||
| Maternal age (years) | <0.001 1 | ||||||
| 15-19 | 259 | 3.7 | 308 | 6.0 | |||
| 20-24 | 2129 | 30.3 | 1669 | 32.6 | |||
| 25-29 | 2261 | 32.2 | 1516 | 29.6 | |||
| 30-34 | 1518 | 21.6 | 1028 | 20.1 | |||
| 35-39 | 656 | 9.3 | 452 | 8.8 | |||
| 40+ | 207 | 2.9 | 141 | 2.8 | |||
| Missing | 3 | 3 | |||||
| Gender | <0.001 2 | ||||||
| Male | 3359 | 47.8 | 2923 | 57.1 | |||
| Female | 3674 | 52.2 | 2194 | 42.9 | |||
| Birth weight according to gestational age | 0.019 2 | ||||||
| Normal weight, full-term | 5759 | 90.5 | 4039 | 89.7 | |||
| Normal weight, pre-term | 286 | 4.5 | 196 | 4.4 | |||
| Low weight, pre-term | 152 | 2.4 | 120 | 2.7 | |||
| Low weight, full-term | 169 | 2.7 | 148 | 3.3 | |||
| Missing 3 | 667 | 614 | |||||
1. χ2 test for trend.
2. χ2 test for association.
3. Primarily due to missing data on gestational age.
Adjustment using probability weights (to account for the observed differences) did not substantially alter the size of the effect estimates when compared with the results obtained for the unweighted analysis (data not shown). Exclusion of subjects from the cohort being analysed (because of missing outcome data) was therefore unlikely to have biased the effect estimates obtained.
DISCUSSION
The aim of this study was to investigate the association between obstetric and perinatal factors and psychological distress at ages 45-51 years and, in particular, to investigate the pathway through which these early life factors may act on adult mental health. We found that children born at full term but of low birth weight (<5.5 lb) had an increased odds of psychological distress in later life, which persisted after adjustment for potential confounders. No such increase was seen for those of low birth weight who were born early. Further adjustment for childhood factors (IQ and behavioural problems) did not alter the strength of the association between low birth weight at full term and adult psychological distress. This suggests that low birth weight at full term has a direct effect on adult mental health rather than simply reflecting a pathway through childhood cognition and/or behaviour.
Severe pre-eclampsia/eclampsia was also associated with an increased odds of psychological distress in adulthood, although this may be due to chance given the small numbers with this condition. As others have suggested (Reference Cannon, Jones and MurrayCannon et al, 2002), notwithstanding the large sample size there still may be limits on the factors that can be explored given the low prevalence of obstetric complications.
In line with the finding of an earlier case-control study (Reference Preti, Cardascia and ZenPreti et al, 2000), more recent results from birth cohort studies have shown that low birth weight is associated with affective disorder in adulthood (Reference Thompson, Syddall and RodinThompson et al, 2001; Reference Cheung, Khoo and KarlbergCheung et al, 2002; Reference Gale and MartynGale & Martyn, 2004). Gale & Martyn (Reference Gale and Martyn2004) also reported that the effect of low birth weight on depression at age 26 years was stronger among those born at full term, which is in agreement with our findings. Studies of the Dutch Hunger Winter and subsequent linkage with the Dutch psychiatric registry (Reference Brown, van Os and DriessensBrown et al, 2000) have also shown an association between prenatal famine (in the second and third trimester) and hospitalisation for major affective disorder. However, the study of hospitalised patients (Reference Brown, van Os and DriessensBrown et al, 2000; Reference Preti, Cardascia and ZenPreti et al, 2000) is likely to introduce selection bias. Adjustment for confounding factors was also lacking (Reference Brown, van Os and DriessensBrown et al, 2000) or limited (Reference Thompson, Syddall and RodinThompson et al, 2001) in previous investigations.
Using data from the 1970 birth cohort, Gale & Martyn (Reference Gale and Martyn2004) conducted separate analyses to examine the relationship between birth weight and psychological distress at age 16 years, history of depression between 16 and 26 years and depression at 26 years. However, the relationship between birth weight, psychological distress in late childhood (age 16 years) and adult depression was not explored. Similarly, data on childhood behavioural problems and cognition were available for participants of the 1958 birth cohort, but the influence of these factors was not examined by Cheung et al (Reference Cheung, Khoo and Karlberg2002). We are not aware of any previous study investigating the mechanism by which birth weight, childhood factors and adult mental health are linked and we have found that term low birth weight has a direct effect on psychological distress in adulthood.
Strengths and limitations
The Aberdeen Children of the 1950s cohort covers residents of a specific geographical area, whereas the 1946, 1958 and 1970 cohorts include births from across the entire UK. IQ scores of ACDS participants are known to be comparable with other studies (Reference Birch, Richardson and BairdBirch et al, 1970), but fathers of children participating in ACDS were of lower social class compared with figures for Scotland or other birth cohorts (Reference Batty, Morton and CampbellBatty et al, 2004).
The Aberdeen Children of the 1950s study has the advantage of having detailed obstetric data recorded prior to the onset of psychological distress (via the AMND). Furthermore, detailed information was available on potential confounders. The only major omissions were the lack of data on maternal smoking and parental mental health. Studies have suggested links between maternal psychosocial factors and low birth weight for gestational age (Reference Paarlberg, Vingerhoets and PasschierPaarlberg et al, 1999) and between parental mental health and child cognition and/or behaviour (Reference Ramchandani and SteinRamchandani & Stein, 2003). However, for primary cases of major depression, heritability has been estimated at approximately 20% (Reference Kendler, Neale and KesslerKendler et al, 1992), a relatively small figure. Having adjusted for major confounders (paternal social class, maternal age, parity, gender, adult social class and adult marital status), confounding is therefore unlikely to explain the observed association between term low birth weight and psychological distress in adulthood, although we cannot exclude such a possibility.
One potential limitation of our study is the measurement of adult psychological distress using the GHQ rather than a standardised psychiatric interview. However, the GHQ has been used widely in population studies and is a valid and reliable instrument (Reference Goldberg and WilliamsGoldberg & Williams, 1988). A shortened version of the GHQ was used for practical reasons and the four items derived from a principal-components analysis of data from a large (n=7726) nationwide prospective cohort study (Reference Weich and LewisWeich & Lewis, 1998). Using these four items, the prevalence of psychological distress was similar to that observed in other population studies (Reference Weich and LewisWeich & Lewis, 1998). Furthermore, we conducted a sensitivity analysis (data not shown) to examine the effect of different methods of scoring the GHQ on the results. This supported our findings of an association between term low birth weight and adult psychological distress.
In common with other birth cohorts (Reference Gale and MartynGale & Martyn, 2004), those not responding to the follow-up questionnaire were more likely to be born to younger mothers, to have fathers of lower social class and to be male. However, there were no differences in the profile of birth weight according to gestational age among respondents and non-respondents. In order to address the potential impact of the above differences, a weighted analysis was conducted; the results differed little from the unweighted figures. Attrition is therefore unlikely to have biased the study findings.
Possible aetiological mechanisms
Low birth weight for gestational age is a marker of impaired foetal growth. The observed association with adult psychological distress provides further evidence for the theory that adult psychiatric morbidity may be a consequence of impaired neurodevelopment. In infants born at full-term, this is usually attributed to placental insufficiency (which leads to a reduction in oxygen and nutrients to the developing foetus), whereas in pre-term infants there are many other potential pathophysiological processes that might affect the brain. Studies of the Dutch Hunger Winter (Reference Brown, van Os and DriessensBrown et al, 2000) noted that the effect of birth weight was confined to the second or third trimester, which suggests that there may be a ‘critical' period (Reference Ben Shlomo and KuhBen Shlomo & Kuh, 2002) during which neuroimpairment occurs, thereby increasing the later susceptibility to psychological distress. In addition, the fact that low birth weight had a direct effect on adult health (rather than acting via effects on childhood cognition and/or behaviour) implies that an environmental trigger in later life may result in psychological distress in vulnerable individuals. As has been proposed for schizophrenia (Reference Keshavan and HogartyKeshavan & Hogarty, 1999), this delayed effect may also reflect a maturational developmental process. This theory is supported by work in rats where neonatal excitotoxic hippocampal damage resulted in abnormal behaviour in adulthood (Reference Lipska and WeinbergerLipska & Weinberger, 1994).
Structural changes relating to a number of biological mechanisms have been implicated. These include the hypothalamic-pituitary-adrenal axis (Reference Thompson, Syddall and RodinThompson et al, 2001; Reference Gale and MartynGale & Martyn, 2004), the growth hormone axis (Reference Thompson, Syddall and RodinThompson et al, 2001) and thyroid function (Reference Thompson, Syddall and RodinThompson et al, 2001). However, understanding the involvement of such mechanisms is complicated by the overlap between these systems and cognitive function. Alternatively, neuropathological abnormalities in areas that are involved with emotional response (observed in structural imaging studies (Reference Manji, Drevets and CharneyManji et al, 2001)) may reflect the influence of early life factors.
Others have suggested that low levels of maternal insulin-like growth factor (IGF-1) during pregnancy are associated with restricted foetal growth (Reference Holmes, Holly and SoothillHolmes et al, 1998). There is also experimental evidence that mice deficient in liver IGF-1 have reduced insulin sensitivity (Reference Haluzik, Yakar and GavrilovaHaluzik et al, 2003). The modulatory role of IGF-1 is further supported by recent work showing an inverse relationship between insulin resistance and depression (Reference Lawlor, Davey Smith and EbrahimLawlor et al, 2003). Recently, IGF has been implicated in the association of markers of foetal growth impairment with schizophrenia (Reference Gunnell and HollyGunnell & Holly, 2004). IGF-1 can cross the blood-brain barrier and has been suggested to directly influence brain development (Reference Gunnell and HollyGunnell & Holly, 2004). While the trend for an increased odds of psychological distress in adulthood across the entire spectrum of birth weight for gestational age (Z-score analysis) suggests that hormonal effects may be involved, it is unlikely that there is a sole aetiological factor underlying low birth weight (Reference Soothill, Bobrow and HolmesSoothill et al, 1999).
In conclusion, low birth weight babies, particularly at term, were more likely to experience psychological distress in adulthood. This appears to be a direct relationship, rather than being mediated by childhood factors. A neurodevelopmental pathway is thus implicated in the development of common affective disorder. Further work is required to elucidate the biological mechanism underlying this relationship.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Children born at full term but of low birth weight (<5.5 lb) are more likely to experience psychological distress in adulthood. This association appears to be direct, not mediated by childhood factors.
-
▪ This delayed effect may reflect a maturational developmental process.
-
▪ A neurodevelopmental pathway is implicated in the development of common affective disorder, not just schizophrenia.
LIMITATIONS
-
▪ Psychological distress was based on self-report rather than clinical interview.
-
▪ No data were available on parental mental health, which may be a possible confounder.
-
▪ Results are based on a cohort of individuals from one geographical region of the UK.
Acknowledgements
We thank Raymond Illsley for providing us with the data from the Aberdeen Child Development Survey and for his advice. Graeme Ford played a crucial role in identifying individual cohort members. Sally Macintyre, Doris Campbell, George Davey Smith, Marion Hall, Bianca de Stavola, Susan Morton, David Batty, David Godden, Di Kuh, Debbie Lawlor and Viveca stberg collaborated with David Leon to revitalise the cohort. Heather Clark managed the study at the Dugald Baird Centre, Aberdeen with the assistance of Margaret Beveridge. We would also like to thank staff at the Information and Statistics Division (Edinburgh), the General Register Office (Scotland) and the National Health Service Central Register (Southport) for their substantial contributions and John Lemon who undertook the linkage to the Aberdeen Maternity and Neonatal Databank. We also thank Dr Kate Tilling for advice on the use of probability weights and Professor David Gunnell for his comments on an earlier draft of this paper. Finally, we thank the study participants who responded to a mailed questionnaire 40 years after the the original survey was completed.
The Aberdeen Children of the 1950s Study was funded as a component project (G0828205) of a Medical Research Council Co-Operative Group Life-Course and Trans-Generational Influences on Disease Risk (G9819083). A project on cognition and adult health in the cohort has been funded by the Chief Scientist's Office, Scottish Executive Health Department, which currently funds Heather Clark.











eLetters
No eLetters have been published for this article.