Substance use is widespread in the community (Reference Costa e SilvaCosta e Silva, 2002). Cannabis is the most widely used illegal substance in Europe (European Monitoring Centre for Drugs and Drug Addiction, 2001), the USA (Substance Abuse and Mental Health Services Administration, 2001) and Australia (Australian Institute of Health and Welfare, 2002). Studies by Arseneault et al (Reference Arseneault, Cannon and Poulton2002), van Os et al (Reference van Os, Bak and Hanssen2002) and Zammit et al (Reference Zammit, Allebeck and Andreasson2002) have reported an association between cannabis use and later psychosis. However, sharp increases in cannabis use have not been reflected in an increased prevalence of schizophrenia (Reference Degenhardt, Hall and LynskeyDegenhardt et al, 2003). Also, a notable feature of the available literature has been the conflicting findings on the prevalence of substance use and associated outcomes on psychosis (Reference Rabinowitz, Bromet and LavelleRabinowitz et al, 1998). The conflicting results have been attributed to factors such as sample composition (Reference Mueser, Yarnold and LevinsonMueser et al, 1990; Reference Blanchard, Brown and HoranBlanchard et al, 2000), country (Reference Hambrecht and HafnerHambrecht & Häfner, 1996), recruitment source (Reference Mueser, Yarnold and LevinsonMueser et al, 1990; Reference Hambrecht and HafnerHambrecht & Häfner, 1996; Reference Fowler, Carr and CarterFowler et al, 1998) and issues associated with diagnosis and method of data collection (Reference Mueser, Yarnold and LevinsonMueser et al, 1990; Reference Hambrecht and HafnerHambrecht & Häfner, 1996; Reference Fowler, Carr and CarterFowler et al, 1998; Reference Blanchard, Brown and HoranBlanchard et al, 2000). However, little research has been undertaken into factors contributing to the variability in prevalence estimates. The aim of our review is to obtain more reliable estimates of the prevalence of cannabis use based on larger samples, to examine factors that may be associated with variability in prevalence estimates and to compare prevalence estimates of individuals with and without psychosis.
METHOD
We examined reports of cannabis use and misuse prevalence, and whether the variability in these prevalence estimates was associated with factors identified by the researchers as potentially important. These factors included age and percentage of males in studies, median year of data collection, geographic area, recruitment source, first-episode status, specificity of diagnosis of psychosis and use of standard diagnostic classification criteria.
Inclusion criteria
Citations and academic databases were searched to identify English-language studies published between 1990 and 2002 which might contain data on the use or misuse of cannabis by people diagnosed with psychosis, schizophrenia-spectrum disorders or schizophrenia. Search terms used in PsycInfo and Medline were CANNABIS, MARIHUANA, MARIJUANA or HASHISH combined with SCHIZOPHRENIA, PSYCHOSIS or PSYCHOTIC. A second search was conducted using the term DUAL DIAGNOSIS. Where possible the authors of studies were contacted to identify whether specific information on cannabis and psychosis or schizophrenia was available. We identified 164 clinical studies that might have contained information on cannabis use and psychosis. The following review is based on 53 studies that met the inclusion criteria. In addition, five epidemiological studies that met the inclusion criteria were analysed separately.
In-patient and community patient studies were included if the prevalence of cannabis use or misuse among patients with psychosis, schizophrenia-spectrum disorders or schizophrenia could be calculated (e.g. studies were excluded if there was no breakdown by diagnosis or it was not clear whether all patients had psychotic symptoms); information was available regarding the prevalence interval used; substance use was not an inclusion criterion; the study did not oversample by age, gender or other criteria; and patients were only included once. Research on the same sample was not included twice for the same prevalence interval. Where a study reported prevalence by psychosis in general, as well as by subgroups such as schizophrenia, the more specific information was selected.
For the purpose of this review, misuse (including dependence) was the focus, since specific dependence data were not frequently reported. One study (Reference Duke, Pantelis and McPhillipsDuke et al, 2001) reporting misuse was included with the studies reporting use, since ‘misuse’ was defined as ‘any use’. Three time intervals for reporting prevalence of cannabis use and misuse were examined. Studies that reported prevalence in terms of use or misuse at a baseline assessment or in a 6-month period were categorised as current use or misuse. Studies that reported prevalence in terms of a 12-month to 18-month period were categorised as 12-month prevalence studies, whereas studies reporting any use or misuse ever were categorised as lifetime studies.
Analysis
Three sets of analyses were conducted. The first analysis involved the calculation of current, 12-month and lifetime prevalence estimates. For each prevalence interval (e.g. current use), the total number of reported cannabis users in studies that contained current use data was divided by the total sample size of the respective studies to calculate a weighted average.
To examine potential sources of variability in prevalence estimates, four multivariate analyses were performed. The respective prevalence interval (e.g. lifetime misuse) was the dependent variable and the following variables were entered as independent variables: recruitment source (whether study participants were recruited from a hospital, community setting or a combination of both); geographic area (studies were grouped as being conducted in either Australasia, continental Europe, North America or the UK); use of standardised substance misuse classification criteria (criteria reflecting an ICD or DSM diagnosis, as opposed to criteria devised by study authors); specificity of the diagnosis of psychosis (psychosis, schizophrenia-spectrum disorders or schizophrenia only) and first-episode status (a specific first-episode sample or not). Average age of the study samples, percentage of males in a study and the median year of data collection for each study were covariates. Missing values for average age and percentage of males resulted in some studies not being included in the multivariate analyses (Table 1). Multinomial logistic regression, which can be used to analyse dichotomous variables, was selected in preference to logistic regression for the analyses, because it has the advantage of calculating the likelihood ratio test for each individual independent variable (Reference MenardMenard, 2001). The likelihood ratio test is useful for determining the significance of variables included in a logistic regression model. The odds ratios reported in Tables 4 and 5 refer to the respective increase or decrease in the odds of cannabis use or misuse associated with each independent variable.
Table 1 Studies included in the analyses of clinical data

| Study | Prevalence data | Study distinguished between misuse and dependence |
|---|---|---|
| Arndt et al (Reference Arndt, Tyrrell and Flaum1992) | Lifetime misuse | No |
| Bersani et al (Reference Bersani, Orlandi and Kotzalidis2002) | Lifetime misuse, lifetime use | No |
| Brewer et al (Reference Brewer, Pantelis and Anderson2001) | Current use | No |
| Cantor-Graae et al (Reference Cantor-Graae, Nordstrom and McNeil2001) | Lifetime misuse | No |
| Cantwell et al (Reference Cantwell, Brewin and Glazebrook1999) | 12-month misuse | No |
| Carr et al (Reference Carr, Lewin and Barnard2002) | Lifetime misuse, 12-month use | No |
| Chouljian et al (Reference Chouljian, Shumway and Balancio1995) | Current misuse | No |
| Claassen et al (Reference Claassen, Gilfillan and Orsulak1997) | Urine test | No |
| Condren et al (Reference Condren, O'Connor and Browne2001) | Lifetime misuse | No |
| DeQuardo et al (Reference DeQuai do, Carpenter and Tandon1994) | Lifetime misuse | No |
| Dervaux et al (Reference Dervaux, Bayle and Laqueille2001) | Lifetime misuse | No |
| Diwan et al (Reference Diwan, Castine and Pomerleau1998) | Current use, lifetime use | No |
| Dixon et al (Reference Dixon, Haas and Wieden1991) | Lifetime misuse | No |
| Duke et al (Reference Duke, Pantelis and McPhillips2001) | Current use, lifetime use | No |
| Fowler et al (Reference Fowler, Carr and Carter1998) | Current use and misuse, urine test, lifetime use and misuse | Yes |
| Gearon et al (Reference Gearon, Bellack and Rach Beisel2001) | Lifetime misuse | No |
| Graham et al (Reference Graham, Maslin and Copello2001) | 12-month use and misuse | Yes |
| Gut-Fayand et al (Reference Gut-Fayand, Dervaux and Olie2001) | Lifetime misuse | Yes |
| Hambrecht & Häfner (Reference Hambrecht and Hafner1996) | Lifetime misuse | No |
| Jablensky et al (Reference Jablensky, McGrath and Herman2000) | Lifetime use and misuse | No |
| Kamali et al (Reference Kamali, Kelly and Gervin2000) | Current misuse, lifetime misuse | No |
| King et al (Reference King, Coker and Leavey1994)1 | Urine test, lifetime use | No |
| Kirkpatrick et al (Reference Kirkpatrick, Amador and Flaum1996) | Current use and misuse, lifetime use and misuse | No |
| Kovasznay et al (Reference Kovasznay, Fletcher and Tanenberg-Karant1997) | Current use | No |
| Krausz et al (Reference Krausz, Haasen and Mass1996)1 | Lifetime use and misuse | No |
| Ley et al (Reference Ley, Jeffery and Ruiz2002) | Urine test | No |
| Martinez-Arevalo et al (Reference Martinez-Arevalo, Calcedo-Ordonez and Varo-Prieto1994) | Current use, lifetime use | No |
| Mathers et al (Reference Mathers, Ghodse and Caan1991)1 | Urine test, lifetime use | No |
| McCreadie (Reference McCreadie2002) | Lifetime misuse, 12-month use and misuse | No |
| McGuire et al (Reference McGuire, Jones and Harvey1994) | Urine test | No |
| Menezes et al (Reference Menezes, Johnson and Thornicroft1996) | Lifetime use, 12-month use and misuse | No |
| Modestin et al (Reference Modestin, Nussbaumer and Angst1997)1 | Current use, urine test | No |
| Mueser et al (Reference Mueser, Yarnold and Levinson1990) | Current and lifetime misuse | No |
| Mueser et al (Reference Mueser, Yarnold and Bellack1992) | Lifetime misuse | No |
| Mueser et al (Reference Mueser, Yarnold and Rosenberg2000) | Lifetime misuse | No |
| Negrete & Gill (Reference Negrete, Gill, Nahas, Sutin and Harvey1999) | Current use and misuse | No |
| Núñez & Gurpegui (Reference Nunez and Gurpegui2002) | Urine test | No |
| Peralta & Cuesta (Reference Peralta and Cuesta1992) | 12-month misuse | No |
| Rabinowitz et al (Reference Rabinowitz, Bromet and Lavelle1998) | Lifetime misuse | No |
| Sembhi & Lee (Reference Sembhi and Lee1999) | Current and lifetime use, urine test | No |
| Sevy et al (Reference Sevy, Robinson and Solloway2001) | Lifetime misuse | Yes |
| Shaner et al (Reference Shaner, Khalsa and Roberts1993) | Current misuse | No |
| Shumway et al (Reference Shumway, Chouljian and Hargreaves1994) | 12-month use | No |
| Sokolski et al (Reference Sokolski, Cummings and Abrams1994) | Lifetime misuse | No |
| Soyka et al (Reference Soyka, Albus and Kathmann1993) | Current and lifetime misuse | No |
| Steadman et al (Reference Steadman, Mulvey and Monahan1998) | Current and lifetime use | No |
| Veen et al (Reference Veen, Selten and Hoek2002) | Current and lifetime use, 12-month misuse | No |
| Verdoux et al (Reference Verdoux, Gonzales and Assens1999) | Current use, lifetime misuse, urine test | No |
| Warner et al (Reference Warner, Taylor and Wright1994) | Current and lifetime use | No |
| Wolford et al (Reference Wolford, Rosenberg and Drake1999) | Urine test | No |
| Wright et al (Reference Wright, Gournay and Glorney2001) | Current misuse, lifetime and 12-month use | No |
| Zaretsky et al (Reference Zaretsky, Rector and Seeman1993)1 | Current use | No |
| Ziedonis & Trudeau (Reference Ziedonis and Trudeau1997) | Current misuse | No |
Table 2 Prevalence of cannabis use as a weighted average
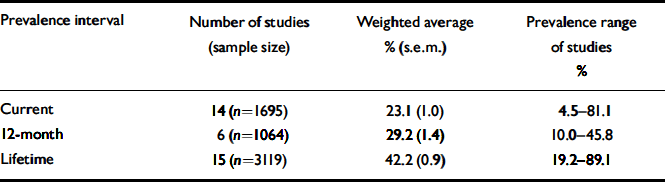
| Prevalence interval | Number of studies (sample size) | Weighted average % (s.e.m.) | Prevalence range of studies % |
|---|---|---|---|
| Current | 14 (n=1695) | 23.1 (1.0) | 4.5-81.1 |
| 12-month | 6 (n=1064) | 29.2 (1.4) | 10.0-45.8 |
| Lifetime | 15 (n=3119) | 42.2 (0.9) | 19.2-89.1 |
Table 3 Prevalence of cannabis misuse as a weighted average
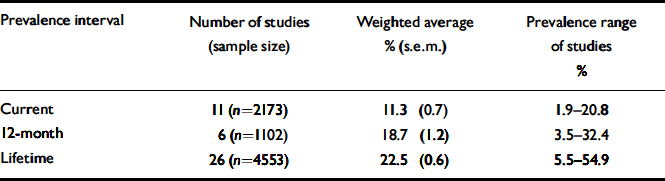
| Prevalence interval | Number of studies (sample size) | Weighted average % (s.e.m.) | Prevalence range of studies % |
|---|---|---|---|
| Current | 11 (n=2173) | 11.3 (0.7) | 1.9-20.8 |
| 12-month | 6 (n=1102) | 18.7 (1.2) | 3.5-32.4 |
| Lifetime | 26 (n=4553) | 22.5 (0.6) | 5.5-54.9 |
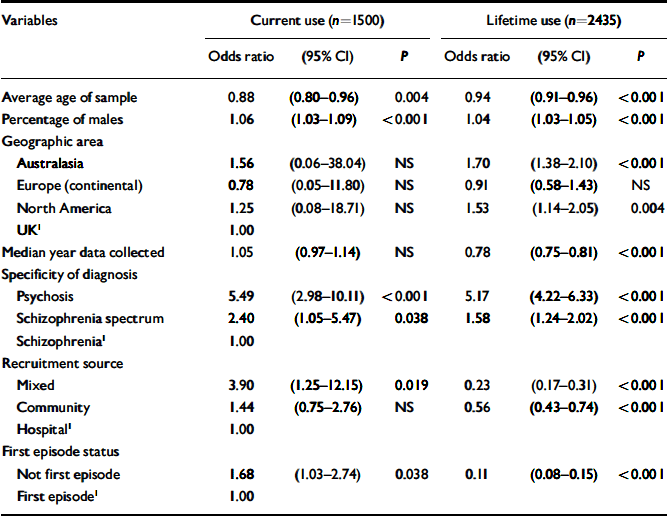
Table 4 Multinomial logistic regression of variables associated with cannabis use
| Variables | Current use (n=1500) | Lifetime use (n=2435) | ||||
|---|---|---|---|---|---|---|
| Odds ratio | (95% CI) | P | Odds ratio | (95% CI) | P | |
| Average age of sample | 0.88 | (0.80-0.96) | 0.004 | 0.94 | (0.91-0.96) | <0.001 |
| Percentage of males | 1.06 | (1.03-1.09) | <0.001 | 1.04 | (1.03-1.05) | <0.001 |
| Geographic area | ||||||
| Australasia | 1.56 | (0.06-38.04) | NS | 1.70 | (1.38-2.10) | <0.001 |
| Europe (continental) | 0.78 | (0.05-11.80) | NS | 0.91 | (0.58-1.43) | NS |
| North America | 1.25 | (0.08-18.71) | NS | 1.53 | (1.14-2.05) | 0.004 |
| UK1 | 1.00 | |||||
| Median year data collected | 1.05 | (0.97-1.14) | NS | 0.78 | (0.75-0.81) | <0.001 |
| Specificity of diagnosis | ||||||
| Psychosis | 5.49 | (2.98-10.11) | <0.001 | 5.17 | (4.22-6.33) | <0.001 |
| Schizophrenia spectrum | 2.40 | (1.05-5.47) | 0.038 | 1.58 | (1.24-2.02) | <0.001 |
| Schizophrenia1 | 1.00 | |||||
| Recruitment source | ||||||
| Mixed | 3.90 | (1.25-12.15) | 0.019 | 0.23 | (0.17-0.31) | <0.001 |
| Community | 1.44 | (0.75-2.76) | NS | 0.56 | (0.43-0.74) | <0.001 |
| Hospital1 | 1.00 | |||||
| First episode status | ||||||
| Not first episode | 1.68 | (1.03-2.74) | 0.038 | 0.11 | (0.08-0.15) | <0.001 |
| First episode1 | 1.00 | |||||
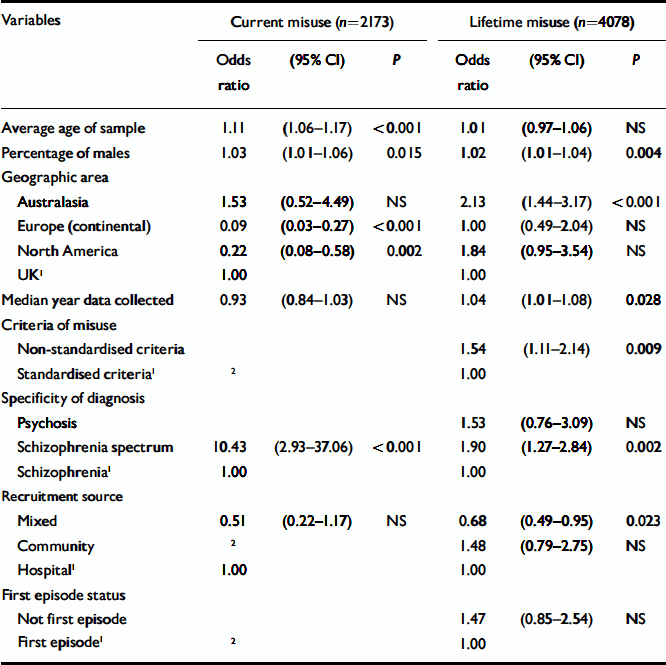
Table 5 Multinomial logistic regression of variables associated with cannabis misuse
| Variables | Current misuse (n=2173) | Lifetime misuse (n=4078) | ||||
|---|---|---|---|---|---|---|
| Odds ratio | (95% CI) | P | Odds ratio | (95% CI) | P | |
| Average age of sample | 1.11 | (1.06-1.17) | <0.001 | 1.01 | (0.97-1.06) | NS |
| Percentage of males | 1.03 | (1.01-1.06) | 0.015 | 1.02 | (1.01-1.04) | 0.004 |
| Geographic area | ||||||
| Australasia | 1.53 | (0.52-4.49) | NS | 2.13 | (1.44-3.17) | <0.001 |
| Europe (continental) | 0.09 | (0.03-0.27) | <0.001 | 1.00 | (0.49-2.04) | NS |
| North America | 0.22 | (0.08-0.58) | 0.002 | 1.84 | (0.95-3.54) | NS |
| UK1 | 1.00 | 1.00 | ||||
| Median year data collected | 0.93 | (0.84-1.03) | NS | 1.04 | (1.01-1.08) | 0.028 |
| Criteria of misuse | ||||||
| Non-standardised criteria | 1.54 | (1.11-2.14) | 0.009 | |||
| Standardised criteria1 | 2 | 1.00 | ||||
| Specificity of diagnosis | ||||||
| Psychosis | 1.53 | (0.76-3.09) | NS | |||
| Schizophrenia spectrum | 10.43 | (2.93-37.06) | <0.001 | 1.90 | (1.27-2.84) | 0.002 |
| Schizophrenia1 | 1.00 | 1.00 | ||||
| Recruitment source | ||||||
| Mixed | 0.51 | (0.22-1.17) | NS | 0.68 | (0.49-0.95) | 0.023 |
| Community | 2 | 1.48 | (0.79-2.75) | NS | ||
| Hospital1 | 1.00 | 1.00 | ||||
| First episode status | ||||||
| Not first episode | 1.47 | (0.85-2.54) | NS | |||
| First episode1 | 2 | 1.00 | ||||
The third analysis compared prevalence estimates among individuals with and without psychosis in community population studies. Uncorrected odds ratios were calculated for epidemiological studies using data provided by the respective study authors. All analyses were performed using the Statistical Package for the Social Sciences, version 10.
RESULTS
Cannabis use and misuse prevalence estimates from treatment samples
Tables 2 and 3 display prevalences of current, 12-month and lifetime cannabis use and misuse, respectively. Few studies have examined use and misuse in the same study. The average percentage of people using cannabis whose use was classified as ‘misuse’ was 42.9% for current use, 44.7% for 12-month use and 53.5% for lifetime use. Most studies reporting the prevalence of cannabis misuse did not distinguish between misuse and dependence (see Table 1). Of the four studies that provided data on misuse and dependence, three reported that over 75% of those with cannabis misuse met the criteria for misuse, rather than dependence. In contrast, the fourth study reported that 78.6% of patients with lifetime use and 68.0% of those with current use were diagnosed with dependence rather than misuse. The age and gender compositions of this latter study and the other community-based study with misuse–dependence data were similar. However, the study diagnoses were based, respectively, on data collected by a trained research assistant who administered the structured clinical interview for DSM–III–R, and on ratings made by key-workers on scales based on DSM–IV criteria.
Studies that used criteria from a standardised classification system reported a prevalence of 22.1% for lifetime misuse and 19.1% for 12-month misuse. The respective prevalence rates for lifetime misuse and 12-month misuse reported by the studies that did not use criteria from a standardised classification system were 25.4% and 17.7%. All studies reporting current misuse had used criteria from a standardised classification system (e.g. DSM or ICD) to make this diagnosis.
Prevalence estimates obtained from urine testing of treatment samples
The prevalence of cannabis use detected by urine testing was 12.3% (s.e.m.=0.9). This was based on a sample of 1460 pooled from 12 studies. Information on the cut-off criteria used to determine the presence of cannabinoids in urine was reported in only seven of the available studies. Criteria ranged from 20 ng/ml to 100 ng/ml. The respective percentages of positive urine tests were 12.0% at 20 ng/ml (three studies), 31.4% at 35 ng/ml (one study), 14.6% at 50 ng/ml (one study) and 10.0% at 100 ng/ml (two studies).
Multivariate analysis
The results of the multinomial logistic regression are reported in Tables 4 and 5. Variables were initially entered in the following order: recruitment source, geographic area, use of standardised substance misuse classification criteria, specificity of diagnosis of psychosis, and first-episode status. Average age of the study samples, percentage of males in a study and the median year of data collection for each study were covariates. The largest odds were consistently associated with a broader diagnosis of psychosis (e.g. psychosis or schizophrenia-spectrum disorder compared with schizophrenia). The significance levels obtained for each of the four models indicated that the independent variables significantly contributed to each model, but they were weak predictors as indicated by the resulting McFadden statistics (ranged from 0.019 to 0.155) which are analogues of R 2 (Reference MenardMenard, 2001). Each analysis obtained a statistically significant model chi-square.
Cannabis use and misuse prevalence in epidemiological studies
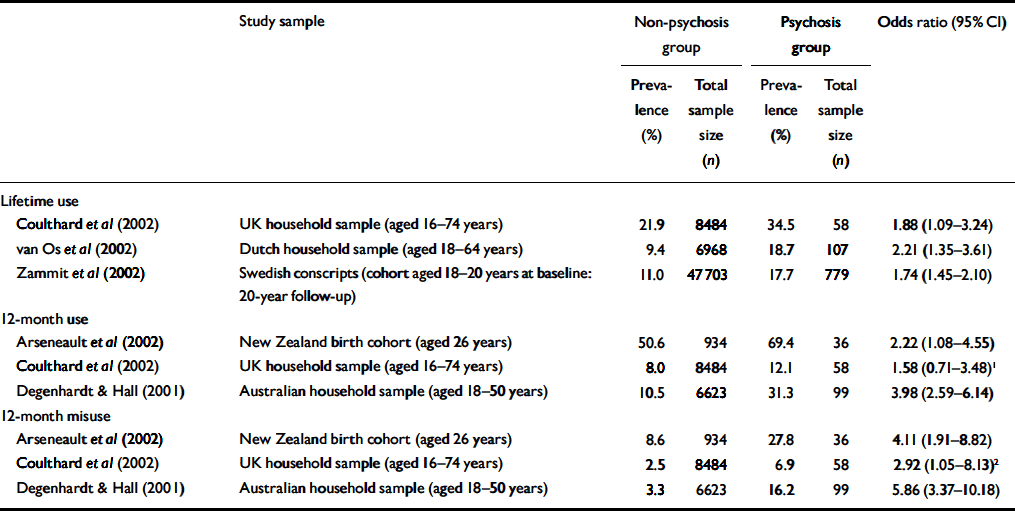
Table 6 lists the prevalence estimates obtained from epidemiological studies. All the studies showed higher odds of cannabis use or misuse for people with psychosis. The lifetime use estimates (Reference van Os, Bak and Hanssenvan Os et al, 2002; Reference Zammit, Allebeck and AndreassonZammit et al, 2002) were lower than the lifetime use estimates in any study reported in Table 2. The 12-month prevalence use and misuse estimates for the psychosis group in the Degenhardt & Hall (Reference Degenhardt and Hall2001) study are comparable to the estimates in Tables 2 and 3.
Table 6 Prevalence of cannabis use and misuse estimates from epidemiological studies
| Study sample | Non-psychosis group | Psychosis group | Odds ratio (95% CI) | |||
|---|---|---|---|---|---|---|
| Prevalence (%) | Total sample size (n) | Prevalence (%) | Total sample size (n) | |||
| Lifetime use | ||||||
| Coulthard et al (Reference Coulthard, Farrell and Singleton2002) | UK household sample (aged 16-74 years) | 21.9 | 8484 | 34.5 | 58 | 1.88 (1.09-3.24) |
| van Os et al (Reference van Os, Bak and Hanssen2002) | Dutch household sample (aged 18-64 years) | 9.4 | 6968 | 18.7 | 107 | 2.21 (1.35-3.61) |
| Zammit et al (Reference Zammit, Allebeck and Andreasson2002) | Swedish conscripts (cohort aged 18-20 years at baseline: 20-year follow-up) | 11.0 | 47703 | 17.7 | 779 | 1.74 (1.45-2.10) |
| 12-month use | ||||||
| Arseneault et al (Reference Arseneault, Cannon and Poulton2002) | New Zealand birth cohort (aged 26 years) | 50.6 | 934 | 69.4 | 36 | 2.22 (1.08-4.55) |
| Coulthard et al (Reference Coulthard, Farrell and Singleton2002) | UK household sample (aged 16-74 years) | 8.0 | 8484 | 12.1 | 58 | 1.58 (0.71-3.48)1 |
| Degenhardt & Hall (Reference Degenhardt and Hall2001) | Australian household sample (aged 18-50 years) | 10.5 | 6623 | 31.3 | 99 | 3.98 (2.59-6.14) |
| 12-month misuse | ||||||
| Arseneault et al (Reference Arseneault, Cannon and Poulton2002) | New Zealand birth cohort (aged 26 years) | 8.6 | 934 | 27.8 | 36 | 4.11 (1.91-8.82) |
| Coulthard et al (Reference Coulthard, Farrell and Singleton2002) | UK household sample (aged 16-74 years) | 2.5 | 8484 | 6.9 | 58 | 2.92 (1.05-8.13)2 |
| Degenhardt & Hall (Reference Degenhardt and Hall2001) | Australian household sample (aged 18-50 years) | 3.3 | 6623 | 16.2 | 99 | 5.86 (3.37-10.18) |
The standard reference on cannabis misuse prevalence in the community among people with schizophrenia is the Epidemiologic Catchment Area study (Reference Regier, Farmer and RaeRegier et al, 1990). The unweighted prevalence of a lifetime DSM–III cannabis misuse diagnosis among people with schizophrenia in this latter study was 19.7%, 13.4% in the household sample and a 36.2% prevalence in the institutional sample (D. Rae, personal communication, 2002).
DISCUSSION
A systematic review of published studies found that the prevalence of misuse of cannabis was approximately half that of its use, and that 12-month misuse prevalence provided a sound indication of lifetime misuse prevalence. Current misuse prevalence displayed the least variation across studies. These estimates provide a benchmark to evaluate prevalence reported in subsequent research, as well as to assist with decisions regarding the selection of appropriate prevalence intervals. The prevalence estimates were based on a total sample that was larger than has previously been reported.
Study recruitment source
We found no consistent pattern of increased or decreased odds associated with recruitment source, although analysis of epidemiological data indicated a consistent pattern of increased odds of cannabis use and misuse associated with psychosis. Despite different study designs, the prevalence estimates obtained for people with psychosis from the epidemiological studies were consistently higher than the estimates for non-psychosis samples. Although the low lifetime prevalence use in the Swedish birth cohort study (Reference Zammit, Allebeck and AndreassonZammit et al, 2002) could be attributed to the fact that the data were collected in 1969–70, the prevalence estimate was similar to the Dutch household study (Reference van Os, Bak and Hanssenvan Os et al, 2002) which collected data in 1996. The lifetime prevalence in the latter study was almost half the current use prevalence reported in a population-based first-incidence Dutch psychosis study (Reference Veen, Selten and HoekVeen et al, 2002). Given that cannabis is readily available in The Netherlands, the low lifetime prevalence reported in the epidemiological study supports the hypothesis that prevalence estimates may be inflated in clinical samples. In contrast, the Australian household study (Reference Degenhardt and HallDegenhardt & Hall, 2001) obtained 12-month prevalence estimates similar to those reported in Tables 2 and 3.
Epidemiological studies have important advantages over clinical samples in relation to sample size and representativeness; however, with the exception of the Swedish birth cohort study (Reference Zammit, Allebeck and AndreassonZammit et al, 2002), the number of people in the epidemiological studies with psychosis was relatively small. Additionally, across the studies there was variation in the methods used and clinical experience of the researchers employed to identify individuals with psychosis.
In relation to treatment samples, only two studies provided prevalence estimates for samples from different sources (Reference Soyka, Albus and KathmannSoyka et al, 1993; Reference Carr, Lewin and BarnardCarr et al, 2002). In the earlier study differences in the prevalence estimates might be accounted for by differences in admission criteria and functions of the hospitals, and the fact that the university sample had a significantly lower percentage of males – indeed, the lowest percentage of males of any study reviewed.
Diagnostic criteria and data collection
The most consistent finding across the multivariate analyses was the increased odds associated with a broader diagnosis (e.g. psychosis compared with schizophrenia). This suggests that a fundamental criterion for inclusion in a study might account for some of the variation in prevalence estimates. One explanation for the increased odds associated with the broader diagnosis of psychosis is the possible inclusion of individuals with drug-induced psychoses.
The criteria for diagnosing substance misuse could only be examined for lifetime misuse, as all studies of current misuse had adopted some form of standardised criteria. It was originally intended to examine prevalence in terms of the method used to diagnose substance misuse; however, the diversity of approaches in reviewed studies (e.g. the use of some questions from structured interviews within clinical interviews) made categorising studies using this criterion problematic.
Differences in prevalence have been accounted for by both criteria and information variance (Reference KlermanKlerman, 1985). The importance of considering the criteria used comes from a study that compared substance use diagnoses in a first-episode patient sample made by a research team with those made by clinicians. The research team and clinicians diagnosed cannabis use disorder in 8.5% and 33.3% of the patients respectively. Generally, disagreement was attributed to differences in applying diagnostic criteria rather than differences in the information that was available (Reference Fennig, Naisberg-Fennig and CraigFennig et al, 1996). In contrast, the differences in prevalence estimates reported in the Epidemiologic Catchment Area and National Comorbidity Survey studies have been attributed to information variance (Reference Regier, Kaelber and RaeRegier et al, 1998; Reference Narrow, Rae and RobinsNarrow et al, 2002). This information variance was considered to be due to differences in the nature of interviews that were employed.
Study design has also been reported to affect disclosure of sensitive information (Reference Kessler, Wittchen, Abelson, Stone, Turkkan and BachrachKessler et al, 2000). Inconsistencies in reporting have been found to be greater among people using cocaine compared with those using cannabis, with inconsistent accounts of lifetime use more likely by people with lower levels of use (Reference Fendrich and Mackesy AmitiFendrich & Mackesy Amiti, 1995). Although the presence of underreporting can be difficult to determine, patient self-report has been found to accord with urine tests (Reference Fowler, Carr and CarterFowler et al, 1998) and collateral sources (Reference Carey and SimonsCarey & Simons, 2000). However, a study by Swartz et al (Reference Swartz, Swanson and Hannon2003) found that cannabis prevalence differed according to the method of data collection: self-report 9.4%, urine testing 6.4% and hair analysis 19.9%. The prevalence obtained by hair analysis is closest to the current use reported in Table 2.
Prevalence estimates obtained by urine testing raise two issues of interest. First, prevalence was not markedly lower when a higher cut-off criterion was used. Second, some studies noted that patients who reported cannabis use did not return a positive result (Reference Condren, O'Connor and BrowneCondren et al, 2001). A similar finding has been reported in relation to hair analysis (Reference Selten, Bosman and de BoerSelten et al, 2002). A factor accounting for the former finding and differences in prevalence is likely to be the frequency of cannabis use and the time interval from use to testing. At the 20 ng/ml cut-off level, infrequent cannabis users would on average be expected to test positive 2–3 days after cannabis use, whereas frequent users would on average test positive for 9–12 days (Reference Kelly and JonesKelly & Jones, 1992). Information on when testing was conducted (e.g. average days after admission), method of testing and cut-off criteria employed are necessary to evaluate more fully cannabis prevalence data based on urine testing.
Age and gender
Age was associated with slightly increased odds of misuse (current and lifetime) and decreased odds of use (current and lifetime); higher percentages of males in a study sample were associated with a small increase in odds of use and misuse across the prevalence intervals. Although two studies were identified that did not find differences in either age or gender between those using cannabis and other patients (Reference Peralta and CuestaPeralta & Cuesta, 1992; Reference Sembhi and LeeSembhi & Lee, 1999), a number of studies have found that cannabis use and misuse are associated with younger age (Mueser et al, Reference Mueser, Yarnold and Levinson1990, Reference Mueser, Yarnold and Rosenberg2000; Reference Mathers, Ghodse and CaanMathers et al, 1991; Reference Bersani, Orlandi and KotzalidisBersani et al, 2002; Reference Veen, Selten and HoekVeen et al, 2002) and being male (Mueser et al, Reference Mueser, Yarnold and Levinson1990, Reference Mueser, Yarnold and Bellack1992, Reference Mueser, Yarnold and Rosenberg2000; Reference Mathers, Ghodse and CaanMathers et al, 1991; Reference Negrete, Gill, Nahas, Sutin and HarveyNegrete & Gill, 1999; Reference Nunez and GurpeguiNúñez & Gurpegui, 2002; Reference Veen, Selten and HoekVeen et al, 2002). The findings from our review also suggest that the age and gender composition of study samples would be expected to contribute to variation in prevalence estimates across studies.
Year of data collection
No consistent association was found between prevalence and median year of data collection. A review by Cuffel (Reference Cuffel1992) reported an association between the year of data collection and alcohol or amphetamine use; in that review, more recent studies reported higher prevalence. The studies included by Cuffel were from the period 1960–1991 and there were insufficient studies on cannabis to examine this relationship. Our review included studies published between 1990 and 2002, which collected data between 1983 and 2002. It may be the case that more time is required to determine a temporal pattern, or that other factors may interact with time period, such as changes in cannabis availability.
An illustration of how prevalence estimates vary over time is illustrated by two US studies. The first study, which collected data between 1983 and 1986 (Reference Mueser, Yarnold and LevinsonMueser et al, 1990), reported a 40% lifetime prevalence of cannabis use. A subsequent study from the same area (Reference Mueser, Yarnold and BellackMueser et al, 1992) that collected data between 1986 and 1990 reported a lifetime prevalence of 15.7%. These findings need to be considered in the context of the decreasing use of cannabis reported in the USA in the 1980s and the increased use of cocaine in the same period (Reference Costa e SilvaCosta e Silva, 2002).
Geographic area
No consistent association was found between prevalence of use or misuse and geographic area. Where prevalence estimates vary by geographic area this may be due to factors such as drug availability or changing trends in drug preference, as well as preferences for different research designs.
Limitations of our study
A limitation of our review is that studies of varying methodologies and methodological rigour were combined. The impact of different methods on prevalence estimates is difficult to determine and requires further attention; the issue of study quality was addressed by only including studies that met the inclusion criteria, especially the requirement that adequate detail was available. Pooling studies from different countries and time periods may have been problematic; however, these variables were included in the logistic regression and specific prevalence estimates for these variables were provided separately.
Future research
This review produced cannabis prevalence estimates based on the most comprehensive data to date and systematically examined factors that might account for the variation in prevalence estimates across studies. The increased odds of cannabis use and misuse among the population-based studies supports the view that the high prevalence rates in treatment samples are not simply a sampling artefact. Among the treatment samples, specificity of the diagnosis of psychosis was the variable most consistently associated with increased odds of cannabis use or misuse. The percentage of male participants in the study samples was associated with a small increase in odds of use and misuse, whereas age was associated with increased odds of misuse and decreased odds of use. This was the one consistent difference between the use and misuse models. As the majority of variance in predicting use and misuse was not accounted for by the common methodological variables included in this review, a more finely grained examination of the impact of different data collection tools is required. It will be important to examine additional factors such as motivation, disorder severity, craving and consumption levels, which might account for continued cannabis use and misuse. Such research has both clinical and policy implications, particularly in countries with high prevalence estimates.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The high prevalence of cannabis use and misuse among people with psychosis does not appear to be an artefact of sampling.
-
▪ Least variability in prevalence estimates was found when current misuse was diagnosed using a standardised assessment approach.
-
▪ For urine testing to be an effective means of determining current use, issues such as the interval between use and testing, cut-off levels and method need to be considered.
LIMITATIONS
-
▪ Studies of varying methodologies and methodological rigour were combined.
-
▪ Pooling studies from different countries and time periods may be problematic.
-
▪ A more fine-grained approach to examining how data collection differed across studies was not undertaken.
Acknowledgements
The assistance of cited authors and their colleagues who provided supplementary information is acknowledged, as is the assistance of Scott Menard, who provided advice on logistic regression.











eLetters
No eLetters have been published for this article.