Abnormal illness behaviour was first described as abnormalities in care-eliciting behaviours and relationships with healthcare professionals (Reference PilowskyPilowsky, 1997). The concept has been further refined into somatising and factitious illness behaviour. It is also possible to exhibit abnormal illness behaviour by proxy, that is those who have the care of dependent others may present them to healthcare professionals as sick. The most common form of proxy abnormal illness behaviour occurs in mothers, and has been described by Meadow (Reference Meadow1977) as Munchhausen syndrome by proxy, with reference to the persistent help-seeking behaviour exhibited by these mothers. The preferred term for this behaviour is now factitious illness by proxy, which reflects the deceptive and self-induced aspect of the help-seeking behaviour.
The psychopathological origins of this behaviour are still unclear. There is evidence that an individual's early childhood experiences with parents unconsciously influence care-eliciting behaviours, both normal and abnormal. Attachment theory may be useful for understanding both normal and abnormal care-eliciting behaviours by mothers because it provides an account of both care-eliciting and caregiving as behavioural systems operating between parents and children (Reference BowlbyBowlby, 1980; Reference George and SolomonGeorge & Solomon, 1996). Attachment theory suggests that mothers with factitious illness by proxy have insecure mental representations of caregiving and care-eliciting relationships, and that unresolved psychological distress in response to previous childhood illness or loss is common in factitious illness by proxy (Reference Main, Hesse, Greenberg, Cichetti and CummingsMain & Hesse, 1990).
We assessed attachment representations in a case series of mothers with factitious illness by proxy, using a semistructured interview based on attachment theory.
METHOD
Eighty-five mothers were identified through referral for medico-legal assessment to K.B., who has developed a specialist practice in this area. The assessment was usually required for child protection purposes (civil cases) or for the criminal courts (in seven cases). In all but three cases, a court had established that the mother had carried out some sort of abnormal illness behaviour by proxy or that there were reasonable grounds for child protection intervention.
In relation to the family court hearings, the court appointed K.B. as a single joint expert (a single expert jointly instructed by all parties) in care proceedings. All but three mothers accepted the court's findings, although they sometimes disputed the extent of the harm or possible risk to the children, and they were opposed to their children being taken into care. For the seven criminal cases, K.B. was instructed by the defence, usually in relation to sentencing. All seven women had been convicted of manslaughter, grievous bodily harm or child cruelty; four received probation orders. Only one of these cases was the subject of disputed expert testimony, to our knowledge.
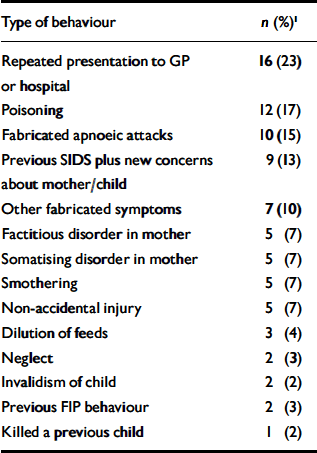
In terms of physical invasiveness, the behaviours ranged from inappropriate repeated presentation to a general practitioner (GP) to deliberate smothering or poisoning to induce medical symptoms in the child (see Table 1). In two cases, there was no new behaviour, but there was a history of previous factitious illness by proxy behaviour towards other children. In nine cases, there was a history of previous sudden infant death syndrome in addition to new factitious illness by proxy behaviour and/or concerns about the mother's parenting ability.
Table 1 Factitious illness by proxy (FIP) behaviours in 67 mothers
| Type of behaviour | n (%)1 |
|---|---|
| Repeated presentation to GP or hospital | 16 (23) |
| Poisoning | 12 (17) |
| Fabricated apnoeic attacks | 10 (15) |
| Previous SIDS plus new concerns about mother/child | 9 (13) |
| Other fabricated symptoms | 7 (10) |
| Factitious disorder in mother | 5 (7) |
| Somatising disorder in mother | 5 (7) |
| Smothering | 5 (7) |
| Non-accidental injury | 5 (7) |
| Dilution of feeds | 3 (4) |
| Neglect | 2 (3) |
| Invalidism of child | 2 (2) |
| Previous FIP behaviour | 2 (3) |
| Killed a previous child | 1 (2) |
Participants had a clinical psychiatric assessment with an experienced psychiatrist (K.B.), who also had access to psychiatric and general practice records. A subgroup of participants completed the Millon Clinical Multiaxial Inventory – III (MCMI–III; Reference MillonMillon, 1994), a personality assessment.
Potential participants were asked whether they would agree to an additional interview about their childhood experiences as well as the regular psychiatric examination. The results of this interview would inform the final report, although they would not be included in the report or submitted to the court. Assessment of a parent's own history of being cared for as a child is indicated as an essential part of assessment in child protection cases (Department of Health, 2000).
The interview used was the Adult Attachment Interview (AAI; Reference George, Kaplan and MainGeorge et al, 1994), which is a semi-structured interview, providing a detailed account of early care experiences. It has excellent psychometric properties when carried out and rated by trained professionals (Reference Hesse, Cassidy and ShaverHesse, 1999). K.B. is trained in the use of the AAI and carried out the interviews. These were taped and transcribed, and then sent for rating. K.B. was not involved in the rating of the interviews.
Transcripts were rated according to a manual. Raters undergo an extensive 2-week training and then complete a 30-case interrater reliability check. To qualify as a rater for research purposes, raters must achieve at least 80% interrater reliability. G.A. is trained as a rater.
Information from this interview was used to inform the conclusion of the final report and to make therapeutic recommendations. The mothers gave their consent to the use of anonymised material from these interviews, either directly or through their legal representatives.
Analysis
The AAI is rated using linguistic analysis of transcriptions of the taped interviews (Reference Hesse, Cassidy and ShaverHesse, 1999). This allows the rater to categorise the transcribed narratives as either (a) secure or insecure; or (b) insecure dismissing, insecure preoccupied or cannot classify. In addition, transcripts may also be categorised as either resolved or unresolved for traumatic experiences of loss or fear.
After transcription, each narrative was rated for both security and type of insecurity. The rating could not be done with complete masking, given the context, but the rater was not aware of the details of the allegations or established behaviours.
In addition to data collected from the AAI, data analysed included available demographic information, results of the MCMI–III personality assessment, and psychiatric diagnoses (based on clinical interview and examination of past records).
RESULTS
Eighty-five mothers completed the AAI. Five refused to take part in the research and three women's cases were not established as factitious illness by proxy behaviour. Ten interviews were lost in transcription. This left 67 transcripts for analysis.
The mean age of the mothers was 28 years and the mean age of the index child was 2.3 years. Most mothers (38, 55%) were in a partnership or married. Most children had siblings and no particular birth order was more common than another; 32 (53%) of the children were male.
Of the 67 mothers, 31 (46%) had histories of childhood trauma and 19 (28%) gave histories of adult trauma, usually rape or domestic violence; 30 mothers (45%) had histories of childhood illness or injury and 16 (24%) recalled a member of the family suffering from significant illness during their childhood; 36 mothers (54%) had experienced bereavement, either as adults or children.
Previous psychiatric diagnosis (based on case notes or GP records only)
Thirty-six mothers (52%) had histories of psychiatric treatment, either in childhood or adulthood, at the level of primary care only; 6 had histories of childhood psychiatric illness alone. The most common previous psychiatric diagnoses were somatising disorder (7) and eating disorders (7). Only 5 mothers had previous diagnoses of personality disorder, although 14 had demonstrated behaviours that might be associated with personality disorder, such as self-harm and/or taking overdoses.
Psychiatric diagnosis at interview
Based on the clinical assessment of mental state, only 12 mothers received any sort of diagnosis at interview (depression, 8; personality disorder, 4). None received a diagnosis of severe mental illness.
Psychological assessment
Thirty-nine participants completed the MCMI–III. One set of responses showed an invalid response pattern. Of the remaining 38, only in 9 cases (23%) were the scores indicative of definite personality disorder. Four out of those nine participants with a score indicative of personality disorder had profiles indicating borderline personality disorder. Seventeen women showed abnormally elevated personality traits, most commonly compulsive, dependent or histrionic traits. These women had also had psychiatric care in the past, and included those who had previously received a diagnosis of personality disorder. Twelve mothers showed no evidence of abnormal responses.
Attachment data
Secure or insecure
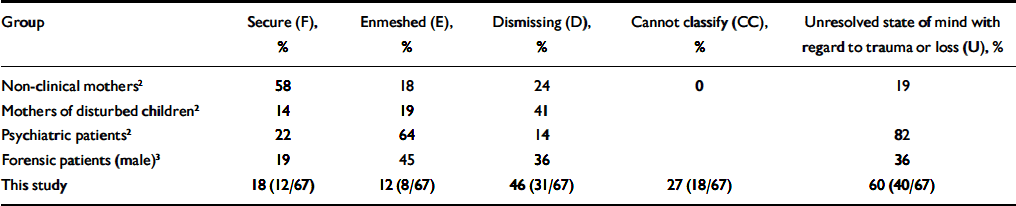
Fifty-seven (85%) of the transcripts were rated as insecure. The different categories of insecurity are described in Table 2, together with data from previously published studies of non-clinical samples, clinical samples, abusive mothers and offender groups.
Table 2 Adult Attachment Interview categories
| Group | Secure (F), % | Enmeshed (E), % | Dismissing (D), % | Cannot classify (CC), % | Unresolved state of mind with regard to trauma or loss (U), % |
|---|---|---|---|---|---|
| Non-clinical mothers2 | 58 | 18 | 24 | 0 | 19 |
| Mothers of disturbed children2 | 14 | 19 | 41 | ||
| Psychiatric patients2 | 22 | 64 | 14 | 82 | |
| Forensic patients (male)3 | 19 | 45 | 36 | 36 | |
| This study | 18 (12/67) | 12 (8/67) | 46 (31/67) | 27 (18/67) | 60 (40/67) |
The secure (F) category was underrepresented in our sample, which is not surprising given the prevalence of past psychiatric illness, personality abnormalities and childhood histories of divorce (7.3%) or maltreatment/neglect (51%). Our sample therefore resembles clinical groups, rather than normal mothers. It is perhaps surprising to find any secure mothers in this group.
Patterns of insecurity
Insecure–dismissing (D). This category was overrepresented in our sample. A similar excess of D representations is described in offender groups (Reference Fonagy, Target, Steele, Atkinson and ZuckerFonagy et al, 1997) and in parents who maltreat their children (Reference Crittenden, Partridge and ClaussenCrittenden et al, 1991). Individuals with a dismissing approach to attachments dismiss distress at times of illness, fear or loss, which may be associated with lack of empathy for others’ distress (Reference Fonagy, Target, Steele, Atkinson and ZuckerFonagy et al, 1997). There is a particular sub-class of dismissing attachment (Ds2), which is associated with fear of the loss of a child through death, and could theoretically give rise to excessive medical help-seeking behaviour. We did not find evidence of this subgroup in our sample.
Insecure–enmeshed (E). This category is underrepresented in our sample. Individuals with the E categorisation find it hard to see themselves as separate persons from their families of origin; the ‘enmeshment’ is with the attachment figures of childhood. Such individuals often have had over-close relationships with their own mothers or had to act as carers for their own parents. The E category has also been associated with borderline personality disorder, which has been described as common in factitious illness by proxy (Reference Bools, Neale and MeadowBools et al, 1994).
Insecure–cannot classify (CC). This categorisation indicates an attachment narrative that is highly disorganised. There are different ways for an attachment narrative to be rated as CC: the entire narrative may be grossly incoherent or the narrative may indicate that the individual exhibits a mixture of both D and E states of mind with regard to attachment (Reference Hesse, Cassidy and ShaverHesse, 1999). Participants in the CC category seemed unable to find any words to describe past relationships (although they were perfectly articulate in other areas). They were also unable to access any memories of their childhoods, and seemed to find the task alien and uninteresting.
Main & Hesse (Reference Main, Hesse, Greenberg, Cichetti and Cummings1990) suggested that CC mothers are both frightened and frightening as parents, which may then cause disorganisation of attachment in their children. Long-term follow-up studies of children with disorganised attachment have found that they often become either compulsive carers or controlling carers. Factitious illness by proxy behaviour could be considered both compulsive and controlling caregiving, and therefore as one manifestation of highly disorganised attachment in mothers.
Lack of resolution of psychological distress following trauma or loss (U). The AAI asks individuals about experiences of trauma and loss in childhood. Responses are rated for linguistic evidence of resolution of normal distress or evidence of abnormal distress. Ratings are made for both trauma (such as childhood abuse, carefully defined in the manual) and bereavement experiences. There was an excess of the unresolved (U) categorisation in our sample compared with both clinical and non-clinical groups, suggesting that these mothers may still be struggling with unresolved fear or grief reactions.
Loss or trauma experiences were common in our sample. Out of 40 mothers, 22 (55%) described experiences of either physical or sexual abuse or neglect in childhood; 19 described adult trauma such as domestic violence or rape; 25 (62.5%) had experienced bereavement, either in childhood or adulthood. These data are similar to those from the Great Ormond Street cohort (Reference Gray and BentovimGray & Bentovim, 1996).
Traumatic bereavement is the most common type of trauma that people are likely to experience (Reference Breslau and YehudaBreslau, 1998), and is defined as sudden, unexpected or violent bereavement. Given the comparatively young mean age of our participants (28 years), the prevalence of bereavement experiences seems high. For some, the fact that they were bereaved as children may have been traumatic; for others, the bereavement may have been traumatic because it involved a sudden death. Nine mothers had previously lost a child to sudden infant death syndrome. Two out of the nine had two previous children who had died of this syndrome. Some had experienced multiple bereavements in their lives or been bereaved when pregnant. The question raised by these data is whether the experience of bereavement led to a profound disorganisation of the attachment system for these mothers and contributed to the risk of this type of maltreatment.
DISCUSSION
Normal and abnormal illness behaviour
Illness behaviour is a term that refers to the ways individuals perceive, experience and respond to illness. Illness behaviour is influenced by individual, social and cultural experiences and constructions of illness, and may be subject to special expectations. For example, in Western cultures, those who are ill are expected to desire to get well, to comply with treatment and to seek help (or elicit care) appropriately (Reference ParsonsParsons, 1964). Although not specified, it may be assumed that proxy illness behaviour has the same expectations.
Factitious illness by proxy behaviour involves three forms of abnormal illness behaviour: false accounts of symptoms, fabricated symptoms and induction of symptoms (Reference BoolsBools, 1996). The last group is most dangerous and most likely to come to the attention of healthcare professionals. The few available cohort studies describe cases of more serious and life-threatening behaviours, resulting in referral to (and detection in) specialist centres (Reference Bools, Neale and MeadowBools et al, 1994; Reference Gray and BentovimGray & Bentovim, 1996; Reference Southall, Plunkett and BanksSouthall et al, 1997). The exact prevalence of this behaviour is unknown; the more severe forms are rare (0.5 per 100 000 children; Reference McClure, Davies and MeadowMcClure et al, 1996) and are associated with appreciable mortality, similar to other types of child abuse (Reference SheridanSheridan, 2003).
Meadow's original account stated that the mother's intention was to obtain attention to her own needs, and this is still his position (Reference MeadowMeadow, 2002). Other theorists have argued that it is a manifestation of a perverse relationship between mothers and doctors, or it is an extended form of self-harm (Reference SchreierSchreier, 2002). We suggest, based on our data, that the mother's own caregiving and care-eliciting behavioural systems have become disorganised, perhaps as a consequence of unresolved grief after bereavement or as one aspect of disordered personality. Personality disorder is a common diagnosis in perpetrators of child maltreatment generally (Reference Famularo, Kinscherff and FentonFamularo et al, 1992; Reference Dinwiddie and BucholzDinwiddie & Bucholz, 1993), and particularly in those with factitious illness by proxy (Reference Bools, Neale and MeadowBools et al, 1994).
We did not find a high prevalence of personality disorder in our group. This may be because we were not able to use a structured assessment measure of personality disorder in the whole group, and were able to use the MCMI–III in only half the sample. Our data suggest that abusive or risky behaviour is not synonymous with a diagnosis of personality disorder, and may be compatible with comparatively good mental health. Also, the attachment data may reflect an aspect of psychological functioning that is not measured by personality disorder assessment tools. Alternatively, if personality disorder is considered a disorder of interpersonal functioning, then perhaps it is possible for the disorder to be localised to one set of relationships – perhaps those characterised by disparities of vulnerability or those that have an attachment function. One might then think of these mothers as having a personality disorder confined to caring relationships; just as some men are only abusive or cruel in the context of marital relationships.
As expected, we did not find any connection between any one type of AAI classification and factitious illness by proxy behaviour. The illness behaviour is likely to be a ‘final common pathway’ of a generally unstable relationship between mother and child, and evidence of the mother's hostility to the child. The AAI categorisation can indicate only a general state of mind in relation to attachment relationships; it does not offer details of those relationships. This would come from more detailed analysis of the narratives, on which we are currently engaged. Why a mother would choose one type of behaviour over another is likely to be influenced by many factors, including unconscious symbolism and ease of access/opportunity. Our data support the general premise that there is no direct causal link between any single psychiatric diagnosis and complex behaviours that are deemed criminal or otherwise dangerous by the courts.
Illness behaviour and childhood care and attachment
Factitious illness by proxy might be better understood using the concept of ‘abnormal care-eliciting behaviours’. Mechanic (Reference Mechanic1978) described a number of different variables, both social and individual, associated with ‘normal’ care-eliciting behaviour. Henderson (Reference Henderson1974) first suggested that adverse childhood experiences of being cared for might explain ‘abnormal’ care-eliciting behaviour in adulthood, such as malingering or fabricating accounts of symptoms, and self-harming behaviours. Bools found a history of factitious disorder and somatising disorder to be more common in this group; hence the suggestion that the mothers themselves should be diagnosed as having factitious illness by proxy (Reference Bools, Neale and MeadowBools et al, 1994, Reference BoolsBools, 1996). In our series, a subgroup of the mothers did have apparent histories of somatising disorder, insofar as they either had been given that diagnosis in the past or their medical records strongly indicated such a disorder (repeated presentation for unexplained medical symptoms in themselves, as opposed to their children).
Somatising disorders are arguably another form of abnormal illness behaviour, in which individuals present to GPs and hospital medical services with medically unexplained symptoms. There is evidence that the experience of childhood illness and lack of parental care is associated with somatising disorders in adulthood (Reference Craig, Boardman and MillsCraig et al, 1993; Reference Hotopf, Mayou and WadsworthHotopf et al, 1999; Reference Craig, Cox and KleinCraig et al, 2002; Reference Crane and MartinCrane & Martin, 2002). One explanation for the abnormal caregiving behaviour in our study is that caregiving attitudes were disorganised by an experience of illness in childhood. Out of 67 mothers, 37 (55%) had experience of being ill as children and requiring either regular visits to the GP or hospital. A further 12 had experiences of a family member suffering illness when they were children. These experiences would have put them at risk of somatising disorder in adulthood.
The key question is how the experience of illness or poor care in childhood affects the capacity to care for others in adulthood. Mothers who have a secure attachment to their own parents are generally better able to provide good enough care for their children (Reference Van IJzendoornvan IJzendoorn, 1995). Mothers who provide poor care (in terms of neglect or maltreatment) are more likely to have insecure models of attachment than mothers who provide good enough care (Reference Crittenden, Partridge and ClaussenCrittenden et al, 1991). Somatising mothers have children with more health problems and with higher medical consultation rates than those of well mothers or organically ill mothers (Reference Craig, Cox and KleinCraig et al, 2002).
The fact that these mothers involve their children in abnormal illness behaviour suggests that their attachment to the children, and related capacity to care for them, has become disorganised. The argument that their experience of illness in childhood affects their proxy care-eliciting behaviours is consistent with the work of Craig et al (Reference Craig, Cox and Klein2002) on somatising mothers and research by Hill et al (Reference Hill, Murray and Woodhall2004), who found that a mother's experience of maternal care affected how she related to professionals involved in the care of her child's health.
It is reasonable to assume that factitious illness by proxy behaviours represent somatising disorder extended to the care of a child. This may be true for a minority but is unlikely to be a sufficient explanation; rather, somatising disorder in mothers may be a risk factor in some cases, if only because it indicates both personality pathology and heightened anxiety in relation to physical illness.
The mothers’ attachment styles
In terms of their attachment histories, the study group differs from non-clinical samples of normal mothers. They resemble clinical samples, with an excess of unresolved states of mind and CC transcripts. This supports the thesis that these mothers are in highly disorganised states of mind when they think about caring and being cared for in their own childhoods, and confirms that an attachment paradigm is reasonable for hypothesis generation and testing for this type of child maltreatment.
The excess of insecure attachment representations is in accordance with the Henderson hypothesis (Reference HendersonHenderson, 1974) that insecurity of attachment influences abnormal care-eliciting behaviour in adults, and with the now abundant evidence that early childhood experience of illness influences medical help-seeking behaviour, both for adults themselves and when they seek care on behalf of others (Reference Craig, Cox and KleinCraig et al, 2002). Our data are also consistent with evidence that attachment style influences general illness behaviour in both adults and children (Reference Feeney and RyanFeeney & Ryan, 1994; Reference Ciechanowski, Katon and RussoCiechanowski et al, 2001; Reference WilkinsonWilkinson, 2003).
The resemblance of our sample to a clinical group is striking, given that only a minority of participants received psychiatric diagnoses or (for those who completed the MCMI–III) showed abnormal personality traits. It is possible that standardised diagnostic interviews would have revealed more psychiatric pathology. However, only a minority had a previous psychiatric history, and these were usually those with clinical elevations on the MCMI–III. We suggest that these data show the complexity of the relationship between individual psychopathology and interpersonal behaviour within family groups. Forensic studies on offenders within the family make it clear that family violence is compatible with apparent psychiatric and psychological health. This suggests that better research tools are needed to understand abusive and exploitative relationships between intimates.
These data might also influence the advice we give to courts about mothers’ parenting abilities. Attachment history and representation seem to be more relevant to the capacity to care for children than psychopathology per se. This is consistent with previous research which suggests that mental illness does not always reduce the capacity to parent.
Unresolved distress and bereavement
We found high levels of unresolved distress in this group. The U categorisation is associated with mental illness and dysfunction in some studies (Reference Hesse, Cassidy and ShaverHesse, 1999). Although the prevalence of childhood abuse or neglect was similar in our sample to that in previous studies, the key issue psychologically is the degree to which the individual has come to terms with that experience mentally. If there is unresolved distress, then this can disorganise attachments to others and reduce parenting capacity as much as other types of psychological dysfunction. Unresolved distress in relation to trauma would certainly affect ability to care for a child, and has significant therapeutic implications. A subgroup of these women might benefit from interventions for post-traumatic stress symptomatology, such as cognitive–behavioural therapy, exposure therapy or antidepressant medication. Bereavement during pregnancy or in the first postnatal year might also significantly affect the mother's attachment to her own child, and this could be asked about routinely, so that therapeutic interventions could be offered.
Strengths and weaknesses of the study
There are no other studies to our knowledge that have examined attachment representations in individuals with abnormal illness behaviour by proxy. The main strength of the study is the large size of the sample. The nature of the behaviour (being both deceptive and illegal) has made it difficult to identify large samples of mothers for study. The Stafford group (Reference Southall, Plunkett and BanksSouthall et al, 1997) and the Bools group (Reference Bools, Neale and MeadowBools et al, 1994) both published clinical data on such mothers, but their sample sizes (for interview) were 33 and 17, respectively.
Our attachment-based interviews provide a wealth of data, not just about attachment representations, but also about the mothers’ experiences of their children, their fears, wishes and disappointments. The study's main weakness is the lack of a comparison group, allowing only limited inferences from our data. Insecurity of attachment is likely to be a risk factor for child maltreatment, prima facie, but it is only one among many and is unlikely to be either predictive or specific. The type of insecurity may be relevant, as may the nature of the experiences that give rise to that insecurity. This can only be explored with a comparison group and a prospective study. It is not clear which comparison group would be most effective. Eminson (Reference Eminson2000) argued that mothers with psychiatric illness and normal children are the most informative comparison group, whereas Meadow (Reference Meadow2000) suggested mothers of children with established physical illness. We agree with Meadow and are recruiting for such a study now.
It is also problematic to make inferences from mothers referred for forensic assessment. Clearly this leads to sampling bias in that only identified cases will be included, which are likely to overrepresent cases of perceived high risk to children. In terms of psychological mechanisms, it would be useful to have a comparison group of mothers who present with less extreme or harmful abnormal care-eliciting by proxy, although it is hard to see how these might be identified. Sampling bias could also be introduced in the choice of expert assessor, which is made partly by lawyers, but partly by family court judges. However, judges’ decisions are affected by factors independent of the assessor, such as pressure on court time and availability of other witnesses, and it is hard to see how this would affect the results.
It is possible that because all our participants were involved in legal proceedings of enormous personal significance, this made them more defensive in their interactions, and affected the coherence of the narrative discourse. This could only be assessed using a comparison group; for example, if the AAI were offered in the context of treatment for these women, this might produce different narratives. It is highly unlikely that any mother who had been detected in factitious illness by proxy behaviour would not face legal proceedings; using samples in which abnormal illness behaviour was merely suspected would be practically difficult and ethically problematic. It should also be noted that the preponderance of the dismissing category was found in other studies of attachment in forensic groups.
Our main finding is that mothers with factitious illness by proxy are more like a clinical group than not, and therefore are likely to have unmet treatment needs, which may be relevant to future risk. There is a dearth of facilities for psychological and psychiatric treatment of maltreating parents, unless families are likely to be reconciled (Reference JonesJones, 1987). Given the lack of resources, this discrimination is not unreasonable. However, all of the women in our study were of reproductive age, and in two cases there had been previous established factitious illness by proxy behaviour, which suggests that the behaviour might recur. We would argue for the development of psychological treatment services for all maltreating parents, to include psychological therapy, psychoeducational interventions and medication where appropriate, and an active approach to risk management. From our own clinical experience, we know that these women are people who need to deal with their rage, shame and hostility to their children if they are to be safe in the future.
Acknowledgements
This research was initially carried out with the support of a grant from the Peel Research Trust, developed during G.A.'s time as a University of Reading Health Research Fellow (2002–2004), and the report was prepared with the support of a grant from the Health Foundation. We acknowledge the support of Professors Lynne Murray and Peter Cooper, Winnicott Research Unit, University of Reading with previous drafts of this paper. We also thank colleagues at the Traumatic Stress Clinic and Camden and Islington Mental Health Trust, Denise Mitchell who transcribed many of the interviews and our secretaries, Anne Kavanagh and Pat Freeth.







eLetters
No eLetters have been published for this article.