‘The practitioner must choose. Shall he remain on the high ground where he can solve relatively unimportant problems according to prevailing standards of rigour, or shall he descend to the swamp of important problems and non-rigorous enquiry?’ (Reference SchönSchön, 1990, p. 3).
The 1990s saw a growing optimism about better outcomes in schizophrenia and related psychoses. This was encouraged by the advent of second-generation antipsychotic medications and a belief that a special focus on the early phases of illness could result in a substantial reduction in morbidity and better quality of life. The potential benefits of early intervention include: reduced morbidity; more rapid recovery; better prognosis; preservation of social skills, family and social supports; and decreased need for hospitalisation (Reference Birchwood, Todd and JacksonBirchwood et al, 1998).
A large number of clinical and research programmes focusing on early psychosis have now been established (Reference Edwards and McGorryEdwards & McGorry, 2002; Reference Nordentoft and McGorryNordentoft & McGorry, 2002). For example, in Australia and New Zealand there are networks and interest groups, strong and diverse service initiatives, conferences at state, national and international levels; there are considerable activities in Scandinavia, German-speaking countries, The Netherlands and major reform is underway in the UK; there are several early psychosis service initiatives in the USA; Canada has early psychosis programmes in most provinces, which have influenced mental health policy; there are first-episode psychosis (FEP) projects in Hong Kong and Singapore, and an Asian early psychosis network is planned.
There are three key elements in the management of early psychosis: early recognition and assistance, initial assessment and treatment, and promoting recovery (Reference McGorryMcGorry, 2002). The focus here is on the treatment of FEP, supporting the view that ‘detecting an illness early is of value only if effective treatment is readily available’ (Reference Falloon, Coverdale and LaidlawFalloon et al, 1998, p. 33). There are many studies on two related topics which will not be covered in this paper: the period of active psychosis prior to initiation of treatment, known as duration of untreated psychosis (DUP; Reference Norman and MallaNorman & Malla, 2001), and the prodromal period prior to the onset of FEP (Reference Heinssen, Perkins and AppelbaumHeinssen et al, 2001). The research and ethical considerations concerning DUP and prodrome initiatives are different from those surrounding FEP service development (see Reference Schaffner and McGorrySchaffner & McGorry, 2001; Reference Malla and NormanMalla & Norman, 2002; Reference Verdoux and CougnardVerdoux & Cougnard, 2003).
METHOD
Model multi-element services
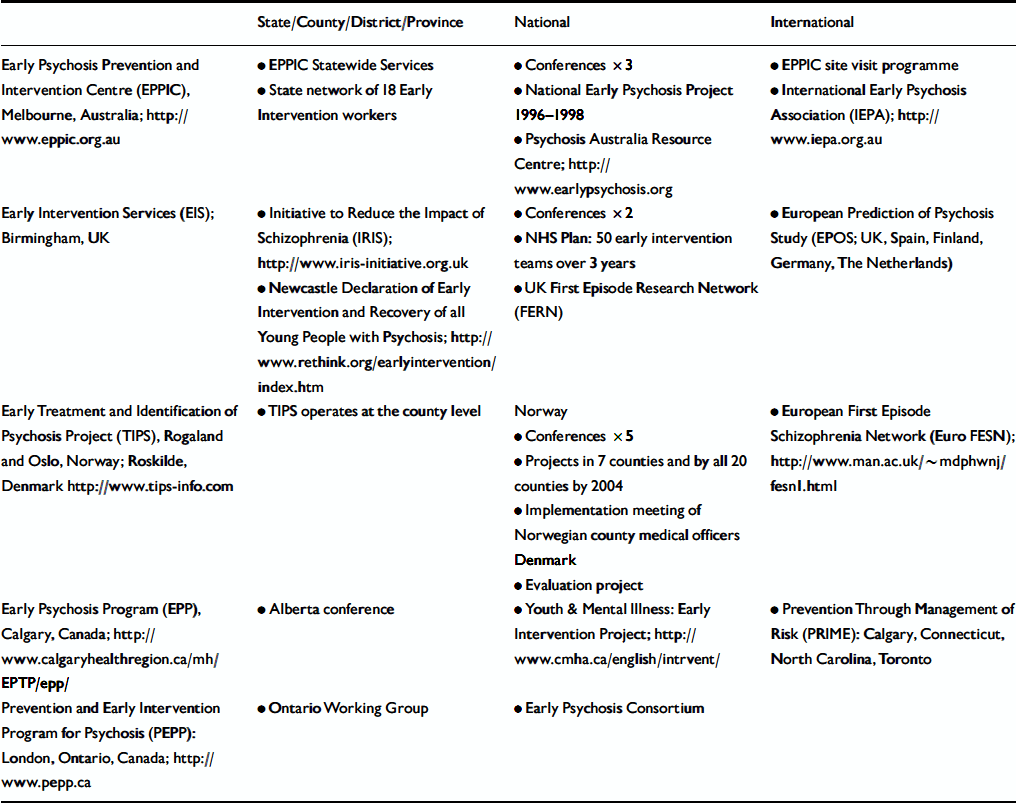
Table 1 lists five well-advanced multielement models of early intervention that focus on early detection and provision of optimal treatment, and are engaged in substantial clinical research (see Reference Edwards and McGorryEdwards & McGorry, 2002 for more extensive descriptions). Many other quality programmes exist; however, these five examples illustrate key features of FEP service development, and have been influential nationally and internationally, as summarised in Table 1.
Table 1 Five multi-element programmes of early intervention and their influences/linkages at regional, national and international levels
| State/County/District/Province | National | International | |
|---|---|---|---|
| Early Psychosis Prevention and Intervention Centre (EPPIC), Melbourne, Australia; http://www.eppic.org.au | • EPPIC Statewide Services | • Conferences × 3 | • EPPIC site visit programme |
| • State network of 18 Early Intervention workers | • National Early Psychosis Project 1996-1998 | • International Early Psychosis Association (IEPA); http://www.iepa.org.au | |
| • Psychosis Australia Resource Centre; http://www.earlypsychosis.org | |||
| Early Intervention Services (EIS); Birmingham, UK | • Initiative to Reduce the Impact of Schizophrenia (IRIS); http://www.iris-initiative.org.uk | • Conferences × 2 | • European Prediction of Psychosis Study (EPOS; UK, Spain, Finland, Germany, The Netherlands) |
| • Newcastle Declaration of Early Intervention and Recovery of all Young People with Psychosis; http://www.rethink.org/earlyintervention/index.htm | • NHS Plan: 50 early intervention teams over 3 years | ||
| • UK First Episode Research Network (FERN) | |||
| Early Treatment and Identification of Psychosis Project (TIPS), Rogaland and Oslo, Norway; Roskilde, Denmark http://www.tips-info.com | • TIPS operates at the county level | Norway | • European First Episode Schizophrenia Network (Euro FESN); http://www.man.ac.uk/∼mdphwnj/fesnl.html |
| • Conferences × 5 | |||
| • Projects in 7 counties and by all 20 counties by 2004 | |||
| • Implementation meeting of Norwegian county medical officers Denmark | |||
| • Evaluation project | |||
| Early Psychosis Program (EPP), Calgary, Canada; http://www.calgaryhealthregion.ca/mh/EPTP/epp/ | • Alberta conference | • Youth & Mental Illness: Early Intervention Project; http://www.cmha.ca/english/intrvent/ | • Prevention Through Management of Risk (PRIME): Calgary, Connecticut, North Carolina, Toronto |
| Prevention and Early Intervention Program for Psychosis (PEPP): London, Ontario, Canada; http://www.pepp.ca | • Ontario Working Group | • Early Psychosis Consortium |
The planning for the Early Psychosis Prevention and Intervention Centre (EPPIC) and the Early Treatment and Identification of Psychosis Project (TIPS) began in the 1980s, and underwent many years of development. A key aim of EPPIC is to progress innovative phase-oriented treatment of FEP within a specialist structure. TIPS delivers optimal treatment for schizophrenia, informed by the Patient Outcome Research Team (PORT) recommendations (Reference LehmanLehman et al, 1998), within a generic psychiatric setting and aims to shorten DUP through large-scale community education programmes. The Early Intervention Service (EIS) and the two Canadian models commenced in the mid 1990s, and like EPPIC, have therapeutic case management as a unifying framework in which cognitive–behavioural cognitive–behavioural interventions are offered, tailored to the needs of FEP (Reference BirchwoodBirchwood, 2003; Reference Gleeson and McGorryGleeson & McGorry, 2004).
The evolution and characteristics of each service need to be considered in terms of the local mental health service context. For example, EPPIC is located in a mental health services environment in which 24-h mobile assessment and treatment teams are mandated by the state government; Norwegian mental health services have a psychodynamic basis; and in Canada there is a strong emphasis on consumer- and family-led initiatives. EPPIC and the EIS lowered their upper age limit from 45 to 30 years, and EPPIC recently further reduced its upper age limit to 25, reflecting moves to youth service models. Both of these programmes accept patients with all psychotic disorders, whereas TIPS and the two Canadian programmes are restricted to non-affective psychosis and have a broader age range.
The five services have a number of features in common, including leadership by clinician–researchers who fulfil multiple roles (Reference Wasylenki and GoeringWasylenki & Goering, 1995). Their early development was shaped by needs analyses and pilot studies, local conferences to raise awareness of early intervention, and active dialogue with key representatives of other FEP services. They developed written statements of their philosophy and vision, and sought funding. The middle phase of development has been characterised by methodical documentation of their practices and procedures, and by collaborations with other services. On reaching maturity, the services have accumulated outcome data and attempted to influence mental health policy – Early Intervention Service/Initiative to Reduce the Impact of Schizophrenia (IRIS) with notable success.
Is specialised biopsychosocial treatment of FEP associated with better outcomes?
Despite the rapid expansion of early intervention initiatives for psychosis worldwide, supporting evidence from well-designed randomised controlled trials (RCTs) and planned, prospective comparison studies is still emerging. A key evaluation question to be addressed is whether specialised biopsychosocial treatment of first-episode psychosis, delivered at initiation of treatment for FEP, is associated with better outcomes. This section discusses key methodological challenges in FEP service evaluation, and describes emerging results from three current studies.
Evaluations of FEP programmes have included pre- and post-reports (e.g. Reference Malla, Norman and McLeanMalla et al, 2001; Reference Addington, Leriger and AddingtonAddington et al, 2003), historical comparisons (e.g. Reference McGorry, Edwards and MihalopoulosMcGorry et al, 1996; Reference Malla, Norman and ManchandaMalla et al, 2002), prospective comparisons (e.g. Reference Catts, O'Donnell, Spencer, Keshima, Falloon and MizunoCatts et al, 2002; Reference Cullberg, Levander and HolmqvistCullberg et al, 2002) and RCTs (e.g. Nordentoft et al, Reference Nordentoft, Jeppesen and Abel2002, Reference Nordentoft, Jeppesen and Petersen2003). There are clear advantages to the inclusion of comparison groups. However, in historical control group designs, the inability to control for factors that may influence outcome, such as changes in population and treatment characteristics over time, or variation in research procedures and instruments over time, may limit the usefulness of historical controls as comparison groups. Prospective cohorts are also subject to potential limitations, for example, where study cohorts differ on important baseline characteristics, such as severity of illness, or socio-economic status indicators.
Although RCTs have clear superiority over both historical and prospective designs, they are not without their difficulties. Key methodological issues for RCTs of FEP services include the implementation of criteria recommended by the Consensus Statement on Reporting of Trials statement, which is designed to improve the quality of reports of simple two-group parallel RCTs. Such recommendations include accounting for how the sample size was determined, providing an adequate description of randomisation procedures, attempting to mask assessors to treatment allocation (difficult to achieve in service evaluation research), and the need for analysis according to the intention-to-treat principle (Reference Moher, Shulz and AltmanMoher et al, 2001). In studies comparing treatment conditions, including RCTs, negative feelings of staff providing control treatments are a factor to be reckoned with (e.g., Reference Catts, O'Donnell, Spencer, Keshima, Falloon and MizunoCatts et al, 2002). In addition, the pragmatics and politics of withholding specialised FEP services from patients for the purposes of an RCT may be difficult to navigate. Potential issues include community concerns about changes to the availability of the existing treatment or service, and the response from other mental health services in the region whose practice may be directly affected by the requirements of the RCT design. These issues have been highlighted by recent preliminary investigations into the feasibility of undertaking an RCT within the EPPIC catchment area. These difficulties are not likely to be encountered if the service/project is a new development (e.g. Reference Nordentoft, Jeppesen and AbelNordentoft et al, 2002), however, new services may not have sufficient time to develop and document key interventions, ensure clinical skill development (Reference Catts, O'Donnell, Spencer, Keshima, Falloon and MizunoCatts et al, 2002) and high treatment integrity prior to the commencement of evaluation.
Recent studies
The Parachute Project in Sweden compared a group of patients treated within an experimental FEP treatment programme with prospective and historical FEP comparison groups. Seventeen Swedish psychiatric clinics covering a population of 1.5 million people were involved in the study. A total of 253 individuals with FEP aged 18–45 years were recruited between 1996 and 1997 and six key early psychosis treatment principles were applied. Assessments occurred at 1, 3 and 5 years. The 1-year follow-up of 175 patients (Reference Cullberg, Levander and HolmqvistCullberg et al, 2002) indicated that the experimental treatment group used fewer in-patient bed days than both the historical control and prospective control groups and received lower doses of neuroleptic medication than the historical control group. The Global Assessment of Functioning (GAF; Reference Endicott, Spitzer and FleissEndicott et al, 1976) score was significantly higher in the experimental group at 1-year follow-up compared with the historical control group (n=71) but was similar to the prospective comparison group (n=64). Patients and relatives indicated that they were largely satisfied with the care received through the Parachute intervention, however satisfaction ratings were not available for either of the comparison groups.
The OPUS project in Denmark had two components; the first compared one city with a FEP detection project with another providing usual practice to determine whether the DUP could be reduced; the second examined whether the provision of modified assertive community treatment leads to better course and outcome in young patients with schizophrenia-spectrum disorders compared with patients treated with standard care. Patients with FEP were randomised to standard treatment or integrated care (assertive community treatment, psychoeducational multi-family groups and social skills training) for 2 years. Principles of antipsychotic medication were similar in both groups. The 1-year follow-up of the first 341 participants demonstrated advantages for integrated treatment care: there was significantly less hopelessness, reduction in psychotic symptoms was greater, and clients and families were more satisfied with treatment (Nordentoft et al, Reference Nordentoft, Jeppesen and Abel2002, Reference Nordentoft, Jeppesen and Petersen2003). A 2-year follow-up is underway.
One of the potential limitations of the OPUS and Parachute projects is that the 18- to 45-year age bands used in both studies exclude the substantial proportion of individuals who have the onset of psychosis prior to 18 years of age (Reference Amminger, Harris and ElkinsAmminger et al, 2002) and consequently shifts the content of interventions away from youth issues. In addition, the specificity of the psychosocial components to FEP in OPUS is unclear. Methodological weaknesses of the Parachute study include differences in the sampling strategies, recruitment procedures, types of measures and information sources used across the three groups. Further, comparisons with the historical group in particular could be confounded by differences in treatment policies affecting patient resources and the availability of new and possibly more effective antipsychotic medication in the intervention group. However, on the positive side, Pelosi & Birchwood (Reference Pelosi and Birchwood2003) note that engagement of young people and their satisfaction with services should be key outcomes in developing services as ‘without this, even our best treatments have no chance of working and we risk getting caught up in a cycle of coercion’ (p. 197). The results of the Parachute and OPUS studies are encouraging in this regard.
One other RCT of an FEP service has just been completed. The Lambeth Early Onset (LEO) service in London (Reference Garety and JolleyGarety & Jolley, 2000; Reference Craig, Garety and PowerCraig et al, 2004) includes an 18-bed in-patient service and an assertive outreach team, treating 16 to 40-year-olds (the upper age limit has recently been lowered to 35 years) with schizophrenia-spectrum disorders in a catchment area of approximately 270 000. Patients were randomised at referral to the specialised service or standard care through pre-existing teams, and consent for research interviews and follow-up was sought from the patients after randomisation. The treatment involved psychological intervention, family work, assisting with education and employment, user involvement in the service, integrated care for dual diagnosis and optimal low-dose antipsychotic medications. Patients were assessed at 1 week, 6 months and 18 months. Primary outcome measures included rates of relapse and readmission to hospital. The specialised care group (n=71) experienced significantly lower rates of relapse and readmission compared with the standard care group (n=73), however, differences in rate of relapse became non-significant when group imbalances in gender, past episode and ethnicity were statistically adjusted. The difficulties in drawing firm conclusions due to relatively modest sample sizes is highlighted by the results of this study.
Emerging results from these and other studies currently in progress represent a considerable advance in the availability of evidence supporting the effectiveness of FEP programmes. However, they may be considered ‘first generation’ in the sense that the comprehensive service-level nature of interventions has rendered evaluation of scientific merit problematic; detailed treatment manuals were not available; and insufficient attention was paid to measuring treatment fidelity. The pace of early psychosis reform around the world demonstrates that once a convincing clinical rationale or evidence supporting a programme's effectiveness has been documented, the programme may be rapidly disseminated or replicated (Reference Paulson, Post and HerinckxPaulson et al, 2002). However, as outlined in the previous section of this paper, FEP programmes vary substantially, reflecting differences in underlying philosophies, objectives, service delivery model and local contextual factors. Thus, the package of interventions being evaluated needs to be well articulated and replicable, ideally reflected in detailed treatment manuals, and should adhere to current thinking in terms of best practice treatment for FEP. Further, the study should measure the extent to which core elements of the intervention are actually received on an individual patient basis. This information helps to ensure that the nature and quality of the interventions is explicit, and that valid conclusions can be drawn about the effectiveness of the FEP programmes. It also provides guidance as to whether the specific programme under study can be exported faithfully to another setting and be expected to achieve similar outcomes.
RESULTS
Efforts required to bridge the ‘high ground’ and the ‘swamp’
‘There is an especially large gap between clinical trial data and treatment recommendations for first first episode schizophrenia…. Evidence-based therapeutics depend on knowledgeable and wise clinicians to translate data into individualised treatment’ (Reference CarpenterCarpenter, 2001, pp. 1771–1773).
In addition to the ongoing need for studies that evaluate the complex intervention packages offered by FEP services, the early psychosis field now also needs RCTs using more highly specified interventions delivered in ‘real-world’ clinical settings. Few RCTs have been performed with individuals with FEP, particularly with regard to psychosocial components of treatment (e.g., Reference Linszen, Dingemans and LeniorLinszen et al, 2001; Reference Lewis, Tarrier and HaddockLewis et al, 2002). However, such interventions may be of particular value given the limitations and problems of biological treatments for FEP patients, such as low medication adherence rates, and prolonged recovery in a substantial proportion of patients (Reference Gleeson, Larsen and McGorryGleeson et al, 2003). Examples of the evaluation of specific aspects of clinical practice undertaken at EPPIC are described below.
Psychological therapies
The Early Psychosis Prevention and Intervention Centre has been developing manuals and support materials for psychoeducation, cognitively oriented psychotherapy for early psychosis (COPE; Reference Jackson, McGorry, Edwards, Corrigan and PennJackson et al, 2001; ACE; Reference Killackey, Jackson and BendallKillackey et al, 2002), cannabis use (CAP; Reference Hinton, Elkins and EdwardsHinton et al, 2002; Reference Edwards, Hinton, Elkins, Graham, Copello and BirchwoodEdwards et al, 2003), suicide prevention (Lifespan; Reference Power, Bell and MillsPower et al, 2003) and relapse prevention. COPE, ACE, CAP and Lifespan are each the subject of RCTs. These psychological approaches have been summarised within a case-management manual (EPPIC, 2001), which recognises the importance of low-dose second-generation antipsychotic medications (Reference Zipursky, Zipursky and SchulzZipursky, 2002) alongside psychosocial aspects of care.
Prolonged recovery
Early identification and specialised treatment of patients who do not achieve remission from FEP has the potential to accelerate the recovery process. The Treatment Resistance Early Assessment Team (TREAT) identifies individuals who are experiencing persisting positive and/or negative symptoms following their first or subsequent acute episode (Reference Edwards, Maude and Herrmann-DoigEdwards et al, 2002). It provides a consultancy service to case managers and doctors that aims to prevent established treatment resistance. Systematic Treatment of Persistent Psychosis (STOPP) is a psychological approach to facilitating recovery in young people experiencing enduring positive symptoms (Reference Edwards, Wade, Herrmann-Doig, Gleeson and McGorryEdwards et al, 2004).
Clozapine treatment and cognitive–behavioural therapies have achieved promising results in chronic schizophrenia. The relative and combined effects of clozapine and STOPP are being investigated in young people with FEP falling below a predefined level of remission after 12–26 weeks of initial treatment. The first phase of the study has been completed (n=48) and we are currently examining the results. Manuals detailing the TREAT (EPPIC, 2002) and STOPP (Reference Herrmann-Doig, Maude and EdwardsHerrmann-Doig et al, 2003) approaches have been developed.
Is developing FEP services justified?
‘Strictly speaking randomised controlled trials are still needed to confirm the effectiveness of early detection and intervention services. However, the testimony of patients and families, non-randomised evaluations of services such as those provided by EPPIC and obvious validity or common sense supports their wider introduction’ (Reference Lewis and DrakeLewis & Drake, 2001, p. 142).
Sceptics insist on definitive evidence before reform of FEP services is commenced (Reference WarnerWarner, 2001 – and replies by Reference McGorry and EdwardsMcGorry & Edwards, 2002; Reference WarnerWarner, 2002; Reference Pelosi and BirchwoodPelosi & Birchwood, 2003). However, many researchers, clinicians, patients and families believe that staged reform in practice and service provision is necessary, not just to improve care but also to enable further data to be collected.
Psychiatric service reform is a sociological and political process informed by scientific evidence, but evidence is not the only legitimate influence on the direction and pace of reform. Thornicroft & Tansella (Reference Thornicroft and Tansella1999) argue that complex planning choices in mental health should be informed by evidence-based medicine, but ‘counter-balanced by a principal ethical base, and in our view the primary responsibility for introducing clinical value to these decisions lies with clinicians’ (p. 141). The wide-spread introduction of case management in mental health services is an example of practice becoming established before evidence for efficacy was available (Reference Ziguras and StuartZiguras & Stuart, 2000).
Specifically, other factors that may influence the successful development and implementation of specialist FEP services include, but are not limited to, the prevailing political environment, advocacy efforts of consumer and carer groups and advocacy bodies, and the commitment of service providers to ensuring the presence of key service components essential to effective service provision for this target group.
Political environment
Central to the development of early psychosis services has been the political acknowledgement of the limitations of service provision to FEP clients within generic mental health service systems (e.g. Reference Yung, Organ and HarrisYung et al, 2003), supported by a commitment to funding early psychosis services. The UK has seen encouraging developments, with mental health nominated as one of three priority areas in the National Health Service (NHS) Plan 2000 (Department of Health, 2000). The Plan announced funding for 50 early intervention services for FEP to be established in England, and specified guidelines for the implementation of these services (Department of Health, 2001). In Australia, the Victorian state government's funding of the statewide Early Intervention Worker Initiative has been an important first step in addressing the specific needs of FEP clients on a broader scale. This initiative funds a mental health clinician embedded within primary mental health teams in each of Victoria's 21 geographically defined mental health regions. Their role focuses on early identification and treatment of FEP, and other serious mental disorders, in young people aged 16–25 years (Department of Human Services, 2000).
Advocacy
‘Early intervention does not simply involve “bringing forward” best practice to this early phase; it requires special care in recognition ofthe biological, psychological and familial challenges and changes that are active in this period’ (Reference Spencer, Birchwood and McGovernSpencer et al, 2001, p. 139).
Advocacy efforts by service providers, consumers and carers are playing a growing role in ensuring early psychosis service reform. The level of international support and advocacy for early intervention targeted to FEP is evident in the International Early Psychosis Association (IEPA) consensus statement (Reference Edwards and McGorryEdwards & McGorry, 2002). The statement identifies principles for addressing current deficiencies in preventive intervention, and proposes strategies to enhance clinical care. The statement was developed with input from 26 invited international consultants, subsequently ratified by the executive of the IEPA and presented at the Third International Conference on Early Psychosis (September 2002, Copenhagen).
The UK NHS Plan was influenced by lobbying from IRIS and the National Schizophrenia Fellowship, which advanced arguments about the poor quality of existing services, confused access points for FEP clients, the need for youth-friendly services and the potential benefits of early intervention in reducing the occurrence of secondary problems, such as school drop-out, unemployment, forensic issues and suicide.
The Early Psychosis Declaration (formerly the Newcastle Declaration) was developed in Newcastle upon Tyne by service users, family members and expert practitioners, in conjunction with representatives from the World Health Organization (WHO), Rethink and IRIS. The declaration identifies a set of expected standards of care for people experiencing early psychosis and their families. There are future plans for this document to be formally endorsed and released by the WHO and the IEPA. The declaration will also inform the work of the IEPA in developing a set of international quality indicators for early intervention services.
Carer advocacy efforts have played a strong role in ensuring the funding of a specific early psychosis service in Winnipeg, Canada (Reference LinesLines, 2002). In response to the lack of available specialist early psychosis services for their children, a group of family members launched a significant advocacy campaign targeted at policymakers, funding institutions and the general public. These advocacy efforts in partnership with local mental health clinicians have resulted in the financial support of EPPIS – the Early Psychosis Prevention and Intervention Service.
DISCUSSION
Worldwide there has been enormous growth and investment in early intervention in psychosis. Considerable progress has been made in terms of influencing practice in the assessment and treatment of early psychosis. There is an active network of clinicians and researchers working in this field who are willing to share information and resources, aiming to circumvent the tendency to ‘reinvent the wheel’ and propel FEP service developments forward. There remains a need for quality clinical and research efforts to inform and accelerate progress in this burgeoning field. Evidence from RCTs and other planned, prospective comparison studies is required to establish the effectiveness of early detection and intervention services for psychosis, and of phase-specific interventions. However, it should be acknowledged that scientific evidence is not the only driver of service reform; sociopolitical factors, including political pressure and community demand based on perceived gaps and deficiencies, are also potent forces.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ There are several well-advanced, multi-element models of early intervention in first-episode psychosis (FEP) that incorporate early detection, provision of optimal treatment and clinical research. These have influenced mental health policy and provide guidance to new service developments.
-
▪ The results from well-designed randomised controlled trials (RCTs) and planned, prospective studies are now emerging, providing evidence that specialised biopsychosocial treatment, delivered at initiation of treatment, is associated with improved course and outcome in FEP.
-
▪ Mental health service reform should be informed by scientific evidence, but is also influenced by sociopolitical factors, such as political pressure and community demand in response to perceived gaps and deficiencies in existing service systems.
LIMITATIONS
-
▪ Despite the rapid expansion of early psychosis initiatives, there remain evidence gaps in the evaluation of complex intervention packages and specific interventions for FEP.
-
▪ More RCTs examining the effectiveness of highly specified interventions, particularly psychosocial components of treatment, are needed to inform treatment recommendations and guide clinicians in providing individualised treatment to FEP patients.
-
▪ Failure to evaluate the treatment integrity of FEP interventions may impede the interpretation of results from effectiveness studies, and limit confidence in the replicability of interventions across different service environments.
Acknowledgements
Thanks to G. Paul Amminger, Giovanni de Girolamo, John Gleeson, Susy Harrigan and Patrick D. McGorry for reviewing earlier drafts of this paper.






eLetters
No eLetters have been published for this article.