Epidemiological studies have highlighted several factors that may be associated with an increased risk of suffering a severe post-partum episode of psychosis. These include: (a) primiparity, (b) pregnancy complications, (c) delivery complications, (d) Caesarean section, (e) female baby and (f) shorter gestation period (Kendell et al, Reference Kendell, Rennie and Clarke1981, Reference Kendell, Chalmers and Platz1987; Reference Paffenbarger, Brockington and KumarPaffenbarger, 1982). Findings are consistent only for primiparity. Here we compare deliveries, affected and unaffected by severe post-partum illness, within a sample of 129 women who have all experienced an episode of bipolar affective puerperal psychosis and explore whether any of the six risk factors listed above are linked to the development of the illness. By examining the affected and unaffected deliveries of these women, we are able to control for potential confounders that may have reduced power to identify associations in previous studies that relied on comparisons of unaffected and affected pregnancies cross-sectionally between samples of women with puerperal psychosis and controls.
METHOD
Recruitment
The ascertainment, recruitment and clinical assessment of the women in our sample are described in detail elsewhere (Reference Robertson, Jones and BenjaminRobertson et al, 2000). Briefly, women were recruited through a variety of sources, including mental health teams, Action on Puerperal Psychosis (a group which provides information about the illness and current research findings) and national and local publicity. Ethical approval was obtained prior to data collection and written informed consent was obtained from each participant.
The sample comprised 129 females born in the UK who were recruited for clinical and genetic studies of bipolar affective puerperal psychosis and who met the following inclusion criteria: (a) a lifetime diagnosis of DSM-IV bipolar I disorder or schizoaffective disorder (bipolar type; American Psychiatric Association, 1994); (b) recruitment for molecular genetic studies, UK/Eire White ethnicity; and (c) experience of a manic or affective psychotic episode within 4 weeks of childbirth (97% of women in our sample had an onset of puerperal illness beginning within 2 weeks of giving birth).
Assessment
All participants were interviewed by a trained psychologist or psychiatrist using the Schedules for Clinical Assessment in Neuropsychiatry (SCAN; Reference Wing, Babor and BrughaWing et al, 1990) and information was obtained from case notes. Consensus best-estimate ratings of episode and lifetime diagnoses, according to DSM-IV criteria (American Psychiatric Association, 1994), were made on the basis of all available clinical information by two independent investigators.
Pregnancies resulting in a miscarriage or termination were not included in the analysis, and there were no stillbirths to women in the sample. Obstetric complications were identified based on each woman's self-report of her delivery and supplemented with information from obstetric case notes where available. We reviewed the Royal College of Obstetricians and Gynaecologists' (2001) guidelines for clinical risk management in delivery and sought the opinions of clinical and academic obstetricians. On the basis of these, a complication during pregnancy was defined as a maternal or foetal medical condition severe enough to warrant treatment by the antenatal healthcare provider, either as an out-patient or through hospital admission.
Pregnancy complications included antepartum haemorrhage, gestational diabetes and pre-eclampsia. Delivery complications included breech presentation, foetal distress and cord accidents. Consensus ratings were made of obstetric complications by two independent researchers and a consultant obstetrician masked to outcome with respect to puerperal episodes of illness.
Statistical analysis
In order to compare differences between all deliveries to women in the sample that were affected and unaffected by puerperal psychosis, a repeated-measures stepwise logistic regression analysis (Reference AltmanAltman, 1991) was performed. It was necessary to account for the fact that multiple deliveries could come from one individual (and could not therefore be considered independent observations) by including a repeated-measures factor that indicated the individual participant involved. We also tested the association of categorical variables with the χ2 statistic and employed McNemar's test for categorical variables and Wilcoxon's matched pairs signed ranks test for continuous variables, to compare affected and unaffected deliveries in the set of women having both types of delivery outcome.
RESULTS
All of the 129 women, by definition of the inclusion criteria, had lifetime best-estimate consensus diagnoses of a bipolar-spectrum disorder according to DSM-IV criteria. The majority (84%, n=109) were diagnosed with bipolar I disorder; the remaining 20 (16%) were diagnosed with schizoaffective disorder (bipolar type). Clinical and demographic information is given in Table 1.
Table 1 Clinical and demographic information at the time of interview on the 129 women studied

| Variable | |
|---|---|
| Lifetime diagnosis, n (%) | |
| Bipolar I disorder | 109 (84) |
| Schizoaffective disorder (bipolar type) | 20 (16) |
| Age, years: mean (s.d.; range) | 40.0 (9.2; 19-69) |
| Age at first episode of puerperal psychosis, years: mean (s.d.; range) | 26.7 (5.2; 17-43) |
| Deliveries, n | 242 |
| Episodes of puerperal psychosis, n | 167 |
| Time since first episode of puerperal psychosis, years: | 11.1 (7.9; 0.5-32.5) |
| mean (s.d.; range) | |
| Marital status, n (%) | |
| Married/cohabiting | 98 (76) |
| Divorced/separated | 29 (22.5) |
| Single | 2 (1.6) |
| Employment status, n (%) | |
| Homemaker | 41 (31.8) |
| Employed | 71 (55) |
| Unemployed | 15 (11.6) |
| Student/retired | 2 (1.6) |
The mean age at the first episode of puerperal psychosis was 26.7 years (s.d.=5.2, range=17-43 years). There were 287 pregnancies for the 129 participants, of which 242 resulted in delivery. Of the 45 pregnancies that did not result in a full-term delivery, there were 30 miscarriages (a rate of 10% of all pregnancies, with 50% of miscarriages occurring in the first pregnancy), 14 terminations (all but one occurring prior to the index puerperal psychotic episode) and 1 ectopic pregnancy. The median number of pregnancies was 2 (range=1-6) and the median number of deliveries was 2 (range=1-6).
There was a total of 167 puerperal psychotic episodes for the 129 women. The majority of women experienced puerperal psychosis following their first delivery (106 out of 129, 82%); 93 women (72%) had one episode of puerperal psychosis as defined by the study criteria, 35 (27%) had two episodes and 1 woman (1%) had three episodes. The proportions of deliveries affected by the obstetric variables studied are shown in Table 2 - for all deliveries and for those affected and unaffected by puerperal psychosis.
Table 2 Proportion of deliveries affected by the obstetric variables studied
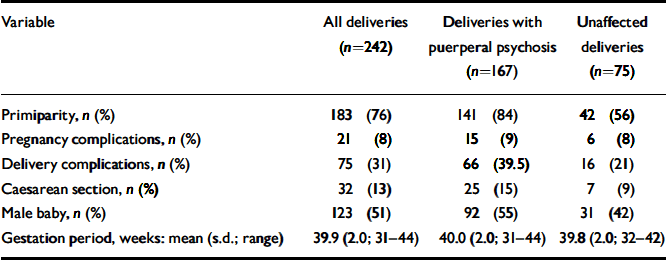
| Variable | All deliveries (n=242) | Deliveries with puerperal psychosis (n=167) | Unaffected deliveries (n=75) |
|---|---|---|---|
| Primiparity, n (%) | 183 (76) | 141 (84) | 42 (56) |
| Pregnancy complications, n (%) | 21 (8) | 15 (9) | 6 (8) |
| Delivery complications, n (%) | 75 (31) | 66 (39.5) | 16 (21) |
| Caesarean section, n (%) | 32 (13) | 25 (15) | 7 (9) |
| Male baby, n (%) | 123 (51) | 92 (55) | 31 (42) |
| Gestation period, weeks: mean (s.d.; range) | 39.9 (2.0; 31-44) | 40.0 (2.0; 31-44) | 39.8 (2.0; 32-42) |
Logistic regression
Our primary analysis used a stepwise logistic regression analysis to compare differences between all deliveries to women in the sample that were affected and unaffected by puerperal psychosis. With puerperal psychosis status after delivery (yes/no) as the dependent variable, the independent variables were primiparity, having a male baby, obstetric complications in pregnancy and delivery, having a Caesarean section, gestation period expressed in weeks, the age of the woman at delivery and, because multiple deliveries occurred in some women, a variable identifying each individual woman.
The results in Table 3 show that only two variables were independently significantly associated with an episode of puerperal psychosis - primiparity and complications during delivery. Together these two variables correctly predicted 88% of deliveries affected by puerperal psychosis. The only other variable which approaches significance is ‘male baby’, but a larger sample is needed to confirm or refute the suggestion that giving birth to a male baby may contribute to the onset of an episode of puerperal psychosis.
Table 3 Independent associations of variables with puerperal psychosis by logistic regression

| Variable | P | OR (95% CI) |
|---|---|---|
| Primiparity | <0.001 | 3.76 (1.94-7.27) |
| Delivery complication | <0.022 | 2.68 (1.15-6.25) |
| Pregnancy complication | 0.988 | 1.01 (0.31-3.33) |
| Caesarean section | 0.460 | 1.56 (0.48-5.0) |
| Male baby | 0.107 | 1.64 (0.98-2.95) |
| Gestation period | 0.878 | 0.99 (0.84-1.16) |
| Identification of participant | 0.488 | 1.00 (0.99-1.01) |
Affected and unaffected deliveries from the same woman
It is possible that the effect of parity demonstrated by the logistic regression simply reflects a bias resulting from women who suffer a severe post-partum affective episode being less likely to go on to have further children. For this reason we also performed an analysis on women who had multiple deliveries. We identified a subgroup of 53 women who were (a) multiparous and (b) had experienced at least one delivery affected by puerperal psychosis and one delivery which was unaffected by any major affective disturbance.
A binomial test of proportions was used to test the null hypothesis that the distribution of puerperal psychotic episodes would be equal across first and subsequent deliveries. The results again confirmed the importance of primiparity as a risk factor for puerperal episodes, with 43 of the puerperal episodes being in first deliveries and 10 in second deliveries (P=0.00002).
Employing McNemar's test for categorical variables and Wilcoxon's matched pairs signed ranks test for continuous variables, we also compared the pairs of affected and unaffected deliveries for the other risk variables on a ‘one-at-a-time’ basis. Consistent with the logistic regression where all risk variables were considered in combination, we found that delivery complications were significantly associated with episodes of puerperal psychosis (χ2=5.82, d.f.=1, P=0.016). No significant associations with developing puerperal psychosis were found for pregnancy complications (χ2=0.25, d.f.=1, P=0.62), gestation period (Z=-0.92, P < 0.35), gender of the baby (χ2=0.53, d.f.=1, P < 0.25) or Caesarean section (χ2=1.29, d.f.=1, P < 0.25).
DISCUSSION
Puerperal psychosis is a severe and relatively uncommon form of postnatal affective illness occurring following less than 1 per 1000 deliveries (Reference BrockingtonBrockington, 1996). The boundaries of the concept of puerperal psychosis remain subject to heated debate, but it is clear that women with bipolar disorder are at greatly increased risk of an episode of illness in the immediate post-partum period (Reference Jones and CraddockJones & Craddock, 2001). The detailed aetiology of bipolar affective puerperal psychosis is not known, although familial genetic factors have been shown to be important in influencing susceptibility (Reference Dean, Williams and BrockingtonDean et al, 1989; Reference Jones and CraddockJones & Craddock, 2001).
We have previously examined the rates of puerperal and non-puerperal recurrence of illness following an index episode of post-partum psychosis and found that a positive family history of mental illness predicts a shorter time to non-puerperal recurrence (Reference Robertson, Jones and HaqueRobertson et al, 2005). We here focus on all deliveries (affected and unaffected) to women with bipolar affective puerperal psychosis and examine whether a number of obstetric variables predict those deliveries followed by a post-partum episode. Establishing clear and well-replicated risk factors for puerperal psychosis is an important goal for two reasons. First, it may enable a greater sophistication and accuracy in predicting which women are at risk of severe postnatal illness. Second, it has the potential to give important leads in the search to uncover the aetiology of both puerperal psychosis and affective disorder more generally.
Evidence from both epidemiological and cross-sectional studies has suggested a number of obstetric factors that may be associated with triggering of puerperal psychotic episodes in individuals at risk. However, with the exception of the effect of parity, there has been little consistency between studies as to which factors are important. In this study we were able to examine a number of the risk factors implicated by previous studies, both separately and in combination and, uniquely, were able to make comparisons with the unaffected deliveries of women with puerperal psychosis. In this way the women acted as their own controls, minimising possible confounding variables.
Parity
Our finding that primiparity was associated with a higher risk of puerperal psychosis is consistent with the existing literature. It is well established that puerperal psychosis is observed most frequently after a first delivery (Reference Videbech and GouliaevVidebech & Gouliaev, 1995; Reference Kirpinar, Coskun and CayköylüKirpinar et al, 1999). Paffenbarger (Reference Paffenbarger, Brockington and Kumar1982) calculated the relative risk observed in first compared with later deliveries as 2.04, and Kendell et al (Reference Kendell, Chalmers and Platz1987) found that the incidence dropped from 2.6 per 1000 after first pregnancies to 1.4 per 1000 after later deliveries.
The reason for the excessive risk in primiparous women is not clear. An important bias is that women with a severe episode of post-partum psychosis may be less likely to have further children, thus producing a lower observed rate. However, this is unlikely to be the sole or even the main explanation. For example, Kendell et al (Reference Kendell, Chalmers and Platz1987) were not able to account for the effect of primiparity solely by age or avoidance of further pregnancies. In our study we were able to test the association with first pregnancies in the subsample of women who had two or more deliveries and again confirmed the effect of primiparity. If women were less likely to have a further baby following puerperal psychosis, this subsample would be biased to women who had puerperal psychosis in their second pregnancy and therefore the association with first pregnancies is even more impressive.
Another possible explanation is that first pregnancies are a greater psychosocial stressor than subsequent deliveries. Undoubtedly the transition to new parenthood is a cause of greater stress than having further children but, although psychosocial factors have been shown to play a role in the aetiology of non-psychotic episodes of postnatal depression, this has not been demonstrated for psychosis in the puerperium (Reference Brockington, Martin and BrownBrockington et al, 1990; Reference Dowlatshahi and PaykelDowlatshahi & Paykel, 1990).
The possibility remains, therefore, that the effect of primiparity results, at least in part, from biological differences between first and subsequent pregnancies. The comparison with other pregnancy-related conditions in humans is pertinent - pregnancy-induced hypertension, for example, is ten times more common in first pregnancies (Reference Lewis and ChamberlainLewis & Chamberlain, 1990). Interestingly, the fact that the rate of pregnancy-induced hypertension in subsequent pregnancies is increased with a new partner raises the possibility of an immunological aetiology (Reference Tubbergen, Lachmeijer and AlthuisiusTubbergen et al, 1999). Immunological mechanisms have been suggested to play a role in postnatal depressive disorders (Reference Maes, Lin and OmbeletMaes et al, 2000) and are a candidate for involvement in puerperal psychosis. Indeed, the often-described association of thyroid antibodies and post-partum mood symptoms (Reference Kuijpens, Vader and DrexhageKuijpens et al, 2001; Reference Harris, Oretti and LazarusHarris et al, 2002) might reflect a more general heightened immunological state rather than a specific influence of thyroid function on mood (Reference Harris, Oretti and LazarusHarris et al, 2002). It would be of great interest to examine whether the rates of puerperal psychosis in subsequent pregnancies are influenced by whether the father is the same or a different partner, but it is likely that these data would only be available in sufficient numbers from studies of national birth registers. The hormonal changes that occur following delivery are believed to play an important role in the triggering of episodes of puerperal psychosis (Reference BrockingtonBrockington, 1996; Reference Jones, Lendon and CoyleJones et al, 2001) and offer another important avenue for research to identify an intermediate mechanism between obstetric variables and brain changes involved in the onset of an episode of illness. Hormonal, immunological and other biological differences between first and subsequent pregnancies are therefore interesting targets for further investigation into the aetiology of puerperal psychosis and, in particular, will suggest candidate genes for molecular genetic studies of this condition.
Obstetric complications
Paffenbarger (Reference Paffenbarger, Brockington and Kumar1982) reported that women with puerperal psychotic illness had a higher rate of obstetric complications compared with a control group. However, subsequent case-control studies failed to replicate these findings and it has been suggested that complications during pregnancy and delivery do not play a major role in the pathogenesis of puerperal psychosis (Kendell et al, Reference Kendell, Rennie and Clarke1981, Reference Kendell, Chalmers and Platz1987; Reference McNeil and BlennowMcNeil & Blennow, 1988; Reference Kumar, Marks and PlatzKumar et al, 1995; Reference Videbech and GouliaevVidebech & Gouliaev, 1995). In the current study, although complications in pregnancy were not associated with an increased risk of puerperal psychosis, experiencing a complication during delivery more than doubled the risk. We were, however, unable to discern more specific risk factors from among the set of delivery complications because of small numbers of individual complications.
The mechanism behind the increased risk is again unclear, but there are a number of possibilities that should be examined in further studies. Complications at delivery might cause a magnified stress response, with particularly high or prolonged increased levels of cortisol. Alternatively, complications may be associated with prolonged labours that result in excessive sleep disturbance. Although we did not examine sleep disruption in this study, further prospective studies of women at high risk would be useful. Finally, and given the discussion regarding primiparity above, the potential for obstetric complications to lead to (or reflect) altered maternal-foetal immunological interaction (Reference Poole and ClamanPoole & Claman, 2004) is worth further consideration.
Delivery by Caesarean section
The evidence for an association between delivery by Caesarean section and developing puerperal psychosis is equivocal. Kendell et al (Reference Kendell, Rennie and Clarke1981) reported that delivery by Caesarean section appeared to be a risk factor for psychiatric admission with psychosis following childbirth. A similar non-significant trend was found in a larger subsequent study, in which there was a higher number of Caesarean sections among those who experienced psychotic symptoms (Reference Kendell, Chalmers and PlatzKendell et al, 1987). Although further epidemiological studies have not been conducted to replicate these results, the findings from cross-sectional clinical studies of post-partum psychosis have shown no differences between the rates of Caesarean sections in probands and matched controls (Reference Kumar, Marks and PlatzKumar et al, 1995; Reference Videbech and GouliaevVidebech & Gouliaev, 1995).
In the current study, we found no significant relationship between Caesarean section and puerperal psychosis, but it is of interest that the trend is for a modest excess of Caesarean section deliveries prior to the puerperal psychotic episodes (odds ratio≈1.6). Of the 21 Caesarean sections performed for first deliveries, 20 were followed by puerperal psychosis (χ2=2.7, d.f.=1, P < 0.09). This warrants further study in larger samples.
Gender of the child
The results of studies examining the relationship between gender of the baby and puerperal psychosis are inconclusive, but a number of studies have reported an association with female births (Reference Kendell, Chalmers and PlatzKendell et al, 1987; Reference Agrawal, Bhatia and MalikAgrawal et al, 1990; Reference Okano, Nomura and KumarOkano et al, 1998). In one study this rate was surprisingly high at 74% of cases (Reference Agrawal, Bhatia and MalikAgrawal et al, 1990) but in others there was a more modest increase (56%; Reference Okano, Nomura and KumarOkano et al, 1998). The current study, in contrast, found a trend for episodes of puerperal psychosis to follow the delivery of male babies. This association, however, was not statistically significant and a number of other studies have found no difference in the gender ratio (Reference Kendell, Rennie and ClarkeKendell et al, 1981; Reference Videbech and GouliaevVidebech & Gouliaev, 1995). It is difficult to explain this association and it is possible that it may merely reflect chance variation.
Short gestation period
It has been reported that preterm delivery may be associated with puerperal psychosis. In a matched control study, Videbech & Gouliaev (Reference Videbech and Gouliaev1995) found that probands had more than a twofold increased risk of preterm delivery and lower birth weight of the child compared with the carefully matched obstetric controls - a finding that could not be explained by differences in parity among the two groups. Paffenbarger (Reference Paffenbarger, Brockington and Kumar1982) reported a similar association. Others have failed to confirm the association with either a short gestation period or low birth weight (Reference Kendell, Chalmers and PlatzKendell et al, 1987). Our analyses showed no difference in gestation period between deliveries affected and unaffected by puerperal psychosis.
Limitations
The findings outlined above must be interpreted in the light of a number of limitations of this study. First, although the number of women with an episode of puerperal psychosis was large, at 129, the number who had had another delivery unaffected by affective illness was much lower, at 53. Larger samples would clearly be desirable to enhance the power to identify risk factors.
Second, the range of possible risk factors examined was limited to a number of those that had been implicated in previous studies. There may be other risk factors that we have not examined that are associated with vulnerability to puerperal psychosis.
Third, much information was obtained retrospectively, predominantly by self-report. Although prospective studies would be preferable, it would be practically impossible to obtain data on this number of women with puerperal psychosis, and we have shown that both the diagnosis of the puerperal episode and the information collected on the key variables studied have high reliability.
Conclusions
This study provides further evidence regarding the association between lower parity and puerperal psychosis. It also suggests that experiencing complications during delivery is associated with developing a severe episode of post-partum psychosis. Further studies examining the link between puerperal psychosis and these factors would be of benefit. Increasing our under-standing of the risk factors associated with puerperal psychosis has implications for the identification and treatment of women at risk, and may also give important clues to the aetiology of affective disorders both in the puerperium and at other times.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The risk of puerperal psychosis is highest following the birth of a first baby.
-
▪ The risk of puerperal psychosis may also be increased following deliveries affected by obstetric complications.
-
▪ Psychological and biological differences between first and subsequent deliveries and between those with and without obstetric complications are important avenues for further research into the aetiology of puerperal psychosis.
LIMITATIONS
-
▪ Despite a large overall sample and a within-subject design, the numbers in some analyses were relatively small.
-
▪ There may be risk factors other than those examined here that are associated with vulnerability to puerperal psychosis.
-
▪ The information was obtained retrospectively and may be subject to bias.
Acknowledgements
We thank all of the women who participated in this study. We also thank Dr Anne Biringer, Assistant Professor of Family and Community Medicine at the University of Toronto and Director of Primary Care Obstetrics at Mount Sinai Hospital, Toronto and Dr Donna Stewart, Professor and Chair of Women's Health, University of Toronto and University Health Network. This work was supported by grants from the Wellcome Trust, the West Midlands Regional Health Authority Research & Development Directorate, South Birmingham Mental Health NHS Trust and the Women's Mental Health Trust. E.R.B. was a New Blood Research Fellow and I.J. was a Wellcome Trust Training Fellow in Mental Health at the time the study was conducted.








eLetters
No eLetters have been published for this article.