With 81% of local authorities in the UK reporting problems recruiting and retaining social workers, staffing is more problematic in social work than in any other professional group (Employers' Organisation & Provincial Employers' Organisations, 2002). High vacancy (5-16%) and turnover rates (7-30%) contribute to staff shortages, excessive workloads and reliance on temporary staff, making modern social work practice increasingly difficult (Reference Eborall and GarmesonEborall & Garmeson, 2001). Work pressures can lead to burnout - a combination of emotional exhaustion, depersonalisation and low personal accomplishment. Few studies have examined burnout in social workers (Reference Siefert, Jayaratne and ChessSiefert et al, 1991; Reference RossRoss, 1993; Reference ZunzZunz, 1998; Reference Lloyd and KingLloyd & King, 2002) but commitment to their work and service users, even when under severe stress, was reaffirmed in two UK studies (Reference McLean and AndrewMcLean & Andrew, 2000; Reference Eborall and GarmesonEborall & Garmeson, 2001).
Studies of other professional groups have shown that stress commonly arises where one has little control (decision latitude) over one's work (Reference KarasekKarasek, 1979). Higher levels of decision latitude are associated with a greater sense of personal accomplishment and satisfaction (Reference Joseph and ConradJoseph & Conrad, 1979). Workers with high job demands, low decision latitude and low support at work are the most stressed (Reference KarasekKarasek, 1979). These factors have not been studied in relation to one key member of multidisciplinary mental health teams - mental health social workers. This national study fills that gap and complements a parallel study of psychiatrists conducted using the same methodology (Reference Pajak, Mears and KendallPajak et al, 2003).
The study aimed to: (a) characterise the mental health social work workforce in terms of demography, experience, job content, workload, working environment, health and well-being; and (b) explain the nature and direction of associations between these explanatory variables and mental health, burnout and job satisfaction.
METHOD
Design
A multi-method design was adopted. Questionnaire content was informed by two focus groups involving practising social workers from the South London and Maudsley NHS Trust. Three structured, standardised instruments were added to the questionnaire, prior to piloting with social workers, who were ineligible for the main study. Following minor revisions, the questionnaire was included in a national postal survey of a randomly selected sample of mental health social workers in England and Wales. The sampling frame is described below. Participants were asked to return the questionnaire in a stamped addressed envelope within 1 month.
Dependant variables
The General Health Questionnaire (GHQ-12; Reference GoldbergGoldberg, 1992) is a dimensional indicator of common mental disorder (Reference Goldberg and HuxleyGoldberg & Huxley, 1992) from which a summed score is produced; higher scores indicate poorer mental health. It has satisfactory psychometric properties (Reference GoldbergGoldberg, 1992) and has been widely used on various occupational health samples (Reference Banks, Clegg and JacksonBanks et al, 1980; Reference Banks and JacksonBanks & Jackson, 1982), including mental health professionals (Reference Prosser, Johnson and KuipersProsser et al, 1996).
Burnout is defined as exhaustion resulting from excessive demands on energy and resources. The Maslach Burnout Inventory (Reference Maslach and JacksonMaslach & Jackson, 1986) is the most widely used measure of burnout and has previously been used in mental health services research (Reference Prosser, Johnson and KuipersProsser et al, 1996). This 22-item, 6-point anchored Likert scale has three components: ‘emotional exhaustion’ (the depletion of emotional resources, leading workers to feel unable to give of themselves at a psychological level); ‘depersonalisation’ (negative, cynical attitudes and feelings about clients); and reduced ‘personal accomplishment’ (evaluating oneself negatively, particularly with regard to work with clients). Burnout exists when the thresholds for each sub-scale are reached (emotional exhaustion 521; depersonalisation 58; personal accomplishment 428; Reference Prosser, Johnson and KuipersProsser et al, 1996).
Job satisfaction was measured by a single-item, standardised rating of ‘satisfaction with your current job’, rated using the seven-point ‘delighted-terrible’ scale (Reference Andrews and WitheyAndrews & Withey, 1976).
Explanatory variables
The main variables used to explain the dependent variables were the nature of the job and the immediate context in which it took place. The Karasek Job Content Questionnaire (Reference KarasekKarasek, 1979) provided standardised sub-scale ratings of decision latitude, psychological job demands and social support in the workplace (from supervisors and co-workers). Other standardised ratings related to feelings about the employer, the place of social work in modern mental health services, government policy on mental health and the proposed new Mental Health Act. The questionnaire also included data relating to demographics and personal characteristics such as qualifications and job history, and objective and subjective questions about work context and environment.
The sample
There is no readily available sampling frame from which to draw a sample of mental health social workers or approved social workers (ASWs); therefore a sampling frame was generated through the Association of Directors of Social Services. Directors provided contact details for their leading manager for mental health services, who was asked to provide a complete list of current mental health social work staff (excluding emergency duty teams, agency staff and managers). A one-in-five sample was selected from the list of names provided by each council with social services responsibilities using the Statistical Package for the Social Sciences (SPSS) random sample generator, limiting the number of participants in each council to four.
Of the 171 councils with social services responsibilities in England and Wales, 145 were willing to participate (85%); 109 of these 145 (75%) provided a list of their mental health social workers within the deadline. Preliminary analyses indicated that responding authorities did not differ from non-responding authorities in terms of authority type (county, unitary, metropolitan, London borough) or the National Audit Office's (2002) comprehensive performance analysis (a star rating system of service quality) results for adult services.
There were 610 questionnaires (plus diaries) distributed. Staff in 88 authorities responded (52% of all councils with social services responsibilities, 61% of those willing to participate, and 81% of those providing a list within the deadline). There were 462 questionnaires returned (76%) but 125 of these (27%) were ineligible because they did not match the specified inclusion criteria (i.e. they were from students, managers or members of emergency duty teams). There were 237 (39%) questionnaires eligible for inclusion in the analysis, giving an adjusted response rate of 49% (237/(6107125) ×100). The real response rate is probably higher given that more than a quarter of the questionnaires returned were ineligible, assuming that a similar proportion of non-responders would have been ineligible.
Statistical analysis
Data were analysed using SPSS for Windows, version 11.0. Descriptive statistics were used to describe the sample in terms of personal characteristics, work context and environment, health, well-being and job satisfaction.
One-way analysis of variance (ANOVA; with Bonferroni correction, to allow for multiple comparisons) was used to examine between-group differences in GHQ total score, Maslach sub-scores and job satisfaction. The independent variables for these ANOVAs were constructed by classifying each of the Karasek sub-scales (job demands, decision latitude and social support) into categorical variables representing low, medium and high scores, according to recommended thresholds (Reference KarasekKarasek, 1979). The GHQ total was computed using both the GHQ scoring method and the Likert method, to facilitate comparison with previous studies.
A series of linear regression models was constructed (using the ‘enter’ method) to explain the variance in the main dependent variables, and the relative magnitude and direction of their associations with job demands, decision latitude and social support, when other confounding and mediating effects were controlled for. The model assumed that each of the dependent variables was associated directly with job demand, decision latitude and social support but that these associations might be confounded by work context/environment and subjective feelings about that environment, but mediated by personal characteristics. Each model included:
-
(a) total scores for each of the Karasek sub-scales;
-
(b) work context and environment variables, specifically social work vacancy rate within the team, number of extra hours worked per week, case-load, time spent on duty (the social work equivalent of first on call for ASWs or time spent providing emergency response to new referrals at the office base), and being a member of an integrated team (a dummy variable);
-
(c) subjective variables relating to feelings about pay, being valued, the place of social work in mental health services and the proposed mental health bill;
-
(d) personal characteristic variables for age, gender, length of time in this post, number of days sick taken in the past year and whether active as an ASW (dummy).
The number of variables entered was kept within recommended limits (total cases=8 × number of variables in the model+50 cases; Reference Tabachnick and FidellTabachnick & Fidell, 2001).
RESULTS
Personal characteristics
Sixty-one per cent (n=145) of respondents were female. Most of the sample was aged under 50 (n=133, 58% of the 228 respondents who answered this question) and the mean age was 46 years (s.d.=9.2). Only 10% (n=24) of the sample were from minority ethnic or other cultural groups; 2% (n=5) were Black Caribbean and 1% (n=2) Black African, the rest were from other European countries, America or Australia. Demographically, our sample of mental health social workers included more females, was older and more ethnically diverse than participants in a large survey of generic social workers (Reference McLean and AndrewMcLean & Andrew, 2000).
Eighty-three per cent (n=197) of the sample worked full-time. Respondents worked a mean of 43 h (s.d.=7.0) per week (8393 h/195 workers), an excess over contracted hours of approximately 6 per week per worker. Thirty-nine per cent of the working week was spent in face-to-face contact with service users or carers and 29% on administration (partly owing to limited support). Respondents reported a mean of 15 h (s.d.=10.9) on duty during the working week. The mean job tenure with the current employer was 7.6 years (s.d.=7.0), although not necessarily in mental health work for the whole period. Respondents were experienced workers with a mean of 11.9 years (s.d.=8.7) since social work qualification. Sixty-eight per cent of the sample (n=162) were active ASWs; most of the remainder (referred to in the results as non-ASWs) were awaiting ASW training. ASWs had been approved for a mean of 7.0 years (s.d.=6.0) and were older than non-ASWs (mean age 48 (s.d.=8.2) v. 42 years (s.d.=10.0)).
Work context and the working environment
Respondents worked in teams that had a mean of 16.5 (s.d.=8.2) members (median 14; mode 12; range 4-40). Integrated teams tended to be larger, having a mean of 18 members (s.d.=8.1). The mean case-load was 24.3 (s.d.=13.1; median 24; mode 25; range 1-70). Ten per cent (n=24) had case-loads of over 40. Members of integrated teams had somewhat larger case-loads (mean=24.7; s.d. 11.2) than members of smaller specialist (e.g. assertive outreach) teams (mean=18.1; s.d. 11.6). Sixty-three per cent of staff (n=150) reported doing additional work to cover for absent (primarily owing to sick leave) colleagues or for staff vacancies. Respondents reported being unable to take time off in lieu for working out of office hours, because of pressure of work and the vacancy situation. Seventy per cent (n=166) of respondents thought that their current grade did not reflect the duties they performed and 43% (n=102) felt undervalued at work.
Health and well-being
Forty-seven per cent (n=111) of respondents scored 4 or above on the GHQ-12, indicating a potential psychological disorder. When the lower cut-off for the identification of probable common mental disorders (2/3) was used, the GHQ-12-positive rate rose to 55% (n=130). Using the Likert scoring method, the mean score was 26.9 (s.d.=6.0).
Table 1 shows that mean scores on each of the Maslach Burnout Inventory sub-scales were higher than the reported mental health category norms (Reference Maslach and JacksonMaslach & Jackson, 1986). Mental health social workers were more emotionally exhausted and more depersonalised than the average mental health worker but experienced more personal accomplishment. They were also more emotionally exhausted than psychiatrists in the parallel study (Reference Pajak, Mears and KendallPajak et al, 2003) but were less depersonalised and experienced less personal accomplishment. Nevertheless, only 8% of respondents met the threshold for burnout as defined above (n=18).
Table 1 Features of burnout in mental health professionals

| Dependent variable | MHSWs (n=237) | Consultant psychiatrists (n=181) 1 | Mental health category norms (n=730) 2 | |
|---|---|---|---|---|
| Maslach Burnout Inventory sub-scale score: mean (s.d.) | ||||
| Emotional exhaustion | 26.3 (10.1) | 24.2 (11.3) | 16.9 (8.9) | |
| Depersonalisation | 7.3 (5.2) | 8.5 (6.1) | 5.7 (4.6) | |
| Personal accomplishment | 33.9 (6.8) | 36.0 (5.7) | 30.9 (6.4) | |
MHSWs, mental health social workers.
1. Data from Reference Pajak, Mears and KendallPajak et al, 2003.
2. Data from Reference Maslach and JacksonMaslach & Jackson, 1986.
Approved social workers reported taking more sick leave (mean 12 days, s.d.=30.1) than non-ASWs (mean=7 days, s.d.=12.4). The rate for ASWs was skewed by three cases of more than 90 days' sickness but the difference between ASWs and non-ASWs just failed to reach significance (t=-1.91 (229), P=0.057). Nevertheless, the mean duration of sick leave for ASWs was twice that for psychiatrists (Reference Pajak, Mears and KendallPajak et al, 2003). Approved social workers were also more likely than non-ASWs to report taking unspecified stress-relieving medications (10% (n=16) v. 7% ((n=5)), another non-significant difference (χ2=0.63 (1), P=0.30).
Job satisfaction
Forty-seven per cent (n=111) of respondents were at least ‘mostly satisfied’ with their current job but 35% (n=83) were ambivalent and 19% (n=43) were dissatisfied; the mean job satisfaction rating was 4.4 (s.d.=1.2, range 1-7). Far fewer people were satisfied with their employer, 22% (n=52) being at least ‘mostly satisfied’, 37% ambivalent (n=88) and 41% (n=98) dissatisfied (mean=3.7, s.d.=1.2, range 1-7).
Over a quarter of respondents (28%, n=66) had a strong or very strong desire to leave their present post and 21% (n=48) had specific plans to do so. A strong or very strong desire to leave one's job was related to ASW status: 33% of ASWs compared with 19% of non-ASWs wanted to leave (χ2=9.6 (3), P <50.05).
Associations with mental health, burnout and job satisfaction
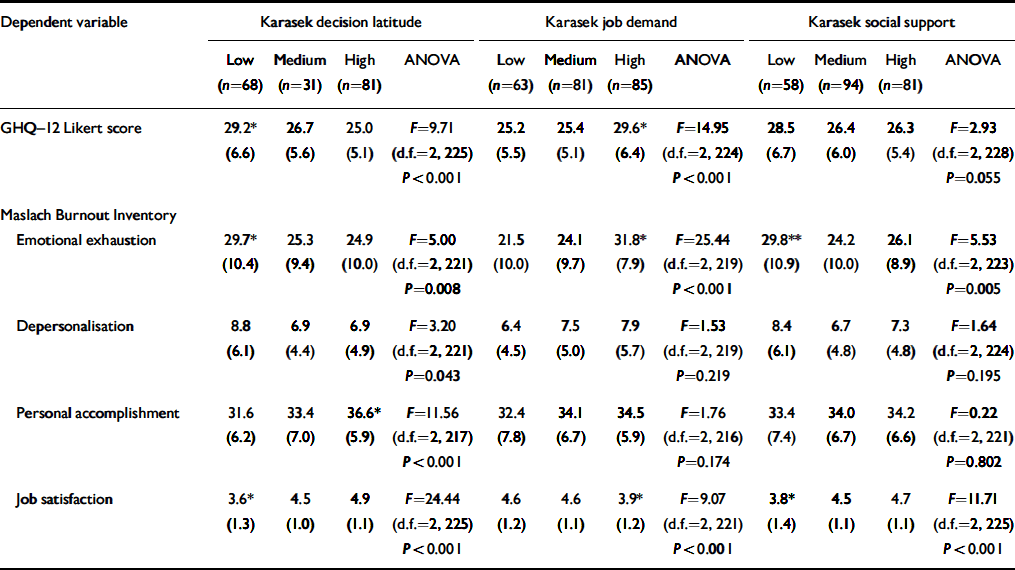
The ANOVA results presented in Table 2 demonstrate that low decision latitude and high job demands were associated with poor mental health (determined by higher GHQ-12 scores) and emotional exhaustion. Conversely, greater decision latitude and lower job demands were associated with higher levels of job satisfaction. Low social support was also associated with emotional exhaustion whereas medium or high social support were associated with greater job satisfaction. Few job content characteristics were associated with personal accomplishment or depersonalisation.
Table 2 Variation in mental health, burnout and job satisfaction scores (mean (s.d.)) according to job decision latitude, job demand and social support in the workplace
| Dependent variable | Karasek decision latitude | Karasek job demand | Karasek social support | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Low (n=68) | Medium (n=31) | High (n=81) | ANOVA | Low (n=63) | Medium (n=81) | High (n=85) | ANOVA | Low (n=58) | Medium (n=94) | High (n=81) | ANOVA | ||||||||||
| GHQ—12 Likert score | 29.2 * (6.6) | 26.7 (5.6) | 25.0 (5.1) | F=9.71 (d.f.=2,225) P<0.001 | 25.2 (5.5) | 25.4 (5.1) | 29.6 * (6.4) | F=14.95 (d.f.=2,224) P<0.001 | 28.5 (6.7) | 26.4 (6.0) | 26.3 (5.4) | F=2.93 (d.f.=2,228) P=0.055 | |||||||||
| Maslach Burnout Inventory Emotional exhaustion | 29.7 * (10.4) | 25.3 (9.4) | 24.9 (10.0) | F=5.00 (d.f.=2,221) P=0.008 | 21.5 (10.0) | 24.1 (9.7) | 31.8 * (7.9) | F=25.44 (d.f.=2,219) P<0.001 | 29.8 ** (10.9) | 24.2 (10.0) | 26.1 (8.9) | F=5.53 (d.f.=2,223) P=0.005 | |||||||||
| Depersonalisation | 8.8 (6.1) | 6.9 (4.4) | 6.9 (4.9) | F=3.20 (d.f.=2,221) P=0.043 | 6.4 (4.5) | 7.5 (5.0) | 7.9 (5.7) | F=1.53 (d.f.=2,219) P=0.219 | 8.4 (6.1) | 6.7 (4.8) | 7.3 (4.8) | F=1.64 (d.f.=2,224) P=0.195 | |||||||||
| Personal accomplishment | 31.6 (6.2) | 33.4 (7.0) | 36.6 * (5.9) | F=11.56 (d.f.=2,217) P<0.001 | 32.4 (7.8) | 34.1 (6.7) | 34.5 (5.9) | F=1.76 (d.f.=2,216) P=0.174 | 33.4 (7.4) | 34.0 (6.7) | 34.2 (6.6) | F=0.22 (d.f.=2,221) P=0.802 | |||||||||
| Job satisfaction | 3.6 * (1.3) | 4.5 (1.0) | 4.9 (1.1) | F=24.44 (d.f.=2,225) P<0.001 | 4.6 (1.2) | 4.6 (1.1) | 3.9 * (1.2) | F=9.07 (d.f.=2,221) P<0.001 | 3.8 * (1.4) | 4.5 (1.1) | 4.7 (1.1) | F=11.71 (d.f.=2,225) P<0.001 | |||||||||
GHQ—12, General Health Questionnaire; ANOVA, analysis of variance.
* Significantly different from both other categories when Bonferroni procedure applied.
** Significancy different from medium-support category when Bonferroni procedure applied.
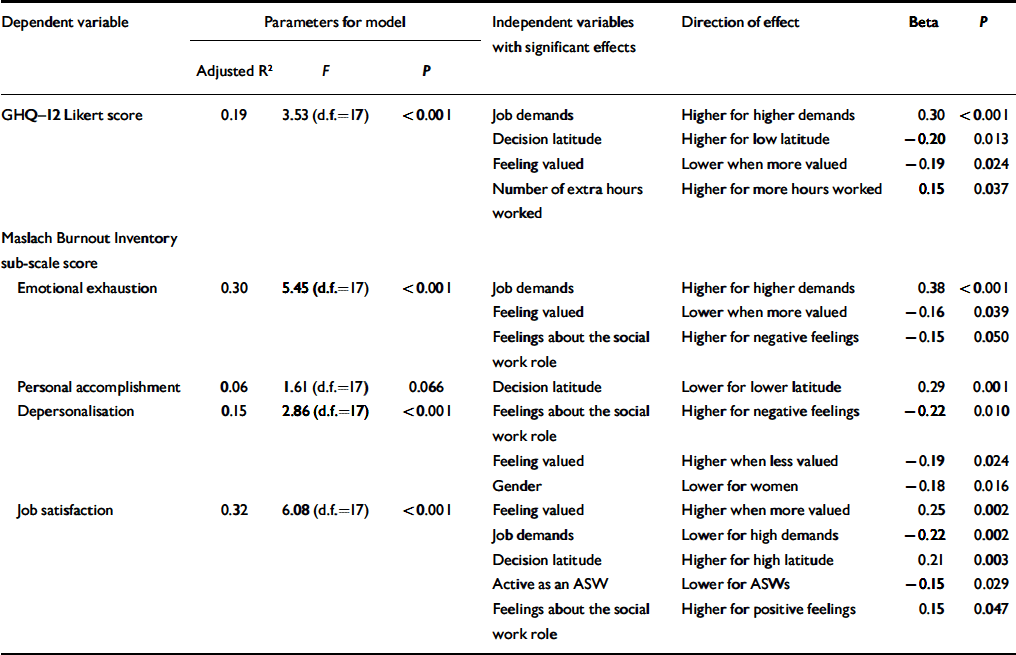
Table 3 shows the results of multivariate analyses that examined whether the effects of decision latitude, job demands and social support were independent of work context/environment, subjective feelings and personal characteristics, and explored which other variables contributed to the explanation of the dependent variables.
Table 3 Linear regression models explaining the association between of mental health, burnout and job satisfaction
| Dependent variable | Parameters for model | Independent variables with significant effects | Direction of effect | Beta | P | ||||
|---|---|---|---|---|---|---|---|---|---|
| Adjusted R2 | F | P | |||||||
| GHQ-12 Likert score | 0.19 | 3.53 (d.f.=17) | <0.001 | Job demands | Higher for higher demands | 0.30 | <0.001 | ||
| Decision latitude | Higher for low latitude | −0.20 | 0.013 | ||||||
| Feeling valued | Lower when more valued | −0.19 | 0.024 | ||||||
| Number of extra hours worked | Higher for more hours worked | 0.15 | 0.037 | ||||||
| Maslach Burnout Inventory sub-scale score | |||||||||
| Emotional exhaustion | 0.30 | 5.45 (d.f.=17) | <0.001 | Job demands | Higher for higher demands | 0.38 | <0.001 | ||
| Feeling valued | Lower when more valued | −0.16 | 0.039 | ||||||
| Feelings about the social work role | Higher for negative feelings | −0.15 | 0.050 | ||||||
| Personal accomplishment | 0.06 | 1.61 (d.f.=17) | 0.066 | Decision latitude | Lower for lower latitude | 0.29 | 0.001 | ||
| Depersonalisation | 0.15 | 2.86 (d.f.=17) | <0.001 | Feelings about the social work role | Higher for negative feelings | −0.22 | 0.010 | ||
| Feeling valued | Higher when less valued | −0.19 | 0.024 | ||||||
| Gender | Lower for women | −0.18 | 0.016 | ||||||
| Job satisfaction | 0.32 | 6.08 (d.f.=17) | <0.001 | Feeling valued | Higher when more valued | 0.25 | 0.002 | ||
| Job demands | Lower for high demands | −0.22 | 0.002 | ||||||
| Decision latitude | Higher for high latitude | 0.21 | 0.003 | ||||||
| Active as an ASW | Lower for ASWs | −0.15 | 0.029 | ||||||
| Feelings about the social work role | Higher for positive feelings | 0.15 | 0.047 | ||||||
GHQ-12, General Health Questionnaire; ASW, approved social worker.
The results suggested that high job demands and low decision latitude were independently associated with poor mental health but high GHQ-12 scores were also associated with the number of additional hours worked per week and not feeling valued by the employer.
High emotional exhaustion was also associated directly with higher job demands but not with low decision latitude or low social support, when features of the work environment, personal characteristics and subjective feelings were controlled for. These results suggest that the original associations between emotional exhaustion and these aspects of job content (based on ANOVAs) might have been confounded. Personal accomplishment was associated with high decision latitude, suggesting that it was not confounded with the other explanatory factors. Depersonalisation was still not associated with any aspect of job content (decision latitude, job demands and social support) but was associated with dissatisfaction about the role of mental health social work in the current mental health services, not feeling valued by the employer and being male.
Finally, job satisfaction was associated directly with lower job demands and higher decision latitude but not with social support, when other explanatory variables were included in the model. Being valued by their employer and positive feelings about the role of social work in current mental health services were also associated with job satisfaction, whereas being active as an ASW was associated most strongly with job dissatisfaction. These results suggest that personal characteristics, aspects of the working environment or feelings about that environment might confound the univariate association between job satisfaction and social support.
The model explained similar amounts of variance in emotional exhaustion and job satisfaction, less in mental health and little of the variance in other aspects of burnout.
DISCUSSION
The most striking findings of the survey are the very high levels of stress and emotional exhaustion in the sample. Mean GHQ-12 scores for mental health social workers were almost double the highest rate reported by Prosser et al (Reference Prosser, Johnson and Kuipers1996), which was for community-based mental health staff. The GHQ-positive rate was 47% using the cut-off of 4, which was almost double the rate for consultant psychiatrists (25%; Reference Pajak, Mears and KendallPajak et al, 2003) and nearly three times the level in the general population (17%; Department of Health, 1995). Similarly, mean scores for emotional exhaustion were higher than for psychiatrists (Reference Pajak, Mears and KendallPajak et al, 2003) and mean scores on all three burnout sub-scales were higher than norms for the mental health workforce (Reference Maslach and JacksonMaslach & Jackson, 1986). The main determination of the high rates of stress and emotional exhaustion appear to be high job demand and not feeling valued for the work that you do. Other factors, such as number of hours worked, decision latitude and feelings about the way in which social work is perceived within mental health services, are also important determinants of stress and features of burnout.
High levels of stress and emotional exhaustion among the workforce are a concern and likely to contribute further to the high vacancy rates associated with recruitment and retention problems within the social work profession (Reference Eborall and GarmesonEborall & Garmeson, 2001; Employers' Organisation & Provincial Employers' Organisations, 2002). One might have expected to find a direct association between team vacancy rates and stress/emotional exhaustion but these relationships failed to appear. This might be due to the low level of actual vacancies in most teams - 65% of participants reported no social work vacancies in their team. Nevertheless, 63% of respondents provided cover for absent colleagues, which may have included training or sick leave, not simply for vacant posts. The practice of using agency workers to cover vacancies in teams may have reduced the vacancy rates reported. Further research is required to determine whether the practice of employing agency staff, at higher rates of pay than statutory sector employees and without statutory responsibilities, exacerbates job dissatisfaction, burnout and recruitment and retention problems.
The high levels of job dissatisfaction and dissatisfaction with the employer give further cause for concern. The burden of statutory responsibilities associated with the ASW function under the Mental Health Act 1983 also emerged as an important factor in job dissatisfaction (although this finding is unlikely to be applicable outside the UK where social workers do not carry these responsibilities). Perhaps as a consequence, ASWs take slightly more sick leave than non-ASWs and take sick leave at twice the rate of psychiatrists (Reference Pajak, Mears and KendallPajak et al, 2003). It is worrying that 20% of our sample had a strong desire to leave their current post and 21% had specific plans to do so.
Social workers make a significant contribution to the work of community mental health teams, offering a unique perspective and currently providing a unique role through the ASW function, but they are a scarce and declining resource. This is in stark contrast to many other countries, notably the USA, where social workers are the main professional group in mental health services, but also closer to home in Northern Ireland, where the rates (per 1000 population) of social workers in mental health services are three times those in England and Wales (Department of Health, Social Services and Public Safety, 2004). Employers and central government will need to consider ways of improving conditions for mental health social workers, focusing on how to make staff feel valued, enhancing decision latitude, reducing job demands and reconsidering the role of social work within current mental health services, as these features were also associated with job satisfaction.
Limitations
The following factors should be considered when interpreting these data:
-
(a) the study was undertaken at a time of uncertainty for mental health social workers owing to the changing role of the ASW and the proposals included in the Draft Mental Health Bill, which may have been reflected in our findings;
-
(b) self-selection and factors external to the job might have contributed to high rates of stress within the workforce, although random selection and the regression results suggest that the impact was unlikely to be substantial;
-
(c) although acceptable, the return rate from individual social workers suggests that a degree of caution should be exercised when interpreting the results;
-
(d) the cross-sectional design of the study means that causal direction cannot be determined.
Conclusions
Multidisciplinary teams are the preferred model of mental healthcare provision, and in the UK these now operate from integrated health and social care ‘partnership’ trusts. The present study highlights that: the environments in which mental health social workers work are associated with job dissatisfaction and poor mental health; many mental health social workers in these services are overstressed, emotionally exhausted and feel undervalued. These factors might exacerbate recruitment and retention problems if employers continue to fail to recognise the demands placed on mental health social workers and to value their contribution; a large proportion of mental health social workers have negative feelings about their current job, with many having a strong desire to leave their current post, which has implications for workforce planning; further research is required into ways to decrease stress and improve job satisfaction among mental health social workers and ASWs, with the aim of improving recruitment and retention.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Many mental health social workers are overstressed, emotionally exhausted and feel undervalued. These factors might exacerbate recruitment and retention problems.
-
▪ Excessive job demands, limited latitude in decision-making and unhappiness about the place of the mental health social worker in modern services contribute to poor job satisfaction and burnout.
-
▪ Employers must recognise the demands placed on mental health social workers and value their contribution to mental health services.
LIMITATIONS
-
▪ Self-selection and external factors might have contributed to the high rate of stress found among mental health social workers.
-
▪ The return rate suggests that caution should be exercised when interpreting the results. The cross-sectional study design means that causal direction cannot be determined.
-
▪ The study was undertaken at a time of uncertainty for mental health social workers.
Acknowledgement
This study was funded by the Department of Health.








eLetters
No eLetters have been published for this article.