Information provided on the presence of anxiety, depression and alcoholism in relatives has been found to be influenced by the informants’ own psychiatric status (Reference Kendler, Silberg and NealeKendler et al, 1991; Reference Chapman, Mannuzza and KleinChapman et al, 1994; Reference Roy, Walsh and PrescottRoy et al, 1994; Reference Heun, Maier and MüllerHeun et al, 1997). This suggests that for these disorders a bias in estimates of morbidity risk will occur if diagnoses for relatives are made solely on the basis of information obtained from probands (Reference KendlerKendler, 1991). To our knowledge, no UK studies have investigated whether an informant's own psychiatric history of anxiety, depression or alcoholism influences their account of psychiatric morbidity in relatives.
METHOD
Study participants consisted of 115 proband–relative pairs who were recruited into a family aggregation study of generalised social phobia and generalised anxiety disorder. The probands were all women recruited from the community, with a mean age of 32.1 years (s.d.=3.77). As shown in Table 1, 39 probands had a lifetime history of DSM–IV mood disorder (i.e. major depessive disorder or dysthymia)/alcohol dependence (MD/AD) with or without a lifetime history of anxiety disorder, 45 probands had no history of MD/AD (despite having a history of anxiety disorder), and 31 probands had no history of a DSM–IV Axis I disorder. Of the total of 115 probands, 80 had a lifetime history of anxiety disorder. Proband diagnoses were made using the Structured Clinical Interview for DSM–IV Axis I Disorders (SCID–1; Reference First, Spitzer and GibbonFirst et al, 1995).
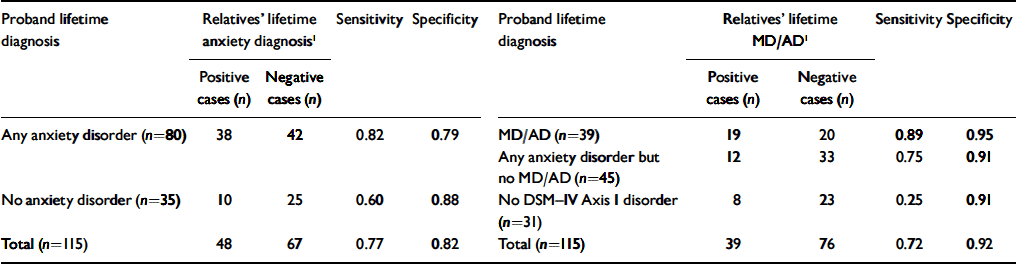
Table 1 Accuracy of probands’ predictions of anxiety disorder and mood disorder/alcohol (MD/AD) dependence according to probands’ own psychiatric history
| Proband lifetime diagnosis | Relatives' lifetime anxiety diagnosis1 | Sensitivity | Specificity | Proband lifetime diagnosis | Relatives' lifetime MD/AD1 | Sensitivity | Specificity | ||
|---|---|---|---|---|---|---|---|---|---|
| Positive cases (n) | Negative cases (n) | Positive cases (n) | Negative cases (n) | ||||||
| Any anxiety disorder (n=80) | 38 | 42 | 0.82 | 0.79 | MD/AD (n=39) | 19 | 20 | 0.89 | 0.95 |
| Any anxiety disorder but no MD/AD (n=45) | 12 | 33 | 0.75 | 0.91 | |||||
| No anxiety disorder (n=35) | 10 | 25 | 0.60 | 0.88 | No DSM—IV Axis I disorder (n=31) | 8 | 23 | 0.25 | 0.91 |
| Total (n=115) | 48 | 67 | 0.77 | 0.82 | Total (n=115) | 39 | 76 | 0.72 | 0.92 |
The 115 relatives were the mothers of the probands in all but 8% of cases (father in 1%, brother in 1% and sister in 6%). The mean age of the relatives was 56.8 years (s.d.=8.56).
Relatives were also interviewed using the SCID–1, with interviewers masked to the probands’ psychiatric status. Lifetime diagnoses of anxiety disorders, depressive disorders and alcohol dependence were made in consensus meetings between the SCID interviewer and one of the authors (P.J.C.).
Probands were interviewed about the psychiatric histories of their relatives. For MD and generalised anxiety disorder, established criteria were used (Reference Endicott, Andreasen and SpitzerEndicott et al, 1975; Reference Kendler, Davis and KesslerKendler et al, 1997). For the other disorders detailed research criteria were specified. Lifetime diagnoses were again made in independent consensus meetings (with P.J.C.), and these were compared with the ‘gold-standard’ diagnosis that was obtained from the direct interview.
The sensitivity and specificity of probands’ accounts of their relatives’ lifetime history of any DSM–IV anxiety disorder (a composite category because of the low numbers involved) and MD/AD were calculated, and binary logistic regression models were fitted to assess whether the accuracy of the probands’ information on relatives’ diagnoses was predicted by their own psychiatric histories of these disorders (taking into account the age difference between the proband and the other informant).
RESULTS
The sensitivity and specificity of the probands’ predictions of lifetime anxiety disorder in their relatives are shown in Table 1. There was no difference in the proportion of false-negative or false-positive diagnoses made by probands with and without a history of anxiety disorder (Fisher's exact test: P=0.21 and P=0.52 respectively). A binary logistic regression model confirmed that the likelihood of a correct prediction of anxiety disorder in relatives was the same for anxiety-disorder and non-anxiety-disorder probands (odds ratio 1.01, 95% CI 0.36–2.86; P=0.98).
Table 1 also shows the sensitivity and specificity of the probands’ accounts of lifetime MD/AD in their relatives, according to whether the probands themselves had a lifetime diagnosis of MD/AD, anxiety disorder without MD/AD, or no disorder. Probands who had never met the criteria for any DSM–IV Axis I disorder were more likely to make a false-negative prediction of MD/AD in their relatives than either probands who themselves had a lifetime diagnosis of MD/AD (Fisher's exact test: P=0.002) or probands who had a lifetime diagnosis of any anxiety disorder without MD/AD (Fisher's exact test: P=0.07). The proportion of false-negative predictions of MD/AD in their relatives made by the probands in the two psychopathology groups did not differ significantly. Similarly, the proportion of false-positive predictions of MD/AD in the relatives did not differ significantly between the three proband groups. A binary logistic regression model indicated that, compared with probands who had no lifetime DSM–IV Axis I disorder, the probands with a history of MD/AD were more than four times as likely to correctly predict a history of MD/AD in their relatives (odds ratio 4.03, 95% CI 0.95–17.14; P=0.06). Although not statistically significant, probands with a lifetime diagnosis of any anxiety disorder without MD/AD were approximately two and a half times more likely to correctly predict a history of MD/AD in their relatives (odds ratio 2.56, 95% CI 0.74–8.92; P=0.14).
DISCUSSION
In contrast to previous studies (Reference Kendler, Silberg and NealeKendler et al, 1991; Reference Chapman, Mannuzza and KleinChapman et al, 1994), we did not find that probands with and without a history of anxiety disorder differed in the accuracy of their reporting of anxiety disorder in their relatives. One possible reason for this discrepancy is that the commonest anxiety disorder in the present study was social phobia, and it may be that these cases do not show the same trend towards decreased specificity and increased sensitivity (when predicting the same disorder in relatives) as that shown by informants with panic disorder (Reference Chapman, Mannuzza and KleinChapman et al, 1994) and generalised anxiety disorder (Reference Kendler, Silberg and NealeKendler et al, 1991). Our results suggest that for family studies of anxiety disorder in the UK, no bias in estimates of morbidity rates would be likely to occur if diagnoses were made according to information obtained from probands alone.
With regard to MD/AD, as has been reported previously (Reference Chapman, Mannuzza and KleinChapman et al, 1994; Reference Roy, Walsh and PrescottRoy et al, 1994; Reference Heun, Maier and MüllerHeun et al, 1997), we found that probands with a history of such disorders showed higher sensitivity in their predictions of MD/AD in their relatives than probands with no history of a DSM–IV Axis I disorder. Furthermore, again as reported previously (Reference Chapman, Mannuzza and KleinChapman et al, 1994; Reference Roy, Walsh and PrescottRoy et al, 1994), our data suggest that this increased sensitivity was not specific to MD/AD in the probands. Probands with a history of an anxiety disorder without MD/AD were also more sensitive in their predictions of MD/AD in relatives than probands with no history of disorder. We found no evidence that the probands in the psychopathology groups were less specific in their predictions of MD/AD in their relatives than probands with no history of disorder. It could be argued that the use of the composite category of MD/AD for these analyses might have obscured diagnostically specific links. However, although we could not perform separate analyses for prediction of alcoholism in relatives (because of their low rate of this disorder), when only mood disorder diagnoses for relatives were selected, the pattern of results did not change.
It is also possible that our findings were influenced by specific aspects of the sample that was studied. The present study principally concerned mothers and daughters and it is possible that the findings may not generalise to other family relationships. Women may be more aware than men of psychiatric disorder in their relatives, although there is no evidence that psychiatric disturbance would have a different impact on the sensitivity and specificity of men's predictions compared with those of women.
Finally, given that (to our knowledge) this is the first UK study to investigate whether probands’ predictions of anxiety disorder and MD/AD in relatives are influenced by the probands’ own psychiatric history, it is important to consider that differences between our findings and those of previous studies may be due to cultural factors in the UK. These might include taboos about mental illness, societal understanding of mental illness, and the way in which UK families communicate – in particular, the way in which they discuss mental health issues.
Acknowledgements
We thank Susan Campbell, Barbara Kennedy, Paula Libberton, Monika Parkinson, Melanie Royal-Lawson and Sheila Summers for recruiting and assessing the proband sample, and Françoise Hentges, Jo Pearson and Hannah Seabrook for assisting in the assessment of relatives. We also thank all the participants in this study.
This research was funded by the Medical Research Council and the Health Foundation.






eLetters
No eLetters have been published for this article.