Accumulating evidence suggests an excess of psychiatric symptoms among veterans deployed to the 1991 Persian Gulf War relative to veterans of the same era not deployed to that conflict (era veterans) (Presidential Advisory Committee on Gulf War Veterans’ Illness, 1996; Iowa Persian Gulf Study Group, 1997; Reference Fukuda, Nisenbaum and StewartFukuda et al, 1998; Reference Kroenke, Koslowe and RoyKroenke et al, 1998; Reference Unwin, Blatchley and CokerUnwin et al, 1999; Reference Kang, Mahan and LeeKang et al, 2000; Reference Cherry, Creed and SilmanCherry et al, 2001; Reference Grant, Stinson and HarfordGrant et al, 2001; Reference Hallman, Kipen and DiefenbachHallman et al, 2003). Only one study to date has investigated psychiatric disorders among Gulf War veterans using a structured interview (Reference Ismail, Kent and BrughaIsmail et al, 2002); however, the purpose of that study was to determine the extent to which psychiatric disorder accounted for Gulf War illness, defined as disability status. Our study contributes to the existing Gulf War literature by comparing the 12-month prevalence of Axis I psychiatric disorders between random samples of Gulf War-deployed and era veterans, about 10 years after the conflict.
METHOD
Sampling
The Defense Manpower Data Center of the United States Department of Defense provided a random sample from all US troops deployed (n=1765) and not deployed (era veterans; n=1832) to the Persian Gulf during the period of Operations Desert Shield and Desert Storm (5 August 1990 to 31 July 1991). Those selected for the study were sent a letter describing the project and requesting their consent to be interviewed. Records from the Internal Revenue Service and national directory assistance databases (e.g. TeleMatch) were used to locate veterans whose letters were returned without forwarding information. These databases did not include cellphone (mobile telephone) numbers.
Questionnaire
All telephone interviews were administered using a computer-assisted telephone interview program. Participants were asked to rate their current health status, to report on 40 medical conditions diagnosed by a physician and to rate the presence and severity of 60 symptoms (further details available from the author upon request).
The overall purpose of our study was to determine the current symptoms and psychiatric disorders of Gulf War veterans. Therefore, as part of the telephone interview, participants were administered the Composite International Diagnostic Interview – Short Form/Diagnostic and Statistical Manual IV (CIDI–SF/DSM–IV; World Health Organization, 2002) to assess generalised anxiety, panic disorder, simple phobia, social phobia, agoraphobia, obsessive–compulsive disorder, major depression, alcohol dependence and drug dependence for the past 12 months. The 12-month version of the CIDI (World Health Organization, 1997) for the DSM–IV (American Psychiatric Association, 1994) was used to assess post-traumatic stress disorder (PTSD), mania, anorexia nervosa and bulimia. Methodological studies have not been completed for all versions of the CIDI. However, reliability and validity data are available for the DSM–III–R lifetime CIDI: for example, kappa test–retest (1–3 days) reliabilities for the lifetime CIDI range from 0.64 for bulimia to 0.84 for panic disorder (Reference WittchenWittchen, 1994). Furthermore, sensitivity and specificity of the CIDI–SF/DSM–III–R were acceptable relative to results achieved with the lifetime CIDI/DSM–III–R administered in the National Comorbidity Survey (average sensitivity 90.75, range 77.0–100; average specificity 98.04, range 93.9–99.9; Reference Kessler, Wittchen and AbelsonKessler et al, 1998). The only essential difference between the DSM–III–R and DSM–IV versions of the CIDI–SF was the added requirement that symptoms result in clinically significant distress or impairment.
Positive predictive values for the lifetime CIDI compared with the Structured Clinical Interview for DSM–III–R have been calculated for diagnosis-specific random subsamples of the National Comorbidity Survey respondents. Positive predictive values ranged from 0.21 for generalised anxiety to 0.95 for social phobia (Reference Kessler, Wittchen and AbelsonKessler et al, 1998). These predictive values were for lifetime rather than 12-month diagnoses, however, and thus may be somewhat lower than would be expected for 12-month diagnoses. A more recent study comparing the CIDI 12-month version with a structured clinical interview conducted by a clinician found an overall positive predictive value of 0.89 for any neurotic disorder (Reference Jordanova, Wickramasinghe and GeradaJordanova et al, 2004). Owing to the infrequency of non-affective psychosis and bipolar disorder in the general population, it is difficult to achieve reliable diagnoses (Reference Kendler, Gallagher and AbelsonKendler et al, 1996; Reference Kessler, Rubinow and HolmesKessler et al, 1997). Therefore, these diagnoses were not evaluated.
Diagnostic scoring was based on the procedures outlined for the CIDI–SF and CIDI 12-month version, with the exception of somatisation. Because of time constraints, a full interview for somatisation disorder was not possible. An abridged definition requiring a minimum of six symptoms for women or four symptoms for men (Reference Escobar, Burnam and KarnoEscobar et al, 1987) was used to establish somatisation. If the person rated as moderate or severe any of 16 symptoms, similar to those used in the Primary Care Evaluation of Mental Disorders (PRIME–MD; Reference Spitzer, Williams and KroenkeSpitzer et al, 1994) to screen for somatisation (e.g. fainting, menstrual problems or abdominal pain), the symptom was counted toward a diagnosis of somatisation disorder. For each somatisation symptom reported, the probe flow procedure from the CIDI was used to rule out medical explanations. Medical explanations were reviewed, masked, by a physician (H.M.K.) for consistency with the symptom.
Thirty interviewers, experienced in social science interviews, were trained by clinicians to administer the interview and were tested individually using a set of live mock interviews. The probe flow method for the CIDI 12-month version was sequentially programmed. To ensure quality control throughout the study, portions of interviews conducted by each interviewer were covertly monitored twice per shift and 10% of the interviews were monitored in their entirety. Participants were told as a part of the informed consent that their interview could be monitored by a clinician or supervisor. Concordance on question sequence and coding was 100% for all cases monitored. The median interview length was 46.7 min (minimum 18.4 min, maximum 213.6). The interviewers were trained to recognise suicidal or homicidal intent and to alert the on-call clinical psychologist.
Procedure
The protocol and verbal consent were reviewed and approved by the institutional review boards of Robert Wood Johnson Medical School, Rutgers University and the Centers for Disease Control and Prevention. In accordance with US government requirements, a certificate of confidentiality was issued under the authority of the Department of Health and Human Services. Individuals selected and sent a letter describing the study were asked to return a prepaid postcard indicating a preference of date and time to be interviewed. Those who failed to return their postcards within 5 days were telephoned, to enquire about their interest in the study, answer questions and, if possible, obtain verbal consent and set up an interview time. Participant recruitment and interviewing took place from February 2000 until October 2001.
Statistical analyses
Chi-squared analyses (using the Statistical Package for the Social Sciences, version 12.1 for Windows) were used to analyse participant characteristics and to compare respondents and non-respondents. Twelve-month prevalence of psychiatric disorders was stratified by deployment status and gender. Separate logistic regressions to predict psychiatric diagnoses used the demographic variables for Gulf War and era veterans listed in Table 3. To increase the stability of the models, participants with any one of the following anxiety disorders were included in the combined logistic regression for anxiety: agoraphobia, general anxiety disorder, obsessive–compulsive disorder, panic attack, social phobia, simple phobia and PTSD. A second logistic regression model was developed for major depression and a third for drug or alcohol dependence. Owing to the small number of cases, logistic regression analyses were not performed to predict mania.
The logistic regression analyses used to summarise these data roughly followed the procedures of Hosmer & Lemeshow (Reference Hosmer and Lemeshow2000). The logistic regression models were fitted using a stepwise forward inclusion algorithm, with inclusion and exclusion criteria of P≤0.15 and P≥0.2 respectively. If a variable was a significant predictor in the model, then that variable with all of its sub-categories was used as the sole predictor of the diagnosis in a new analysis. To obtain a more parsimonious and interpretable model, sub-categories of the variable within the single predictor model with similar odds ratios were combined whereas sub-categories with large confidence intervals were excluded; the overall logistic regression model was then repeated with the new sub-categories and all other predictors included in the model. Referents for each variable were generally chosen based on the sub-category with the largest number of participants (see Table 5). All two-way interactions among predictors were evaluated, but none was significant at P≤0.05.
RESULTS
Response rates
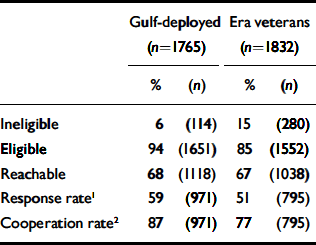
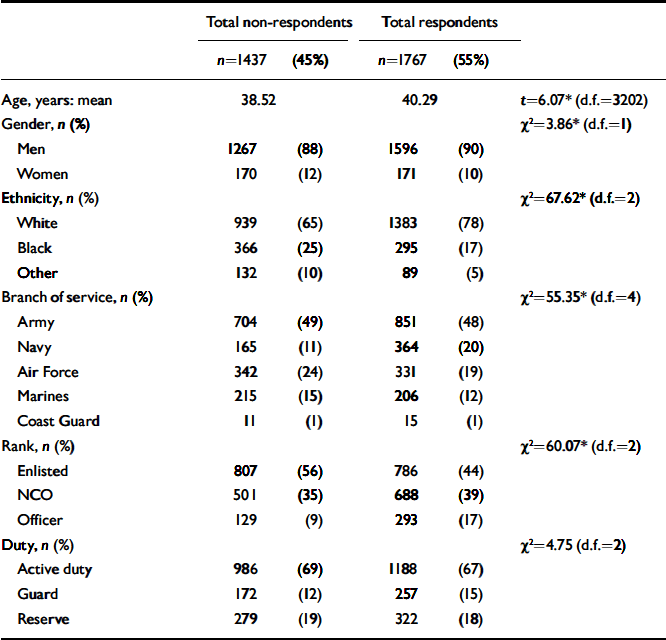
Response and cooperation rates are shown in Table 1. Overall response rates were lowered because valid addresses or telephone numbers could not be located for about one-third of the sample. In addition, some veterans in our sample were ineligible (e.g. incarcerated, dead, not in the military during the Gulf War). However, for those veterans contacted and eligible, the cooperation rate was relatively high. An overall comparison of respondents and nonrespondents was based on the demographic data available from Department of Defense records (Table 2). This comparison revealed that greater proportions of White veterans, non-commissioned non-commissioned and warrant officers, and commissioned officers responded. Although age, gender and branch of service also differed significantly between respondents and non-respondents, the differences were relatively small.
Table 1 Response and cooperation rates
| Gulf-deployed (n=1765) | Era veterans (n=1832) | |||
|---|---|---|---|---|
| % | (n) | % | (n) | |
| Ineligible | 6 | (114) | 15 | (280) |
| Eligible | 94 | (1651) | 85 | (1552) |
| Reachable | 68 | (1118) | 67 | (1038) |
| Response rate1 | 59 | (971) | 51 | (795) |
| Cooperation rate2 | 87 | (971) | 77 | (795) |
Table 2 Demographic characteristics of respondents and non-respondents
| Total non-respondents | Total respondents | ||||
|---|---|---|---|---|---|
| n=1437 | (45%) | n=1767 | (55%) | ||
| Age, years: mean | 38.52 | 40.29 | t=6.07* (d.f.=3202) | ||
| Gender, n (%) | χ2=3.86* (d.f.=1) | ||||
| Men | 1267 | (88) | 1596 | (90) | |
| Women | 170 | (12) | 171 | (10) | |
| Ethnicity, n (%) | χ2=67.62* (d.f.=2) | ||||
| White | 939 | (65) | 1383 | (78) | |
| Black | 366 | (25) | 295 | (17) | |
| Other | 132 | (10) | 89 | (5) | |
| Branch of service, n (%) | χ2=55.35* (d.f.=4) | ||||
| Army | 704 | (49) | 851 | (48) | |
| Navy | 165 | (11) | 364 | (20) | |
| Air Force | 342 | (24) | 331 | (19) | |
| Marines | 215 | (15) | 206 | (12) | |
| Coast Guard | 11 | (1) | 15 | (1) | |
| Rank, n (%) | χ2=60.07* (d.f.=2) | ||||
| Enlisted | 807 | (56) | 786 | (44) | |
| NCO | 501 | (35) | 688 | (39) | |
| Officer | 129 | (9) | 293 | (17) | |
| Duty, n (%) | χ2=4.75 (d.f.=2) | ||||
| Active duty | 986 | (69) | 1188 | (67) | |
| Guard | 172 | (12) | 257 | (15) | |
| Reserve | 279 | (19) | 322 | (18) | |
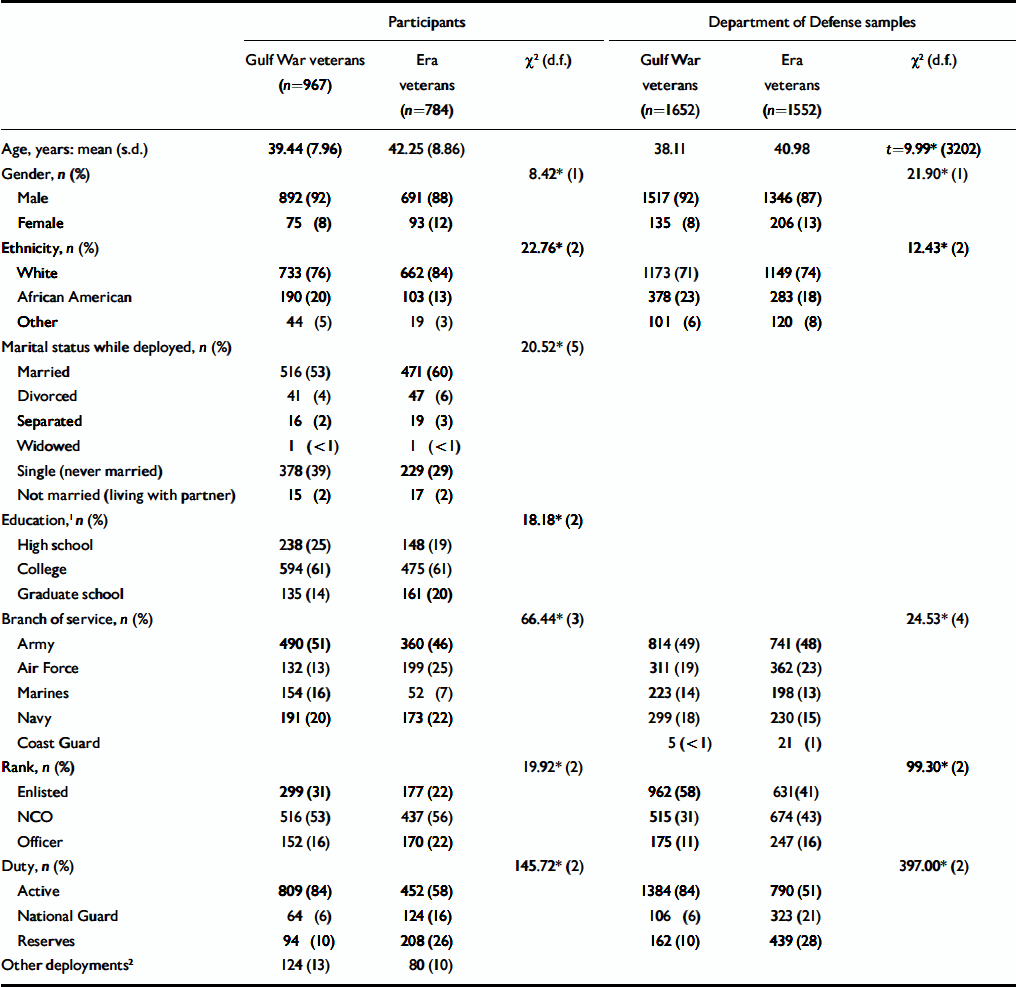
Table 3 Demographic characteristics of Gulf War veterans and era veterans
| Participants | Department of Defense samples | |||||
|---|---|---|---|---|---|---|
| Gulf War veterans (n=967) | Era veterans (n=784) | χ2 (d.f.) | Gulf War veterans (n=1652) | Era veterans (n=1552) | χ2 (d.f.) | |
| Age, years: mean (s.d.) | 39.44 (7.96) | 42.25 (8.86) | 38.11 | 40.98 | t=9.99* (3202) | |
| Gender, n (%) | 8.42* (1) | 21.90* (1) | ||||
| Male | 892 (92) | 691 (88) | 1517 (92) | 1346 (87) | ||
| Female | 75 (8) | 93 (12) | 135 (8) | 206 (13) | ||
| Ethnicity, n (%) | 22.76* (2) | 12.43* (2) | ||||
| White | 733 (76) | 662 (84) | 1173 (71) | 1149 (74) | ||
| African American | 190 (20) | 103 (13) | 378 (23) | 283 (18) | ||
| Other | 44 (5) | 19 (3) | 101 (6) | 120 (8) | ||
| Marital status while deployed, n (%) | 20.52* (5) | |||||
| Married | 516 (53) | 471 (60) | ||||
| Divorced | 41 (4) | 47 (6) | ||||
| Separated | 16 (2) | 19 (3) | ||||
| Widowed | 1 (<1) | 1 (<1) | ||||
| Single (never married) | 378 (39) | 229 (29) | ||||
| Not married (living with partner) | 15 (2) | 17 (2) | ||||
| Education,1 n (%) | 18.18* (2) | |||||
| High school | 238 (25) | 148 (19) | ||||
| College | 594 (61) | 475 (61) | ||||
| Graduate school | 135 (14) | 161 (20) | ||||
| Branch of service, n (%) | 66.44* (3) | 24.53* (4) | ||||
| Army | 490 (51) | 360 (46) | 814 (49) | 741 (48) | ||
| Air Force | 132 (13) | 199 (25) | 311 (19) | 362 (23) | ||
| Marines | 154 (16) | 52 (7) | 223 (14) | 198 (13) | ||
| Navy | 191 (20) | 173 (22) | 299 (18) | 230 (15) | ||
| Coast Guard | 5 (<1) | 21 (1) | ||||
| Rank, n (%) | 19.92* (2) | 99.30* (2) | ||||
| Enlisted | 299 (31) | 177 (22) | 962 (58) | 631 (41) | ||
| NCO | 516 (53) | 437 (56) | 515 (31) | 674 (43) | ||
| Officer | 152 (16) | 170 (22) | 175 (11) | 247 (16) | ||
| Duty, n (%) | 145.72* (2) | 397.00* (2) | ||||
| Active | 809 (84) | 452 (58) | 1384 (84) | 790 (51) | ||
| National Guard | 64 (6) | 124 (16) | 106 (6) | 323 (21) | ||
| Reserves | 94 (10) | 208 (26) | 162 (10) | 439 (28) | ||
| Other deployments2 | 124 (13) | 80 (10) | ||||
Sample characteristics
Relative to the other branches of the military (Army, Navy, Marines and Air Force), the sample contained a relatively small number of Coast Guard veterans (11 nondeployed; 4 deployed), who were excluded from all analyses. Furthermore, one member of the Gulf War-deployed group had missing data and was excluded from further analyses (Gulf War group, n=967; era group, n=784). Relative to the era veterans, a significantly greater proportion of Gulf War veterans were male, high-school educated, single during the war, and of African American or ‘other’ ethnic background (Table 3). The two groups were of comparable age. A significantly greater proportion of Gulf veterans were on active duty prior to the conflict, enlisted and in the Army or Marines, whereas a greater proportion of era veterans were in the National Guard or reserves prior to the conflict, officers and in the Air Force. However, comparison of the demographic profiles of the samples for Gulf War and era veterans provided by the Department of Defense revealed differences between the two groups similar to those reflected in our sample of respondents. That is, Gulf War veterans were somewhat younger and had a greater proportion of African Americans than the era group. The Gulf War group also had a greater proportion of men on active duty, in the Army, Navy or Marines, and of enlisted rank, than the era group (Table 3).
Twelve-month prevalence of psychiatric disorders
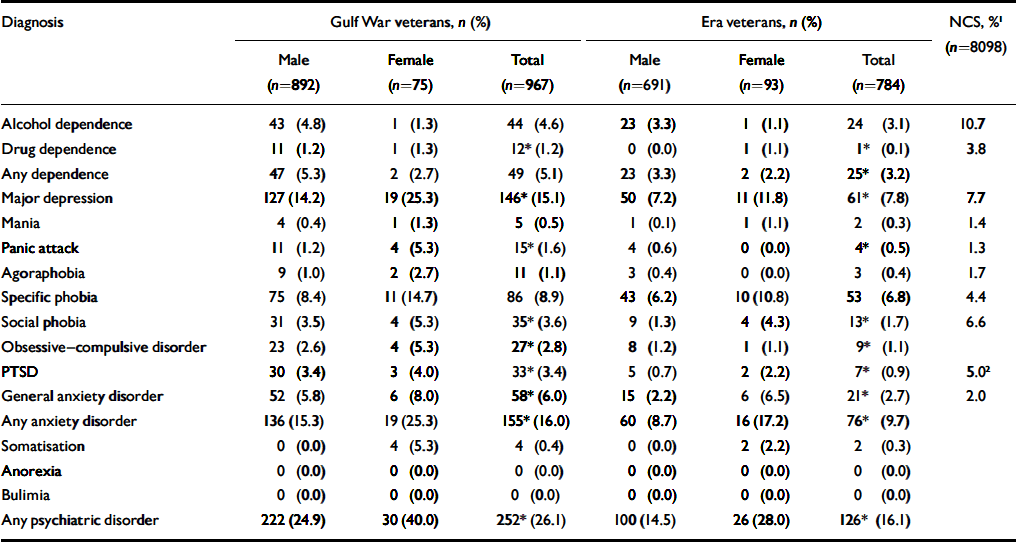
Overall, the Gulf War veterans met criteria for one or more psychiatric disorders more often than the era group (Table 4). Although little difference was seen in rates of alcohol dependence, specific phobia, mania and somatisation, prevalence rates for the remaining anxiety disorders, depression and drug dependence were two to three times higher for the Gulf War group relative to the era group. Within the former group, women had higher rates of every disorder except alcohol and drug dependence. Within the era group, women had higher rates of every disorder except alcohol dependence. For all psychiatric disorders, women in the era group had higher rates than male Gulf War veterans.
Table 4 Twelve-month prevalence of psychiatric diagnosis for Gulf War veterans v. era veterans, males v. females
| Diagnosis | Gulf War veterans, n (%) | Era veterans, n (%) | NCS, %1 (n=8098) | ||||
|---|---|---|---|---|---|---|---|
| Male (n=892) | Female (n=75) | Total (n=967) | Male (n=691) | Female (n=93) | Total (n=784) | ||
| Alcohol dependence | 43 (4.8) | 1 (1.3) | 44 (4.6) | 23 (3.3) | 1 (1.1) | 24 (3.1) | 10.7 |
| Drug dependence | 11 (1.2) | 1 (1.3) | 12* (1.2) | 0 (0.0) | 1 (1.1) | 1* (0.1) | 3.8 |
| Any dependence | 47 (5.3) | 2 (2.7) | 49 (5.1) | 23 (3.3) | 2 (2.2) | 25* (3.2) | |
| Major depression | 127 (14.2) | 19 (25.3) | 146* (15.1) | 50 (7.2) | 11 (11.8) | 61* (7.8) | 7.7 |
| Mania | 4 (0.4) | 1 (1.3) | 5 (0.5) | 1 (0.1) | 1 (1.1) | 2 (0.3) | 1.4 |
| Panic attack | 11 (1.2) | 4 (5.3) | 15* (1.6) | 4 (0.6) | 0 (0.0) | 4* (0.5) | 1.3 |
| Agoraphobia | 9 (1.0) | 2 (2.7) | 11 (1.1) | 3 (0.4) | 0 (0.0) | 3 (0.4) | 1.7 |
| Specific phobia | 75 (8.4) | 11 (14.7) | 86 (8.9) | 43 (6.2) | 10 (10.8) | 53 (6.8) | 4.4 |
| Social phobia | 31 (3.5) | 4 (5.3) | 35* (3.6) | 9 (1.3) | 4 (4.3) | 13* (1.7) | 6.6 |
| Obsessive—compulsive disorder | 23 (2.6) | 4 (5.3) | 27* (2.8) | 8 (1.2) | 1 (1.1) | 9* (1.1) | |
| PTSD | 30 (3.4) | 3 (4.0) | 33* (3.4) | 5 (0.7) | 2 (2.2) | 7* (0.9) | 5.02 |
| General anxiety disorder | 52 (5.8) | 6 (8.0) | 58* (6.0) | 15 (2.2) | 6 (6.5) | 21* (2.7) | 2.0 |
| Any anxiety disorder | 136 (15.3) | 19 (25.3) | 155* (16.0) | 60 (8.7) | 16 (17.2) | 76* (9.7) | |
| Somatisation | 0 (0.0) | 4 (5.3) | 4 (0.4) | 0 (0.0) | 2 (2.2) | 2 (0.3) | |
| Anorexia | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | |
| Bulimia | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | |
| Any psychiatric disorder | 222 (24.9) | 30 (40.0) | 252* (26.1) | 100 (14.5) | 26 (28.0) | 126* (16.1) | |
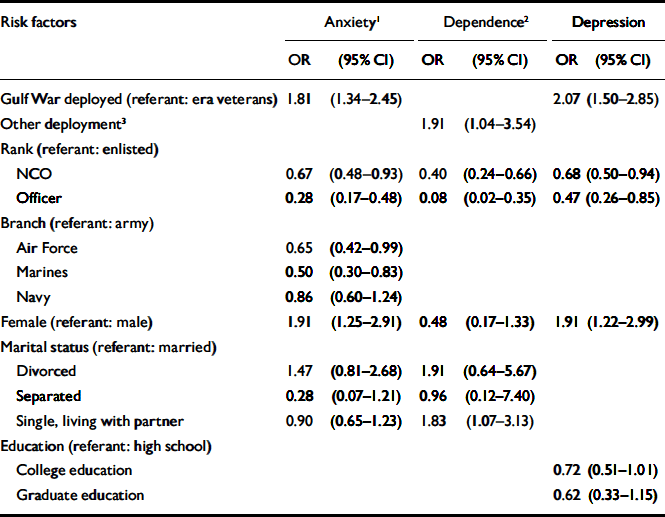
Table 5 Stepwise logistic regression models to predict psychiatric disorder
| Risk factors | Anxiety1 | Dependence2 | Depression | |||
|---|---|---|---|---|---|---|
| OR | (95% CI) | OR | (95% CI) | OR | (95% CI) | |
| Gulf War deployed (referant: era veterans) | 1.81 | (1.34-2.45) | 2.07 | (1.50-2.85) | ||
| Other deployment3 | 1.91 | (1.04-3.54) | ||||
| Rank (referant: enlisted) | ||||||
| NCO | 0.67 | (0.48-0.93) | 0.40 | (0.24-0.66) | 0.68 | (0.50-0.94) |
| Officer | 0.28 | (0.17-0.48) | 0.08 | (0.02-0.35) | 0.47 | (0.26-0.85) |
| Branch (referant: army) | ||||||
| Air Force | 0.65 | (0.42-0.99) | ||||
| Marines | 0.50 | (0.30-0.83) | ||||
| Navy | 0.86 | (0.60-1.24) | ||||
| Female (referant: male) | 1.91 | (1.25-2.91) | 0.48 | (0.17-1.33) | 1.91 | (1.22-2.99) |
| Marital status (referant: married) | ||||||
| Divorced | 1.47 | (0.81-2.68) | 1.91 | (0.64-5.67) | ||
| Separated | 0.28 | (0.07-1.21) | 0.96 | (0.12-7.40) | ||
| Single, living with partner | 0.90 | (0.65-1.23) | 1.83 | (1.07-3.13) | ||
| Education (referant: high school) | ||||||
| College education | 0.72 | (0.51-1.01) | ||||
| Graduate education | 0.62 | (0.33-1.15) | ||||
For depression, being deployed to the Gulf, female, high-school educated and enlisted were each significant independent predictors in the logistic regression model (see Table 5). Predictors for anxiety disorders included Gulf deployment, female gender, being divorced at the time of the Gulf War, enlisted relative to non-commissioned officer (NCO) or officer rank, and being in the Army relative to the other services. For alcohol or drug dependence, being male, enlisted, divorced, single or living with someone and deployment other than to the Persian Gulf were significant independent risk factors. No two-way interaction was a significant predictor for any of the psychiatric disorders.
DISCUSSION
Veterans deployed to the Gulf War had significantly higher prevalence of psychiatric diagnoses than era veterans, with deployment as a powerful predictor of current (past 12 months) depression and anxiety disorders approximately 10 years after the end of the Gulf War. These findings confirm and extend those of several previous studies among Gulf War veterans, showing increased psychological distress when assessed by questionnaire (Reference Perconte, Wilson and PontiusPerconte et al, 1993; Reference Stretch, Bliese and MarloweStretch et al, 1996; Reference Hallman, Kipen and DiefenbachHallman et al, 2003), increased reporting of physician-diagnosed PTSD and of hospitalisation for depression in a telephone survey (Reference McCauley, Lasarev and StickerMcCauley et al, 2002), and increased rates of depression, PTSD and alcohol misuse among deployed v. non-deployed veterans (Iowa Persian Gulf Study Group, 1997). Despite the frequency and psychological stress associated with deployment among service personnel, our study is one of the few to evaluate the effects of deployment on the 12-month prevalence of Axis I DSM–IV psychiatric disorders (excluding psychoses) among random samples of veterans.
For a subset of veterans deployed to sites in addition to the Gulf, these other deployments were associated with an increased risk of alcohol/drug dependence but not of depression or anxiety disorders. Experiencing multiple deployments and being single or divorced may increase the risk of alcohol/drug dependence because of isolation and lack of support, both of which have been associated with increased risk of substance misuse (Reference Grant, Stinson and HarfordGrant et al, 2001; Reference Schuckit and SmithSchuckit & Smith, 2001). Other deployments included locations such as Vietnam, for which significantly elevated rates of alcohol misuse or dependence (13.7%) have been reported (CDC Vietnam Experience Study, 1988). However, the number of veterans (n=204) with other deployments is substantially smaller than the number of veterans deployed to the Gulf, making these results less reliable.
Rank and psychiatric disorder
Enlisted status relative to NCO and officer rank was associated with increased risk of multiple psychiatric disorders including anxiety, depression and drug/alcohol dependence. Other investigators of Gulf War veterans have also reported that lower rank is associated with poorer psychological and physical health (Reference Ismail, Blatchley and HotopfIsmail et al, 2000) and increased risk of multisymptom illness (Reference Fukuda, Nisenbaum and StewartFukuda et al, 1998; Reference Gray, Hawksworth and SmithGray et al, 1998). In our study, being in the Army increased the risk of an anxiety disorder, whereas being in the Air Force, Marines or Navy was protective. These findings suggest that those with the least control by virtue of lower rank are more likely to be adversely affected by their war experience years after the war has ended, although causality cannot be inferred from the present study design. Furthermore, lower rank may be a surrogate for lower socio-economic status: this is known to contribute to psychiatric disorders and the stresses that accompany lower status may have contributed to the onset of psychiatric conditions after the war and/or made it difficult to receive adequate care for psychiatric conditions that began during the war.
Demographic predictors of psychiatric disorder
Non-military factors, including education, marital status during the war and gender were also predictive of current psychiatric disorders. Similar to previous findings from community samples (Reference Neeleman, Ormel and BijlNeeleman et al, 2001), veterans with the lowest level of education were at increased risk of depression relative to their better-educated peers, and veterans who were divorced at the time of their service in the Gulf were at increased risk of anxiety disorder and drug/alcohol dependence relative to those who were married. Divorce has been associated with increased symptoms of anxiety and depression among individuals both as they go through divorce (Reference Hackney and RibordyHackney & Ribordy, 1980) and also years after the divorce (Reference Richards, Hardy and WadsworthRichards et al, 1997). Predictors of dependence disorders included being male and divorced or single/living with a partner, findings consistent with community studies that show higher rates of alcohol/drug dependence among males (Reference Kessler, McGonagle and ZhaoKessler et al, 1994; Reference Grant, Stinson and HarfordGrant et al, 2001) and among those who are divorced or never married (Reference Richards, Hardy and WadsworthRichards et al, 1997; Reference Grant, Stinson and HarfordGrant et al, 2001). These factors suggest that those with less education or who have other stressors such as divorce show increased risk of psychiatric disorder beyond the risks associated with military service. Similar to nonmilitary samples, women were consistently at greater risk for anxiety and depression but at less risk than men for drug/alcohol dependence (Reference Kessler, McGonagle and ZhaoKessler et al, 1994). Unwin et al (Reference Unwin, Hotopf and Hull2002) did not find gender differences among UK service personnel deployed to the Persian Gulf conflict and to Bosnia. However, they evaluated psychological symptoms rather than psychiatric diagnoses.
Comparison with the National Comorbidity Survey
Although veterans in our study were most probably healthier than the representative sample of the US population participating in the National Comorbidity Survey (Reference Kessler, McGonagle and ZhaoKessler et al, 1994), the 12-month prevalence of psychiatric disorders for males in the Survey provides a rough comparison for males in our study (see Table 4). Rates of major depression, generalised anxiety and simple phobia were approximately doubled for deployed male veterans relative to the male Survey sample, which in turn were comparable to the prevalence of these disorders for non-deployed veterans. Prevalence rates of agoraphobia without panic, panic disorder, social phobia, mania and drug and alcohol dependence were either comparable or lower among deployed male veterans relative to US males. With the exception of generalised anxiety, our results suggest that non-deployed women were at no greater risk of any disorder relative to community rates reported by Kessler et al (Reference Kessler, McGonagle and Zhao1994), although the number of women in our study limits the reliability of our findings.
Rates of PTSD in the Gulf Wardeployed troops were below those reported by the National Comorbidity Survey, but the latter evaluated lifetime rather than 12-month prevalence. Similarly, McCauley et al (Reference McCauley, Lasarev and Sticker2002) and Wolfe et al (Reference Wolfe, Proctor and Erickson1999) also reported higher rates of PTSD than in our study, although the rates reported by McCauley et al (Reference McCauley, Lasarev and Sticker2002) were based on participants’ report of a physician diagnosis over the 9 years since the Gulf War, whereas the Wolfe et al (Reference Wolfe, Proctor and Erickson1999) rates were based on a relatively smaller subsample of Gulf War veterans who were high and low symptom reporters and oversampled for women. The current rates for PTSD, however, were comparable with the 3% reported by Ismail et al (Reference Ismail, Kent and Brugha2002) for disabled UK Gulf War veterans, disabled Bosnia veterans and era veterans based on assessment of symptoms during the past 4 weeks. Thus, the 12-month prevalence rates of PTSD are comparable for veterans who were deployed and veterans who were disabled, and may reflect the fact that Gulf War veterans’ combat exposure was relatively less than in previous wars. Prevalence of somatisation was low among Gulf War veterans and was not diagnosed for any era veterans, a finding also consistent with that of Ismail et al (Reference Ismail, Kent and Brugha2002), who reported a low prevalence of somatisation disorder among disabled Gulf veterans with no case of somatisation among non-disabled Gulf veterans, disabled Bosnia veterans or era veterans. Ismail et al (Reference Ismail, Kent and Brugha2002) reported an increased prevalence of undifferentiated somatoform disorders among disabled Gulf War veterans relative to their comparison groups. This finding appears consistent with increased prevalence of unexplained symptoms among disabled Gulf War veterans, since these symptoms often overlap those defining undifferentiated somatoform disorders.
Implications of the study
This study is the largest random sample of US Gulf War-deployed and era veterans in which a standardised and validated method was used to evaluate all Axis I psychiatric disorders. Although the sample size was relatively large, the overall response rate was suboptimal and may attenuate the generalisability of this study. Respondents differed from non-respondents, with the most notable differences being the greater proportions of White and NCO/officer rank individuals volunteering for the study. However, such differences are a typical bias in epidemiological surveys, for which White individuals and those with more education are more likely to volunteer. Furthermore, demographic factors were controlled for in the logistic regression models used to predict psychiatric disorders. The psychiatric diagnoses remain provisional, since interviews were conducted by lay interviewers rather than trained clinicians. However, because the CIDI is designed for use by unqualified interviewers, reliance on clinical judgement is minimised.
The study's results reflect the 12-month prevalence of psychiatric disorders and do not address the prevalence of psychiatric morbidity for the entire period from the end of the conflict up to 10 years after the war. Nevertheless, when other known risk factors for psychiatric illness such as gender, divorce and educational attainment were controlled for, having been deployed remained a significant, independent risk factor for diagnoses of anxiety and/or depression, whereas being of lower rank (i.e. enlisted) increased risks for all psychiatric disorders. These findings suggest that in addition to the usual demographic risk factors for psychiatric illness, veterans have the burden of increased risk as a result of their deployment, particularly if they were of lower rank. The effects of a relatively brief war with limited physical trauma have a lasting impact on veterans that could be attenuated by prevention programmes to reduce the impact of war on veterans’ mental health.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Deployment contributes to psychiatric morbidity among veterans 10 years after the war.
-
▪ Veterans of lower rank are at greater risk of psychiatric disorder.
-
▪ Prevention and debriefing programmes need to be developed to mitigate the impact of deployment.
LIMITATIONS
-
▪ The response rate of veterans in the sample was suboptimal.
-
▪ Psychiatric diagnoses were provisional.
-
▪ Respondents were more likely to be White and of non-commissioned officer or officer rank.
Acknowledgements
We thank the members of our scientific advisory committee, Evelyn Bromet, PhD, Javier Escobar, MD, Steven Stellman, PhD, and William C. Reeves, MD, who offered invaluable input into the research design and execution of this study. Dr Ronald Kessler contributed his expertise in the design of our psychiatric interview and graciously allowed us the use of the Composite International Diagnostic Interview – Short Form/Diagnostic and Statistical Manual IV. In addition, we thank Joyce Kosmoski, who assisted with numerous revisions of the manuscript.
Research, in part, was supported by grants from the Centers for Disease Control and Prevention (CDC; U50/CCU214463) and the National Institute of Environmental Health Sciences Center (P30ESO5022). The CDC awarded the University of Medicine and Dentistry of New Jersey and Robert Wood Johnson Medical School a cooperative agreement to conduct this project. Consequently, scientists with the CDC were involved in the study design, collection, analysis and interpretation of the data, and also reviewed the manuscript before it was submitted for publication.










eLetters
No eLetters have been published for this article.