Although avoidant personality disorder is highly prevalent in the community (e.g. Reference Torgersen, Kringlen and CramerTorgersen et al, 2001) and is associated with even more impairment than major depression (Reference Skodol, Gunderson and McGlashanSkodol et al, 2002), to date no study has compared the effectiveness of different types of individual psychotherapy for people with this disorder. Two studies evaluated the effectiveness of various individual psychotherapies for cluster C personality disorders (Winston et al, Reference Winston, Pollack and McCullough1991, Reference Winston, Laikin and Pollack1994; Reference Svartberg, Stiles and SeltzerSvartberg et al, 2004), but neither study specifically analysed the results for individuals with avoidant disorder.
Our study was designed to evaluate the comparative effectiveness of brief dynamic therapy and cognitive-behavioural therapy for patients with avoidant personality disorder as their primary problem. Given the overlap of traits in cluster C personality disorders (Reference Van Velzen, Emmelkamp, Derksen, Groen and Maffeivan Velzen & Emmelkamp, 1999), we were interested not only in the results of treatment on avoidance and social distress but also in whether treatment effects generalised to dependent and obsessive-compulsive traits.
METHOD
Patients
Patients referred consecutively to the Community Mental Health Centre in Groningen in the northern part of The Netherlands were screened by means of the Personality Diagnostic Questionnaire for DSM-IV (PDQ-4; Reference HylerHyler, 1994). Patients younger than 23 years old were excluded, given that the personality disorder diagnosis requires a stable, chronic pattern, not being influenced by adjustment in the transition from adolescence to adulthood. Patients older than 65 years were not approached. Patients who fulfilled the criteria for avoidant personality disorder on the PDQ-4 and met the inclusion criteria were asked to take part in the study, which was approved by the ethics committee of the Department of Psychology at the University of Groningen and by the national ethics committee for research with patients in psychiatry (Bennekom). Of these 127 eligible patients, 114 signed the informed consent form and were subsequently invited for a face-to-face structured interview using the Structured Clinical Interview for DSM-IV Axis II Disorders (SCID-II; Reference First, Spitzer and GibbonFirst et al, 1996). Exclusion criteria were:
-
(a) avoidant personality disorder not the primary disorder;
-
(b) a history of psychotic disorder;
-
(c) a high risk of suicide;
-
(d) patient currently undergoing psychotherapy or having had psychotherapy in the previous 3 years;
-
(e) patient unable to complete questionnaires.
Of the 114 patients who consented to possible inclusion in the trial, 49 did not meet the entry criteria and 3 refused to participate. The reasons for exclusion were as follows:
-
(a) patients did not fulfil criteria for avoidant personality disorder on the SCID-II (n=30);
-
(b) other personality disorders were more important (n=10: paranoid 3, schizotypal 1, dependent 2, depressive 3, not otherwise specified 1);
-
(c) severe Axis I disorder required immediate treatment (n=7: depressive disorder 4, obsessive-compulsive disorder 1, panic disorder and agoraphobia 1, somatoform disorder 1);
-
(d) patients chose pharmacotherapy instead of psychological therapy (n=2).
This left 62 patients for inclusion in the trial. The sample (30 men, 32 women) ranged in age from 24 years to 61 years (mean=34.3, s.d.=8.9). Educational level ranged from elementary (14%), medium (24%), above average (36%) to high (26%). Patients were randomly assigned to cognitive-behavioural therapy (CBT; n=21), brief dynamic therapy (BDT; n=23) or a waiting-list control group (n=18). Patients in the control group were randomly assigned to receive one of the therapies (CBT, n=18, BDT, n=8) after the waiting period (Fig. 1).

Fig. 1 Progress of participants through the trial (BDT, brief dynamic therapy; CBT, cognitive-behavioural therapy; WLC, waiting-list control).
Therapists
The psychotherapists were either licensed psychiatrists or psychologists. All had at least 5 years of postgraduate clinical experience. Twelve female and four male therapists participated in the study. Therapists were versed in either cognitive-behavioural or brief dynamic therapy. All therapists were monitored by means of audiotapes, which were analysed by reviewers masked to the therapist's identity for adherence to treatment strategies. Therapists were trained and supervised by qualified supervisors: those providing cognitive-behavioural therapy were supervised by A.B. and A.K. and those providing brief dynamic therapy by G.A.F. and H.C.K.
Treatments
Treatment consisted of 20 sessions over a 6-month period. Individual treatment sessions, each lasting 45 min, were scheduled once a week. Both treatment approaches were manual-guided.
Cognitive-behavioural therapy
Cognitive-behavioural therapy is based on the assumption that anxiety and avoidance are related to individuals' maladaptive beliefs and related thought processes. The model emphasises collaborative interactions between patient and therapist in conjunction with specific cognitive and behavioural techniques such as Socratic dialogue, monitoring of beliefs, analysing advantages and disadvantages of avoidance, activity monitoring and scheduling, graded exposure assignments, behavioural experiments and role-play (Reference Beck and FreemanBeck & Freeman, 1990; Reference Emmelkamp, Bouman and ScholingEmmelkamp et al, 1992).
Brief dynamic therapy
Brief dynamic therapy is based on the assumption that anxiety and avoidance are related to individuals' unconscious psychodynamic conflicts, in addition to which shame has a major role. Treatment was directed at defence and affect restructuring. The model emphasises a therapeutic alliance on the basis of which the most essential unconscious conflict can be clarified and resolved with the help of expressive techniques such as clarification, confrontation and, especially, interpretation (Malan, Reference Malan1976, Reference Malan1979). However, in a number of cases a more supportive attitude and technique was used to bolster threatened equilibrium and relieve the consequences of unconscious conflict by means of methods such as suggestion, reassurance and encouragement (primarily supportive mode) (Reference LuborskyLuborsky, 1984; Reference Luborsky, Mark, Crits-Cristoph and BarberLuborsky & Mark, 1991; Reference Pinsker, Rosenthal, McCullough, Crits-Cristoph and BarberPinsker et al, 1991). In these instances the therapist clarifies rather than confronts defences in order to regulate rather than to provoke anxiety.
Waiting-list control
Patients in the control condition received no therapy between the initial assessment and the post-treatment assessment 20 weeks later.
Assessment
Diagnoses were derived using the SCID-II, completed by an independent clinician (a psychologist). The SCID-II was limited to the subset of personality disorders that screened positive on the PDQ-4. Our primary outcome measures were SCID-II diagnosis by an independent assessor at the 6-month follow-up, and self-report measures completed by the patients at three time points: pre-treatment, immediately post-treatment and 6 months after the treatment was completed. Self-report measures included the Personality Disorder Belief Questionnaire (PDBQ; Reference Arntz, Dreessen and SchoutenArntz et al, 2004) avoidant personality sub-scale; the Lehrer Woolfolk Anxiety Symptoms Questionnaire (LWASQ; Reference Scholing and EmmelkampScholing & Emmelkamp, 1992); the social phobia sub-scale of the Social Phobia Anxiety Inventory (SPAI; Reference Beidel, Borden and TurnerBeidel et al, 1989); and the Avoidance Scale, consisting of five idiosyncratic situations which were avoided pre-treatment (Reference EmmelkampEmmelkamp, 1982). To assess whether treatment applied to other personality traits from the cluster C domain, participants also completed the PDBQ dependent and obsessive-compulsive sub-scales.
RESULTS
Statistical analysis
Time effects per group were analysed with t-tests for dependent samples. Between-group effects were tested with univariate analyses of covariance, with the pre-treatment test as covariate. To assess treatment differences between control group patients and patients who received therapy, improvements in patients who started the intervention treatment immediately were compared with the results of the no-treatment phase of the control group patients. To assess the eventual differences between the active treatments, data of patients who started treatment immediately were pooled with the data of patients who received the treatments after the waiting-list period, in order to enhance statistical power. After weighing the risks of chance findings v. loss of power, a significance level of α=0.1 was set for the analyses in the between-group comparisons.
Six patients in total withdrew before the post-treatment assessment: two from the control group, one who never started treatment (from the CBT group), two who discontinued treatment prematurely from the CBT group and one with missing data (BDT group). In one case (CBT) treatment had to be continued between the post-treatment and follow-up assessments, which meant the data could not be used in the follow-up analysis. Five patients (two from the CBT group and three from the BDT group) did not show up for the follow-up assessment, and in the BDT group follow-up questionnaires were missing for two patients, leaving 46 cases for follow-up analyses.
The mean actual number of therapy sessions was 18.5 (range 14-20) in the CBT group and 18.8 (range 13-20) in the BDT group.
Within-group differences
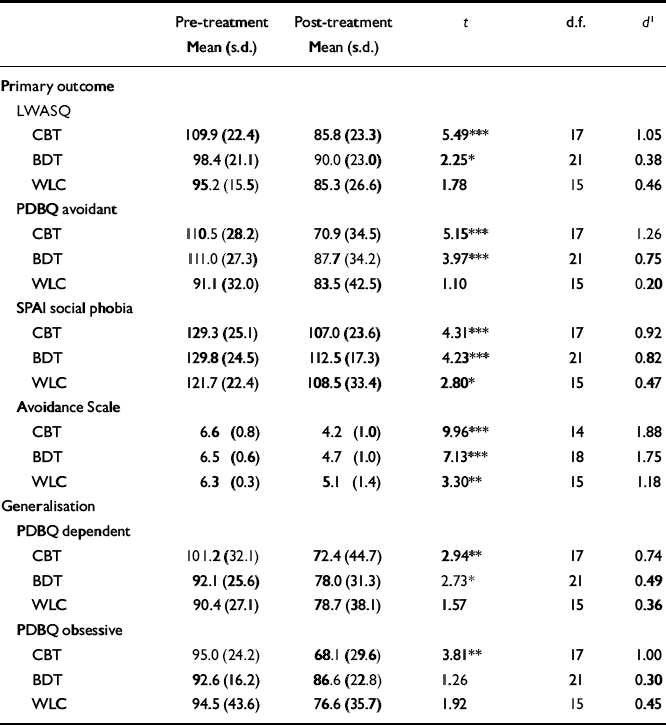
Results of treatment are shown in Table 1. Both intervention therapies as first treatment led to significant improvement on all primary outcome measure (PDBQ avoidant sub-scale, LWASQ, SPAI social phobia sub-scale and Avoidance Scale) and on the generalisation measure PDBQ dependent sub-scale. In addition, cognitive-behavioural therapy led to significant improvement on the PDBQ obsessive-compulsive sub-scale. Control group patients significantly improved between pre-treatment and post-treatment assessments on the SPAI social phobia sub-scale and the Avoidance Scale. The effect sizes that were computed mirror this pattern of changes. According to Cohen (Reference Cohen1977), effect sizes of 0.20, 0.50 and 0.80 may be considered to correspond to small, medium and large effects respectively. According to this rule of thumb, the effect sizes of cognitive-behavioural therapy are large on five out of six measures, the effects of brief dynamic therapy are generally medium to large, and the effects of the control condition are small to medium (apart from the Avoidance Scale measure, for which the effect size can be considered large).
Table 1 Scores on outcome measures at the pre-treatment and post-treatment assessments
| Pre-treatment Mean (s.d.) | Post-treatment Mean (s.d.) | t | d.f. | d 1 | |
|---|---|---|---|---|---|
| Primary outcome | |||||
| LWASQ | |||||
| CBT | 109.9 (22.4) | 85.8 (23.3) | 5.49 *** | 17 | 1.05 |
| BDT | 98.4 (21.1) | 90.0 (23.0) | 2.25 * | 21 | 0.38 |
| WLC | 95.2 (15.5) | 85.3 (26.6) | 1.78 | 15 | 0.46 |
| PDBQ avoidant | |||||
| CBT | 110.5 (28.2) | 70.9 (34.5) | 5.15 *** | 17 | 1.26 |
| BDT | 111.0 (27.3) | 87.7 (34.2) | 3.97 *** | 21 | 0.75 |
| WLC | 91.1 (32.0) | 83.5 (42.5) | 1.10 | 15 | 0.20 |
| SPAI social phobia | |||||
| CBT | 129.3 (25.1) | 107.0 (23.6) | 4.31 *** | 17 | 0.92 |
| BDT | 129.8 (24.5) | 112.5 (17.3) | 4.23 *** | 21 | 0.82 |
| WLC | 121.7 (22.4) | 108.5 (33.4) | 2.80 * | 15 | 0.47 |
| Avoidance Scale | |||||
| CBT | 6.6 (0.8) | 4.2 (1.0) | 9.96 *** | 14 | 1.88 |
| BDT | 6.5 (0.6) | 4.7 (1.0) | 7.13 *** | 18 | 1.75 |
| WLC | 6.3 (0.3) | 5.1 (1.4) | 3.30 ** | 15 | 1.18 |
| Generalisation | |||||
| PDBQ dependent | |||||
| CBT | 101.2 (32.1) | 72.4 (44.7) | 2.94 ** | 17 | 0.74 |
| BDT | 92.1 (25.6) | 78.0 (31.3) | 2.73 * | 21 | 0.49 |
| WLC | 90.4 (27.1) | 78.7 (38.1) | 1.57 | 15 | 0.36 |
| PDBQ obsessive | |||||
| CBT | 95.0 (24.2) | 68.1 (29.6) | 3.81 ** | 17 | 1.00 |
| BDT | 92.6 (16.2) | 86.6 (22.8) | 1.26 | 21 | 0.30 |
| WLC | 94.5 (43.6) | 76.6 (35.7) | 1.92 | 15 | 0.45 |
BDT, brief dynamic therapy; CBT, cognitive–behavioural therapy; LWASQ, Lehrer Woolfolk Anxiety Symptoms Questionnaire; PDBQ, Personality Disorder Belief Questionnaire; SPAI, Social Phobia Anxiety Inventory; WLC, waiting-list control
1. Cohen's d effect size: d=0.20 is small, d=0.50 is medium and d > 0.80 is large
* P < 0.05
** P < 0.01
*** P < 0.001
Treatment v. no treatment
Analyses of covariance to assess differences between CBT (n=18) and BDT (n=22) v. control (n=16) revealed that CBT was significantly superior to the control condition on primary outcome measures PDBQ avoidant sub-scale (F (1,52)=7.39, P=0.01) and Avoidance Scale (F (1,46)=5.39, P=0.02). No significant difference was found between BDT and control.
CBT v. BDT post-treatment
Analyses of covariance to assess differences between CBT (n=26) and BDT (n=28) revealed that CBT was significantly superior to BDT on all primary outcome measures: PDBQ avoidant sub-scale (F (1,51)=5.92, P=0.02), LWASQ (F (1,51)=5.69, P=0.02), SPAI social phobia sub-scale (F (1,51)=2.98, P=0.09) and Avoidance Scale (F (1,45)=5.25, P=0.03), and on the generalisation measure PDBQ obsessive-compulsive sub-scale (F (1,51)=10.84, P=0.002). On none of the measures was BDT superior to CBT.
CBT v. BDT at follow-up
In the period between post-treatment assessment and follow-up, no treatment took place. A comparison between the post-treatment and follow-up scores for CBT (n=23) and BDT (n=23) groups revealed that results were maintained. Only brief dynamic therapy resulted in significant improvement on the PDBQ obsessive-compulsive scale (t (22)=2.14, P=0.04).
Analyses of covariance to assess differences between CBT and BDT at follow-up revealed that CBT was significantly superior to BDT on the PDBQ avoidant sub-scale (F (1,40)=5.96, P=0.02), PDBQ obsessive-compulsive sub-scale (F (1,44)=5.95, P=0.02) and PDBQ dependent sub-scale (F (1,44)=6.144, P=0.02).
At follow-up, patients were reassessed with the SCID-II. In the CBT group 2 out of 22 patients (9%) and in the BDT group 9 out of 25 patients (36%) still fulfilled the criteria for avoidant personality disorder. The difference was statistically significant (χ2=4.73, P=0.03).
DISCUSSION
This is the first randomised trial involving a clinical sample of patients with avoidant personality disorder as their primary complaint in which two types of individual therapy - cognitive-behavioural and brief dynamic therapy - are compared with a waiting-list control group in terms of outcome measures. Our findings add useful empirical data to the scant research on the effect of different types of psychotherapy on avoidant personality disorder (Reference Alden, Laposa and TaylorAlden et al, 2002) and shed some light on the relative efficacy of the two therapies in this disorder. The results at the post-treatment assessment indicate that the most favourable outcome at this stage was obtained from cognitive-behavioural therapy: this was more effective than waiting-list control for some measures and was more effective than brief dynamic therapy for all primary outcome measures. This order of effectiveness (CBT>BDT>control) was also reflected in Cohen's d effect sizes. The use of within-condition effect sizes allows ready comparison of the magnitude of change across measures within a study.
At follow-up, improvements within patient groups were stable: some patients improved between the post-treatment assessment and follow-up, whereas others relapsed slightly. At follow-up, the difference in effectiveness between the two therapies was still seen: cognitive-behavioural therapy was found to be significantly superior to brief dynamic therapy on four out of seven measures. On follow-up, the SCID-II test showed that only 9% of the CBT group were still classed as having avoidant personality disorder, whereas 36% of the BDT group still fulfilled the diagnostic criteria. This was a significant difference. This finding is of considerable clinical interest, given that of all the personality disorders the avoidant type is found to be the most persistent (Reference Shea, Stout and GundersonShea et al, 2002), even tending to worsen over time (Reference Seivewright, Tyrer and JohnsonSeivewright et al, 2002). In the Collaborative Longitudinal Personality Disorders study (Reference Shea, Stout and GundersonShea et al, 2002), 67% of patients with avoidant disorder still fulfilled the criteria for this disorder at 6-month follow-up, despite the fact that most patients had received clinical care. The reduction in disorder in our study of 64% in the BDT group is substantial and that of 91% in the CBT group is very substantial in comparison with the 33% reduction in the study by Shea et al (Reference Shea, Stout and Gunderson2002).
Results of brief dynamic therapy in our study were statistically significant with effect sizes ranging from medium to large, but were less than those achieved with cognitive-behavioural therapy. It should be noted, however, that the results of the latter therapy on self-report measures were also modest. It is unclear whether prolonged treatment would have resulted in superior results. Other studies investigating brief dynamic psychotherapy (Reference Winston, Laikin and PollackWinston et al, 1994; Reference Svartberg, Stiles and SeltzerSvartberg et al, 2004) usually involved 40 sessions. Whether prolonging therapy after 20 sessions would enhance the effectiveness of treatment needs to be investigated.
To date, few studies have evaluated the effects of (cognitive) behavioural therapy in patients with avoidant personality disorder. Our study supports earlier studies that evaluated behavioural treatments in patients classified as having this disorder (Reference AldenAlden, 1989; Reference Renneberg, Goldstein and PhillipsRenneberg et al, 1990; Reference Stravinsky, Belisle and MarcouillerStravinsky et al, 1994). The behavioural treatments investigated in these studies included social skills training and exposure to real-life social situations, but none looked at cognitive therapy. Whether cognitive therapy enhances the effects of behavioural therapy deserves further study.
In interpreting the findings of our study, several limitations should be considered. The first limitation was engendered by the need to balance methodological and ethical concerns. More specifically, for ethical reasons it was decided that patients assigned to the waiting-list control group could not be denied treatment for longer than the 20-week waiting period. This meant we were not able to assess the long-term effects of the intervention therapies in comparison with this control group. Moreover, all patients in the waiting-list group knew that they would eventually receive treatment, which might have influenced results at the post-treatment assessment. The (limited) improvements seen in the control group might be related to the positive effect of expectancy and hope.
Given the large number of therapists (n=16) involved in this study, results are likely to generalise to other community mental health settings. However, it should be noted that the therapists were experts in their respective forms of psychotherapy. Furthermore, they were selected and trained for this project and supervised during the study. Consequently, it is unknown whether our findings would apply to untrained therapists working in other kinds of community setting.
In summary, our results suggest that cognitive-behavioural therapy is superior to waiting-list control and brief dynamic therapy. There was no evidence that brief dynamic therapy was more effective than the waiting-list control. Given the high prevalence of avoidant personality disorder in the community (Reference Torgersen, Kringlen and CramerTorgersen et al, 2001), the persistence of the disorder (Reference Shea, Stout and GundersonShea et al, 2002) and the high level of functional impairment associated with the disorder (Reference Van Velzen, Emmelkamp and Scholingvan Velzen et al, 2000; Reference Skodol, Gunderson and McGlashanSkodol et al, 2002), our findings on the effectiveness of different types of therapy for this condition provide an important step forward for community mental healthcare.
Acknowledgements
The study was supported financially by funds from GGz Groningen and by a programme grant from the Mental Health Research Foundation VCVGZ (Stichting tot Steun, Bennekom). The sustained cooperation in the research by the patients is acknowledged, as are the consistent efforts of the therapists and the independent clinical assessors.







eLetters
No eLetters have been published for this article.