As evidenced by several trials there are effective psychosocial treatments for social phobia (Reference Rodebaugh, Holaway and HeimbergRodebaugh et al, 2004). However, far from all of those with this condition seek treatment (Reference Baldwin, Buis, Bandelow and SteinBaldwin & Buis, 2004). Apart from a shortage of skilled therapists, long waiting lists and high costs, a major problem is that those with social phobia may not seek therapy because of the fear of embarrassment associated with help-seeking (Reference King and PoulosKing & Poulos, 1998; Reference Newman, Erickson and PrzeworskiNewman et al, 2003). Consequently, a challenge is to increase the accessibility of evidence-based psychological treatment. A recent approach is internet-based self-help with minimal therapist contact by email (Reference Andersson, Carlbring and HolmströmAndersson et al, 2006). Although the results are promising, there is a problem with treatment adherence. In this study we attempted to increase adherence by adding short, weekly telephone calls to the internet-based self-help programme.
METHOD
Participants were selected by means of a computerised screening interview consisting of the highly specific and sensitive Social Phobia Screening Questionnaire (SPSQ; Reference Furmark, Tillfors and EverzFurmark et al, 1999), the self-rated version of the Montgomery–Åsberg Depression Rating Scale (MADRS–S; Reference Svanborg and AsbergSvanborg & Åsberg, 1994) and ten additional questions regarding current and past treatment. To be included in the study, participants had to meet the following ten criteria:
-
(a) fulfil the DSM–IV (American Psychiatric Association, 1994) criteria for social phobia according to the SPSQ;
-
(b) have a total score of below 31 on the MADRS–S depression scale and a score of less than 4 on the suicide item of this scale;
-
(c) agree to undergo no other psychological treatment for the duration of the study, and have no history of earlier cognitive–behavioural therapy;
-
(d) if taking prescribed drugs for anxiety or depression, the dosage had to be constant for 3 months before the start of the treatment, and the participants had to agree to keep the dosage constant throughout the study;
-
(e) have access to a computer with internet connection;
-
(f) be at least 18 years old;
-
(g) live in Sweden;
-
(h) be able to speak to the therapists on the telephone on a weekly basis
-
(i) following telephone-administration (Structured Clinical Interview for DSM–IV, SCID; Reference First, Gibbon and SpitzerFirst et al, 1997), must have social phobia as the primary diagnosis if other comorbid disorders were present;
-
(j) not currently meet diagnostic criteria for psychosis or substance misuse.
Excluded participants were sent personal emails encouraging them to seek help elsewhere.
Of the 243 individuals who applied to participate, 127 fulfilled the first eight criteria. Of these individuals, the first 62 who were reachable by telephone were included. Out of this number 60 met all ten inclusion criteria and were divided into two groups (treatment or waiting-list control) by an online true random-number service independent of the investigators and therapists. This service is run by the Department of Computer Science at the University of Dublin and the numbers are generated using a purely random process (atmospheric disturbances in space). All participants were informed about the risk of unauthorised interception of emails and were advised to use a free email service that automatically encrypts messages. The study protocol was approved by the ethics committee, and written informed consent was obtained from all participants.
Outcome measures
The following social anxiety scales constituted the primary outcome measures: the Liebowitz Social Anxiety Scale self-report version (LSAS–SR; Reference LiebowitzLiebowitz, 1987), the Social Phobia Scale (SPS) and Social Interaction Anxiety Scale (SIAS; Reference Mattick and ClarkeMattick & Clarke, 1998) and the Social Phobia Screening Questionnaire (SPSQ; Reference Furmark, Tillfors and EverzFurmark et al, 1999). In addition, the following secondary measures were used to assess general anxiety, depression and quality of life: the Beck Anxiety Inventory (BAI; Reference Beck, Epstein and BrownBeck et al, 1988), the MADRS–S (Reference Svanborg and AsbergSvanborg & Åsberg, 1994), and the Quality of Life Inventory (QoLI; Reference Frisch, Cornell and VillanuevaFrisch et al, 1992). The outcome measures were administered after all inclusion criteria were met, i.e. after the SCID interview. Internet administration of questionnaires has generally resulted in adequate psychometric properties (see Reference Carlbring, Brunt and BohmanCarlbring et al, 2007).
Intervention
Whereas those in the control group remain on a waiting list and receive no treatment, those in the treatment group receive internet-administered self-help including minimal therapist contact via email supplemented with short weekly telephone calls as outlined below.
Treatment
The treatment was based on established cognitive–behavioural methods as described in self-help books (e.g. Reference RapeeRapee, 1998; Reference Antony and SwinsonAntony & Swinson, 2000). The text, consisting of 186 pages, was taken from an existing manual (Reference Furmark, Holmström and SparthanFurmark et al, 2006), divided into nine modules and adapted for the internet. Each module included information, exercises and an interactive quiz, and ended with three to eight essay questions. Participants were asked to explain in their own words the most important sections of the module they had just completed, provide thought records, and describe their experience with and outcome of their exposure exercises. The questions were intended to promote learning and to enable the online therapists to assess whether the participants had assimilated the material. For each module participants were required to post at least one message in an online discussion group about a predetermined topic.
Feedback on homework assignments was usually given within 24 h after participants had sent their answers by email. On the basis of these emails, an assessment was made of whether the participant was ready to continue; if so, the password to the next module was sent. If not, the participant received instructions on what needed to be completed before proceeding to the next module.
Telephone calls
One weekly telephone call was made by the therapists to each participant in the treatment group. The purpose was to provide positive feedback and to answer any questions the participant might have regarding the modules. All conversations were timed, and each of the nine calls lasted an average of 10.5 min (s.d.=3.6).
Therapists
The therapists were two students completing their last semester of the Master's degree programme to become clinical psychologists. The mean total time per week spent on each participant was approximately 22 min, including telephone calls, administration, and reading and responding to emails. Hence, the total human contact time per participant including screening was over 2.5 h.
Statistical analysis
Significance testing of group differences in demographic data and pre-treatment measures was conducted with χ2 and t-tests. Participants’ scores before and after treatment were analysed using two-way analysis of variance with repeated measures. These were followed by t-tests with Bonferroni-corrected P values, set at 0.0125. This limit was obtained by dividing the traditional alpha level with the maximum number of individual group comparisons (i.e. 4). Effect sizes (Cohen's d) were calculated both within and between groups, and all calculations were based on the pooled standard deviation.
RESULTS
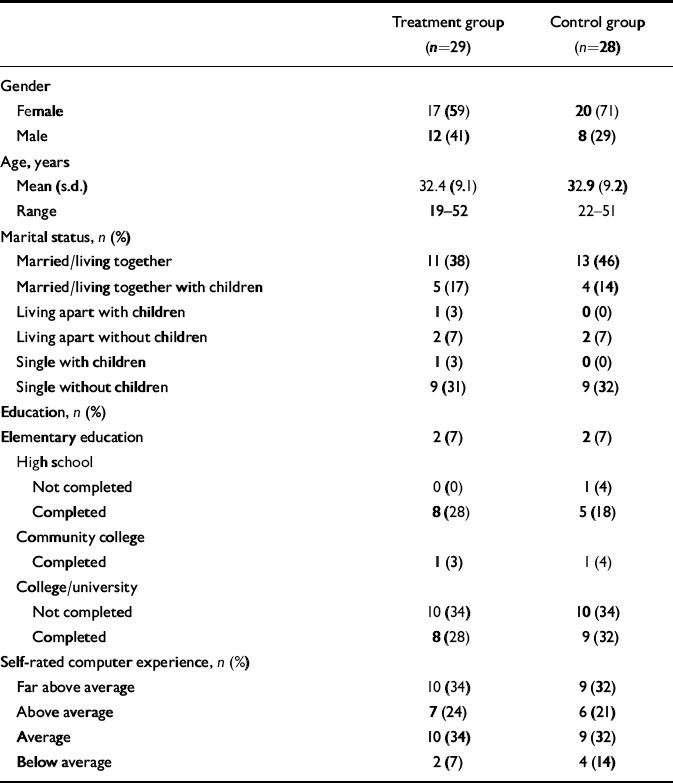
The flow of participants through the trial is shown in Fig. 1 and the characteristics of the sample are given in Table 1.
Table 1 Demographic description of the participants
| Treatment group (n=29) | Control group (n=28) | |
|---|---|---|
| Gender | ||
| Female | 17 (59) | 20 (71) |
| Male | 12 (41) | 8 (29) |
| Age, years | ||
| Mean (s.d.) | 32.4 (9.1) | 32.9 (9.2) |
| Range | 19-52 | 22-51 |
| Marital status, n (%) | ||
| Married/living together | 11 (38) | 13 (46) |
| Married/living together with children | 5 (17) | 4 (14) |
| Living apart with children | 1 (3) | 0 (0) |
| Living apart without children | 2 (7) | 2 (7) |
| Single with children | 1 (3) | 0 (0) |
| Single without children | 9 (31) | 9 (32) |
| Education, n (%) | ||
| Elementary education | 2 (7) | 2 (7) |
| High school | ||
| Not completed | 0 (0) | 1 (4) |
| Completed | 8 (28) | 5 (18) |
| Community college | ||
| Completed | 1 (3) | 1 (4) |
| College/university | ||
| Not completed | 10 (34) | 10 (34) |
| Completed | 8 (28) | 9 (32) |
| Self-rated computer experience, n (%) | ||
| Far above average | 10 (34) | 9 (32) |
| Above average | 7 (24) | 6 (21) |
| Average | 10 (34) | 9 (32) |
| Below average | 2 (7) | 4 (14) |
Attrition
Two participants, one in each condition, were excluded from the analysis since they started other treatment during the period. A total of 27 of the 29 people in the treatment group completed all nine modules within the intended 9-week time frame. Lack of time was provided as the explanation for terminating treatment prematurely. One of them did not send in post-treatment measures, which explains why intention-to-treat analysis was used. Finally, after randomisation but before answering the pre-treatment questionnaires, one person in the waiting-list chose to refrain from participation because of lack of computer access. Thus, data for 29 participants in the treatment group and 28 in the control group were eligible for analysis.

Fig. 1 Study profile. CBT, cognitive–behavioural therapy; MADRS–S, Montgomery-Åsberg Depression Rating Scale–Self-rated; SCID, Structured Clinical Interview for DSM–IV; SPSQ, Social Phobia Screening Questionnaire.
Pre-treatment differences
The two groups did not differ significantly on any of the measures at the pre-treatment assessment (t 62=0.08–0.76, P=0.94–0.45).
Primary outcome measures
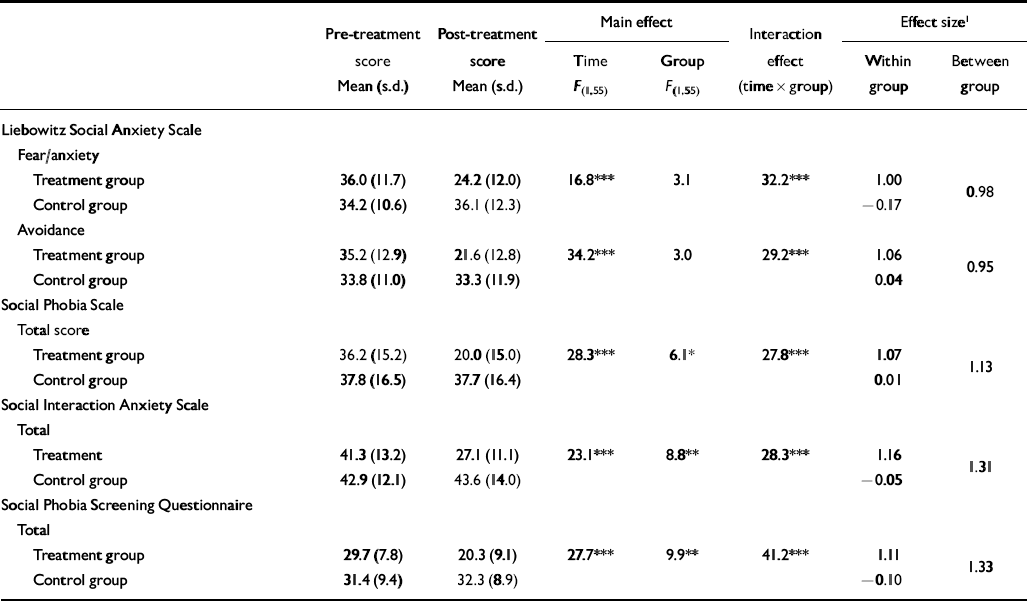
Significant group by time interactions were obtained for all primary measures (Table 2). For all scales post hoc t-tests with Bonferroni-corrected P values indicated that the intervention group had improved significantly between the pre-treatment and post-treatment assessments (t 28=6.3–7.2, P<0.001), whereas the control group had not (t 27=0.4–1.2, P>0.23). Moreover, following treatment the treated group had lower social anxiety levels on all scales compared with controls (t 55=3.6–5.1, P<0.001).
Table 2 Social phobia: main and interaction effects and pooled effect sizes for each group
| Pre-treatment score Mean (s.d.) | Post-treatment score Mean (s.d.) | Main effect | Interaction effect (time × group) | Effect size1 | |||
|---|---|---|---|---|---|---|---|
| Time F (1,55) | Group F (1,55) | Within group | Between group | ||||
| Liebowitz Social Anxiety Scale | |||||||
| Fear/anxiety | |||||||
| Treatment group | 36.0 (11.7) | 24.2 (12.0) | 16.8*** | 3.1 | 32.2*** | 1.00 | 0.98 |
| Control group | 34.2 (10.6) | 36.1 (12.3) | -0.17 | ||||
| Avoidance | |||||||
| Treatment group | 35.2 (12.9) | 21.6 (12.8) | 34.2*** | 3.0 | 29.2*** | 1.06 | 0.95 |
| Control group | 33.8 (11.0) | 33.3 (11.9) | 0.04 | ||||
| Social Phobia Scale | |||||||
| Total score | |||||||
| Treatment group | 36.2 (15.2) | 20.0 (15.0) | 28.3*** | 6.1* | 27.8*** | 1.07 | 1.13 |
| Control group | 37.8 (16.5) | 37.7 (16.4) | 0.01 | ||||
| Social Interaction Anxiety Scale | |||||||
| Total | |||||||
| Treatment | 41.3 (13.2) | 27.1 (11.1) | 23.1*** | 8.8** | 28.3*** | 1.16 | 1.31 |
| Control group | 42.9 (12.1) | 43.6 (14.0) | -0.05 | ||||
| Social Phobia Screening Questionnaire | |||||||
| Total | |||||||
| Treatment group | 29.7 (7.8) | 20.3 (9.1) | 27.7*** | 9.9** | 41.2*** | 1.11 | 1.33 |
| Control group | 31.4 (9.4) | 32.3 (8.9) | -0.10 | ||||
Secondary outcome measures
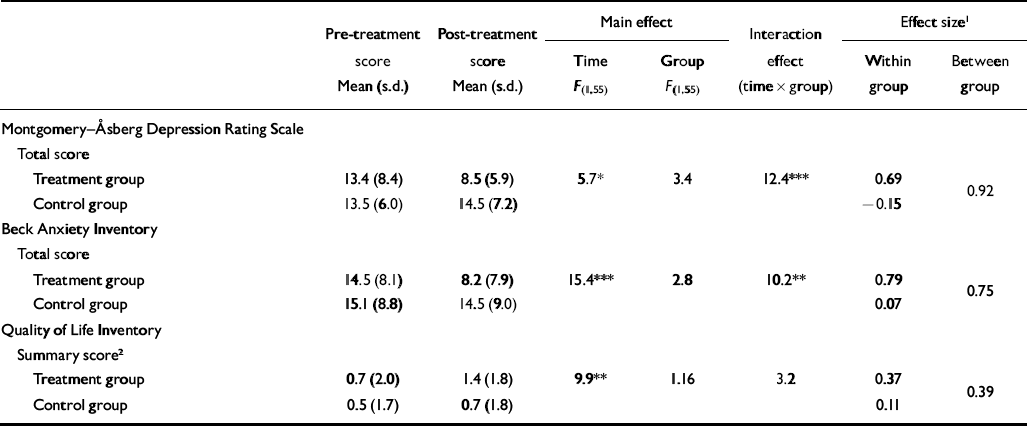
Significant group by time interactions were obtained for scores on the MADRS–S and BAI (Table 3). The QoLI only showed a trend (P=0.08). For all secondary scales, post-hoc t-tests with Bonferroni-corrected P values indicated that the intervention group had improved significantly between the pre-treatment and post-treatment assessments (t 28=3.2–4.6, P<0.004), whereas the control group had not (t 27=0.6–1.1, P>0.29). Moreover, following treatment, the intervention group had lower distress levels on two of the scales (MADRS–S and BAI) compared with the control group (t 55=2.8–3.4, P<0.007). However, we found no significant post-treatment difference in QoLI score between the groups (t 55=1.6, P=0.12).
Table 3 Depression, anxiety level and quality of life: main and interaction effects and pooled effect sizes for each group
| Pre-treatment score Mean (s.d.) | Post-treatment score Mean (s.d.) | Main effect | Interaction effect (time × group) | Effect size1 | |||
|---|---|---|---|---|---|---|---|
| Time F (1,55) | Group F (1,55) | Within group | Between group | ||||
| Montgomery—Åsberg Depression Rating Scale | |||||||
| Total score | |||||||
| Treatment group | 13.4 (8.4) | 8.5 (5.9) | 5.7* | 3.4 | 12.4*** | 0.69 | 0.92 |
| Control group | 13.5 (6.0) | 14.5 (7.2) | -0.15 | ||||
| Beck Anxiety Inventory | |||||||
| Total score | |||||||
| Treatment group | 14.5 (8.1) | 8.2 (7.9) | 15.4*** | 2.8 | 10.2** | 0.79 | 0.75 |
| Control group | 15.1 (8.8) | 14.5 (9.0) | 0.07 | ||||
| Quality of Life Inventory | |||||||
| Summary score2 | |||||||
| Treatment group | 0.7 (2.0) | 1.4 (1.8) | 9.9** | 1.16 | 3.2 | 0.37 | 0.39 |
| Control group | 0.5 (1.7) | 0.7 (1.8) | 0.11 | ||||
Effect sizes
The mean within-group effect size was high at d=0.95. The between-group effect size varied markedly across the different measures: the highest value was found on the SPSQ (d=1.31) whereas the lowest was found for QoLI (d=0.39). The mean between-group effect size across all measures was d=1.00.
One-year follow-up
Of the 29 people in the treatment group, 28 returned the 1-year follow-up questionnaires; hence intention-to-treat analysis was again used. Paired t-tests showed that there were significant differences between pre-treatment and follow-up scores (t 28=3.4–8.1, P<0.003), but almost no robust post-treatment v. follow-up changes (t 28=0.2–1.9, P<0.86–0.07). The only significant post-treatment v. follow-up change was in QoLI (t 28=2.55; P=.017). The following 1-year results were observed: LSAS–SR, sub-scale fear, mean 22.31 (s.d.=11.43); LSAS sub-scale avoidance, mean 20.55 (s.d.=11.95); SPS, mean 20.28 (s.d.=14.60); SIAS, mean 25.69 (s.d.=10.63); SPSQ total score, mean 18.00 (s.d.=10.12); MADRS–S, mean 7.93 (s.d.=7.75); BAI, mean 7.62 (s.d.=8.93); QoLI, mean 1.94 (s.d.=1.67). In sum, the average effect size at follow-up was d=1.02. There was no correlation between number of postings on the online discussion and change scores at post-treatment or follow-up assessment (all r <0.17 and all P>0.40).
DISCUSSION
Participants receiving the intervention improved significantly on all the measures used, whereas those on the waiting list control group did not. Specifically, the treated participants achieved significant improvement on measures of social anxiety, fear, avoidance, depression and general anxiety. The differences in quality of life were marked but not significant, and this may represent a type II error. Apart from power issues, a reason could be that the treatment period was too short to have an impact on this measure, which has broad items such as ‘number of children’. In fact, at the 1-year follow-up the quality of life measure had caught up and was significant. Unfortunately, since people on the waiting list received treatment before the follow-up data were collected, there is no between-group comparison at the 1-year follow-up.
Effect size
The treatment had a substantial within-group effect size (Cohen's d=0.95), which should be compared with the within-group effect size reported in a meta-analysis by Taylor (Reference Taylor1996) for placebo (d=0.48), exposure alone (d=0.81), cognitive therapy (d=0.63), social skills training (d=0.65), and cognitive and exposure therapy combined (d=1.06).
Adherence
Although self-administered treatments for various problems have shown promising results in many studies (Reference Carlbring and AnderssonCarlbring & Andersson, 2006), a crucial problem is the low adherence to treatment. This study added weekly telephone calls, which resulted in a considerably higher proportion of participants finishing the entire treatment package within the 9-week time frame, compared with a previous study (Reference Andersson, Carlbring and HolmströmAndersson et al, 2006) conducted without telephone support (93% v. 62%). However, direct comparisons are needed to draw firm conclusions regarding the relative value of whether therapist interaction over the telephone improves retention and outcomes.
Limitations
One of the advantages of internet-based therapy is the possibility of treating people who would not otherwise seek treatment. Asking participants to come to a clinical selection interview might induce a self-selection bias for people with less severe problems. Our study was designed to target anyone with social phobia, whether they were able to travel or not; we therefore decided to administer the clinical interview over the telephone, which might have compromised diagnostic reliability. Because the research staff never met the participants in person, there was a risk of including those with extreme suicidal tendencies. To minimise this risk we excluded people who, according to their MADRS–S, responses, were suicidal. In theory this might have led to a sample of people who were less depressed than participants in other studies. However, the results on the measures are comparable with those reported elsewhere for the target population (Reference Orsillo, Antony, Orsillo and RoemerOrsillo, 2001). Nevertheless, it is still uncertain how the treatment would affect a more severely depressed group.
Another caveat with this study is that the educational level of the participants was high. One in three Swedish adults aged 25–64 years has some form of post-secondary education (Statistics Sweden, 2003). That is considerably lower than in our study sample, which raises the question of how well the treatment would work with individuals with lower levels of education. Also, as the sample was selected from individuals who had expressed an interest in an internet-administered self-help programme, it is possible that selection biases yield a more effective result for this treatment compared with standard live treatment. Finally, a major weakness is the sole reliance on self-report measures. A clinical global impression and a behavioural test including psychophysiological measures would have strengthened the results.
Future research
As we did not include a comparison treatment, specificity of the findings cannot be assured. Consequently, future studies should investigate the issue of specificity of internet-based self-help interventions, the role of community online support and the non-specifics of therapist contact that are likely to be present in both telephone and internet consultations. Furthermore, larger studies are needed to allow an examination of individual characteristics and treatment response. Additionally, comparisons with standardised face-to-face therapy are imperative (compare with Reference Carlbring, Nilsson-Ihrfelt and WaaraCarlbring et al, 2005). Dismantling studies are strongly encouraged in order to evaluate the cost–benefit of briefer or more intensive combined treatments (e.g. internet plus live therapist sessions in severe cases).
Acknowledgements
This study was funded in part by a grant from the Swedish Research Council and the Söderström Königska Foundation.









eLetters
No eLetters have been published for this article.