Reserve forces have increasingly supplemented UK regular armed forces during deployments. Since the Iraq War (Operation TELIC) began in January 2003 more than 12 000 reservists have been deployed, making up 11% of the UK forces in Iraq (National Audit Office, 2006). Reserve forces consist of approximately 36 000 volunteer reserves and 52 000 regular reserves (former regular personnel who retain a call-out liability; National Audit Office, 2006). Reservists take on a variety of roles, many of which require specialist skills (e.g. medical), and therefore tend to be older and have higher educational attainment than regular personnel. The context in which reservists deploy is different from that of regular forces; reservists often deploy as individuals with units of regular personnel and in many cases they will not have prior knowledge of many, or any, of their comrades. Owing to the nature of deployment, reservists may be more likely than regular forces to undertake work in theatre for which they have not been specifically trained or not experienced in their civilian employment. They also have the additional pressures of leaving civilian life behind, including their work colleagues, families and friends, who may have little understanding of what the reservist could face while away.
As the numbers of mobilised reservists increases, so too do concerns about their health (BBC News, 2006). We recently reported on the health outcomes in a random sample of UK armed forces personnel who were deployed to Iraq in 2003 (Reference Hotopf, Hull and FearHotopf et al, 2006). Although there was no major health effect of deployment for regulars, deployed reservists had a higher prevalence of five health outcomes compared with non-deployed reservists. Common mental disorders and fatigue were more common in deployed reservists than non-deployed reservists, and although confidence intervals were wide, odds ratios suggested that there was a potential effect of deployment for reservists for post-traumatic stress disorder (PTSD) symptoms, multiple physical symptoms, and general perception of health. In our previous paper, we showed that this effect was not related to sociodemographic confounders (Reference Hotopf, Hull and FearHotopf et al, 2006). Here, we assess whether differences in health outcomes between reservists and regulars after deployment to Iraq could be attributed to socio-demographic differences, experiences during deployment (including main duty in theatre, exposure to potentially traumatic events or unit cohesion) or to problems at home (readjustment or relationship difficulties). We also investigated marital satisfaction in reserve and regular forces who deployed to Iraq and in personnel who did not deploy.
METHODS
Details of the sampling methods, participants and measures used are reported in our previous publication (Reference Hotopf, Hull and FearHotopf et al, 2006). The study was the first wave of a cohort study of military personnel comparing health and other outcomes between individuals who had been deployed on Operation TELIC 1 (the initial phase of the Iraq War, when major combat duties took place) and individuals who were in the military at the time but who were not deployed on this operation (referred to as ‘era’). Random samples of a comparable size from each of these populations were selected, with reservists oversampled by a factor of 2:1. We made two sets of comparisons: primarily, between deployed reservists (referred to as ‘TELIC reservists’) and deployed regulars (referred to as ‘TELIC regulars’) and, when comparing marital satisfaction, additional comparisons with non-deployed reservists (referred to as ‘era reservists’) and non-deployed regulars (referred to as ‘era regulars’).
Health outcomes and exposures
A questionnaire was devised, and data were collected both by visits to military bases and by mail-outs of the questionnaires. Participants completed the following measures of current health: the 12-item General Health Questionnaire (GHQ–12; Reference Goldberg and WilliamsGoldberg & Williams, 1988; Reference Goldberg, Gater and SartoriusGoldberg et al, 1997) to measure symptoms of common mental disorder; the 17-item National Center for Post Traumatic Stress Disorder PTSD Checklist – Civilian Version (Reference Blanchard, Jones–Alexander and BuckleyBlanchard et al, 1996) as a measure of symptoms of PTSD; the Chalder Fatigue Scale (Reference Chalder, Berelowitz and PawlikowskaChalder et al, 1993) to measure fatigue symptoms; and a checklist of 53 physical symptoms similar to those used in our previous study of Gulf War veterans (Reference Unwin, Blatchley and CokerUnwin et al, 1999). We also asked participants to rate their current general health using a single item taken from the 36-item Short Form Health Survey (SF–36; Reference Ware and SherbourneWare & Sherbourne, 1992). The defined cut-off values for each measure used in the analyses are shown in Table 1. Participants also provided information about demographic characteristics, experiences while on deployment (including main duty, potentially traumatic experiences, comradeship and unit cohesion) and experiences at home before, during and after deployment.
Table 1 Criteria for case definition

| Scale | Case definition |
|---|---|
| General Health Questionnaire | Score of ≥4 |
| PTSD Checklist | Score of ≥50 |
| Chalder Fatigue Scale | Score of ≥4 |
| Multiple physical symptoms | ≥18 |
| Health perception | Rating health as ‘poor’ or ‘fair’ |
Statistical analysis
Statistically significant differences between the proportions were identified using Pearson's χ2 statistic and we took P values of less than 0.05 to indicate statistical significance. Odds ratios and 95% confidence intervals were computed by multivariable logistic regression to estimate the effect of enlistment status (regular or reserve) on health outcomes. Odds ratios were calculated with and without adjustment for age, gender, marital and education status, having children under age 18 years not living at home, service branch (Navy, Army, Air Force) and rank. We also calculated odds ratios adjusting for potentially traumatic experiences and main duty in theatre, unit cohesion and home life variables. Amounts of missing data regarding home variables were large; we therefore adjusted only for major problems at home during and following deployment. Reserve types were combined because the number of regular reservists was too low to make meaningful comparisons with volunteer reservists. The statistical software package Stata version 9.0 for Windows was used for all analyses.
RESULTS
Detailed information on response rates and characteristics of non-responders are given elsewhere (Reference Hotopf, Hull and FearHotopf et al, 2006). We obtained completed questionnaires for 786 of 1400 (56%) TELIC reservists, 3936 of 6295 (63%) TELIC regulars, 800 of 1811 (44%) era reservists and 4750 of 8192 (58%) era regulars. Non-participation was associated with reservist status, lower rank, younger age, not deploying on TELIC and male gender. In an intensive follow-up survey non-responders were found to have similar rates of the outcomes under study (Reference Hotopf, Hull and FearHotopf et al, 2006).
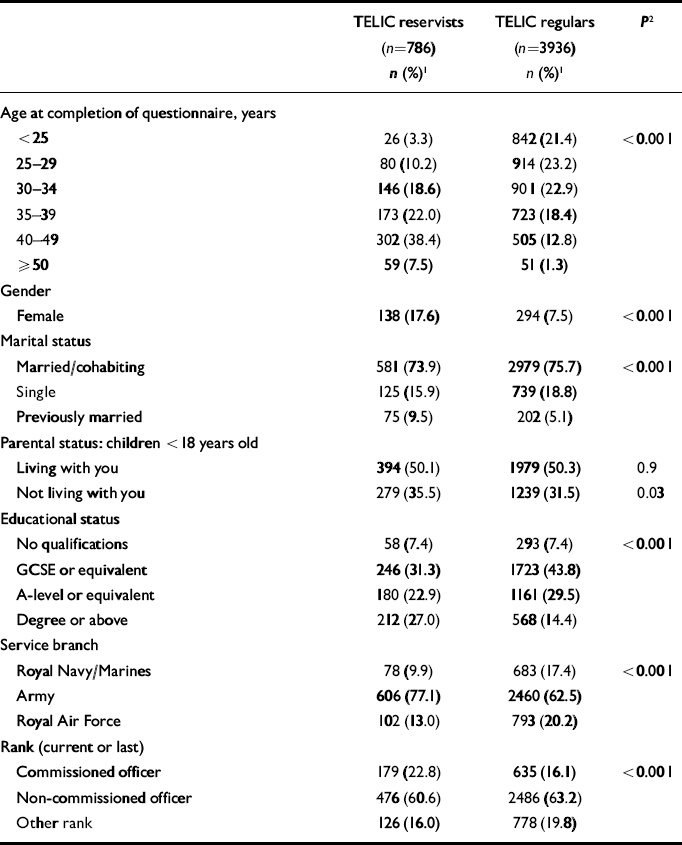
The socio-demographic characteristics of TELIC reservists and TELIC regulars are described in Table 2. Significant differences existed between these two groups for all socio-demographic variables except having children under the age of 18 years living at home. The TELIC reservists were older, better educated and higher in rank than TELIC regulars. A greater proportion were female, in the Army and previously married (i.e. separated, divorced or widowed).
Table 2 Socio-demographic variables
| TELIC reservists (n=786) n (%)1 | TELIC regulars (n=3936) n (%)1 | p 2 | |
|---|---|---|---|
| Age at completion of questionnaire, years | |||
| <25 | 26 (3.3) | 842 (21.4) | <0.001 |
| 25-29 | 80 (10.2) | 914 (23.2) | |
| 30-34 | 146 (18.6) | 901 (22.9) | |
| 35-39 | 173 (22.0) | 723 (18.4) | |
| 40-49 | 302 (38.4) | 505 (12.8) | |
| ≥50 | 59 (7.5) | 51 (1.3) | |
| Gender | |||
| Female | 138 (17.6) | 294 (7.5) | <0.001 |
| Marital status | |||
| Married/cohabiting | 581 (73.9) | 2979 (75.7) | <0.001 |
| Single | 125 (15.9) | 739 (18.8) | |
| Previously married | 75 (9.5) | 202 (5.1) | |
| Parental status: children <18 years old | |||
| Living with you | 394 (50.1) | 1979 (50.3) | 0.9 |
| Not living with you | 279 (35.5) | 1239 (31.5) | 0.03 |
| Educational status | |||
| No qualifications | 58 (7.4) | 293 (7.4) | <0.001 |
| GCSE or equivalent | 246 (31.3) | 1723 (43.8) | |
| A-level or equivalent | 180 (22.9) | 1161 (29.5) | |
| Degree or above | 212 (27.0) | 568 (14.4) | |
| Service branch | |||
| Royal Navy/Marines | 78 (9.9) | 683 (17.4) | <0.001 |
| Army | 606 (77.1) | 2460 (62.5) | |
| Royal Air Force | 102 (13.0) | 793 (20.2) | |
| Rank (current or last) | |||
| Commissioned officer | 179 (22.8) | 635 (16.1) | <0.001 |
| Non-commissioned officer | 476 (60.6) | 2486 (63.2) | |
| Other rank | 126 (16.0) | 778 (19.8) |
Table 3 shows deployment experiences, including exposure to potentially traumatic events in theatre, comradeship and unit cohesion. The patterns of exposures were different: although regulars were more likely to have discharged their weapons and come under small-arms fire, many other potentially adverse experiences were more common in reservists. This particularly applied to aiding wounded and handling bodies. A quarter (26%) of TELIC reservists undertook a medical or welfare role in theatre compared with 7% of TELIC regulars. When these personnel were excluded from the denominator, all statistically significant differences with regard to seeing and aiding casualties disappeared and the effect was reversed for the handling of bodies (data not shown).
Table 3 Deployment experiences on Operation TELIC 1

| TELIC reservists (n=786) n (%)1 | TELIC regulars (n=3936) n (%)1 | p 2 | |
|---|---|---|---|
| Potentially adverse experiences in theatre | |||
| Discharged weapon in direct combat | 63 (8.0) | 689 (17.5) | <0.001 |
| Thought might be killed | 507 (64.5) | 2154 (54.7) | <0.001 |
| Came under small-arms fire | 224 (28.5) | 1270 (32.3) | 0.04 |
| Came under mortar, Scud or artillery fire | 481 (61.2) | 2032 (51.6) | <0.001 |
| Experienced a landmine strike | 26 (3.3) | 172 (4.4) | 0.2 |
| Experienced hostility from civilians | 331 (42.1) | 1650 (41.9) | 0.9 |
| Saw personnel wounded or killed (any) | 386 (49.1) | 1754 (44.6) | 0.02 |
| Handled bodies (any) | 157 (20.0) | 579 (14.7) | <0.001 |
| Aided wounded (any) | 233 (29.6) | 650 (16.5) | <0.001 |
| Main duty in theatre | |||
| Combat | 88 (11.2) | 992 (25.2) | <0.0013 |
| Medical/welfare | 202 (25.7) | 269 (6.8) | |
| Logistics | 162 (20.6) | 615 (15.6) | |
| Communication | 37 (4.7) | 315 (8.0) | |
| Other | 288 (36.6) | 1604 (40.8) | |
| Comradeship and unit cohesion | |||
| Deployed with parent unit | 163 (20.7) | 2553 (64.9) | <0.001 |
| Felt sense of comradeship with others in unit | 591 (75.2) | 3149 (80.0) | <0.001 |
| Could have gone to most people in unit with personal problems | 356 (45.3) | 1865 (47.4) | 0.1 |
| Seniors were interested in what I did and thought | 350 (44.5) | 2103 (53.4) | <0.001 |
| Felt well informed about what was going on | 325 (41.4) | 2055 (52.2) | <0.001 |
| Capability for deployment | |||
| Work in theatre was outside trade experience or ability | 86 (10.9) | 190 (4.8) | <0.001 |
| Been previously deployed | 247 (31.4) | 2869 (72.9) | <0.001 |
Reservists reported slightly lower levels of comradeship and unit cohesion than regulars. They felt less well informed (41% of reservists and 52% of regulars) and were less likely to work under a chain of command they felt was interested in what they did and thought (44% of reservists and 53% of regulars). Only 21% of reservists reported being deployed with their parent unit, compared with 65% of regulars, although despite that only a minority (11% of reservists and 5% of regulars) reported working in an unfamiliar role. Fewer reservists (31%) had been deployed on previous operations than regulars (73%).
The TELIC reservists were more likely to describe their families as being proud that they had been deployed compared with regulars (Table 4); yet during mobilisation to Iraq, major problems at home regarding children, finances or other factors were more commonly reported in reservists. Following deployment, reservists reported experiencing significantly more major problems and readjustment difficulties than regulars. Marital satisfaction was generally high in all groups, but married or cohabiting TELIC reservists reported lower marital satisfaction than married or cohabiting TELIC regulars, era reservists and era regulars, although these differences were slight. There was a larger difference between groups when asked whether they had considered divorce or separation. We detected an interaction between deployment and enlistment status (P=0.006), indicating that deployment on Operation TELIC was associated with more reservists – but not regulars – having considered separation in the previous year.
Table 4 Family and home life

| TELIC reservists (n=786) n (%)1 | TELIC regulars (n=3936) n (%)1 | Era reservists (n=800) n (%)1 | Era regulars (n=4750) n (%)1 | P 2 | |
|---|---|---|---|---|---|
| Pre-deployment | |||||
| Family was proud I was being deployed | 564 (71.8) | 2305 (58.6) | <0.001 | ||
| Family did not want me to go | 544 (69.2) | 2650 (67.3) | 0.6 | ||
| Was not well supported by my family | 29 (3.7) | 127 (3.2) | 0.6 | ||
| On deployment | |||||
| Had major problems at home | 293 (37.3) | 1073 (27.3) | <0.001 | ||
| After deployment | |||||
| Had major problems on return from deployment | 263 (33.5) | 712 (18.1) | <0.001 | ||
| Found it difficult to adjust to being back home | 377 (48.0) | 1194 (30.3) | <0.001 | ||
| People didn't understand what I'd been through | 605 (77.0) | 2527 (64.2) | <0.001 | ||
| Did not want to talk to family or friends about experiences | 315 (40.1) | 1416 (36.0) | 0.09 | ||
| Current marital satisfaction3 | |||||
| Am satisfied with current partner | 527 (90.7) | 2787 (93.6) | 559 (92.2) | 3504 (93.7) | 0.007 |
| My relationship makes me happy | 524 (90.2) | 2764 (92.8) | 547 (90.3) | 3498 (93.5) | <0.001 |
| Divorce or separation has been suggested in past year | 124 (21.3) | 556 (18.7) | 83 (13.7) | 655 (17.5) | 0.002 |
All adverse health outcomes were more common in TELIC reservists than TELIC regulars, with unadjusted odds ratios ranging from 1.38 to 1.54 (Table 5). The first model adjusted for socio-demographic differences; this led to a reduction in the effect size for all outcomes, except PTSD for which the odds ratio increased. After adjustment, common mental disorders, PTSD and fatigue remained significantly associated with reservist status. The second model adjusted for potentially traumatic experiences and main duty in theatre. These adjustments led to a further reduction in effect sizes, and only PTSD symptoms remained statistically significantly associated with enlistment status. We conducted a further analysis excluding medical and welfare personnel and found an almost identical pattern of univariate association (data not shown), indicating the effect is not limited to reservists who undertook a medical or welfare role in theatre. Model three adjusted for measures of unit cohesion and main duty in theatre. This model was associated with similar reductions in effect sizes as model two, and as in model two, PTSD remained associated with reservist status, albeit with borderline statistical significance. The final model (model four) controlled for reported problems at home during and following deployment. This led to the greatest reduction in effect sizes, including PTSD, with no outcome now being associated with reservist status.
Table 5 Distribution of main health outcomes by enlistment status

| Cases, n (%) | Unadjusted OR (95% CI) | Adjusted OR (95% CI)1 | |||||
|---|---|---|---|---|---|---|---|
| TELIC reservists (n=786) | TELIC regulars (n=3936) | Model 1 | Model 2 | Model 3 | Model 4 | ||
| Common mental disorder | 206 (26.3) | 747 (19.4) | 1.49 (1.24-1.77) | 1.28 (1.04-1.59) | 1.17 (0.93-1.46) | 1.18 (0.93-1.49) | 0.94 (0.74-1.19) |
| (GHQ—12) | |||||||
| PTSD (PTSD Checklist) | 46 (6.0) | 155 (4.0) | 1.52 (1.08-2.14) | 1.71 (1.13-2.60) | 1.62 (1.05-2.52) | 1.57 (0.99-2.48) | 1.15 (0.73-1.79) |
| Chalder Fatigue Scale | 315 (41.0) | 1225 (31.9) | 1.48 (1.26-1.74) | 1.28 (1.06-1.55) | 1.18 (0.97-1.44) | 1.12 (0.91-1.38) | 1.02 (0.84-1.26) |
| Multiple physical symptoms | 120 (15.3) | 455 (11.6) | 1.38 (1.11-1.71) | 1.11 (0.85-1.44) | 0.96 (0.73-1.26) | 0.98 (0.73-1.31) | 0.77 (0.58-1.03) |
| Fair or poor general health | 122 (15.6) | 415 (10.7) | 1.54 (1.24-1.92) | 1.12 (0.86-1.46) | 1.04 (0.79-1.38) | 1.11 (0.83-1.48) | 0.86 (0.65-1.14) |
DISCUSSION
We have found numerous differences in the experiences of UK reservists and regulars when deployed to a major operation. There were major differences in the reservists’ socio-demographic characteristics, and also in the way they were deployed (usually not in a parent unit) and their reported experiences during deployment. Although reservists were more likely to report their families feeling proud of their contribution, when compared with regular personnel they also experienced more difficulties and less marital satisfaction on their return. Our analyses suggest that although demographic differences between reservists and regulars do contribute to the health effects we report, controlling for experiences on deployment accounts for most of the differences in health outcomes we observed, except PTSD symptoms. These were most strongly accounted for by problems at home during and following deployment.
Limitations
This study is the largest health study ever undertaken in the UK reserve armed forces and is representative of all three branches of service, including serving and ex-serving personnel. However, the study has limitations. We were unable to contact everyone in the cohort as the mobile nature of military life meant that contact information was often unreliable. Participation was incomplete, with a total participation rate (adjusted for individuals whose address details were unknown) of 61% (Reference Hotopf, Hull and FearHotopf et al, 2006). However, our intensive tracing of non-responders, including reservists, suggested that non-responder bias was unlikely, because the prevalence of the main outcomes was similar to that in study responders (Reference Hotopf, Hull and FearHotopf et al, 2006). The study is cross-sectional, and therefore it is impossible to determine the direction of causation for the associations we report. This may apply particularly to the more subjective measures regarding comradeship and problems at home, which are likely to be affected by current mood. Some of the measures, for example of deployment-related experiences, have not previously been validated.
Consistency with other studies
Although many epidemiological studies have reported on the mental health of regular armed forces personnel following deployment (Reference Unwin, Blatchley and CokerUnwin et al, 1999; Reference Pizarro, Silver and PrausePizarro et al, 2006), research into the health and well-being of reserve forces has been limited. Several studies have reported a possible association between reservist status and mental disorders (Reference Solomon, Noy and Bar–OnSolomon et al, 1987; Iowa Persian Gulf Study Group, 1997; Reference McAllister, Blair and PhilpottMcAllister et al, 2004; Reference Smith, Corbeil and RyanSmith et al, 2004; Reference Turner, Kiernan and McKechanieTurner et al, 2005). Our findings support this association, and this paper proposes explanations that might account for the higher risk of mental ill health in reservists when compared with their regular comrades following a major deployment.
Interpretation
Our findings show that TELIC reserve personnel reported potentially traumatising exposures in theatre at levels that were often higher than those reported by regular personnel. For exposures relating to aiding the wounded or handling bodies this difference is likely to be accounted for by the large number of reservists in medical or welfare roles. The fact that reservists were less likely to discharge their own weapons or come under small-arms fire is similarly likely to be a reflection of the relatively few reservists in combat roles. However, reservists were more likely to report coming under artillery fire or thinking that they might be killed. These findings may reflect the front-line duties of reservists (for example, medical reservists who are often supporting combat units); however, it is also possible that there is a difference in the perception of risk among reservists and regulars. We suggest that if the reporting of artillery fire exposure or risk to one's own life were accurate, it would be surprising for the reservists – of whom only 11% were involved in combat duties – to have higher rates of such exposures compared with the regulars, 25% of whom were in such duties. We suggest that, owing perhaps to their lack of previous deployment experience, reservists’ perception of exposure to life-threatening events might be higher. This might also be the result of recall bias, with the observed increase in distress levels leading to greater reporting, as has been found elsewhere (Reference Wessely, Unwin and HotopfWessely et al, 2003). Additionally, reserve units reported slightly lower unit cohesion and effective leadership, both of which have been shown to put combat support units at greater risk of poor psychological health (Reference Malone, Paige–Dobson and OhlMalone et al, 1996). The health of medical combat support personnel will be examined in more detail in a future paper.
Another possible explanation for our results is that the majority of reservists deployed as individuals, not with their parent unit. Unit cohesion has been shown to be the single most important sustaining and motivating force among troops, and psychiatric injuries are more prevalent in personnel who do not form close relationships within their unit (Reference RiellyRielly, 2000). Feeling isolated and lack of unit cohesion are likely to have had detrimental effects upon psychological health and may also have contributed to poorer relationships with the chain of command. For all outcomes except PTSD symptoms we found that differences in demographic variables, potentially traumatic exposures and unit cohesion accounted for the health effect in reservists.
It is not clear why PTSD symptoms differed from the other health outcomes, and it is perhaps counterintuitive that the excess in PTSD symptoms in reservists was not accounted for by controlling for differences in potentially traumatic exposures. The reduction in the health effect when homecoming experiences were taken into account might be due to reverse causation. For example, PTSD symptoms might have had a major effect on the experience of homecoming, and controlling for these experiences spuriously lowers the odds ratio for reservist status. Alternatively, it might be a genuine effect, indicating that (for example) adverse domestic experiences lead to the prolongation of PTSD symptoms, which in a happier environment might spontaneously remit.
Reserve personnel are at greater risk of psychological stress because of rapid mobilisation, leaving them minimal time to process adverse fears and put their affairs in order (Reference Malone, Paige–Dobson and OhlMalone et al, 1996). The unexpected disruption to families and careers and resulting financial pressures may have been contributory to problems at home. It is also possible that major problems at home reported following deployment incorporated relationship difficulties. We found TELIC reservists’ relationships were particularly at risk following deployment to Iraq. In a separate unpublished study, reservists who deployed on a subsequent operation to Iraq believed that had welfare support been provided for their spouses during deployment their marriage breakdown would have been prevented (C. French, personal communication, 2006). This may have been a factor contributing to our findings. An alternative explanation is that some TELIC reservists had poorer marriages prior to their deployment to Iraq, and might have volunteered for the operation to escape problems at home.
Implications
The poorer health outcome of reservists following deployment is a source of considerable concern, especially given that recent deployments have seen an increase in their use. The UK Ministry of Defence has recently changed its policy to provide enhanced mental health services for reservists, who previously were not eligible to use Defence Medical Services following deployment (Ministry of Defence, 2006). However, a more important question is whether such illness can be prevented in reservists. The data we provide indicate that there may be important aspects to the way in which reservists are deployed, and their homecoming experiences, which might account for their poorer health. Attention should be paid to the provision of support for reservists deployed to unfamiliar units and welfare for their families.
Acknowledgements
We thank the UK Ministry of Defence for their cooperation; in particular we thank the Defence Analytical Services Agency, the Veterans Policy Unit, the Armed Forces Personnel Administration Agency, the Defence Medical Services Department and the Director of Reserve Forces and Cadets. This study was funded by the UK Ministry of Defence.










eLetters
No eLetters have been published for this article.