In clinical psychiatry there is a longstanding belief that comorbid personality psychopathology adversely affects the outcome of treatment in major depression. Recent reviews (Reference MulderMulder, 2002; Reference Kool, Schoevers and de MaatKool et al, 2005; Reference Newton–Howes, Tyrer and JohnsonNewton-Howes et al, 2006), although contradictory, challenge these beliefs. Mulder's systematic review and the meta-analysis of antidepressant drug randomised controlled trials by Kool et al report no adverse effect of comorbid personality disorders on the outcome of major depression. However, the meta-analysis of Newton-Howes et al included all treatments for major depression and reported a small but significant adverse effect of personality disorder. These inconsistent findings may reflect differences in treatment outcome related to different forms of therapy: Newton-Howes et al (Reference Newton–Howes, Tyrer and Johnson2006) reported a trend for psychotherapies to produce a poorer outcome in patients with a personality disorder compared with treatment with antidepressant drugs.
We have longstanding interests in the prediction of treatment responses in depression (Joyce et al, Reference Joyce, Mulder and Luty2002, Reference Joyce, Mulder and Luty2003) and have reported that comorbid personality disorder has little impact on outcome in patients treated with antidepressant medication (Reference Joyce, Mulder and LutyJoyce et al, 2003; Mulder et al, Reference Mulder, Joyce and Luty2003, Reference Mulder, Joyce and Frampton2006). In this paper we examine whether personality disorder or traits as assessed by a clinician interview based on DSM–IV, or a self-report of temperament and character (Reference Cloninger, Svrakic and PrzybeckCloninger et al, 1993), have an impact on treatment response in patients with depression receiving psychotherapy. We also investigate whether the type of psychotherapy – in this study interpersonal psychotherapy and cognitive–behavioural therapy – has any impact.
METHOD
The method and sample are detailed in the companion paper (Reference Luty, Carter and McKenzieLuty et al, 2007, this issue). Only methodological issues additional to those described and relevant to this paper are expanded upon. The study was approved by the Canterbury (New Zealand) ethics committee.
Participants
The companion paper (Reference Luty, Carter and McKenzieLuty et al, 2007, this issue) describes the clinical features of the sample, comprising 177 persons (mean age 35.2 years, 72% female) who were randomised to receive either interpersonal psychotherapy or cognitive–behavioural therapy for depression. Ten patients who had been assessed for Axis I disorders and who had been randomised to treatment withdrew from the study within the first few weeks of treatment and prior to an assessment of Axis II personality psychopathology. Thus, this study, which is focused on personality disorders, personality traits, temperament and character, analyses the data for the 167 patients with depression for whom we had complete personality measures. The 10 patients who withdrew (4 randomised to interpersonal psychotherapy; 6 to cognitive–behavioural therapy) did not differ significantly from the 167 patients remaining in the study with regard to depression severity or melancholia.
Assessment
After obtaining written informed consent, the therapists (two psychiatrists and three clinical psychologists) completed an assessment of Axis I disorders using the Structured Clinical Interview for DSM–IV (SCID–I; Reference Spitzer, Williams and GibbonSpitzer et al, 1987). Depression severity was assessed using the Montgomery–Åsberg Depression Rating Scale (MADRS; Reference Montgomery and ÅsbergMontgomery & Åsberg, 1979).
Among the self-report questionnaires completed by participants at this baseline assessment were the Structured Clinical Interview for Personality Disorders Questionnaire (SCID–PQ; Reference First, Gibbon and SpitzerFirst et al, 1997) and the Temperament and Character Inventory (TCI; Reference Cloninger, Pryzbeck and SvrakicCloninger et al, 1994). The TCI measures four independently inherited temperament traits: harm avoidance, reward dependence, novelty seeking and persistence. Respectively these four traits represent our unconscious bias in the inhibition or cessation of behaviours (harm avoidance), our need for other people (reward dependence), our bias in the activation or initiation of behaviour (novelty seeking) and our tendency to continue striving in the absence of reward (persistence). In contrast, character represents our conscious self-concepts. Three character dimensions have been described: self-directedness, cooperativeness and self-transcendence. Respectively these represent our self-concept as an autonomous individual (self-directedness), our self-concept in relationship to others (cooperativeness) and our view of ourselves as part of the universe (self-transcendence). Low self-directedness and low cooperativeness are related to the presence of a clinically defined personality disorder, whereas temperament influences what type of personality disorder a person may have (Reference Cloninger, Svrakic and PrzybeckCloninger et al, 1993; Reference Svrakic, Whitehead and PrzybeckSvrakic et al, 1993; Reference Mulder and JoyceMulder & Joyce, 1997; Reference Casey and JoyceCasey & Joyce, 1999; Reference Mulder, Joyce and SullivanMulder et al, 1999). Results from these questionnaires were not available to the therapists.
Approximately 6 weeks after assessment, randomisation and commencement of therapy, an independent clinician (one of four psychiatrists and three clinical psychologists, all trained in personality disorder assessments) completed the Structured Clinical Interview for DSM–IV Axis II Personality Disorders (SCID–II; Reference Spitzer, Williams and GibbonSpitzer et al, 1987). From the SCID–II we used both categorical (yes/no) measures of personality disorder and dimensional measures based upon number of personality disorder criteria rated as positive. Clinician-assessed severity of personality disorder was based on the proposal of Tyrer (Reference Tyrer2005), which codes the level of personality disorder severity as 0–3: no personality disorder codes as 0, sub-threshold personality disorder codes as 1, meeting criteria for one or more personality disorders within the same cluster codes as 2 and meeting criteria for two or more personality disorders from different clusters codes as 3. The therapists were not permitted to know the results from this structured assessment of Axis II psychopathology.
Details of the two intervention therapies, training and supervision, treatment integrity and outcome are detailed in the companion paper (Reference Luty, Carter and McKenzieLuty et al, 2007).
Statistical methods
Baseline characteristics of the participants with complete personality disorder assessment data were compared using ω2 tests, t-tests or Pearson correlation coefficients. The primary outcome measure used in this study was the percentage improvement in the MADRS score from baseline to the end of weekly therapy, with last measure carried forward in patients who did not complete weekly therapy. Given the interrelationships among the personality disorder, temperament and character measures, a stepwise multiple linear regression was run independently for each therapy within each of these three domains. Further stepwise multiple linear regressions, one for personality disorder measures and the second for the combined temperament and character measures, were run within therapies, followed by analyses combining both therapies and incorporating interaction terms with therapy.
RESULTS
Table 1 shows the gender, age, depression severity, temperament, character and personality disorder status of the 87 participants randomised to interpersonal therapy and the 80 participants randomised to cognitive–behavioural therapy. The latter group scored lower on the self-reported self-directedness item from the TCI, were rated by a clinician as being more likely to have one or more personality disorders and had a higher rate of obsessive–compulsive personality disorder.
Table 1 Temperament, character and personality disorders in depressed patients by therapy

| IPT (n=87) | CBT (n=80) | ||
|---|---|---|---|
| Female, % (n/N) | 76 (66/87) | 70 (56/80) | χ2=0.73, NS |
| Age, years: mean (s.d.) | 35.5 (10.4) | 35.8 (10.0) | t=0.16, NS |
| MADRS score: mean (s.d.) | 23.3 (6.4) | 24.3 (6.2) | t=-1.04, NS |
| TCI score: mean (s.d.) | |||
| Novelty seeking | 19.4 (5.3) | 18.6 (6.8) | t=0.80, NS |
| Harm avoidance | 23.9 (6.2) | 25.3 (7.0) | t=1.43, NS |
| Reward dependence | 21.9 (6.4) | 21.9 (6.0) | t=0.01, NS |
| Persistence | 20.3 (8.7) | 18.9 (8.7) | t=1.03, NS |
| Self-directedness | 25.0 (8.5) | 21.5 (9.0) | t=2.65, P=0.009 |
| Cooperativeness | 33.2 (5.7) | 31.8 (5.8) | t=1.56, NS |
| Self-transcendence | 15.9 (9.6) | 15.7 (10.3) | t=0.14, NS |
| Personality disorder diagnoses, % (n/N) | |||
| Avoidant PD | 23 (20/87) | 31 (25/80) | χ2=1.44, NS |
| Dependant PD | 0 (0/87) | 3 (2/80) | Fisher's NS |
| Obsessive—compulsive PD | 3 (3/87) | 23 (18/80) | χ2=13.76, P<0.001 |
| Paranoid PD | 8 (7/87) | 14 (11/80) | χ2=1.41, NS |
| Schizotypal PD | 2 (2/87) | 3 (2/80) | Fisher's NS |
| Schizoid PD | 3 (3/87) | 4 (3/80) | Fisher's NS |
| Narcissistic PD | 1 (1/87) | 0 (0/80) | Fisher's NS |
| Histrionic PD | 0 (0/87) | 0 (0/80) | Fisher's NS |
| Borderline PD | 8 (7/87) | 15 (12/80) | χ2=2.00, NS |
| Any PD | 37 (32/87) | 54 (43/80) | χ2=4.85, P=0.028 |
Clinician-assessed personality disorder and treatment response
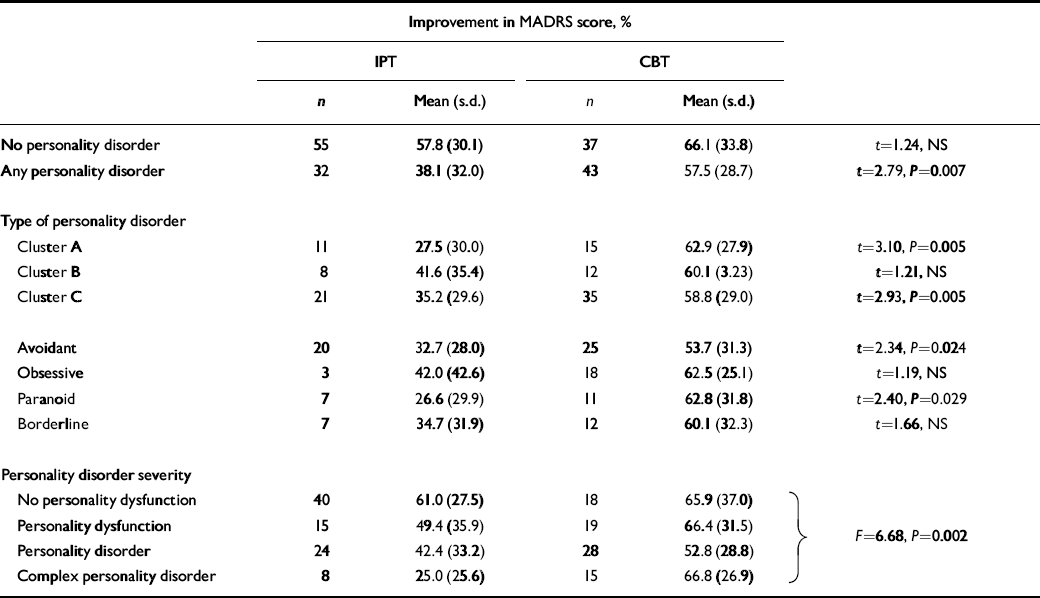
Table 2 shows the effect of clinician-assessed personality disorder on treatment outcome by therapy. For participants without a personality disorder the two therapies produced comparable treatment responses. However, for participants with any personality disorder interpersonal psychotherapy had a poorer treatment outcome than cognitive–behavioural therapy. Although numbers are limiting when response is examined by specific personality disorder cluster, or by the four most common individual personality disorders, the results consistently show a pattern of personality disorder adversely affecting treatment outcome with interpersonal psychotherapy but not with cognitive–behavioural therapy. Statistically significantly poorer treatment response with interpersonal psychotherapy is found in those with cluster A and C personality disorders and in avoidant and paranoid personality disorders. Personality disorder severity shows a comparable finding, with more severe personality disorder adversely affecting response to interpersonal psychotherapy but not cognitive–behavioural therapy.
Table 2 Percentage improvement in depression score by therapy and personality disorder
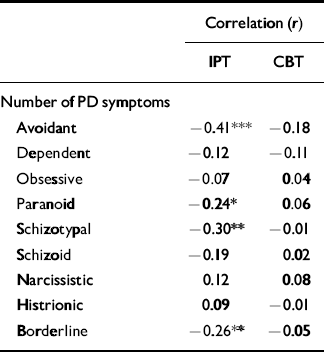
From Table 3, which shows the univariate correlations of number of personality disorder symptoms with treatment response, by therapy, it can be seen that response to cognitive–behavioural therapy is unrelated to number of specific personality disorder symptoms. Conversely, a poorer response to interpersonal psychotherapy is seen in participants with more avoidant, paranoid, schizotypal or borderline symptoms.
Table 3 Univariate correlations of personality disorder symptoms with percentage improvement, by therapy
| Correlation (r) | ||
|---|---|---|
| IPT | CBT | |
| Number of PD symptoms | ||
| Avoidant | -0.41*** | -0.18 |
| Dependent | -0.12 | -0.11 |
| Obsessive | -0.07 | 0.04 |
| Paranoid | -0.24* | 0.06 |
| Schizotypal | -0.30** | -0.01 |
| Schizoid | -0.19 | 0.02 |
| Narcissistic | 0.12 | 0.08 |
| Histrionic | 0.09 | -0.01 |
| Borderline | -0.26** | -0.05 |
Self-report temperament and character and treatment response
Table 4 shows the univariate correlations of self-report temperament and character with treatment response, by therapy. For cognitive–behavioural therapy only low persistence predicts a worse treatment outcome. For interpersonal psychotherapy high harm avoidance and low self-directedness strongly predict a poor treatment response; low novelty seeking and low reward dependence also significantly predict a poorer treatment response.
Table 4 Univariate correlations of temperament and character with percentage improvement, by therapy

| Correlation (r) | ||
|---|---|---|
| IPT | CBT | |
| Temperament | ||
| Novelty seeking | 0.22* | 0.09 |
| Harm avoidance | -0.37*** | -0.17 |
| Reward dependence | 0.24 | 0.18 |
| Persistence | 0.06 | 0.22* |
| Character | ||
| Self-directedness | 0.35*** | 0.18 |
| Cooperativeness | 0.20 | 0.09 |
| Self-transcendence | -0.02 | 0.07 |
Relationships between personality disorder, temperament and character
The relationships (correlations) between clinician-interview personality disorder symptoms and self-report temperament and character were consistent with expectations and previous reports (Reference Cloninger, Svrakic and PrzybeckCloninger et al, 1993; Reference Mulder and JoyceMulder & Joyce, 1997; Reference Casey and JoyceCasey & Joyce, 1999; Reference Mulder, Joyce and SullivanMulder et al, 1999).
Low self-directedness and low cooperativeness both correlated with total personality disorder symptoms (r=0.48, P< 0.001). Novelty seeking was positively correlated with cluster B personality disorder symptoms (r=0.25, P<0.01) and with borderline symptoms (r=0.22, P<0.01). Harm avoidance was correlated with cluster C personality disorder symptoms (r=0.47, P<0.001), plus avoidant symptoms (r=0.52, P<0.001), dependent symptoms (r=0.28, P<0.001), paranoid symptoms (r=0.31, P<0.001), schizotypal symptoms (r=0.32, P<0.001) and borderline symptoms (r=0.24, P<0.001). Low reward dependence was most strongly correlated with cluster A personality disorder symptoms (r=0.39, P<0.001) and schizoid symptoms (r=0.38, P<0.001).
Multivariate prediction of treatment response by therapy
Table 5 shows the results of a series of stepwise multiple regressions predicting mean percentage improvement from personality variables by therapy. The first observation of note from this table is that personality minimally predicts outcome for patients randomised to cognitive–behavioural therapy. The corollary of these findings is that neither personality traits nor disorders have an adverse impact on the outcome of patients with depression treated with this therapy.
Table 5 Multivariate prediction of percentage improvement from personality disorder symptoms, temperament and character, by therapy

| IPT | CBT | |||
|---|---|---|---|---|
| Coefficient | P | Coefficient | P | |
| Clinician interview | ||||
| Personality disorder (yes/no): R 2 | 0.089 | 0.005 | 0.018 | NS |
| Personality disorder severity (4 categories): R 2 | 0.123 | 0.001 | 0.004 | NS |
| Personality disorder symptoms: R 2 | 0.204 | 0.032 | NS | |
| Avoidant symptoms: β | -0.41 | < 0.001 | ||
| Schizoid symptoms: β | -0.19 | 0.058 | ||
| Self-report | ||||
| Temperament: R 2 | 0.180 | 0.049 | ||
| Harm avoidance: β | -0.35 | 0.001 | ||
| Reward dependence: β | 0.21 | 0.035 | ||
| Persistence: β | 0.22 | 0.050 | ||
| Character: R 2 | 0.125 | 0.033 | NS | |
| Self-directedness: β | 0.35 | 0.001 | ||
| Combined interview and self-report: R 2 | 0.257 | No new model | ||
| Harm avoidance: β | -0.25 | 0.017 | ||
| Avoidant symptoms: β | -0.31 | 0.004 | ||
| Schizoid symptoms: β | -0.20 | 0.036 | ||
However, for interpersonal psychotherapy, personality can have a major impact on treatment response in patients with depression. A simple categorical personality disorder diagnosis (yes/no) explains 8.9% of outcome, with those with a personality disorder having a poorer outcome (see Table 2). Using Tyrer's four-point measure of personality disorder severity (Reference TyrerTyrer, 2005) explains 12% of treatment outcome, with a mean improvement of 61% in those with no personality dysfunction declining to a 25% improvement in those with complex personality disorder (i.e. disorders in at least two separate clusters). However, counts of personality disorder symptoms explain 20% of treatment response, with avoidant and schizoid symptoms predicting poor outcome.
The TCI similarly predicts response to interpersonal psychotherapy. Temperament explains 18% of treatment outcome, with high harm avoidance and low reward dependence predicting poor outcome (related respectively to avoidant and schizoid symptoms). Self-directedness explains 12.5% of the treatment outcome. Combining temperament and character scales does not improve on the 18% explained by temperament, as harm avoidance and self-directedness are negatively correlated 0.5.
Finally, the combination of clinician interview and the TCI explains 26% of treatment outcome, with both high harm avoidance and avoidant personality disorder symptoms (despite being correlated 0.52) and schizoid personality disorder symptoms being the significant variables.
Prediction of treatment response across therapies
Table 6 shows the results of multiple regression across therapies for clinician interview and TCI data separately. From the clinician interview data it can be seen that high levels of avoidant personality disorder symptoms contribute to a poorer treatment outcome, and that for both high avoidant personality disorder symptoms and schizoid symptoms there is an interaction with therapy such that those with high personality disorder symptoms do worse with interpersonal psychotherapy.
Table 6 Multivariate prediction of percentage improvement from temperament and character, and personality disorder symptoms across therapies

| R 2 | F | P | |
|---|---|---|---|
| Clinician interview | 0.148 | ||
| Avoidant symptoms | 19.19 | < 0.001 | |
| Avoidant symptoms × therapy | 6.79 | 0.010 | |
| Schizoid symptoms × therapy | 3.72 | 0.056 | |
| Self-report | 0.135 | ||
| Harm avoidance | 9.69 | 0.002 | |
| Reward dependence | 4.85 | 0.029 | |
| Harm avoidance × therapy | 9.63 | 0.002 |
The results with the TCI are generally similar, in that high harm avoidance and low reward dependence are associated with a poorer treatment outcome. There is also an interaction of harm avoidance with therapy, such that for those with high harm avoidance interpersonal psychotherapy is associated with a poorer treatment outcome.
Confounding by severity of depression
In the companion paper (Reference Luty, Carter and McKenzieLuty et al, 2007) it was reported that interpersonal psychotherapy was associated with a poorer outcome in severe depression (MADRS score ≥30). We ran analyses again including severity and severity × therapy. The personality predictors and the severity × therapy findings remained in the final multiple regression, and the inclusion of the severity × therapy variable added approximately a further 3% to the variance explained by the personality predictors of outcome.
DISCUSSION
In this randomised clinical trial we found that neither personality disorder nor personality traits adversely affected the outcome when patients with major depression were randomised to cognitive–behavioural therapy. Conversely, the presence of any personality disorder did adversely affect treatment outcome for patients with major depression randomised to interpersonal psychotherapy. Not unexpectedly, a dimensional measure of personality disorder severity was more statistically powerful in explaining a poorer outcome with interpersonal psychotherapy than a categorical personality disorder diagnosis. Thus, whereas the categorical diagnosis explained 9% of treatment outcome, the dimensional model of personality disorder severity explained 12% of treatment outcome. Self-directedness from the TCI, which is a self-report measure of personality disorder severity, explains a comparable 12.5% of the treatment outcome with interpersonal psychotherapy.
When we moved beyond personality disorder or personality disorder severity, and examined combinations of personality disorder symptoms as dimensions, or temperament, then 18–20% of variance in outcome with interpersonal psychotherapy was explained. With the clinician interview the major determinant of outcome was avoidant symptoms and the secondary determinant was schizoid symptoms. With the TCI temperament scales the major determinant of poorer outcome was high harm avoidance and the secondary determinant was low reward dependence. Given that avoidant symptoms correlated with harm avoidance (0.52) and that schizoid symptoms correlated with low reward dependence (0.38), these are highly congruent findings. It is also noteworthy that a combination of clinician interview and self-report personality variables explains over 25% of the treatment outcome with interpersonal psychotherapy, which suggests that neither method of assessing personality fully captures the personality traits that are influencing the outcome of this therapy.
When outcome was assessed across therapies, personality variables interacted with therapy in predicting outcome. The major finding with clinician interview data was the interaction of therapy with avoidant symptoms, whereas the comparable finding with the TCI was the interaction of therapy with harm avoidance. Either way, this suggests that for patients with avoidant symptoms or high harm avoidance cognitive–behavioural therapy may be superior to interpersonal psychotherapy. Indeed, for patients with depression and avoidant personality disorder, cognitive–behavioural therapy was superior. These findings are congruent with the study by Barber & Muenz (Reference Barber and Muenz1996), whose analysis of data from the National Institute of Mental Health Collaborative Treatment of Depression Study showed cognitive–behavioural therapy to be superior to interpersonal psychotherapy for patients with depression and avoidant personality. Their other finding, that interpersonal psychotherapy was superior to cognitive–behavioural therapy in those with obsessive–compulsive personality (Reference Barber and MuenzBarber & Muenz, 1996), was not replicated by us; indeed, our results tended in the opposite direction.
Our results need to be considered in the context of the strengths and limitations of this randomised clinical trial. Although this is the largest direct comparison of interpersonal psychotherapy and cognitive–behavioural therapy for depression, for analyses of subgroups of patients with depression and specific personality disorders the numbers were perhaps marginal. However, the use of dimensional measures of personality, which tend to be more statistically powerful, produced significant results. The key outcome in this study was percentage improvement in depressive symptoms after 16 weeks of weekly therapy, and the results reported may not be relevant to the prediction of longer-term outcome.
Our finding that personality disorder does not have an adverse impact on treatment response to cognitive–behavioural therapy in depression is consistent with findings that personality disorder does not adversely affect treatment response to antidepressant drugs in depression (Reference MulderMulder, 2002; Reference Kool, Schoevers and de MaatKool et al, 2005). However, it is therefore interesting that personality disorder does adversely affect treatment response to interpersonal psychotherapy. It is also interesting to speculate whether the latter finding extends to other ‘dynamic’ psychotherapies, thus suggesting they should not be treatments of choice for depression in patients with personality disorders. This suggestion would be at odds with the traditional clinical belief that dynamic psychotherapies are indicated for patients with personality disorders.
The finding that high harm avoidance and/or avoidant personality symptoms interfere with the efficacy of interpersonal psychotherapy is consistent with findings that high negative affect or neuroticism is a negative prognostic factor in the treatment of depression. The more original finding that low reward dependence and/or schizoid symptoms decrease treatment response could be interpreted as evidence for interpersonal deficits (Reference Luty, Joyce and MulderLuty et al, 1998), which have been considered the most difficult of the interpersonal problem areas in which to effect therapeutic gain. An alternative way of interpreting the findings regarding schizoid symptoms is that interpersonal psychotherapy, which formulates depression within an interpersonal context, is not indicated in patients who have a low need for interpersonal contact (schizoid and/or low reward dependence).
Even though the two therapies had comparable treatment efficacy for depression, our findings that personality disorder does not adversely affect the outcome for depression treated with cognitive–behavioural therapy but does adversely affect the outcome of treatment with interpersonal psychotherapy suggests that these two psychotherapies may work for different patients or by different mechanisms.
Acknowledgements
We thank Isobel Stevens, Andrea Bartram and Robyn Abbott for their assistance in completing this study. We wish to acknowledge the therapists, Dr Janet Carter, Dr Jenny Jordan, Associate Professor Sue Luty, Dr Alma Rae and Ms Jenny Wilson, and the psychotherapy supervisors and trainers, Dr Eileen Britt, Dr Gini McIntosh and Dr Jan McKenzie. We thank Dr Robert Cloninger for ongoing collaboration in the use of the Temperament and Character Inventory. The study was funded by grants from the Health Research Council of New Zealand.











eLetters
No eLetters have been published for this article.