Since the beginning of systematic outcome assessment in schizophrenia in the 1960s, there has been a wide consensus among researchers and clinicians that capturing psychopathological symptoms alone is not sufficient to reflect relevant outcomes. Particularly for evaluating long-term outcomes, information on the social situation of patients is regarded as essential. Social outcomes assess how patients live, function in society and perform their various roles.
Social outcomes are commonly used throughout healthcare. Yet, there are some specific reasons for their popularity in the treatment of schizophrenia:
-
(a) The disorder is often persistent and affects patients lifelong. Symptoms and the associated distress may fluctuate, and establishing symptoms at any point in time might therefore yield a less relevant picture than the more stable social situation.
-
(b) Longitudinal research has shown that antipsychotic medication can reduce productive symptoms and prevent relapses with subsequent re-hospitalisation. Yet, this effect was not necessarily linked with an improved social situation. Symptom improvement and prevention of relapses alone do not make patients necessarily more likely to complete education, find employment and have social relationships. These outcomes need therefore to be assessed separately from symptoms.
-
(c) As a result of mental health reforms in most high-income countries, the focus of care has shifted from the asylum to the community. Former long-term hospitalised patients were discharged, and there was an interest in how they fared in the community without the institutional protection of the asylum.
-
(d) Mental health reforms have been associated with the formation of patient organisations. Such organisations have acquired an important voice in debates on mental health policies and commonly demand that social outcomes are given more prominence in both research and practice.
Other stakeholder groups often share the perspective of patient organisations. In public and professional debates on mental healthcare, it is often felt that what really matters is how patients live (e.g. whether they do or do not have a job and friends) rather than symptoms of illness.
IMPACT OF TREATMENT ON SOCIAL OUTCOMES
How can treatment of schizophrenia affect social outcomes? There are at least three possible mechanisms:
-
(a) Treatment can improve psychopathological symptoms. A lower symptom level can enable people with schizophrenia to function and perform better in their social context and subsequently achieve more favourable social outcomes.
-
(b) Treatment may have an impact not only on conventional psychopathological symptoms, but also on other cognitive and social deficits that are illness related, but are usually not captured in psychopathological assessments (e.g. the concept of social cognition, which has received wide attention in the past 5 years). If treatment diminishes deficits in social cognition, patients might be more likely to establish and maintain useful relationships and improve social outcomes.
-
(c) Some care interventions focus directly on social outcomes. For instance, vocational rehabilitation programmes may improve the work situation, and the effect is not mediated by a reduction of symptom levels or other illness-related deficits.
Although the latter mechanism mainly applies to a range of social management interventions, the other mechanisms can operate with all forms of psychological, pharmacological and socio-therapeutic treatments. In practice and research, the mechanisms can be intertwined in a complex way and are difficult to disentangle. Yet, it may be concluded that social outcomes can be used to assess the effects of all forms of treatment in schizophrenia.
Because of the indirect nature of the potential treatment effect on social outcomes, they have been termed ‘distal’, as opposed to the more ‘proximal’ outcome criterion of psychopathological symptoms (Reference Watts and PriebeWatts & Priebe, 2002). The effect on social outcomes is less immediate than on symptoms, and achieving improvements in a person's social situation usually takes time.
SOCIETAL CONTEXT AND CEILING EFFECTS
For the analysis of treatment effects on social outcomes, two fundamental issues should be considered. One is the dependency of social outcomes on the societal context. For example, the likelihood of a person with schizophrenia obtaining competitive employment as a result of treatment will heavily depend on societal factors such as the general unemployment rate and legislation for the employment of people with disabilities. Thus, social outcomes will rarely be a function of treatment alone. Another issue when using social outcomes for evaluating treatment is their distribution in the treated sample at baseline. Psychopathological symptoms define the illness and will always be at a considerable level at the beginning of treatment, which leaves room for improvement. To some extent, this also applied to social outcomes in many studies when people with schizophrenia were discharged after long-term hospitalisation or began treatment in very unfavourable circumstances. However, there can be exceptions. It is possible that people have symptoms of schizophrenia but at the same time hold a respectable and satisfactory social position and perform well in different societal roles. In such a case, no treatment can improve the social situation. At best it can help to maintain the current level. Thus, unlike psychopathological symptoms, treatment cannot always aim to improve social outcomes, and whether maintaining the given social situation can be rated a success is a difficult question and depends on the quality of the social situation before treatment.
CONCEPTS OF SOCIAL OUTCOMES
Different concepts have been used to reflect and summarise social outcomes in people with schizophrenia. These include standard of living, quality of life, social integration, social adaptation, social functioning, social integration, needs for care and, more recently, social inclusion. None of these concepts was introduced into psychiatry on the basis of a theoretical model. If a theoretical literature existed in psychology and sociology – e.g. for the quality of life concept – it was rarely considered when new concepts were suggested and new assessment tools were designed in psychiatry.
The reason for introducing a new concept was commonly the intuitive appeal of the term, which then led to efforts to find definitions and, subsequently, develop corresponding assessment tools. There is no universally accepted definition for any of the concepts, and each can be used and has been used in various ways, depending on the perspective and interest of whoever uses them. Since the 1980s researchers have published definitions and taken a pragmatic and often ad hoc approach to developing operationalised methods for the assessment. The operationalisation usually required some focus and narrowing down of the various potential meanings of the concepts. As a result, there is a tendency that all assessment instruments for social concepts lead to a disappointment in at least some stakeholder groups because they do not exactly reflect the specific or vague understanding of the concept in the given group. To a different degree, this has happened whenever new concepts of social outcomes have superseded previous concepts. Books on quality of life and social functioning, the two dominating concepts, were published in the 1990s (Reference Tyrer and CaseyTyrer & Casey 1993; Reference Katschnig, Freeman and SartoriusKatschnig et al, 1997; Reference Priebe, Oliver and KaiserPriebe et al, 1999b ) with limited conceptual and methodological progress since.
OBJECTIVE AND SUBJECTIVE INDICATORS
Whatever concept is used in the assessment of social outcomes, there are objective and subjective indicators. Objective indicators are facts about the social situation, which – at least in theory – can be objectively and unequivocally assessed. These include whether a patient does or does not have employment, a partner, independent accommodation and social contacts. Such ‘hard’ outcomes are transparent, straightforward to interpret and of obvious relevance. Out of all outcome criteria in schizophrenia, they arguably have the highest appeal to the public and user organisations. If a treatment has a demonstrabable positive effect on the employment of patients, to most stakeholders this will be more persuasive of its value than an impact on scales assessing symptoms or other psychological constructs.
Objective indicators are important, widely accepted and relatively easy to establish. Why is it then that they are not more widely used and reported in studies on the outcome of treatment in schizophrenia? There are several reasons:
-
(a) Objective aspects of the social situation are hard to influence and are very ‘distal’ outcome criteria. For example, pharmaceutical companies might argue that influencing the objective social situation is too ambitious an aim for treatment with antipsychotic medication, that demonstrating an impact on the objective social situation would take much longer than the usual length of clinical trials, and that such a criterion would be inappropriate because pharmacological treatments were developed to reduce symptoms, not as ‘employment-finding’ drugs.
-
(b) Objective indicators tend to be difficult to change. Even over longer periods people with schizophrenia will not easily move into competitive employment, find a partner and achieve independent living. In a larger sample some might improve on any one of these criteria, but seldom on all. For meaningful statistical testing of changes over time, the different aspects would have to be combined to have a sufficient frequency of changes and to avoid multiple testing. Interestingly, such a combined measure of objective indicators does not exist.
-
(c) Any outcome criterion may have problems with floor and ceiling effects but this applies particularly to hard social outcomes. People who already are in independent living and competitive employment cannot improve any more, so that these criteria become meaningless as outcomes.
-
(d) Although objective indicators capture hard facts and are usually straightforward to analyse, their interpretation requires values, and these values can vary depending on cultural background, social context and individual perspectives. For example, for most people being in employment is clearly desirable, but how does one assess social outcome in a person who does not want to work and can afford to live on other income? The dependency of the assessment on values is even more obvious with respect to partnership and social contacts. People might choose to live alone rather than being forced into this as a result of illness-related impairment. One solution to this dilemma is to ask patients about their expectations and aspirations, and relate their social situation to their wishes. Following this approach, social isolation would be a negative outcome only if the person would prefer to have more contacts. This, however, goes beyond objective indicators and introduces a subjective dimension.
Subjective indicators comprise patient ratings of feelings, thoughts and views on their social situation. An appropriate description of the full range of social indicators used in different concepts is beyond the scope of this review, but it will focus on quality of life, which is the most frequently used concept in social outcomes in the psychiatric literature.
QUALITY OF LIFE
Since the 1980s, quality of life has been increasingly used as an outcome criterion in psychiatric research. Commonly, objective and subjective indicators are considered. Lehman et al (Reference Lehman, Ward and Linn1982) introduced a measurement approach, which assesses personal characteristics, objective indicators in different domains of life and subjective quality of life in the same life domains. Subjective quality of life represents the person's appraisal of their objective life conditions, mostly captured by rating scales of satisfaction with life domains and life as a whole. The life domains covered usually include work, accommodation, family, social relations, leisure, safety, finances, and physical and mental health. The mean score of the satisfaction ratings – or similar subjective ratings – is taken as the level of subjective quality of life (Reference Priebe, Huxley and KnightPriebe et al, 1999a ).
Patients' appraisal of their life is influenced by three major processes: a comparison with original expectations and aspirations; a comparison with the life situation and achievements of others; and an adaptation over time. The latter two may be particularly relevant for people with chronic schizophrenia, whose peer group is often people with similar impairments, and who may adapt to circumstances that they might have found unsatisfactory many years earlier. As a result, people with persistent disorders who often live in conditions that seem adversarial and unpleasant to clinicians and observers, nevertheless express relative satisfaction with their life (Reference Arns and LinneyArns & Linney, 1993; Reference Awad, Vorauganti and HeslegraveAwad et al, 1997; Reference Katschnig, Freeman and SartoriusKatschnig et al, 1997; Reference Priebe, Oliver and KaiserPriebe et al, 1999b ).
Correlations between objective and subjective indicators are reported to be weak to moderate (ranging from 0.04 to 0.57; Reference Priebe and FakhouryPriebe & Fakhoury, 2007). The low association between objective life situation and patients' subjective appraisal has often been counterintuitive to clinicians and other observers, who subsequently questioned the validity of patient ratings. Yet, if patients are asked to give a subjective appraisal of their situation and express a high satisfaction with how they live, there is hardly any external criterion based on which such an appraisal may be disqualified. Thus, patients' views and satisfaction ratings may look surprising to the independent observer, but need to be respected as subjective indicators.
Assessment instruments
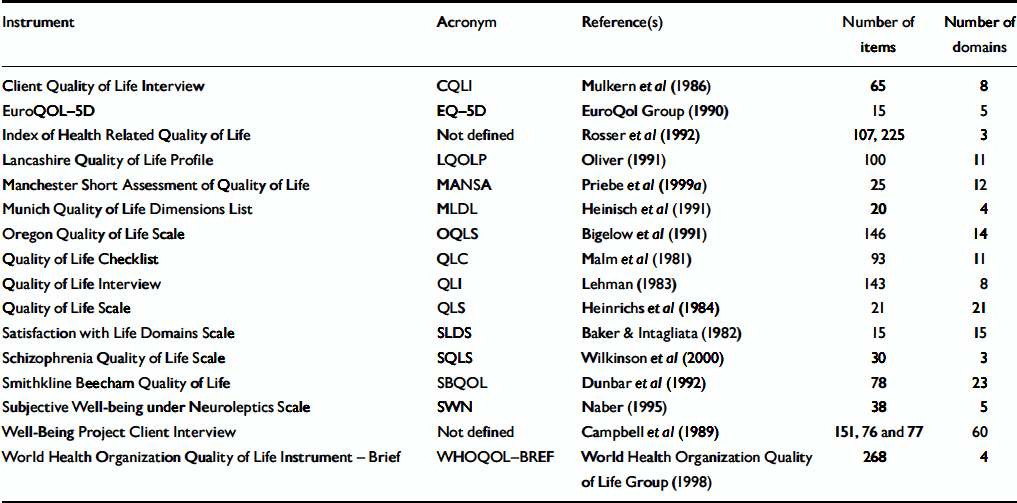
A range of scales, checklists and structured and semi-structured interviews have been developed to assess quality of life in people with schizophrenia. The results of scales assessing symptom levels, particularly of depression, have been repeatedly reported as quality of life scores, although the scales have been developed neither to assess quality of life nor to capture objective and subjective indicators. These proxy measures will not be considered here. Table 1 shows a number of established scales that have been specifically developed to assess quality of life and have been used in people with schizophrenia. The listed assessment instruments for quality of life – and later social functioning – were identified through a non-systematic and non-exhaustive literature search and were selected on the basis of their use in research.
Table 1 Instruments designed for the assessment of quality of life
| Instrument | Acronym | Reference(s) | Number of items | Number of domains |
|---|---|---|---|---|
| Client Quality of Life Interview | CQLI | Mulkern et al (Reference Mulkern, Agosta and Ashbaugh1986) | 65 | 8 |
| EuroQOL-5D | EQ-5D | EuroQol Group (1990) | 15 | 5 |
| Index of Health Related Quality of Life | Not defined | Rosser et al (Reference Rosser, Cottee, Rabin and Hopkins1992) | 107, 225 | 3 |
| Lancashire Quality of Life Profile | LQOLP | Oliver (Reference Oliver1991) | 100 | 11 |
| Manchester Short Assessment of Quality of Life | MANSA | Priebe et al (Reference Priebe, Huxley and Knight1999a ) | 25 | 12 |
| Munich Quality of Life Dimensions List | MLDL | Heinisch et al (Reference Heinisch, Ludwig, Bullinger, Bullinger, Ludwig and von Steinbüchel1991) | 20 | 4 |
| Oregon Quality of Life Scale | OQLS | Bigelow et al (Reference Bigelow, McFarland and Olson1991) | 146 | 14 |
| Quality of Life Checklist | QLC | Malm et al (Reference Malm, May and Dencker1981) | 93 | 11 |
| Quality of Life Interview | QLI | Lehman (Reference Lehman1983) | 143 | 8 |
| Quality of Life Scale | QLS | Heinrichs et al (Reference Heinrichs, Hanlon and Carpenter1984) | 21 | 21 |
| Satisfaction with Life Domains Scale | SLDS | Baker & Intagliata (Reference Baker and Intagliata1982) | 15 | 15 |
| Schizophrenia Quality of Life Scale | SQLS | Wilkinson et al (Reference Wilkinson, Hesdon and Wild2000) | 30 | 3 |
| Smithkline Beecham Quality of Life | SBQOL | Dunbar et al (Reference Dunbar, Stroker and Hodges1992) | 78 | 23 |
| Subjective Well-being under Neuroleptics Scale | SWN | Naber (Reference Naber1995) | 38 | 5 |
| Well-Being Project Client Interview | Not defined | Campbell et al (Reference Campbell, Schraiber and Temkin1989) | 151, 76 and 77 | 60 |
| World Health Organization Quality of Life Instrument - Brief | WHOQOL-BREF | World Health Organization Quality of Life Group (1998) | 268 | 4 |
To assess quality of life in people with schizophrenia, generic, health-related and disease-specific instruments can be used. Generic scales can be applied to the general population and any group of people with health problems, including schizophrenia. Scales often include questions on physical and mental health, but these are not specific to any illness or treatment. Results can be compared across groups with different characteristics and disorders, irrespective of the type of intervention received. Examples are the Quality of Life Interview (QLI; Reference LehmanLehman, 1983), the Lancashire Quality of Life Profile (LQOLP; Reference OliverOliver, 1991) and the Manchester Short Assessment of Quality of Life (MANSA; Reference Priebe, Huxley and KnightPriebe et al, 1999a ).
Health-related quality of life measures are targeted to assess the quality of life of samples with health problems irrespective of the type of illness and interventions. Examples are the Medical Outcome Study Questionnaire (MOS), which was modified and shortened to the 36-item Short-Form General Health Survey (SF–36; Reference Ware and SherbourneWare & Sherbourne, 1992), and the EuroQOL–5D (EQ–5D; EuroQol Group, 1990).
There are also disease-specific measures, and several of these have been designed to assess the quality of life of people with schizophrenia. A widely used disease-specific instrument is the Quality of Life Scale (QLS; Reference Heinrichs, Hanlon and CarpenterHeinrichs et al, 1984), which is a clinician rating scale with acceptable psychometric properties. It was developed to assess symptom levels and functional status of people with schizophrenia in longitudinal studies and trials. Other, less widely used examples of disease-specific scales are the Subjective Well-being under Neuroleptics Scale (SWN; Reference NaberNaber, 1995) and the Schizophrenia Quality of Life Scale (SQLS; Reference Wilkinson, Hesdon and WildWilkinson et al, 2000). These scales tend to capture symptoms, in particular mood symptoms, and side-effects of antipsychotic medication. Although they may be important in influencing quality of life, the labelling of these factors as quality of life is questionable and can blur the concept. It might be preferable to measure symptoms as symptoms and side-effects as side-effects, instead of declaring them to be a direct indicator of quality of life.
There are differences in the use of the scales worldwide. In the USA, the QLS, QLI and the Oregon Quality of Life Scale (OQLS; Reference Bigelow, McFarland and OlsonBigelow et al, 1991) have been more widely used, whereas in Europe the LQOLP, the MANSA and the EQ–5D are more popular. The previous use of an instrument and the availability of data for comparison are powerful determinants of the choice of instrument. Other determinants are the time to complete the instrument, the requirements for training, the properties of the instrument, its overall approach and exact content, and the purpose of the data collection.
Properties of instruments
With respect to instrument properties, the literature usually reports psychometric characteristics such as validity, reliability and objectivity. Yet, these terms are based on psychological test theory and the assumption that there is a well-defined construct that needs to be measured. In the assessment of social outcomes, one might argue that there is no well-defined concept and psychological test theory does not apply. Are social outcomes tested or are they simply assessed and documented? In the latter case, assessment tools are methods to document objective indicators and patient statements. The results on each question can – unlike in psychological test theory – be directly interpreted. Items can be summarised in scores, but the score does not necessarily reflect an underlying construct. To be administered usefully in longitudinal assessments, scales still need to have certain qualities, such as providing stable results over time in the absence of changes in the person's social situation. Yet, this would not be a conventional test–retest reliability because there is no construct to be ‘tested’. This is a theoretical debate which, however, is important for interpreting results of social outcome measures, and should be addressed in the future development of new instruments.
SOCIAL FUNCTIONING
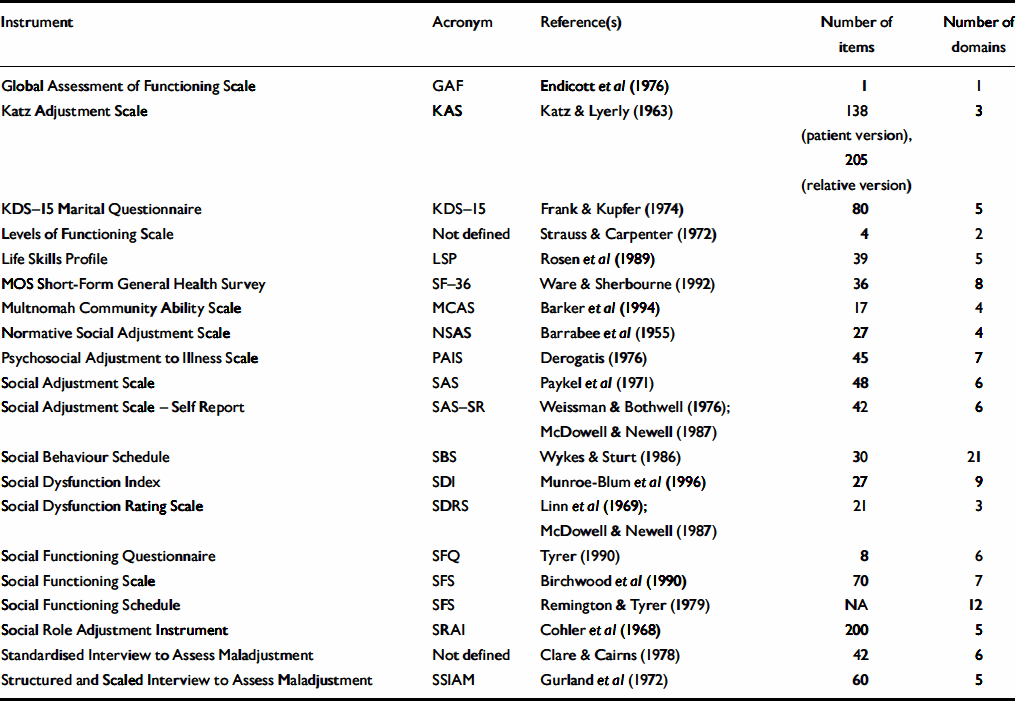
After quality of life, social functioning of people with schizophrenia has received the most extensive attention in the psychiatric literature. Instruments assessing social functioning capture the capacity of a person to function in different societal roles and their actual social performance. Table 2 shows instruments to assess social functioning in people with schizophrenia.
Table 2 Instruments for the assessment of social functioning
| Instrument | Acronym | Reference(s) | Number of items | Number of domains |
|---|---|---|---|---|
| Global Assessment of Functioning Scale | GAF | Endicott et al (Reference Endicott, Spitzer and Fleiss1976) | 1 | 1 |
| Katz Adjustment Scale | KAS | Katz & Lyerly (Reference Katz and Lyerly1963) | 138 | 3 |
| (patient version), 205 | ||||
| (relative version) | ||||
| KDS-15 Marital Questionnaire | KDS-15 | Frank & Kupfer (Reference Frank and Kupfer1974) | 80 | 5 |
| Levels of Functioning Scale | Not defined | Strauss & Carpenter (Reference Strauss and Carpenter1972) | 4 | 2 |
| Life Skills Profile | LSP | Rosen et al (Reference Rosen, Hadzi-Pavlovic and Parker1989) | 39 | 5 |
| MOS Short-Form General Health Survey | SF-36 | Ware & Sherbourne (Reference Ware and Sherbourne1992) | 36 | 8 |
| Multnomah Community Ability Scale | MCAS | Barker et al (Reference Barker, Barron and McFarland1994) | 17 | 4 |
| Normative Social Adjustment Scale | NSAS | Barrabee et al (Reference Barrabee, Barrabee and Finesinger1955) | 27 | 4 |
| Psychosocial Adjustment to Illness Scale | PAIS | Derogatis (Reference Derogatis1976) | 45 | 7 |
| Social Adjustment Scale | SAS | Paykel et al (Reference Paykel, Weissman and Prusoff1971) | 48 | 6 |
| Social Adjustment Scale - Self Report | SAS-SR | Weissman & Bothwell (Reference Weissman and Bothwell1976); McDowell & Newell (Reference McDowell and Newell1987) | 42 | 6 |
| Social Behaviour Schedule | SBS | Wykes & Sturt (Reference Wykes and Sturt1986) | 30 | 21 |
| Social Dysfunction Index | SDI | Munroe-Blum et al (Reference Munroe-Blum, Collins and McCleary1996) | 27 | 9 |
| Social Dysfunction Rating Scale | SDRS | Linn et al (Reference Linn, Sculthorpe and Evje1969); McDowell & Newell (Reference McDowell and Newell1987) | 21 | 3 |
| Social Functioning Questionnaire | SFQ | Tyrer (Reference Tyrer, Peck and Shapiro1990) | 8 | 6 |
| Social Functioning Scale | SFS | Birchwood et al (Reference Birchwood, Smith and Cochrane1990) | 70 | 7 |
| Social Functioning Schedule | SFS | Remington & Tyrer (Reference Remington and Tyrer1979) | NA | 12 |
| Social Role Adjustment Instrument | SRAI | Cohler et al (Reference Cohler, Woolsey and Weiss1968) | 200 | 5 |
| Standardised Interview to Assess Maladjustment | Not defined | Clare & Cairns (Reference Clare and Cairns1978) | 42 | 6 |
| Structured and Scaled Interview to Assess Maladjustment | SSIAM | Gurland et al (Reference Gurland, Yorkston and Stone1972) | 60 | 5 |
NA, not applicable
As in quality of life assessment, the selection of an instrument depends on various factors, and an ideal scale for all purposes does not exist.
EMPIRICAL FINDINGS
The literature on social outcomes in general in people with schizophrenia and on their quality of life specifically is vast. Some results cast light on the strengths and weaknesses of social outcomes, in particular subjective indicators.
Subjective quality of life is less favourable in people with schizophrenia who are younger, male, live alone or are homeless, have a high level of education and are not employed (Reference Lehman, Kernan and DeforgeLehman et al, 1995; Reference Priebe, Warner and HubschmidPriebe et al, 1998; Reference Priebe and FakhouryPriebe & Fakhoury, 2007). Yet, these characteristics explain only a small amount of the variance of subjective quality of life scores in clinical samples. The most consistent and relevant factor influencing subjective quality of life in people with schizophrenia is the level of psychopathological symptoms, in particular mood. The more depressed a person is the lower the subjective quality of life. This applies to both cross-sectional and longitudinal associations (Reference Kaiser, Priebe and BarrKaiser et al, 1997; Reference Priebe, Röder-Wanner and KaiserPriebe et al, 2000). The causality of the association, however, is not straightforward. Depression may lead to a negative appraisal of life, and, vice versa, a negative experience of the life situation may lead to depression. Also, both depression and negative appraisal may be symptoms of the same underlying cognitive and affective processes. In any case, an assessment of subjective indicators of social outcomes needs to control for mood as a potential confounding factor.
Social outcomes have been used widely to evaluate the effects of different treatment methods in schizophrenia. Although programmes aimed at improving the social situation directly, such as vocational rehabilitation and discharge from long-term hospitalisation (Reference Priebe, Hoffmann and IsermannPriebe et al, 2002), can have a substantial effect, such an impact has only rarely been demonstrated for established pharmacological and psychotherapeutic interventions (Reference Corrigan, Reinke and LandsbergerCorrigan et al, 2003; Reference Wiersma, Jenner and NienhuisWiersma et al, 2004).
CONCLUSIONS
Social outcomes have a high intuitive appeal and are called for by different stakeholder groups, including the public and user organisations. However, established scales to assess social outcomes lack a theoretical model, are not based on universally agreed definitions, focus on a limited number of aspects and, subsequently, often lead to disappointment. The distinction between objective and subjective indicators appears to be essential. With respect to objective indicators, any routine documentation and trial should assess whether people have work, how they live, and whether they have social contacts. Future research might benefit from a consistent definition of the categories used so that findings can be compared and benchmarked across studies and services. Statistical analyses would be helped by a method to synthesise different aspects of the objective living situation into one overall index.
The spectrum of measures to assess subjective indicators of social outcomes is huge and growing every year. Some concepts, most notably subjective quality of life and social functioning, have been extensively used in schizophrenia research, yielding data for comparison and specific findings of interest. Their strengths and weaknesses have been well documented. On balance, they should be used to assess outcome and capture the central view of the patients concerned. To use them appropriately, there are at least three requirements: (a) whoever uses such concepts should be aware of the limitations and have a good understanding of what the selected instrument actually assesses, independent of the title of the scale; the contents of scales need to be considered along with practical aspects, when the best instrument for the given purpose is selected; (b) it is difficult to justify the use of more than one instrument to assess subjective indicators of social outcomes in the same study; what the scales assess is conceptually not distinct, and scores of different instruments overlap (Reference Fakhoury, Kaiser and Roder-WannerFakhoury et al, 2002); (c) symptom levels, and in particular mood, need to be assessed and controlled for in any analysis of patient ratings of social outcomes.
Rather than taking new appealing terms and pragmatically developing scales to assess them, future work on improving assessment tools should be based on defined theoretical models and take the existing empirical findings into account.
Within psychiatry, schizophrenia research has led in the development of methods to assess social outcomes. It is widely seen as mandatory to assess social outcomes in epidemiological studies and clinical trials. The literature provides sufficient evidence for the use of assessment instruments and appropriate interpretation of the results. Yet, despite several decades of research, more needs to be done to specify the concepts and develop better assessment instruments. This requires approaches that are qualitatively new, and not just more of the same.







eLetters
No eLetters have been published for this article.