The asylum movement of the 19th century could be regarded as part of a state-guided sanitary movement to cleanse society of the harmful impact of those with mental illness. Although stigmatisation and fear were instrumental in this process, there is now strong evidence for genuine adverse outcomes of schizophrenia on society. Deinstitutionalisation and community care, which have become widespread since the 1970s, have re-exposed the general public to such outcomes, accompanied by a fear of violence, and particularly homicide perpetrated by people with schizophrenia, fuelled by media attention. Suicide and self-harm are much more prevalent outcomes in this group, however, and victimisation of people with schizophrenia is especially neglected. Substance misuse, unemployment and homelessness are also prevalent outcomes of public concern. The prevalence and risk factors for each of these six adverse outcomes in schizophrenia will be reviewed, with an examination of the contribution to society as a whole. There are few validated instruments for measuring these ‘societal outcomes’, but their assessment at both the individual and population level will be considered.
VIOLENCE
Prevalence and risk factors
It is now widely accepted that people with schizophrenia are more likely to behave violently. Varying estimates of the prevalence and relative risk of violence in schizophrenia are dependent on the definition of schizophrenia, the type of violence measured and the location of the study. There is also no consensus as to which variables should be treated as confounding factors or mediators. Unselected birth cohorts have reported relative risks of between 2 and 7 times for serious violence compared with the general population (Reference Tiihonen, Isohanni and RäsänenTiihonen et al, 1997; Reference Arseneault, Moffitt and CaspiArseneault et al, 2000; Reference Brennan, Mednick and HodginsBrennan et al, 2000). People with schizophrenia have been shown to be convicted of a greater number of violent crimes than their neighbours of a similar age (Reference Wallace, Mullen and BurgessWallace et al, 2004) and schizophrenia is overrepresented in prisoners (Reference TeplinTeplin, 1990; Reference Eronen, Hakola and TiihonenEronen et al, 1996). Although schizophrenia independently increases the risk of committing violence (Reference Brennan, Mednick and HodginsBrennan et al, 2000), this risk is increased significantly by comorbid substance misuse (Reference Wallace, Mullen and BurgessWallace et al 2004 ), personality disorder (Reference Moran and HodginsMoran & Hodgins, 2004), a lack of adherence to medication (Reference Swanson, Estroff and SwartzSwanson et al, 1997) and acute psychotic symptoms (Reference TaylorTaylor, 1998).
Risk to society
With most research to date focusing on relative risk, it is encouraging to see estimates of absolute risk emerging in the literature. The population attributable risk (i.e. the fall in levels of violence in society that would occur if violent incidents by people with schizophrenia were discarded) is an approximate calculation. This approach assumes causality between schizophrenia and violent conviction and fails to take account of associated factors, such as substance misuse and personality disorders. Wallace et al (Reference Wallace, Mullen and Burgess2004) estimated that 6–11% of violent convictions are attributable to schizophrenia. Fazel & Grann (Reference Fazel and Grann2006) found a population attributable risk fraction of just 2.3%, which increased to 5% for psychosis. They suggest that in countries with more liberal gun laws, the attributable risk is lower for homicide, but others argue that those with schizophrenia are responsible for 5–10% of homicides irrespective of the baseline homicide rate (Reference Wallace, Mullen and BurgessWallace et al, 2004).
Measurement
Measurement of violent behaviour has relied upon various single or combined sources of information (self-report, informant, case notes, official records). All single sources bias towards underreporting: self-report from a desire for social acceptability or fear of adverse consequences of reporting; informants, often nominated by patients, being unreliable or unaware; and case notes being invariably incomplete. The proportion of violent acts leading to arrest, prosecution and conviction varies with the intensity and quality of policing, the behaviour of the suspect, the availability of diversion to the mental health system and the severity of offence. Most people who are violent are not convicted (Elliott et al, 1986). Only the more serious violent acts lead to conviction; hence the association between schizophrenia and more minor forms of violence is impossible to estimate from official sources.
The recent use of multiple combined measures has improved the detection of violent behaviour. Steadman et al (Reference Steadman, Mulvey and Monahan1998) showed that the detection of violence increased steadily as methods were combined, and reached six times the rate of official convictions alone. Multiple measures require judgements about what constitutes a single violent event and handling inconsistencies between reports.
The definition of violence varies enormously between studies, and most neglect contextual aspects. The MacArthur Community Violence Interview (Reference Steadman, Mulvey and MonahanSteadman et al, 1998) in the USA is an important step towards consistency. It measures lifetime violence, and includes information on recent aggressive behaviour and victimisation. It incorporates a clear and structured definition of different levels of violence and considers the context for each episode. There is also a version for use with collateral sources. Encouragingly, its use is increasing (Reference Elbogen, Van Dorn and SwansonElbogen et al, 2006; Reference Swanson, Van Dorn and MonahanSwanson et al, 2006).
Predicting violence
Measuring violence is less problematic than predicting it. Assessing the risk of violence has become an increasingly important part of clinical practice in psychiatry, with time and resource implications. The clinical usefulness of specific risk assessment procedures depends on: (a) the accuracy of prediction (predictive validity); (b) the applicability to the patient group; and (c) the ability of clinicians to act on the results to reduce predicted risk.
Predictive validity has been at the heart of the debate concerning two differing approaches–actuarial v. clinical risk assessment. The former relies on the identification of largely static risk factors defining at-risk groups within populations while the latter is an individually focused case formulation, which underpins routine clinical practice. To combine the advantages and minimise the disadvantages of the two approaches, several structured risk assessment instruments have been devised and tested (Reference Dolan and DoyleDolan & Doyle, 2000), including the Violence Risk Scale (VRS; Reference Wong and GordonWong & Gordon, 2000)
A statistical assessment of predictive validity is essential both for considering the clinical value of a particular instrument and for comparing instruments. Receiver operating characteristics (ROC) analysis integrates the concepts of sensitivity and specificity, and are relatively independent of the base rate of violence within the population (Reference KronerKroner, 2005). A recent UK study compared the relative efficacy of the Historical Clinical Risk 20 items scale (HCR-20; Reference Douglas, Webster and HartDouglas et al, 2001), the Psychopathy Checklist Screening Version (PCL:SV; Reference Hart, Cox and HareHart, et al, 1995) and the Offender Group Reconviction Scale (OGRS; Reference Copas and MarshallCopas & Marshall, 1998) prospectively over 2 years in a group discharged from a medium secure unit (Reference Gray, Snowden and MacCullochGray et al, 2004). All three instruments were predictive of offending over the follow-up period, but the purely criminogenic scale (OGRS) performed best. This finding that actuarial instruments outperform even structured clinical assessments in mentally disordered offenders is consistent across different settings (Reference Bonta, Law and HansonBonta et al, 1998), but both types of assessment outperform unaided clinical judgement. However, instruments validated in offenders may have less predictive validity in general adult than forensic psychiatry. The HCR–20 has been validated in both settings (Reference Douglas, Webster and HartDouglas et al, 2001).
In clinical practice the usefulness of any risk assessment method will also depend on the implications for intervention. Static factors such as gender and past criminal behaviour offer limited scope to inform clinical intervention. Consideration of dynamic, clinical factors, such as active psychotic symptoms and substance misuse, may contribute more to the usefulness of a risk assessment instrument in clinical practice (Reference MillsMills, 2005), enabling the shift from risk assessment to risk management or risk reduction.
Imperfect risk prediction has serious implications for individuals. Even instruments with relatively high predictive validity will generate both false-positives and false-negatives. The potential implications have been elegantly demonstrated by Buchanan & Leese (Reference Buchanan and Leese2001) who pooled results from 23 studies employing violence risk assessments and concluded that 6 people would need to be detained to prevent one violent act. Routine violence risk assessment might also detract from the consideration of other outcomes, such as those reviewed below.
VICTIMISATION
Prevalence and risk factors
People with severe mental illnesses such as schizophrenia are more likely to be victims of violence than perpetrators of a violent act (Reference Brekke, Prindle and BaeBrekke et al, 2001). Silver (Reference Silver2002) reported that people with severe mental illness and/or personality disorder were more than twice as likely to be the victims of violence than their neighbours. Recent US figures are much higher (Reference Teplin, McClelland and AbramTeplin et al, 2005) and are supported by findings from the Dunedin Study, in which over half of those with schizophreniform disorder reported being assaulted in a 12-month period (Reference Silver, Arseneault and LangleySilver et al, 2005).
It has been suggested that this increased risk of victimisation arises from increased aggressive behaviour. Although this may play a part, the increased risk of victimisation in people with psychosis remains irrespective of the individual's own violent behaviour (Reference Hiday, Swartz and SwansonHiday et al, 2002; Reference SilverSilver, 2002). People with schizophrenia now live within the community and Silver (Reference Silver2002) has shown that their victimisation can be mediated by conflict within social relationships. Elevated rates have also been found to be prospectively associated with comorbid personality disorder, young age at illness onset, previous victimisation and infrequent contact with family members (further details available from K.D.).
Risk to society
Little is known about the impact of victimisation on either the individual or society. It is likely that victims of violence who have schizophrenia will be particularly vulnerable to a range of adverse outcomes, such as homelessness (Reference Lam and RosenheckLam & Rosenheck, 1998), which have significant cost implications.
Measurement
Victimisation is poorly recognised in clinical practice (Reference Cascardi, Mueser and De GiralomoCascardi et al, 1996), often neglected in schizophrenia research and optimal methods of measurement have yet to be established. Two types of instruments have been used. Questionnaires have been designed for use with people with mental disorders, but not specifically to examine victimisation. The MacArthur Community Violence Interview includes a number of questions on victimisation and its context (Reference SilverSilver, 2002). The Lancashire Quality of Life Profile includes items on experience of victimisation, but without detail of the frequency, severity or context (Reference OliverOliver, 1991). Questionnaires have also been designed to examine victimisation in the general population. The National Crime Victimisation Survey was applied to a sample of people with serious mental illnesses by Reference Teplin, McClelland and AbramTeplin et al, 2005 who described the instrument as the most comprehensive available to assess victimisation because it elicits detailed information about each event reported. The instrument required some modification for use with people with mental disorders.
As many acts of violence are not reported to the police (and this may be more likely for victims with mental illnesses) self-report measures will continue to be the best method for obtaining data on victimisation. Reporting past victimisation may be subject to recall difficulties and may not be reliable. Incorporation of ‘bounding interviews’ to establish reference points for future recalling of index events might reduce ‘telescoping’, whereby incidents occurring prior to the required recall period are reported (Reference Teplin, McClelland and AbramTeplin et al, 2005). Collateral sources (family members, keyworkers or residential support staff), although generally likely to underestimate victimisation, may complement participant-reporting and enable some assessment of reliability. As with the measurement of all societal outcomes, the use of multiple sources of information is optimal.
Attention has been focused on establishing the prevalence of victimisation and associated risk factors, rather than understanding in detail its nature, context and impact on those with schizophrenia and other serious mental disorders. Future measures of victimisation should consider factors such as acute symptoms, service contacts and presence of comorbid illness. In addition to exploiting multiple sources, instruments should be specifically designed for people with mental illness and should assess victimisation in detail.
SUICIDE AND SELF HARM
Prevalence and risk factors
Suicide is a significant cause of premature death in people with schizophrenia (Reference Caldwell and GottesmanCaldwell & Gottesman, 1992), with lifetime estimates ranging from 5 to 13% (Reference MilesMiles, 1977; Reference Caldwell and GottesmanCaldwell & Gottesman, 1990; Reference Palmer, Pankratz and BostwickPalmer et al, 2005). Most suicides occur soon after illness onset (Reference Palmer, Pankratz and BostwickPalmer et al, 2005) and may have increased greatly over the past century (Reference Healy, Harris and TranterHealy et al, 2006). Non-fatal acts of self-harm are also increased, with a study of people with chronic schizophrenia finding that 38% had at least one episode of self-harm in a 2- to 12-year follow-up period (Reference Breier, Schreiber and DyerBreier et al, 1991).
A recent meta-analysis identified the following as risk factors for suicide in schizophrenia: recent loss; fear of mental disintegration; agitation or motor restlessness; poor adherence to treatment; drug misuse; and previous depressive disorders and suicide attempts (Reference Hawton, Sutton and HawHawton et al, 2005). Suicidal behaviour in individuals with schizophrenia does not appear to be associated with particular psychotic symptoms. The usual higher incidence of self-harm in females is not present in schizophrenia (Reference Haw, Hawton and SuttonHaw et al, 2005) and, strikingly, people witih schizophrenia from more affluent socio-economic groups are at increased risk of self-harm (further details available from the authors). Approximately 20% of suicides in those under 35 are accounted for by schizophrenia (Reference Appleby, Cooper and AmosAppleby et al, 1999a ).
Measurement
Accurate estimation of suicide rates is difficult; official statistics and coroners' reports are known to underestimate suicide rates, but such errors do not invalidate epidemiological conclusions based on these figures (Reference Sainsbury and JenkinsSainsbury & Jenkins, 1982; Reference Speechley and StavrakySpeechley & Stavraky, 1991). Some estimates rely on proportionate mortality (the percentage of those dead who died by suicide) rather than case fatality rates (the percentage of a sample of patients who will die by suicide). The use of proportionate mortality rates assumes a constant rate of suicide, which given the increased rate of early suicide in schizophrenia might lead to an overestimate of the lifetime suicide risk (Reference Palmer, Pankratz and BostwickPalmer et al, 2005).
A number of risk factors have been consistently associated with suicide in schizophrenia, but their low sensitivity and specificity, plus the rarity of suicide, diminish their clinical usefulness. Evaluating the predictive power of suicide risk factors in psychiatric in-patients, Powell et al (Reference Powell, Geddes and Howton2000) found several to be strongly associated, but the resulting model was unable to predict the majority of suicides without an unacceptably high false-positive rate.
The definition of self-harm is not well established (Reference SkeggSkegg, 2005). Behaviours vary and there is no consensus on inclusion of suicidal intent, which can be difficult to measure in psychosis. Clinical records underestimate self-harm compared with self-report questionnaires (Reference Hawton, Rodham and EvansHawton et al, 2002), but self-report alone may be unreliable. Some studies combine self-report with review of routine case records. Instruments including a limited number of items relating to self-harm have been used to estimate its prevalence in schizophrenia. These include the WHO Life Chart (World Health Organization, 1992), the Structured Clinical Interview for DSM (SCID; Reference Spitzer, Williams and GibbonSpitzer et al, 1994), the Functional Assessment Rating Scale (FARS; Reference Ward and DowWard & Dow, 1995) and the Psychiatric and Personal History Schedule (PPHS; Reference Jablensky, Sartorius and ErnbergJablensky et al, 1992).
The European Parasuicide Study Interview Schedule (EPSIS) has been specifically developed to examine parasuicidal behaviour, suicidal thoughts and associated factors in detail (Reference Platt, Bille-Brahe and KerkhofPlatt et al, 1992), but has only been used to a limited extent in samples with psychotic disorders (Reference Nordentoft, Jeppesen and AbelNordentoft et al, 2002).
SUBSTANCE USE
Prevalence and risk factors
In the USA 40–60% of people with schizophrenia misuse substances, excluding cigarettes (Reference Cantor-Graae, Nordstrom and McNeilCantor-Graae et al, 2001). The pattern of substances misused varies locally but rates are universally higher than in the healthy population (McCreadie et al, 2002). Substances misused include all substance classes and appear to be increasing dramatically (Reference Boutros, Bowers and QuilanBoutros et al, 1998), although proportionally to the rise within the general population (Reference Wallace, Mullen and BurgessWallace et al, 2004).
Substance misuse is increased prior to the onset of schizophrenia. This might be due to causality of psychosis by drugs such as cannabis (Arsenault et al, 2004; Reference Fergusson, Horwood and LynskeyFergusson et al, 2003) or confounders such as a shared underlying neurological vulnerability (Reference Janowsky, El-Yousef and DavisJanowsky et al, 1973; Reference Liberman, Mueser and WallaceLiberman et al, 1986) or antisocial personality disorder (Reference Reiger, Farmer and RaeReiger et al, 1990). Substance misuse is also an outcome of schizophrenia. A substantial number of people use drugs for the first time after the onset of schizophrenia (Reference Hambrecht and HafnerHambrecht & Hafner, 1996). Such patients with dual diagnosis report using street drugs to counter depression and anxiety (Reference Dixon, Haas and WiedenDixon et al, 1990; Reference Addington and DuchakAddington & Duchak, 1997), negative symptoms such as apathy and anhedonia (Reference Pristach and SmithPristach & Smith, 1996), and to assist sleeping and reduce extrapyramidal side-effects. Cocaine use may temporarily reduce negative symptoms (Reference Serper, Alpert and TrujilloSerper et al, 1996). Evidence that people use street drugs to treat positive symptoms is equivocal. People with schizophrenia often feel alienated from society (Sainsbury Centre for Mental Health, 1998) and, rejected by peers, may drift into networks of drug users, who may be more accepting of them (Reference LambLamb, 1982).
Substance misuse is clearly an adverse outcome: people with dual diagnosis are generally younger, less adherent to treatment (Reference Swofford, Kasckow and Scheller-GilkeySwofford et al, 1996), have more positive symptoms (Reference Hambrecht and HafnerHambrecht & Hafner, 1996), more psychiatric admissions (Reference Hunt, Bergen and BahirHunt et al, 2002), higher rates of violence (Reference HodginsHodgins, 1992; Reference Scott, Johnson and MenezesScott et al, 1998), are more likely to die by suicide (Reference Appleby, Shaw and AmosAppleby et al, 1999b ), be unemployed (Reference Seibyl, Satel and AnthonySeibyl et al, 1993), homeless (Reference Drake, Wallach and TeagueDrake et al, 1991; Reference Soyka, Albus and KathmannSoyka et al, 1993) and create excess service costs (Reference Hoff and RosenheckHoff & Rosenheck, 1999). The extent of the damage is underlined by this group's superior premorbid intellectual functioning and socio-economic status compared with people with schizophrenia who do not misuse substances (Reference Kirkpatrick, Amador and FlaumKirkpatrick et al, 1996; Reference Sevy, Robinson and HollowaySevy et al, 2001). Much of the three-fold higher mortality in schizophrenia can be attributed to excess substance misuse, especially cigarette smoking (Reference Brown, Barraclough and InskipBrown et al, 2000).
Measurement
Clinicians and family informants are poor at estimating substance misuse in the absence of dependency, and patients grossly underreport their use (particularly for stimulants and opiates) when compared with toxicology screens (Reference Swartz, Swanson and HannonSwartz et al, 2003). Detection by professionals depends on the level of training in drug/alcohol issues and familiarity with the patient (Reference Ananth, Vandewater and KamalAnanth et al, 1989). Staff suspicion and questioning should be combined with toxicology screens, but these also require staff training and provide only binary outcomes (i.e. used/not used). Saliva tests avoid the risk of patients corrupting samples and awkward supervision, but it remains unclear whether they are more or less accurate than urine tests. Breathaliser tests are practical and valid for measuring alcohol intoxication. For detecting more distal substance use, radioimmunoassay of hair specimens is non-intrusive and reliable (Reference Swartz, Swanson and HannonSwartz et al, 2003).
‘Use’ can be quantified by frequency, quantity or duration, and should be differentiated from ‘misuse’ and ‘dependency’, but for convenience, poorly defined pooled categories have been preferred. Common examples include ‘substance use disorder’ (Reference Mueser and DrakeMueser & Drake, 1998) and ‘problem use’ which has been variably equated to harmful or dependent use combined (Reference McCreadieMcCreadie, 2002), or any use (for example Reference Duke, Pantellis and McPhillipsDuke et al, 2001). Studies vary in the extent of substance inclusion, particularly of legal (nicotine, caffeine, alcohol) and prescribed substances (benzodiazepines, anticholinergics). Substance use diagnoses can refer to current, past or lifetime criteria.
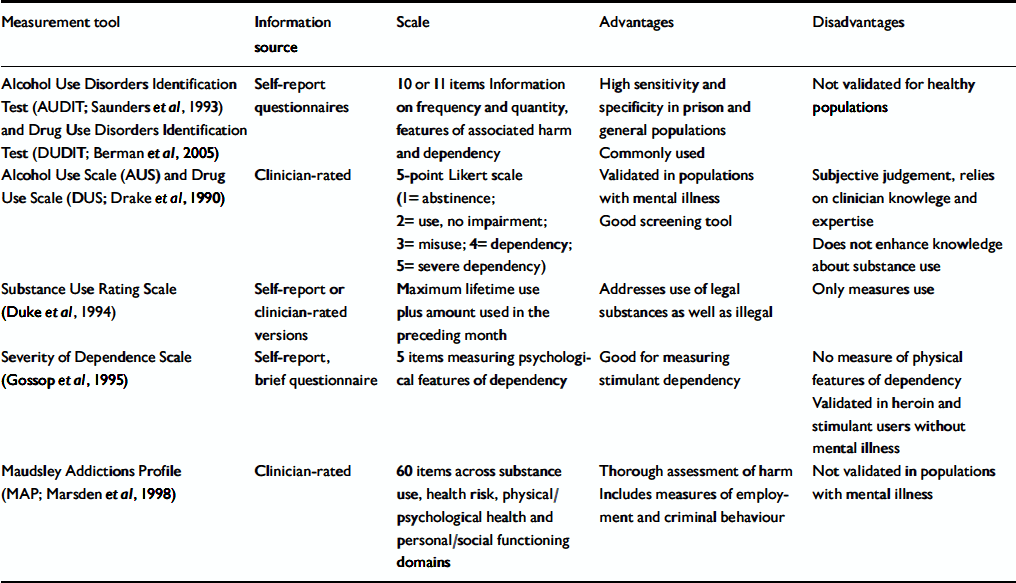
Most research studies use case notes or unstructured interviews. Structured interviews minimise information variance and are more reliable (Reference Blanchard and BrownBlanchard & Brown, 1998). Some standardised measurement tools are listed in Table 1 but these are rarely used outside of research. Multiple measures are increasingly being used (Reference Swartz, Wagner and SwansonSwartz et al, 2006).
Table 1 Standardised tools for measuring substance use in people with mental disorders
| Measurement tool | Information source | Scale | Advantages | Disadvantages |
|---|---|---|---|---|
| Alcohol Use Disorders Identification Test (AUDIT; Reference Saunders, Aasland and BaborSaunders et al, 1993) and Drug Use Disorders Identification Test (DUDIT; Reference Berman, Bergman and PalmstiernaBerman et al, 2005) | Self-report questionnaires | 10 or 11 items Information on frequency and quantity, features of associated harm and dependency | High sensitivity and specificity in prison and general populations Commonly used | Not validated for healthy populations |
| Alcohol Use Scale (AUS) and Drug Use Scale (DUS; Reference Drake, Osher and NoordsyDrake et al, 1990) | Clinician-rated | 5-point Likert scale (1= abstinence; 2= use, no impairment; 3= misuse; 4= dependency; 5= severe dependency) | Validated in populations with mental illness Good screening tool | Subjective judgement, relies on clinician knowlege and expertise |
| Does not enhance knowledge about substance use | ||||
| Substance Use Rating Scale (Reference Duke, Pantelis and BarnesDuke et al, 1994) | Self-report or clinician-rated versions | Maximum lifetime use plus amount used in the preceding month | Addresses use of legal substances as well as illegal | Only measures use |
| Severity of Dependence Scale (Reference Gossop, Darke and GriffithsGossop et al, 1995) | Self-report, brief questionnaire | 5 items measuring psychological features of dependency | Good for measuring stimulant dependency | No measure of physical features of dependency Validated in heroin and stimulant users without mental illness |
| Maudsley Addictions Profile (MAP; Reference Marsden, Gossop and StewartMarsden et al, 1998) | Clinician-rated | 60 items across substance use, health risk, physical/psychological health and personal/social functioning domains | Thorough assessment of harm Includes measures of employment and criminal behaviour | Not validated in populations with mental illness |
Routine screening for substance misuse in people with schizophrenia is an important component of assessing risk and planning treatment. Self-report measures assessing readiness to change are reliable (Reference Carey, Maisto and CareyCarey et al, 2001). However, evidence for effectiveness of psychological interventions targeting substance misuse over standard care for people with schizophrenia has been lacking (Reference Ley, Jeffrey and McClarenLey et al, 2000), but is improving (Reference Haddock, Barrowclough and TarrierHaddock et al, 2003).
HOMELESSNESS
Prevalence and risk factors
Homelessness is a well recognised outcome of schizophrenia but there have been few attempts to quantify it. Rates vary across borders and time. A US community study (Reference Folsom, Hawthorne and LindamerFolsom et al, 2005) found that about a fifth of more than 4000 people with schizophrenia had no fixed address, which was 2.4 times higher than for major depression. The European Schizophrenia Cohort (Reference Bebbington, Angermeyer and AzorinBebbington et al, 2005) found that 32.8% of the British sample had experienced homelessness in their lifetime compared with 8.4% in Germany and 12.9% in France. The rate in London was even higher (43%) and 13.2% of the British sample had experienced rooflessness, despite those who were currently roofless being excluded from the study.
Large US schizophrenia studies consistently find homelessness to be associated with substance misuse and severity of symptoms, but have also found associations with African–American ethnicity (Reference Folsom, Hawthorne and LindamerFolsom et al, 2005), lower global functioning (Reference Olfson, Mechanic and HansellOlfson et al, 1999) and more autistic preoccupations (Reference Opler, White and CatonOpler et al, 2001).
Housing instability in people with schizophrenia predisposes to institutionalisation in prisons and hospitals (Reference Appleby and DesaiAppleby & Desai, 1987), non-adherence with treatment, psychosocial problems (Reference Drake, Wallach and HoffmanDrake et al, 1989) and decreased quality of life (Reference Lehman, Kernan and DeForgeLehman et al, 1995). Physical and sexual abuse are extremely common in both male and female homeless (Reference Wenzel, Koegel and GelbergWenzel et al, 2000). Mortality is more than 3 times higher in the homeless (Reference Hibbs, Benner and KlugmanHibbs et al, 1994). Outcomes may be poorer for homeless people with schizophrenia in urban compared with rural areas (Reference Drake, Wallach and TeagueDrake et al, 1991).
Risk to society
The proportions of homeless people with schizophrenia vary with levels of social and mental health provision, for example 12% for males in Munich (Reference Fichter, Quadflieg and KoniarczykFichter et al, 1999) and 23% for males in Sydney (Teesson et al, 2004), but are higher in urban areas and significantly higher in the female homeless (46% in Sydney; Teesson et al, 2004).
Measurement
‘Rooflessness’ refers to those living on the streets, and defines the group of most public concern but which is hardest to locate or follow-up. Most studies (e.g. Reference Folsom, Hawthorne and LindamerFolsom et al, 2005) use a looser definition of having no fixed address and include people living in hostels and emergency accommodation. Some researchers have further widened the concept to include a spectrum of ‘housing instability’, signifying tenuousness of housing tenure and associated stress (Reference Drake, Wallach and TeagueDrake et al, 1991). This group of so-called sofa-surfers move frequently between friends, family and emergency housing.
There are no valid national databases of housing because of unofficial rental, unregistered housing by friends and family, and the rapid movements of individuals. Case manager rating scales of housing instability have been used, such as a 5-point Likert scale sceening device (Reference Drake, Wallach and TeagueDrake et al, 1991), which rates accommodation from ‘highly supportive’ to ‘highly stressful’. This may help to identify people with housing problems who can then be given a more detailed structured interview
However, people who are living on the streets, especially those with prominent negative symptoms or an itinerant lifestyle, are less likely to be in regular contact with mental health services, thus rates of homelessness in people with schizophrenia may be underestimated. Assertive screening of the homeless for mental illness might reduce the exclusion of this group from mental health services.
UNEMPLOYMENT
Prevalence and risk factors
The European Schizophrenia Cohort (Reference Bebbington, Angermeyer and AzorinBebbington et al, 2005) found that only 11.5% of the British sample were actively employed, including sheltered employment. The French rate was similar (12.9%) but the German much higher (30.3%). Estimates of about 22% have been made in both the USA (Reference Mechanic, Blider and McAlpineMechanic et al, 2002) and Australia (Reference Carr, Lewin and NeilCarr et al, 2004). More encouragingly, the International Study of Schizophrenia (IsoS) found that 37% of people with schizophrenia had received paid work for most of the past 2 years (Reference Harrison, Hopper and CraigHarrison et al, 2001), but attrition rates were high.
The gradual decline in rates of employment over many years leading up to diagnosis in a large Danish population cohort (Reference Agerbo, Bryne and EatonAgerbo et al, 2004) suggests impairment during the prodromal phase. Rates of employment deteriorate further after first presentation (Reference Mechanic, Blider and McAlpineMechanic et al, 2002; Reference Agerbo, Bryne and EatonAgerbo et al, 2004). Among people with schizophrenia, past admission to hospital predicts current unemployment (Reference Munk-Jorgensen and MortensenMunk-Jorgensen & Mortensen, 1992).
Unemployment is associated with decreased quality of life in schizophrenia (Reference Caron, Mercier and DiazCaron et al, 2005). Lewine (Reference Lewine2005) showed that job expectation prior to the onset of schizophrenia significantly correlated with depression and hopelessness, and both were increased in higher socio-economic groups.
Educational attainment is the best protective factor for employment in people with schizophrenia, as in the general population (Reference Mechanic, Blider and McAlpineMechanic et al, 2002). Cognitive functioning is a significant predictor of job tenure (Reference Gold, Godberg and McNaryGold et al, 2002) and response to vocational rehabilitation (Reference McGurk and MueserMcGurk & Mueser, 2004).
Risk to society
The cost of unemployment owing to schizophrenia is considerable. Numbers of American recipients of disability benefits for schizophrenia rose by 35% between 1994 and 2003 (Reference RosenheckRosenheck, 2006). Not surprisingly several initiatives are underway to improve employment in this group. A Cochrane review (Reference Crowther, Marshall and BondCrowther et al, 2001) concluded that supported employment, such as individual placement and support (Reference Bond, Drake and MueserBond et al, 1997), is more effective than pre-vocational training for obtaining competitive employment.
Measurement
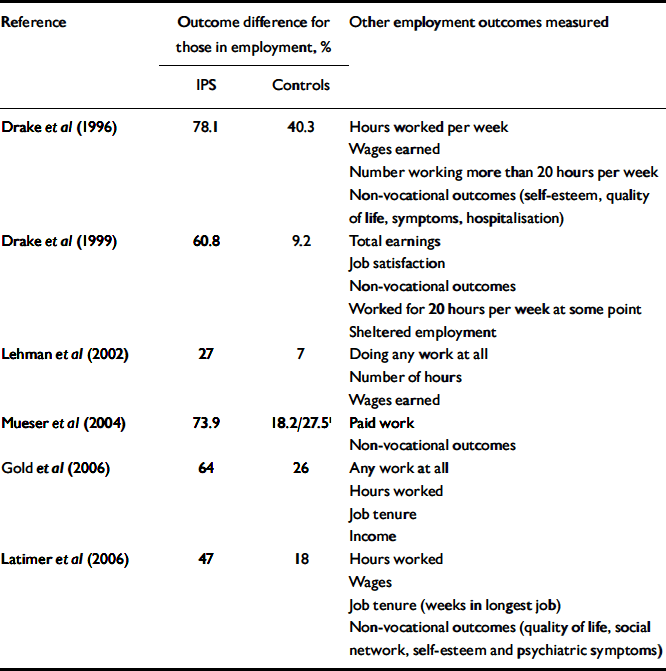
Employment is not an all-or-nothing phenomenon and should be considered in terms of quantity and quality, both for the individual and research purposes. Studies examining the impact of individual placement schemes in assisting attaining employment have used quite consistent measures of employment (Table 2). These studies all principally examined the proportion of people with mental health problems who attained competitive employment, which has been defined as a job in which payment is at least the minimum wage, is not reserved for people with disabilities and fewer than half of the person's co-workers have disabilities (Reference Latimer, Lecomte and BeckerLatimer et al, 2006). However, sheltered employment, although less lucrative and unable to supply the same level of integration, can also increase skills and self-esteem.
Table 2 Studies of the effectiveness of individual placement schemes for people with severe mental illness
| Reference | Outcome difference for those in employment, % | Other employment outcomes measured | ||
|---|---|---|---|---|
| IPS | Controls | |||
| Drake et al (Reference Drake, Mc Hugo and Becker1996) | 78.1 | 40.3 | Hours worked per week | |
| Wages earned | ||||
| Number working more than 20 hours per week | ||||
| Non-vocational outcomes (self-esteem, quality of life, symptoms, hospitalisation) | ||||
| Drake et al (Reference Drake, McHugo and Bebout1999) | 60.8 | 9.2 | Total earnings | |
| Job satisfaction | ||||
| Non-vocational outcomes | ||||
| Worked for 20 hours per week at some point | ||||
| Sheltered employment | ||||
| Lehman et al (Reference Lehman, Goldberg and Dixon2002) | 27 | 7 | Doing any work at all | |
| Number of hours | ||||
| Wages earned | ||||
| Mueser et al (Reference Mueser, Clark and Haines2004) | 73.9 | 18.2/27.5 1 | Paid work | |
| Non-vocational outcomes | ||||
| Gold et al (Reference Gold, Meisler and Santos2006) | 64 | 26 | Any work at all | |
| Hours worked | ||||
| Job tenure | ||||
| Income | ||||
| Latimer et al (Reference Latimer, Lecomte and Becker2006) | 47 | 18 | Hours worked | |
| Wages | ||||
| Job tenure (weeks in longest job) | ||||
| Non-vocational outcomes (quality of life, social network, self-esteem and psychiatric symptoms) | ||||
IPS, individual placement scheme
1. 18.2% for psychosocial rehabilitation and 27.5% for standard care
Quantity of employment can be measured by either hours worked or income earned. Quality of employment can be measured by: (a) job tenure, i.e how long each job is held; working for short periods in a variety of jobs is likely to be less fullfilling and give a lower sense of financial security; (b) job satisfaction; and (c) secondary benefits, such as social contact, quality of life, etc.
The studies described above all used a combination of self-report and keyworker ratings every 6 months. Latimer et al (Reference Latimer, Lecomte and Becker2006) supplemented these interviews with two monthly telephone interviews. However, self-report measures may overestimate levels of employment owing to bias arising from social desirability, denial and grandiosity. Few studies have included employer interviews, which participants may not consent to.
Receiving benefits has been used as a proxy measure for employment. However, some unemployed people are supported by savings or family members/partners and are either ineligible or choose not to collect benefits. Another group collect benefits but work legally part-time, or work occasionally or frequently ‘off the books’.
CONCLUSIONS
Schizophrenia is strongly associated with a range of adverse outcomes, which have an impact at the societal level. There is much intercorrelation between these outcomes, suggesting the possibility of a domino-like effect for an individual person, whereby each outcome leads to another. To limit this downward spiral, it is crucial that all of these outcomes are considered simultaneously. Reducing these outcomes would require implementation of a combination of strategies at national, local and patient levels (e.g. the matrix model of healthcare provision; Reference Tansella and ThornicroftTansella & Thornicroft, 1998).
There are few standardised definitions, let alone validated measures for these outcomes, which makes comparison or collation of research findings problematic. A systematic review of studies proposing implementation of routine mental health outcome measures (Reference SladeSlade, 2002) identified few studies examining any of the outcomes discussed here. For clinical purposes, therefore, the mere consideration of these outcomes, alongside thorough assessment and the use of multiple information sources, allows the best chance of a positive outcome. For research purposes, a collection of validated and brief assessments or even a single instrument to systematically measure these societal outcomes would be extremely useful.







eLetters
No eLetters have been published for this article.